What Does the Sinus P Look Like?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The ECG in the figure below was obtained from a woman in her 50s who complained of intermittent chest discomfort in recent weeks. She was hemodynamically stable at the time this tracing was obtained. How might one interpret this ECG?
The rhythm is irregular. The QRS complex is narrow. P waves are present, albeit P wave morphology is changing. There are three different shapes of P waves in the long lead II rhythm strip. That is, P waves are tall and pointed in front of beats 1, 5, 6, 7, and 8; P waves are round in front of beats 2, 9, and 10; P waves are pointed, but not quite as tall, in front of beats 3, 4, 11, and 12.
Each P wave in this long lead II is conducting. For each of these three different P wave shapes, all beats of that shape manifest the same PR interval. The principal differential diagnoses for an irregular rhythm with different-shape P waves that are conducting are: sinus rhythm with multiple premature atrial contractions (PACs), multifocal atrial tachycardia (MAT), or wandering pacemaker.
This is not sinus rhythm with PACs because there is no predominant underlying sinus rhythm. Although R-R intervals are shorter in some places, there are no beats that are especially early (i.e., there are no PACs). This is not MAT because P wave morphology and the PR interval do not change from one beat to the next. Instead, there is gradual change in the site of the supraventricular pacemaker over the course of several beats. This strongly suggests the presence of a wandering atrial pacemaker. Other than the rhythm, there are minimal nonspecific ST-T wave abnormalities in several leads that do not appear to be acute.
Wandering atrial pacemaker is virtually always a benign rhythm. Technically, there should be at least three different atrial sites to distinguish a wandering atrial pacemaker from a simple atrial escape rhythm. The clinical reality is that most of the time the period of monitoring available for scrutiny simply will not be long enough to appreciate gradual shift in the site of the atrial pacemaker to at least three different sites. As a result, true wandering pacemaker is not a common diagnosis.
This case is unique in clinical experience for allowing definitive diagnosis of this rhythm in no more than a short long lead II rhythm strip. Most of the time, a much longer period of monitoring is needed.
For more information about and further discussion on this case, please visit: https://bit.ly/2DjFWDW.
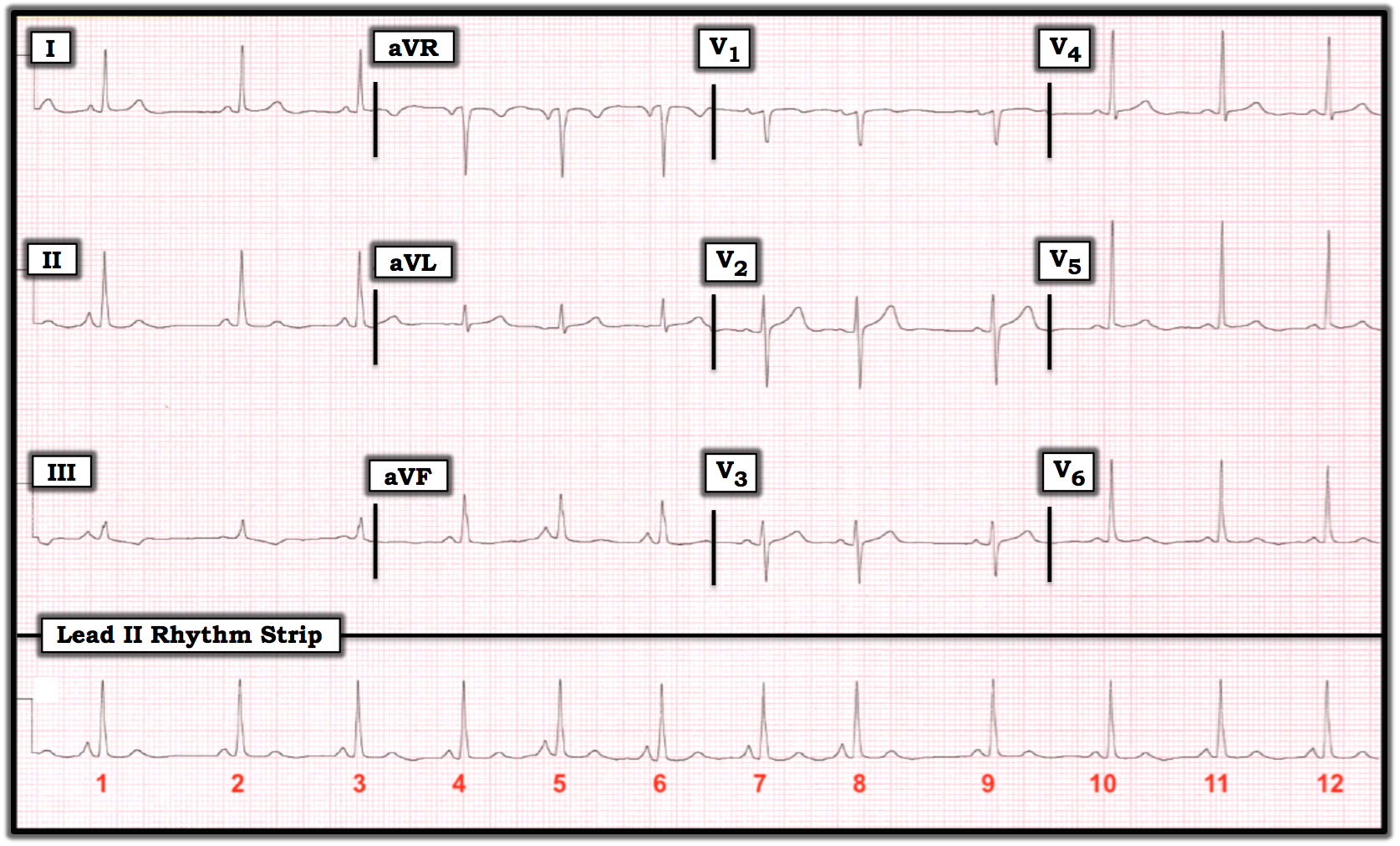
The ECG in the figure was obtained from a woman in her 50s who complained of intermittent chest discomfort in recent weeks. She was hemodynamically stable at the time this tracing was obtained. How might one interpret the ECG?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
