Mammalian Bites
May 1, 2018
Reprints
AUTHORS
Mara S. Aloi, MD, Residency Program Director, Department of Emergency Medicine, Allegheny General Hospital, Pittsburgh, PA
Brian Rempe, MD, Director, AGH Emergency Medicine Residency Simulation Program, Allegheny General Hospital, Pittsburgh, PA
Linda Truong, MD, Department of Emergency Medicine, Allegheny General Hospital, Pittsburgh, PA
PEER REVIEWER
Colin G. Kaide, MD, FACEP, FAAEM, Associate Professor of Emergency Medicine, Department of Emergency Medicine, Wexner Medical Center, The Ohio State University, Columbus
EXECUTIVE SUMMARY
- Cat bites are complicated by infection in 30-50% of cases with about 6% requiring hospitalization. Cat teeth are needle-like and are able to puncture more deeply into the soft tissues, even breaching joint capsules or the periosteum in the case of digital injuries. This puncture injury delivers microbial inoculum deep into the soft tissues, which then seals over the point of entry, allowing for colonization to progress to infection.
- Human bite wounds may be the result of interpersonal violence, sporting accidents, sexual activity, abuse, or self-defense. They can be categorized as occlusive bite injuries, which result from teeth closing on tissue with sufficient force to breach the skin, or clenched fist injuries, commonly known as “fight bites,” which are the result of the hand impacting teeth during a fight or assault.
- Infections from animal bite wounds are usually polymicrobial. The most common organisms found in both dog and cat bite wounds are Pasteurella species: Pasteurella canis in dogs and Pasteurella multocida and Pasteurella septica in cats.
- The hallmark of a Pasteurella infection is a local intense cellulitis seen within 24 hours of injury; low-grade fever and associated regional lymphadenopathy may be apparent. In one study, clinical signs of infection were seen within 15 hours of exposure. In contrast, infections from other pathogens typically do not present for two to three days.
- Capnocytophaga canimorsus is found in the oral flora of 16-41% of dogs and is an increasingly recognized complication of dog bites, particularly in the alcoholic or splenectomized patient population. Sepsis is the most common presentation and meningitis is the second most common, with complications including disseminated intravascular coagulation, hemolytic uremic syndrome, thrombotic thrombocytopenic purpura, and Waterhouse-Friderichsen syndrome.
- Bartonella henselae, a gram-negative rod that is transmitted by bites or scratches from infected cats, usually kittens, is the organism responsible for cat-scratch disease. These typically are self-limited infections, causing tender, regional lymphadenopathy and fever approximately two to three weeks after inoculation.
- Infection rates in wounds greater than 3 cm in length and in puncture injuries are three times higher than for all other wounds.
- A rare complication of cat bites that can result in vascular injury is septic pseudoaneurysm. This is thought to be a consequence of both direct trauma to a vessel along with colonization by Staphylococcus aureus, which leads to local inflammatory response, thereby damaging the arterial wall. Pseudoaneurysms present as pain, swelling, and a pulsatile mass at the site of a bite and can be confirmed using duplex ultrasonography.
- Primary closure of dog bite wounds, particularly in cosmetically significant areas, is indicated especially within the first eight hours after the injury.
Bites, whether dog, cat, or human, are a common reason for emergency department (ED) visits. Clinicians are challenged to decide issues regarding wound closure and antibiotic prophylaxis. The authors review the complexities of different types of bites ED providers may encounter and issues regarding closure and antibiotic prophylaxis, in addition to vaccination concerns.
— Ann M. Dietrich, MD, Editor
Definition of the Problem
Based on population studies, it is estimated that nearly 50% of U.S. household have at least one pet.1 Consequently, more than 90% of bites are from domestic animals, with 80-90% caused by dogs and 5-15% by cats.2 Human bites are less common, only accounting for approximately 3% of bite injuries. Mammalian bites account for 1-2% of all ED visits annually in the United States, with an estimated cost of more than $850 million. This amount does not include costs related to rehabilitation, long-term disability, or time off from work.3 Given these statistics, knowledge of current management guidelines for bite injuries is vital to providing safe and effective care and to preventing long-term complications. This issue will review management options for bite-related injuries, including discussion of controversies regarding wound closure and antimicrobial prophylaxis.
Epidemiology
Dog Bites
