Why Is the QRS Wide?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The ECG in the figure below belongs to an older woman who called EMS because of new-onset chest pain. How might one interpret the tracing? Why is the QRS complex wide?
The rhythm is sinus at ~85 beats/minute. The QRS complex is wide. QRS morphology is consistent with complete left bundle branch block (LBBB) in that there is a monophasic R wave in left-sided leads I and V6 and a predominantly negative QRS complex in right-sided lead V1.
Much of the time, a diagnosis of acute myocardial infarction (MI) will be more difficult in the setting of complete LBBB. That said, there are instances in which definitive diagnosis of an acute ST-segment elevation MI (STEMI) is possible. The ECG in the figure is one of those instances. Typically, with either left or right bundle branch block, the direction of the ST-T waves in the three key leads (I, V1, and V6) will be opposite the last QRS deflection. For example, since the QRS complex in left-sided leads I and V6 is all upright when there is complete LBBB, we expect the ST-T wave to be oppositely directed, or negative. Instead, there is subtle-but-real ST elevation in lead V6. Leads V4 and V5 exhibit an even more abnormal appearance. That is, there is frank ST elevation in lead V5, which should not be there, and the T wave in lead V4 is hyperacute (disproportionately tall, fatter than expected at its peak, and unusually wide at its base). Similar hyperacute changes can be observed for the ST-T waves in each inferior lead. Although more subtle in leads III and aVF, there is little doubt that the ST-T wave in lead II is disproportionately tall, fatter than expected at its peak, and much wider than expected at its base.
This patient was in process of evolving a large acute inferoposterolateral STEMI, with development of this new LBBB just minutes after the initial ECG was recorded. The patient was taken to the cardiac catheterization lab soon after arrival at the hospital. The “culprit” artery was the obtuse marginal branch of the left circumflex artery.
For more information and further discussion on this case, please visit: http://bit.ly/2Zheqjh.
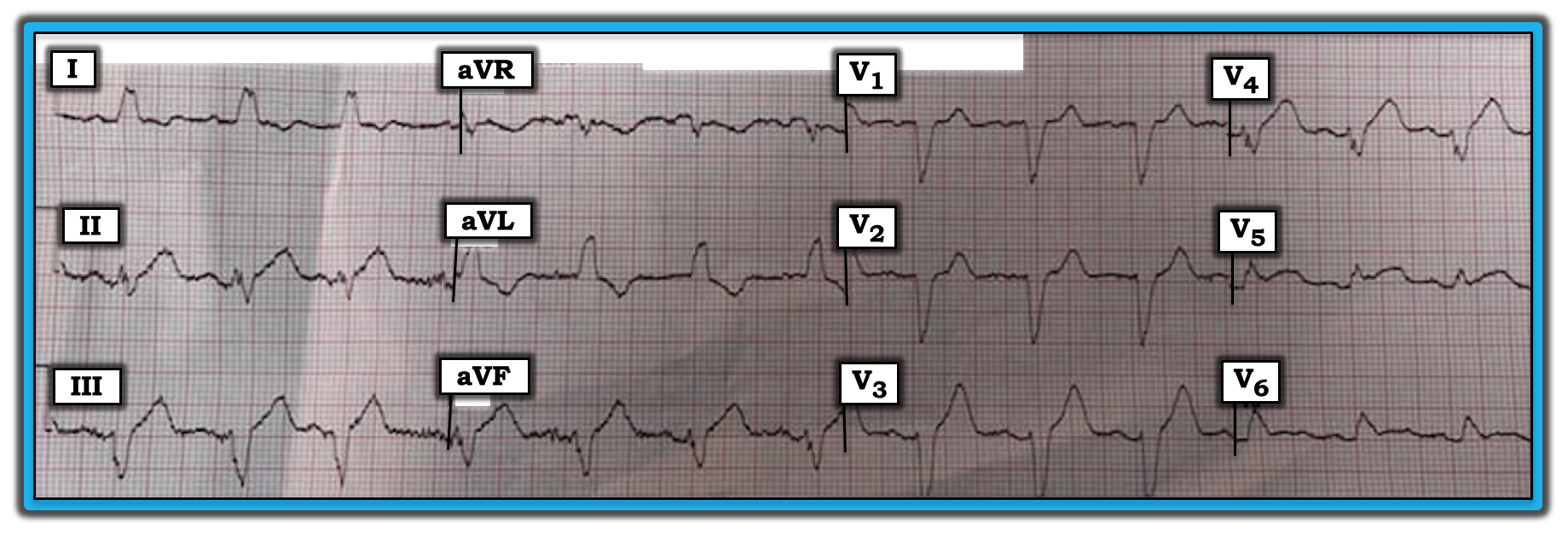
The ECG in the figure belongs to an older woman who called EMS because of new-onset chest pain. How might one interpret the tracing? Why is the QRS complex wide?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
