Use of a Low-carbohydrate, Ketogenic Diet to Treat Obesity
October 1, 2018
Reprints
AUTHORS
Eric C. Westman, MD, MHS, Division of General Internal Medicine, Department of Medicine, Duke University Medical Center; HEAL Diabetes Clinics, Durham, NC
Justin Tondt, MD, Ghent Family Medicine Residency, Eastern Virginia Medical School, Norfolk, VA
Jacqueline Eberstein, RN, HEAL Diabetes Clinics, Durham, NC
William S. Yancy Jr., MD, MHS, Division of General Internal Medicine, Department of Medicine, Duke University Medical Center; Center for Health Services Research in Primary Care, Durham Veterans Affairs Medical Center; and Duke Diet and Fitness Center, Duke University Health System, Durham
PEER REVIEWER
Carlos Jordan, MD, Assistant Professor of Internal Medicine, Wright State University, Hospitalist, SDACC, Dayton, OH; Diplomate, American Board of Obesity Medicine
EXECUTIVE SUMMARY
Few clinical conditions are more problematic and challenging for primary care physicians than the management of obesity. For patients who are motivated to lose weight, there are a legion of dietary interventions that compete for their attention through advertisements and that bewilder practitioners. Many practitioners are aware of the typically low success rates of most diets, and both they and their patients are often frustrated with the likelihood of failure.
- Obese and overweight populations have increased dramatically in the United States, with a prevalence now reaching nearly 40%.
- The American Board of Obesity Medicine publishes guidelines for the treatment of obesity and, along with the American Medical Association, designates obesity as a disease.
- Ketogenic diets have been under increased scientific study and acceptance since the first published report of an individual using a low-carbohydrate diet to treat obesity in 1863.
- Advantages of low-carbohydrate diets, which may be combined with intermittent fasting, include reduction in hunger, improved serum triglyceride and high-density lipoprotein, association with reduced cardiovascular disease risk, and greater glycemic control.
- Side effects include mild symptoms of fatigue, headache, and less frequent stooling, often confused with constipation and muscle cramps. Because of the diet’s beneficial effects on blood sugar, patients on hypoglycemic agents need to be monitored carefully.
Overweight and obesity have reached epidemic proportions in the United States. For individuals affected by obesity, clinical studies have shown that carbohydrate restriction, including a low-carbohydrate, ketogenic diet, can be a safe and effective treatment. This article includes a narrative review of clinical research studies and a practical description of implementing a “keto” diet for obesity.
Introduction
The prevalence of overweight and obesity has increased dramatically over the years, with obesity levels now reaching 39.8% in the United States.1 Obesity brings with it an increased risk for premature mortality and development of comorbidities, including hypertension, dyslipidemia, and type 2 diabetes mellitus.2 Although in the past, many healthcare providers regarded obesity as a problem of “lack of will power,” now it is recognized as a disease by the Obesity Medicine Association (OMA) and the American Medical Association.3,4 The designation of obesity as a disease compels primary care providers to become involved in its treatment, and has led to an increase in insurance coverage of its treatment.
Obesity medicine specialists are specially trained in safe and effective medical treatments that include nutrition, physical activity, and medications to treat and maintain long-term remission of obesity.5 In fact, it is now possible for physicians to receive advanced training and a diploma from the American Board of Obesity Medicine (ABOM).6 However, not all doctors need to become ABOM certified in obesity medicine, as many of the principles that obesity medicine specialists employ can be used in the context of a primary care practice.
