Methamphetamines in the Emergency Department: Part of the Drug Epidemic
December 15, 2019
Reprints
AUTHORS
Amy Young, MD, Department of Emergency Medicine, University of Texas Southwestern, Dallas
Stephanie T. Weiss, MD, PhD, Addiction Medicine Research Fellowship Program, Wake Forest School of Medicine, Winston-Salem, NC
Brett A. Roth, MD, FACEP, FACMT, FASAM, Clinical Professor, Department of Emergency Medicine, University of Texas Southwestern, Dallas; Medical Director, North Texas Poison Center
Larissa Velez, MD, Associate Dean for Graduate Medical Education, Vice Chair for Education, Department of Emergency Medicine, University
of Texas Southwestern Medical Center, Dallas
PEER REVIEWER
Frank LoVecchio, DO, MPH, FACEP, Professor of Emergency Medicine, Associate Medical Director, Banner Poison and Drug Information Center, Phoenix, AZ
EXECUTIVE SUMMARY
• Methamphetamine, also known as meth, ice, and crystal meth, is an important drug of abuse, implicated in or contributing to more than 8,000 annual deaths in the United States. There are more than 750,000 users of methamphetamine in the United States.
• Methamphetamine can be inhaled, taken orally, or taken intravenously. Its effect lasts about eight hours.
• Drug testing has variable results, with many false-positive and false-negative results.
• Methamphetamine can cause an acute “fight or flight” reaction in lower doses, with diaphoresis, mydriasis, nausea, and tachycardia. In higher doses, psychosis and paranoia may occur, along with hyperthermia, cardiotoxicity (including hypertension, coronary vasospasm, and aortic dissection), neurotoxicity (seizures, stroke), and acute renal disease (rhabdomyolysis, vasospasm).
• Treatment is primarily with benzodiazepines.
I recently moved from the Northeast to the Southwest. Although I had seen quite a few patients on meth in the Northeast, I was a bit shocked at the prevalence of meth, and the amount of toxicity, seen in my new location. One of my first patients was an elderly woman who had been “doing meth” all day with her friends. She presented with hyperthermia, acute renal failure with hyperkalemia, multiple dysrhythmias, hypotension, and mesenteric infarction. Despite aggressive treatment, she eventually died, and I became a bit more impressed with the toxicity of this drug. Even though we have been focused on the opioid epidemic, it is important to remember there are other drugs, such as meth, that lead to death and long-term disability.
— Sandra Schneider, MD, FACEP, Editor
Introduction
Amphetamines belong to the beta-adrenergic stimulant class of drugs that includes cocaine, ephedrine, and the cathinones. Methamphetamine is a Controlled Substances Act (CSA) Schedule II amphetamine derivative with limited medical indications (i.e., treatment of obesity and attention deficit hyperactivity disorder) and high abuse potential. Methamphetamines are currently some of the most widely abused substances in the United States, behind alcohol, tobacco, and marijuana.1 The problem is not limited to the United States; methamphetamine abuse is a growing worldwide problem.2
Psychostimulant is a term used in forensic sciences to describe amphetamine derivatives that have both hallucinogenic and stimulant effects. These substances, which include the cathinones and methylenedioxymethamphetamine (MDMA), will not be discussed here in detail. This review will focus on the history, epidemiology, pharmacology, toxicity, testing, management, and legal issues surrounding methamphetamine, as well as some of its CSA Schedule I psychostimulant derivatives.
Discovery
Ephedra, the botanic extract of Ephedra sinica, has been used in traditional Chinese medicine and called ma huang for more than 5,000 years. In 1885, ephedrine, the active alkaloid present in ephedra, was chemically extracted and studied. The search for a synthetic substitute for ephedrine resulted in the development of amphetamine-type stimulants, which were produced through modification of the ephedrine skeleton. Amphetamine was first synthesized in 1887 in Germany by Romanian chemist Lazăr Edeleanu. Subsequently, in 1919 Japanese chemist Akira Ogata synthesized methamphetamine using ephedrine as a precursor.3 Initial pharmaceutical goals at the time included central nervous system (CNS) stimulation, bronchodilation, and nasal vasoconstriction.
History and Emergence as a Drug of Abuse
Early amphetamine use was primarily via nasal insufflation when it was first marketed by Smith, Kline, and French in 1932 as the nasal decongestant Benzedrine.4 During World War II, both amphetamine and methamphetamine were supplied as stimulants for soldiers and prisoners of war. Amphetamines were used to increase alertness, reduce fatigue, and suppress the appetite of soldiers. World leaders, including Adolf Hitler and later President John F. Kennedy, were said to have received frequent doses of methamphetamines administered by well-intending physicians.
As the stimulant and euphoric effects were recognized, amphetamine abuse became increasingly problematic, with early reports starting in 1940. Amphetamine pills, or “pep pills,” were sold for nonmedical purposes and, during that time, they were used as “diligent drugs” to enhance workers’ performance.5
From 1950 to the 1970s, sporadic periods of widespread amphetamine use and abuse occurred in the United States. It has been estimated that in 1958 legal pharmaceutical production of amphetamine was 3.5 billion tablets, or enough to supply every person in the United States at the time with 20 standard doses.6 Prescriptions of amphetamine peaked in 1967 to 31 million. By 1970, amphetamine production had increased to 10 billion tablets. In addition to prescriptions, amphetamines also were sold on the black market.
