Skin Infestations: Fungal and Scabies
April 15, 2018
Reprints
AUTHORS
Jessica Perkins, DO, PGY-3, Dermatology Resident, Nova Southeastern University College of Osteopathic Medicine/Largo Medical Center, Largo, FL
Molly Buckland, DO, PGY-1, Dermatology Resident, Nova Southeastern University College of Osteopathic Medicine/Largo Medical Center, Largo, FL
Richard A. Miller, DO, Program Director, Dermatology Residency Program, Nova Southeastern University College of Osteopathic Medicine/Largo Medical Center, Largo, FL
PEER REVIEWER
Karl K. Kellawan, MD, Forefront Dermatology, Centerville, OH
EXECUTIVE SUMMARY
- Tinea is a common skin disorder seen in primary care practices, but it often is misdiagnosed and can be mistaken for mimickers.
- Unlike other fungi, dermatophytes metabolize keratin as an energy source and typically are not particularly virulent.
- Tinea is more common in black and Asian patients, has a predilection for young adults, and is three to four times more common in males.
- The clinical dermatophyte infections tend to be named for the involved body area.
- First-line treatment involves topical agents such as azoles, allylamines, ciclopirox, butenafine, and tolnaftate, but the treatment of choice for tinea capitis and tinea barbae is griseofulvin.
- Scabies is caused by the mite Sarcoptes scabiei and must be considered in differential diagnosis, but the distribution and appearance of lesions typically are distinctive.
- Scabies treatment involves two topical applications of permethrin 5% cream given seven days apart.
Most of us will hardly flinch if we hear “Cardiac arrest coming in,” but will recoil in terror at “How are you at rashes?” I am not a dermatologist — and don’t want to be. But there is hardly a day that goes by that I am not asked by someone (a patient, a colleague, a friend, or a family member) to look at a rash or lesion on the skin. While some patients present for their rash primarily, many will “add it on” to the visit. In many emergency departments (EDs), a dermatology, or even primary care, follow-up visit is not an option. Therefore, emergency providers need a working understanding of common rashes, and also should recognize those rashes that need referral.
This article provides an in-depth look at common rashes caused by fungi and scabies. We have included some information about potassium hydroxide (KOH) staining, which long has been the standard for making the diagnosis of tinea. I recognize that many no longer have a microscope available in the ED, and many ED providers may not even know how to use one. That information is included for the few of you who can use it.
Although cutaneous fungal infections rarely are life-threatening, they are common, and they are irritating. This review should help you diagnose and treat these infections.
— Sandra M. Schneider, MD, Editor
Introduction
Tinea refers to a superficial fungal infection of the skin, hair, and nails caused by dermatophytes. Dermatophytes are filamentous fungi; the three genera that cause disease are Microsporum, Trichophyton, and Epidermophyton.1 Trichophyton rubrum is the most common cause of dermatophyte infection, accounting for nearly 70% of infections worldwide.1 These infections are extremely common, but are more prominent in warm, tropical climates. Tinea is seen more commonly in black and Asian patients, has a predilection for young adults, and is three to four times more common in males.1 Dermatophyte infections are alike in their physiology, morphology, and pathogenicity and are referred to clinically as “tinea.”
Transmission may be anthropophilic (human to human), zoophilic (animal to human), or geophilic (soil to human/animal).1 Unlike other fungi, dermatophytes metabolize keratin as an energy source. They are not particularly virulent and typically invade only the cornified, outer layers of the epidermis. Mannans in the dermatophyte cell wall contribute to invasion of the skin by decreasing epidermal proliferation and by exhibiting immune-inhibitory effects.1 Defects in the skin barrier (diseases such as Darier disease, Hailey-Hailey disease, and ichthyosis) or maceration tend to encourage dermatophyte invasion.1 Protective host factors that limit invasion to the keratinized tissue include protease inhibitors, sebum, serum factors, and the host immune system.1 Immunodeficient hosts (chronic mucocutaneous candidiasis, common variable immunodeficiency, and HIV) tend to have more severe, chronic, or recurrent infections than immunocompetent hosts.
