Ocular Trauma
November 1, 2018
Reprints
AUTHORS
Lauren Wendell, MD, MS, Department of Emergency Medicine, Maine Medical Center, Portland, ME
Christopher Allison, MD, Emergency Medicine Resident, Maine Medical Center, Portland, ME
PEER REVIEWER
Steven Winograd, MD, FACEP, Attending Physician, Mt. Sinai Queens Hospital Center, Assistant Clinical Professor of Emergency Medicine, Mt. Sinai Medical School, Jamaica Queens, NY
EXECUTIVE SUMMARY
- Atraumatic periorbital ecchymosis has been reported to be caused by sneezing, but caution should be exercised before attributing this to trivial occult trauma, given that it can be a presenting sign of malignancy (e.g., neuroblastoma in children), clotting dysfunction, or systemic disorders such as multiple myeloma.
- Features that define a complex lid laceration include involvement of lid margins, levator muscle or tendon, canthal tendons, tissue loss, penetration of the orbital septum, or location medial to the punctae. Any fat visible in the wound signifies orbital septum laceration, given that there is no subcutaneous fat in the eyelids. These injuries have a high incidence of globe penetration and intraorbital foreign bodies.
- The inferior wall, also known as the orbital floor, is weakest and is the most common site of fracture, leading to communication between the maxillary sinus and the orbit.
- Orbital compartment syndrome is diagnosed most appropriately clinically prior to imaging. Clinical findings include vision loss, proptosis, limited extraocular movement, and elevated intraocular pressure.
- A corneal ulcer appears as a white patch visible without fluorescein staining, sometimes only on slit-lamp examination. The majority of corneal ulcers are bacterial, although fungal and herpes infections occur. The most important risk factor is contact lens use. A culture of the ulcer and ophthalmologic consultation are recommended prior to initiation of treatment.
- Research regarding treatment for corneal abrasions is ongoing. Currently, no ophthalmological organization has endorsed prescribing home local anesthetic for corneal abrasions, and it is not the standard of care.
- The most important concept regarding chemical exposures is that treatment must be instituted immediately, even before vision testing. Beginning at the site of injury, irrigation using running tap water for at least 30 minutes before transport has been shown to improve outcomes.
- Iritis usually presents with findings that include “ciliary flush” (conjunctivitis focused around the limbus), a poorly reactive pupil, and photophobia. Pain in the affected eye when light is shone into the unaffected eye is termed consensual photophobia, which demonstrates pain is originating from the iris contraction and is consistent with uveitis. Slit-lamp exam may show cells and flare in the anterior chamber as is seen in nontraumatic uveitis.
- Conditions that create connective tissue weakness, including Marfan syndrome, homocysteinuria, and tertiary syphilis, predispose to lens subluxation.
In 2016, approximately 131,000 eye injuries constituted 4.8% of work-related injuries in the United States.1 Approximately 3% of emergency department (ED) visits are for eye trauma complaints.2 Appropriate diagnosis, workup, symptomatic care, and potentially vision-saving interventions rely on knowledge of eye anatomy and predicted injury patterns. The first step of evaluation must include screening for potential life-threatening injuries. Patients with trauma to the face and neck should have a proper primary and secondary trauma survey to exclude any imminently harmful injuries. Then it is safe to proceed to a careful evaluation of the eye and surrounding structures.
The comprehensive physical exam of the eye includes multiple aspects: visual acuity, visual fields, eyelid eversion, extraocular movements, pupil examination and reactivity, slit lamp examination of cornea and anterior chamber, fluorescein staining, intraocular pressure, and fundoscopy. Individual components of the exam are either mandatory or contraindicated depending on the presenting case, as will be discussed. However, the importance of assessing and documenting visual acuity cannot be overemphasized.
This review includes both can’t-miss and common traumatic injuries to the eye. After completing this review, the practitioner should be more comfortable evaluating and treating a patient with a traumatic eye complaint and understanding when to involve ophthalmology and with what urgency.
Periorbital Contusion
Familiar to laypersons as a “black eye,” a contusion to the orbit and nearby tissue results in ecchymosis and variable degrees of swelling. Although periorbital contusion generally is a self-limited condition, its presence is correlated with facial fractures,3 basilar skull fractures,4 orbital wall fractures,5 and other injuries.
Further, eyelid swelling can limit visual acuity assessment and examination of the eye for more serious injuries, such as globe rupture. After evaluating for and stabilizing life-threatening injuries, prompt examination of the eye prior to maximum swelling may allow for better assessment. When available, Desmarres retractors facilitate examination while minimizing pressure on the globe.
Care should be taken to avoid confusing periorbital ecchymosis caused by direct trauma to capillaries with “raccoon eyes” caused by blood from a basilar skull fracture tracking along tissue planes.6 Atraumatic periorbital ecchymosis has been reported to be caused by sneezing,7 but caution should be exercised before attributing this to trivial occult trauma, given that it can be a presenting sign of malignancy (e.g., neuroblastoma in children8), clotting dysfunction, or systemic disorders such as multiple myeloma.9
As with other soft tissue contusions, treatment is supportive with head elevation and cold compresses. The patient should be given instructions to seek follow-up care if he or she develops symptoms suggestive of injury not obvious on initial presentation (such as decreased vision, flashing or floaters, or diplopia) or symptoms suggestive of infection (such as increased pain, swelling, or fever).
Eyelid Lacerations
A patient with an eyelid laceration first must undergo evaluation for a laceration to deeper structures. The wound should be evaluated for foreign bodies. Many eyelid lacerations are complex and require referral to ophthalmology or plastic surgery for repair to minimize the risk of missed deeper injuries and for precise repair that optimizes functional and cosmetic outcomes. Features that define a complex laceration include involvement of lid margins, levator muscle or tendon, canthal tendons, tissue loss, penetration of the orbital septum, or location medial to the punctae.10 (See Figure 1.) Any fat visible in the wound signifies orbital septum laceration, given that there is no subcutaneous fat in the eyelids, and these injuries have a high incidence of globe penetration and intraorbital foreign bodies.11
Figure 1. Lower Lid Laceration |
|
Lower lid laceration with canaliculus involvement as a result of a dog bite.
|
|
Image used with permission from: Jessica S. Watson, MD. |
Canalicular involvement should be suspected in lacerations medial to the punctae.12 If there is doubt regarding canalicular involvement, fluorescein instilled in the eye may appear in the wound.13 Scarring and stenosis after unrecognized canalicular injuries can result in epiphora, in which inadequately drained tears continuously overflow onto the cheek.
Simple, superficial lacerations involving less than 25% of the lid heal well by secondary intention and, thus, do not require repair.14 If indicated, emergency physicians may repair simple lacerations with 6-0 to 7-0 interrupted sutures. Absorbable sutures, including fast-absorbing plain gut, have been used with acceptable outcomes15,16 and are convenient for patients. Nonabsorbable nylon or polypropylene sutures are removed in three to five days.10 Suture ends should be trimmed short or buried, if possible, to avoid contact with the cornea.
