The Evaluation of the Dizzy Patient
June 1, 2018
Reprints
AUTHORS
Dennis Hanlon, MD, FAAEM, Vice Chairman, Operations, Emergency Medicine Residency, Allegheny Health Network, Pittsburgh, PA
Megan Bedolla, MD, Allegheny General Hospital, Pittsburgh, PA
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Assistant Clinical Professor of Emergency Medicine, Mt. Sinai, NY
EXECUTIVE SUMMARY
- Patients who present with sustained symptoms are best evaluated by HINTS or HINTS plus. HINTS consists of testing for nystagmus, head impulse test, and skew. HINTS plus adds a test for hearing.
- The Dix-Hallpike test is used to assess patients whose symptoms are resolved or are triggered with movement.
- Horizontal nystagmus with the fast component consistently to the same side generally is benign. All other nystagmus should suggest a central cause.
- Patients often cannot describe their symptoms adequately and differentiate between vertigo and lightheadedness.
Many of the tests and maneuvers described in this issue are better learned by watching examples online. There are excellent examples on YouTube and other educational options.
— Sandra M. Schneider, MD, Editor
Introduction
Dizziness is a common complaint among emergency department (ED) patients. Many cases have minor or self-limited causes. An important minority of the patients will have treatable, serious underlying cardiovascular or cerebrovascular disease. Emergency providers need to differentiate benign from serious causes. After separating the general medical and cardiac cases, differentiating stroke from benign peripheral vestibular symptoms while using the fewest possible resources is quite challenging. A large survey of emergency physicians revealed that the top priority in the development of clinical decision rules for adults was a rule to identify serious causes of vertigo.1 Although these clinical decision rules have not yet been developed, this article reviews the epidemiology of dizziness and the approach to the dizzy patient. An emphasis is placed on a detailed history focusing on the paradigm shift to the timing and triggers of dizziness rather than the more traditional focus on the quality or type of dizziness.2 The appropriate use of specific physical exam tests will be discussed, as well as important causes.
Epidemiology
Dizziness is the chief complaint for approximately 3.5% of ED visits.3 The lifetime prevalence of vertigo in patients 18 to 79 years of age is 7.4%, with a definitive, age-related increase in prevalence.4 With the aging of the population, dizzy patients will continue to present to EDs and the numbers may increase. The majority of patients presenting with dizziness will have general medical conditions or cardiac etiologies. In a large database study, these patients accounted for approximately half of patients.3 A substantial portion will have vestibular disorders and central nervous system disorders, with the former being more common and the latter being more serious. The differentiation of these disorders can be difficult and expensive. It has been stated that healthcare costs for patients with dizziness in the United States exceed $10 billion per year.2 A significant amount of these expenses is due to neuroimaging and hospital admissions.6
Efficiently evaluating dizzy patients while avoiding the misdiagnosis of posterior stroke remains difficult. In a large, multistate study, vertigo and dizziness were the symptoms most tightly linked to missed stroke.7 Although the absolute risk of missed stroke in patients with vertigo and dizziness is low, the relative risk of a missed posterior stroke remains high.6
Approximately 10% of patients with a posterior stroke present with symptoms that mimic vestibular neuritis.8 Acute vestibular syndrome is a clinical syndrome of continuous vertigo/dizziness, nausea, vomiting, gait instability, and nystagmus that lasts days to weeks. The majority of these patients have a benign, peripheral vestibular cause, but 25% of these patients will have a cerebellar or brainstem stroke.9 Ischemic strokes in young patients are caused more often by arterial dissection, vasculopathies, and cardiogenic sources such as a patent foramen ovale rather than atherosclerosis.10 The likelihood of stroke is the same in patients with vertigo and those with non-vertiginous dizziness.11
History
On initial presentation, patients with obvious causes for their vertigo, such as trauma, severe hypotension, or malignant arrhythmia, often are separated during triage screening or within a few minutes of presenting to the ED. Recent new medications can be a cause. However, a large percentage of patients will not have an obvious cause on presentation, and obtaining further information is essential in differentiating benign peripheral sources from concerning central causes.
Traditionally, emphasis was placed on describing the quality of symptoms. Patients were asked to describe the sensation in order to categorize it as lightheadedness, a feeling of the room spinning, faintness, or other descriptors. However, more than half of ED patients were inconsistent in their terminology when asked at multiple points during an ED stay, and 79% chose descriptors from more than one category.13 New studies have suggested that categorizing patients with a focus on timing and the presence of triggers is more reliable and aids in differentiating central causes of vertigo.2,12 Determining onset also is useful, as a gradual onset suggests a peripheral cause while an abrupt onset predicts a central cause.9 Furthermore, the presence of continuous vs. intermittent symptoms is important for deciding on further specialized physical exam techniques.
After obtaining information regarding the timing of symptoms, the presence or absence of associated symptoms is the next area of focus. Associated craniocervical pain, including headache, diplopia, or new auditory symptoms, increases the likelihood of a central cause.9,14 Sudden sensorineural hearing loss increases the risk of subsequent stroke by 1.6 times in a five-year period. This likely is due to an anterior inferior cerebellar artery (AICA) territory infarction with a possibility of wider progression in the posterior circulation.15,16 Another red flag is reported symptoms out of proportion to the exam. Severe ataxia or nausea greater than expected suggests a central cause.9
Despite the theoretical association, there is little evidence that an isolated prodromal illness increases the likelihood of a peripheral cause. However, multiple prodromal events strongly increase the likelihood of a central cause.9
Multiple brief episodes of vertigo suggest underlying vascular disease, which can progress to posterior circulation stroke. Other vascular risk factors and patient age > 50 years also increase the likelihood of vertigo due to stroke.9
General Categories
On presentation, associated symptoms can help determine the pathology. However, when vertigo presents in isolation, further separation of the differential diagnosis is more challenging. The TITRATE algorithm can assist in distinguishing categories. It consists of timing, triggers, and targeted exams.17 Specifically, the approach concerns questions related to the timing (acute vs. chronic) as well as duration (continuous vs. intermittent) of symptoms. For the purposes of emergency medicine patients, acute causes are the more likely presentation. These patients can be categorized further into continuous symptoms (acute vestibular syndrome), intermittent triggered episodes (triggered vestibular syndrome), and intermittent non-triggered episodes (spontaneous episodic syndrome). Table 1 summarizes these three broad categories.