More than 1.5 million people were treated in U.S. EDs for dog bites between 2005 and 2009.4 Confounding the data is the fact that dog bites may be underreported. Not all bite victims seek care. The CDC estimated that in 1994, 4.7 million people sustained dog bites, with most of these bites going unreported.5 Certain groups are known to be at higher risk than others. In one report, which tracked dog bites from 2005-2009, males predominated, accounting for 52.9% of injuries.4 The age of the victim also appears to play a role, as the probability of a bite declined with increasing age. The group most at risk was children younger than 15 years of age, who accounted for 35.9% of bites. Children ages 5-9 years were the most at-risk group. According to developmental psychologists, young children are unlikely to recognize behavioral cues of animals and are more likely to exhibit behaviors that could incite an attack (e.g., attempting to play with an animal as it is eating, grabbing at the tail or ears).6
Most bites are inflicted by dogs known to the victim.1 It has been reported that 30% of bites in those 18 years of age and younger are from a family-owned dog, and 50% of bites are from a neighbor’s dog.5 Although dog bites account for the majority of mammalian bites evaluated each year in the United States, infection occurs in less than 25% of cases.7 This is likely because dog teeth tend to be broader and less sharp than those of cats and give rise to skin lacerations of superficial tissues. These wounds are easier to irrigate and explore.8
While most bites are minor, on average there are 19 dog bite-related fatalities reported annually in the United States.9,10 Pit bulls and pit bull mixes are responsible for the majority of deaths.11 Some dogs can deliver significant crushing force with their bite. For example, estimates of a pit bull’s biting force indicate that it can reach almost 450 psi,9 and some have reported that trained police dogs can exert a biting force in excess of 1,500 pounds.12 (See Figure 1.) There is a suggestion that neutering dogs possibly may decrease the likelihood of fatal dog attacks, as only 1 of 20 dogs involved in a fatal dog attack had been neutered.11
Figure 1. Dog Bite |
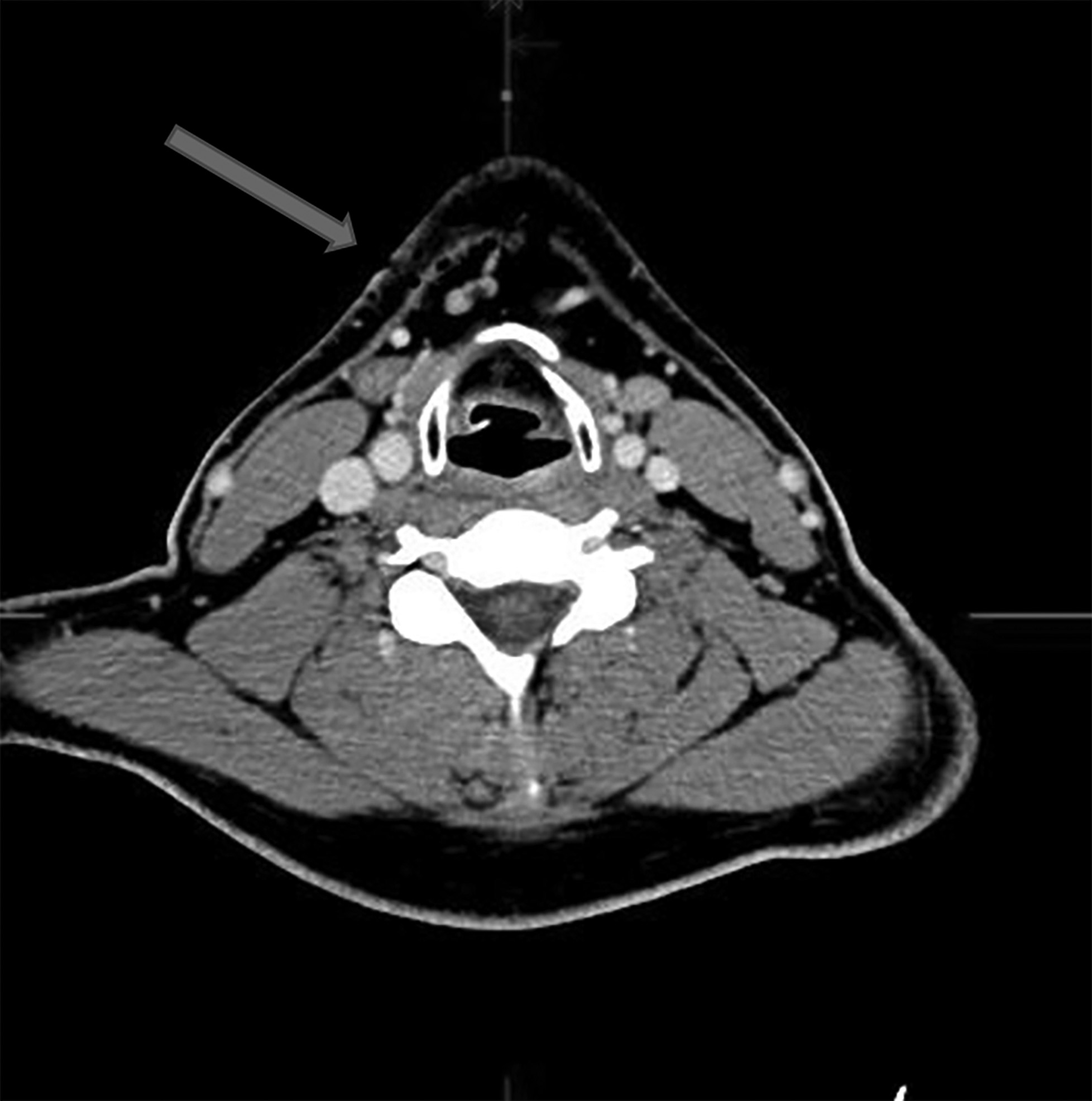 |
Dog bite wound to the neck with violation of the platysma.
Cat Bites
It is estimated that cat bites account for 5-15% of all animal bite wounds, with approximately 400,000 cat bites reported annually in the United States.13 However, as with dog bites, the true incidence may be higher as a result of underreporting. This may be because cat bites tend to be less serious initially than those caused by dogs, and patients may not seek immediate medical attention. Patients may be unaware of the complication risks associated with cat bites and may not present until complications have already developed. In one study, 75% of patients who had sustained a dog bite presented to the hospital within 24 hours of injury. In contrast, all of the cat bite victims presented later, only after a complication had developed.14 Injuries inflicted by cats are more prevalent in female patients, with a 2:1 female to male ratio and a peak incidence in the third decade.15
Despite the public’s perception that cat bites and scratches are benign, these injuries can be deceptively dangerous. Although they are only responsible for a modest percentage of all animal bites, cat bites actually result in nearly twice the rate of clinical infection when compared to dog bites, likely because of the unique mechanism of injury. There is less initial blunt trauma in cat bites than is seen after dog bites. However, cat teeth are needle-like and are able to puncture more deeply into the soft tissues, even breaching joint capsules or the periosteum in the case of digital injuries. This puncture injury delivers microbial inoculum deep into the soft tissues, which then seals over the point of entry, allowing for colonization to progress to infection. Exploration and irrigation of puncture wounds is more difficult.
Another factor likely leading to the increased rate of infection is the fact that up to 85% of cat bites are to the upper extremity, particularly the hand and wrist, where tendons, joint spaces, and bones are more superficially located and more susceptible to injury.16 (See Figure 2.) Cat bites are complicated by infection in 30-50% of cases.2 Approximately 6% require hospitalization for treatment of complications.17
Figure 2. Cat Bite of the Hand |
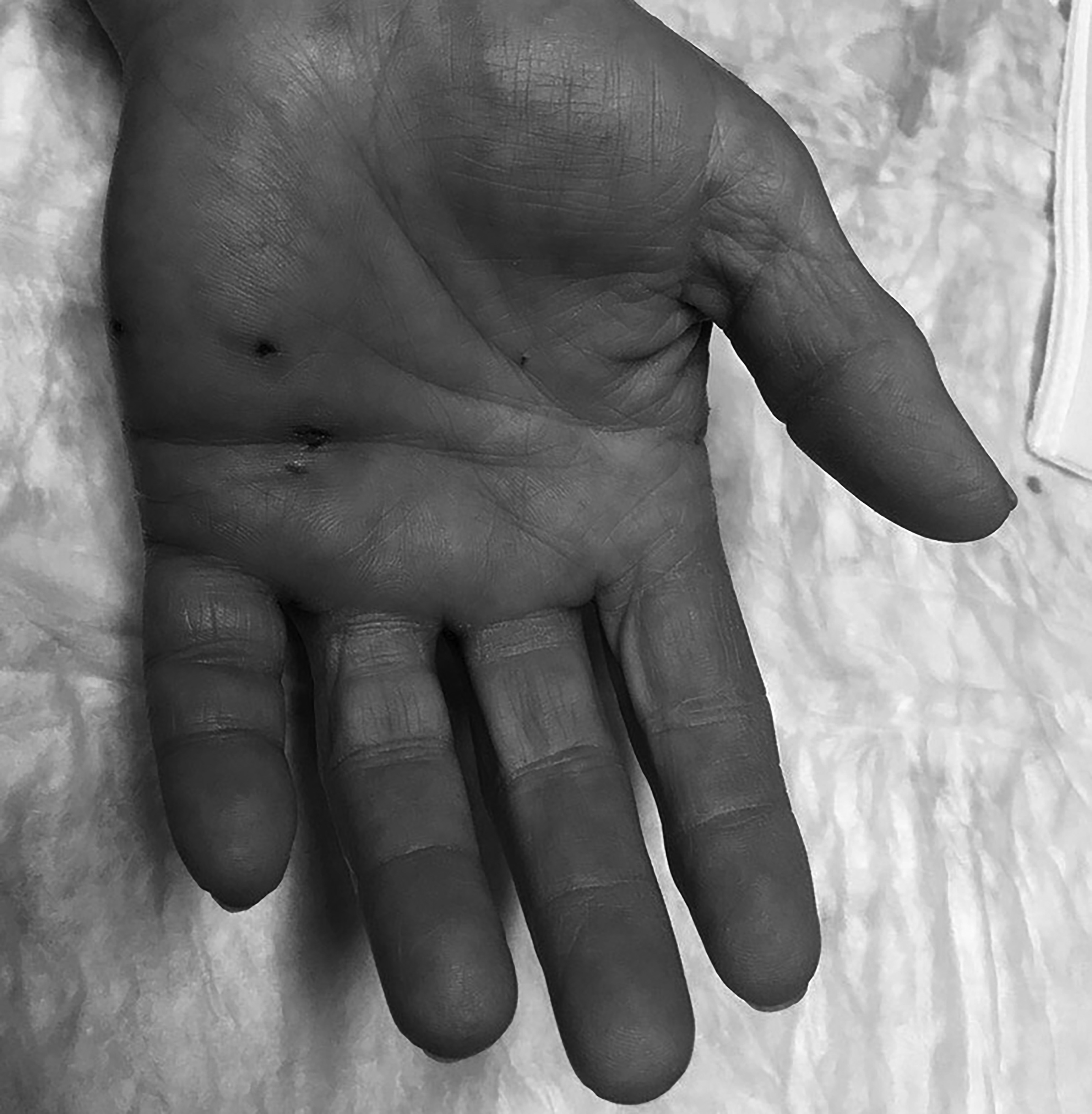 |
Human Bites
Estimates for the percentage of mammalian bites attributed to humans range from 3.6% to 23%.18 The estimated rate of infection in human bites is greater than 10%.19 The number of ED visits for human bite wounds likely underestimates the true incidence. Many people do not present because of limited severity of injury, self-care at home, embarrassment, inebriation, or fear of police involvement, depending on the mechanism of their injury.