Orbital Wall Fractures
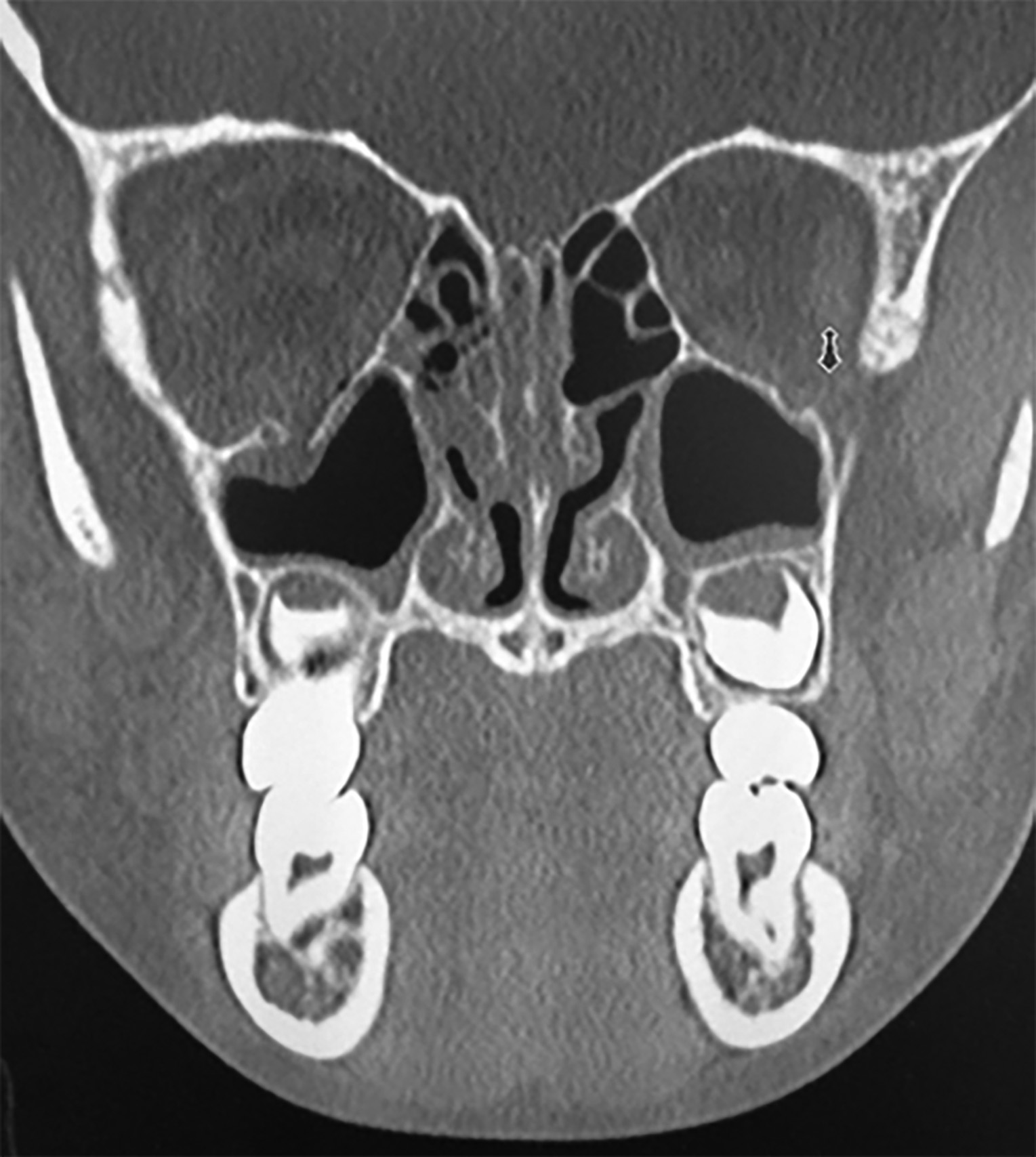
Trauma to the globe and orbit most commonly occurs from falls, interpersonal violence, sports, and motor vehicle collisions. The trauma can result in fracture of one or more walls of the orbit, which often is termed a “blowout fracture.”17 There is debate regarding whether pressure directly on the globe is redirected into the orbital wall resulting in fracture in most cases, or if compressive forces on the orbital rim cause these fractures.17 Regardless of the exact mechanism, the two most common sites are the medial and inferior wall. The inferior wall, also known as the orbital floor, is weakest and is the most common site of fracture, leading to communication between the maxillary sinus and the orbit. (See Figure 2.) This communication causes orbital emphysema or air within the orbit. The maxillary (V2) branch of the trigeminal nerve traverses the orbital floor and can be injured, resulting in hypoesthesia in a V2 distribution (i.e., the ipsilateral cheek and upper lip). Herniation of orbital tissue, with or without the muscle itself, entraps movement of the inferior rectus muscle, limiting upward gaze.
The second most common site of orbital blowout fracture is the medial wall, composed of the aptly named lamina papyracea (paper layer) of the ethmoid bone. Fracture will cause communication with ethmoid air cells and orbital emphysema. Analogously to inferior rectus entrapment, medial wall fracture can entrap the medial rectus muscle and cause diplopia.
Figure 2. Orbital Floor Fracture |
|
Orbital floor fracture with fat herniation on CT scan.
|
|
Image used with permission from: Jessica S. Watson, MD. |
Orbital emphysema is an almost universally benign condition that self-resolves, with only rare cases of increased intraorbital pressure nerve compression leading to vision loss.18 Nonetheless, avoiding Valsalva and nose blowing helps limit orbital emphysema.
Plain films of the orbits have poor sensitivity for orbital fractures, with reported rates of 64-78% as compared with computed tomography (CT),19,20 and are not recommended. CT imaging with coronal reconstruction is the test of choice.21,22
If the fracture involves an infected sinus, there is a clear indication for antibiotics with sinus flora coverage, such as amoxicillin-clavulanate for 10 days, accompanied by an oral decongestant. Currently, the evidence regarding routine prophylactic antibiotics after isolated orbital wall fracture to prevent orbital cellulitis is inadequate to assess efficacy or safety.23,24
In many cases of entrapment, restricted eye movement results from herniation through the fracture of edematous soft tissue other than the extraocular muscle itself. Head elevation and cold compresses for 48 hours after injury help reduce this swelling with minimal risk. In a single, small, double-blind, randomized, controlled trial (n = 38), corticosteroids were shown to speed the resolution of diplopia, obviating the need for surgery in some cases and decreasing time to resolution of diplopia postoperatively.25
Blindness is rare and is reported at a rate of one in 1,500 cases.26 The major complications of orbital wall fractures are diplopia and enophthalmos. Enophthalmos is the abnormal retraction of the globe within the orbit, which can decrease field of vision and has adverse cosmetic effects. Operative interventions may be utilized to correct these deficits if performed after swelling from the initial injury has decreased. The indications for surgery and its optimal timing are debated. In the United States, the general consensus is that early surgery (within one to three weeks) is performed for persistent diplopia, enophthalmos > 2-3 mm, or substantial tissue herniation into the maxillary sinus.17
In summary, orbital wall fractures should be diagnosed primarily with CT and should be treated with ice and head elevation for 48 hours. The patient should avoid nose-blowing. Consider steroids and antibiotics. Refer the patient to ophthalmology/plastic surgery for evaluation and possible consideration of surgery in one to three weeks.
Retrobulbar Hematoma
Trauma to the globe and orbit can result in hemorrhage within the orbit, leading to retrobulbar hematoma (i.e., hematoma behind the globe). This can lead to orbital compartment syndrome, in which increased pressure within the confines of the orbit leads to decreased perfusion of the retina and optic nerve, with the potential for permanent vision loss.
In a review of 1,386 patients with eye trauma at a single U.S. Level I trauma center, researchers found a 3.4% incidence of retrobulbar hematoma, 54% of whom underwent lateral canthotomy.27
Retrobulbar hematoma is seen on CT imaging. However, orbital compartment syndrome is diagnosed most appropriately clinically prior to imaging. Clinical findings include vision loss, proptosis, limited extraocular movement, and elevated intraocular pressure (IOP).10 Normal IOP is 10-20 mmHg. Recommendations vary for an IOP threshold at which to perform immediate decompression: IOP within 20 mmHg of mean arterial pressure,28 IOP greater than 40 mmHg,29,30 or IOP greater than 30 mmHg.31 A reasonable approach would be to have a lower threshold for lateral canthotomy and cantholysis in which the condition of the patient precludes assessment of visual acuity.