Table 1. Vestibular Syndromes |
||||
|
Duration |
Frequency |
Triggers |
Differential Considerations |
|
|
Triggered |
Seconds to minutes |
Intermittent |
Motion |
Benign paroxysmal peripheral vertigo, orthostatic hypotension |
|
Spontaneous Episodic |
Minutes to days |
Intermittent |
None |
Migraine, Ménière’s, transient ischemic attack, cardiac arrhythmia |
|
Acute |
Days to weeks |
Continuous |
None |
Posterior cerebrovascular accident, vestibular neuritis, labyrinthitis, drug induced, Wernicke’s, multiple sclerosis |
The most common cause of acute vestibular syndrome is vestibular neuritis (dizziness only) or labyrinthitis (dizziness plus hearing loss or tinnitus).9 The most frequent dangerous cause is posterior circulation ischemic stroke, most often in the cerebellum or lateral brainstem.9 Of note, despite the thinking that posterior ischemia presents as continuous symptoms, 27% of patients with transient acute symptoms had a stroke in a recent study.14 A rarer cause of acute vestibular syndrome is multiple sclerosis.18
Physical Exam
Initial screening for vital sign abnormalities, arrhythmias, murmurs, and orthostatic hypotension can rapidly differentiate cardiac etiologies. However, in the patient with nonspecific associated symptoms and a reassuring triage exam, a full neurologic exam, including cranial nerves, motor and sensory testing, gait testing, as well as the evaluation of cerebellar signs (finger-nose-finger, heel shin, and rapid alternating movements), is essential.19 Even if the patient is unable to walk, truncal ataxia can be assessed while the patient is seated.19
The presence of gait instability or a subtle focal neurologic deficit has a significant predictive value for central causes. Focal findings include oculomotor deficits, focal weakness, or dysmetria.20 Approximately 30-60% of patients with a posterior stroke will have a focal neurologic deficit.21 The presence of nystagmus is of special importance when attempting to differentiate causes of vertigo. The type of nystagmus is just as informative as the presence or absence of nystagmus.19 Horizontal, unidirectional nystagmus is associated with peripheral causes but is not diagnostic. Torsional, direction-changing, or vertical nystagmus strongly suggests a central cause and should prompt further evaluation. Visual fixation can extinguish nystagmus in both peripheral and central causes.
Following the history, the patient is categorized into a subset of vertigo. This combination of a neurological examination plus additional focused bedside tests can assist in making the clinical distinction between vestibular neuritis and posterior circulation stroke with greater sensitivity than early magnetic resonance imaging (MRI).22,23 However, these results were obtained by neuro-otologists using a targeted oculomotor examination, the HINTS exam, consisting of three components — the head impulse test (HIT), testing for nystagmus, and skew deviation.24 It is not clear that testing in the ED is as sensitive. However, studies suggest emergency physicians can effectively perform these tests.24
Special Tests
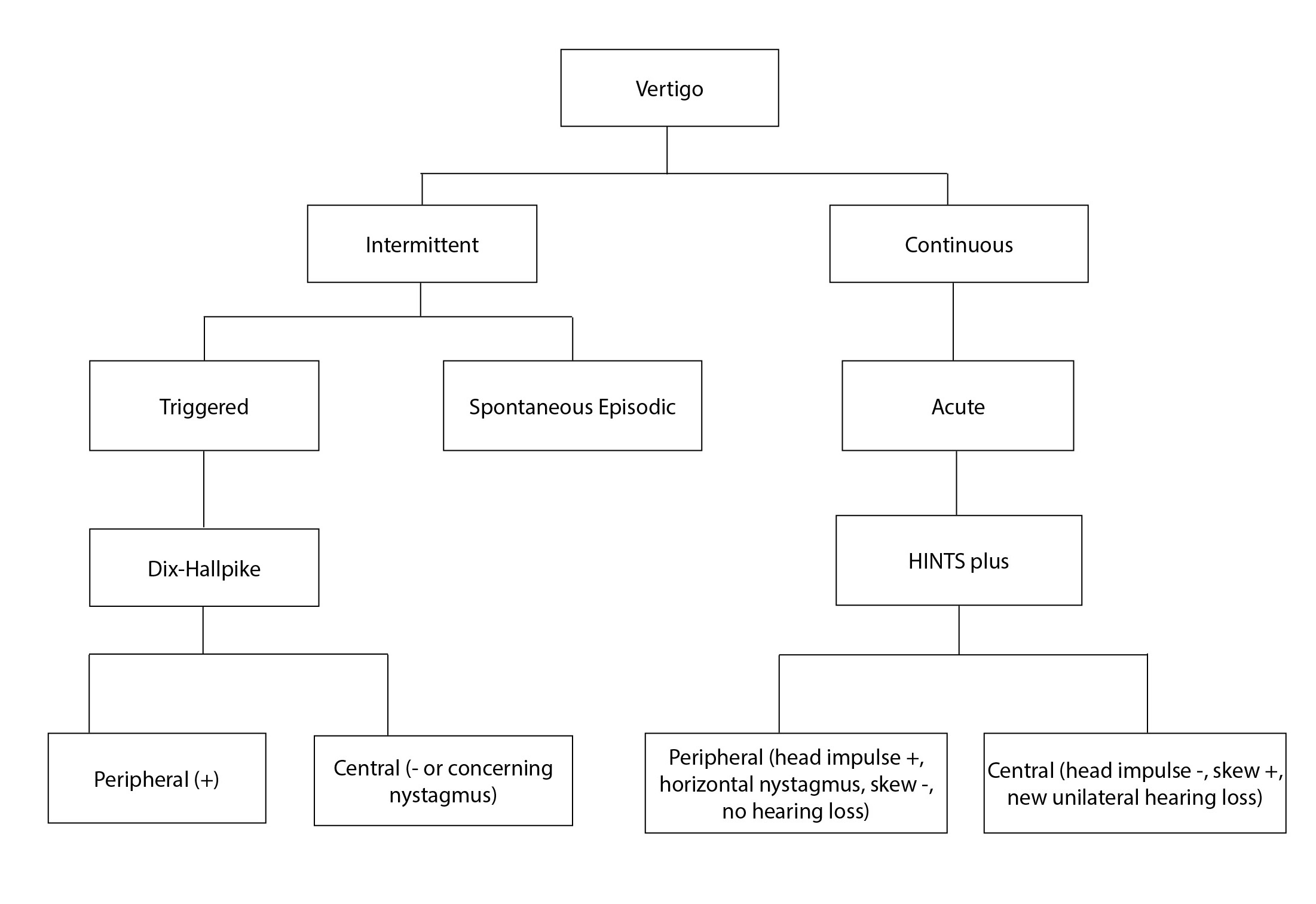
Two commonly used tests in the evaluation of vertigo are: the HINTS (or HINTS plus) exam and the Dix-Hallpike test (often followed by the Epley maneuver for treatment). Their use is determined by the presence of intermittent vs. continuous symptoms and whether nystagmus is present during the physical exam. (See Figure 1 for an algorithm on testing in patients with dizziness.) A HINTS plus exam should be performed on patients with persistent symptoms and nystagmus. If continuous nystagmus is present, then there is little utility in performing a Dix-Hallpike maneuver, which may cause the patient unnecessary discomfort without providing any diagnostic value.19 A Dix-Hallpike maneuver is indicated only in patients with intermittent symptoms who currently are asymptomatic and without nystagmus.