Human bite wounds may be the result of interpersonal violence, sporting accidents, sexual activity, abuse, or self-defense.3 They can be categorized as occlusive bite injuries, which result from teeth closing on tissue with sufficient force to breach the skin, or clenched fist injuries, commonly known as “fight bites,” which are the result of the hand impacting teeth during a fight or assault.
Human occlusive bites usually are elliptical or ovoid, representing the shape of the mouth. Avulsions are rare, but do occur. There is a 3:1 ratio of male to female victims.20 The location on the body often varies with age and gender. Females are more commonly injured on the breasts, genitalia, legs, or arms, whereas males often present with injuries on the hands, arms, or shoulders. Overall, more than 50% of human bites occur in the upper extremities.15
The majority of patients present to the ED within 12 hours of injury (76.2%). Most biting offenders are known to their victims (70% vs. 29.5% of offenders who are strangers). More than half of these occur in public.21 Police officers, security personnel, and medical staff are groups at particular risk of being bitten. Sexual partners or spouses are the perpetrators in 17% of cases. Self-inflicted bite wounds account for 2% of patients and are more prevalent in patients with dementia or behavioral health issues, such as Lesch-Nyhan syndrome, which includes self-mutilatory behavior. Sports injuries accounted for only 1% of reported human bite wounds.21
Microbiology
Infections from animal bite wounds usually are polymicrobial, with an average of two to seven different species of bacteria found in cat and dog bite wounds and a median of seven organisms found in abscesses (five in purulent wounds and two in non-purulent wounds).22 These include organisms from both the patient’s skin flora as well as the oral microbiota of the animal, such as Staphylococcus species. This has been reported as one of the main causes of infections in humans after animal bites or scratches, likely because of virulence as well as high resistance to common antibiotics. Mirroring trends in antibiotic resistance seen elsewhere, there is a rise in methicillin-resistant staphylococci seen in both healthy and sick animals. In one study, up to 14% of Staphylococcus isolates were found to be methicillin-resistant Staphylococcus aureus.23
Pasteurella multocida is a component of the oral flora of many animals, with cats having the highest colonization rate, estimated at approximately 70-90%.24 The organism is a small, gram-negative coccobacillus that is a facultative anaerobe. In 1999, Talan et al published a prospective study in the New England Journal of Medicine of 107 patients who presented with an infected dog or cat bite.26 The most common organisms found in both dog and cat bite wounds were Pasteurella species. Fifty percent of dog bite wounds were infected with Pasteurella species, most commonly Pasteurella canis, compared to P. multocida and Pasteurella septica in cat bites.
Infections are more common in elderly patients, especially those with comorbidities such as diabetes mellitus, coronary artery disease, hypertension, and malignancies. Immunocompromised states also confer risk of infection. The hallmark of a Pasteurella infection is a local intense cellulitis seen within 24 hours of injury. Marked local tenderness, low-grade fever, and associated regional lymphadenopathy may be apparent.25 In one study, clinical signs of infection were seen within 15 hours of exposure.26 In contrast, infections from other pathogens typically do not present for two to three days.
Pulmonary disease is the second most common manifestation of P. multocida and is due to inhaled secretions of infected animals. In rare cases, pneumonia can be complicated by empyema or lung abscess.27 Elderly male patients and those with underlying pulmonary disease are more susceptible to pulmonary complications.28 Systemic infections, such as bacteremia, have been reported in up to 11% of cases.29 Diagnosis is largely clinical, as isolation of the organism via culture can be difficult. In addition, using bipolar staining techniques when infections are caused by Haemophilus influenzae, Neisseria species, and Actinobacter species can result in false-positive results.30 Treatment should be started based on clinical suspicion and not delayed for laboratory results to become available.
Capnocytophaga canimorsus is found in the oral flora of 16-41% of dogs.31 Infection with this organism is an increasingly recognized complication of dog bites, particularly in the alcoholic or splenectomized patient population. The real incidence of this infection is not known because of the difficulty of isolating these fastidious gram-negative organisms in the laboratory setting. Sepsis is the most common presentation, with complications including disseminated intravascular coagulation, hemolytic uremic syndrome, thrombotic thrombocytopenic purpura, and Waterhouse-Friderichsen syndrome. The second most common presentation is meningitis. Endocarditis also has been reported, as has bacteremia in a left ventricular assist device (LVAD) patient.
An unusual feature of the bacterium is that local wound infection generally does not appear severe in patients with high-grade bacteremia noted, which may cause a delay in diagnosis, as the wound initially may not be thought to be the source of bacteremia, and Capnocytophaga may not be considered. The most common patients are males older than 50 years of age who were bitten a few days before presentation. The age of reported victims ranged from a 12-day-old infant with a dog-related scratch to the face to a 99-year-old. Of 292 cases since 1990, 60% involved dog bites and another 24% involved some other contact with dogs, such as scratches or licking. Of note, cats were involved in only 3% of cases. Capnocytophaga canimorsus is susceptible to many antibiotics, including penicillins, but has a high fatality rate of 26%.32
Bartonella henselae, a gram-negative rod that is transmitted by bites or scratches from infected cats, usually kittens, is the organism responsible for cat-scratch disease. These typically are self-limited infections, causing tender, regional lymphadenopathy and fever approximately two to three weeks after inoculation. A pustule or papule may be seen where the injury occurred. As these lesions recede, regional lymph nodes may swell and occasionally suppurate. In rare cases, Parinaud oculoglandular disease, manifested as conjunctivitis with fever and lymphadenopathy near the ear and neck of the affected side, may develop.33 The pathogen is very difficult to isolate in culture.34 Polymerase chain reaction (PCR) is highly specific but not very sensitive, so cat-scratch disease is a clinical diagnosis. For patients with severe pain and lymphadenitis, lymph node aspiration may provide pain relief. For patients with severe systemic signs, rifampin and trimethoprim/sulfamethoxazole have been shown to reduce local signs and symptoms.35
Sporothrix schenckii, known commonly as the “rose gardener disease,” can be found in animal oral cavities, nasal cavities, nails, and feces. Animals may not show any outward signs of infection or may display infected nodules or ulcers on their bodies. Fungal spores are transmitted from the bite or scratch of an infected animal. Human infections are delayed and usually are not clinically evident for three to 12 weeks after inoculation. This infection should be suspected when there is a poor response to the typical antibiotics prescribed after an animal-related injury or if lesions on the patient’s skin follow the classic “sporotrichoid” spread, which is the development of papules or pustules proximal to the initial wound along the path of lymphatic drainage.