In the 1960s, the term “speed freaks” was used to describe high-dose compulsive users in the Haight-Ashbury district of San Francisco. These high-dose users often exhibited hyperactivity and paranoia.7 Methamphetamine became known as a “biker drug” in the 1960s and 1970s. Illegal manufacture and distribution by biker gangs, such as the Hell’s Angels along the Pacific Coast, contributed up to 90% of the methamphetamine produced in the United States in the 1970s and 1980s, as diversion of legally produced methamphetamines became more difficult. The nickname “crank” originated from the practice of transporting methamphetamine in the crankcases of motorcycles.1 Abuse was primarily via the intranasal route. Over the years, and depending on the country and the region, methamphetamine has been known by a variety of slang terms. Table 1 summarizes these slang names.
Table 1. Methamphetamine Slang Terms |
|
|
Meth Speed Ice Crystal meth Glass Go fast Crank Stove top Yaba Tina Shabu Shisheh Batu |
Dimethylphenethylamine Methedrine Desoxyn Chalk Poor man’s cocaine Tweak Tik Uppers Trash Yellow barn Methlies quick Biker’s coffee Black beauties |
|
Adapted from: Vearrier D, et al. Methamphetamine: History, pathophysiology, adverse health effects, current trends, and hazards associated with the clandestine manufacture of methamphetamine. Dis Mon 2012;58:38-89. |
|
In the 1960s and early 1970s, various amphetamine derivatives, such as methylenedioxyamphetamine (MDA), para-methoxyamphetamine (PMA), and para-methoxymethamphetamine (PMMA), gained popularity because of their additional hallucinogenic properties.8,9 The Controlled Substances Act of 1970 listed amphetamines as Schedule II to prevent the diversion of pharmaceutical amphetamines for non-medicinal uses. Abuse of amphetamines subsequently declined in the 1970s and early 1980s.
However, in the mid-1980s, illicit production increased. During this period, a new form of methamphetamine called “ice” or “crystal meth” became available. This methamphetamine hydrochloride could be smoked, which resulted in an almost immediate onset of euphoria popular among its users. The new epidemic started in West Honolulu and, over time, expanded to the West Coast and throughout the United States.1,10 Increased demand resulted in an expansion of manufacturing practices. In areas with sufficient illicit drug infrastructure and high demand, such as the Central Valley of California, organized networks of “super labs” and distributors predominated. In rural areas with infrastructure that was less established, the methamphetamine was produced by local “cooks.” The ease and low cost of methamphetamine synthesis using easily available precursors encouraged the establishment of illegal clandestine laboratories throughout the United States.4
More legislation was passed, including the Methamphetamine Control Act of 1996, to strengthen penalties on the precursors used in production. The Combat Methamphetamine Epidemic Act of 2005 was passed to regulate the purchase of products containing the methamphetamine precursors pseudoephedrine, ephedrine, and phenylpropanolamine. Retail purchases of pseudoephedrine in the United States are currently limited to a maximum of 3.6 g per day. Clandestine lab manufacturers would circumvent these restrictions by “smurfing” or sending multiple people to purchase pseudoephedrine at different retail locations.4
Production
Methamphetamine is prevalent and widely available. Most of the methamphetamine in the United States is produced in Mexico and smuggled across the southwest border by transnational criminal organizations.11 Production in the United States occurs at much lower levels than in Mexico, and seizures of domestic methamphetamine laboratories have declined steadily for many years. Corresponding seizures of methamphetamine along the southwestern border of the United States have increased steadily.12
The Mexican drug cartels traffic both methamphetamine and its precursors into the United States. This is the result of tighter pressures on domestic production and the ease with which cartels are able to purchase precursor chemicals from India, Germany, China, and other countries with less strict oversight. Nearly all of the methamphetamine nationwide is produced in Mexico now through super labs using phenyl-2-propanone (PCP).13 Globally, the methamphetamine market also has undergone remarkable changes in the past decade, going from a market where manufacture was concentrated in specific subregions to a market with global trafficking flows and global seizure quantities growing more than six times since 2008.14
Analysis of domestic methamphetamine purchases from January 2012 through March 2017 indicates that the price per pure gram of methamphetamine decreased from $81 to $70, a decline of 13.6%. The purity (measured by the amount of any chiral form of methamphetamine) and potency for methamphetamine (measured by the amount of the highly potent d-isomer present) both have reached all-time peaks of approximately 95%.12
Methamphetamine Emergence/Epidemiology
Methamphetamine is widely available throughout the United States, with the highest availability in the West and Midwest. Recently, methamphetamine prevalence has been increasing in areas such as the Northeast that historically have not been major markets for the drug.15
Data from the 2017 National Survey on Drug Use and Health (NSDUH) show that about 774,000 people 12 years of age and older were current methamphetamine users in 2017, about 0.3% of the population.16 Data from 2017 show a significant increase in rates compared to the 2016 NSDUH, which showed that 667,000 people 12 years of age and older were current methamphetamine users.
