Ultrasound-guided Nerve Blocks in the Emergency Department
March 1, 2018
Reprints
AUTHORS
Caleb P. Canders, MD, Department of Emergency Medicine, University of California, Los Angeles
David A. Morales, MD, Department of Emergency Medicine, University of California, Los Angeles
Sophie W. Sha, University of California, Los Angeles
PEER REVIEWERS
Andrew Kitchen, MD, Department of Emergency Medicine, Carolinas Medical Center, Charlotte, NC
Michael A. Gibbs, MD, FACEP, FAAEM, Professor and Chair, Department of Emergency Medicine, Carolinas Medical Center, Charlotte, NC
EXECUTIVE SUMMARY
- Ultrasound allows the administration of the anesthetic to the nerve area, avoiding vascular injection and providing faster anesthesia.
- Patients receiving nerve blocks should be alert and awake so they can report pain from puncture of the nerve or subsequent compartment syndrome.
- Nerves appear on ultrasound as dark stripes surrounded by a white line. This honeycomb appearance is shown in Figure 2.
- When performing the nerve block, the needle should be kept 1 cm from the nerve. Nerve blocks should not be performed on patients allergic to local anesthetics.
Introduction
Pain management is an important but often challenging task for emergency providers. Oral and intravenous analgesics have inherent risks, which may limit their use in certain populations, such as the elderly. Nonsteroidal inflammatory drugs, for example, can cause kidney injury and gastrointestinal bleeding and are associated with high rates of hypersensitivity reactions.1,2 Opiates can cause sedation, apnea, and hypotension.3,4 In addition, the use of opiates in the emergency department (ED) has been linked to subsequent misuse, addiction, and overdose.5-7 As a result of concerns regarding the safety profiles and addiction potential of analgesics, patients often receive suboptimal pain management in the ED.8,9
Ultrasound-guided nerve blocks offer effective and safe alternatives to systemic analgesics to manage pain in the ED. Studies have shown that with minimal training, emergency providers can perform nerve blocks successfully in both pediatric and adult patients in the prehospital and ED settings.10-18 Ultrasound-guided nerve blocks also can be performed quickly and require only basic equipment that is already available in most EDs. Most importantly, the administration of a nerve blocks for some injuries (e.g., hip fractures) is associated with improved analgesia, decreased intravenous narcotic use, and improved morbidity and mortality when compared to use of intravenous analgesics alone.19,20
This article reviews the literature supporting the use of ultrasound-guided nerve blocks in the ED and describes how to perform some of the most basic nerve blocks, including forearm (median, radial, and ulnar nerves), femoral, and posterior tibial nerve blocks. Additional ultrasound-guided nerve blocks that have been performed in the ED and described in the literature will not be reviewed here. It is assumed that the reader has a basic understanding of ultrasound, although some emergency providers may require additional ultrasound training prior to performing a nerve block independently. By increasing the awareness of and performance of ultrasound-guided nerve blocks in the ED, either alone or in conjunction with other pain management modalities, it may be possible to decrease the use of opiates and other systemic analgesics for pain control.
Landmark-based vs. Ultrasound-guided Nerve Blocks
The use of ultrasound when performing nerve blocks allows the emergency provider to visualize the nerve and its adjacent vascular structures, thereby targeting the injection of the anesthetic and avoiding adjacent blood vessels. Compared to “blind,” landmark-based techniques, ultrasound-guided nerve blocks have been shown to have higher rates of successful sensory block, decreased amounts of anesthetic required to achieve effect, less damage to vascular structures, and faster pain control.12,21-25 The use of ultrasound also helps emergency providers to perform nerve blocks in areas without adequate anatomic landmarks, such as an ulnar nerve block in the mid-forearm.26
Patient Selection
Ultrasound-guided nerve blocks are safe and effective in most patients, including children.11,17,18 In addition, given that they require minimal supplies, ultrasound-guided nerve blocks can be performed in a variety of settings, including combat and disaster settings.13-16 One important contraindication to nerve blocks is an allergy to local anesthetic. In addition, nerve blocks should be performed only on awake and alert patients. (See Table 1.) Patients should understand the risks and benefits of the nerve block, provide consent, and be able to report any pain or paresthesia during the nerve block, which suggests the nerve has been punctured and the needle should be redirected. Depending on the injury, some patients also may be predisposed to compartment syndrome and, therefore, should be able to report unpredicted changes in sensory function. Finally, some blocks are technically challenging and require that the patient remain still and follow instructions.
Table 1. General Contraindications to Performing an Ultrasound-guided Nerve Block
- Allergy to local anesthetic
- Signs of soft tissue infection overlying the area to be blocked
- Neurologic deficit in the affected extremity
- Potential to develop compartment syndrome in the affected extremity
- Altered level of consciousness
General Technique
Prior to Performing the Nerve Block
Prior to starting any nerve block, adjust the height of the bed and position the patient and ultrasound machine to facilitate the procedure. (See Table 2 and Figure 1.) Identify the nerve on ultrasound at the anticipated site of injection and then follow the nerve both proximally and distally. On ultrasound, nerves typically appear as hypoechoic (dark) fascicles surrounded by hyperechoic (bright) connective tissue, also described as a “honeycomb” appearance. (See Figure 2.) For most nerve blocks, we recommend placing a local skin wheal of a rapid-onset anesthetic (e.g., lidocaine) using a 25- to 30-gauge needle over the anticipated point of entry for the block. The skin wheal usually is placed just adjacent to the ultrasound probe, and sterile technique should be used.
Table 2. Equipment Required to Perform an Ultrasound-guided Nerve Block
- Ultrasound machine with probe (usually a high-frequency linear probe)
- Sterile ultrasound probe cover and gel
- Sterile gloves
- Skin disinfectant and antiseptic (e.g., chlorhexidine or povidone-iodine)
- Local anesthetic
- Syringe (size will depend on type of block being performed)
- 18-gauge needle to draw up anesthetic
- 25- to 30-gauge needle to place skin wheal
- Blunt needle for nerve block (see section on needle selection)
Note: Intravascular injection of anesthetic can lead to local anesthetic systemic toxicity. Consider placing the patient on a monitor to assess for tachycardia. Lipid emulsion therapy (e.g., intralipids) should be readily available.
