Lifestyle Modification for the Prevention and Reversal of Cardiovascular Disease
March 1, 2019
Reprints
AUTHORS
Harvey S. Hahn, MD, FACC, Director, Cardiovascular Fellowship Training Program and Co-Director KPN CV Quality, Kettering Medical Center, Associate Professor of Clinical Medicine, Wright State University/Boonshoft School of Medicine and Loma Linda University, Kettering, OH
Erik Poldemann, MD, Cardiology Fellow, Kettering Medical Center, Kettering, OH
PEER REVIEWER
Michael H. Crawford, MD, Professor of Medicine, Chief of Clinical Cardiology, University of California, San Francisco
Executive Summary
Lifestyle choices have a significant effect on cardiovascular disease prevalence as well as outcomes.
- Lifestyle is a critical determinant of the common risk factors for cardiovascular disease (hypertension, diabetes, hyperlipidemia, and smoking) that have been well-known to predict disease outcomes.
- Lifestyle medicine can be used in conjunction with traditional medications to provide the best care to patients.
- With the dual epidemics of obesity and type 2 diabetes, an aging population, and increased population growth, lifestyle modification stands as the most cost-effective way to manage population health.
- Medical providers need to act now to prevent being overwhelmed with the eventual increase in coronary artery disease following the obesity/diabetes epidemic.
Although there has been a 56% drop in mortality from cardiovascular disease (CVD) over the past 50 years, CVD still is the No. 1 cause of mortality in the United States.1 Stroke, which is the No. 3 cause of mortality, is linked to coronary artery disease because of shared risk factors.2 These improvements in mortality reduction have started to plateau.3 For the third year in a row, the average life expectancy in the United States has fallen, which has not happened since World War I.
Although important factors in CVD onset and progression once were thought to be mostly genetic in nature, we now realize that many of these factors are lifestyle-mediated. These include diet, exercise, sleep, stress, and other environmental factors. Cancer, the No. 2 cause of mortality, also can be affected by lifestyle changes. It is now believed that genetic risk explains only 7% of human longevity.4 This was studied by looking at the public portion of an ancestry website, which includes more than 54 million family trees with more than 6 billion individuals. In comparison, an ideal lifestyle could add up to 14 years of life for women and 12 years for men.5
The interplay between lifestyle and the genetic risk of heart disease was examined in three published cohorts.6 The relative risk for CVD was 91% higher in the highest genetic risk group determined by a polygenic risk score. Healthy lifestyle (measured as currently not smoking, no obesity, regular physical activity, and a healthy diet) attenuated the risk by about 50% across all groups. Furthermore, a healthy lifestyle reduced the objective CT calcium scores across all genetic risk groups as well. Anticoagulants and diabetes medications are cited most frequently as leading to emergency department visits.7,8,9 This trend may increase with the rapid rise in both atrial fibrillation leading to more anticoagulation and the obesity/type 2 diabetes epidemic.
Another aspect is contamination of medications, which recently has affected high blood pressure treatment with multiple recalls of angiotensin receptor antagonists. Multiple lots of valsartan were recalled for accidentally containing N-nitrosodimethylamine, which may cause cancer.10 Recalls, contamination, drug shortages, and even deaths have affected and interrupted patient care. Contaminated heparin led to multiple hypersensitivity reactions in patients undergoing dialysis and more than 80 deaths.11 All these factors will continue to threaten patient care as long as patients are reliant on medications.
Furthermore, there is the problem of medication noncompliance. Medication compliance is a major issue and most likely only will worsen with misinformation on the internet and distrust of large pharmaceutical companies. A recent study specifically examining statin adherence found that pharmacy refill rates were only 79% in post-myocardial infarction (MI) patients, 67% in patients with diabetes, and 63% in patients without diabetes and CVD.12
Even more sobering is the recent ARTEMIS trial, which tested if vouchers to cover the copay for P2Y12 inhibitors would increase compliance.13 Although the trial was positive in that there was a statistically significant increase in medication compliance, the improvement was only a 2.3% absolute increase, which did not translate into any further major event reduction.
Finally, our vast medical arsenal is not working. In a meta-analysis of the COURAGE, BARI 2D, and FREEDOM studies of secondary prevention, CVD risk factor control was poor.14 By one year, goal low-density lipoprotein (LDL) was reached in less than 80% of patients, goal blood pressure (BP) in less than 60%, and goal hemoglobin A1c (HbA1c) was just above 50%. The percentage of patients reaching all four metrics (the above three and smoking cessation) ranged from less than 10% in the FREEDOM trial to just under 50% in the COURAGE trial. This is discouraging, as clinical trials are optimal environments for follow-up care.
Outside of clinical trials, the overall population rates of risk factor prevalence and control are just as alarming. The lone exception is smoking, which has declined considerably. The 2016 National Health Interview Survey estimated that cigarette smoking in U.S. adults decreased from 20.9% to 15.5% between 2005 and 2016.15 However, the upsurge in vaping and marijuana use may reverse this trend, since these are recognized gateways to tobacco smoking.
Hypertension affects at least one in three U.S. adults, depending on which blood pressure guideline is followed. The prevalence of hypertension in U.S. adults is 31.9% under the previous definitions of hypertension (> 140/90 mmHg), and the prevalence rose to 45.6% under the 2017 American College of Cardiology (ACC)/American Heart Association (AHA) guideline definition of hypertension (> 130/80 mmHg).16 In the face of this high prevalence, only 54% are at goal BP.17 The Centers for Disease Control and Prevention currently estimates 9.4% of the U.S. population has diabetes; of those, 23.8% have yet to be diagnosed.18 In addition, 33.9% of the U.S. population has prediabetes. Of those individuals with prediabetes, only 11.6% reported being told by a provider that they had the condition. Researchers estimated that 49% of all Californians are diabetic or prediabetic.19
The National Health and Nutrition Examination Survey (NHANES) reported that 36.7% of U.S. adults had hyperlipidemia.20 Of those, 55.5% were taking cholesterol-lowering medication and 46.6% reported making lifestyle modifications to lower their cholesterol. Only 9.5% of patients had LDL levels below 70 mg/dL.20 Interestingly, 93% of those patients were on medication, with 57% also making lifestyle modifications. Another 26.9% had LDL levels between 70-100 mg/dL, with 74% taking medications and 50% also using lifestyle changes. The overall total control rate was only 36.4%.20
In a study of patients with known heart disease, researchers measured smoking, glucose control, low-dose aspirin use, BP control, physical activity, lipid control, and ideal body mass index (BMI) and found that all seven metrics aligned in less than 1% of study participants.21 A reason for this could be the medical community’s focus on medical management rather than a combined effort promoting healthy lifestyle behavior change supplemented by appropriate medical management. There is a limit to what medications can control in the setting of unhealthy habits such as overeating, smoking, and not exercising. There is a growing body of evidence supporting the effect of lifestyle choices on cardiovascular outcomes, as well as the need for improvement in those choices.
Researchers measured the degree of seven AHA health metrics, including BP control, lipid control, glucose control, BMI, healthy diet score, adequate physical activity, and smoking. The first four are objective, commonly measured medical metrics. The last three are lifestyle/behavior choices. It is clear that the last three affect the first four metrics. This list has been renamed the AHA Life’s Simple 7 (LS7). Less than 2% of the overall population had all risk factors optimized with both medications and lifestyle.22
Researchers at the Mayo clinic performed a similar analysis looking at only four metrics and found just 2.7% of the study group had optimal metrics for smoking, healthy diet, normal percent body fat, and physical activity.23
Stroke patients have similar poor health metrics. In a study using the AHA LS7 metrics, researchers found only a single patient (not 1%, but a single patient) out of 67,514 had all seven ideal metrics.22 Furthermore, from 1988 to 1994, blood pressure and lipid control improved, but diet, physical activity, and BMI all worsened.24 In fact, the proportion of patients who had a low LS7 score doubled from 17.9% to 35.4% during that time. Addressing these metrics is even more important now, as investigators estimated that the worldwide risk of stroke for those older than 25 years of age is now 25%.25 Clearly, there is much work to do in the medical community and patient population to change this statistic.