Globally, amphetamine-type stimulants are the second most widely used drugs after cannabis, with use levels often exceeding those of heroin and/or cocaine. Along with amphetamines, the continued growth of the new psychoactive substances (NPS) marketed over the last several years has become a policy challenge and a major international concern.14
Mortality
Among all 2017 drug overdose deaths in the United States, 10,333 (14.7%) involved psychostimulants.17 Eighty-five percent of such deaths included a mention of methamphetamine.12
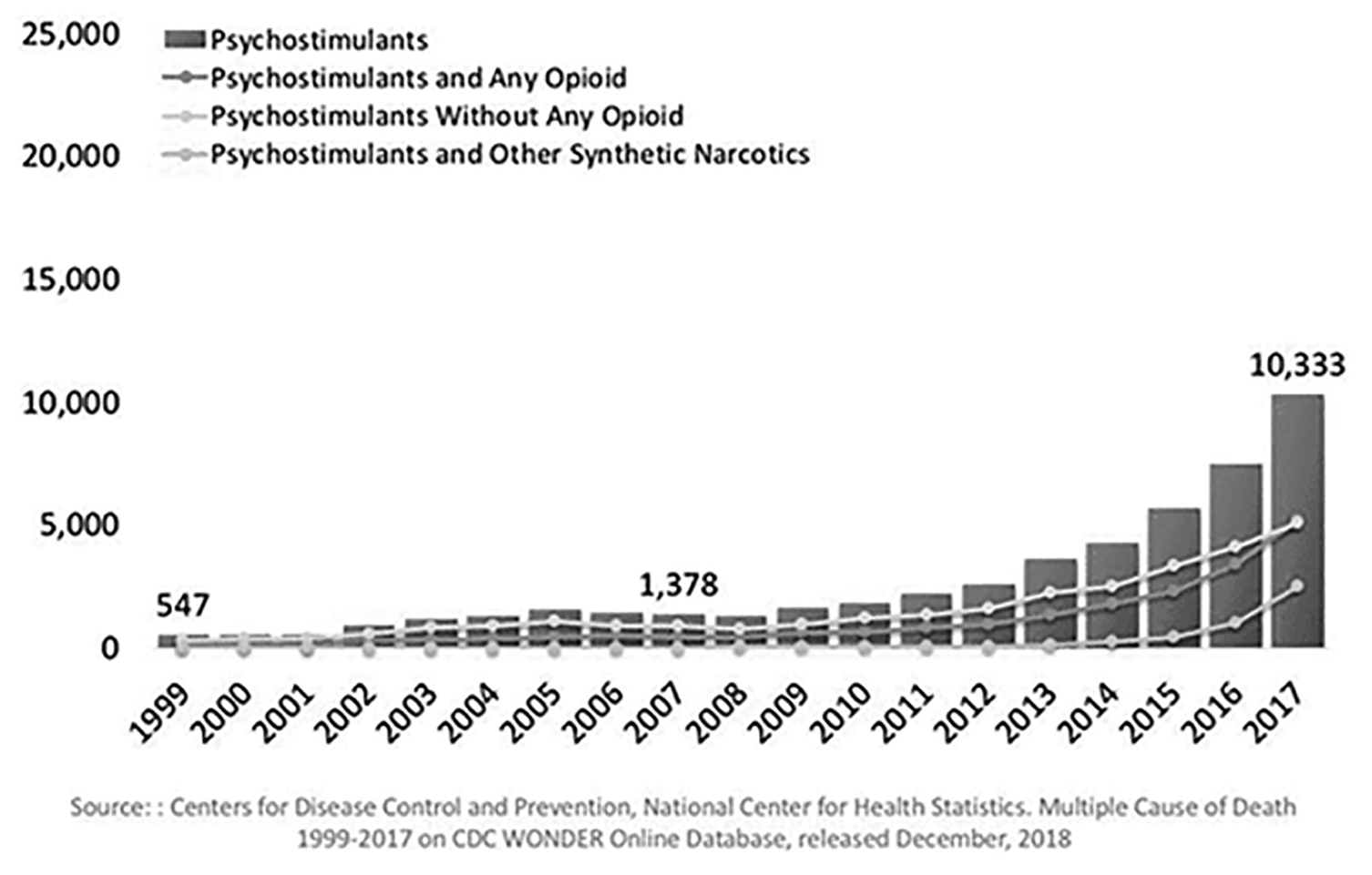
Recent Centers for Disease Control and Prevention (CDC) statistics examining changes in trends during 2003-2017 indicated that overdose death rates involving psychostimulants remained stable from 2003 to 2010, then increased annually by 29% from 2010 to 2017. (See Figure 1.) Increasing death rates reflect greater availability, increased use rates, as well as increased purity (> 90%) and low cost. Death rates also are affected by mixing potent opioids with psychostimulants. In 2017, opioids were involved in 50% of psychostimulant-involved overdoses, suggesting that increases in psychostimulant overdose deaths from 2012 to 2017 were driven primarily by synthetic opioids. Current findings support that increases in stimulant-involved deaths are part of a growing polysubstance landscape that includes opioids.17-19
Figure 1. National Drug Overdose Deaths Involving Pyschostimulants With Abuse Potential (Including Methamphetamine), by Opioid Involvement; Number Among All Ages, 1999-2017 |
 |
|
Source: Centers for Disease Control and Prevention, National Center for Health Statistics. Multiple Cause of Death 1999-2017 on CDC WONDER Online Database, released December 2018 |
Pharmacology and Toxicology of Methamphetamine
Both amphetamine and methamphetamine are chiral compounds with two enantiomers (mirror images) that have distinct pharmacological profiles.20 The levo (l) isomers of amphetamine and methamphetamine are much less active in the CNS than the dextro (d) isomers are, which is why the l-isomers may be found in pharmaceutical preparations such as Vick’s inhalers.20-22
Pharmacokinetics
Significant absorption of methamphetamine can occur via the inhalational, oral, or intravenous (IV) routes. Time to achieve peak serum concentrations is rapid via the inhaled or IV routes, with detectable cardiovascular and subjective effects occurring within two minutes after IV infusion of methamphetamine.23 The half-life of methamphetamine is estimated to be about 10-12 hours, but this is variable, based on chronicity and heaviness of use.23-25 Acute effects typically persist for up to eight hours after a single moderate dose of methamphetamine.25
One of the most important metabolic pathways for methamphetamine involves its conversion to amphetamine via N-dealkylation.22,25 Thus, patients who take methamphetamine also will have amphetamine present. In addition, amphetamines are metabolized in part by the polymorphic cytochrome CYP2D6 enzyme, which raises the possibility of increased toxicity in users who are poor CYP2D6 metabolizers or who are taking medications, such as fluoxetine or paroxetine, that are CYP2D6 enzyme inhibitors.20 It has been estimated that more than 7% of black and white Americans may be poor CYP2D6 metabolizers,26 and the polymorphism in this enzyme has been proposed as an explanation for why certain patients are more susceptible to methamphetamine toxicity.20,25
Mechanisms of Action
Methamphetamine is thought to increase the synaptic concentrations of dopamine, serotonin, and norepinephrine indirectly by several mechanisms, including increased neurotransmitter (NT) release from presynaptic nerve terminals and decreased NT reuptake from the synapse. Increased NT release occurs because amphetamines compete with dopamine, serotonin, and norepinephrine for their respective NT reuptake transporters. In addition, amphetamines block vesicular uptake of dopamine and increase vesicular release of dopamine into the cytoplasm, which increases the pool of cytoplasmic dopamine available to be transported out of the neuron.20,24,25,27
Many of the clinical effects of amphetamines also can be explained via these mechanisms, although in some cases there are other likely factors at work as well. For example, amphetamine-induced psychosis is thought to be due primarily to increased release of serotonin and dopamine. The mechanism of the hyperthermia caused by amphetamines is not entirely understood, but it may be secondary to serotonin syndrome and/or dopaminergic excess along with muscular heat generation. In contrast, the cause of the liver injury sometimes seen with amphetamine use may be due to the generation of reactive oxygen species, and the cause of amphetamine-induced rhabdomyolysis is likely multifactorial relating to agitation, hyperthermia, and seizures. The cause of poor dental hygiene or “meth mouth” seen in chronic methamphetamine users is not well understood but can be due to a combination of xerostomia, bruxism, increased carbohydrate intake, and poor dental hygiene.20
Testing and Diagnosis