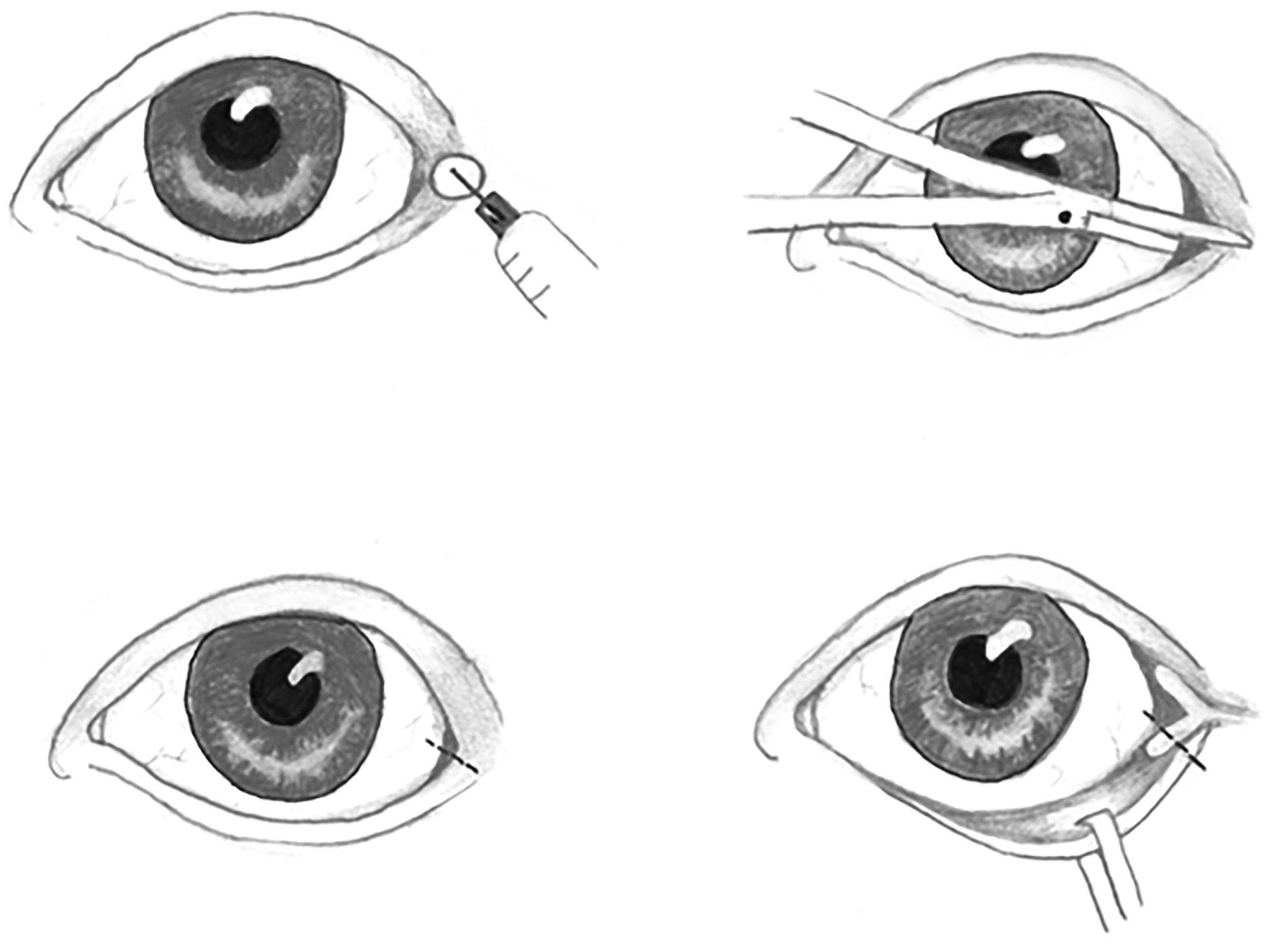
Orbital compartment syndrome mandates emergent decompression. Animal models have shown tolerance of retinal ischemia up to approximately 100 minutes, but irreversible damage after 100-240 minutes.32,33 For this reason, decompression is recommended within 100-120 minutes of symptom onset.34,35 Emergency physicians achieve decompression via bedside lateral canthotomy and cantholysis (see Figure 3), a simple and potentially vision-saving procedure.28,29,36
Figure 3. Lateral Canthotomy |
|
Illustration of the steps of a lateral canthotomy. Step 1: Anesthetize the tissue overlying the lateral canthus. Step 2: Clamp and then snip the lateral canthus full thickness. Step 3: Note landmarks of the inferior crus. Step 4: Grasp the lateral lower eyelid with toothed forceps. Pull the lower eyelid anteriorly. Strum the lateral tendon and cut.
|
|
Illustration by Marguerite Adolf. |
In cases of only mild elevation in IOP, or when additional pressure reduction after decompression is required, medications to reduce IOP are indicated, for example, a carbonic anhydrase inhibitor such as acetazolamide, a topical beta-blocker such as timolol, and 1 to 2 grams per kilogram of intravenous (IV) mannitol.10 Obtain ophthalmology consultation in all cases for definitive decompression.
Corneal Foreign Body/Abrasion
Patients with corneal abrasion may present with a foreign body sensation, pain, and photophobia. Decreased visual acuity may be present if the abrasion involves the visual axis. If a diagnostic dilemma exists, significant relief from topical local anesthetic is consistent with a superficial pathological process.37
Diagnosis is made using a Wood’s lamp and visualizing abnormal epithelial fluorescein uptake. (See Figure 4.) Flow of aqueous humor from the defect (Seidel’s sign) suggests a corneal perforation or potentially a globe rupture. Care should be taken not to misdiagnose a corneal ulcer as a corneal abrasion. A corneal ulcer appears as a white patch visible without fluorescein staining, sometimes only on slit-lamp examination. The majority of corneal ulcers are bacterial, but fungal and herpes infections also occur. The most important risk factor is contact lens use. A culture of the ulcer and ophthalmologic consultation are recommended prior to initiation of treatment.10
Figure 4. Corneal Abrasion |
|
Corneal abrasion with fluorescein staining over visual axis.
|
|
Image used with permission from: Jessica S. Watson, MD. |
Treatment of corneal abrasions includes topical antibiotics, generally erythromycin ointment. Contact lens wearers require Pseudomonas coverage with tobramycin or moxifloxacin 0.5%, one to two drops every four hours.38 Pain control may be achieved with cycloplegics (contraindicated in glaucoma), and there is evidence for significant relief with topical non-steroidal anti-inflammatory drugs (NSAIDs), such as ketorolac 0.5% or diclofenac 0.1% four times daily.39 Multiple Cochrane reviews have concluded that eye patching for corneal abrasion does not improve healing rates or pain and should not be recommended routinely.40,41
Historically, topical anesthetics such as tetracaine or proparacaine have been considered contraindicated for the home treatment of corneal abrasions42,43 because of concerns that the anesthetic may impair healing, have direct toxicity, and/or mask more serious conditions. This idea has been challenged by physicians who cite small trials showing efficacy without adverse events and a track record of safety when used for photorefractive keratectomy (which creates an epithelial defect similar to a corneal abrasion).44
Waldman et al recently published a non-randomized observational adult study in which tetracaine 1% up to every 30 minutes for 24 hours was prescribed for “simple corneal abrasions.” These included abrasions that occurred within 48 hours of evaluation and were due to a simple traumatic cause without contamination, not from chemicals, contact lens use, thermal burns, or infection, and not requiring immediate ophthalmologic evaluation. No adverse events were seen in the 303 simple corneal abrasions treated; however, 151 patients with non-simple corneal abrasions were prescribed tetracaine inappropriately, several of whom had serious conditions (e.g., herpes keratitis, anterior uveitis).45 Persistent pain typically is the symptom that drives patients with more serious conditions to follow up with ophthalmology. Masking that pain poses a real risk of adverse outcomes from delayed diagnosis. Research in this area is ongoing. Currently, no ophthalmological organization has endorsed prescribing home local anesthetic for corneal abrasions, and it is not the standard of care.