Dermatophyte infections commonly are misdiagnosed in clinical practice. The clinical appearance of these infections can vary, and many other dermatologic diseases may have a similar appearance. This review will help you diagnose and treat your patients and provide the most current treatment regimens.
Subtypes of Tinea Infections
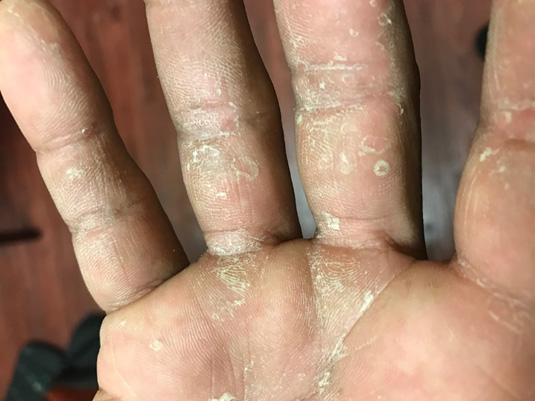
Clinical dermatophyte infections tend to be named for the involved body area. The clinical subtypes include tinea corporis (body), tinea capitis (scalp), tinea cruris (groin), tinea pedis (feet), tinea manuum (hands), tinea unguium (nails), tinea barbae (beard), and tinea faciei (face). See Figure 1 for a clinical presentation of tinea manuum. See Table 1 for the clinical features of tinea and its mimickers.
Figure 1. Tinea Manuum |
|
Small collarettes of scale are typical of superficial fungal infections located on the palms and soles.
|
|
Image courtesy of Jessica Perkins, DO. |
Table 1. Typical Clinical Features of Tinea and Mimickers |
|
|
Tinea Corporis |
Annular plaques with a central clearing and a leading edge of scale |
|
Nummular Eczema |
Nummular or “coin-shaped” erythematous, scaly plaques in typical distributions (antecubital and popliteal fossa, posterior neck, lower extremities), atopic diathesis |
|
Erythema Annulare Centrifugum |
Annular erythema with a trailing scale; may be a response to a tinea infection; perform full skin exam |
|
Scabies |
Erythematous papules to pustules with excoriations and possible burrows, flexor wrists, interdigital webspaces, umbilicus, genitals |
|
Lichen Planus |
Purple, polygonal, flat-topped papules ± lacy reticulated scale; flexor wrists, ankles, trunk ± oral lesions |
|
Psoriasis Vulgaris |
Elevated, well-demarcated, erythematous plaques with overlying silvery scale |
|
Seborrheic Dermatitis |
Waxy, yellow scale on an erythematous base; scalp, central face, eyebrows, beard, central chest |
|
Pustular Psoriasis |
Deep, yellow papules ± brown collarettes of scale on the plantar/palmar surfaces |
|
Subacute Cutaneous Lupus Erythematosus |
Annular, erythematous plaques with central clearing in a photodistribution (V-neck and upper back ± upper arms) |
|
Pityriasis Rosea |
Single patch (herald patch) followed by eruption of flesh to erythematous colored scaly patches in a “Christmas tree” distribution on the trunk |
|
Source: Author created. |
|
Tinea Corporis
Tinea corporis is an infection of the body surfaces other than palms/soles, groin, face, scalp, hair, and nails. It usually occurs on exposed skin of the trunk and extremities and generally is confined to the epidermis. It is usually acquired by direct contact or secondarily spread from another infected body area.1 The most common pathogen is T. rubrum, followed by T. mentagrophytes.1 Infection with T. tonsurans may occur in adults from contact with a child with tinea capitis.2 Direct contact with an infected cat or dog may lead to infection with Microsporum canis.2 This infection is found globally; however, it is more common in tropical regions. The classic presentation is referred to as “ringworm” and is characterized by a pruritic, erythematous, scaly patch with a raised border and central clearing.3
Clinical Variants of Tinea Corporis
Majocchi’s granuloma is a rare, deep infection of the hair follicle that invades the dermis or subcutaneous tissue.2 Inciting events include shaving legs, trauma to skin, or immunosuppression. It is characterized by perifollicular papulopustules or granulomatous nodules.1 Tinea profunda results from excessive inflammation in response to a dermatophyte infection. It may have a granulomatous or verrucous appearance and can be mistaken for cutaneous tuberculosis or squamous cell carcinoma.1
Tinea imbricata (Tokelau ringworm) is a chronic infection caused by T. concentricum and is characterized by concentric annular, scaly, erythematous plaques.1 It occurs in the equatorial regions of the world.