The OMA publishes its guidelines for the treatment of adult obesity in the form of an algorithm,3 in which obesity is defined as “a chronic, relapsing, multi-factorial, neurobehavioral disease, wherein an increase in body fat promotes adipose tissue dysfunction and abnormal fat mass physical forces, resulting in adverse metabolic, biomechanical, and psychosocial health consequences.” One of the important changes in the updated algorithm is the recommendation to use “patient-first” language (i.e., an individual affected by obesity) and a comprehensive review of the evaluation and the treatment of obesity. Other sources for practical information and office tools can be found in the textbook, Obesity: Evaluation & Treatment Essentials, as well as materials from the Obesity Action Coalition.7,8
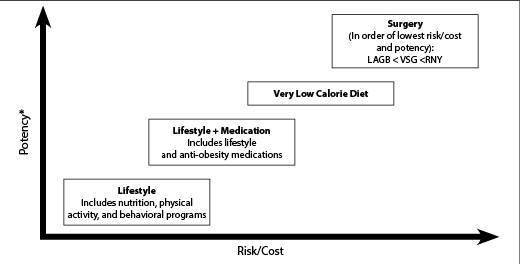
The OMA includes several evidence-based nutritional approaches for the treatment of obesity in its algorithm. (See Figure 1.) Traditional nutritional approaches have involved the explicit restriction of calories (“eat fewer calories”) and the recommendation for people to increase energy expenditure (“exercise to burn more calories”). Although many people can benefit from calorie restriction, another conceptual approach to obesity is to understand it fundamentally as a hormonal problem of excessive insulin, which then leads to the use of carbohydrate restriction because dietary carbohydrates potentially raise insulin levels.9 This article will provide a definition of obesity, review the clinical research supporting the use of carbohydrate-restricted diets for weight loss, and give examples of how to use carbohydrate restriction to treat obesity effectively in a medical setting.
Figure 1. Current Treatment Options for Obesity |
|
*Potency includes many factors, such as the amount, rate, and sustainability of weight loss, and the long-term resolution of adiposopathy and fat mass disease. Potency varies greatly for each individual (i.e., long-term adherence to a lifestyle program can be as potent as gastric bypass surgery). |
|
LAGB: laparoscopic adjustable gastric banding; VSG: vertical sleeve gastrectomy; RNY: Roux-en-Y gastric bypass Reprinted with permission. © Obesity Medicine Association® 2018. All rights reserved Bays HE, Seger, J, Primack C, Long J, Shah NN, Clark TW, McCarthy W. Obesity Algorithm, presented by the Obesity Medicine Association. 2017-2018. www.obesityalgorithm.org (Accessed Sept. 18, 2018). |
Clinical Vignette
Mr. S is a 60-year-old male who came to our clinic because he was not able to lose weight, despite multiple attempts on his own, and he didn’t want to use medications to lose weight. He worked as a photographer, but especially enjoyed being a Boy Scout leader, which involved hiking and camping. At his highest weight, he did not think that he would be able to attend the annual national Scout gathering because he was not able to hike anymore. His maximum weight was 332 pounds in February 2010, and his body mass index (BMI) was 45.7 kg/m2. Over the next eight years, by following a low-carbohydrate, ketogenic diet, he lost weight and maintained his weight at 208.8 pounds (BMI, 28.0 kg/m2). He now is able to hike at the annual Scout gathering and plans to continue this lifestyle to maintain his health and quality of life.
Definitions
Disease is defined as a condition of the living animal or plant body or of one of its parts that impairs normal functioning and typically is manifested by distinguishing signs and symptoms.
Obesity is defined as “a chronic, relapsing, multifactorial, neurobehavioral disease, wherein an increase in body fat promotes adipose tissue dysfunction and abnormal fat mass physical forces, resulting in adverse metabolic, biomechanical, and psychosocial health consequences.”
Diagnosis of Obesity. Although there is no perfect way to diagnose excessive body fat accumulation, most experts use a BMI > 30 kg/m2, increased percent body fat (> 32% for women and > 25% for men), or increased abdominal girth (> 35 inches for women and > 40 inches for men). (See Table 1.)