Figure 1. Equipment Required to Perform an Ultrasound-guided Nerve Block
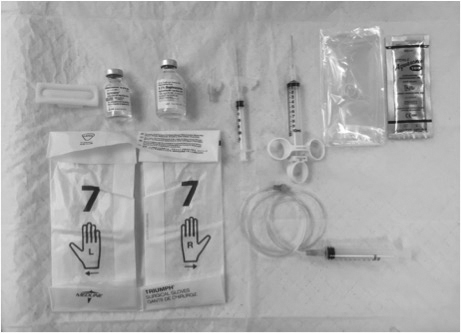
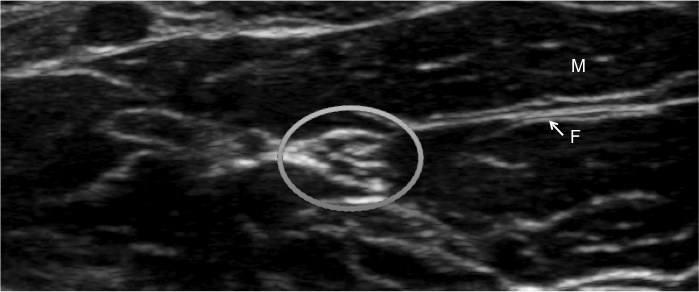
Figure 2. Honeycomb Appearance of a Nerve on Ultrasound, With Adjacent Muscle and Fascia
In-plane vs. Out-of-plane Techniques
Most peripheral nerve blocks are performed using an in-plane technique to ensure visualization of the entire needle, including its tip, throughout the procedure. In the in-plane technique, the provider holds the ultrasound probe in his/her nondominant hand, resting the palm on the patient’s skin for stability. A skin wheal of local anesthetic is placed just medial or lateral to the probe, usually on the opposite side of any vascular structures to avoid accidental puncture during the procedure. Using his or her dominant hand, the provider advances the needle through the skin wheal and toward the nerve. (See Figure 3.) The angle of entry will depend on the depth of the nerve. To avoid injury to neurovascular structures, the needle should not be advanced unless the tip is visualized, which is best achieved when the bevel faces up toward the transducer.27
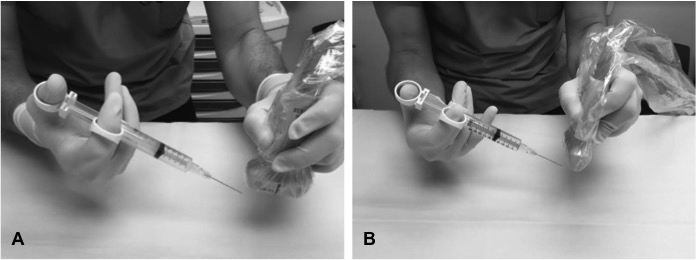
Figure 3. In-plane (A) vs. Out-of-plane (B) Technique for Ultrasound-guided Nerve Block
The out-of-plane technique is reserved for nerve blocks that are restricted by the patient’s anatomy, such as the posterior tibial nerve located behind the medial malleolus. This technique may be more familiar to emergency providers, as it is the technique used most commonly for ultrasound-guided central line placement. In the out-of-plane technique, the provider holds the ultrasound probe with his/her nondominant hand, resting the palm on the patient’s skin for stability. A skin wheal of local anesthetic is placed just adjacent to the probe at its midline. Using his or her dominant hand, the provider advances the needle through the skin wheal and toward the nerve. In this technique, only the tip of the needle is visualized during the procedure.
Regardless of the technique used to visualize the needle during the procedure, the nerve block needle tip should always remain at least 1 cm from the nerve to avoid accidental puncture. Inadvertent injection of the nerve can lead to temporary or permanent sensory or motor deficits.28,29 Anesthetic, which appears hypoechoic (dark) on ultrasound, typically is injected above and below the nerve using “v-shaped” redirections. Redirecting the needle and injecting small aliquots of anesthetic around the nerve to obtain full circumferential spread is ideal although not required for successful sensory block. Many blocks are successful if at least half of the nerve is surrounded by anesthetic. The amount of anesthetic injected depends on the type and concentration of anesthetic used and the nerve being targeted.
One- vs. Two-person Techniques
Nerve blocks can be performed with one or two providers. If only one provider is available, the provider typically holds the ultrasound probe in the nondominant hand and the syringe with a blunt needle in the dominant hand. (See Figure 3.) The use of a control syringe, which allows the provider to inject and aspirate with one hand, simplifies the one-person technique.
The two-person technique generally is easier and allows the performing provider to hold the needle in the dominant hand, allowing greater dexterity during the procedure. The needle is connected via sterile tubing to a syringe, which the assisting provider controls. (See Figure 4.)
Figure 4. Two-person Technique for Ultrasound-guided Nerve Block

Needle Selection
Nerve blocks usually are performed with a blunt needle to decrease the risk of intraneural and intravascular injection.28,29 Sharp needles generally are not used, although they may be safe when performing blocks on small, peripheral nerves (e.g., forearm nerves). Several types of blunt needles can be used for nerve blocks including the “blunt tip” 20- to 22-gauge block needles (ideal for superficial nerves), Quincke tip spinal needles (20- to 22-gauge), and Tuohy epidural needles (useful for deeper blocks, such as femoral nerve blocks). It is advised to use the shortest needle possible to reach the targeted nerve to avoid injury to deeper structures. A caveat to using a blunt needle is that penetrating the skin is more difficult with these needles, so it often is necessary to start perpendicular to the skin and then flatten out the needle.
Anesthetic Selection
The type and amount of anesthetic used to perform nerve blocks depends on the nerve being targeted and the reason for performing the nerve block. A rapid-onset, short-acting anesthetic, such as lidocaine, is adequate to facilitate quick procedures, such as suturing or reductions. Long-acting anesthetics, such as bupivacaine and ropivacaine, are preferred to manage pain associated with fractures, including hip fractures. Of note, mepivacaine and bupivacaine may cross the placenta and are contraindicated in pregnancy (Category C).30,31 See Table 3 for onset time, duration, and doses of commonly used anesthetics.
Table 3. Common Anesthetics Used to Perform Nerve Blocks
Anesthetic |
Onset Time |
Duration |
Maximum Dose (maximum total) |
|
3% 2-Chloroprocaine |
5-10 min |
≤ 1 hour |
11 mg/kg (800 mg) |
|
1% Lidocaine without epinephrine |
1-2 min |
≤ 1 hour |
4 mg/kg (300 mg) |
|
1% Lidocaine with epinephrine |
1-2 min |
2 hours |
7 mg/kg (500 mg) |
|
1.5% Mepivacaine |
3-20 min |
2-3 hours |
7 mg/kg (400 mg) |
|
0.5% Bupivacaine |
2-10 min |
2-6 hours |
2 mg/kg (175 mg) |
|
1% Ropivacaine |
15-30 min |
4-8 hour |
3 mg/kg (300mg) |
Documentation
All ultrasound-guided nerve blocks require proper documentation in the medical record. This includes the clinical examinations prior to and after the nerve blocks, sterile preparation, the type and amount of anesthetic used, the time of injection (to monitor longer blocks), and any complications.