The treatment of choice is itraconazole for a four- to 24-week course, depending on the extent of the lesions.36
Other common bacteria in both dog and cat bites are streptococci, Moraxella, Corynebacterium, and Neisseria species. Common anaerobes included Fusobacterium, Bacteroides, Porphyromomas, and Prevotella.26
The human mouth is home to a plethora of pathogens, including facultative species as well as obligate anaerobes. Saliva itself has a dense bacterial load with more than 50 species of bacteria, including Campylobacter species, Corynebacterium, Eikenella corrodens, Haemophilus, Peptostreptococcus, Fusobacterium, Prevotella, Staphylococcus, and Streptococcus species. Although rare, E. corrodens species can spread hematogenously and result in life-threatening bacteremia, sepsis, and endocarditis. Group A Streptococcus is found only in human bites but not in canine or feline bites.37 Conversely, only animal bites grow Pasteurella multocida. Viral pathogens in human bite wounds include the hepatitides, human immunodeficiency virus (HIV), herpes simplex virus (HSV), cytomegalovirus (CMV), and human T-cell lymphotropic virus type 1 (HLTV-1).38,39 The risk of transmission of hepatitis C (HCV) and HIV is low. However, there are isolated case reports describing transmission secondary to human bites. Hepatitis B is 100 times more infectious than HIV in human saliva.
Rabies is a disease that occurs in all mammals and is caused by RNA viruses of the family Rhabdoviridae, genus Lyssavirus. It is transmitted by the saliva of infected animals.40 Worldwide, rabies accounts for 59,000 deaths annually. Domestic dogs carrying a specific rabies variant cause 98% of these deaths. Fortunately, this variant has been eradicated in the United States. Of 5,508 cases of animal rabies reported in the United States in 2015, only 67 cases were in dogs. Geographically, the highest concentration of rabid dogs was in Texas (13), with higher numbers also noted in Puerto Rico (8), North Carolina (6), Georgia (6), and Oklahoma (6).
By comparison, in 2015, rabies was discovered in 244 cats. These cases were focused in the states of Pennsylvania, New York, Maryland, and Virginia. Cats in these areas were thought to be infected mostly by rabid raccoons.
In the United States, more than 90% of rabid animals live in the wild. In 2015, bats made up the largest group of infected animals, with 1,704 cases (30.9% of the total). Racoons, skunks, and foxes also were found to be rabid in significant numbers. In 2015, there were three rabies cases in humans, only one of which was associated with a dog, which the patient had been exposed to while travelling abroad. The other two cases involved a bat and a mongoose.41
Initial Evaluation
History
As with most emergency conditions, history plays a key role in determining what evaluation should take place. The history in patients with mammalian bites should include the following:
- Time and physical location of injury (for example, to the extremities vs. the head);
- Type of animal and circumstances of the bite (i.e., rabies vaccination history, behavior provoked or unprovoked, health, location);
- If vaccination status of an animal is unknown, the animal should be observed for a 10-day period to determine whether it is potentially infected with the rabies virus (BR6).
- Unprovoked injury by wild animals, such as foxes or raccoons, and injury from an ill-appearing animal should heighten concerns for rabies exposure. - Past medical history: Screen for immunocompromised status or other risk factors that would make the patient more susceptible to complications and review patient’s immunization status;
- History of allergies to antibiotics or conditions or medications contraindicating the use of antibiotics also should be considered.
Physical Exam
Evaluation of the wound depth and length and assessment for foreign body and possible associated injuries should be performed. Infection rates in wounds greater than 3 cm in length and in puncture injuries are three times higher than for all other wounds.2 A focus on damage to related structures, proximity to joints, blood vessels, tendon function, as well as neurovascular status all should be assessed. With multiple bites, severe bites, or bites of unknown severity, and for all young children who are victims of an animal attack, a complete trauma-type assessment should be performed. In some cases, dog bites have been associated with fractures, injuries to joints, or neurovascular injury.42 Bites to digits or joints should be explored through range of motion to evaluate for tendon injury.
A rare complication of cat bites that can result in vascular injury is septic pseudoaneurysm.43 This is thought to be a consequence of both direct trauma to a vessel along with colonization by S. aureus, which leads to local inflammatory response, thereby damaging the arterial wall. Pseudoaneurysms present as pain, swelling, and a pulsatile mass at the site of a bite and can be confirmed using duplex ultrasonography.
Bite wounds to the hand deserve special consideration because of the proximity of relatively poorly perfused structures, such as tendons and ligaments, to the skin surface and the risk of serious morbidity from tenosynovitis, septic arthritis, osteomyelitis, and even sepsis.3 A unique hand bite wound is the clenched fist injury, colloquially known as a “fight bite,” which occurs when a closed fist impacts another person’s teeth with sufficient force to break the skin of the hand. Typically, the dorsal surface of the metacarpophalangeal (MCP) joint is affected because of its prominence when a fist is clenched. Bacteria spread through the extension of the MCP joint of the hand, allowing movement of inoculum proximally.
Fight bites are easy to miss during initial evaluation, as they can appear relatively innocuous (the true wound depth may be hidden) and may be treated as minor injuries.39 Patients may not be forthcoming about being involved in physical altercations.44 Two-thirds of fight bites penetrate the extensor tendon and MCP joint capsule.45 There can be significant tendon, cartilage, or bone injury secondary to a fight bite. Morbidity can be significant, as the MCP joint and extensor tendon have poor vascularity and are more prone to infection.19
Complications from fight bites include rapidly destructive septic arthritis of the MCP joint. Very few patients regain previous function if this occurs, and amputation rates for fingers can be greater than 20%. Bacteria also may spread to the palmar surface of the hand, infecting the flexor tendon sheaths. When evaluating infected hand wounds, one should assess for signs of flexor tenosynovitis. These were classically described by Kanavel and are known as the Kanavel signs. (See Table 1.) To assess for tendon injury, consider using the Elson test (positioning the proximal interphalangeal [PIP] at 90 degrees flexed over the edge of a table and having the patient extend against resistance). Weakness or inability to extend the joint indicates rupture of the central slip.46
With regard to the evaluation of human bites in children, the prevailing sentiment since the 1980s is that all bite marks on a child are abuse (non-accidental trauma) until proven otherwise.47 It is commonly believed that measuring the intercanine distance on bite impressions in the skin can help healthcare providers determine whether the injury was inflicted by a child or an adult. An intercanine distance of greater than 3 cm is more likely to be from an adult. However, keep in mind that a dental “adult” can include anyone with permanent teeth, typically > 12 years of age. There also can be significant distortion of the skin depending on the mechanism of the bite or secondary to edema and infection. In addition, there is a relatively large standard deviation in intercanine distance in all age and gender categories. In a study of intercanine distance as a parameter for bite mark analysis, the measurements were found to be unreliable because of three factors: skin distortion, the fact that skin is a poor registration material, and variation in the dynamics of biting.48 Thus, photographing and measuring bite wounds may not be a reliable method to determine whether the perpetrator was a child or an adult.
Table 1. Kanavel Signs |
|
• Affected digit held in a flexed posture • Pain with passive extension of the involved finger • Fusiform swelling of the digit • Tenderness along the tendon sheath |
Diagnostics
In general, a thorough history and physical examination are the highest-yield aspects of the initial evaluation of a bite wound. Most routine diagnostic studies are not useful. A complete blood count (CBC) is rarely useful, as the results may be normal in the case of acute blood loss or with the presence of infection. The erythrocyte sedimentation rate and C-reactive protein may be elevated in patients with clinically evident infections. In patients with a joint prosthesis, these tests may be helpful in identifying occult septic arthritis. Routine HIV testing after human bites is not recommended in most circumstances unless there is visible blood in the saliva or the victim or perpetrator is known to have a history of HCV or HIV.