Corneal abrasions heal quickly and are characterized by rapid improvement in symptoms. If symptoms do not improve or if they worsen after 24 hours, patients should be instructed to obtain urgent ophthalmology evaluation.
Corneal Foreign Body
Corneal foreign bodies most frequently occur from accidents involving small fragments of metal. Prevention involves use of appropriate protective eyewear during risky activities.
Evaluation includes assurance that corneal perforation, and thus the potential for globe rupture, is not present. This is performed with fluorescein staining. A flow of aqueous humor from the anterior chamber seen on fluorescein exam (Seidel’s sign) signifies corneal perforation.
Small, superficial corneal bodies that cannot be removed with a moistened cotton swab often are removed easily at the bedside of a cooperative patient with the use of a topical anesthetic and a small needle or ophthalmic burr device.46 The patient’s face should be resting forward in contact with a slit lamp, and the provider’s hand should be braced against the frame of the slit lamp and the patient’s face. A syringe attached to the needle may make the procedure easier. Metallic foreign bodies often will leave a rust ring after removal. Rust rings become more superficial 24 hours after foreign body removal, making them easier to remove with ophthalmic burr at an ophthalmology office visit.
Standard treatment includes topical antibiotic ointment, although as with corneal abrasion, the necessity is not well established with existing data. Tetanus immunization status also should be addressed.
Photokeratitis
Photokeratitis or ultraviolet keratitis, commonly known as “welder’s keratitis,” is a painful condition caused by exposure to either natural ultraviolet (UV) or artificial rays, which are absorbed in the corneal epithelium causing desquamation. Most commonly known causes are welder’s arc burns and “snow-blindness.” The exposure may not be known to the patient, as there typically is a latent period of six to 12 hours before symptoms start.47 Symptoms include bilateral eye pain, burning, foreign body sensation, photophobia, excessive tearing, and the inability to open eyes. Often, the patient will be pacing or showing signs of distress. Although the condition is excruciatingly painful, most often it is self-limiting, with complete resolution in 48-72 hours.47
A careful history often will lead to the diagnosis based on antecedent exposure. Patients also may have signs of facial and eyelid erythema. Visual acuity often is preserved or only mildly decreased, but frequently requires topical anesthetic to obtain an assessment. There will be tearing and injection with possible chemosis of the conjunctiva; however, the tarsal conjunctiva should be spared. There is diffuse punctate uptake of fluorescein when instilled. Otherwise, the exam is unremarkable.
Because photokeratitis is a self-limiting process, symptomatic treatment is the mainstay of therapy. There are no clinical trial data on the efficacy or validity of these treatments. Symptomatic treatments include lubricating therapy, such as erythromycin ointment three to four times per day for three days, to prevent corneal infection. Oral pain regimens are up to the prescribing provider. Topical cycloplegics, such as cyclopentolate (0.5%-2%, 1-2 drops) and homatropine (2-5%, 1-2 drops every four hours), may be prescribed to limit pain associated with pupillary changes.47 Again, home topical anesthetics have not been supported by any ophthalmological society and are not considered the standard of care.
Outpatient ophthalmology follow-up is recommended. Symptoms should resolve in two to three days. There often are no long-term sequelae unless there is chronic exposure. Prevention with proper eye protection should be emphasized.
Chemical Burns
Chemical exposures to the eye make up 12-22% of ocular injuries.48 These injuries can be devastating, and the best outcome depends on early and aggressive irrigation. Strong alkaline chemicals, which are common in household and industrial cleaning products, tend to cause deeper burns, as the liquefactive necrosis produced allows penetration deeper into tissues. In contrast, strong acids cause coagulative necrosis, often limiting damage to more superficial layers. Examples of exposures that can cause significant chemical injury include lye, cements, plasters, airbag powder, ammonia, battery acid, pool cleaner, vinegar, solvents, detergents, and mace.49
The most important concept regarding chemical exposures is that treatment must be instituted immediately, even before vision testing. Beginning at the site of injury, irrigation using running tap water for at least 30 minutes before transport has been shown to improve outcomes.50,51 The hypo-osmolarity of water used for irrigation may cause corneal edema, which may be beneficial by increasing the distance chemicals must diffuse before reaching deeper structures.52 Particulate matter, if present, is removed from the eye with a moist cotton swab. Use of a contact lens irrigation device, such as Morgan Lens, allows for continuous irrigation without a provider present, which can be facilitated by a topical anesthetic.
Although multiple options are available, the choice of irrigation solution is less important than the promptness and thoroughness of irrigation.53 Normal saline and lactated Ringer’s commonly are used because of their widespread availability. There is evidence that the borate-based buffer solution Cederroth Eye Wash solution and the amphoteric polyvalent buffer Diphoterine are more effective than water or isotonic saline for normalizing eye pH after chemical exposure.51
During irrigation, the ocular surface pH should be tested about every 20 minutes with litmus paper until the pH has normalized. Consultation with ophthalmology should be obtained in all cases. Preservative-free artificial tears are the mainstay of chemical burn treatment and are believed to promote epithelialization and speed visual recovery.48 Depending on the case, the ophthalmologist may employ adjunctive therapies, including steroids, antibiotics, citrate, growth factor supplementation from a variety of biological sources, and/or surgery.
Traumatic Hyphema
Trauma to the eye can cause bleeding within the anterior chamber. The characteristic layering of blood in the anterior chamber is termed hyphema. Photophobia usually is present. If large enough, an afferent pupillary defect may occur.
The most serious complication is acute glaucoma, which can occur when clotted blood impairs outflow of aqueous humor from the anterior chamber. This presents with pain, vision loss, and increased intraocular pressure. Initial treatment includes medications to decrease aqueous humor production: topical beta-blocker (timolol), topical alpha-agonist (brimonidine or apraclonidine), and IV carbonic anhydrase inhibitor (acetazolamide). IV mannitol is used in severe cases.10
Special consideration is given to patients with sickle cell disease. The anterior chamber is relatively hypoxic and acidic, which promotes sickling and subsequent obstruction of aqueous humor outflow. Acetazolamide is avoided because of its association with increased sickling. Topical timolol is the starting treatment, with other agents given in consultation with ophthalmology.10
The most common complication is rebleeding, reported at rates of 6-33%,54,55 and it occurs most commonly on days 2 to 5.10 For this reason, antiplatelet agents should be avoided.
The data for optimal initial treatment are limited. Traditional practices included bed rest, head elevation to 30-45 degrees, and an eye shield; however, the authors of a Cochrane review of studies evaluating these practices concluded that sample sizes are too small to evaluate efficacy.56 The authors of this same Cochrane review concluded that current evidence suggests antifibrinolytics, such as aminocaproic acid and tranexamic acid, reduce rates of rebleeding. However, there are insufficient data on the important outcomes of corneal staining and vision loss or on safety.56 It has been hypothesized that long-term visual loss usually is related to concurrent eye trauma and not the hyphema per se,57 offering an explanation as to why larger hyphema and rebleeding are associated with vision loss as a marker of more severe trauma, yet treatments that reduce rebleeding have not reduced vision loss consistently.
