Acute Flaccid Myelitis 2018
By Stan Deresinski, MD, FACP, FIDSA
Clinical Professor of Medicine, Stanford University
Dr. Deresinski reports no financial relationships relevant to this field of study.
SYNOPSIS: The number of reported cases of acute flaccid myelitis, a paralytic disease of unknown etiology, has increased.
SOURCE: McKay SL, Lee AD, Lopez AS, et al. Increase in acute flaccid myelitis — United States, 2018. MMWR Morb Mortal Wkly Rep 2018;67:1273-1275.
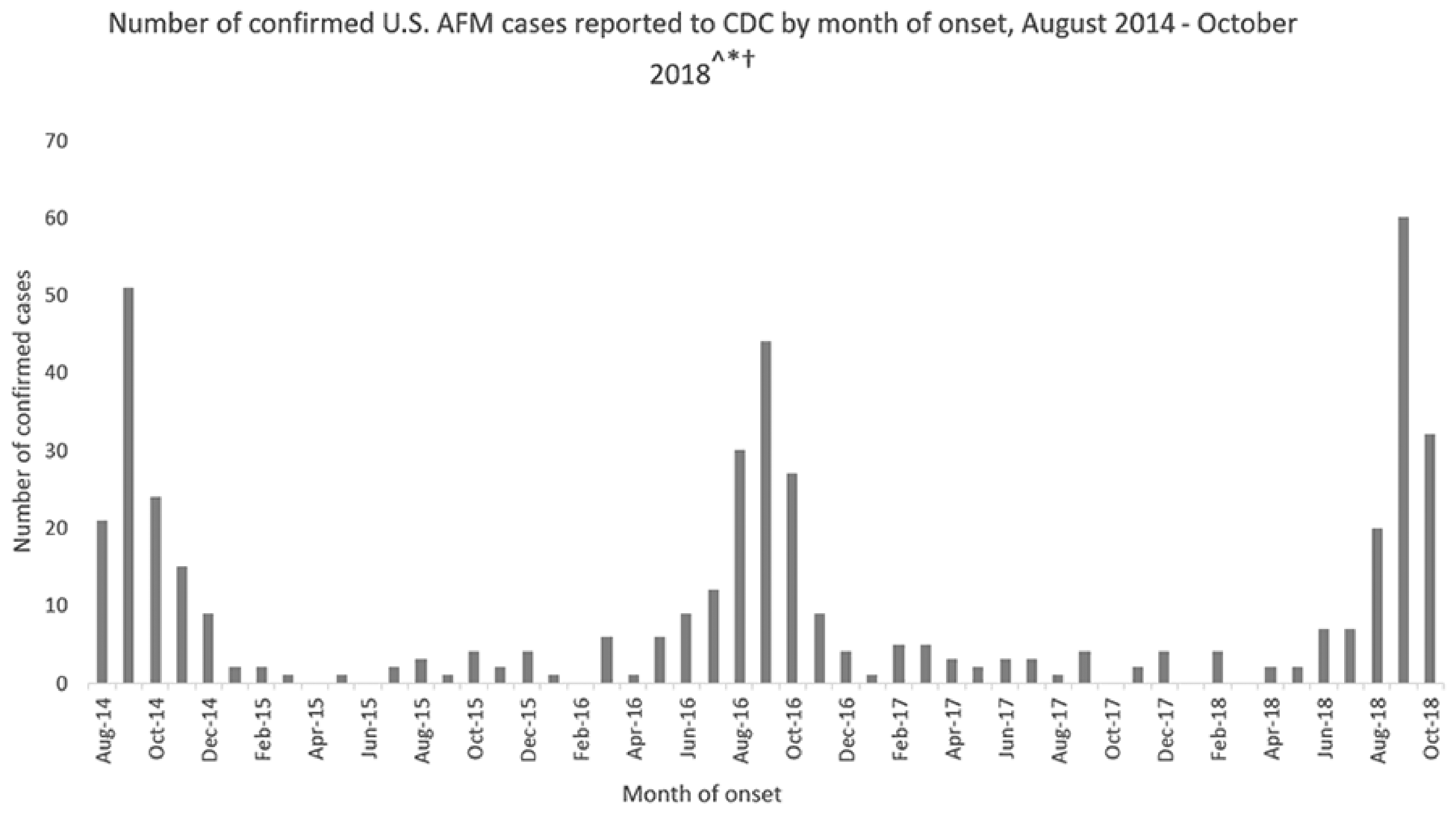
The Centers for Disease Control and Prevention (CDC) recognized an apparent increase in reported cases of acute flaccid myelitis (AFM) when 120 cases were confirmed in the summer and autumn of 2014. This led to the establishment of standardized surveillance the following year. (See Figure 1.) Although only 21 confirmed cases and three probable cases were identified in 2015, cases have rebounded subsequently. From Jan. 1 to Nov. 2, 2018, there was a threefold increase over the same period in 2017. Among the 106 reported cases that had undergone classification (see Table 1), 80 were confirmed, six were probable, and the diagnosis was rejected in 20. The patients’ ages ranged from 7 months to 32 years, with a median of 4 years and interquartile range of 2.4-7.6 years; 59% were male.