Mimickers of Tinea Corporis
The following conditions can mimic tinea corporis: dermatitis (including nummular eczema, stasis, atopic, contact, and seborrheic dermatitis), pityriasis versicolor, pityriasis rosea, parapsoriasis, erythema annulare centrifugum, elastosis perforans serpiginosa, annular psoriasis, granuloma annulare, subacute lupus erythematosus, mycosis fungoides, and impetigo.1
Tinea Capitis
Tinea capitis is a dermatophyte infection of the scalp hair that primarily affects children. The peak age is 3 to 7 years, and it is more common in boys.3 T. tonsurans accounts for more than 90% of tinea capitis in the United States, with M. canis following as the second most frequent cause.1 Other etiologies include T. violaceum (endemic in Africa) and M. audouinii (Europe).1 Tinea capitis can have a range of clinical presentations that depend on the causative organism as well as the host’s immune response. Alopecia with or without scale is the most common presentation; however, it can vary from mild scaling to a severe pustular eruption with alopecia called a kerion.1
The three patterns of invasion for dermatophytes that infect the hair include endothrix, ectothrix, and favus. Endothrix patterns result from anthropophilic Trichophyton infection within the hair shaft, and common causes include T. tonsurans and T. violaceum.1 Ectothrix patterns occur when the infection is outside the hair shaft and results in destruction of the cuticle. The presentation varies from non-inflamed, scaly, patchy alopecia to kerion formation. Microsporum infections may fluoresce under Wood’s lamp. The favus pattern is caused by T. schoenleinii and is the most severe. It presents as thick, yellow crusts and has a bluish fluorescence under a Wood’s lamp.1 Scarring alopecia may develop if the infection is chronic. It is important to note that many scalp/hair conditions can cause scaling or alopecia, and it is very important to consider and rule out a fungal infection.
Mimickers of Tinea Capitis
Seborrheic dermatitis, alopecia areata, psoriasis, and trichotillomania can mimic tinea capitis. If pustules are present, pyoderma gangrenosum and folliculitis can resemble tinea capitis.1 If scarring is present, lichen planus, discoid lupus erythematosus, and central centrifugal cicatricial alopecia should be part of the differential diagnosis.1
Tinea Cruris
Commonly known as jock itch, tinea cruris is a dermatophyte infection of the inguinal area. Usually it is seen on the inner aspect of the upper thighs and crural folds, but may be seen in the gluteal cleft and buttocks as well. The three most common pathogens are T. rubrum, E. floccosum, and T. mentagrophytes.1 It is more common in men because the scrotum provides an ideal environment and because more often men have concomitant tinea pedis, which can be transferred to the groin by pulling on undergarments over the feet.1 Characteristically, lesions are sharply demarcated with a raised, erythematous, scaly advancing border. Lesions may have vesicles, and may be unilateral or bilateral. In males, the scrotum usually is spared. Providers should consider cutaneous candidiasis if the scrotum is involved.1
Mimickers of Tinea Cruris
The following conditions can mimic tinea cruris: inverse psoriasis, erythrasma, seborrheic dermatitis, candidal intertrigo, contact dermatitis, lichen simplex chronicus, parapsoriasis, Hailey-Hailey disease, and Langerhans cell histiocytosis.1
Tinea Pedis
Also known as athlete’s foot, tinea pedis is the most common location for dermatophyte infection. Infection typically occurs on the soles of the feet and, most commonly, in the interdigital area. The major types of tinea pedis are interdigital, hyperkeratotic (moccasin-type), vesiculobullous (inflammatory), and ulcerative. The characteristic finding in the interdigital type is pruritic, erythematous scales and/or erosions that usually present in between the third and fourth toes. Moccasin-type tinea pedis presents as a diffuse, erythematous, hyperkeratotic lesion that covers the soles plus the medial and lateral edges of the feet. (See Figure 2.) The vesiculobullous type presents as an erythematous vesicular or bullous eruption that may be pruritic or painful, and it is most common on the medial aspect of the foot. Similar to tinea cruris, the most common pathogens responsible are T. rubrum, E. floccosum, and T. mentagrophytes.1 Patients also may have a secondary bacterial infection if they present with malodorous erosions or ulcerations.