Admission is recommended for patients with hyphema > 50%, vision loss, or increased IOP, and for all patients with sickle cell disease.10 Less acutely impaired drainage of aqueous humor, corneal blood staining, and impaired accommodation affecting near vision are longer-term complications for which patients may follow up with an ophthalmologist.57
Traumatic Uveitis
Trauma to structures of the anterior chamber, including the iris, ciliary body, and choroid (i.e., the uvea), can provoke pain and inflammation variably termed uveitis, iritis, and iridocyclitis. Exam findings include “ciliary flush” (conjunctivitis focused around the limbus), a poorly reactive pupil, and photophobia. Pain in the affected eye when light is shone into the unaffected eye is termed consensual photophobia, which demonstrates pain is originating from the iris contraction and is consistent with uveitis. Slit-lamp exam may show cells and flare in the anterior chamber as is seen in nontraumatic uveitis.58
The mainstay of treatment is pain control achieved by a drug that paralyzes the iris (i.e., a cycloplegic). Homatropine hydrobromide 5% can be prescribed for use four to five times daily for seven to 10 days. Symptoms typically improve within one week. Ophthalmologists may use a short course of topical steroid if inflammation does not resolve in this timeframe.58
Temporary miosis or mydriasis may persist for several days after blunt trauma to the iris. More severe injuries may cause permanent damage to the pupillary sphincter muscles, resulting in an irregular pupil border or permanent mydriasis. Shearing of the outer edges of the iris from the ciliary body is known as iridodialysis and may result in a hole through which light can enter the globe, sometimes termed a “secondary pupil.” Iridodialysis can cause monocular diplopia and requires ophthalmology consultation.58
Traumatic uveitis generally has very good visual outcomes but may require long-term ophthalmology care for subsequent glaucoma and cataracts.58
Lens Subluxation and Dislocation
Blunt trauma may partially or completely disrupt the zonules that hold the crystalline lens in place, resulting in lens subluxation or dislocation, respectively. Lens subluxation will result in distorted vision or monocular diplopia, whereas complete dislocation will cause profound blurring of vision in the affected eye.
Conditions that create connective tissue weakness, including Marfan syndrome, homocysteinuria, and tertiary syphilis, predispose to lens subluxation. Patients with these conditions may present with lens subluxation or dislocation after minimal trauma.
As with other conditions affecting the anterior and posterior chamber, secondary glaucoma may occur, and IOP should be monitored.59
Subluxation is diagnosed by visualization of a lens edge within the pupil, facilitated by eye dilation. If there is doubt, orbital CT can reveal the diagnosis. However, provider-performed ocular ultrasound is likely to show the diagnosis, with a single observational study on traumatic eye injury patients showing sensitivity of 85% and specificity of 98% compared to orbital CT.60 Ocular ultrasound is contraindicated in suspected globe rupture, given the risk of pressure on the globe.
Immediate ophthalmology consultation is indicated for consideration of surgical management or observation.
Traumatic Vitreous Hemorrhage
Bleeding into the vitreous humor may occur spontaneously or because of trauma. Hemorrhage can be from anterior uveal structures or from the retina.
Presenting symptoms include reduced visual acuity and the presence of floaters. Floaters are darkened spots within the patient’s vision that move with head and eye movement. In this case, they are caused by hemorrhage and clots blocking the path of light to the retina.
The fundus will be difficult to visualize on fundoscopy. Bedside ultrasound has been shown to be useful for this diagnosis and will reveal hyperechoic, mobile material within the vitreous humor that swirls with eye movement.61
Treatment consists of avoiding Valsalva and allowing blood to settle by keeping the head elevated. Antiplatelets and anticoagulants should be avoided and/or reversed if the benefit outweighs the risk.
Ophthalmology should be consulted for traumatic vitreous hemorrhage, particularly given the risk for concurrent retinal injury. Vitrectomy may be performed in some cases.
Retinal Injuries
Trauma can result in retinal tears allowing a separation of the retina from the retinal pigment epithelium on which it lies. This is a relatively rare diagnosis, with a reported incidence of approximately 0.6-2 per 100,000 people.62 Trauma is responsible for about 6-19% of retinal detachments.63 Retinal tears occur immediately after trauma; however, the slow or delayed flow of viscous vitreous humor through the defect can result in retinal detachment months to years after the initial injury, with a reported average interval of five years after blunt trauma.63
Symptoms include floaters from vitreous bleeding, flashing lights from abnormal stimulation of retinal neurons, and visual field cuts. Whether visual field acuity is decreased depends on whether the detachment involves the macula. Indeed, macular involvement at the time of diagnosis is the most important prognostic factor, with a good outcome (defined by long-term visual acuity of at least 20/40) occurring in 42% without macular involvement and in 28% with macular involvement.64
On fundoscopy, a detached retina appears as crinkled, billowing tissue at the margins. Indirect ophthalmoscopy and eye dilation provide increased sensitivity. Provider-performed ultrasound has been shown to be a useful tool, with two studies showing sensitivity of 97-100% and specificity of 83-92% compared to the final diagnosis made by an ophthalmologist.65,66 False-positive ultrasound results from vitreous hemorrhage were most common.
Patients with suspected retinal detachment require immediate ophthalmologic evaluation for consideration of various interventions, including photocoagulation and/or surgery to tack down the retina and prevent further detachment. Given the potential for delayed retinal detachment, patients discharged after any eye trauma are counseled to return if they develop visual symptoms.
Ruptured Globe
Globe rupture, also known as scleral rupture, is among the most severe traumatic injuries to the eye and can be caused by penetrating and blunt trauma. It is one of the most common causes of monocular blindness, with a global incidence of 3.5 per 100,000.67
The most common sites of rupture are at the limbus (i.e., the junction of the cornea and the sclera) and at the insertion sites of intraocular muscles. Pain and decreased vision are common. Coincident vitreous hemorrhage and retinal detachment are frequent. Rupture at the limbus may be obvious, manifesting as a laceration or as herniation of the iris and other components of the uvea through the defect, resulting in a teardrop-shaped iris. The diagnosis is more difficult if the injury results in significant conjunctival hemorrhage, termed bloody chemosis; suspicion for globe rupture should be high in these cases.68 A full-thickness corneal laceration can be identified on fluorescein exam by the flow of aqueous humor out of the anterior chamber, known as Seidel’s sign, and should be treated like a globe rupture. Measurement of intraocular pressure is contraindicated in cases of obvious globe rupture.68
The diagnosis of “occult globe rupture,” often posteriorly at extraocular muscle insertion sites, requires special consideration. A missed occult rupture could be worsened by a sudden increase in IOP, such as from sneezing or coughing, mandating prompt diagnosis. Deepening of the anterior chamber after trauma is nearly pathognomonic.69 Assessment of anterior chamber depth requires expertise with a slit lamp that is unlikely for emergency medicine providers, but the assessment also can be performed with CT.70 The specificity of bloody chemosis for globe rupture is unknown, but it should increase suspicion if present.68 Orbital CT has a reported sensitivity of 75-76% and a specificity of 85-94% compared to final ophthalmologist diagnosis,71,72 making CT useful but inadequate to exclude this diagnosis. (See Figure 5.)