HINTS testing includes three components: head impulse, nystagmus, and test of skew. The HINTS plus test includes the additional step of assessment for new unilateral hearing loss. In patients with at least one risk factor for stroke, HINTS and HINTS plus have a higher sensitivity and specificity than ABCD2 for detecting a central cause of vertigo.25 HINTS also is more sensitive than MRI within the first 48 hours of symptoms.22,26
Figure 1. A Schematic of the Subcategories and Applicable Testing |
 |
To perform a HINTS exam, it is often easier to start with nystagmus, as that symptom typically is noted on the initial physical or neurologic exam. Observe for the presence of nystagmus, both spontaneous and gaze-evoked. Initially, have the patient look straight in a neutral or primary gaze and observe for spontaneous nystagmus. If nystagmus is present, the direction of the nystagmus is named by the direction of the fast component.
The provider can have the patient look to the right for several seconds and then to the left. The patient only needs to move the eyes 15° to 20° off center when testing for gaze-evoked nystagmus. If nystagmus is present, the direction of the fast beat can help differentiate a peripheral cause from a central one. A fast beat in the same direction regardless of the laterality of gaze is described as a fixed nystagmus and suggests a peripheral cause. If the fast beat changes direction with the gaze, it is referred to as direction-changing and indicates a central cause. Nystagmus that is torsional or vertical also suggests a central cause. The finding of a central cause of nystagmus in the setting of an acute vestibular syndrome suggests the cause is a stroke until proven otherwise.
To be certain that nystagmus is absent, the patient should be tested with visual fixation removed. The absence of nystagmus in a patient examined with visual fixation removed essentially excludes a vestibular cause for the dizziness.24,27 Furthermore, if nystagmus is truly absent, then the etiology is unlikely to be a vestibular process, and the head impulse test is not indicated and may yield false information.24
The second step of the HINTS exam is the head impulse test, also referred to as the vestibulo-ocular reflex (VOR). The provider asks the patient to focus his or her vision on a nearby object (often the examiner’s nose). The patient’s head is rotated rapidly from midline to the left or right while the patient is directed to continue focusing on the chosen object. In a normal person, the eyes will remain fixed on the object as the head is turned. If the reflex is impaired (as in peripheral causes of vertigo), as the patient’s head is rotated, his or her focus will shift off the target with a subsequent rapid saccade back when rotation stops. Both directions of rotation must be tested. Rotation toward the affected side will evoke the abnormal reflex. A central cause of vertigo will have a normal VOR or negative head impulse test. The absence of a corrective saccade in acute vestibular syndrome during the head impulse test is consistent with a stroke.
The third step of the HINTS exam is test of skew, also known as the alternate eye cover test. The provider again asks the patient to fix his or her vision on a nearby object. One eye is covered. In central causes of vertigo, this can result in a vertical misalignment. When the eye is uncovered, a corrective vertical saccade may be seen. In peripheral causes, the test of skew will be negative. Skew testing is not very sensitive but has a 98% specificity when positive for a central cause.19
It is important to pay strict attention to the terminology of testing for HINTS. An overview of the interpretation of the HINTS plus exam is listed in Table 2. A peripheral cause is supported by a positive (or abnormal) head impulse test and a negative test of skew. A negative (normal) head impulse test is concerning for a central cause. If any part of the HINTS plus exam indicates a possible central cause, further testing is warranted. A reassuring HINTS exam in combination with the absence of cranial nerve or cerebellar signs and no ataxia reduces the odds of a stroke by 50-fold.9
Table 2. HINTS Plus Exam |
||
|
Peripheral |
Central |
|
|
Head impulse |
Positive (unilateral saccade present, rapid toward affected side) |
Negative (no saccade/normal) |
|
Nystagmus |
Horizontal (beats away from affected side) |
Vertical, rotary, or direction-changing but also can mimic peripheral |
|
Test of skew (eye cover) |
Negative (no skew) |
May be positive (deviation present) |
|
Hearing |
Normal |
New unilateral loss |
The sensitivity for detecting central causes of vertigo can be improved further by adding an additional step, HINTS plus. The new unilateral hearing loss is detected with the ability to hear fingers being rubbed together near the ear. New hearing loss is associated with a central cause as opposed to peripheral (or more benign) etiology. Sudden hearing loss with vertigo is more predictive of stroke than either symptom individually.28
A pilot project using HINTS plus in an ED was able to reduce MRI use from 52% to 31% without any re-admission or re-presentations within 30 days.29
On initial exam, if the patient is determined to be in the category of triggered vestibular syndrome, performing the Dix-Hallpike maneuver may be beneficial. This exam requires that the patient have asymptomatic periods so that nystagmus can be evoked. There are different tests for each semicircular canal. However, the posterior canal is the most commonly affected, and is tested by the Dix-Hallpike test.9
To perform the Dix-Hallpike maneuver, the patient is positioned on the bed so that the patient’s head will be hanging off the end of the bed when supine. The patient’s head is rotated 45 degrees to one side. The examiner assists the patient to move rapidly from sitting to supine with the head hanging off the end of the bed and extension of approximately 20 degrees. The examiner observes for nystagmus. Rotation of the head to the left and right is tested independently.
Frequently, there is a latent period of a few seconds before nystagmus, and the nystagmus should fatigue on repeat testing. If nystagmus is evoked, the test is positive and suggests a peripheral cause, specifically benign paroxysmal peripheral vertigo (BPPV). This cause of vertigo often can be treated with an Epley maneuver. If the Dix-Hallpike test is negative, the patient may have a peripheral cause, but further testing is warranted.
Emergency Department Testing
Most of the essential information is obtained on history and physical exam; however, cardiac monitoring and an electrocardiogram (ECG) may determine cardiac etiologies of dizziness or vertigo quickly. Vital signs may suggest general medical causes and may reveal orthostasis in the patient with a triggered vestibular syndrome. There are no routine laboratory tests required in the evaluation of the dizzy patient.