In general, emergency clinicians should not rely on the results of urine drug screens (UDS) to diagnose patients with methamphetamine or amphetamine toxicity, as the results of these tests are preliminary and are subject to many external variables that can affect the results.21,22 For example, the amount of parent amphetamines and metabolites that are excreted in the urine varies according to the urine pH.22 Because of the poor correlation between UDS results and clinical presentation, the diagnosis of amphetamine toxicity should be based primarily on the patient’s history and clinical presentation. A discussion of several of the major pitfalls of UDS testing along with recommendations for correctly interpreting UDS results follow.
Pitfalls of ED Testing
False Positives
UDS screens, which are immunoassay-based technology, are not adequately specific to confirm the use of amphetamines.20 Most UDS screens use an antibody that has been designed to bind to the chemical structure of amphetamines.20,21 Since many other compounds besides methamphetamine and amphetamine have the phenethylamine structural backbone of amphetamines, false-positive results for amphetamines on UDS screens due to pharmaceutical compounds with similar structures, such as the over-the-counter decongestant pseudoephedrine, are extremely common.20,21 Some illicit drugs, such as 3,4-methylenedioxymethamphetamine (MDMA), also may react with the immunoassay antibodies and give a positive UDS result.20 One study that evaluated the positive predictive value (PPV) of a UDS for amphetamines found that the PPV was only 74.1%.21
True Positives for Prescribed Drugs
Some legally prescribed pharmaceuticals are metabolized to l-methamphetamine and/or l-amphetamine in vivo.20,22 This may result in a true positive UDS result that is not due to illicit drug use. Notably, patients who are taking legally prescribed amphetamines (brand names Dexedrine and Adderall) or methamphetamine (brand name Desoxyn) for conditions such as attention deficit hyperactivity disorder (ADHD) will test positive for amphetamines on a UDS. Some less prevalent agents, such as the anti-Parkinson’s disease drug selegiline (also called deprenyl, brand name Eldepryl) and the anorectant benzphetamine (brand name Didrex) are metabolized to l-methamphetamine, l-amphetamine, or both and also will test positive on the UDS.22
Table 2 provides a sampling of pharmaceutical agents that can cause both true-positive and false-positive results for amphetamines on a UDS that are not due to illicit drug use. This list is not exhaustive, and many other compounds also have been reported to potentially cause false-positive results for amphetamines on UDS. Clinicians should check with their hospital laboratory for further information on pharmaceuticals and other compounds that are known to cause false-positive results for amphetamines on the particular UDS immunoassay being used at their institution.
Table 2. Common Agents That Can Cause Positive Results for Amphetamines on Urine Drug Screen Not Due to Illicit Drug Use21,22 |
|
|
Pharmaceuticals Causing True Positive Results on Urine Drug Screen Not Due to Illicit Drug Use |
Common Pharmaceuticals Causing False-Positive Results on Urine Drug Screen |
|
|
False Negatives
A positive UDS test result occurs when the concentration of the drug in the urine is greater than a predetermined cutoff value. Urine drug levels of amphetamine or methamphetamine that are lower than the cutoff value will be reported as negative even if the drug is present in low amounts.20,21 As of 2017, the current U.S. Substance Abuse and Mental Health Services Administration cutoff for the presence of amphetamine and methamphetamine in initial UDS testing of federal employees is 500 ng/mL, but hospital UDS cutoff levels may vary by institution.28 Another caveat is that UDS cutoff levels may not be accurate in children since children have more dilute urine than adults.21
Noncorrelation of Testing With Clinical Presentation
Even in the event of a true positive UDS result, a patient’s clinical presentation may not be related to the presence of amphetamines in the urine.21 Also, there is no consistent relationship between the levels of amphetamines in blood or urine and the degree of patient intoxication. Therefore, the results of drug testing always must be correlated to the patient’s clinical presentation and history.20 Clinicians should be aware that amphetamine and methamphetamine may be detected in the urine for two to seven days after use, which may be long after the clinical effects of the drug have resolved.21,25
Interpretation of Positive Results and Confirmatory Testing
Given the potentially serious repercussions of a false-positive UDS result, such as job loss or loss of child custody, confirmatory testing with gas chromatography-mass spectrometry (GC-MS) should be performed in any case in which an accurate drug testing result is needed.22 Although there still is a potential for false positives or false negatives, GC-MS is extremely sensitive and specific.20-22 GC-MS techniques also are available for investigating whether a positive UDS is due to l-amphetamines, d-amphetamines, or both.20,21 The downsides of using GC-MS are that it is costly and time-consuming compared to a UDS immunoassay,20,21 and many clinicians may not have ready access to this type of testing in a clinically relevant timeframe.