Figure 5. Globe Rupture Demonstrated on Computed Tomography |
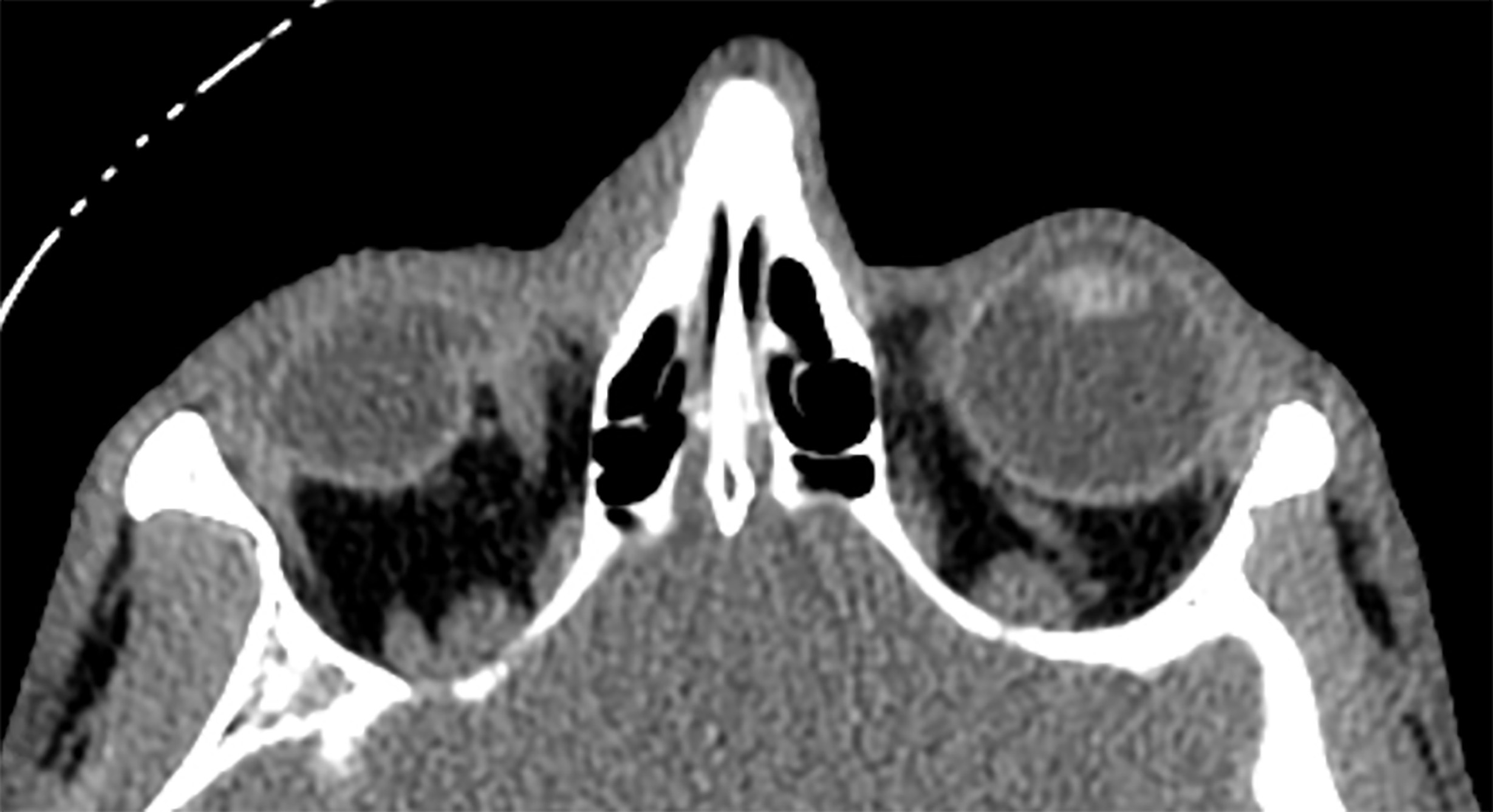 |
If occult globe rupture is suspected despite negative CT, it is acceptable, in consultation with an ophthalmologist, to measure IOP gently. IOP usually is slightly lower (about 2 mmHg) in the affected eye than the contralateral eye, but the pressure may be normal.68 Very low pressure is pathognomonic. Ultrasonography usually is contraindicated because of the risk of increasing IOP, but some ophthalmologists may use this method as an adjunct if there is a diagnostic dilemma and for assessment of other injuries, such as retinal detachment, if the physical exam is limited.68,73
Initial treatment consists of avoiding increased IOP and further pressure on the globe. A hard eye shield should be placed over the orbit. Antiemetics should be given, and the patient should not eat or drink anything pending surgical management. Prophylactic IV antibiotics are given, although data supporting a specific regimen are limited, and no controlled trials exist. Regimens should cover the most common causes of post-traumatic endophthalmitis, such as streptococci, staphylococci, and gram-positive and gram-negative bacilli, including Pseudomonas.74 Fungal infections are less common, causing 4-14% of post-traumatic endophthalmitis, and appear to be more common after injuries from vegetation.75 Oral levofloxacin 500 mg daily for 5-10 days achieves adequate vitreous concentrations76 and is a common antibiotic choice.77 High-risk patients receive IV vancomycin and ceftazidime, supplemented by topical antibiotics.77,78 Antifungal prophylaxis is not standard practice. Endophthalmitis occurs in 3-17% of globe rupture cases. However, in a center with a standardized protocol of 48 hours of IV vancomycin and ceftazidime followed by topical antibiotics, the reported rate was 0.9% among 558 cases.79
If patients with open globe injuries require intubation, traditional teaching has been that succinylcholine is contraindicated because of fears of increasing IOP. There is no evidence to support this concern. A single case series showed no adverse outcomes in open globe patients pre-treated with a low “defasciculating dose” of a non-depolarizing paralytic (e.g., rocuronium) prior to succinylcholine.80 Given the absence of evidence of harm, this concern should not delay optimization of intubating conditions in patients who require immediate airway management.
Immediate ophthalmology consultation is required in all cases of globe rupture.
Penetrating Eye Injury
Scleral lacerations and full-thickness corneal lacerations receive the same initial treatment and precautions as globe rupture with blunt trauma. There is evidence that penetrating mechanisms of open globe injury have a better prognosis compared to blunt globe rupture.81,82
Superficial corneal lacerations without gaping are treated with topical antibiotics, a cycloplegic, and a pressure patch, followed by urgent ophthalmology follow-up.10 A pressure patch consists of two soft eye pads held in place with tape, applied while the patient has both eyes gently closed. Applying upward traction on the skin of the cheek while tape is placed results in a snug fit that keeps the eyelid closed.83 Note that patching corneal abrasions (rather than lacerations) has been shown to be ineffective and may reduce 24-hour healing rates.41
Partial thickness corneal lacerations are repaired in an operating room setting by ophthalmology.
Intraocular foreign bodies are managed on a case-by-case basis. Orbital X-rays and CT are useful for evaluating for radio-opaque foreign bodies. Known acute intraocular foreign bodies should be managed as other acute open globe injuries with IV and topical antibiotics. Surgical removal and intravitreal prophylactic antibiotics may be considered by the ophthalmologist.
Endophthalmitis/Sympathetic Ophthalmia
Infection of anterior, posterior, and/or vitreous chambers of the eye, termed endophthalmitis, is a feared complication of eye trauma. Presenting features include pain, vision loss, conjunctival injections, hypopyon (layering pus in the anterior chamber), and increased opacity of the affected chambers. Treatment consists of prompt infectious disease and ophthalmology consultation for intraocular antibiotics. IV vancomycin and ceftazidime are common choices.
The deep structures of the eye are thought to contain antigens normally not visible to the immune system. Trauma and/or infection that violates the blood-eye barrier can expose these antigens, leading to an autoimmune inflammation of both the injured and uninjured eyes, which is known as sympathetic ophthalmia. It is rare, affecting 0.03 per 100,000 persons per year.84 Patients with this condition present similarly to those with uveitis, and symptoms include pain, photophobia, and decreased visual acuity. Treatment consists of immune suppression and consideration of enucleation of the injured eye. The prognosis is relatively poor, with half of patients demonstrating 20/40 or worse vision, and a third of patients becoming legally blind.85
Conclusion
Patients with trauma to the face and neck should receive a proper primary and secondary trauma survey to exclude any imminently harmful injuries. This should be followed by a careful evaluation of the eye and surrounding structures. Early recognition and careful assessment and management of potential vision-threatening injuries may avert visual loss and improve patients’ outcomes.