Neuroimaging
The specific role for neuroimaging has not been defined fully. Between 1995 and 2004, there was a 169% increase in the use of neuroimaging studies in patients who presented to the ED with dizziness.25 There is considerable practice variation in the use of these studies. In one large study, there was a greater than 10% variation in the use of computed tomography (CT) scan, and an eight-fold variation in the use of MRI.30 The sites with increased use of neuroimaging did not have a concomitant increase in the diagnosis of stroke.30
The CT scan is the most readily available of neuroimaging studies. However, a CT scan has a low sensitivity for ischemic stroke, especially in the first 24 hours and particularly in the posterior fossa.31,32 Several studies demonstrated a very low (< 1%) yield of CT scan in patients with dizziness or vertigo alone.5,31,32
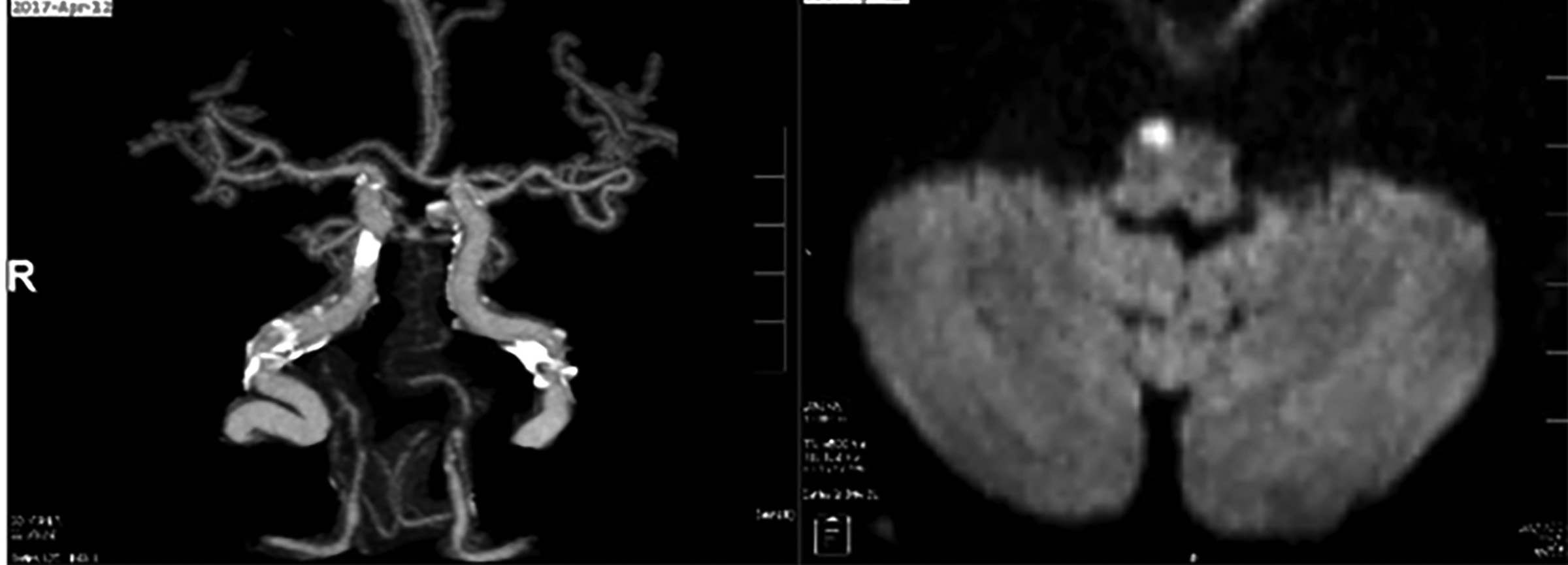
An early MRI also was falsely negative in almost 15% of patients with infarctions confirmed on delayed MRI.26 In small brainstem strokes, diffusion-weighted MRI still can miss up to 50% of the first small strokes when tested within 48 hours.23 Despite its limitations, MRI still is the diagnostic test of choice when a posterior stroke is suspected. Figure 2 shows a small acute infarct right medial ventral medulla that was not identified on CT.
Figure 2. CTA and MRI of Stroke |
 |
|
On the right, CT angiography shows extensive calcifications of cerebrovascular vessels. On the left, MRI demonstrates small acute infarct right medial ventral medulla. This stroke was missed on two CT scans. |
A history of vertigo with headache or neck pain suggests a vertebral artery dissection, and CT angiography (CTA) is the test of choice.33
Avoiding unnecessary neuroimaging in patients with a clear diagnosis of a peripheral vestibular disorder could save nearly $1 billion per year in healthcare expenditures.6
Important Clinical Entities
Acute Vestibular Syndromes
Posterior Circulation Stroke. Although most strokes in the anterior or middle circulations do not present a diagnostic dilemma, diagnosing an acute cerebellar infarction can be very challenging. The most common symptoms are dizziness, vertigo, and gait instability, which are nonspecific and frequently have benign causes.4 Posterior fossa strokes may present with spontaneous acute vestibular syndrome that completely mimics vestibular neuritis (or labyrinthitis if auditory symptoms are associated).34 In fact, cerebellar infarction presenting with isolated vertigo mimicking vestibular neuronitis is more common than previously thought.8 However, it is an uncommon event and remains difficult to identify. Approximately 4% of patients presenting with vertigo or dizziness will receive a cerebrovascular diagnosis.35 That rises to approximately 25% among acute vestibular syndrome presentations.9 Patients with cerebellar stroke have a negative (normal) head impulse test (HIT).8,24,26 This is because the circuit of the VOR does not loop through the cerebellum.
Occasionally, patients with brainstem stroke have a falsely positive (abnormal) HIT because a lateral brainstem infarct involves the location where the vestibular nerve enters the brainstem.8,24,26 Such strokes are uncommon and involve the anterior inferior cerebellar artery (AICA). Strokes in the AICA distribution usually present with associated acute hearing loss. The addition of a bedside test of hearing (HINTS plus) helps identify an AICA stroke.26 The blood supply to the labyrinth is from the branches of the AICA. Ischemia due to narrowing of these branches can cause hearing loss, so the combination of hearing loss and dizziness can occur from a stroke.36,37,38 This is important because some may assume that when both hearing deficits and dizziness are present, then the problem is peripheral.36,37,38
The key features distinguishing stroke from vestibular neuritis are the pattern of nystagmus and the results of the head impulse test.39 Down-beating nystagmus or bidirectional gaze-evoked nystagmus is an immediate indication that the cause must be in the central nervous system. Another highly suspicious pattern of nystagmus is a pure torsional pattern. Although all patients with vestibular neuritis have an unsteady gait, the true inability to walk is another red flag for cerebellar or brainstem infarction.8 In patients with suspected acute brainstem or cerebellar stroke, admission and neurologic consultation are warranted for definitive neuroimaging and treatment, even in the presence of negative initial neuroimaging.