There are many reasons that physicians do not try routinely to help patients modify their lifestyle behaviors. Probably the most important reason is a knowledge gap in medical training. A survey of cardiovascular fellows and attendings found that the majority had little to no training in nutrition during medical school (31%), residency (59%), or fellowship (90%).26 Although 95% believed that dietary interventions were important, only 8% described themselves as experts in nutrition. Taken from the opposite perspective, authors of another study found that very low levels of lifestyle advice were given to overweight patients (only 21.4%) and only 44.2% of obese patients received any lifestyle counseling.27
Another barrier is that physicians often believe patients will not or cannot change. The data are sobering. When looking for comprehensive lifestyle change post-infarct or post-stroke, only 4% of patients will modify their diet, exercise more, and stop smoking after a life-changing event.28 One possible reason is that providers may be more comfortable prescribing medications than advocating for a healthier lifestyle. Physicians also can feel uncomfortable bringing up the topic of lifestyle, especially weight loss, since the patient may take it as criticism and it often is considered politically incorrect. The most important reason probably is that many physicians believe lifestyle modification does not work and that medications are clearly superior. The rest of the article will focus on changing the knowledge gap. (See Figure 1.)
Figure 1. Factors Contributing to Development of Cardiovascular Disease |
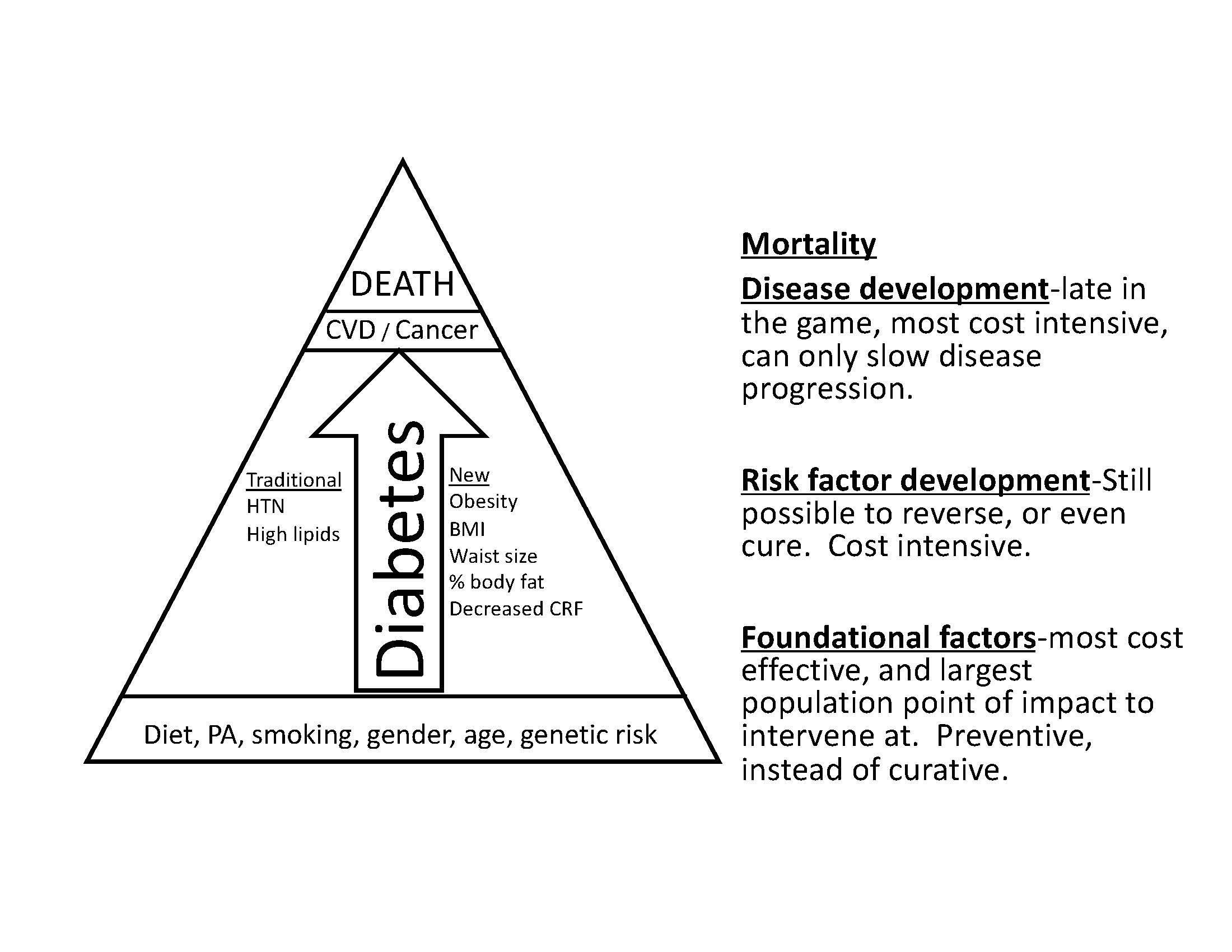 |
Treating the Cause
Even if providers could manage patients’ BP, lipids, or diabetes perfectly with medication, patients still would be hypertensive, hyperlipidemic, and diabetic. The only way to possibly reverse these conditions is lifestyle modification. Although this will not result in a cure always, striving for that goal will help in management. (See Table 1.)
Table 1. Comparative Effectiveness and Safety of Lifestyle Medicine and Traditional Pharmacotherapy |
|
Traditional Pharmacotherapy |
Lifestyle Medicine |
|
Pros
Cons
|
Pros
Cons
|
The most cost-effective and safe treatment strategy is one of lifestyle modification to try to reverse the disease process itself rather than treat the end symptoms. Medications can be a significant cause of morbidity and mortality.7 Authors of a large meta-analysis compared the cost and impact of various interventions on CVD outcomes. Procedures such as left ventricular assist devices and cardiac transplantation are lifesaving but expensive. Furthermore, they only affect a small proportion of the population. In comparison, treating the obesity epidemic would have a significant population-level effect and is much less cost intensive.29
In an interesting meta-analysis, researchers compared the relative risk reduction with lifestyle changes to the typical medications prescribed to patients with coronary artery disease. The estimated reduction was 35% with smoking cessation, 25% with increased physical activity, and 45% with dietary changes.30 This is in comparison to reductions of 18% with low-dose aspirin use, 21% with statins, 23% with beta-blockers, and 26% with angiotensin-converting enzyme inhibitors. This is not to say that providers should use lifestyle modification in isolation, but to demonstrate its effectiveness and highlight the potentially complimentary, additive, or even synergistic effect of combined lifestyle modification with optimal medical therapy.
During a United Nations meeting about noncommunicable diseases, World Health Organization Director-General Margaret Chan called noncommunicable diseases a “slow-motion disaster.”31 The answer was not to increase the use of high-tech medicine, but to emphasize prevention in the form of smoking cessation, increased physical activity, decreased alcohol use, and healthier diets. These were called the best-buy interventions to address the growing risk factors that lead to chronic diseases.
The AHA and the ACC have launched initiatives promoting and educating both patients and physicians in lifestyle medicine. The ACC has demonstrated its commitment through an ongoing series called CV Health Promotion and recently dedicated an issue of the Journal of the American College of Cardiology to this topic.32 The AHA issued a call to action to effect behavior change. It published detailed recommendations on how to assess and intervene on behalf of patients by using a system called the 5 As: Assess unhealthy behavior, Advise the patient how to change, Agree through a shared process on the goals, Assist with treatment, and Arrange for follow-up and accountability.33
Traditional Risk Factors
Well-known risk factors for CVD include age, male gender, smoking, diabetes, high blood pressure, and high cholesterol. Of these, age and gender are not modifiable. Only gender is binary, but all others affect risk in proportion to their values. Thus, making any change in blood pressure, lipids, or diabetes control is helpful, or in the case of worsening control, detrimental to health. These classic risk factors have formed the basis of the Framingham risk score, which has stood the test of time. (See Table 2.)