REFERENCES
- Centers for Disease Control and Prevention. National Institute for Occupational Safety and Health (NIOSH) Division of Safety Research. Work-Related Injury Statistics Query System 2016. Available at: https://wwwn.cdc.gov/wisards/workrisqs/workrisqs_estimates.aspx. Accessed Aug. 31, 2016.
- Bord SP, Linden J. Trauma to the globe and orbit. Emerg Med Clin North Am 2008;26:97-123.
- Smith HL, Chrischilles E, Janus TJ, et al. Clinical indicators of midface fracture in patients with trauma. Dent Traumatol 2013;29:313-318.
- Somasundaram A, Laxton AW, Perrin RG. The clinical features of periorbital ecchymosis in a series of trauma patients. Injury 2014;45:203-205.
- Joseph JM, Glavas IP. Orbital fractures: A review. Clin Ophthalmol 2011;5:95-100.
- Herbella FA, Mudo M, Delmonti C, et al. “Raccoon eyes” (periorbital haematoma) as a sign of skull base fracture. Injury 2001;32:745-747.
- Maramattom BV. Raccoon eyes following vigorous sneezing. Neurocrit Care 2006;4:151-152.
- Alvi S, Karadaghy O, Manalang M, Weatherly R. Clinical manifestations of neuroblastoma with head and neck involvement in children. Int J Pediatr Otorhinolaryngol 2017;97:157-162.
- Loo H, Forman WB, Levine MR, et al. Periorbital ecchymosis as the initial sign in multiple myeloma. Ann Ophthalmol 1982;14:1066-1068.
- Sharma R, Brunette DD. Ophthalmology. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 8th ed. St. Louis, MO: Saunders; 2014:909-930.
- Chang EL, Rubin PA. Management of complex eyelid lacerations. Int Ophthalmol Clin 2002;42:187-120.
- Brown DJ, Jaffe JE, Henson JK. Advanced laceration management. Emerg Med Clin North Am 2007;25:83-99.
- Mayersak RJ. Facial Trauma. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 8th ed. St. Louis, MO: Mosby, Inc.; 2014:378.
- Chandler DB, Gausas RE. Lower eyelid reconstruction. Otolaryngol Clin North Am 2005;38:1033-1042.
- Custer PL, Vick V. Repair of marginal eyelid defects with 7-0 chromic sutures. Ophthal Plast Reconstr Surg 2006;22:256-258.
- Burroughs JR, Soparkar CN, Patrinely JR. 7 tips for traumatic eyelid lacerations. Review of Ophthalmology; July 19, 2001. Available at: https://www.reviewofophthalmology.com/article/7-tips-for-traumatic-eyelid-lacerations. Accessed Sept. 1, 2018.
- Brady SM, McMann MA, Mazzoli RA, et al. The diagnosis and management of orbital blowout fractures: Update 2001. Am J Emerg Med 2001;19:147-154.
- Zimmer-Galler IE, Bartley GB. Orbital emphysema: Case reports and review of the literature. Mayo Clinic Proc 1994;69:115-121.
- Ng P, Chu C, Young N, Soo M. Imaging of orbital floor fractures. Australas Radiol 1996;40:264-268.
- Iinuma T, Hirota Y, Ishio K. Orbital wall fractures: Conventional views and CT. Rhinology 1994;32:81-83.
- Kubal WS. Imaging of orbital trauma. Radiographics 2008;28:1729-1739.
- Joseph JM, Glavas IP. Orbital fractures: A review. Clin Ophthalmol 2011;5:95-100.
- Mundinger GS, Borsuk DE, Okhah Z, et al. Antibiotics and facial fractures: Evidence-based recommendations compared with experience-based practice. Craniomaxillofac Trauma Reconstr 2015;8:64-78.
- Martin B, Ghosh A. Antibiotics in orbital floor fractures. Emerg Med J 2003;20:66.
- Millman AL, Della Rocca RC, Spector S, et al. Steroids and orbital blowout fractures — a new systematic concept in medical management and surgical decision-making. Adv Ophthalmic Plast Reconstr Surg 1987;6:291.
- Wilkins RB, Havins WE. Current treatment of blow-out fractures. Ophthalmology 1982;89:464-466.
- Fattahi T, Brewer K, Retana A, Ogledzki M. Incidence of retrobulbar hemorrhage in the emergency department. J Oral Maxillofac Surg 2014;72:2500-2502.
- Han JK, Caughey RJ, Gross CW, Newman S. Management of retrobulbar hematoma. Am J Rhinol 2008;22:522-524.
- Knoop KJ, Dennis WR. Ophthalmologic procedures. In: Roberts JR, ed. Clinical Procedures in Emergency Medicine. 6th ed. Philadelphia, PA: Elsevier; 2014:1259-1297.
- Harrahill M. A case report of traumatic eye compartment syndrome. J Emerg Nurs 2006;32:104-105.
- Cubano MA, ed. Emergency War Surgery. 4th ed. Borden Institute, US Army Medical Department Center and School, Fort Sam Houston, Texas; Office of The Surgeon General, United States Army, Falls Church, VA; 2013:205-217.
- Hayreh SS, Weingeist TA. Experimental occlusion of the central artery of the retina, IV: Retinal tolerance time to acute ischaemia. Br J Ophthalmol 1980;64:818-825.
- Hayreh SS, Zimmerman MB, Kimura A, Sanon A. Central retinal artery occlusion: Retinal survival time. Exp Eye Res 2004;78:723-736.
- Ballard SR, Enzenauer RW, O’Donnell T, et al. Emergency lateral canthotomy and cantholysis: A simple procedure to preserve vision from sight threatening orbital hemorrhage. J Spec Oper Med 2009;9:26-32.
- Winterton JV, Patel K, Mizen KD. Review of management options for a retrobulbar hemorrhage. J Oral Maxillofac Surg 2007;65:296-299.
- Oester AE Jr, Sahu P, Fowler B, Fleming JC. Radiographic predictors of visual outcome in orbital compartment syndrome. Ophthal Plast Reconstr Surg 2012;28:7-10.
- Sklar DP, Lauth JE, Johnson DR. Topical anesthesia of the eye as a diagnostic test. Ann Emerg Med 1989;18:1209-1211.
- Stern GA. Pseudomonas keratitis and contact lens wear: The lens/eye is at fault. Cornea 1990;9(Suppl 1):S36-S40.
- Calder LA, Balasubramanian S, Fergusson D. Topical nonsteroidal anti-inflammatory drugs for corneal abrasions: Meta-analysis of randomized trials. Acad Emerg Med 2005;12:467-473.
- Turner A, Rabiu M. Patching for corneal abrasion. Cochrane Database Syst Rev 2006;19:CD004764.
- Lim CH, Turner A, Lim BX. Patching for corneal abrasion. Cochrane Database Syst Rev 2016; 7:CD004764.
- Huecker MR, Danzl DF. Nontraumatic ocular emergencies. In: Markovchick VJ, Pons PT, Bakes KM, Buchanan JA. Emergency Medicine Secrets. 6th ed. Philadelphia: Elsevier; 2015:134-139.
- Bhatia K, Sharma R. Eye emergencies. In: Adams JG, ed. Emergency Medicine Clinical Essentials. 2nd ed. Philadelphia: Elsevier Saunders; 2013:209-225.
- Swaminathan A, Otterness K, Milne K, Resaie S. The safety of topical anesthetics in the treatment of corneal abrasions: A review. J Emerg Med 2015;49:810-815.