Local Anesthetic Systemic Toxicity
Local anesthetic systemic toxicity (LAST) occurs when a local anesthetic is injected intravascularly, leading to a dose-dependent blockade of sodium channel receptors in the cardiovascular and central nervous systems.32 Patients with mild symptoms may report oral tingling, nausea, tinnitus, or metallic taste. Patients with severe symptoms may develop seizures, bradycardia, arrhythmias, respiratory depression, and cardiac arrest. Patients with severe LAST should be treated with a 1.5 mL/kg bolus of lipid emulsion therapy, followed by a continuous infusion at 0.25 mL/kg per minute.32,33 Patients with persistent cardiovascular collapse can be given repeat boluses of lipid emulsion therapy. Seizures associated with LAST are treated with benzodiazepines.32
Forearm Nerve Blocks
Hand and forearm injuries are common complaints seen in the ED. Three major nerves, the median, ulnar, and radial nerves, innervate the hand and forearm distal to the elbow. Forearm nerve blocks can be performed to manage pain associated with lacerations, burns, fractures, dislocations, and other acute injuries.10 Forearm nerve blocks do not provide anesthesia to the volar forearm or wrist and, therefore, are not indicated for most wrist fractures. Forearm nerve blocks can be performed in isolation or in combination, depending on the distribution of pain. (See Figure 5.) Studies have shown that emergency providers can learn to perform ultrasound-guided forearm nerve blocks after minimal training and as few as five supervised scans.10 Each forearm nerve blocks takes approximately 5-10 minutes to perform, and patients who receive forearm nerve blocks usually report high satisfaction with the procedure and rarely require additional analgesia.10 Similarly, forearm nerve blocks are easy to perform and have high rates of success and patient satisfaction in children.11 As a result, some EDs have incorporated ultrasound-guided nerve blocks into pain management protocols for certain forearm injuries.34,35
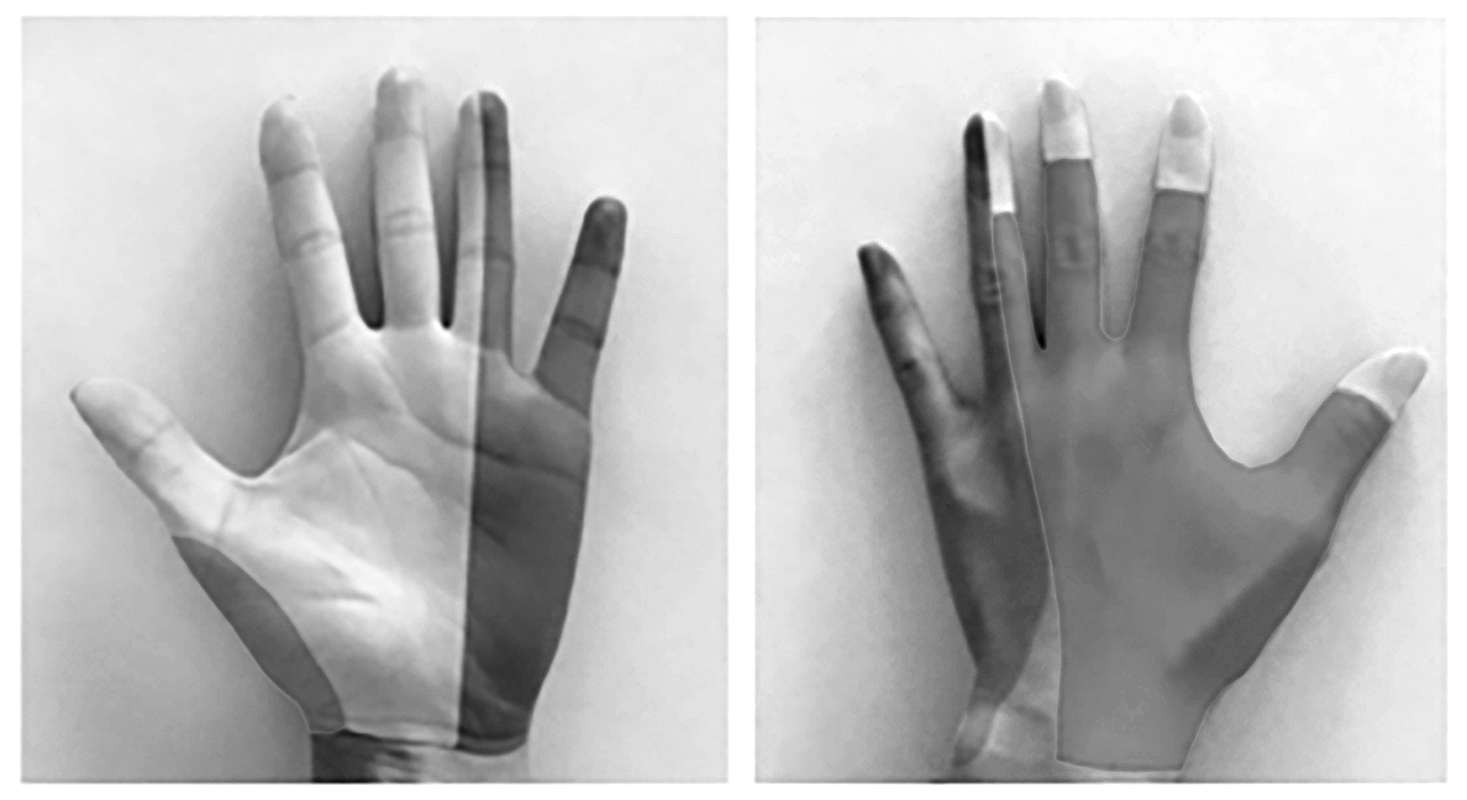
Figure 5. Sensory Distributions of the Median (white), Radial (light gray), and Ulnar (dark gray) Nerves in the Hand
Median Nerve Block: Anatomy and Technique
The median nerve lies between the flexor carpi radialis and palmaris longus tendons at the wrist. It supplies sensory innervation to the thumb, index finger, third finger, lateral aspect of the ring finger, and palm. It provides motor innervation to the thenar muscles and first and second lumbricals. Unlike the ulnar and radial nerves, the median nerve usually is not associated with a vascular structure.
- The patient lies supine with his or her hand resting on a hard surface (e.g., Mayo stand).
- Place the ultrasound machine on the side that is opposite the affected extremity, facing the provider. (See Figure 6A.)
- Hold a high-frequency linear probe in transverse orientation over the midline of the volar wrist to identify the median nerve. (See Figure 6B.) In general, the median nerve becomes easier to differentiate from the flexor tendons as one moves proximally from the wrist crease. Except in rare cases, there is no artery associated with the nerve. The block typically is performed in the mid-forearm, where the median nerve can be distinguished from adjacent flexor digitorum superficialis and flexor digitorum profundus muscles.