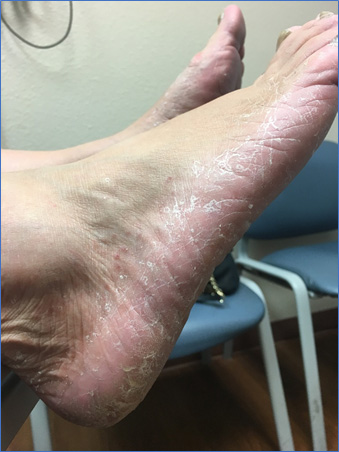
Figure 2. Tinea Pedis |
|
Shows the classic appearance of tinea pedis with small collarettes of scale extending past the mid-lateral foot with a minor erythema noted on the base. Tinea unguium also is noted, making this a straightforward clinical case.
|
|
Image courtesy of Jessica Perkins, DO. |
Tinea manuum has a characteristic presentation of unilateral hyperkeratotic lesions on the palms and interdigital spaces.1,4 The most common pathogens are the same as for tinea pedis and tinea cruris, and these infections often occur concomitantly.
Mimickers of Tinea Pedis
Mimickers of tinea pedis include dermatitis (dishydrotic and contact), psoriasis vulgaris or pustular psoriasis, secondary syphilis, pitted keratolysis, hereditary keratosis palmoplantaris, and juvenile plantar dermatosis.1,3 Erythrasma or bacterial infection may resemble the interdigital type of tinea pedis.1
Tinea Unguium
Tinea unguium is a dermatophyte infection of the nail unit, most commonly caused by T. rubrum, T. mentagrophytes, and E. floccosum.1 Often, this infection is referred to as onychomycosis, an umbrella term that encompasses all fungal infections of the nails including non-dermatophyte causes. However, dermatophytes account for approximately 90% of onychomycosis cases. Tinea unguium is more common in men, is often associated with chronic tinea pedis, and occurs on the toenails more than the fingernails. It may be unilateral or bilateral and may affect only one nail or multiple nails. There are three common patterns that are based on the point of entry for the infection. The distal/lateral subungual type is the most common and presents with onycholysis, yellowing, and thickening of the nails.1 (See Figure 3.) The superficial white type is confined to the dorsal surface of the nail, and presents as white patches (T. mentagrophytes) or transverse striate bands (T. rubrum).1 The proximal subungual type invades underneath the proximal nail fold and usually is found in immunocompromised patients.1
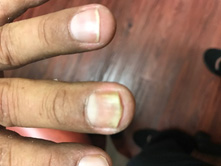
Figure 3. Tinea Unguium |
|
Distal yellow debris on the middle fingernail can serve as a clue to tinea unguium. It is prudent to check the feet in any nail infection, as tinea manuum and pedis are commonly present.
|
|
Image courtesy of Jessica Perkins, DO. |
Mimickers of Tinea Unguium
Numerous pathogens (dermatophyte and non-dermatophyte) cause onychomycosis, and many factors may cause dystrophy of the nails, making accurate diagnosis a challenge. Diagnoses that can mimic tinea unguium are Candida infections, the nail manifestations of psoriasis, lichen planus, dermatitis, hyperthyroidism, external trauma, pachyonychia, and Darier disease.1 Tinea unguium can be difficult to treat because of the required prolonged treatment times, medication side effects, and recurrences.
Tinea Faciei
A dermatophyte infection on the skin of the face, tinea faciei usually is caused by the same organisms as tinea corporis.4 Infections with T. rubrum can be especially difficult to diagnose, as the margins of the lesion are often indistinguishable. Tinea faciei is seen more frequently in AIDS patients.