Signs and/or symptoms suggesting the presence of a viral illness had occurred in the four weeks prior to the onset of limb weakness in 79 (99%) patients. Thirty-eight (47.5%) patients had only upper limb weakness, seven (8.8%) had only lower limb involvement, 12 (15.0%) had weakness in two to three limbs, and 23 (28.8%) had involvement of all four limbs.
The results of cerebrospinal fluid (CSF) tests were available for 78 (98%) patients. Pleocytosis was present in 65 (83%), with 6-814 nucleated cells per mm3 (median 103/mm3), with most having lymphocyte predominance. The median protein and glucose concentrations were 47 mg/dL (range, 8-289) and 59 mg/dL (range, 40-138).
Polymerase chain reaction (PCR) testing of CSF, upper respiratory samples, and/or stool/rectal swabs detected enterovirus/rhinovirus (EV/RV) in 38 (54%) patients, with identification of EV-A71 in 11 (29%), EV-D68 in 14 (37%), and other viruses in 13 (34%). Only two patients had positive CSF samples — EV-A71 and EV-D68 in one each.
Figure 1: Confirmed Acute Flaccid Myelitis Cases Reported to CDC |
|
Source: Centers for Disease Control and Prevention |
Table 1: Acute Flaccid Myelitis Clinical Criteria |
Clinical CriteriaAn illness with onset of acute flaccid limb weakness Laboratory Criteria
Case ClassificationConfirmed:
Probable:
* Spinal cord lesions may not be present on initial MRI; a negative or normal MRI performed within the first 72 hours after onset of limb weakness does not rule out AFM. † Terms in the spinal cord MRI report such as “affecting mostly gray matter,” “affecting the anterior horn or anterior horn cells,” “affecting the central cord,” “anterior myelitis,” or “poliomyelitis” would all be consistent with this terminology. Source: Centers for Disease Control and Prevention. Available at: https://wwwn.cdc.gov/nndss/conditions/acute-flaccid-myelitis/case-definition/2018/. Accessed Dec. 9, 2018. |
COMMENTARY
AFM is a subtype of acute flaccid paralysis, which also includes a variety of paralytic diseases such as Guillain-Barré syndrome, acute transverse myelitis, and other entities.
The etiology of most cases of AFM remains unknown. A chief suspect has been EV-D68, an outbreak of which in 2014 was associated temporally with the emergence of AFM that year. However, EV-D68 was detected in the CSF of only two patients in the interval examined by McKay and colleagues, although it was found in other samples in several patients. The inability to detect a virus in CSF at the time of paralysis in most cases, together with the fact that 99% of patients had a preceding illness consistent with a viral infection, suggests the possibility that AMF may represent a post-infectious immunological disease.
CDC recommends the following:
“Parents and caregivers are urged to seek immediate medical care for a child who develops sudden weakness of the arms or legs. In the evaluation of a child with acute flaccid limb weakness, clinicians are advised to inquire about recent fever with or without antecedent respiratory or gastrointestinal symptoms and to collect timely specimens for viral testing, including CSF, serum, respiratory, and stool specimens. Additional information for clinicians is available at https://www.cdc.gov/acute-flaccid-myelitis/hcp/index.html. Patients with acute flaccid limb weakness should be reported to their health departments as soon as possible regardless of laboratory or MRI findings.”
The number of reported cases of acute flaccid myelitis, a paralytic disease of unknown etiology, has increased.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.