Table 2. Classic and New Risk Factors or Metrics (Therapeutic Targets) |
|||
Classic or Traditional Risk Factors |
New Objective Risk Factors
|
New Subjective Risk Factors or Metrics |
Emerging Risk Factors* |
|
|
|
|
|
* Not discussed in this article |
|||
New Risk Scoring Systems
The major determinants of these risk factors are not genetic, but lifestyle mediated. There has been increased interest at looking directly at measures of lifestyle, such as diet quality, amount of physical activity, and amount and quality of sleep, to further assess patients alongside the traditional risk factors. Adding to the Framingham score, newer risk scores have been able to predict risk by accounting for classic risk factors and measuring the lifestyle components that most likely are driving those same risk factors. Like traditional risk factors, these new risk factors also are potential therapeutic targets.
Newer risk factors include weight, obesity, BMI, waist circumference, body composition (percent body fat), amount of physical activity, fitness level, type of diet, stress, sleep, and environmental factors, such as noise and particulate pollution. These risk factors can be modified by both medications and lifestyle techniques.
Although researchers have looked at most of these risk factors individually, several new analyses have helped us better understand their respective roles. Using methods such as population attributable risk, researchers for studies such as INTERHEART have been able to determine the degree of effect a certain risk factor will have on development of CVD.34 More than half the risk of myocardial infarction in men and women could be attributed to lifestyle habits. When traditional risk factors were added, they could account for more than 90% of the risk profile of both men and women.
In another analysis of the COURAGE trial, researchers measured overall survival by risk factor control.35 Factors that predicted increased survival were nonsmoking status, regular physical activity, controlled BP, and following the AHA step 2 diet. Having four to six metrics at goal compared to zero to one metric resulted in a 36% reduction in mortality.
In an Australian study of more than 231,048 people, researchers tracked smoking, alcohol use, diet, physical activity, sedentary behavior, and sleep duration to calculate a risk score. People who scored the worst on all six had an almost six-fold increase in death than those who scored the best in all six areas.36
Achieving all seven of the AHA LS7 metrics is the ideal goal, but even meeting three to four of these metrics is protective. Meeting five to seven metrics was associated with a 72% reduction in CVD events, and meeting three to four metrics was associated with a still sizable and significant 47% reduction in events.37
Lifestyle change also is effective in the high-risk diabetes group. Behavior changes reduced CV incidence by 52% and mortality by 68% in patients with diabetes.38 More importantly, healthy lifestyle (measured by cholesterol levels, BP, diet, smoking status, physical activity, and BMI), in a dose-dependent fashion, could reduce the risk of developing type 2 diabetes by up to 80%, showing the powerful preventive effect of lifestyle.39
Therapeutic Targets
The Hard Targets: Weight, BMI, Waist Circumference, and Percent Body Fat
Obesity has increased gradually in the United States and the world over the past few decades. Obesity rates have climbed from 28.8% to 36.9% in men and from 29.8% to 38.0% in women from 1980 to 2013.40 This coincides with the increase in type 2 diabetes. Because of differences in height and body build, BMI has become the most commonly used method to assess if a patient is overweight or obese. Being 40 pounds over goal weight is one definition of obesity. Weight is not only a prognostic sign, but frequent weight fluctuations, such as with yo-yo dieting, can negatively affect health. As little as a 3.88-pound (1.76 kg) increase in weight was associated with a 64% increased risk of any coronary event, an 85% higher risk of any CVD event, and a surprising 124% increased risk of death.41
Obesity is not only a health-related issue, but also one of national security. The authors of a recent bipartisan report, “Unhealthy and Unprepared: National Security Depends on Promoting Healthy Lifestyles From an Early Age,” found that 71% of applicants to the armed forces are not eligible, and 31% are excluded because of obesity.42
A BMI of > 25 kg/m2 is considered overweight, while a BMI of > 30 kg/m2 is obese. BMI has some problems, one of which is that although both height and weight need to be measured, outside of research protocols, patients often just state the values. Furthermore, the use of BMI does not work well at the extremes of weight. Professional athletes commonly are included in the obese category because of their heavier weights, but they typically have low body fat and should not be classified as such. A recent study of National Football League combine players found an obesity rate of 53.4% based on BMI. When graded by percentage of body fat, the obesity rate dropped to 8.9%.43 A population for whom BMI may become particularly helpful is children. By measuring a patient’s BMI trajectory, researchers were able to predict by 6 years of age which children would be obese as adolescents,44 thus, perhaps allowing doctors and parents to screen for high-risk children and intervene as early as possible.
A simple, fairly reproducible measurement is a waist circumference measurement. Taken at the hips, it is part of diagnosing metabolic syndrome, but it also independently is related to mortality regardless of BMI.45 To be at risk based on waist circumference, measurements have to be > 40 inches (94 cm) in men and > 35 inches (80 cm) in women.46
In the latest NHANES report, weight, BMI, and waist circumference all have increased from 1999 to 2016.27 Height did not change. For men, the mean weight has increased from 189.4 pounds to 197.9 pounds. The mean weight for women went up by 6.8 pounds. The mean waist circumference increased to 40.2 inches (102.1 cm) in men and to 38.6 in (98.0 cm) in women. Similarly, BMI has increased for both men and women. The mean BMI is now 29.1 kg/m2 in men and 29.6 kg/m2 in women.47
A better way to risk stratify patients is body composition, which can be measured by looking at percent body fat or lean body mass. Measuring body fat is becoming more important for a number of reasons. Weight loss has been the traditional way to measure improvement in health, but with the increased focus on exercise, and especially resistance training, it became more important to track changes in body composition since muscle is denser than fat. For men, a percent body fat of 18-25% is normal, > 26% is overweight, and > 38% is obese. For women, 25-31% is normal, > 32% is overweight, and > 42% is obese.
Muscle mass may be more important than degree of fatness. Grouped by high or low muscle and high or low fat, there was almost a 20% reduction in mortality in the two groups with high muscle mass vs. those with low muscle mass regardless of percent body fat content.48
Making direct measurements has become even more important because of two new phenomena. The first is the increase in the weight of the U.S. population, leading to a change in what is perceived as normal. When photos of overweight or obese children are shown to other children or mothers, they often are rated in the next lower category. Obese children often are rated as overweight, and overweight children often are graded as normal.49 This is caused by a drift or normalization of body size and weight due to the change in our population. Also, there is the new concept of TOFI — thin on the outside, fat on the inside — in which people have normal BMI but increased body fat.50 Physicians no longer can rely on the eyeball test or on patients’ stated metrics.
The Soft Target: Diet
Using food as medicine has been borne out in numerous studies showing the fundamental effect of diet on not only risk factor development, but also overall event rates and even mortality. Metrics such as BP, LDL, and HbA1c can be measured easily and accurately. Weight, waist circumference, BMI, and percent body fat also can be measured reproducibly and accurately. However, it is harder to measure dietary intake. Most studies are done by surveys that rely on patient recall, which allows for errors and bias. An editorial called for the exclusion of dietary survey data in the medical literature since it was not of high enough scientific quality.51 Although the quality of the data is observational and lower in quality because of the collection methods, the results have been impressively uniform.