Vertebral Artery Dissection. Cervical arterial dissection (which includes both carotid and vertebral arterial dissections) causes approximately 1-2% of all ischemic strokes, but causes up to 25% of ischemic strokes in younger patients.33 Vertebral artery dissection is more common in younger individuals, particularly women, and should be suspected in any patient who presents with headache, neck pain, and vertigo. These patients may not have any associated focal neurologic signs.40,41 If vertebral artery dissection is suspected, CTA is the preferred test over magnetic resonance angiography (MRA).42 The optimal treatment of dissections has not been demonstrated in the literature. Antiplatelet therapy or anticoagulation may be used with the goal of preventing ischemic complications.
Vestibular Neuritis. Vestibular neuritis is a benign, self-limited, presumed viral or post-viral inflammatory condition affecting the vestibular nerve and causing spontaneous acute vestibular syndrome.43 Some cases are associated with underlying inflammatory disorders, such as multiple sclerosis or sarcoidosis, but most cases are idiopathic and may be linked to herpes simplex infections.43 Although vestibular neuritis usually is abrupt in onset, 25% of cases will have a brief prodromal episode in the previous week.43 Patients with vestibular neuritis nearly always report true vertigo, which is described characteristically as a sensation of spinning of the environment or perception of movement when none is present.39,43 The symptoms typically are severe for the first couple of days with gradual resolution over the subsequent weeks to months. The diagnosis is clinical and requires excluding other causes. The clinician’s main goal is differentiating an acute vestibular syndrome caused by vestibular neuritis from a potential posterior circulation stroke. The only pattern of nystagmus that can result from a peripheral vestibular lesion is unidirectional, horizontal nystagmus. In an acute, severe dizziness presentation, any other pattern should be considered a central nervous system sign.39 A patient with unidirectional nystagmus, a positive head thrust in the direction opposite the fast phase of nystagmus, and no other neurologic features can be diagnosed with vestibular neuritis with a high degree of certainty.39
A short course of corticosteroids can be considered for patients with vestibular neuritis. A randomized controlled trial found that patients with vestibular neuritis treated with corticosteroids within three days of symptom onset had a greater likelihood of recovery of the peripheral vestibular caloric response at one year.44 After the initial severely symptomatic period, it is important that patients resume activities because this helps the brain to adjust and compensate for the asymmetry of vestibular signals. In a randomized trial, a formal vestibular therapy was found to lead to improved outcomes in patients with vestibular neuritis.45
Multiple Sclerosis. Multiple sclerosis (MS) is a chronic inflammatory disorder that affects the brain, spinal cord, and optic nerve and typically presents in young adults between 20 and 45 years of age. A hallmark of MS is multiple episodes of inflammation that produce neurological symptoms separated in space and time. Vertigo is the initial symptom in nearly 5% of patients diagnosed with MS, and 50% of patients with MS will have vertigo during the course of their disease.4,46 The history of present illness, past medical history, and associated neurological symptoms can help differentiate MS from more common causes of the acute vestibular syndrome. MRI is diagnostic for MS, but it does not need to be obtained urgently unless stroke has not been excluded.
Triggered, Episodic Vestibular Syndromes
Benign Paroxysmal Positional Vertigo. (Table 3 summarizes the features of BPPV.) BPPV is the most common vestibular cause of dizziness, and the incidence increases with age. BPPV results from mobile crystalline debris in one or more semicircular canals (canaliths) in the vestibular labyrinth. The most common semicircular canal affected is the posterior canal because of its dependent anatomic location. BPPV is characterized by brief, repetitive periods of rotational vertigo triggered by head movement. These episodes generally last more than a few seconds but less than a minute.47 Occasionally, nausea or a mild lightheadedness can last longer than one minute, but if any positional dizziness persists more than one minute, the provider should strongly consider other potential causes.24,43 In more difficult cases, BPPV can produce non-vertiginous symptoms that are triggered with head movement.14,24
Table 3. Characteristics of the Types of Benign Paroxysmal Positional Vertigo |
||||
|
Type of Benign Paroxysmal Positional Vertigo (Canal) |
Incidence |
Diagnostic Maneuver |
Nystagmus Produced |
Treatment |
|
Posterior (classic BPPV) |
60-90% |
Dix-Hallpike |
Upbeat-torsional |
Epley maneuver |
|
Horizontal (HC-BPPV) |
10-20% |
Supine roll test |
Supine roll test horizontal |
Gufoni maneuver |
|
Anterior |
3% |
Dix-Hallpike |
Down-beating |
Epley maneuver |
The diagnosis is confirmed by reproducing symptoms using canal-specific positional testing maneuvers and identifying a canal-specific nystagmus.24,47 Since the offending canal generally is not known in advance, a sequence of diagnostic maneuvers typically is performed. The Dix-Hallpike maneuver typically is performed first because it tests the posterior canal, which is involved most commonly.27 When the patient with posterior canal BPPV is placed in the head-hanging position (Dix-Hallpike test) with the head turned toward the affected side, a burst of upbeat and torsional nystagmus is observed. When the head is turned to the side during the Dix-Hallpike test, the plane of the posterior canal on that side is now higher and allows the canaliths to drop down by gravity. The nystagmus typically lasts 15 to 25 seconds before it fatigues.
BPPV of the anterior canal is quite rare.48 When anterior canal BPPV is present, the Dix-Hallpike test will trigger a short burst of down-beating nystagmus.48,49
BPPV commonly is treated with various medications, including anticholinergics, antihistamines, or benzodiazepines. All three of these medication groups have adverse effects. Bedside canalith repositioning (the Epley maneuver) may be used as treatment with equal efficacy.50,51 Success of the maneuver can be confirmed by re-testing. If the Dix Hallpike test continues to trigger nystagmus, the Epley maneuver can be repeated.39,51 BPPV of the anterior canal also will respond to the Epley maneuver.39,48 The annual recurrence rate of BPPV is 15%.52
With horizontal canal benign paroxysmal positional vertigo (HC-BPPV), the nystagmus triggered by head movement is a horizontal nystagmus rather than the vertical-torsional nystagmus seen with the more common BPPV of the posterior canal.39,52 HC-BPPV is more likely to resolve spontaneously than other types of BPPV, so its incidence may be underestimated.52 If the patient lies supine and turns the head to either side, thus in the plane of the horizontal canal, nystagmus will be triggered. The nystagmus of HC-BPPV typically lasts longer than nystagmus triggered by posterior canal BPPV.48 The two potential patterns of nystagmus in HC-BPPV are geotropic and apogeotropic. In geotropic HC-BPPV, the nystagmus beats toward the floor or toward the earth.53 In apogeotropic HC-BPPV, the nystagmus beats to the ceiling or away from the earth.54 The pattern that occurs depends on the location of the debris within the horizontal canal.