Mimickers of Tinea Faciei
Seborrheic, perioral, or contact dermatitis can mimic tinea faciei. Other mimickers include rosacea, lupus erythematosus, acne, and annular psoriasis in children.1
Tinea Barbae
Tinea barbae occurs exclusively in the beard hair distribution of the face and neck of men. It is commonly transmitted by animals, and the typical causative pathogens are T. mentagrophytes and T. verrucosum.1 The clinical presentation may be severe in the zoophilic pathogens, and often it presents with intense inflammation, pustules, and abscesses with bacterial superinfection.4 T. rubrum causes a mild, superficial variant similar to tinea corporis.
Mimickers of Tinea Barbae
Bacterial folliculitis, herpes simplex/zoster, acne vulgaris, and cervicofacial actinomycosis can mimic tinea barbae.1
Diagnosis
The most important factor in the diagnosis of a dermatophyte infection is a thorough physical exam. It is important to remember that there may be more than one area of the body infected at the same time, which warrants a complete cutaneous exam. For example, tinea pedis often occurs with tinea unguium or tinea cruris.2
Clinical findings suspicious for a dermatophyte infection should be followed by confirmation testing. Diagnosis usually is confirmed with a potassium hydroxide (KOH) examination via microscopy. Most EDs have removed the microscopes and reagents. For those who still have access to these useful tests, a KOH prep can be very helpful. KOH examinations may be enhanced with chlorazol black E stain. The disadvantage of KOH testing is that it often yields false-negative results.5 A skin scraping for a KOH examination should be taken from the active edge of the lesion with a No. 15 blade.6 The provider should apply alcohol to the lesion before scraping to enhance the scale adhering to the blade.
All dermatophytes appear the same in KOH examinations. If there is a need to identify a particular species, a culture is required. Cultures are slow growing and need many weeks of incubation time.7 If KOH examination and fungal cultures are negative and a dermatophyte infection is still suspected, a skin biopsy may be performed. Although, in general, fungal cultures and skin biopsies are well outside of the emergency physician’s normal practice, many insurance companies require a positive culture before they will cover the treatment. As the cost of some of the drugs may be in the hundreds of dollars, patients may prefer referral to a dermatologist if an expensive or long-term treatment is anticipated (onychomycosis). Skin biopsies will show fungal hyphae within the stratum corneum. Periodic acid-Schiff (PAS) stains and silver stains often are used to enhance fungal elements in biopsy specimens. Techniques using polymerase chain reaction (PCR) and mass spectroscopy also can be used to identify dermatophyte strains.8 PCR is a fast, simple procedure that is highly specific for diagnosis of dermatophyte infections.9 There are also promising studies for immunochromatographic diagnosis of dermatophytes.10 The most reliable way to diagnose onychomycosis is by histologic examination of a formalin-fixed, PAS-stained nail plate.1 The practitioner places a nail clipping into formalin and sends it to the local pathology lab for review.