Researchers have studied and continue to study diet extensively, mostly in observational trials. One of the most important and interesting studies was the Mr-FIT study about Japanese migration.52 These investigators tracked Japanese patients in Japan, Hawaii, and San Francisco. When those of Japanese descent migrated from Japan to Hawaii to San Francisco, their CVD event rates doubled and their lipid levels increased similarly. BP did not follow this same pattern. Furthermore, at that time, smoking was nearly universal in the Japanese culture, so the change in event rates would be explained best by changes in lipids, which most likely would be explained by dietary changes.
Currently, the healthiest cardiovascular subpopulation is the Tsimané tribe in Bolivia, South America. They have the lowest degree of CT calcium scoring ever recorded for a subgroup.53 Eighty-five percent of the population had a coronary calcium score of zero. Only 3% had a score higher than 100. Almost no typical risk factors for CVD (hypertension, high lipids, diabetes) and almost no clinical CVD events exist in their tribe, despite members eating 70% carbohydrates and having a high inflammatory burden (measured by elevated high-sensitivity C-reactive protein levels in 51% of the population). The tribe is very active, eats mostly whole foods, does not smoke, and typically has normal BMIs. It will be interesting to see what happens as the modern world affects their tribe.
In comparison, SAD is the current acronym for the standard American diet. Americans eat a high-carbohydrate diet that consists mostly of highly processed and high-sugar foods.54 The PURE study investigators demonstrated that a high-carbohydrate diet was associated with a 28% increased rate of overall mortality compared to a diet with higher fat consumption.55 Interestingly, CVD mortality and events were not higher in the higher-carbohydrate group.
Authors of another study demonstrated the relative contribution of different dietary habits on mortality in the United States.56 Unlike the PURE study, which focused mostly on macronutrients, this study looked at subclasses of food (sodium intake, nuts, processed meats, seafood, vegetables, fruits, high sugar beverages, whole grains, and red meat). The most interesting part of this study was its longitudinal nature that allowed the investigators to track the changing U.S. dietary patterns. Both sodium and red meat intake increased over the time of the study. Conversely, nut, whole grain, and fruit intake all unfortunately declined. An encouraging finding was that sugar-sweetened beverages decreased almost 15%.
A good starting point to try to change these dietary patterns is the Harvard Healthy Plate,57 which is built on evidence-based data and has some significant differences from the FDA food plate. Of note, both the choosemyplate.gov and Harvard healthy plate recommend that half of one’s plate include fruits and vegetables.
Over time, there has been more evidence that increased servings of fruits and vegetables confer protection from heart disease and cancer. Authors of the most recent study found that there is still increasing incremental benefit of up to 10 servings a day.58 This large meta-analysis of more than 95 studies involving more than 2 million patients showed a 24% reduction in heart disease, 33% reduction in stroke, 13% reduction in cancer, and 31% reduction in premature mortality. Also, the threshold to achieve any risk reduction was only 2.5 servings a day or less than one serving per meal.
The PURE healthy diet score is a scoring system for diet quality.59 The score uses seven foods that were linked with survival — fruits, vegetables, nuts, legumes, dairy, red meat, and fish. Scores are from 1 to 5 in all seven categories for a total score of 7 to 35. The best groups were eight fruits/vegetables per day, 2.5 legumes and nuts per day, three servings of full-fat dairy, 1.5 servings of unprocessed meat, and two servings of fish per week. When comparing the healthiest scored diets to those of the lowest group, there was a significant effect on mortality and hard cardiovascular endpoints. When the score was applied to several large trials, researchers noted the following reductions. Diet was associated with a 24% reduction in mortality in the ONTARGET and TRANSCEND studies, with a 22% reduction in the INTERHEART study, and with a 25% reduction in stroke in the INTERSTROKE study.34,60-62
A vegan diet can have the same effect on LDL as low-intensity statin therapy. Adhering to a completely vegan diet resulted in a 30% reduction of LDL in four weeks.63 This was similar to what was achieved with a low-intensity statin treatment over the same time. However, being vegetarian or vegan is not necessarily healthy. A recent study grading diet quality found that an unhealthy plant-based diet afforded the same risks as animal-based diets.64 So the type of diet, per se, may not be as important as the actual elements being consumed. While it is outside the scope of this review to discuss different diet strategies, data from a well-done review article showed consistent elements between low-carb, low-fat/vegetarian/vegan, low-glycemic, Mediterranean, Paleolithic, and mixed/balanced diets. These included limited refined starches, added sugars, and processed foods; limited intake of certain fats; and increased intake of whole plant foods.65
Authors of several large studies have found that nut intake of any kind, not just walnuts (which the AHA has supported for years), reduces mortality.66,67 Daily nut intake was associated with a 20% relative risk reduction. These studies could not differentiate between types of nuts or even salted vs. non-salted. The intake of any type of nuts was protective. A concern with nut intake is that nuts are calorie dense and could lead to weight gain.
Fiber has been recommended for risk reduction of overall mortality, CVD, type 2 diabetes, and colon cancer. In a large meta-analysis, investigators recently demonstrated a 15-30% reduction in the above-mentioned outcomes when comparing the highest to the lowest fiber consumers.68 The current recommendation is at least 25 g of fiber per day.
Furthermore, in a substudy of the PESA trial, investigators analyzed the importance of eating breakfast.69 Although they found that eating breakfast was protective, they further divided the groups into eating clusters: a Mediterranean eating cluster, a Western eating cluster, and a social business eating cluster. The social eating cluster skipped breakfast most often and snacked the most. This probably correlates with a busy schedule, rushed eating, and eating on the go. Not surprisingly, this group also had the worst outcomes, thus pointing to the possibility that a busy lifestyle and eating fast food, rather than skipping breakfast, actually is the more problematic habit.
Sugar intake has been directly associated with mortality. There is a four-fold increase in mortality from the lowest to the highest sugar consumers. The highest sugar consumers obtained more than 30% of their calories from sugar.70 The largest contributor of excess sugar is sweetened beverages, including soda, tea, energy drinks, and juices. Researchers estimated the amount of excess deaths in countries attributed to soda consumption and found Mexico had the most deaths attributable to soda and the United States was fourth.71 Thirty percent of the risk of death in Mexico was attributable to this. Worldwide, the model estimated that 184,000 people die annually from this cause. Deaths from sugar-
sweetened beverages were predicted to outpace violent deaths in Mexico. A strategy of reducing exposure to these products and drinking water instead could have a substantial effect on population health.
Many suggest that sugar-free drinks may not be harmful because of the lack of refined sugar. In direct opposition to this notion, researchers recently found an almost 300% increase in stroke and dementia from consuming diet soda.72 Moreover, in another study looking at the gut biome, investigators found that about one in five people have a gut flora pattern that made patients who ingested artificial sweeteners more susceptible to diabetes even though they were not ingesting real sugar.73
There is growing evidence that meat intake affects mortality adversely. One daily serving of red meat can increase mortality by 13% and processed meats can increase it by 20%.74 Conversely, when meat is replaced by another protein source, such as beans, whole grains, or nuts, mortality is reduced by 10%, 14%, and 19%, respectively.
Further supporting these observational data are several mechanistic studies explaining how meat can lead to increased cardiovascular events and mortality. Two important studies demonstrated that when L-carnitine, which is a nutrient found in red meat, is processed by normal gut flora, it produces TMAO, which leads to platelet hyperreactivity and promotes atherosclerosis.75,76 Another mechanism is heme iron and nitrates, which may explain why red meat is associated with cardiovascular disease more strongly than white meat.77
The Mediterranean diet, which is based on consuming extra virgin olive oil, fruits and vegetables, fish, nuts, and limited red meat, has been found to reduce mortality by about 30%.78 Using a risk score based on compliance with the Mediterranean diet, researchers found that as patients ate more of the recommended foods, CVD event rates were reduced.79 For every one-point increase in diet score, there was a 5% reduction in event rates. There was an absolute 3.5% risk reduction comparing the highest to the lowest diet group. This gives a number needed to treat of only 28 patients to avoid one major CVD event. The authors noted that a better strategy may be to focus on recommending that people eat more of the good food items rather than focusing on what foods to avoid.