Although in some cases HC-BPPV can resolve spontaneously, it can be more difficult to treat than posterior canal BPPV.39 A common repositioning strategy is to have the patient roll toward the unaffected side (360 degrees) in 90-degree increments.39 The unaffected side generally is the side that triggers less severe nystagmus.
Another approach, Vanucchi’s forced prolonged position, involves instructing the patient to lie on the unaffected side for 12 hours, which can be done at home rather than in the ED.39,52 A method that can be used for both geotropic or apogeotropic HC-BPPV is the Gufoni maneuver.52 The patient quickly lies down on the unaffected ear for one to two minutes, and the head then is rotated toward the floor for two minutes before the patient sits up.53 To use the Gufoni maneuver for apogeotropic HC-BPPV, the patient quickly lies down on the affected ear for one to two minutes, and the head then is rotated toward the ceiling for two minutes before the patient sits up.54
Orthostatic Hypotension. Orthostatic hypotension is the other common cause for a triggered episodic vestibular syndrome.43 The most common causes of acute orthostatic hypotension are medications and hypovolemia. Particularly in the elderly, BPPV can mimic the postural lightheadedness of orthostatic hypotension.43,55,56
Central Paroxysmal Positional Vertigo. Rarely, a patient who clinically seems to have BPPV actually has a central mimic, called central paroxysmal positional vertigo (CPPV).43 CPPV results from a lesion of the cerebellum or the brainstem, including Chiari malformation, cerebellar tumor, multiple sclerosis, and degenerative ataxia disorders.39 The key to distinguishing a central nervous system disorder from a peripheral vestibular disorder is the pattern of nystagmus. The most common pattern of central positional nystagmus is pure down-beating nystagmus that persists. Pure torsional nystagmus is another type of central positional nystagmus.
In addition to the pattern of nystagmus, several factors should be considered in distinguishing BPPV from CPPV: the presence of symptoms or signs that are not seen in BPPV, such as headache, diplopia, or abnormal cranial nerve or cerebellar function; the presence of nystagmus without dizziness; a poor response to therapeutic maneuvers; and frequent recurrent symptoms.39,43 Although down-beating nystagmus can be seen with anterior canal BPPV, BPPV of this canal is rare. It is safer for emergency physicians to consider this finding concerning for a central lesion.39
Spontaneous, Episodic Vestibular Syndromes
Vertebrobasilar Transient Ischemic Attack. Transient ischemic attacks (TIAs) should be the primary concern in the patient who presents with new-onset, recurrent, spontaneous episodes of dizziness.39,43 Dizziness and even isolated attacks of vertigo can be caused by TIAs.57 Prompt diagnosis is critical since 5% of TIA patients progress to experience a stroke within 48 hours.58,59 Recurrent dizziness or vertigo is possibly the only symptom of an impending basilar artery occlusion.43,60 Also, dizziness is the most common presenting symptom of vertebral artery dissection.41,61 Since the symptoms generally have resolved at the time of patient presentation, the diagnosis of a TIA is based predominantly on the patient’s history. A CT scan is not helpful. CTA, MRI, and MRA are the tests to consider when the posterior circulation needs to be assessed.39
Migrainous Vertigo. The most common benign cause of spontaneous, episodic vestibular syndrome is vestibular migraine; however, it remains a diagnosis of exclusion. If the symptoms are new in onset, stroke or TIA must be considered if the features do not fit a peripheral vestibular disorder.62,63,64 The duration of individual episodes can vary from seconds to days.65
Vestibular migraine may be differentiated from BPPV by more frequent number of recurrences, younger age, and atypical positional nystagmus.64 Symptoms can present as an acute severe attack, positional episodes, or recurrent spontaneous attacks.62,63 Patients frequently report that stimuli, such as light, sound, or motion, trigger or aggravate the symptoms, similar to non-vestibular migraines.39 A headache at the onset of dizziness frequently is reported but is not required, and this headache may differ from a patient’s typical migraine.65
The diagnosis of vestibular migraine requires recurrent attacks with vestibular symptoms, a history of migraine according to the International Classification of Headache Disorders, and migraine symptoms during at least half of the attacks.65 As with TIA, the diagnosis of vestibular migraine is based on clinical history and the exclusion of alternative causes.65
Ménière’s Disease. Patients with Ménière’s disease have recurrent, severe episodes of dizziness/vertigo with nausea, vomiting, and imbalance.66 These episodes are accompanied by unilateral hearing loss and tinnitus. Only 25% of these patients present with the complete symptom triad. In addition, nonvertiginous dizziness is common.39 The tinnitus of Ménière’s disease classically is described as a loud roaring, unilateral tinnitus.39,66 Although the nystagmus may not follow all the rules of peripheral vestibular nystagmus described in vestibular neuritis, the same red flags for central causes apply. The head impulse test generally is normal since the vestibular nerve is intact. The definitive diagnosis of Ménière’s disease requires at least two spontaneous episodes of vertigo lasting at least 20 minutes and audiometrically documented hearing loss and tinnitus with other causes of these symptoms to be excluded.66 With these diagnostic requirements, it is not possible to diagnose new-onset Ménière’s disease definitively in the ED, although the disease may be suspected.
Pitfalls
The evaluation of the dizzy patient remains challenging and has many pitfalls. Overreliance on the qualitative description of the dizziness has been linked to potential misdiagnosis.13,67 The history must focus on triggers and timing to categorize these patients appropriately with the proper vestibular syndrome.43
A patient’s description that the dizziness worsened with head movement is not equal to dizziness triggered by head movement. A patient with dizziness from any cause will feel worse with certain position changes, but the patient with BPPV has dizziness that is triggered by positional changes and then returns to normal baseline between attacks. A patient with vestibular neuritis often is misclassified as having BPPV because the symptoms improve when the patient remains still and worsen with movement. However, that is different from the patient who returns entirely to normal at rest. Even more important is not to assume the patient has a benign vestibular syndrome because the patient’s symptoms increased with head movement.
The National Institutes of Health Stroke Scale (NIHSS) is heavily weighted toward the neurological deficits caused by anterior circulation strokes. In fact, truncal ataxia is not part of the NIHSS, yet it was the most common physical finding in patients with a score of 0 on the NIHSS but MRI-proven strokes.69 While the NIHSS is very important to standardize discussions about the severity of a stroke, a low score does not rule out a posterior stroke.
It is important not to neglect eye findings. The presence or absence of nystagmus and its pattern are extremely important when trying to distinguish benign from serious causes of dizziness.39,43,69 The finding of nystagmus means that either peripheral or central components of the vestibular system are involved.39 Nystagmus usually rules out most general medical disorders.39 Any pattern of nystagmus other than fixed or unidirectional horizontal nystagmus suggests a central cause for the presentation.