Cultures in acute bites are not indicated because cultures of apparently uninfected bite wounds predict neither which wounds will become infected nor what the pathogen will be.3,49 Moreover, 8.5% of wound cultures are positive for bacteria before clinical infection sets in, representing colonization.38 Deep tissue cultures obtained in the operating room can be useful for narrowing antibiotic selection in infected wounds. Practitioners should notify the laboratory about the animal source of wound contaminants so that appropriate laboratory techniques can be employed. For example, Pasteurella is a slow-growing pathogen and cultures should be held for up to 10 days. Other organisms may require special growth media.
Radiology workup should be tailored to the situation based on the initial history and physical examination. Plain films are indicated if there are concerns for bone involvement. Occult fractures, the presence of air in the joint, or osteomyelitis may be discovered. In addition, plain films should be used to evaluate for the presence of foreign bodies (e.g., teeth) in the wound, which are of particular concern in bites by cats, small-breed dogs, and older animals that may have extensive periodontal disease, which increases the risk of tooth breakage when biting.50 For delayed presentations, plain films also can be used to evaluate for signs of osteomyelitis (e.g., periarticular osteoporosis, joint space narrowing, bony erosion). Joint involvement is best evaluated by CT scanning.
Wound Care
All bite wounds should be considered contaminated, and the goal is to prevent secondary infection. Appropriate wound care is the cornerstone of initial treatment, and should begin with copious irrigation so that lower rates of colonization can be achieved. The choice of irrigant is less important than the amount of fluid used. Tap water has been shown to be effective for irrigation and is less costly than sterile saline. In addition, patients with upper extremity injuries can stand at the sink with the wound under the faucet stream.51 It may be more difficult to irrigate to the base of a cat bite wound adequately because of the narrow caliber of the wound and the tendency of these wounds to seal off the surface. High-pressure irrigation is not recommended, as it may spread inoculum deeper into the subcutaneous tissues or may create false tracts that will interfere with wound exploration.15 Heavily contaminated bite wounds require debridement and further irrigation, possibly in the operating room. If the animal is suspected to be rabid, a povidone-iodine solution has been shown to be virucidal against rabies and is recommended by the CDC for irrigation. A 10% solution can be diluted further and used both to cleanse the surface skin and to irrigate the wound.26
Closure of Bite Wounds
There has long been controversy about whether it is safe to close animal bites primarily, as there is a theoretical increased risk of infection associated with closure. However, allowing the wound to heal by secondary intention results in scar tissue formation that may cause functional impairment if near a joint, especially of the upper limb and digits.52 During the past several years, studies have demonstrated that primary closure is fairly safe in most cases. (See Table 2.) In 1988, Maimaris and Quinton published a randomized, controlled trial involving 169 ED patients who were treated for dog bites.53 The wounds were cleaned and debrided and then the patients were divided into two groups, one that received sutures and the other that did not receive suture repair. Bites requiring plastic surgery consultation and those involving bone, tendon, nerve, etc., were excluded. Some wounds were repaired in the ED by nurses, and others that were deemed more complex were repaired by physicians in the operating room.
Table 2. Summary Table for Management of Selected Mammalian Bites |
|||
|
Treatment |
Dog |
Cat |
Human |
|
Primary closure |
Generally acceptable on the face, not the hand Requires risk assessment in other locations |
Generally not recommended unless on face and is a cosmetically significant wound |
Yes, for facial wounds |
|
Routine antibiotic prophylaxis |
No, unless on the hand or a complex wound as described in the text, or in the immunosuppressed patient |
Yes |
Yes |
|
Recommended antibiotics71 |
Amoxicillin/clavulanate If penicillin-allergic, consider doxycycline or moxifloxacin Trimethoprim-sulfamethoxazole or a second- or third-generation cephalosporin, ciprofloxacin, or levofloxacin, plus anaerobic coverage with clindamycin or flagyl |
Same as for dog bites |
Amoxicillin/clavulanate Alternatives are ampicillin/sulbactam, carbapenems, and doxycycline * However, only doxycycline has good MRSA coverage |
|
Rabies vaccine |
Yes, if dog is unknown and unavailable for observation |
Yes, if cat is unknown and unavailable for observation |
No |
|
Hepatitis B |
No |
No |
Nonvaccinated patients and antibody-negative patients should receive the hepatitis B vaccine. If the biter is HepBsAg positive, the patient should receive Hep B immunoglobulin as well as the vaccine. |
|
HIV prophylaxis |
No |
No |
Consider if blood present in the mouth of the biter, there is breach of the victim’s skin, or the perpetrator is known to be HIV-positive or is willing to be tested and tests positive |
Of 92 wounds that were closed, seven developed clinical infection. Of 77 left open, six developed infection. The authors concluded that, in general, dog bites can be closed on presentation. However, they noted that nine of the 13 infections were in wounds to the hand. Five of 30 (16.7%) sutured hand wounds were infected compared to only four of 45 (8.9%) unsutured hand wounds. Therefore, the authors concluded that special attention should be paid to dog bites of the hand.53
In 2000, Chen et al published an observational cohort study in which 145 patients with mammalian bites were treated with primary closure. Of these, 88 were dog bites. Five of these 88 patients developed an infection, which is a 5.7% rate of infection. The authors concluded that their overall infection rate was acceptable in situations in which cosmetic outcomes were important.54
In 2011, Wu et al published a retrospective chart review of 87 pediatric patients who presented to the ED with dog bites to the face.55 This represents a group of interest because children are more likely to be bitten by dogs, and if bitten, are more likely to be bitten in the face because of their stature.42 None of the patients in the study required scar revision, and none developed an infection, leading to the authors’ conclusion that primary wound closure, even of some more complex dog bite wounds, was safe from an infection standpoint. Of note, all patients received antibiotics, and 51% received wound repair in an operating room. This limits the applicability of this study to the ED.
In 2014, Paschos et al published a randomized, controlled trial involving 168 patients presenting to an ED within 48 hours of a dog bite.56 Similar to the Maimaris study, complex wounds, such as those complicated by fracture or muscle injury, were excluded. Wounds were thoroughly irrigated, scrubbed with povidone-iodine, and debrided. One group received repair with sutures, and the other group’s wounds were left open. All patients received amoxicillin/clavulanic acid. The researchers studied not only wound infection rates but also measured cosmetic appearance in both groups. They found no statistically significant difference in infection rates between the two groups and reported an 8.3% infection rate overall. The infection rate in sutured wounds was similar at 9.7%.
An interesting separate note in the study was that wounds sutured within eight hours of the bite injury had a lower infection rate of 6.1%. Wounds that were left open had an overall infection rate of 6.9%, with a 2.9% infection rate if patients presented within eight hours. The 9.7% rate in sutured wounds vs. the 6.9% rate in nonsutured wounds was considered to be not statistically significant (P = 0.51; odds ratio [OR], 1.44; 95% confidence interval [CI], 0.48-4.35). Using the Vancouver Scar Scale, sutured wounds showed significantly better results at 1.74, compared to 3.05 for nonsutured wounds (P = 0.0001). The study supports the primary closure of dog bite wounds, particularly in cosmetically significant areas and especially within the first eight hours after the injury.56 To further determine the safety of primary closure of bites, including dog bites, a Cochrane Collaboration Intervention Protocol was published in 2015, but to our knowledge has yet to be completed.57
The general consensus is that human bites are considered contaminated wounds and should be closed by either delayed primary or secondary closure; the exception is bites to the face, which should be sutured primarily for the sake of cosmetic outcome.58,59 We recommend the primary closure of bites that are cosmetically significant, such as those to the face, and also of wounds to the extremity, provided they are not on the hand. The infection risk also should be considered individually based on the patient’s history.42 Table 3 lists considerations during the evaluation of any patient sustaining a mammalian bite.