A final concern about eating healthy is the cost. Although many believe eating healthy is cost prohibitive, investigators showed that the cost of healthy, isocaloric foods averages out to only $1.50 per day per person.80 This may not be extrapolated well to organic foods or situations, such as food deserts where healthy food is not an option.
The Soft to Hard Target: Physical Activity
The current Physical Activity Guidelines for Americans recommendations are for 150 to 300 minutes of moderate-intensity physical activity per week, 75 to 150 minutes of vigorous-intensity aerobic physical activity per week, or a combination.81 That averages out to 25 to 50 minutes per day or 12.5 to 25 minutes per day, respectively (assuming six days of activity per week). Only 26% of men, 19% of women, and 20% of adolescents meet these recommendations. A lack of physical activity has led to an estimated cost of $117 billion per year and 10% of all mortality. Meeting these physical activity goals is associated with a 33% reduction in death.
Sitting Disease
Sitting time also is associated with all-cause mortality. The authors of an Australian study of 222,497 adults found that sitting increased mortality.82 Although exercise helped mitigate the effect, it did not eliminate the adverse effects of prolonged sitting completely.
Other investigators found that replacing sedentary behavior with light activity for 30 minutes led to a 17% reduction in mortality. Moderate to vigorous exercise was associated with a 35% reduction.83 To experience the mortality reduction, the patient had to reduce sedentary time (replace it) with physical activity, not simply increase exercise time.
Although most people believe the diabetes and obesity epidemics have been driven mostly by excess calories, some data point to less exercise as the dominant factor. The percentage of people who now do no leisure-time physical activity has doubled from 1988 to 2010.84 Physical activity also has an epigenetic effect on obesity development. In two subgroups of patients who were genetically predisposed to developing obesity, physical activity modified the development of obesity by up to 40%.85
Exercise and obesity are not always related or causal. Researchers found that both physical activity and obesity have their own relative contribution to mortality and, furthermore, that physical activity was more protective than being at ideal weight. Physical activity reduces the risk of death by 7.35% compared to non-obesity, which reduced death by 3.66%, a two-fold difference in effect.86
Physical activity long has been known to decrease mortality. The earliest examples come from the cardiac rehabilitation literature, which showed that supervised physical activity early after MI led to reduced mortality. What is encouraging is that similar results still are seen. In a large, recent study in Sweden, investigators demonstrated that compared to post-MI survivors who were not active, those who were active consistently over the next year had a 71% risk reduction in mortality. Even subjects in the reduced activity group still had a 44% reduction. Finally, those who started late (increased activity group) showed an intermediate 59% reduction.87
Physical activity is similar in effectiveness as standard blood pressure medications. In a large meta-analysis that included 391 trials, exercise had a similar BP-lowering effect as most single pharmacologic agents (-2.9 to -5.0 mmHg). This held true for both endurance and resistance types of exercise.88
In the CLEVER trial, a small study comparing optimal medical therapy vs. stenting vs. physical activity, researchers found physical activity led to the greatest increase in walking distance. The caveat in this study is that the physical activity was supervised exercise therapy and was not patient reported.89
Patients often ask providers for guidance on the minimum they need to do. The level of physical activity needed to affect mortality has been studied extensively and continues to fall. In a large-scale study from Taiwan, researchers showed that not only duration, but also intensity factored into mortality reduction.90 Performing 15 minutes of continuous, moderate exercise was enough to start separating the survival curves. More intense exercise had an earlier impact. In another study, researchers found that 10 minutes of continuous jogging (albeit at a 10-minute per mile pace) reduced mortality,91 but that increased volume and intensity both further reduced mortality.
There are only a few studies that have shown a U-shaped relationship between physical activity and mortality. The most famous was the Copenhagen Heart Study, which demonstrated that both the low physical activity group and the vigorous physical activity groups had the highest mortality, but that there was a progressive decline in mortality from the lowest to the mild to the moderate groups, finally reversing the mortality trend with the more vigorous group.92 The highest physical activity group in this study had relatively high event rates, but since that group was the smallest sample size (36 total patients), this could represent a type II beta error (false positive).
The Copenhagen Heart Study included 3,950 participants. Authors of a later study, which included more than 200,000 patients and more than 57,000 in the vigorous group, found the expected incremental decrease in mortality with increased physical activity.93 Some have expressed concern that short bursts of intermittent physical activity actually could be deleterious to health. Investigators demonstrated that such “weekend warriors” actually benefit from less-than-optimal physical activity. Regularly active men had a 37% reduction in mortality, but the intermittent weekend warriors had a 22% reduction.94
In another study, investigators showed that being active and staying active resulted in the lowest mortality in people with CVD. Being inactive and staying inactive, as expected, had the highest mortality, and active patients who became inactive had the second highest CV mortality. Inactive patients who became active were the same as the active-active group.95
Previous studies of endurance events, such as marathon running, have been associated with a risk of death during the performance.96 Several factors should be noted. The overall event rate was low, at 0.67 per 100,000 persons. During the 10 years in which the researchers collected data, there were only 59 cardiac arrests. Also, while studies have shown acute myocardial performance decline, especially in the right ventricle on echocardiogram and magnetic resonance imaging, and troponin leaks, both were small in size, not clinically relevant, and not permanent.
On the other hand, a large meta-analysis of running studies estimated that runners live three years longer than non-runners, and every hour of running added seven hours to the lifespan.97
Television can harm patients acutely and in longevity. In an Australian study, researchers showed that every one hour of television watching increased overall mortality by 11% and CVD mortality by 18%.98 They also noted an increase in physical injuries caused by televisions, most from flat screens falling on children or glass cuts from shattered screens. This is more common than typically thought and resulted in an average of 17,313 emergency department visits per year.99
The majority of physical activity data are self-reported survey data, with the exception of device measured steps. With the advent of wearables that measure steps, distance, and calories burned, there have been increased interest and data regarding the number of steps needed for optimal health. A large, worldwide study of more than 700,000 patients in 111 countries found the daily average steps to be 4,961. In the United States, the average steps was lower at 4,774. Step count also correlated with national obesity rates, but a stronger correlation was found in activity inequality, which was a measure of the variation in steps across the population of a country. The wider the activity inequality, the higher the obesity rate. In terms of this metric, the United States was the fourth worst country studied. Of interest, the researchers noted the activity inequality metric was mostly due to reduced steps in women.100
All the pitfalls related to self-reporting mentioned in the earlier section on diet also apply to physical activity. One approach is not to ask patients about their amount of physical activity, but to assess their degree of physical fitness, such as by administering a stress test. This changes physical activity from a soft measurement to a hard data point.
Authors of a study on cardiorespiratory fitness (CRF), self-reported physical activity, and grip strength found that increases in any and all of these three areas equated to a reduced degree of developing CVD. The strongest trends were for both measured variables with the weakest trend being self-reported physical activity.101 Measured CRF in middle age can predict not only CVD, but also overall mortality. Men in the Copenhagen male study were stratified into groups based on a bicycle ergometer test and followed for up to 46 years.102 Compared to the below-normal group, the above-normal group lived an average of 4.9 years longer.
Change in CRF is also important, as one can change his or her risk profile by becoming more fit by exercise. In a study with more than 23 years of follow-up, researchers used two separate bicycle stress tests to assess fitness in a group of healthy, middle-aged men.103 The group with the highest event rate was the “became unfit” group. Even those with high fitness at the start of the study had a 235% increase in risk of stroke and a 174% increase in risk of death if they became unfit. In contrast, those with the lowest fitness had a 60% reduction in stroke risk and a 34% reduction in death if they moved into the “became fit” group.