Table 1. Obesity Classification |
|
|
Classification |
Body Mass Index |
|
Normal |
18.5-24.9 kg/m2 |
|
Overweight |
25-29.9 kg/m2 |
|
Obesity Class I |
30-34.9 kg/m2 |
|
Obesity Class II |
35-39.9 kg/m2 |
|
Obesity Class III* |
> 40 kg/m2 |
|
*Replaces morbid obesity Body mass index (BMI) = weight in kg/(height in meters)2 |
|
Metabolic Syndrome. According to guidelines from the National Heart, Lung, and Blood Institute and the American Heart Association, metabolic syndrome is diagnosed when a patient has at least three of the following five conditions:
- Fasting glucose ≥ 100 mg/dL (or receiving drug therapy for hyperglycemia);
- Blood pressure ≥ 130/85 mmHg (or receiving drug therapy for hypertension);
- Triglycerides ≥ 150 mg/dL (or receiving drug therapy for hypertriglyceridemia);
- High-density lipoprotein cholesterol (HDL-C) < 40 mg/dL in men or < 50 mg/dL in women (or receiving drug therapy for reduced HDL-C);
- Waist circumference ≥ 102 cm (40 inches) in men or ≥ 88 cm (35 inches) in women; if Asian American, ≥ 90 cm (35 inches) in men or ≥ 80 cm (32 inches) in women.10
Treatment of Obesity Affects More Than Weight
One of the effects of an increase in body fat is abnormal biomechanical stress on the body, which is relieved with weight loss.11,12 However, an increase in body fat also promotes metabolic health consequences. Adipose tissue is an active endocrine organ with systemic effects on the body. When body fat accumulates past one’s individual threshold, adipose tissue becomes unable to function properly and accumulates in visceral compartments, including intraperitoneal and intraorgan.13 This dysfunctional adipose tissue is a proposed cause of type 2 diabetes, hypertension, and cardiovascular disease and can be recognized by elements of the metabolic syndrome.14 A low-carbohydrate, ketogenic diet appears not only to be effective for obesity, but also to be effective for visceral obesity, leading to an improvement in these comorbid conditions.15,16
General Nutritional Principles to Treat Obesity
The OMA Obesity Algorithm outlines many treatment approaches, including the use of nutrition, physical activity, behavioral therapy, and pharmacotherapy.3 The general principles of healthy nutrition include limiting highly processed foods of little nutritional value (“junk foods”) and limiting energy-dense beverages like sugar-sweetened beverages. Foods that should be encouraged include healthy proteins and fats, vegetables, leafy greens, fruits, nuts, legumes, and whole grains. For obesity treatment, the most appropriate nutritional therapy should be safe, effective, and one to which the patient can adhere.
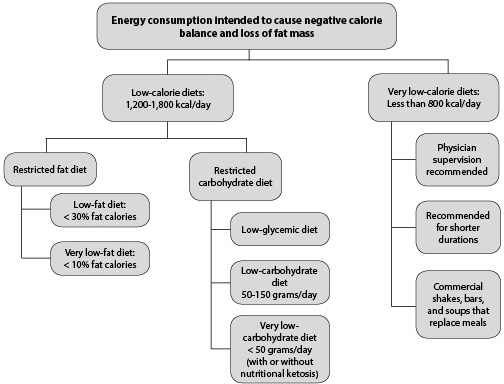
Nutritional approaches for the treatment of obesity include manipulation of the fat or carbohydrate consumption to obtain a lower caloric intake, typically from 1,200 to 1,800 calories/day. (See Figure 2.) Most low-fat approaches teach individuals to count calories, whereas very low-carbohydrate approaches lead to a spontaneous reduction in caloric intake without explicit calorie restriction. Very low-calorie diets typically provide less than 800 calories/day and require specially formulated meal replacements to ensure adequate macro- and micro-nutrient intake; physician supervision is recommended. Since most clinicians are familiar with the low-calorie diets, this paper will address the use of one type of carbohydrate-restricted diet: the low-carbohydrate, ketogenic diet.
Figure 2. Nutritional Therapy for Obesity |
 |
|
Reprinted with permission. © Obesity Medicine Association® 2018. All rights reserved Bays HE, Seger, J, Primack C, Long J, Shah NN, Clark TW, McCarthy W. Obesity Algorithm, presented by the Obesity Medicine Association. 2017-2018. www.obesityalgorithm.org (Accessed Sept. 18, 2018). |
Many experts believe that the common mechanism of weight loss diets is a reduction in insulin levels and insulin resistance.9 Insulin is one of the most potent hormones that promotes lipogenesis and also inhibits lipolysis. This effect often is observed when using exogenous insulin in the treatment of type 2 diabetes mellitus — most individuals will gain weight. The use of insulin to treat type 2 diabetes mellitus, which already is associated with hyperinsulinemia, is counterproductive if weight loss is desired.