Acute Methamphetamine Toxicity
Methamphetamine causes a rapid onset of symptoms and sustained duration of action. This causes a sympathomimetic toxidrome or the classic “fight-or-flight response.” Diaphoresis, mydriasis, nausea, tachypnea, and tremor can result.
The effects of methamphetamine at the low-to-moderate methamphetamine doses (5-30 mg) include arousal, positive mood, cardiac stimulation, improved attention, and psychomotor coordination. Doses used by illicit users typically are ≥ 50 mg and can produce psychosis. Rapid or confused speech, dilated pupils, agitation, paranoia, rapid pulse, sweating, nervousness, and motor restlessness were noted commonly with plasma levels exceeding 100 mcg/L. Further stimulation of the nervous system can result in cardiotoxicity as well as neurotoxicity, including dysrhythmias, vasospasm, tachycardia, agitation, hyperthermia, strokes, and seizures.
The initial evaluation of the methamphetamine-toxic patient must include a full set of vital signs, including temperature, as soon as safe and feasible. To achieve this, temporary physical restraints, rapidly followed by IV administration of sedatives, might be necessary. In general, IV benzodiazepines are the first-line agents.29 Large doses may be necessary to achieve adequate sedation.
Cardiovascular Toxicity
Cardiovascular complications from methamphetamine use can occur and are potentially lethal. High catecholamine levels are known to be cardiotoxic due to increased myocardial demand combined with a reduced oxygen supply. Methamphetamines cause dysrhythmias, hypertension, aortic dissection, and coronary vasospasm acutely.30 Long-term methamphetamine use can cause structural changes to the myocardium, including necrosis, fibrosis, and hypertrophy of cells.31 Sinus tachycardia is the most common dysrhythmia in methamphetamine use that requires treatment with sedation, volume resuscitation, and temperature control. Sedation with benzodiazepines will reduce the intrasynaptic catecholamine surge to control cardiac effects, including tachycardia and hypertension. Ventricular tachycardia, ventricular fibrillation, and QT prolongation can occur, resulting in sudden cardiac death. Standard advanced cardiac life support measures should be followed, including antidysrhythmics, cardioversion, and defibrillation.
Treatment with a titratable dihydropyridine calcium channel blocker, such as nicardipine or nifedipine, may be helpful for vasospasm, aortic dissection, or hypertension. Alpha-antagonists, such as phentolamine and nitrates, also can be used as antihypertensives. Benzodiazepines also can assist with controlling hypertension. Until further study, beta-antagonists should be used with caution in patients with
amphetamine-induced myocardial ischemia because of the potential for coronary vasospasm from unopposed alpha-adrenergic activity, similar to what is seen with cocaine.32
Cardiomyopathy, cardiac ischemia, and coronary infarction are additional cardiovascular concerns in the methamphetamine abuser. Cardiomyopathy can occur in patients who use oral, IV, and smoked forms of methamphetamine. Methamphetamine users have a 3.7-fold increased risk of cardiomyopathy, and the associated left ventricular dysfunction is more severe compared with other patients with cardiomyopathy.33 Similar to cocaine, methamphetamine can cause platelet aggregation and coronary vasospasm. Methamphetamine use is a common risk factor for acute aortic dissection after hypertension.34,35
Central Nervous System Toxicity
Methamphetamine causes excessive stimulation of the sympathetic nervous system. Acute neurologic complications associated with methamphetamine abuse include strokes, seizures, agitation, and hyperthermia.36 Seizures should be treated initially with benzodiazepines. If seizures persist, consider phenobarbital, dexmedetomidine, or propofol with airway protection as needed.
Continued seizure activity that is unresponsive to benzodiazepines and barbiturates should be controlled with neuromuscular blockade, particularly if hyperthermia is occurring. Electroencephalographic monitoring for seizure activity is important in these situations. Phenytoin likely will be ineffective in toxin-induced seizures.
The most commonly reported vascular complication of amphetamine abuse is cerebrovascular hemorrhage. Reports of acute aortic dissection, pulmonary hypertension, ruptured berry aneurysm, and sudden death have occurred. A neurologic exam is important in these patients. If there are focal neurologic deficits or significant alterations in mental status, a computed tomography scan of the head is indicated to evaluate for intracranial bleeding or infarction.
Sexual Health Risks and Renal Effects
Methamphetamine use has been implicated in the term “chemsex,” in which users engage in sexual encounters while intoxicated to enhance the sexual experience.37 This has resulted in increased rates of sexually transmitted diseases and of genital and rectal trauma.
