What Is the Key ECG Finding?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
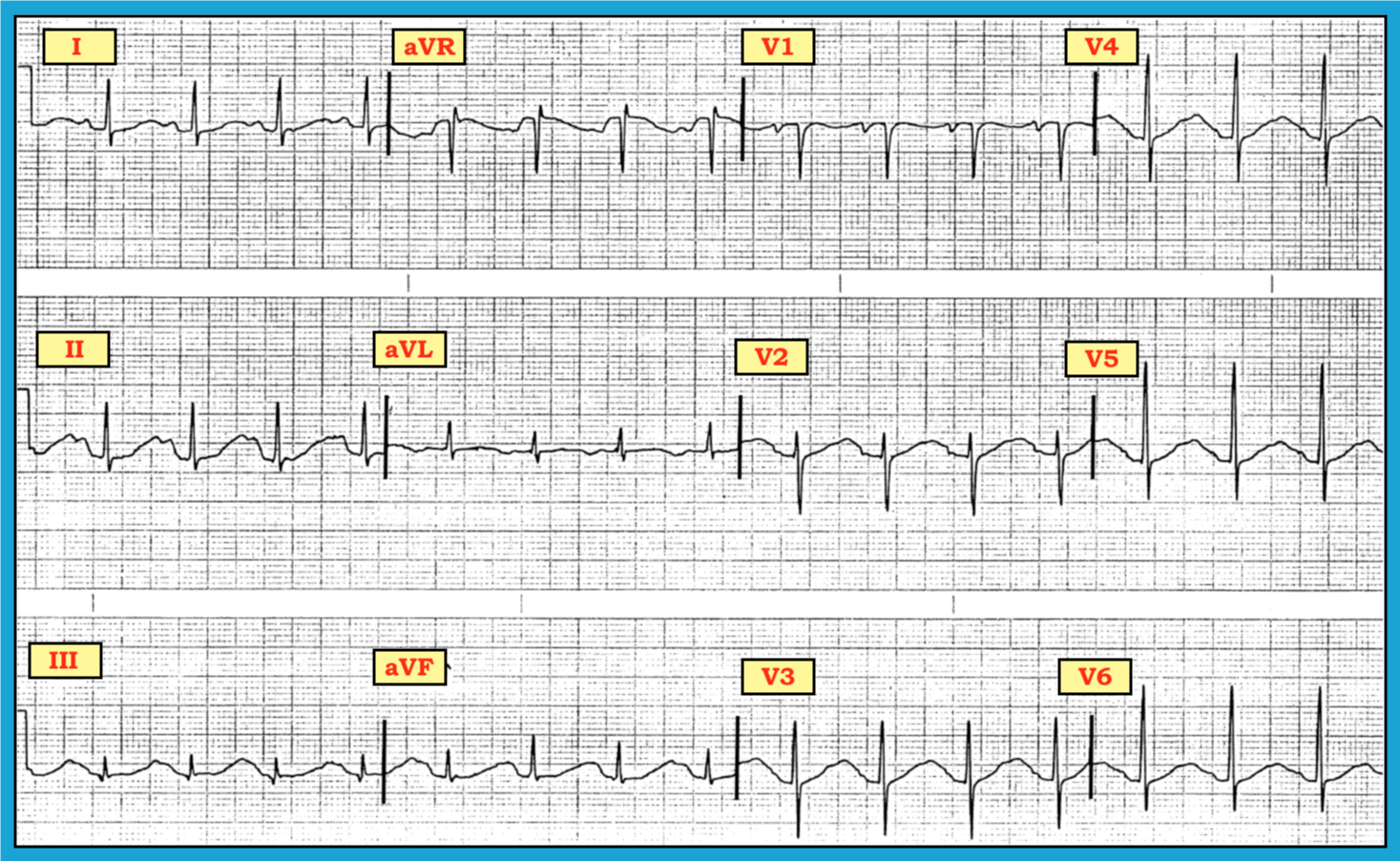
A 59-year-old woman presented to a medical facility in an unresponsive state. Staff presumed the patient had sepsis. The patient underwent an ECG that medical staff read as “normal.” How might one interpret the ECG in the figure below? Which clinical entities could contribute to the irregular findings?
Although P waves are not easily observable in lead II, they are clearly visible with a constant PR interval in leads I and V1. Thus, the underlying rhythm is sinus tachycardia at a rate of ~100/minute. Regarding intervals, the PR interval is normal, and the QRS complex is narrow. However, the QT interval is extremely long. Regarding the rest of the systematic interpretation, the mean QRS axis is normal (about + 40 degrees). There is no chamber enlargement, and one can observe nonspecific ST-T wave abnormalities in several leads (without significant ST elevation or depression).
The principal finding is the very long QT interval, although it is difficult to determine if the suggestion of slight notching toward the end of the T wave in several leads is due to partial fusion with the P wave or fusion with a large U wave. Regardless, the QT interval for this tracing is markedly prolonged. Therefore, the key ECG finding is the long QT. Recognition of a significantly prolonged QT interval should prompt consideration of three causes: drugs, “Lytes” (i.e., electrolyte disorders, specifically Ca++, low serum K+, or Mg++), and central nervous system (CNS) calamities (including bleeding, tumor, seizure, stroke, trauma, or coma).
Of note, while ischemia/infarction and conduction defects also may produce QT lengthening, these conditions usually will be obvious from the ECG. When the principal ECG abnormality is a long QT interval, think “Drugs-Lytes-CNS” as the likely cause(s). Then, correlate clinically.
Because she was unresponsive and staff presumed sepsis, the patient’s altered mental status might account for the prolonged QT visible on her ECG. Additional clinical information is needed on this patient to determine if drug effect, electrolyte disturbance, and/or additional CNS insult also might contribute to the ECG abnormalities.
For more information about and further discussion on this case, please visit: https://bit.ly/2MdyrUU.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