Origins of Ketogenic Diets to Treat Obesity
The first published report of an individual using a low-carbohydrate diet to treat obesity was in 1863.17 In London, William Banting published his experience in the Treatise on Corpulence, and it became a popular method of weight loss for many years. In England, the word “banting” referred to reducing sugar and starch in the diet for the purposes of weight loss. In fact, the most widely recommended diet for obesity until 1950 was a low-carbohydrate diet. John Yudkin, a professor of nutrition in the United Kingdom, brought attention to carbohydrate restriction as a method of losing weight, and suspected that sugar was a culprit in many modern illnesses.18 From about 1970 to 2010, the rise of the idea that dietary fat causes heart disease led to the thought that carbohydrate-restricted approaches were unhealthy. However, recent systematic reviews and lay-press reviews of nutritional science have begun to cast doubt on the idea that dietary fat causes heart disease.19-22
If the dietary carbohydrate intake is sufficiently low to cause an increase in blood or urine ketone bodies (typically < 20-50 grams of carbohydrate/day), then these diets are called “ketogenic diets.” The low-carbohydrate, ketogenic diet decreases hunger, causing a spontaneous decrease in ad libitum calorie consumption.23 Ketosis may be responsible for the suppression of hunger, but an increase in protein and fat intake or an elimination of refined sugar and starch also may contribute to hunger reduction.
Randomized, Controlled Trials of Carbohydrate Restriction for Obesity
In the last 15 years, several independent groups have studied low-carbohydrate diets for the treatment of obesity in the outpatient setting. These studies have been summarized in meta-analyses,24-26 and have shown that low-carbohydrate diets are at least as effective for weight loss as low-fat, reduced-calorie diets, but the metabolic effects are quite different. When compared to low-fat diets, low-carbohydrate ketogenic diets improve serum triglyceride and HDL to a greater degree. Similarly, in the recently published DIETFITS trial, the carbohydrate-restricted group saw a greater improvement in triglycerides and HDL, although carbohydrate intake was not restricted to the point of ketosis, and both groups eliminated refined grains and added sugars.27
Although most of the studies to date about the low-carbohydrate diet involve weight loss, diabetes, or cardiometabolic risk factors, there is one outcome study assessing carotid intimal thickness in which the low-carbohydrate diet was one of three intervention arms.28 In this study, after two years, all diet interventions, including the low-carbohydrate diet, led to significant regression of carotid intimal thickness. In a post hoc analysis, the effect appeared to be mediated by dietary adherence, weight loss, and a reduction in blood pressure. These results are important because they demonstrate that the consumption of dietary fats along with carbohydrate restriction did not have negative effects on carotid intimal thickness, as has been feared. The mechanism of how a ketogenic diet could reduce cardiovascular disease risk may be related to its effect on the metabolic syndrome — improvements in abdominal circumference, blood glucose, blood pressure, serum triglyceride, and HDL-C.29
Instruction/Monitoring of a Ketogenic Diet
There are many ways to provide instruction on how to follow a ketogenic diet, including books, videos, handouts, computer and smart phone apps, and classes.30-31 After an initial medical evaluation, we teach the ketogenic diet in a 60-minute small group setting using handouts developed for our geographic area. (See Table 2.) We ask people to choose foods that they like from a list of very low glycemic foods, and instruct them to consume less than 20 total grams of carbohydrates per day. (See Table 3.) The major sources of nutrition are meat, poultry, fish, shellfish, and eggs. Vegetables and leafy greens are limited such that each meal will have a very low or negligible effect on postprandial rise in blood glucose. Although not necessarily a goal, to achieve ketosis it is necessary to keep the total carbohydrate intake less than 20-50 grams per day. At first, fruits, berries, and nuts are not allowed, as these are common “trigger foods” that cause hunger and, therefore, make it difficult for most people to control portions. After one to two days, hunger is diminished and people reduce their caloric intake without explicitly counting calories. When the hunger is diminished, people often eat once or twice a day, which has been called “intermittent fasting.” Non-sugar sweeteners can be used to treat sugar cravings, and weight loss still will occur.