Methamphetamine can cause renal injury from prolonged agitation and seizures (both leading to rhabdomyolysis). Prolonged vasoconstriction of intramuscular arteries can contribute, causing acute kidney injury associated with rhabdomyolysis. Renal failure without rhabdomyolysis is reported secondary to renal artery vasoconstriction. Chronic use of methamphetamine with prolonged hypertension or dehydration with decreased urine output can be associated with renal failure as well. Adequate hydration and urine output can be maintained with intravenous fluids. In general, urinary alkalinization with bicarbonate infusion should be avoided, as this impairs renal clearance of the methamphetamine.38 Urinary acidification can increase amphetamine elimination, but its inherent risks always outweigh the benefits. Table 3 summarizes acute complications of methamphetamine use.
Table 3. Acute and Chronic Effects of Methamphetamines |
||||
|
Cardiovascular |
Central Nervous System |
Respiratory |
Other |
|
| Acute toxicity | ||||
|
|
|
|
|
| Chronic toxicity | ||||
|
|
|
|
|
|
IVDU = Intravenous drug use Adapted from: Rusyniak DE. Neurologic manifestations of chronic methamphetamine abuse. Psychiatr Clin North Am 2013;36:261-275. |
||||
Chronic Methamphetamine Toxicity
Methamphetamine depletes the brain stores of dopamine with repeated use. Users eventually will have anhedonia and develop depression. They can develop a “washout syndrome” from catecholamine depletion, leading to fatigue and hypotension. Cognitive motor activities or fine-motor dexterity can be affected in chronic methamphetamine abusers.39 Methamphetamines are a risk factor for the development of Parkinson’s disease and other movement disorders.40
Formication is an example of chronic methamphetamine psychosis. These tactile hallucinations can be a risk factor for methicillin-resistant Staphylococcus aureus skin infections, since patients compulsively scratch and pick at their skin.25
Dry mouth also can occur in these patients that can lead to bruxism and tooth fracture.41 Dental caries, tooth erosion, tooth loss, and tooth fractures are seen with what has been termed “meth mouth” in many chronic methamphetamine abusers.42
Methamphetamine users often suffer from poor nutrition, leading to dramatic changes in physical appearance in short periods of time.
Abrupt cessation of repeated methamphetamine use leads to withdrawal syndrome consisting of depressed mood, anxiety, and sleep disturbance. Acute methamphetamine withdrawal can last seven to 10 days.25 Table 3 summarizes the chronic complications of methamphetamine use.
Management and Disposition
Management of a methamphetamine overdose is largely supportive. As mentioned before, sedation very often is needed. Aggressive active cooling is necessary for all hyperthermic patients. With methamphetamine, hyperthermia is a marker of significant toxicity. Mortality and severe outcomes are correlated with elevated temperatures in methamphetamine “body stuffers.”43 Antipsychotics have not been shown to be as effective as benzodiazepines in experimental models. These agents lower the seizure threshold, alter temperature regulation, and cause acute dystonia and cardiac dysrhythmias. However, they can be used selectively in patients with no agitation but who exhibit psychiatric symptoms, such as paranoia and psychosis.44
Table 4 lists the indications for intensive care unit (ICU) admissions.
Table 4. General Indications for Intensive Care Unit Admission |
|
|
|
|
Adapted from: Connors NJ, Hoffman RS. Amphetamines and their derivatives. In: Brent J, Burkhart K, Dargan P, et al. Critical Care Toxicology: Diagnosis and Management of the Critically Poisoned Patient. Switzerland: Springer International Publishing; 2017:1413-1438. |
|
Gastrointestinal decontamination is not needed frequently, since many patients have used the intravenous or inhalational route. However, in body packers or stuffers, gastrointestinal decontamination may be helpful.43 Gastric lavage has no benefit and should not be used. Activated charcoal administration has not been shown to improve outcomes, but it is perhaps the most reasonable decontamination alternative for asymptomatic patients with body packets. However, there is a risk of seizures with methamphetamine toxicity that may result in intubation. Aspiration of charcoal will limit the view of the airway, making this a difficult procedure if activated charcoal has already been given.
Other Issues and Indirect Effects
- Agitation in EMS: Methamphe-tamine causes agitation and paranoia, and these patients might become violent.45 Police assistance and sedation might be necessary prior to transport.
- Fire and explosions in methamphetamine laboratories: Regional burn centers have been reporting increased incidence of burn cases as a result of fires and explosions in the illicit manufacture of methamphetamine.46 In at least one burn center report, these patients had higher surface area of burns, tended to have more inhalational injury associated, and had higher morbidity.47,48 Ocular burns also have been reported widely in the literature.49
- Child abuse and neglect: The use of methamphetamine in parents and caregivers has been associated with increased rates of child abuse and neglect.50 On occasion, accidental pediatric ingestions of corrosives used in the manufacturing process have resulted in injuries and death.51
- Intimate partner violence (IPV): At least one study has shown high rates of methamphetamine use among perpetrators of IPV.52
- Police reports of symptoms during investigations of meth labs: Police investigators report symptoms such as headaches, sore throat, respiratory symptoms, and CNS symptoms.53 It is recommended that investigators and others entering these areas wear appropriate personal protective equipment.54
- Other phenylethylamines: Methamphetamine belongs to a large family of phenylethylamines. These agents have many toxicities, which are listed in Table 5.