Treatment
First-line treatment for uncomplicated, superficial, and localized tinea infections (corporis, cruris, and pedis) is topical antifungals. Topical agents include azoles (clotrimazole, econazole, ketoconazole, efinaconazole, luliconazole, miconazole, oxiconazole, sertaconazole, sulconazole), allylamines (naftifine, terbinafine), ciclopirox, butenafine, and tolnaftate.2 Several of these topical preparations are available over the counter and often are adequate treatment for mild infections. Azoles tend to be more cost effective, although they are not quite as effective as allylamines.6 Topical antifungals should be applied once or twice a day for two to four weeks and should be continued for one week after clinical clearance.6 It is important to note that although topical nystatin is effective in treating Candida, it is not effective in dermatophyte infections.2 Photodynamic therapy is also a treatment option if other methods have failed.6
Infections including tinea manuum, tinea capitis, tinea unguium, and Majocchi’s granuloma; infections covering extensive areas; and infections that fail topical treatment usually require systemic antifungal medication. Oral agents include terbinafine, fluconazole, itraconazole, and griseofulvin. Prescribing guidelines for extensive infections, failure of topical treatment, and relapsing infections suggest terbinafine 250 mg daily for 14 days, fluconazole 50 mg daily for two to four weeks (six weeks for tinea pedis) or 150-200 mg once weekly for two to four weeks, itraconazole 100 mg daily for 15 days or 200 mg daily for seven days (may require longer treatment for tinea pedis and manuum), or griseofulvin microsize 500-1,000 mg daily for two to four weeks.2,6
The treatment of choice for tinea capitis and tinea barbae is griseofulvin. Terbinafine, itraconazole, and fluconazole are not FDA-approved for the treatment of tinea capitis or barbae.1 Adjunct treatment for tinea capitis includes antifungal shampoo (ketoconazole 2% or selenium sulfide 2.5% every other day), disinfecting grooming devices, and treatment of close contacts.1 In addition to antifungal treatment, products containing urea, glycolic acid, and lactic acid can be used in treating tinea pedis or tinea manuum.1,11 Tinea unguium can be extremely difficult to treat and often needs long-term systemic treatment.
Tinea incognito is a condition that occurs if a dermatophyte infection is misdiagnosed and treated with a topical corticosteroid. It can alter the clinical appearance of the infection and make diagnosis difficult. Treatment with corticosteroids also may lead to exacerbation of the infection and cause Majocchi’s granuloma.2 It is not recommended to use topical corticosteroids in conjunction with antifungals even though it may lead to more rapid resolution of inflammation and disease.2
Scabies
The scabies mite, Sarcoptes scabiei var. hominis, causes human scabies.12 The entire life cycle of the mite takes place in the epidermis, with the female mite laying three eggs daily. These eggs mature over the course of 10 days. The mites typically live on the human host for less than three days, except in the case of crusted scabies, in which they may survive up to seven days.12 Crusted scabies is a type of scabies found in individuals with compromised immune systems allowing the mite to survive with minimal symptoms and a large number of mites.12
The cutaneous lesions of scabies have a typical distribution. They often involve the web spaces of the fingers, flexural wrists, posterior neck, and umbilicus. Men often have lesions on the penis and scrotum, while women tend to have vulvar and areolar lesions. The burrow is the classic and distinct clinical finding in scabies and represents the track of the female mite to lay her eggs. Clinically, the burrow presents as a small white to grey winding plaque.12 The burrow may not always be present.12 Other cutaneous findings can include erythematous papules, pustules, or vesicles with excoriations often prominent. The diagnosis can be confirmed via skin scraping, curetting, or microscopic examination of transparent tape from an infested area. A skin biopsy can confirm the diagnosis.12
Symptoms of scabies can present two to six weeks after first exposure or within one to two days on second exposure. The primary symptoms are pruritus and skin lesions. Scabies commonly is known as one of the most pruritic rashes. The pruritus can be exacerbated by a hot shower or can cause insomnia, as it worsens at night. Household contacts often are plagued by the pruritus as well.
Standard treatment of scabies can be completed with two topical treatments of permethrin 5% cream given seven days apart (day 1 and day 8 applications).12 For adults, the cream is applied from the neck down on all skin surfaces at night and washed off in the morning. For elderly patients and infants (2 months of age and older), the cream also should be applied to the face and scalp. Patients with a sensitivity or allergy to formaldehyde or chrysanthemums should avoid using permethrin cream. Other topical medications that may be considered in scabies if resistant or allergic to permethrins include lindane 1% lotion/cream, sulfur ointment (5-10%), and crotamiton 10% lotion/cream. Ivermectin (200 to 400 mcg/kg) orally is also an excellent choice for resistant scabies, treating on day 1 and day 8 or 14.12 Ivermectin may cause central nervous system (CNS) toxicity in infants and young children. Lindane also has potential CNS toxicity in patients weighing less than 50 kg.12 Therefore, these medications are used only when absolutely needed.