Table 3. Clinical Concerns in the Evaluation of Bite Wounds |
|
• Child abuse • Cortical penetration or bony fracture • Envenomation • Foreign body • Human pathogen exposure • Nerve injury • Penetration of joint space • Rabies exposure • Tendon injury • Vascular injury Adapted from Rempe B, Aloi M, Iskyan K. Evidence-based management of mammalian bite wounds. Emerg Med Pract 2009;6:1-18. |
Medications
Healthcare providers often prescribe antibiotics to animal bite patients. The term “prophylactic” may not be correct, as the wounds already are inoculated with bacteria at the time of the bite. The question of whether antibiotic prophylaxis is effective in the therapy of bite wound infections was addressed by the authors of a 2001 Cochrane systematic literature review.60 Researchers identified and analyzed eight studies that met the inclusion criteria. The reviewers found no difference in the rates of wound infections in dog bites, regardless of whether prophylactic antibiotics were used. Notably, they excluded bite wounds to the hand. Four of the eight trials grouped patients according to the site of the bite. When hand wounds were analyzed separately, there was a significant improvement in the infection rate from 28% in the control group to 2% in the antibiotic group (OR, 0.10; 95% CI, 0.01-0.86).
The results of the Cochrane review would suggest that antibiotics have not been shown to reduce infection rates in dog bites located in sites other than the hand. However, these studies occurred before Talan et al published the article describing the culture results of these infections.22 In the included studies, providers prescribed penicillin, oxacillin, dicloxacillin, cephalexin, erythromycin, etc.60 The authors concluded that perhaps with antibiotic choices based on current understanding of the bacteria causing dog bite infections, the treatment would be more effective.60 The authors concluded that there is not sufficient evidence to prove antibiotics are effective in preventing infections in non-hand dog bite wounds, but they recommended more research, as studies so far have been small and the possibility of a type two error exists.60
The goal of initial antimicrobial therapy is to cover staphylococci, streptococci, anaerobes, and Pasteurella species. Cephalexin and dicloxacillin generally would be adequate to cover skin flora; however, these do not cover Pasteurella or Eikenella well. These would be covered by penicillin or ampicillin (amoxicillin). The addition of a beta-lactamase inhibitor to amoxicillin (amoxicillin-clavulanate) would allow for the additional coverage of the beta lactamase-producing staphylococci and anaerobes. The first-line oral therapy is amoxicillin-clavulanate, or in penicillin-allergic patients, a fluoroquinolone or cefotaxime.59,61 A three- to five-day course is recommended. However, if the wound appears infected on presentation, a course of 10 days or longer is recommended. (See Table 2.) For higher-risk infections, the first dose of antibiotics may be given intravenously, followed by an oral course. Cephalexin is not recommended as first-line therapy for empiric treatment of cat bite wounds because of a high resistance rate in Pasteurella species. Monotherapy using aminoglycosides, vancomycin, erythromycin, tetracycline, or clindamycin also is not recommended because of concerns about resistance.23 Trimethoprim-sulfamethoxazole should not be used alone, as Capnocytophaga canimorsus is resistant to this agent.62 (See Table 2.)
There is not significant evidence for a benefit of post-exposure prophylactic (PEP) treatment for HIV in human bites, as saliva has a low viral HIV load. However, if there is blood present in the mouth of the biter, there is a breach of the victim’s skin, or the perpetrator is known to be HIV-positive or is willing to be tested and tests positive, then the risk of HIV transmission is increased. The benefits and harms of treatment associated with PEP must be discussed with the patient and a shared decision should be made so as to provide appropriate preventive therapy.19
Treatment with hepatitis vaccine booster vs. immunoglobulin depends on the vaccination status of the patient. Nonvaccinated patients and vaccinated patients who are antibody-negative should receive the hepatitis B vaccine. If the biter is hepatitis B surface antigen (sAg) positive, the patient should receive hepatitis B immunoglobulin as well as the vaccine.63 HBV prophylaxis is indicated if the bite breaks the skin.3
If rabies transmission is a concern, the CDC recommends human rabies immune globulin (HRIG) to be administered to all patients who have not been vaccinated previously. After thorough wound cleansing, 20 IU/kg should be given at the wound site if feasible, and the remainder given at a site distant from the vaccine administration site. Human diploid cell vaccine or purified chick embryo cell vaccine then should be administered intramuscularly as a 1 mL dose into the deltoid muscle. Doses of rabies vaccine given in the gluteus muscle should not be counted as valid and should be repeated. This should occur on day 0 and then on days 3, 7, and 14. In the setting of immunosuppression, the CDC recommends a fifth dose to be administered on day 28. Immunosuppressed individuals also should be tested for adequate immune response upon completion of the series (per the CDC, the rapid fluorescent focus inhibition test should be performed). In previously immunized individuals, no HRIG is needed, and vaccine is required only on days 0 and 3.40
Table 4. Indications for Prophylactic Antibiotics in Bite Wound Management |
|
Patient Risk Factors • Age • Asplenic • Chronic alcohol use • Diabetes mellitus • Immunocompromised • Location (face, hand, joint) • Preexisting edema in affected area • Severity • Time of bite (greater than 12 hours prior to evaluation) • Vascular disease • Wound characteristics Additional Aspects Potential complications (both likely and rare), controversies, pitfalls, medical legal considerations, cost considerations, ethical concerns, patient advocacy Adapted from Rempe B, Aloi M, Iskyan K. Evidence-based management of mammalian bite wounds. Emerg Med Pract 2009;6:1-18. |
Bites in Children
Children are an overrepresented group in bite-related fatalities, and 29.9% of all deaths occur in children 1 to 4 years of age.10 Those younger than 1 year of age had the highest overall death rate. One factor that may explain this fact is that the location of bites varies with age. Unlike in adults, dog bites to small children tend to be to the head or face, where they are more likely to create fatal wounds.17,64 Young boys tend to sustain dog bites more than girls. In the CDC data from 2001, likelihood of being bitten was 293.2/100,000 for boys vs. 216.7/100,000 for girls. This difference is no longer statistically significant at the age of 15 years.5,65
In children 0 to 4 years of age, 64.9% of dog bites occur to the head or neck. In a retrospective review focusing on neurosurgical issues, Kumar et al reported on 124 patients presenting to a Level I trauma center during a 15-year period.66 In the study, 71% of the attacks were by family pets. Of the 124 patients presenting, 17 required neurosurgical evaluation. The average age of the victims was 30 months, and the injuries involved nine girls and eight boys. The attacks were not provoked, and only one dog had bitten previously. The most common injury was depressed skull fracture, but vascular injury, which led to stroke in two patients, also was reported. One of these involved occlusion via dissection of the left ICA, which led to right hemiparesis. In one case, a dural injury was noted via the anterior fontanelle with the fracture of the child’s skull. One patient had a complete spinal cord injury at the T-6 level. Intracranial hemorrhage in the form of subarachnoid, intraparenchymal, and subdural hemorrhage also was reported. Twelve of the patients required neurosurgery.66
Steen et al presented information on intracranial injuries from dog bites.49 Their review of the literature revealed 21 cases of intracranial injuries related to dog bites in the modern literature. They also presented a case series of 10 patients treated at Geisinger Health System between 1992 and 2010. The mean age of patients was 34.5 months. There were six boys and two girls. Five of 10 patients required neurosurgical management. No patient in the series developed abscess or meningitis. This was in contrast to the results of the authors’ literature review in which four of the 21 patients had meningitis or abscess. Ten patients of the 21 required dural repairs, and four required evacuation of intracranial hematomas. None of the patients in the case series had complications. However, of the 21 patients in the literature search, three had late infections on follow-up, two had hemiparesis, one had peripheral nerve palsies, two had seizures, and one of these patients died during initial admission.