Table 5. Related Amphetamines |
||
|
Name |
Slang Names |
Toxicity |
|
MDMA55 |
Ecstasy, Molly, E, Adam, XTC |
Acute: Hyponatremia, seizures, serotonin syndrome, restlessness, hyperthermia, rhabdomyolysis, disseminated intravascular coagulation Chronic: Damage/loss of serotonergic neurons |
|
MDEA |
Eve |
|
|
MDA |
Love drug |
|
|
Cathinones |
Bath salts, Khat |
Acute: Agitation/excited delirium |
|
Synthetic cathinones: MDPV56 Alpha-PVP Alpha-PPP Mephedrone/4-MMC 3-MMC Naphyrone (O-2482)57 |
PVP = Flakka, gravel Mephedrone/4-MMC = meow meow, MCAT, meph, drone, M-smack |
Acute: Agitation/excited delirium, psychosis, hyperthermia, sympathetic stimulation |
|
Bromo-dragonFLY58 DOB-dragonFLY |
B-fly |
Acute: Hallucinations Vasoconstriction (limb ischemia) |
|
2C series (2CI; 2CB; 2C-T7)59 |
2CB = Nexus |
Acute: Hallucinations, aggression, agitation/excited delirium, euphoria, seizures, hyperthermia, tachycardia, serotonin excess |
|
MBDB60 EBDB MBDP |
Methy-J EBDB = Ethyl-J or Eden MBDP = Methyl-K |
Acute: Lowered inhibitions Euphoria |
|
25I-NBOMe 25C-NBOMe 25B-NBOMe61,62 |
Smiles Wizard N-Bomb Solaris Cimbi |
Acute: Hallucinations Agitation Sympathomimetic Serotonin excess |
Conclusions
The use and abuse of methamphetamine is a worsening global health problem that may be underestimated in light of the current opioid epidemic. Most of the methamphetamine in the United States today is produced in Mexico from easily available precursors. It is transported via large networks originating in industrial-size methamphetamine labs. Purity and potency of street methamphetamine is higher than it has ever been. This, as well as contamination with fentanyl, has contributed to a greater number of deaths. Methamphetamines result in sympathetically mediated agitation and in psychiatric symptoms. Clinicians should be knowledgeable about the recognition and treatment of these disorders, as well as about the other complications, including arrhythmias, cerebrovascular accidents, seizures, dental issues, and systemic and local infections. Hyperthermia is a marker of severe toxicity. New methamphetamine derivatives continue to infiltrate the market and exhibit variable kinetics, potencies, and toxicities.
REFERENCES
- Gonzales R, Mooney L, Rawson RA. The methamphetamine problem in the United States. Annu Rev Public Health 2010;31:385-398.
- Chomchai C, Chomchai S. Global patterns of methamphetamine use. Curr Opin Psychiatry 2015;28:269-274.
- Panenka WJ, Procyshyn RM, Lecomte T, et al. Methamphetamine use: A comprehensive review of molecular, preclinical and clinical findings. Drug Alcohol Depend 2013;129:167-179.
- Vearrier D, Greenberg MI, Miller SN, et al. Methamphetamine: History, pathophysiology, adverse health effects, current trends, and hazards associated with the clandestine manufacture of methamphetamine. Dis Mon 2012;58:38-89.
- United Nations Office on Drugs and Crime. Methamphetamine continues to dominate synthetic drug markets. Global Smart Update 2018;20:1-16.
- Smith DE; Amphetamine Evaluation & Physician Training Project. Amphetamine use, misuse, and abuse: Proceedings of the National Amphetamine Conference, 1978. Boston: G.K. Hall; 1979.
- Smith DE, Fischer CM. An analysis of 310 cases of acute high-dose methamphetamine toxicity in Haight-Ashbury. Clin Toxicol 1970;3:117-124.
- Passie T, BenzenhÖfer U. The history of MDMA as an underground drug in the United States, 1960-1979. J Psychoactive Drugs 2016;48:67-75.
- Lin DL, Liu HC, Yin HL. Recent paramethoxymethamphetamine (PMMA) deaths in Taiwan. J Anal Toxicol 2007;31:109-113.
- Anglin MD, Burke C, Perrochet B, et al. History of the methamphetamine problem. J Psychoactive Drugs 2000;32:137-141.
- Shukla RK, Crump JL, Chrisco ES. An evolving problem: Methamphetamine production and trafficking in the United States. Int J Drug Policy 2012;23:426-435.
- U.S. Department of Justice Drug Enforcement Administration. 2018 National Drug Threat Assessment. October 2018.
- Maxwell JC, Brecht ML. Methamphetamine: Here we go again? Addict Behav 2011;36:1168-1173.
- United Nations Office on Drugs and Crime. Methamphetamine continues to dominate synthetic drug markets. Global Smart Update 2018;20:1-16.
- U.S. Department of Justice Drug Enforcement Administration. 2017 Domestic methamphetamine threat assessment key findings. Jan. 11, 2018.
- Substance Abuse and Mental Health Services Administration. Key substance use and mental health indicators in the United States: Results from the 2017 National Survey on Drug Use and Health. Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration: Rockville, MD; 2018.
- Kariisa M, Scholl L, Wilson N, et al. Drug overdose deaths involving cocaine and psychostimulants with abuse potential — United States, 2003-2017. MMWR Morb Mortal Wkly Rep 2019;68:388-395.
- Gladden RM, O’Donnell J, Mattson CL, Seth P. Changes in opioid-involved overdose deaths by opioid type and presence of benzodiazepines, cocaine, and methamphetamine — 25 states, July-December 2017 to January-June 2018. MMWR Morb Mortal Wkly Rep 2019;68:737-744.
- LaRue L, Twillman RK, Dawson E, et al. Rate of fentanyl positivity among urine drug test results positive for cocaine or methamphetamine. JAMA Netw Open 2019;2:e192851.