- After identifying the nerve, prepare the skin with a disinfectant and antiseptic. Use sterile technique and place a skin wheal, as previously described.
- Given that there usually is not a vascular structure associated with the median nerve, the provider can approach it from the medial or lateral aspect. Advance the needle through a skin wheal as previously described and inject 3-5 mL of anesthetic above and below the nerve using “v-shaped” redirections.
Figure 6 A, B. Median Nerve Block
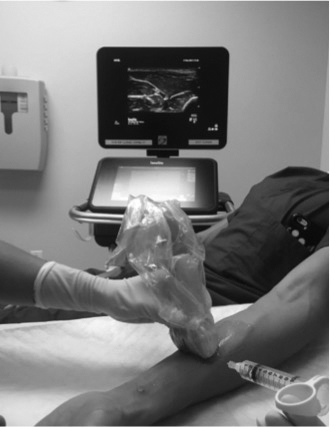
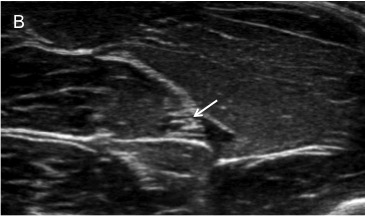
The median nerve can be approached from the medial or lateral direction. The patient and ultrasound machine are positioned so that the provider holds the ultrasound probe in his or her nondominant hand and the needle in his or her dominant hand with a clear view of the ultrasound screen (A). On ultrasound, the median nerve (arrow) appears as hypoechoic (dark) fascicles surrounded by hyperechoic (bright) connective tissue (B).
Radial Nerve Block: Anatomy and Technique
Branches of the radial nerve pass over the styloid process of the radius and the anatomic snuffbox at the wrist. The radial nerve provides sensory innervation to the lateral half of the dorsum of the hand and the dorsal thumb. It provides motor innervation to the extensor muscles in the dorsal forearm. The radial nerve travels medial to the radial artery and vein.
- The patient lies supine with his or her hand resting on a hard surface (e.g., Mayo stand).
- Place the ultrasound machine on the side that is opposite the affected extremity, facing the provider. (See Figure 7A.)
- Hold a high-frequency linear probe in transverse orientation over the radial aspect of the volar wrist. First, identify the radial artery, which appears as a thick-walled, pulsatile, hypoechoic (dark) structure. Second, identify the radial nerve, which lies lateral to the radial artery. (See Figure 7B.) It may be easier to identify the radial nerve by moving proximally from the wrist crease.
- After identifying the nerve, prepare the skin with a disinfectant and antiseptic. Use sterile technique and place a skin wheal, as previously described.
- To avoid puncture of the radial artery and vein, approach the radial nerve from the lateral aspect of the wrist. Advance the needle through a skin wheal as previously described. Typically, the needle is advanced at a shallow angle, given the superficial depth of the nerve. Inject 3-5 mL of anesthetic above and below the nerve.
Figure 7 A, B. Radial Nerve Block
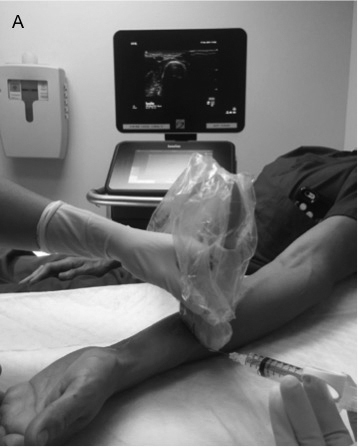
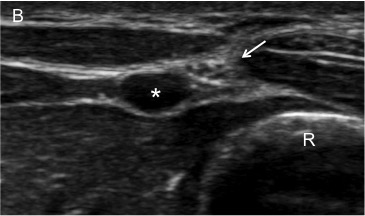
The radial nerve (arrow) is approached from the lateral direction to avoid puncture of the radial artery (star). On ultrasound, the radius (R) appears as a hyperechoic (bright) line with shadowing.
Ulnar Nerve Block: Anatomy and Technique
The ulnar nerve travels deep to the flexor carpi ulnaris at the wrist. It provides sensory innervation to the fifth finger, medial aspect of the ring finger, and the medial hand. It provides motor innervation to the hypothenar and interossei muscles, adductor pollicis, deep head of the flexor pollicis brevis, and the medial two lumbrical muscles. Of note, dorsal and palmar cutaneous branches of the ulnar nerve arise 5-10 cm proximal to the wrist. As a result, ulnar nerve blocks are most successful when performed in the mid-forearm area.26,36
- Given that the ulnar nerve lies medial to its associated vascular structures, the nerve block needle should approach the nerve from the medial aspect of the wrist. This can make patient positioning more challenging than for the other forearm nerve blocks. One method is to stand to the inside of the patient’s shoulder on the affected side, facing away from the patient and positioning the patient with his or her arm extended and elbow supinated. (See Figure 8A.) Another method is to face the patient and position the patient with his or her arm flexed and elbow supinated. (See Figure 8B.)
- Hold a high-frequency linear probe in transverse orientation over the ulnar aspect of the volar wrist to identify the ulnar nerve. First, identify the ulnar artery, which appears as a thick-walled, pulsatile, hypoechoic (dark) structure. Second, identify the ulnar nerve, which lies medial to the ulnar artery. (See Figure 8C.) It may be easier to identify the ulnar nerve by moving proximally from the wrist crease.
- After identifying the nerve, prepare the skin with a disinfectant and antiseptic. Use sterile technique and place a skin wheal, as previously described.
- To avoid puncture of the ulnar artery and vein, approach the ulnar nerve from the lateral aspect of the wrist. Advance the needle through a skin wheal as previously described. Typically, the needle is advanced at a shallow angle, given the superficial depth of the nerve. Inject 3-5 mL of anesthetic above and below the nerve.
Complications of Forearm Nerve Blocks
Ultrasound-guided forearm nerve blocks rarely have immediate or long-term complications.10 As with all nerve blocks, there are risks of introducing a skin or soft tissue infection, vascular puncture/hematoma, intraneuronal injection, and LAST.