Meropenem is recommended as the antibiotic in dog bites with skull penetration, as this antibiotic covers canine oral flora and penetrates the central nervous system. Steen et al also recommend CT when scalp lacerations are present in dog bites, as early recognition may minimize complications by leading to early washout and appropriate antibiotics. Eight of the 21 patients in the case series had missed diagnosis on initial presentation, six of these had complications, with four infections, and two cerebrospinal fluid leaks.49
Patients With Joint Prosthesis
Delayed infection of any joint arthroplasty due to hematogenous spread is a feared complication, as it can lead to joint failure and the need for replacement. Patients who have undergone joint arthroplasty, especially those with coexistent malignancy, are at higher risk of septic arthritis due to P. multocida after an animal bite. This organism has demonstrated consistent ability to cause seeding of a prosthesis, even when post-bite prophylactic antibiotics have been prescribed.67
Prevention
In 2009, Duperrex et al reported on the effect of education of children and adolescents in the prevention of dog bite injuries.64 They found two studies involving infants and children. The authors demonstrated that brief educational programs could be used to change behaviors and improve knowledge base in children. In a 2013 study reported by Dixon et al, children ages 5 to 9 years were given a 14-question test before and after watching a 20-minute educational video on dog safety. The authors reported a three-question improvement after watching the video, with the median score increasing from 11 questions correct to 14. It remains unknown whether such an intervention would translate into decreased numbers of dog bites or dog bite-related fatalities.68
The Blue Dog is a software program designed to instruct children about safe behaviors around dogs by taking them through animated scenarios. Schwebel et al evaluated the effectiveness of this teaching tool. After completing the education program, children were more likely to identify risky dog situations than the controls, but this did not seem to translate into later recall of safe behaviors or improvement in safe behaviors during a live dog interaction.69 Further research in this area is needed.
The psychological effect of dog bites on children must be considered. Up to 50% or more of bite victims may suffer from symptoms of post-traumatic stress disorder.42 In a 2012 study by Boat et al, parents were surveyed one month after having taken their child to the ED for a dog bite. Seventy percent of respondents reported concerning behaviors since the incident. Examples included being fearful of and avoiding dogs, having nightmares, and demonstrating emotional changes.70 Providers should make parents aware of possible behavioral and emotional changes and recommend resources, including counselors, to help deal with the issues.
Disposition
Close follow-up care is crucial in the management of animal bite wounds. It is recommended that low-risk bites be assessed within 48 hours and high-risk bites within 24 hours. Consider admission for patients with hand bites that become infected, because these generally involve deeper structures. Consultation with a hand surgeon is recommended if deep space infection is suspected, if there is tendon sheath or joint involvement, or for contaminated wounds that require debridement and irrigation in the operating room.
REFERENCES
- Kwo S, Agarwal JP, Meletiou S. Current treatment of cat bites to the hand and wrist. J Hand Surg Am 2011;36:152-153.
- Jaindl M, Grünauer J, Platzer P, et al. The management of bite wounds in children — a retrospective analysis at a level I trauma centre. Injury 2012;43:2117-2121.
- Kennedy SA, Stoll LE, Lauder AS. Human and other mammalian bite injuries of the hand: Evaluation and management. J Am Acad Orthop Surg 2015;23:47-57.
- Quirk JT. Non-fatal dog bite injuries in the U.S.A., 2005-2009. Public Health 2012;126:300-302.
- Centers for Disease Control and Prevention (CDC). Nonfatal dog bite-related injuries treated in hospital emergency departments — United States, 2001. MMWR Morb Mortal Wkly Rep 2003;52:605-610.
- Davis AL, Schwebel DC, Morrongiello BA, et al. Dog bite risk: An assessment of child temperament and child-dog interactions. Int J Environ Res Public Health 2012;9:3002-3013.
- Taplitz RA. Managing bite wounds. Currently recommended antibiotics for treatment and prophylaxis. Postgrad Med 2004;116:49-52.
- Esposito S, Picciolli I, Semino M, Principi N. Dog and cat bite-associated infections in children. Eur J Clin Microbiol Infect Dis 2013;32:971-976.
- Ward MA. Bite wound infections. Clin Pediatr Emerg Med 2013;14:88-94.
- Langley RL. Human fatalities resulting from dog attacks in the United States, 1979-2005. Wilderness Environ Med 2009;20:19-25.
- Sacks JJ, Lockwood R, Hornreich J, Sattin RW. Fatal dog attacks, 1989-1994. Pediatrics 1996;97(6 Pt 1):891-895.
- Hutson HR, Anglin D, Pineda GV, et al. Law enforcement K-9 dog bites: Injuries, complications, and trends. Ann Emerg Med 1997;29:637-642.
- Gaston RG, Lewis DR. Animal bites to the hand. Curr Orthopedic Practice 2010;21:559-563.
- Philipsen TE, Molderez C, Gys T. Cat and dog bites: What to do? Guidelines for the treatment of cat and dog bites in humans. Acta Chir Belg 2006;106:692-695.
- Rothe K, Tsokos M, Handrick W. Animal and human bite wounds. Dtch Arztebl Int 2015;112:433-443.
- Benson LS, Edwards SL, Schiff AP, et al. Dog and cat bites to the hand: Treatment and cost assessment. J Hand Surg Am 2006;31A:468-473.
- Aziz H, Rhee P, Pandit V, et al. The current concepts in management of animal (dog, cat, snake, scorpion) and human bite wounds. J Trauma Acute Care Surg 2015;78:641-648.
- Ambro BT, Wright RJ, Heffelfinger RN. Management of bite wounds in the head and neck. Facial Plast Surg 2010;26:456-463.
- Patil PD, Panchabhai TS, Galwankar SC. Managing human bites. J Emerg Trauma Shock 2009;2:186-190.
- Harrison M. A 4-year review of human bite injuries presenting to emergency medicine and proposed evidence-based guidelines. Injury 2009;40:826-830.
- Tabbara M, Hatzigianni P, Fux C, et al. Human bite wounds: A Swiss emergency department experience. Wounds 2012;24:85-90.
- Talan DA, Abrahamian FM, Moran GJ, et al. Clinical presentation and bacteriologic analysis of infected human bites in patients presenting to emergency departments. Clin Infect Dis 2003;37:1481-1489.
- Muniz IM, Penna B, Lilenbaum W. Treating animal bites: Susceptibility of Staphylococci from oral mucosa of cats. Zoonoses Public Health 2012;60:504-508.
- Narsana N, Farhat F. Septic shock due to Pasteurella multocida bacteremia: A case report. J Med Case Rep 2015;9:159.
- Collins C, Flanagan B, Henning JS. An atypical presentation of Pasteurella multocida infection following a cat bite: A case report. Cutis 2012;89:269-272.
- Talan DA, Citron DM, Abrahamian FM, et al. Bacteriologic analysis of infected dog and cat bites: Emergency Medicine Animal Bite Infection Study Group. N Engl J Med 1999;34:85-92.
- Abdelkarim A, Almohammadi A, AhmadJee A, et al. Empyema due to severe Pasteurella multocida treated with quinolone: A case report. Am J Ther 2014;21:e204-e206.
- Blaine H, George MY, Jeandel C. Exposure to domestic cats or dogs: Risk for Pasteurella multocida pneumonia in older people? J Am Geriatr Soc 1998;46:1329-1330.
- Ebright J, Frey AB, Fairfax MR. Pasteurella multocida infections and bacteremia: A twenty-year experience at an urban medical center. Infect Dis Clin Pract 2009;17:102-104.