Another pitfall is application of the wrong test (HINTS vs. Dix-Hallpike). The HINTS (or preferably HINTS plus) should be used for patients who have persistent dizziness and nystagmus. The Dix-Hallpike should be used for patients with a history of dizziness that currently is resolved.
CT scans do not detect posterior circulation strokes reliably. MRI done early in the patient’s course may be falsely normal.
Conclusion
Dizziness is a common complaint caused by numerous diseases that range from benign to extremely serious. Although the majority of such patients have underlying general medical conditions or cardiac etiology, a substantial number of these patients have vestibular and neurologic causes. There is significant overlap in the presentation of patients with these causes; however, only in an extremely rare case can all of the vestibular neuritis examination features be mimicked by a stroke.39 Nonetheless, the diagnosis can be very difficult, leading to the overutilization of resources, particularly neuro-imaging. No single feature is definitely diagnostic, and it is essential that the clinician interpret each individual feature in the setting of the entire clinical encounter.
The newer paradigm for the evaluation of the dizzy patient, based on a history featuring timing and triggers, is more consistent with the current literature. History and physical examination can be more accurate, more directed, more efficient, and more likely to result in a specific diagnosis using this new targeted paradigm rather than the traditional one that relied on symptom quality.2,19
REFERENCES
- Eagles D, Stiell IG, Clement CM, et al. International survey of emergency physicians’ priorities for clinical decision rules. Acad Emerg Med 2008;15:177-182.
- Edlow JA, Gurley KL, Newman-Toker D. A new diagnostic approach to the adult patient with acute dizziness. J Emerg Med 2018;54:469-483.
- Newman-Toker DE, Hsieh YH, Camargo CA Jr, et al. Spectrum of dizziness visits to U.S. emergency departments: Cross-sectional analysis from a nationally representative sample. Mayo Clin Proc 2008;83:765-775.
- Kulstad C, Hannafin B. Dizzy and confused: A step-by-step evaluation of the clinician’s favorite chief complaint. Emerg Med Clin North Am 2010;28:453-469.
- Saber Tehrani AS, Coughlan D, Hsieh YH, et al. Rising annual costs of dizziness presentations to U.S. emergency departments. Acad Emerg Med 2013;20:689-696.
- Newman-Toker DE. Missed stroke in acute vertigo and dizziness: It is time for action, not debate. Ann Neurol 2015;79:27-31.
- Newman-Toker DE, Moy E, Valente E, et al. Missed diagnosis of stroke in the emergency department: A cross-sectional analysis of a large population based sample. Diagnosis 2014;1:155-66.
- Lee H, Sohn SI, Cho YW, et al. Cerebellar infarction presenting isolated vertigo: Frequency and vascular topographical patterns. Neurology 2006;67:1178-1183.
- Tarnutzer AA, Berkowitz AL, Robinson KA, et al. Does my dizzy patient have a stroke? A systematic review of bedside diagnosis in acute vestibular syndrome. CMAJ 2011;183: E571-592.
- Putaala J, Metso AJ, Metso TN, et al. Analysis of 1008 consecutive patients aged 15 to 49 with first-ever ischemic stroke: The Helsinki Young Stroke registry. Stroke 2009;40:1195–1203.
- Kerber KA, Brown DL, Lisabeth LD, et al. Stroke among patients with dizziness, vertigo, and imbalance in the emergency department: A population-based study. Stroke 2006;37:2484-2487.
- Edlow JA. Diagnosing dizziness: We are teaching the wrong paradigm! Acad Emerg Med 2013;20:1064-1066.
- Newman-Toker DE, Cannon LM, Stofferahn ME, et al. Imprecision in patient reports of dizziness symptom uality: A cross-sectional study conducted in an acute care setting. Mayo Clin Proc 2007;82:1329-1340.
- Choi JH, Park MG, Choi SY, et al. Acute transient vestibular syndrome: Prevalence of stroke and efficacy of bedside evaluation. Stroke 2017;48:556-562.
- Lin HC, Chao PZ, Lee HC. Sudden senorineural hearing loss increases the risk of stroke: A 5-year follow-up study. Stroke 2008;39:2744-2748.
- Lee H. Audiovestibular loss in anterior inferior cerebellar artery territory infarction: A window to early detection? J Neurol Sci 2012;313:153-159.
- Newman-Toker DE, Edlow JA. TiTrATE: A novel approach to diagnosing acute dizziness and vertigo. Neurol Clin 2015;33:577-599.
- Edlow JA, Newman-Toker DE. Medical and nonstroke neurologic causes of acute, continuous vestibular symptoms. Neurol Clin 2015;33:699-716.
- Edlow JA, Newman-Toker D. Using the physical examination to diagnose patients with acute dizziness and vertigo. J Emerg Med 2016;50:617-628.
- Chase M, Joyce NR, Carney E, et al. ED patients with vertigo: Can we identify clinical factors associated with acute stroke? Am J Emerg Med 2012;30:587-591.
- Edlow JA, Newman-Toker DE, Savitz SI. Diagnosis and initial management of cerebellar infarction. Lancet Neurol 2008;7:951-964.
- Kattah JC, Talkad AV, Wang DZ, et al. HINTS to diagnose stroke in the acute vestibular syndrome: Three-step bedside oculomotor examination more sensitive than early MRI diffusion-weighted imaging. Stroke 2009;40:3504-3510.
- Saber Tehrani AS, Kattah JC, Mantokoudis G, et al. Small strokes causing severe vertigo: Frequency of false-negative MRIs and nonlacunar mechanisms. Neurology 2014;83:169-173.
- Edlow JA. A new approach to the diagnosis of acute dizziness in adult patients. Emerg Med Clin North Am 2016;34:717-742.
- Navi BB, Kamel H, Shah MP, et al. Application of the ABCD2 score to identify cerebral vascular causes of dizziness in the emergency department. Stroke 2012;43:1484-1489.
- Newman-Toker DE, Kerber KA, Hsieh YH, et al. HINTS outperforms ABCD2 to screen for stroke in acute continuous vertigo and dizziness. Acad Emerg Med 2013;20:987-996.
- Welgampola MS, Bradshaw AP, Lechner C, Halmagyi GM. Bedside assessment of acute dizziness and vertigo. Neurol Clin 2015;33:551-564.
- Chang TP, Wang Z, Winnick AA, et al. Sudden hearing loss with vertigo portends greater stroke risk than sudden hearing loss or vertigo alone. J Stroke Cerebrovasc Dis 2018;27:472-478.
- Dumitrascu OM, Torbati S, Tighiouart M, et al. Pitfalls and rewards for implementing ccular motor testing in acute vestibular syndrome: A pilot project. Neurologist 2017;22:44-47.