Figure 8 A, B, C. Ulnar Nerve Block
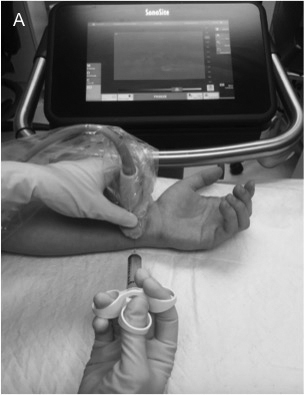
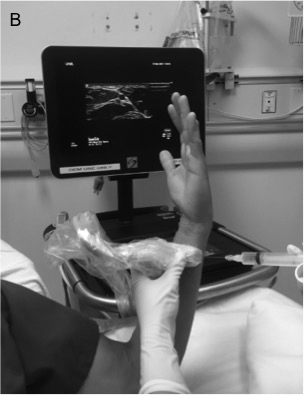
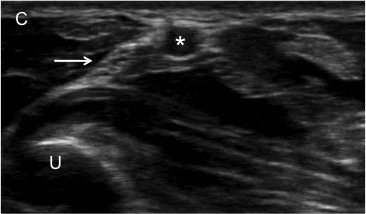
The ulnar nerve (arrow) is approached from the medial direction to avoid puncture of the ulnar artery (star). The patient can be positioned with his or her arm extended and supinated (A) or flexed and supinated (B). On ultrasound, the ulna (U) appears as a hyperechoic (bright) line with shadowing.
Femoral Nerve Blocks
Ultrasound-guided femoral nerve blocks are performed by emergency providers to provide analgesia for intra- and extracapsular hip fractures.37-39 Femoral nerve blocks do not provide analgesia to the lower leg or foot. Uncontrolled pain in patients with hip fractures is associated with increased delirium, poor functional recovery, and increased mortality.40-42 As a result, femoral nerve blocks are an important adjunct to pain control in patients with hip fractures and a procedure that is endorsed by the American Academy of Orthopaedic Surgeons.43 In addition, ultrasound-guided femoral nerve blocks can be performed successfully after minimal training, require little time to complete, have few complications, and usually are successful after a single attempt.38,39,44 Femoral nerve blocks also are safe and effective for controlling pain in pediatric patients with femur fractures and may reduce the need for intravenous analgesics in these patients.20,45,46 Despite this, there is evidence that the use of femoral nerve blocks is underutilized in children.47
Femoral Nerve Block: Anatomy and Technique
The femoral nerve arises from the lumbar plexus (L2-4) and passes below the inguinal ligament, lying 1-2 cm lateral to the femoral artery at the inguinal crease. Inferior to the inguinal ligament, the femoral nerve bifurcates into anterior and posterior branches. The anterior branch provides sensation to the anterior, medial, and lateral thigh and hip, and motor function to the sartorious and pectineus muscles. (See Figure 9.) The posterior branch provides sensation to the knee and medial aspect of the lower leg and motor function to the quadriceps muscle.
Figure 9. Sensory Innervation of the Femoral Nerve in the Lower Extremity
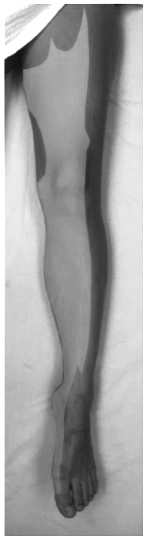
Figure 10 A, B. Femoral Nerve Block
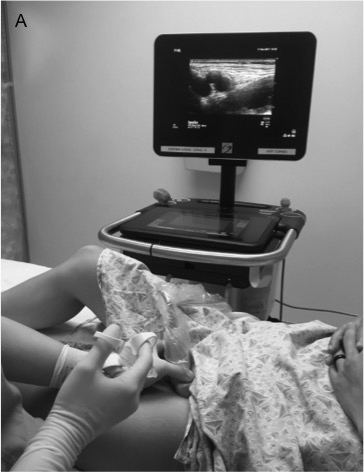
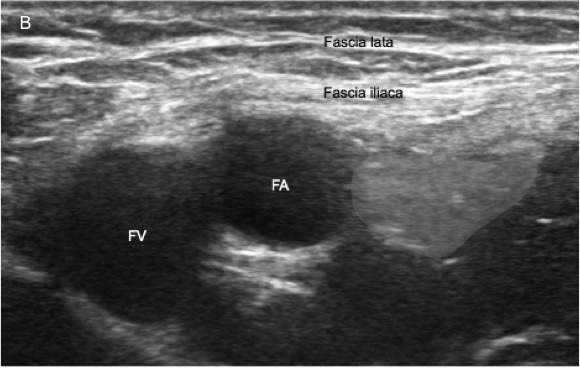
The provider holds the linear probe in his or her nondominant hand in the patient’s inguinal crease in transverse orientation and approaches the femoral nerve from the lateral direction to avoid puncture of the femoral vessels. On ultrasound, the femoral nerve is seen lateral to the femoral artery (FA) and vein (FV). The fascia lata and fascia iliaca appear as hyperechoic (bright) lines overlying the neurovascular structures.
- The patient lies supine with the affected hip in slight abduction. Excess adipose tissue can be pulled out of the inguinal crease superiorly with tape.
- Place the ultrasound machine on the side that is opposite the affected extremity, facing the provider. (See Figure 10A.)
- Hold a high-frequency linear probe in transverse orientation over the inguinal crease, producing an ultrasound image of the femoral vessels and nerve in cross-section. (See Figure 10B.) The femoral vein is the most medial and appears as a thin-walled, collapsible hypoechoic (dark) structure. The femoral artery lies between the femoral vein and nerve and appears as a thick-walled, pulsatile, hypoechoic structure. The femoral nerve lies most lateral and appears as a 3-10 mm, triangular, hyperechoic (bright) structure. It lies deep to two hyperechoic fascial layers: the fascia lata (which surrounds all of the femoral neurovascular structures) and fascia iliaca (which only surrounds the femoral nerve).
- The ideal location to perform a femoral nerve block is at a site below the inguinal ligament where there is a single femoral artery, i.e., proximal to where it divides into the superficial and deep (profunda) branches.
- After identifying the nerve, prepare the skin with a disinfectant and antiseptic. Use sterile technique and place a skin wheal, as previously described.
- To avoid puncture of the femoral vessels, approach the femoral nerve from the lateral aspect of the ultrasound probe, using the in-plane technique. A long, blunt needle (e.g., 20-gauge Tuohy epidural needle) generally is used. Advance the needle through a skin wheal placed approximately 1 cm lateral to the probe. The angle of needle entry depends on the depth of the nerve, but it generally is at 45 degrees to the skin.
- The provider may feel two “pops” as the needle advances through the two layers of fascia. Once the needle is deep to the fascia iliaca, aspirate back on the needle to ensure it is not in a vessel. Remain at least 1 cm lateral to the femoral nerve to avoid intraneuronal injection.
- Inject 10-20 mL of anesthetic, in 3-5 mL aliquots, above and below the nerve until the nerve is surrounded by hypoechoic anesthetic.