Authors of another study measuring CRF found significant differences in overall, cardiovascular, and cancer mortality.104 For each increase in MET (metabolic equivalent) level, there was an 11.6%, 16.1%, and a 14.0% reduction in all-cause, cardiovascular, and cancer mortality. When compared to the most fit group, the least fit group had a 73% increase in all-cause mortality and a doubling of cancer mortality.
Researchers evaluating patients on both muscular strength (based on a preset group of exercises) and aerobic fitness found that the most important factor was muscular strength, not aerobic fitness.105 Measured muscular strength also could become a difficult data point metric to both assess and track in patients.
Investigators demonstrated that increased fitness levels (able to do 10 METs) significantly attenuated patients’ 30-year CVD mortality risk across all groups of risk factor distribution.106 Obtaining a standard treadmill test for exercise prescription may become more commonplace since the population is getting less and less active and people tend to overestimate their level of physical activity. Treadmill tests also can be used to screen for CVD, measure safety of starting an exercise program, and determine prognosis.
Summary
CVD has a significant impact on our patients’ quality of life and is the leading cause of premature morbidity and mortality in the United States and worldwide. The risk factors driving the rates of CVD are well known, and it is becoming clear that lifestyle decisions drive the risk factors. Providers should recommend initiating lifestyle interventions with an individually tailored program that addresses multiple risk factors and lifestyle habits simultaneously. Lifestyle modification represents a highly effective and low-cost intervention that works synergistically with pharmacotherapy to reduce the incidence, progression, and mortality associated with CVD.
REFERENCES
- Mensah GA, Wei GS, Sorlie PD, et al. Decline in cardiovascular mortality: Possible causes and implications. Circ Res 2017;120:366-380.
- Yang Q, Tong X, Schieb L, et al. Vital signs: Recent trends in stroke death rates - United States, 2000-2015. MMWR Morb Mortal Wkly Rep 2017;66:933-939.
- Vaughan AS, Ritchey MD, Hannan J, et al. Widespread recent increases in county-level heart disease mortality across age groups. Ann Epidemiol 2017;27:796-800.
- Ruby JG, Wright KM, Rand KA, et al. Estimates of the heritability of human longevity are substantially inflated due to assortative mating. Genetics 2018;210:1109-1124.
- Li Y, Pan A, Wang DD, et al. Impact of healthy lifestyle factors on life expectancies in the US population. Circulation 2018;138:345-355.
- Khera AV, Edmin CA, Drake I, et al. Genetic risk, adherence to a healthy lifestyle, and coronary disease. N Engl J Med 2016;375:2349-2358.
- Budnitz DS, Lovegrove MC, Shehab N, et al. Emergency hospitalizations for adverse drug events in older Americans. N Engl J Med 2011;365:2002-2012.
- Chaudhury A, Duvoor C, Dendi VS, et al. Clinical review of antidiabetic drugs: Implications for type 2 diabetes mellitus management. Front Endocrinol (Lausanne) 2017;8:6. doi 10.3389/fendo.2017.00006.
- Betten DP, Castle DJ, Hughes MJ, Henney JN. Frequency of return visits to the emergency department in patients discharged following hypoglycemia episodes. Int J Emerg Med 2018;11:28. doi: 10.1186/s12245-018-0186-7.
- U.S. Food & Drug Administration. Statement from FDA Commissioner Scott Gottlieb, M.D., and Janet Woodcock, M.D., Director of the Center for Drug Evaluation and Research on FDA’s ongoing investigation into valsartan impurities and recalls and an update on FDA’s current findings. Aug. 30, 2018. Available at: https://www.fda.gov/newsevents/newsroom/pressannouncements/ucm619024.htm. Accessed Jan. 1, 2019.
- Kishimoto TK, Viswanathan K, Ganguly T, et al. Contaminated heparin associated with adverse clinical events and activation of the contact system. N Engl J Med 2008;258:2457-2467.
- Colantonio LD, Rosenson RS, Deng L, et al. Adherence to statin therapy among US adults between 2007 and 2014. J Am Heart Assoc 2019;8:e010376.
- Wang TY, Kaltenbach LA, Cannon CP, et al. Effect of medication co-payment vouchers on P2Y12 inhibitor use and major adverse cardiovascular events among patients with myocardial infarction: The ARTEMIS randomized clinical trial. JAMA 2019;321:44-55.
- Farkouh ME, Boden WE, Bittner V, et al. Risk factor control for coronary artery disease secondary prevention in large randomized trials. J Am Coll Cardiol 2013;61:1607-1615.
- Jamal A, Phillips E, Gentzke AS, et al. Current cigarette smoking among adults — United States, 2016. MMWR Morb Mortal Wkly Rep 2018;67:53-59.
- Taler SJ. Initial treatment of hypertension. N Engl J Med 2018;378:636-644.
- Merai R, Siegel C, Rakotz M, et al. CDC grand rounds: A public health approach to detect and control hypertension. MMWR Morb Mortal Wkly Rep 2016;65:1261-1264.
- Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2017. Available at: https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf. Accessed Jan. 9, 2019.
- Babey SH, Wolstein J, Diamant AL, Goldstein H. Prediabetes in California: Nearly half of California adults on path to diabetes. Policy Brief UCLA Cent Health Policy Res 2016;(PB2016-1):1-8.
- Mercado C, DeSimone AK, Odom E, et al. Prevalence of cholesterol treatment eligibility and medication use among adults — United States, 2005-2012. MMWR Morb Mortal Wkly Rep 2015;64:1305-1311.
- Brown TM, Voeks JH, Bittner V, et al. Achievement of optimal medical therapy goals for U.S. adults with coronary artery disease: Results from the REGARDS Study (REasons for Geographic And Racial Differences in Stroke). J Am Coll Cardiol 2014;63:1626-1633.
- Yang Q, Cogswell ME, Flanders WD, et al. Trends in cardiovascular health metrics and associations with all-cause and CVD mortality among US adults. JAMA 2012;307:1273-1283.
- Loprinzi PD, Branscum A, Hanks J, Smit E. Healthy lifestyle characteristics and their joint association with cardiovascular disease biomarkers in US adults. Mayo Clin Proc 2016;91:432-442.
- Lin AM, Lin MP, Markovic D, et al. Trends in cardiovascular health among US stroke survivors. Stroke 2018;50:5-12.
- GBD 2016 Lifetime Risk of Stroke Collaborators; Feigin VL, Nguyen G, Cercy K, et al. Global, regional, and country-specific lifetime risks of stroke, 1990 and 2016. N Engl J Med 2018;379:2429-2437.
- Devries S, Agatston A, Aggarwal M, et al. A deficiency of nutrition education and practice in cardiology. Am J Med 2017;130:1298-1305.
- Grabovac I, Smith L, Stefanac S, et al. Health care providers’ advice on lifestyle modification in the US population: Results from the NHANES 2011-2016. Am J Med 2018; Dec 3. pii: S0002-9343(18)31146-X. doi:10.1016/j.amjmed.2018.11.021. [Epub ahead of print].
- Teo K, Lear S, Islam S, et al. Prevalence of a healthy lifestyle among individuals with cardiovascular disease in high-, middle- and low-income countries: The Prospective Urban Rural Epidemiology (PURE) study. JAMA 2013;309:1613-1621.
- Yusuf S, Pitt B. A lifetime of prevention: The case of heart failure. Circulation 2002;106:2997-2998.
- Iestra JA, Kromhout D, van der Schouw YT, et al. Effect size estimates of lifestyle and dietary changes on all-cause mortality in coronary artery disease patients: A systematic review. Circulation 2005;112:924-934.
- Rosenbaum L, Lamas D. Facing a “slow-motion disaster” — The UN meeting on noncommunicable diseases. N Engl J Med 2011;365:2345-2348. doi: 10.1056/NEJMp1112235.
- American College of Cardiology. Special issue: CV health promotion. J Am Coll Cardiol 2018;72.