Mimickers of Scabies
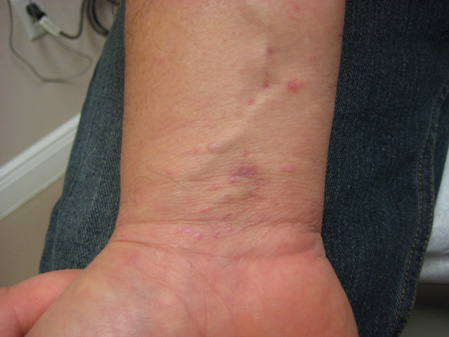
Lesions of lichen planus (see Figure 4) have a typical presentation on the flexor wrists, but are flat-topped, purple papules, often with a white reticulated veil, and will lack the characteristic burrow of scabies. Other mimickers could include viral exanthems, guttate psoriasis, secondary syphilis, drug reactions, or other arthropod assaults.
Figure 4. Lichen Planus |
|
Polygonal, purple, flat-topped papules on the flexor wrist is a classic presentation of lichen planus.
|
|
Image courtesy of George Gibbons, MD. |
Conclusion
Dermatophyte and scabetic infestations are extremely common worldwide and often are misdiagnosed. Patients without access to primary care may seek treatment for these conditions in the emergency department. More often this may be a secondary complaint. Numerous other dermatologic skin conditions may mimic these infections. A thorough cutaneous examination often can reveal clues to the diagnosis. Other lab modalities, such as skin scraping, biopsy, or culture, can further aid in making the correct diagnosis. Patients should be cautioned to seek further care if the rash does not respond to the treatment prescribed. If therapies discussed above fail to treat the skin rash, it is always prudent for physicians to refer to dermatology for further evaluation and treatment.
REFERENCES
- Elewski B, Hughey L, Sobera J, Hay R. Fungal Diseases. In: Bolognia JL, Jorizzo JL, Schaffer JV, eds. Dermatology. 3rd ed. Philadelphia: Elsevier Saunders; 2012: 1251-1284.
- Goldstein A, Goldstein B. Dermatophyte (tinea) infections. UpToDate. Available at: https://www.uptodate.com/contents/dermatophyte-tinea-infections. Accessed July 1, 2017.
- Marcellin L. Tinea Infections. Philadelphia: Elsevier; 2013.
- Hay R. Dermatophytosis (Ringworm) and Other Superficial Mycoses. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. Philadelphia: Elsevier Saunders; 2015.
- Liansheng Z, Xin J, Cheng Q, et al. Diagnostic applicability of confocal laser scanning microscopy in tinea corporis. Int J Dermatol 2013;52:1281-1282.
- Lebwohl M, Heymann WR, Berth-Jones J, Coulson I, eds. Treatment of Skin Disease: Comprehensive Therapeutic Strategies. 4th ed. Philadelphia: Saunders; 2014.
- Rezusta A, de la Fuente S, Gilaberte Y, et al. Evaluation of incubation time for dermatophytes cultures. Mycoses 2016;59:416-418.
- Sahoo AK, Mahajan R. Management of tinea corporis, tinea cruris, and tinea pedis: A comprehensive review. Indian Dermatol Online J 2016;7:77-86.
- Eckert JC, Ertas B, Falk TM, et al. Species identification of dermatophytes in paraffin-embedded biopsies with a new polymerase chain reaction assay targeting the internal transcribed spacer 2 region and comparison with histopathological features. Br J Dermatol 2016;174:869-877.
- Noriki S, Ishida H. Production of an anti-dermatophyte monoclonal antibody and its application: Immunochromatographic detection of dermatophytes. Med Mycol 2016;54:808-815.
- Elewski BE, Haley HR, Robbins CM. The use of 40% urea cream in the treatment of moccasin tinea pedis. Cutis 2004;73:355-357.
- Burkart CN, Burhart, CG, Morrell DS. Chapter 84: Infestations. In: Bolognia J, Jorrizzo JL, Shaffer JV, eds. Dermatology. 3rd ed. Philadelphia: Elsevier Saunders; 2012: 1423-1426.
Although cutaneous fungal infections rarely are life-threatening, they are common, and they are irritating. This article provides an in-depth look at common rashes caused by fungi and scabies.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.