Table 2. Recommended Medical Evaluation Prior to Use of a Ketogenic Diet for Obesity |
|
Table 3. Example of Foods Allowed on a Low-carbohydrate, Ketogenic Diet |
|
Keep the total carbohydrates per day between 20 and 50 grams, depending upon the level of carbohydrate tolerance. |
|
Eat as much as wanted until comfortably full:
|
|
Eat a limited amount of:
|
Continued instruction occurs during the follow-up visits. (See Table 4.) Many clinical practices, including ours, have patients return for a follow-up visit after two to four weeks. In a clinical practice, the expected weight loss is about one to two pounds per week. Some programs may ask patients to use food diaries, computer or smart phone apps, ketone measurements, or daily weight records to enhance or measure adherence. For patients affected by diabetes, home monitoring of blood glucose is essential if taking insulin or a sulfonylurea, and subsequent clinic visits are necessary for de-prescribing to reduce the risk of hypoglycemia. Follow-up clinic visits generally are scheduled at monthly intervals until the patient’s health measures are stable and the patient has adapted to the lifestyle change. The long-term daily carbohydrate intake level is individualized over time based on patient preference, metabolic outcomes, and the control of hunger and cravings essential for long-term success. The measurement of ketones is not necessary, but can be useful for troubleshooting if the weight loss is less than expected.
Table 4. Follow-up Medical Evaluation |
|
‘De-prescribing’ Medication
A healthy lifestyle, including the low-carbohydrate, ketogenic diet, is as potent as multiple prescription medications. In one study for weight loss, the low-carbohydrate, ketogenic diet was as powerful as the low-fat, low-calorie diet AND the weight-loss drug orlistat.34 A related diet, called the ketogenic diet, also has been shown to have potent antiepileptic effects.35 Common medications that may result in overdosage if not adjusted include insulin, other hypoglycemic medications (both oral and injectable), antihypertensives, and diuretics. Hypoglycemic and antihypertensive medications may require rapid tapering (days to weeks) to avoid hypoglycemia and hypotension. Several other medications no longer may be needed, as improvements in heartburn (gastroesophageal reflux disease), irritable bowel syndrome (diarrhea predominant), and polycystic ovary syndrome (PCOS) commonly are seen.36-38 When treating PCOS, nonhormonal contraception should be used to avoid an unwanted pregnancy.
Patients taking medications for certain conditions require more attention and may benefit by referral to an obesity medicine specialist. As the dietary changes and weight loss exert their effects, many medications may need to be adjusted or discontinued. If there is a history of heart failure or salt-sensitive hypertension, then sodium restriction will be continued and close monitoring is in order. However, it is important to note that initiation of the diet is associated with diuresis and natriuesis; therefore, adequate sodium intake is emphasized to prevent dehydration, particularly during initiation of the diet — in the absence of hypertension or heart failure. If a vitamin K antagonist is used for anticoagulation, then vitamin K restriction will be continued. More frequent monitoring of anticoagulation may be needed if there is a significant change in intake of leafy greens or other foods containing vitamin K.
Side Effects
During the first few days of the diet change, there may be mild symptoms of fatigue or headache, which can be prevented or minimized by adequate fluid and sodium intake. If there is no history of hypertension or heart failure, we recommend consuming one to two bouillon cubes (or the sodium equivalent) per day for the first week to reduce the likelihood of these symptoms. If diabetes or hypertension medications are used, then overmedication can occur. (See Table 5.) In addition, home glucose monitoring is mandatory if the patient is taking insulin or taking multiple hypoglycemic agents.
Table 5. Causes of Side Effects During the First 2 Weeks |
|
Side Effect |
Recommended Action |
|
Low blood glucose due to overmedication |
Reduce medication |
|
Low blood pressure due to overmedication |
Reduce medication |
|
Fluid shifts from diuresis |
Discontinue diuretic Add or increase salt (e.g., bouillon), if no history of hypertension or heart failure |
|
Other common illnesses |
Treat as indicated |
During the first weeks to months of adaptation to the ketogenic diet, the most common side effects are constipation and muscle cramps. Many people have fewer bowel movements and confuse this with constipation. Constipation, meaning hard or hard-to-pass stools, usually resolves by increasing fluid intake to a minimum of 2 L per day. Other remedies for constipation include 1 teaspoon of milk of magnesia at bedtime for one week, bouillon supplementation, or a sugar-free fiber supplement. Occasionally, patients may complain of diarrhea, which may be related to metformin or using too many sugar substitutes. Muscle cramps typically resolve with supplementation of 1 teaspoon of milk of magnesia at bedtime for one week or 200 mEq per day of slow-release magnesium chloride daily.