- Spring B, Ockene JK, Gidding SS. Better population health through behavior change in adults. Circulation 2013;128:2169-2176.
- Yusuf S, Hawken S, Ôunpuu S, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): Case-control study. Lancet 2004;364:11-17.
- Maron DJ, Mancini GBJ, Hartigan PM, et al. Healthy behavior, risk factor control, and survival in the COURAGE trial. J Am Coll Cardiol 2018;72:2297-2305.
- Ding D, Rogers K, van der Ploeg, et al. Traditional and emerging lifestyle risk behaviors and all-cause mortality in middle-aged and older adults: Evidence from a large population-based Australian cohort. PLoS Med 2015;12:e1001917.
- Ramírez-Vélez R, Saavedra JM, Lobelo F, et al. Ideal cardiovascular health and incident cardiovascular disease among adults: A systematic review and meta-analysis. Mayo Clin Proc 2018;93:1589-1599.
- Liu G, Li Y, Hu Y, et al. Influence of lifestyle on incident cardiovascular disease and mortality in patients with diabetes mellitus. J Am Coll Cardiol 2018;71:2867-2876.
- Joseph JJ, Bennett A, Echouffo Tcheugui JB, et al. Ideal cardiovascular health, glycaemic status and incident type 2 diabetes mellitus: The REasons for Geographic and Racial Differences in Stroke (REGARDS) study. Diabetologia 2019; Jan 15. doi: 10.1007/s00125-018-4792-y. [Epub ahead of print].
- Ng M, Fleming T, Robinson M, et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014;384:766-781.
- Bangalore S, Fayyad R, Laskey R, et al. Body-weight fluctuations and outcomes in coronary disease. N Engl J Med 2017;376:1332-1340.
- Maxey H, Bishop-Josef, Goodman B. Council for a Strong America. Unhealthy and Unprepared. National security depends on promoting healthy lifestyles from an early age. October 2018. Available at: https://strongnation.s3.amazonaws.com/documents/484/389765e0-2500-49a2-9a67-5c4a090a215b.pdf?1538407400&inline;%20filename=%22Unhealthy%20and%20Unprepared%20report.pdf%22. Accessed Jan. 16, 2019.
- Provencher MT, Chahla J, Sanchez G, et al. Body mass index versus body fat percentage in prospective National Football League athletes: Overestimation of obesity rate in athletes at the National Football League scouting combine. J Strength Cond Res 2018;32:1013-1019.
- Geserick M, Vogel M, Gausche R, et al. Acceleration of BMI in early childhood and risk of sustained obesity. N Engl J Med 2018;379:1303-1312.
- Cerhan JR, Moore SC, Jacobs EJ, et al. A pooled analysis of waist circumference and mortality in 650,000 adults. Mayo Clin Proc 2014;89:335-345.
- Huang P. A comprehensive definition for metabolic syndrome. Dis Model Mech 2009;2:231-237.
- Fryar CD, Kruszon-Moran D, Gu Q, Ogden CL. Mean body weight, height, waist circumference, and body mass index among adults: United States, 1999–2000 through 2015–2016. US Department of Health and Human Services. Centers for Disease Control and Prevention. National Health Statistics Report, 2018. Published December 20, 2018. Available at: https://www.cdc.gov/nchs/data/nhsr/nhsr122-508.pdf. Accessed Jan. 16, 2019.
- Srikanthan P, Horwich TB, Tseng CH. Relation of muscle mass and fat mass to cardiovascular disease mortality. Am J Cardiol 2016;117:1355-1360.
- Sarafrazi N, Hughes JP, Borrud L, et al. Perception of weight status in U.S. children and adolescents aged 8-15 years, 2005-2012. US Department of Health and Human Services. Centers for Disease Control and Prevention. NCHS Data Brief, 2014. Published July, 2014. Available at: https://www.cdc.gov/nchs/data/databriefs/db158.pdf. Accessed Jan. 16, 2019.
- Zdrojewicz Z, Popowicz E, Szyca M, et al. TOFI phenotype — its effect on the occurrence of diabetes. Pediatr Endocrinol Diabetes Metab 2017;23:96-100.
- Archer E, Pavela G, Lavie CJ. The inadmissibility of what we eat in America and NHANES dietary data in nutrition and obesity research and the scientific formulation of national dietary guidelines. Mayo Clin Proc 2015;90:911-926.
- Marmot MG, Syme SL, Kagan A, et al. Epidemiologic studies of coronary heart disease and stroke in Japanese men living in Japan, Hawaii and California: Prevalence of coronary and hypertensive heart disease and associated risk factors. Am J Epidemiol 1975;102:514-525.
- Kaplan H, Thompson RC, Trumble BC, et al. Coronary atherosclerosis in indigenous South American Tsimane: A cross-sectional cohort study. Lancet 2017;389:1730-1739.
- Grotto D, Zied E. The standard American diet and its relationship to the health status of Americans. Nutr Clin Pract 2010;25:603-612.
- Dehghan M, Mente A, Zhang X, et al. Associations of fats and carbohydrate intake with cardiovascular disease and mortality in 18 countries from five continents (PURE): A prospective cohort study. Lancet 2017;390:2050-2062.
- Micha R, Peñalvo JL, Cudhea F, et al. Association between dietary factors and mortality from heart disease, stroke, and type 2 diabetes in the United States. JAMA 2017;317:912-924.
- Harvard T.H. Chan School of Public Health. Healthy Eating Plate. Available at: https://www.hsph.harvard.edu/nutritionsource/healthy-eating-plate/. Accessed Jan. 19, 2019.
- Aune D, Giovannucci E, Boffetta P, et al. Fruit and vegetable intake and the risk of cardiovascular disease, total cancer and all-cause mortality—a systematic review and dose-response meta-analysis of prospective studies. Int J Epidemiol 2017;46:1029-1056.
- Miller V, Mente A, Dehghan M, et al. Fruit, vegetable, and legume intake, and cardiovascular disease and deaths in 18 countries (PURE): A prospective cohort study. Lancet 2017;390:2037-2049.
- Mente A. Higher healthy diet score: Reduced CV disease and mortality worldwide. ESC Congress. 2018.
- ONTARGET Investigators; Yusuf S, Teo KK, Pogue J, et al. Telmisartan, ramipril, or both in patients at high risk for vascular events. N Engl J Med 2008;358:1547-1559.
- O’Donnell MJ, Chin SL, Rangarajan S, et al. Global and regional effects of potentially modifiable risk factors associated with acute stroke in 32 countries (INTERSTROKE): A case-control study. Lancet 2016;388:761-775.
- Jenkins DJ, Kendall CW, Marchie A, et al. Direct comparison of a dietary portfolio of cholesterol-lowering foods with a statin in hypercholesterolemic participants. Am J Clin Nutr 2005;81:380-387.
- Satija A, Bhupathiraju SN, Spiegelman D, et al. Healthful and unhealthful plant-based diets and the risk of coronary heart disease in U.S. adults. J Am Coll Cardiol 2017;70:411-422.
- Katz DL, Meller S. Can we say what diet is best for health? Annu Rev Public Health 2014;35:83-103.
- Bao Y, Han J, Hu FB, et al. Association of nut consumption with total and cause-specific mortality. N Engl J Med 2013;369:2001-2011.
- Hu FB, Stampfer MJ, Manson JE, et al. Dietary fat intake and the risk of coronary heart disease in women. N Eng J Med 1997;337:1491-1499.
- Reynolds A, Mann J, Cummings J, et al. Carbohydrate quality and human health: A series of systematic reviews and meta-analyses. Lancet 2019;393:434-445.
- Uzhova I, Fuster V, Fernández-Ortiz A, et al. The importance of breakfast in atherosclerosis disease: Insights from the PESA study. J Am Coll Cardiol 2017;70:1833-1842.