- Waldman N, Winrow B, Densie I, et al. An observational study to determine whether routinely sending patients home with a 24-hour supply of topical tetracaine from the emergency department for simple corneal abrasion pain is potentially safe. Ann Emerg Med 2018;71:767-778.
- Knoop KJ, Dennis WR. Ophthalmologic procedures. In: Roberts MD, Hedges JR, eds. Clinical Procedures in Emergency Medicine. 6th ed. Philadelphia: Elselvier; 2013: 1259.
- Bagheri N, Wajda B. Ultraviolet Keratopathy. In: Bagheri N, Wajda BN, eds. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease, Seventh Edition. Philadelphia: Wolters Kluwer; 2017:61.
- Wagoner MD. Chemical injuries of the eye: Current concepts in pathophysiology and therapy. Surv Ophthalmol 1997;41:275-313.
- Bagheri N, Wajda B. Trauma. In: Bagheri N, Wajda BN, eds. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease, Seventh Edition. Philadelphia: Wolters Kluwer; 2017: 12-51.
- Ikeda N, Hayasaka S, Hayasaka Y, Watanabe K. Alkali burns of the eye: Effect of immediate copious irrigation with tap water on their severity. Ophthalmologica 2006;220:225-228.
- Rihawi S, Frentz, Schrage NF. Emergency treatment of eye burns: Which rinsing solution should we choose? Graefes Arch Clin Exp Ophthalmol 2006;244:845-854.
- Kompa S, Redbrake C, Hilgers C, et al. Effect of different irrigating solutions on aqueous humour pH changes, intraocular pressure and histological findings after induced alkali burns. Acta Ophthalmol Scand 2005;83:467-470.
- Sharma N, Kaur M, Agarwal T, et al. Treatment of ocular chemical burns. Surv Ophthalmol 2018;63:214-234.
- Fong LP. Secondary hemorrhage in traumatic hyphema. Predictive factors for selective prophylaxis. Ophthalmology 1994;101:1583-1588.
- Rahmani B, Jahadi HR, Rajaeefard A. An analysis of risk for secondary hemorrhage in traumatic hyphema. Ophthalmology 1999;106:380-385.
- Gharaibeh A, Savage HI, Scherer RW, et al. Medical interventions for traumatic hyphema. Cochrane Database Sys Rev 2013;12:CD005431.
- Walton W, Von Hagen S, Grigorian R, Zarbin M. Management of traumatic hyphema. Surv Ophthalmol 2002;47:297-334.
- Engelhard SB, Patrie J, Prenshaw J, et al. Traumatic uveitis in the mid-Atlantic United States. Clin Ophthalmol 2015;9:1869-1874.
- Netland KE, Martinez J, LaCour OJ 3rd, Netland PA. Traumatic anterior lens dislocation: A case report. J Emerg Med 1999;17:637-639.
- Ojaghi Haghighi SH, Morteza Begi HR, Sorkhabi R, et al. Diagnostic accuracy of ultrasound in detection of traumatic lens dislocation. Emerg (Tehran) 2014;2:121-124.
- Rabinowitz R, Yagev R, Shoham A, Lifshitz T. Comparison between clinical and ultrasound findings in patients with vitreous hemorrhage. Eye (Lond) 2004;18:253-256.
- Mitry D, Charteris DG, Fleck BW, et al. The epidemiology of rhegmatogenous retinal detachment: Geographical variation and clinical associations. Br J Opthalmol 2010;94:678-684.
- Hoogewoud F, Chronopoulos A, Varga A, et al. Traumatic retinal detachment — the difficulty and importance of correct diagnosis. Surv Ophthalmol 2016;61:156-163.
- Pastor JC, Fernandez I, Rodriguez de la Rua E, et al. Surgical outcomes for primary rhegmatogenous retinal detachments in phakic and pseudophakic patients: The Retina 1 Project — report 2. Br J Ophthalmol 2008;92:378-382.
- Yoonessi R, Hussain A, Jang TB. Bedside ocular ultrasound for the detection of retinal detachment in the emergency department. Acad Emerg Med 2010;17:913-917.
- Shinar Z, Chan L, Orlinsky M. Use of ocular ultrasound for the evaluation of retinal detachment. J Emerg Med 2011;40:53-57.
- Negrel AD, Thylefors B. The global impact of eye injuries. Ophthalmic Epidemiol 1998;5:143-169.
- Chronopolous A, Ong JM, Thumann G, Schutz JS. Occult globe rupture: Diagnostic and treatment challenge. Surv Ophthalmol 2018;63:694-699.
- Harlan JB Jr, Pieramici DJ. Evaluation of patients with ocular trauma. Ophthalmol Clin North Am 2002;15:153-161.
- Weissman JL, Beatty RL, Hirsch WL, Curtin HD. Enlarged anterior chamber: CT finding of a ruptured globe. AJNR Am J Neuroradiol 1995;16(4 Suppl):936-938.
- Yuan WH, Hsu HC, Cheng HC, et al. CT of globe rupture: Analysis and frequency of findings. AJR Am J Roentgenol 2014;202:1100-1107.
- Chou C, Lou YT, Hanna E, et al. Diagnostic performance of isolated orbital CT scan for assessment of globe rupture in acute blunt facial trauma. Injury 2016;47:1035-1041.
- Schutz JS, Bronson NR 2nd. Ophthalmic contact B-scan ultrasonography. A practical clinical tool. Arch Ophthalmol 1974;92:291-296.
- Cornut PL, Youssef el B, Bron A, et al. French Institutional Endophthalmitis Study (FRIENDS) Group. A multicentre prospective study of post-traumatic endophthalmitis. Acta Ophthalmol 2013;91:475-482.
- Gupta A, Srinivasan R, Kaliaperumal S, Saha I. Post-traumatic fungal endophthalmitis — a prospective study. Eye (Lond) 2008;22:13-17.
- Fiscella RG, Nguyen TK, Cwik MJ, et al. Aqueous and vitreous penetration of levofloxacin after oral administration. Ophthalmology 1999;106:2286-2290.
- Gokce G, Sobaci G, Ozgonul C. Post-traumatic endophthalmitis: A mini-review. Semin Ophthalmol 2015;30:470-474.
- Ahmed Y, Schimel AM, Pathengay A, et al. Endophthalmitis following open-globe injuries. Eye (Lond) 2012;26:212-217.
- Andreoli CM, Andreoli MT, Kloek CE, et al. Low rate of endophthalmitis in a large series of open globe injuries. Am J Ophthalmol 2009;147:601-608.
- Libonati MM, Leahy JJ, Ellison N. The use of succinylcholine in open eye surgery. Anesthesiology 1985;62:637-640.
- Fabian ID, Eliashiv S, Moisseiev J, et al. Prognostic factors and visual outcomes of ruptured and lacerated globe injuries. Eur J Ophthalmol 2014;24:273-279.
- Fujikawa A, Mohamed YH, Kinoshita H, et al. Visual outcomes and prognostic factors in open-globe injuries. BMC Ophthalmol 2018;18:138.
- American Academy of Ophthalmology. Pressure patch. Available at: https://www.aao.org/image/pressure-patch. Published March 7, 2018. Accessed Sept. 3, 2018.
- Sen HN, Nussenblatt RB. Sympathetic ophthalmia: What have we learned? Am J Ophthalmol 2009;148:632-633.
- Chan CC, Roberge RG, Whitcup SM, Nussenblatt RB. 32 cases of sympathetic ophthalmia: A retrospective study at the National Eye Institute, Bethesda, Md., from 1982 to 1992. Arch Ophthalmol 1995;113:597-601.
This review will help the practitioner to be more comfortable evaluating and treating a patient with a traumatic eye complaint and understanding when to involve ophthalmology and with what urgency.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.