Complications
Ultrasound-guided femoral nerve blocks rarely have immediate or long-term complications.10 Failure to penetrate the fascia iliaca is a common pitfall and may lead to inadequate pain relief. As with all nerve blocks, there are risks of introducing a skin or soft tissue infection, vascular puncture/hematoma, intraneuronal injection, and LAST. Puncture of the femoral nerve during the procedure can cause a painful, transient spasm of the quadriceps muscle (“patellar kick”). Following the procedure, the patient may have an increased risk of falls due to the weak and insensate limb.48
Posterior Tibial Nerve Blocks
Ultrasound-guided posterior tibial nerve blocks provide pain relief to patients with calcaneal fractures and injuries to the plantar foot (e.g., lacerations, foreign bodies). These areas often are difficult to anesthetize with local infiltration.49,50 Posterior tibial nerve blocks alone do not provide adequate analgesia for ankle fractures; however, they can be supplemented with other regional blocks for this purpose. Compared to landmark-based techniques, the use of ultrasound-guidance when performing a posterior tibial nerve block has been shown to increase block success rate, decrease the use of adjunct analgesics, and decrease the risk of nerve injury.51-53 Given the superficial location of the nerve, posterior tibial nerve blocks are relatively straightforward to perform and are considered a “beginner-level” block by anesthesiologists.51 One potential contraindication to this type of block is compartment syndrome of the foot, which occurs in 10% patients with calcaneal fractures, because of its effect on the clinical examination.54,55 Therefore, discussion should occur with an orthopedist or podiatrist prior to performing the block.
Posterior Tibial Nerve Block: Anatomy and Technique
The sciatic nerve bifurcates into the posterior tibial and common personal nerves at the popliteal fossa. The posterior tibial nerve travels with the posterior tibial artery in a neurovascular bundle between the superficial and deep compartments of the lower leg. At the ankle, this bundle passes posterior to the medial malleolus. Distal to the ankle, the posterior tibial nerve splits into the medial and lateral plantar nerves. The posterior tibial nerve is a mixed motor and sensory nerve. It provides motor innervation to the flexor muscles of the ankle and foot and sensory innervation to parts of the heel and the majority of the sole of the foot. (See Figure 11.) It does not innervate the lateral heel or extreme medial or lateral aspects of the proximal foot, which are innervated by the sural, saphenous, and sural nerves, respectively.
Figure 11. Sensory Innervation of the Posterior Tibial Nerve in the Foot
Figure 12 A, B. Posterior Tibial Nerve Block
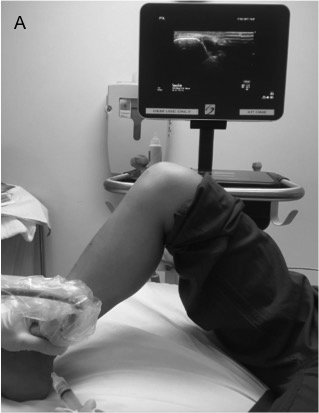
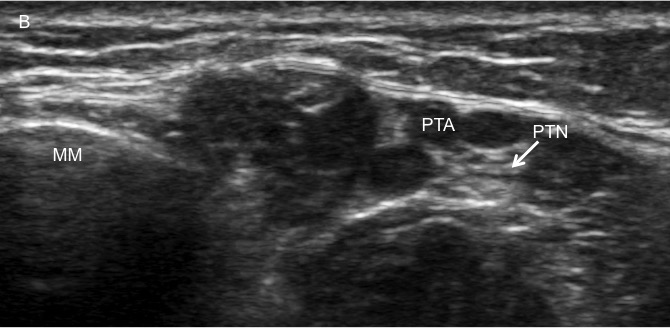
The provider holds the linear ultrasound probe in transverse orientation over the medial leg, proximal to the medial malleolus (MM). On ultrasound, the posterior tibial nerve (PTN) is seen posterior to the medial malleolus and posterior tibial artery (PTA) and vein.
- The patient lies supine with the affected lower extremity externally rotated at the hip and flexed at the knee. Elevate the affected foot with pillows or other supports. Alternatively, the patient can lie on the affected side (i.e., lateral decubitus) with the medial ankle exposed and the unaffected lower extremity held out of the way.
- Place the ultrasound machine on either side of the patient, facing the provider. (See Figure 12A.)
- Hold a high-frequency linear probe in transverse orientation to the long axis of the leg, approximately 3 cm proximal to the medial malleolus. This produces an ultrasound image of the hyperechoic (bright) medial malleolus, hypoechoic (dark) posterior tibial artery, and hyperechoic posterior tibial nerve. (See Figure 12B.) The posterior tibial nerve typically runs posterior to the artery, lies approximately 1-2 cm below the skin, and is 3 mm in diameter.
- After the nerve is identified, prepare the skin with a disinfectant and antiseptic. Use sterile technique, as previously described.
- The nerve block is easiest to perform using an out-of-plane technique, given that the medial malleolus and Achilles tendon often block an in-plane approach anteriorly and posteriorly, respectively. For an out-of-plane technique, center the posterior tibial nerve on the screen and place a local skin wheal just adjacent to the middle of the probe. Using a blunt needle for the block, enter the skin at a steep angle from the posterior direction, 1 cm adjacent to the probe.
- Visualizing the needle tip at all times, advance the needle toward the posterior tibial nerve and avoid the posterior tibial artery. Remain at least 1 cm lateral to the nerve to avoid intra-neuronal injection.
- Inject 5-8 mL of anesthetic in 1-2 mL aliquots, above and below the nerve, until the nerve is surrounded by hypoechoic anesthetic.
Complications
Ultrasound-guided posterior tibial nerve blocks rarely have immediate or long-term complications. As with all nerve blocks, there are risks of introducing a skin or soft tissue infection, vascular puncture/hematoma, intraneuronal injection, and LAST.
Additional Nerve Blocks in the Emergency Setting
Other ultrasound-guided nerve blocks that have been performed by emergency providers and described in the literature include:
- Interscalene nerve block for humerus fracture, shoulder dislocation, and elbow fracture/dislocation (beware that this block has a high risk of temporary hemidiaphragm paralysis)56,57;
- Axillary nerve block for deltoid abscess incision and drainage58;
- Supracondylar radial nerve block for distal radius fracture and reduction59;
- Popliteal sciatic nerve block for injuries below the knee60;
- Intercostal blocks for rib fractures, chest tube placement, and thoracotomy61;
- Transversus abdominis plane blocks for abdominal wall procedures (e.g., abscess incision and drainage), pelvic ring fractures, and pancreatitis62-64;
- Greater auricular nerve blocks for ear lacerations and abscess drainage65;
- Dorsal penile block for paraphimosis and priapism.66
Conclusion
Pain management is an essential aspect of emergency care. However, in many circumstances, systemic analgesics are contraindicated or inadequate at controlling pain. Ultrasound-guided nerve blocks offer safe, effective, and easy-to-perform alternatives to pain control that are within the scope of practice of emergency providers. While some hospitals already have instituted pain management protocols that include ultrasound-guided nerve blocks for specific injuries, such as hip fractures and hand blast injuries, some providers may be hesitant to perform blocks because they are unfamiliar with ultrasound or have misconceptions about the efficacy of blocks.34,35 This article provides step-wise instructions on how to perform common ultrasound-guided nerve blocks, including forearm, femoral, and posterior nerve blocks, which have been shown to be easy to learn, quick to perform, and successful at managing pain, and, therefore, should be adopted into routine clinical use in the ED.