- Byrd RP Jr, Roy TM. Pasteurella multocida respiratory infection: An important cat-associated zoonosis. Arch Intern Med 2003;163:1239.
- Gaastra W, Lipman LJ. Capnocytophaga canimorsus. Vet Microbiol 2010;140:339-346.
- Butler T. Capnocytophaga canimorsus: An emerging cause of sepsis, meningitis, and post-splenectomy infection after dog bites. Eur J Clin Microbiol Infect Dis 2015;34:1271-1280.
- Talan DA, Abrahamian FM, Moran GJ, et al; Emergency Medicine Human Bite Infection Study Group. Clinical presentation and bacteriologic analysis of infected human bites in patients presenting to emergency departments. Clin Infect Dis 2003;37:1481-1489.
- Shin OR, Kim YR, Ban T, et al. A case report of seronegative cat scratch disease, emphasizing the histopathologic point of view. Diagnostic Pathology 2014;9:62-66.
- Margileth AM. Antibiotic therapy for cat-scratch disease: Clinical study of therapeutic outcomes in 268 patients and a review of the literature. Pediatric Infect Dis J 1992;11:474-478.
- Leelavathi M, Siti Aishah MA, Wong YP, Jamil A. Mismanagement of cat bite wound: Lessons to learn. Clin Ter 2013;164:225-227.
- Raval P, Khan W, Hadded B, Mahapatra AN. Bite injuries to the hand — Review of the literature. Open Orthop J 2014;8:204-208.
- Akkoc G, Kepenekli Kadayifci E, Karaaslan A, et al. Human bite-induced cellulitis due to Streptococcus pyogenes. Wounds 2015;27:E20-E23.
- Malahias M, Jordan D, Hughes O, et al. Bite injuries to the hand: Microbiology, virology and management. Open Orthop J 2014;8:157-161.
- Rupprecht CE, Briggs D, Brown CM, et al. Centers for Disease Control and Prevention (CDC). Use of a reduced (4-dose) vaccine schedule for postexposure prophylaxis to prevent human rabies: Recommendations of the advisory committee on immunization practices. MMWR Recomm Rep 2010;59(RR-2):1-9.
- Birhane MG, Cleaton JM, Monroe BP, et al. Rabies surveillance in the United States during 2015. J Am Vet Med Assoc 2017;250:1117-1130.
- Rempe B, Aloi M, Iskyan K. Evidence-based management of mammalian bite wounds. Emerg Med Pract 2009;6:1-18.
- Dryton G, Allen KB, Borkon AM, et al. Do not bite the hand that feeds you. Ann Vasc Surg 2015;29:363.e3-362.e4.
- Perron AD, Miller MD, Brady WJ. Orthopedic pitfalls in the ED: Fight bite. Am J Emerg Med 2002;20:114-117.
- Patzakis MJ, Wilkins J, Bassett RL. Surgical findings in clenched-fist injuries. Clin Orthop Relat Res 1987;220:237-240.
- McBrien B. Fight bite injury: Emergency department assessment and management. Emerg Nurse 2016;24:34-37.
- Wagner GN. Bitemark identification in child abuse cases. Pediatr Dent 1986;8 (1 Spec No):96-100.
- Tarvadi P, Manipady S, Shetty M. Intercanine distance and bite marks analysis using metric method. Egypt J Forensic Sci 2016;6:445-448.
- Steen T, Ravin K, Timmons S, Kershenovich A. Intracranial injuries from dog bites in children. Pediatr Neurosurg 2015;50:187-195.
- Ellis R, Ellis C. Dog and cat bites. Am Fam Physician 2014;90:239-243.
- Moreira ME, Markovchick VJ. Wound management. Emerg Med Clin North Am 2007;25:873-899.
- Naito K, Sugiyana Y, Igeta Y, et al. Thorough debridement and immediate primary wound closure for animal bite injuries of the upper limbs. Eur J Trauma Emerg Surg 2016;42:213-217.
- Maimaris C, Quinton DN. Dog-bite lacerations: A controlled trial of primary wound closure. Arch Emerg Med 1988;5:156-161.
- Chen E, Hornig S, Shepherd SM, Hollander JE. Primary closure of mammalian bites. Acad Emerg Med 2000;7:157-161.
- Wu PS, Beres A, Tashjian DB, Moriarty KP. Primary repair of facial dog bite injuries in children. Pediatr Emerg Care 2011;27:801-803.
- Paschos NK, Makris EA, Gantsos A, Georgoulis AD. Primary closure versus non-closure of dog bite wounds: A randomised controlled trial. Injury 2014;45:237-240.
- Bhaumik S, Kirubakaran R, Chaudhuri S. Primary closure versus delayed or no closure for traumatic wounds due to mammalian bite (Protocol). Cochrane Database Syst Rev 2015;8:CD011822.
- Acheampong AO, Duah M, Selormey R, et al. Orofacial human bite: A six year review of cases from Komfo Anokye Teaching Hospital. Open Journal of Stomatology 2016;6:179-184.
- Patil PD, Panchabhai TS, Galwanker SC. Managing human bites. J Emerg Trauma Shock 2009;2:186-190.
- Medeiros I, Saconato H. Antibiotic prophylaxis for mammalian bites. Cochrane Database Syst Rev 2001;2:CD001738.
- Gustavsson O, Johansson AV, Monstein HJ, et al. A wide spectrum of fastidious and ampicillin-susceptible bacteria dominate in animal-caused wounds. Eur J Clin Microbiol Infect Dis 2016;35:1315-1321.
- Zangenah S, Andersson, AF, Özenci V, Bergman P. Genomic analysis reveals the presence of a class D beta-lactamase with broad substrate specificity an animal bite associated Capnocytophaga species. Eur J Clin Microbiol Infect Dis 2017;36:657-662.
- Akkoc G, Kepenekli Kadayifci E, Karaaslan A, et al. Human bite-induced cellulitis due to Streptococcus pyogenes. Wounds 2015;27:E20-E23.
- Duperrex O, Blackhall K, Burri M, Jeannot E. Education of children and adolescents for the prevention of dog bite injuries. Cochrane Database Syst Rev 2009;2:CD004726.
- Kaye AE, Belz JM, Kirschner RE. Pediatric dog bite injuries: A 5-year review of the experience at the Children’s Hospital of Philadelphia. Plast Reconstr Surg 2009;124:551-558.
- Kumar R, Deleyiannis FW, Wilkinson C, O’Neill BR. Neurosurgical sequelae of domestic dog attacks in children. J Neurosurg Pediatr 2017;19:24-31.
- Kadakia AP, Langkamer VG. Sepsis of total knee arthroplasty after domestic cat bite: Should we warn patients? Am J Orthop 2008;37:370-371.
- Dixon CA, Pomerantz WJ, Hart KW, et al. An evaluation of a dog bite prevention intervention in the pediatric emergency department. J Trauma Acute Care Surg 2013;75(4 Suppl 3):S308-S312.
- Schwebel DC, Morrongiello BA, Davis AL, et al. The Blue Dog: Evaluation of an interactive software program to teach young children how to interact safely with dogs. J Pediatr Psychol 2012;37:272-281.
- Boat BW, Dixon CA, Pearl E, et al. Pediatric dog bite victims: A need for a continuum of care. Clin Pediatr 2012;51:473-477.
- Stevens DL, Bisno AL, Chambers HF, et al; Infectious Diseases Society of America. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014;59:e10-52.
Bites, whether dog, cat, or human, are a common reason for emergency department visits.This article reviews the complexities of different types of bites ED providers may encounter and issues regarding closure and antibiotic prophylaxis, in addition to vaccination concerns.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