- Yang Q, Zhang Z, Gregg EW, et al. Added sugar intake and cardiovascular diseases mortality among US adults. JAMA Intern Med 2014;174:516-524.
- Singh G, Micha R, Khatibzadeh S, et al. Estimated global, regional, and national disease burdens related to sugar-sweetened beverage consumption in 2010. Circulation 2015;132:639-666.
- Pase MP, Himali JJ, Beiser AS, et al. Sugar- and artificially sweetened beverages and the risks of incident stroke and dementia: A prospective cohort study. Stroke 2017;48:1139-1146.
- Suez J, Korem T, Zeevi D, et al. Artificial sweeteners induce glucose intolerance by altering the gut microbiota. Nature 2014;514:181-186.
- Pan A, Sun Q, Bernstein AM, et al. Red meat consumption and mortality: Results from two prospective cohort studies. Arch Intern Med 2012;172:555-563.
- Koeth RA, Wang Z, Levison BS, et al. Intestinal microbiota metabolism of L-carnitine, a nutrient in red meat, promotes atherosclerosis. Nat Med 2013;19:576-585.
- Weifei Z, Gregory JC, Org E, et al. Gut microbial metabolite TMAO enhances platelet hyperreactivity and thrombosis risk. Cell 2016;165:111-124.
- Etemadi A, Sinha R, Ward MH, et al. Mortality from different causes associated with meat, heme iron, nitrates, and nitrites in the NIH-AARP Diet and Health Study: Population based cohort study. BMJ 2017;357:j1957. doi: 10.1136/bmj.j1957.
- Estruch R, Ros E, Salas-Salvadó J, et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N Engl J Med 2013;368:1279-1290.
- Stewart RAH, Wallentin L, Benatar J, et al. Dietary patterns and the risk of major adverse cardiovascular events in a global study of high-risk patients with stable coronary heart disease. Eur Heart J 2016;37:1993-2001.
- Rao M, Afshin A, Singh G, et al. Do healthier foods and diet patterns cost more than less healthy options? A systematic review and meta-analysis. BMJ Open 2013;3:e004277. doi:10.1136/bmjopen-2013-004277.
- Piercy KL, Troiano RP, Ballard RM. The physical activity guidelines for Americans. JAMA 2018;320:2020-2028.
- Van der Ploeg HP, Chey T, Korda RJ, et al. Sitting time and all-cause mortality risk in 222 497 Australian adults. Arch Intern Med 2012;172:494-500.
- Diaz KM, Duran AT, Colabianchi N, et al. Potential effects of replacing sedentary time with short sedentary bouts or physical activity on mortality: A national cohort study. Am J Epidemiol 2018; Dec. 14. doi: 10.1093/aje/kwy271.
- Ladabaum U, Mannalithara A, Myer PA, Singh G. Obesity, abdominal obesity, physical activity, and caloric intake in U.S. adults: 1988-2010. Am J Med 2014;127:717-727.
- Li S, Zhao JH, Luan J, et al. Physical activity attenuates the genetic predisposition to obesity in 20,000 men and women from EPIC-Norfolk prospective population study. PLoS Med 2010;7. pii: e1000332. doi: 10.1371/journal.pmed.1000332.
- Ekelund U, Ward HA, Norat T, et al. Physical activity and all-cause mortality across levels of overall and abdominal adiposity in European men and women: The European Prospective Investigation into Cancer and Nutrition Study (EPIC). Am J Clin Nutr 2015;101:613-621.
- Ekblom O, Ek A, Cider Å, et al. Increased physical activity post-myocardial infarction is related to reduced mortality: Results from the SWEDEHEART Registry. J Am Heart Assoc 2018;7:e010108. doi: 10.1161/JAHA.118.010108.
- Naci H, Salcher-Konrad M, Blum MR, et al. How does exercise treatment compare with antihypertensive medications? A network meta-analysis of 391 randomised controlled trials assessing exercise and medication effects on systolic blood pressure. Br J Sports Med 2018; Dec 18. pii: bjsports-2018-099921. doi: 10.1136/bjsports-2018-099921. [Epub ahead of print].
- Murphy TP, Cutlip DE, Regensteiner JG, et al. Supervised exercise, stent revascularization, or medical therapy for claudication due to aortoiliac peripheral artery disease: The CLEVER study. J Am Coll Cardiol 2015;65:999-1009.
- Wen CP, Wai JP, Tsai Mk, et al. Minimum amount of physical activity for reduced mortality and extended life expectancy: A prospective cohort study. Lancet 2011;378:1244-1253.
- Stewart RAH, Held C, Hadziosmanovic N, et al. Physical activity and mortality in patients with stable coronary heart disease.J Am Coll Cardiol 2017;70:1689-1700.
- Schnohr P, O’Keefe JH, Marott JL, et al. Dose of jogging and long-term mortality: The Copenhagen City Heart Study. J Am Coll Cardiol 2015;65:411-419.
- Gebel K, Ding D, Chey T, et al. Effect of moderate to vigorous physical activity on all-cause mortality in middle-aged and older Australians. JAMA Intern Med 2015;175:970-977.
- O’Donovan G, Lee I, Hamer M. Association of “weekend warrior” and other leisure time physical activity patterns with risks for all-cause, cardiovascular disease, and cancer mortality. JAMA Intern Med 2017;177:335-342.
- Lahtinen M, Toukola T, Junttila MJ, et al. Effect of changes in physical activity on risk for cardiac death in patients with coronary artery disease. Am J Cardiol 2018;121:143-148.
- Kim JH, Malhotra R, Chiampas G, et al. Cardiac arrest during long-distance running races. N Engl J Med 2012;366:130-140.
- Lee DC, Brellenthin AG, Thompson PD, et al. Running as a key lifestyle medicine for longevity. Prog Cardiovasc Dis 2017;60:45-55.
- Dunstan DW, Barr EL, Healy GN, et al. Television viewing time and mortality: The Australian Diabetes, Obesity and Lifestyle Study (AusDiab). Circulation 2010;121:384-391.
- De Roo AC, Chounthirath T, Smith GA. Television-related injuries to children in the United States, 1990-2011. Pediatrics 2013;132:267-274.
- Althoff T, Sosic R, Hicks JL, et al. Large-scale physical activity data reveal worldwide activity inequality. Nature 2017;547:336-339.
- Tikkanen E, Gustafsson S, Ingelsson E. Associations of fitness, physical activity, strength, and genetic risk with cardiovascular disease: Longitudinal analyses in the UK Biobank Study. Circulation 2018;137:2584-2591.
- Clausen JSR, Marott JL, Holtermann A, et al. Midlife cardiorespiratory fitness and the long-term risk of mortality: 46 years of follow-up. J Am Coll Cardiol 2018;72:987-995.
- Prestgaard E, Hodnesdal C, Engeseth K. Long-term predictors of stroke in healthy middle-aged men. Int J Stroke 2017;13:292-300.
- Imboden MT, Harber MP, Whaley MH, et al. Cardiorespiratory fitness and mortality in healthy men and women. N Engl J Med 2018;72:2283-2292.
- Artero EG, Lee DC, Ruiz JR, et al. A prospective study of muscular strength and all-cause mortality in men with hypertension. J Am Coll Cardiol 2011;57:1831-1837.
- Wickramasinghe CD, Ayers CR, Das S, et al. Prediction of 30-year risk for cardiovascular mortality by fitness and risk factor levels: The Cooper Center Longitudinal Study. Circ Cardiovasc Qual Outcomes 2014;7:597-602.
Lifestyle is a critical determinant of the common risk factors for cardiovascular disease (hypertension, diabetes, hyperlipidemia, and smoking) that have been well-known to predict disease outcomes. Lifestyle medicine can be used in conjunction with traditional medications to provide the best care to patients. Clinicians need to act now to prevent being overwhelmed with the eventual increase in coronary artery disease following the obesity/diabetes epidemic.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