- Kim AS, Sidney S, Klingman JG, Johnston SC. Practice variation in neuroimaging to evaluate dizziness in the ED. Am J Emerg Med 2012;30:665-672.
- Wasay M, Dubey N, Bakashi R. Dizziness and yield of emergency head CT scan: Is it cost effective? Emerg Med J 2005;22:312.
- Lawhn-Heath C, Buckle C, Christoforidis G, Straus C. Utility of head CT scan in the evaluation of vertigo/dizziness in the emergency department. Emerg Radiol 2013;20:45-49.
- Robertson JJ, Koyfman A. Cervical artery dissections: A review. J Emerg Med 2015;51:508-518.
- Baloh RW. Clinical practice. Vestibular neuritis. N Engl J Med 2003;348:1027-1032.
- Kerber KA, Meurer WJ, West BT, Fendrick AM. Dizziness presentations in U.S. emergency departments, 1995-2004. Acad Emerg Med 2008;15:744-750.
- Lee H. Neuro-otological aspects of cerebellar stroke syndrome. J Clin Neurol 2009;5:65-73.
- Lee H, Kim JS, Chung EJ, et al. Infarction in the territory of anterior inferior cerebellar artery: Spectrum of audiovestibular loss. Stroke 2009;40:3745-3751.
- Lee SH, Kim JS. Acute diagnosis and management of stroke presenting with dizziness or vertigo. Neurol Clin 2015;33:687-698.
- Kerber KA. Vertigo and dizziness in the emergency department. Emerg Med Clin North Am 2009;27:39-50.
- Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd edition. Cephalgia 2013;33:629- 808.
- Gottesman RF, Sharma P, Robinson KA, et al. Clinical characteristics of symptomatic vertebral artery dissection: A systematic review. Neurologist 2012;18:245-254.
- Vertinsky AT, Schwartz NE, Fischbein NJ, et al. Comparison of multidetector CT angiography and MR imaging of cervical artery dissection. AJNR Am J Neuroradiol 2008;29:1753-1760.
- Edlow JA. Diagnosing patients with acute-onset persistent dizziness. Ann Emerg Med 2018;71:625-631.
- Strupp M, Zingler VC, Arbusow V, et al. Methylprednisolone, valacyclovir, or the combination for vestibular neuritis. N Engl J Med 2004;351:354-361.
- Strupp M, Arbusow V, Maag KP, et al. Vestibular exercises improve central vestibulospinal compensation after vestibular neuritis. Neurology 1998;51:838-844.
- Karatas M. Central vertigo and dizziness: Epidemiology, differential diagnosis, and common causes. Neurologist 2008;14:355-364.
- Fife TD, von Brevern M. Benign paroxysmal positional vertigo in the acute care setting. Neurol Clin 2015;33:601-617.
- Anagnostou E, Kouzi I, Spengos K. Diagnosis and treatment of anterior-canal benign paroxysmal positional vertigo: A systematic review. J Clin Neurol 2015;11:262–267.
- Aw ST, Todd MJ, Aw GE, et al. Benign positional nystagmus: A study of its three-dimensional spatio-temporal characteristics. Neurology 2005;64:1897-1905.
- Sacco RR, Burmeister DB, Rupp VA, Greenberg MR. Management of benign paroxysmal positional vertigo: A randomized controlled trial. J Emerg Med 2014;46:575-581.
- Epley JM. The canalith repositioning procedure: For treatment of benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg 1992;107:399-404.
- Kim JS, Zee DS. Clinical Practice. Benign paroxysmal positional vertigo. N Engl J Med 2014;370:1138-1147.
- Kim JS, Oh SY, Lee SH, et al. Randomized clinical trial for geotropic horizontal canal benign paroxysmal positional vertigo. Neurology 2012;79:700-707.
- Kim JS, Oh SY, Lee SH, et al. Randomized clinical trial for apogeotropic horizontal canal benign paroxysmal positional vertigo. Neurology 2012;78:159-166.
- Lawson J, Johnson I, Bamiou DE, Newton JL. Benign paroxysmal positional vertigo: Clinical characteristics of dizzy patients referred to a falls and syncope unit. QJM 2005;98:357-364.
- Oghalai JS, Manolidis S, Barth JL, et al. Unrecognized benign paroxysmal positional vertigo in elderly patients. Otolaryngol Head Neck Surg 2000;122:630-634.
- Paul NL, Simoni M, Rothwell PM; Oxford Vascular Study. Transient isolated brainstem symptoms preceding posterior circulation stroke: A population-based study. Lancet Neurol 2013;12:65-71.
- Edlow JA. Managing patients with transient ischemic attack. Ann Emerg Med 2018;71:409–415.
- Shah KH, Kleckner K, Edlow JA. Short-term prognosis of stroke among patients diagnosed in the emergency department with a transient ischemic attack. Ann Emerg Med 2008;51:316-323.
- von Campe G, Regli F, Bogousslavsky J. Heralding manifestations of basilar artery occlusion with lethal or severe stroke. J Neurol Neurosurg Psychiatry 2003;74:1621-1626.
- Savitz SI, Caplan LR, Edlow JA. Pitfalls in the diagnosis of cerebellar infarction. Acad Emerg Med 2007;14:63-68.
- Dieterich M, Brandt T. Episodic vertigo related to migraine (90 cases): Vestibular migraine? J Neurol 1999;246:883-892.
- von Brevern M, Zeise D, Neuhauser H, et al. Acute migrainous vertigo: Clinical and oculographic findings. Brain 2005;128:365-374.
- von Brevern M, Radtke A, Clarke AH, Lempert T. Migrainous vertigo presenting as episodic positional vertigo. Neurology 2004;62:469-472.
- Seemungal B, Kaski D, Lopez-Escamez JA. Early diagnosis and management of acute vertigo from vestibular migraine and Meniere’s disease. Neurol Clin 2015;33:619-628.
- Minor LB, Schessel DA, Carey JP. Meniere’s disease. Curr Opin Neurol 2004;17;9-16.
- Kuruvilla A, Bhattacharya P, Rajamani K, Chaturvedi S. Factors associated with misdiagnosis of acute stroke in young adults.
J Stroke Cerebrovasc Dis 2011;20:523-527. - Martin-Schild S, Albright KC, Tanksley J, et al. Zero on the NIHSS does not equal the absence of stroke. Ann Emerg Med 2011;57:42-45.
- Grewel K, Austin PC, Kapral MK, et al. Missed strokes using CT imaging in patients with vertigo: Population-based cohort study. Stroke 2015;46:108-113.
Dizziness is a common complaint among emergency department patients. Emergency providers need to differentiate benign from serious causes.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