Conclusion
Since obesity is recognized as a disease, primary care providers will play an important role in the identification and treatment of obesity. If primary care providers are not having success with obesity treatment, then referral to an obesity medicine specialist may be a good option to improve patient outcomes. Although many nutritional approaches are effective, there is a growing consensus that dietary approaches be tailored to individual patients. The low-carbohydrate, ketogenic diet appears to be particularly effective in individuals with insulin resistance, and considering the large prevalence of insulin resistance, it may provide an important tool for the primary care provider.
REFERENCES
- Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of obesity among adults and youth: United States, 2015–2016. NCHS data brief, no 288. Hyattsville, MD: National Center for Health Statistics; 2017.
- National Institutes of Health; National Heart, Lung, and Blood Institute. Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults—The evidence report. Obes Res 1998;6(Suppl 2):51S–209S.
- Obesity Medicine Association and Obesity Algorithm. Available at: http://www.obesitymedicine.org. Accessed July 9, 2018.
- Pollack A. A.M.A. recognizes obesity as a disease. June 18, 2013. The New York Times. Available at: http://www.nytimes.com/2013/06/19/business/ama-recognizes-obesity-as-a-disease.html. Accessed July 9, 2018.
- Obesity Medicine Association. Available at: http://www.obesitymedicine.org/. Accessed July 9, 2018.
- American Board of Obesity Medicine. Available at: http://www.abom.org/. Accessed July 9, 2018.
- Steelman GM, Westman EC, eds. Obesity: Evaluation & Treatment Essentials. 2nd ed. Boca Raton, FL: CRC Press; 2016.
- Obesity Action Coalition. Available at: http://www.obesityaction.org/. Accessed July 9, 2018.
- Ludwig DS, Ebbeling CB. The carbohydrate-insulin model of obesity: Beyond ‘calories in, calories out.’ JAMA Intern Med 2018;178:1098-1103.
- Grundy SM, Cleeman JI, Daniels SR, et al; American Heart Association; National Heart, Lung, and Blood Institute. Diagnosis and management of the metabolic syndrome: An American Heart Association/National Heart, Lung, and Blood Institute scientific statement. Circulation 2005;112:2735-2752.
- Bays HE, González-Campoy JM, Henry RR, et al; Adiposopathy Working Group. Is adiposopathy (sick fat) an endocrine disease? Int J Clin Pract 2008;62:1474-1483.
- Bays H. Central obesity as a clinical marker of adiposopathy; increased visceral adiposity as a surrogate marker for global fat dysfunction. Curr Opin Endocrinol Diabetes Obes 2014;21:345-351.
- Tchernof A, Després JP. Pathophysiology of human visceral obesity: An update. Physiol Rev 2013;93:359-404.
- Bays HE, González-Campoy JM, Bray GA, et al. Pathogenic potential of adipose tissue and metabolic consequences of adipocyte hypertrophy and increased visceral adiposity. Expert Rev Cardiovasc Ther 2008;6:343-368.
- Volek JS, Sharman MJ, Gómez AL, et al. Comparison of energy-restricted very low-carbohydrate and low-fat diets on weight loss and body composition in overweight men and women. Nutr Metab (Lond) 2004;1:13.
- Gepner Y, Shelef I, Schwarzfuchs D, et al. Effect of distinct lifestyle interventions on mobilization of fat storage pools: The CENTRAL MRI randomized controlled trial. Circulation 2018;137:1143-1157.
- Banting W. Letter on Corpulence, Addressed to the Public. 1863. London: Harrison.
- Yudkin J. The causes and cure of obesity. Lancet 1959;274:1135-1138.
- Siri-Tarino PW, Sun Q, Hu FB, Krauss RM. Meta-analysis of prospective cohort studies evaluating the association of saturated fat with cardiovascular disease. Am J Clin Nutr 2010;91:535-546.