REFERENCES
- Harirforoosh S, Asghar W, Jamali F. Adverse effects of nonsteroidal antiinflammatory drugs: An update of gastrointestinal, cardiovascular and renal complications. J Pharm Pharm Sci 2013;16:821-847.
- Aun MV, Blanca M, Garro LS, et al. Nonsteroidal anti-inflammatory drugs are major causes of drug-induced anaphylaxis. J Allergy Clin Immunol Pract 2014;2:414-420.
- Chen A, Ashburn MA. Cardiac effects of opioid therapy. Pain Med 2015;16 (Suppl 1):S27-31.
- Dahan A, Aarts L, Smith TW. Incidence, reversal, and prevention of opioid-induced respiratory depression. Anesthesiology 2010;112:226-238.
- Poon SJ, Greenwood-Ericksen MB. The opioid prescription epidemic and the role of emergency medicine. Ann Emerg Med 2014;64:490-495.
- Hoppe JA, Nelson LS, Perrone J, et al. Opioid prescribing in a cross section of US emergency departments. Ann Emerg Med 2015;66:253-259.
- Barnett ML, Olenski AR, Jena AB. Opioid-prescribing patterns of emergency physicians and risk of long-term use. N Engl J Med 2017;376:663-673.
- Platts-Mills TF, Esserman DA, Brown DL, et al. Older US emergency department patients are less likely to receive pain medication than younger patients: Results from a national survey. Ann Emerg Med 2012;60:199-206.
- Smith RJ, Rhodes K, Paciotti B, et al. Patient perspectives of acute pain management in the era of the opioid epidemic. Ann Emerg Med 2015;66:246-252.e1.
- Liebmann O, Price D, Mills C, et al. Feasibility of forearm ultrasonography-guided nerve blocks of the radial, ulnar, and median nerves for hand procedures in the emergency department. Ann Emerg Med 2006;48:558-562.
- Frenkel O, Liebmann O, Fischer JW. Ultrasound-guided forearm nerve blocks in kids: A novel method for pain control in the treatment of hand-injured pediatric patients in the emergency department. Pediatr Emerg Care 2015;31:255-259.
- Sohoni A, Nagdev A, Takhar S, Stone M. Forearm ultrasound-guided nerve blocks vs landmark-based wrist blocks for hand anesthesia in healthy volunteers. Am J Emerg Med 2016;34:730-734.
- Lippert SC, Nagdev A, Stone MB, et al. Pain control in disaster settings: A role for ultrasound-guided nerve blocks. Ann Emerg Med 2013;61:690-696.
- Malchow RJ. Ultrasonography for advanced regional anesthesia and acute pain management in a combat environment. US Army Med Dep J 2009; Oct-Dec:64-66.
- Buckenmaier CC 3rd, Rupprecht C, McKnight G, et al. Pain following battlefield injury and evacuation: A survey of 110 casualties from the wars in Iraq and Afghanistan. Pain Med 2009;10:1487-1496.
- Buckenmaier CC, McKnight GM, Winkley JV, et al. Continuous peripheral nerve block for battlefield anesthesia and evacuation. Reg Anesth Pain Med 2005;30:202-205.
- Tsui BC, Pillay JJ. Evidence-based medicine: Assessment of ultrasound imaging for regional anesthesia in infants, children, and adolescents. Reg Anesth Pain Med 2010;35(2 Suppl):S47–S54.
- Rubin K, Sullivan D, Sadhasivam S. Are peripheral and neuraxial blocks with ultrasound guidance more effective and safe in children? Paediatr Anaesth 2009;19:92-96.
- Ritcey B, Pageau P, Woo MY, Perry JJ. Regional nerve blocks for hip and femoral neck fractures in the emergency department: A systematic review. CJEM 2016;18:37-47.
- Black KJ, Bevan CA, Murphy NG, Howard JJ. Nerve blocks for initial pain management of femoral fractures in children. Cochrane Database Syst Rev 2013;12:CD009587.
- Eichenberger U, Stockli S, Marhofer P, et al. Minimal local anesthetic volume for peripheral nerve block: A new ultrasound-guided, nerve dimension-based method. Reg Anesth Pain Med 2009;34:242-246.
- Marhofer P, Schrögendorfer K, Koinig H, et al. Ultrasonographic guidance improves sensory block and onset time of three-in-one blocks [see comment]. Anesth Analg 1997;85:854-857.
- Marhofer P, Schrögendorfer K, Wallner T, et al. Ultrasound guidance reduces the amount of local anesthetic for 3-in-1 blocks. Reg Anesth Pain Med 1998;23:584-588.
- Barrington MJ, Kluger R. Ultrasound guidance reduces the risk of local anesthetic systemic toxicity following peripheral nerve blockade. Reg Anesth Pain Med 2013;38:289-297.
- Watts AC, Gaston P, Hooper G. Randomized trial of buffered versus plain lidocaine for local anaesthesia in open carpal tunnel decompression. J Hand Surg Br 2004;29:30-31.
- Gray AT, Schafhalter-Zoppoth I. Ultrasound guidance for ulnar nerve block in the forearm. Reg Anesth Pain Med 2003;28:335-339.
- Hopkins RE, Bradley M. In-vitro visualization of biopsy needles with ultrasound: A comparative study of standard and echogenic needles using an ultrasound phantom. Clin Radiol 2001;56:499-502.
- Cohen JM, Gray AT. Functional deficits after intraneural injection during interscalene block. Reg Anesth Pain Med 2010;35:397-399.
- Hadzic A, Dilberovic F, Shah S, et al. Combination of intraneural injection and high injection pressure leads to fascicular injury and neurologic deficits in dogs. Reg Anesth Pain Med 2004;29:417-423.
- Bupivacaine HCL Injection [package insert]. Lake Forest, IL: Hospira; 2011.
- Brown WU, Bell GC, Lurie AO, et al. Newborn blood levels of lidocaine and mepivacaine in the first postnatal day following maternal epidural anesthesia. Anesthesiology 1975;42:698-707.
- Dickerson DM, Apfelbaum JL. Local anesthetic systemic toxicity. Aesthet Surg J 2014;34:1111-1119.
- Neal JM, Bernards CM, Butterworth JF 4th, et al. ASRA practice advisory on local anesthetic systemic toxicity. Reg Anesth Pain Med 2010;35:152-161.