- Chowdhury R, Warnakula S, Kunutsor S, et. al. Association of dietary, circulating, and supplement fatty acids with coronary risk: A systematic review and meta-analysis. Ann Intern Med 2014;160:398-406.
- Taubes G. Good Calories, Bad Calories: Challenging the Conventional Wisdom on Diet, Weight Control, and Disease. New York: Alfred A. Knopf; 2007.
- Teicholz N. The Big Fat Surprise. Why Butter, Meat and Cheese Belong in a Healthy Diet. New York: Simon & Schuster; 2014.
- Boden G, Sargrad K, Homko C, et al. Effect of a low-carbohydrate diet on appetite, blood glucose levels, and insulin resistance in obese patients with type 2 diabetes. Ann Intern Med 2005;142:403-411.
- Mansoor N, Vinknes KJ, Veierod MB, Retterstol K. Effects of low-carbohydrate diets v. low-fat diets on body weight and cardiovascular risk factors: A meta-analysis of randomised controlled trials. Brit J Nutr 2016;115:466-479.
- Hu T, Mills KT, Yao L, et al. Effects of low-carbohydrate diets versus low-fat diets on metabolic risk factors: A meta-analysis of randomized controlled clinical trials. Am J Epidemiol 2012;176(Suppl 7):S44-54.
- Santos FL, Esteves SS, da Costa Pereira A, et al. Systematic review and meta-analysis of clinical trials of the effects of low carbohydrate diets on cardiovascular risk factors. Obes Rev 2012;13:1048-1066.
- Gardner CD, Trepanowski JF, Del Gobbo LC, et al. Effect of low-fat vs low-carbohydrate diet on 12-month weight loss in overweight adults and the association with genotype pattern or insulin secretion: The DIETFITS randomized clinical trial. JAMA 2018;319:667-679.
- Shai I, Schwarzfuchs D, Henkin Y, et al. Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. N Engl J Med 2008;359:229-241.
- Volek JS, Feinman RD. Carbohydrate restriction improves the features of metabolic syndrome. Metabolic syndrome may be defined by the response to carbohydrate restriction. Nutr Metab (Lond) 2005;2:31.
- Westman EC, Yancy WS, Edman JS, et al. Effect of 6-month adherence to a very low carbohydrate diet program. Am J Med 2002;113:30-36.
- Westman EC, Phinney SD, Volek JS. The New Atkins for a New You: The Ultimate Diet for Shedding Weight and Feeling Great. New York: Simon & Schuster; 2010.
- Volek J, Phinney S. The Art and Science of Low Carbohydrate Living: An Expert Guide to Making the Life-Saving Benefits of Carbohydrate Restriction Sustainable and Enjoyable. Beyond Obesity LLC; 2011.
- Volek J, Phinney S. The Art and Science of Low Carbohydrate Performance. Beyond Obesity LLC; 2012.
- Yancy WS Jr, Westman EC, McDuffie JR, et al. A randomized trial of a low-carbohydrate diet vs orlistat plus a low-fat diet for weight loss. Arch Intern Med 2010;170:136-145.
- McDonald TJW, Henry-Barron BJ, Felton EA, et al. Improving compliance in adults with epilepsy on a modified Atkins diet: A randomized trial. Seizure 2018;60:132-138.
- Austin GL, Thiny MT, Westman EC, et al. A very low carbohydrate diet improves gastroesophageal reflux and its symptoms: A pilot study. Dig Dis Sci 2006;51:1307-1312.
- Austin GL, Dalton CB, Hu Y, et al. A very-low-carbohydrate diet improves symptoms and quality of life in diarrhea-predominant irritable bowel syndrome. Clin Gastroenterol Hepatol 2009;7:706-708.e1.
- Mavropoulos J, Yancy WS, Hepburn J, Westman EC. The effects of a low-carbohydrate, ketogenic diet on the polycystic ovary syndrome: A pilot study. Nutr Metab (Lond) 2005;2:35.
Overweight and obesity have reached epidemic proportions in the United States. For individuals affected by obesity, clinical studies have shown that carbohydrate restriction, including a low-carbohydrate, ketogenic diet, can be a safe and effective treatment. This article includes a narrative review of clinical research studies and a practical description of implementing a “keto” diet for obesity.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.