- Johnson B, Herring A, Shah S, et al. Door-to-block time: Prioritizing acute pain management for femoral fractures in the ED. Am J Emerg Med 2014;32:801-803.
- Wroe P, O’Shea R, Johnson B, et al. Ultrasound-guided forearm nerve blocks for hand blast injuries: Case series and multidisciplinary protocol. Am J Emerg Med 2016;34:1895-1897.
- McCartney CJ, Xu D, Constantinescu C, et al. Ultrasound examination of peripheral nerves in the forearm. Reg Anesth Pain Med 2007;32:434-439.
- Dickman E, Pushkar I, Likourezos A, et al. Ultrasound-guided nerve blocks for intracapsular and extracapsular hip fractures. Am J Emerg Med 2016;34:586-589.
- Beaudoin FL, Nagdev A, Merchant RC, Becker BM. Ultrasound-guided femoral nerve blocks in elderly patients with hip fractures. Am J Emerg Med 2010;28:76-81.
- Beaudoin FL, Haran JP, Liebmann O. A comparison of ultrasound-guided three-in-one femoral nerve block versus parenteral opioids alone for analgesia in emergency department patients with hip fractures: A randomized controlled trial. Acad Emerg Med 2013;20:584-591.
- Morrison RS, Magaziner J, Gilbert M, et al. Relationship between pain and opioid analgesics on the development of delirium following hip fracture. J Gerontol A Biol Sci Med Sci 2003;58:76-81.
- Marcantonio ER, Flacker JM, Michaels M, et al. Delirium is independently associated with poor functional recovery after hip fracture. J Am Geriatr Soc 2000;48:618-624.
- Dolan MM, Hawkes WG, Zimmerman SI, et al. Delirium on hospital admission in aged hip fracture patients: Prediction of mortality and 2-year functional outcomes. J Gerontol A Biol Sci Med Sci 2000;55:M527-M534.
- Roberts KC, Brox WT, Jevsevar DS, Sevarino K. Management of hip fractures in the elderly. J Am Acad Orthop Surg 2015;23:131-137.
- Akhtar S, Hwang U, Dickman E, et al. A brief educational intervention is effective in teaching the femoral nerve block procedure to first-year emergency medicine residents. J Emerg Med 2013;45:726-730.
- Turner AL, Stevenson MD, Cross KP. Impact of ultrasound-guided femoral nerve blocks in the pediatric emergency department. Pediatr Emerg Care 2014;30:227-229.
- Wathen JE, Gao D, Merritt G, et al. A randomized controlled trial comparing a fascia iliaca compartment nerve block to a traditional systemic analgesic for femur fractures in a pediatric emergency department. Ann Emerg Med 2007;50:162-171.
- Chu RS, Browne GJ, Cheng NG, Lam LT. Femoral nerve block for femoral shaft fractures in a paediatric emergency department: Can it be done better? Eur J Emerg Med 2003;10:258-263.
- Muraskin SI, Conrad B, Zheng N, et al. Falls associated with lower-extremity nerve blocks: A pilot investigation of mechanisms. Reg Anesth Pain Med 2007;32:67-72.
- Clattenburg E, Herring A, Hahn C, et al. ED ultrasound-guided posterior tibial nerve blocks for calcaneal fracture analgesia. Am J Emerg Med 2016;34:1183.e1-3.
- Soares LG, Brull R, Chan VW. Teaching an old block a new trick: Ultrasound-guided posterior tibial nerve block. Acta Anaesthesiol Scand 2008;52:446-447.
- Redborg KE, Antonakakis JG, Beach ML, et al. Ultrasound improves the success rate of a tibial nerve block at the ankle. Reg Anesth Pain Med 2009;34:256-260.
- Wassef MR. Posterior tibial nerve block. A new approach using the bony landmark of the sustentaculum tali. Anaesthesia 1991;46:841-844.
- Delgado-Martinez AD, Marchal JM, Molina M, Palma A. Forefoot surgery with ankle tourniquet: Complete or selective ankle block? Reg Anesth Pain Med 2001;26:184-186.
- Kalsi R, Dempsey A, Bunney EB. Compartment syndrome of the foot after calcaneal fracture. J Emerg Med 2012;43:e101-e106.
- Myerson M, Manoli A. Compartment syndromes of the foot after calcaneal fractures. Clin Orthop Relat Res 1993;290:142-150.
- Blaivas M, Adhikari S, Lander L. A prospective comparison of procedural sedation and ultrasound-guided interscalene nerve block for shoulder reduction in the emergency department. Acad Emerg Med 2011;18:922-927.
- Mantuani D, Nagdev A. Sonographic evaluation of a paralyzed hemidiaphragm from ultrasound-guided interscalene brachial plexus nerve block. Am J Emerg Med 2013;30:2099.e5-7.
- Lyons C, Herring AA. Ultrasound-guided axillary nerve block for ED incision and drainage of deltoid abscess. Am J Emerg Med 2017;35:1032.e3-1032.e7
- Frenkel O, Herring AA, Fischer J, et al. Supracondylar radial nerve block for treatment of distal radius fractures in the emergency department. J Emerg Med 2011;41:386-388.
- Herring AA, Stone MB, Fischer J, et al. Ultrasound-guided distal popliteal sciatic nerve block for ED anesthesia. Am J Emerg Med 2011;29:697.e3-5.
- Stone MB, Carnell J, Fischer JW, et al. Ultrasound-guided intercostal nerve block for traumatic pneumothorax requiring tube thoracostomy. Am J Emerg Med 2011;29:697.e1-2.
- Herring AA, Stone MB, Nagdev AD. Ultrasound-guided abdominal wall nerve blocks in the ED. Am J Emerg Med 2012;30:759-64.
- Schaeffer E, Millot I, Landy C, et al. Another use of continuous transversus abdominis plane (TAP) block in trauma patient: Pelvic ring fractures. Pain Med 2014;15:166-167.
- Smith DI, Hoang K, Gelbard W. Treatment of acute flares of chronic pancreatitis pain with ultrasound guided transversus abdominis plane block: A novel application of a pain management technique in the acute care setting. Case Rep Emerg Med 2014;Epub Sep 25.
- Flores S, Herring AA. Ultrasound-guided greater auricular nerve block for emergency department ear laceration and ear abscess drainage. J Emerg Med 2016;50:651-655.
- Flores S, Herring AA. Ultrasound-guided dorsal penile nerve block for ED paraphimosis reduction. Am J Emerg Med 2015;33:863.e3-5.
Ultrasound-guided nerve blocks offer effective and safe alternatives to systemic analgesics to manage pain in the ED. This article reviews the literature supporting the use of ultrasound-guided nerve blocks in the ED and describes how to perform some of the most basic nerve blocks.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