- Connors NJ, Hoffman RS. Amphetamines and their derivatives. In: Brent J, Burkhart K, Dargan P, et al. Critical Care Toxicology: Diagnosis and Management of the Critically Poisoned Patient. Switzerland: Springer International Publishing; 2017:1413-1438.
- Moeller KE, Lee KC, Kissack JC. Urine drug screening: Practical guide for clinicians. Mayo Clinic Proc 2008;83:66-76.
- Musshoff F. Illegal or legitimate use? Precursor compounds to amphetamine and methamphetamine. Drug Metab Rev 2000;32:15-44.
- Cook CE, Jeffcoat AR, Hill JM, et al. Pharmacokinetics of methamphetamine self-administered to human subjects by smoking S-(+)-methamphetamine hydrochloride. Drug Metab Dispos 1993;21:717-723.
- Chiu VM, Schenk JO. Mechanism of action of methamphetamine within the catecholamine and serotonin areas of the central nervous system. Curr Drug Abuse Rev 2012;5:227-242.
- Cruickshank CC, Dyer KR. A review of the clinical pharmacology of methamphetamine. Addiction 2009;104:1085-1099.
- Bernard S, Neville KA, Nguyen AT, Flockhart DA. Interethnic differences in genetic polymorphisms of CYP2D6 in the U.S. population: Clinical implications. Oncologist 2006;11:126-135.
- Fleckenstein AE, Volz TJ, Riddle EL, et al. New insights into the mechanism of action of amphetamines. Ann Rev Pharmacol Toxicol 2007;47:681-698.
- Substance Abuse and Mental Health Services Administration. Mandatory Guidelines for Federal Workplace Drug Testing Programs. 2017.
- Derlet RW, Albertson TE, Rice P. Antagonism of cocaine, amphetamine, and methamphetamine toxicity. Pharmacol Biochem Behav 1990;36:745-749.
- Kevil CG, Goeders NE, Woolard MD, et al. Methamphetamine use and cardiovascular disease. Arterioscler Thromb Vasc Biol 2019;39:1739-1746.
- Kaye S, McKetin R, Duflou J, Darke S. Methamphetamine and cardiovascular pathology: A review of the evidence. Addiction 2007;102:1204-1211.
- Hoffman RS. Cocaine and beta-blockers: Should the controversy continue? Ann Emerg Med 2008;51:127-129.
- Yeo KK, Wijetunga M, Ito H, et al. The association of methamphetamine use and cardiomyopathy in young patients. Am J Med 2007;120:165-171.
- Swalwell CI, Davis GG. Methamphetamine as a risk factor for acute aortic dissection. J Forensic Sci 1999;44:23-26.
- Wako E, LeDoux D, Mitsumori L, Aldea GS. The emerging epidemic of methamphetamine-induced aortic dissections. J Card Surg 2007;22:390-393.
- Derlet RW, Rice P, Horowitz BZ, Lord RV. Amphetamine toxicity: Experience with 127 cases. J Emerg Med 1989;7:157-161.
- Giorgetti R, Tagliabracci A, Schifano F, et al. When “chems” meet sex: A rising phenomenon called “chemsex.” Curr Neuropharmacol 2017;15:762-770.
- Davis JM, Kopin IJ, Lemberger L, Axelrod J. Effects of urinary pH on amphetamine metabolism. Ann N Y Acad Sci 1971;179:493-501.
- Rusyniak DE. Neurologic manifestations of chronic methamphetamine abuse. Neurol Clin 2011;29:641-655.
- Lappin JM, Darke S, Farrell M. Methamphetamine use and future risk for Parkinson’s disease: Evidence and clinical implications. Drug Alcohol Depend 2018;187:134-140.
- Goodchild JH, Donaldson M. Methamphetamine abuse and dentistry: A review of the literature and presentation of a clinical case. Quintessence Int 2007;38:583-590.
- Goodchild JH, Donaldson M, Mangini DJ. Methamphetamine abuse and the impact on dental health. Dent Today 2007;26:124,126,128-131; quiz 131.
- West PL, McKeown NJ, Hendrickson RG. Methamphetamine body stuffers: An observational case series. Ann Emerg Med 2010;55:190-197.
- Ruha AM, Yarema MC. Pharmacologic treatment of acute pediatric methamphetamine toxicity. Pediatr Emerg Care 2006;22:782-785.
- Friese G. The methamphetamine crisis. What EMS providers need to know to stay safe and treat patients. Emerg Med Serv 2006;35:55-64.
- Neeki MM, Dong F, Youssef D, et al. Burn injuries resulting from methamphetamine and honey oil explosions: A retrospective cohort study. J Burn Care Res 2019;40:828-831.
- Santos AP, Wilson AK, Hornung CA, et al. Methamphetamine laboratory explosions: A new and emerging burn injury. J Burn Care Rehabil 2005;26:228-232.
- Spann MD, McGwin G Jr, Kerby JD, et al. Characteristics of burn patients injured in methamphetamine laboratory explosions. J Burn Care Res 2006;27:496-501.
- Lee JH, Farley CL, Brodrick CD, Blomquist BH. Anhydrous ammonia eye injuries associated with illicit methamphetamine production. Ann Emerg Med 2003;41:157.
- Watanabe-Galloway S, Ryan S, Hansen K, et al. Effects of methamphetamine abuse beyond individual users. J Psychoactive Drugs 2009;41:241-248.
- Burge M, Hunsaker JC 3rd, Davis GJ. Death of a toddler due to ingestion of sulfuric acid at a clandestine home methamphetamine laboratory. Forensic Sci Med Pathol 2009;5:298-301.
- Ernst AA, Weiss SJ, Enright-Smith S, et al. Perpetrators of intimate partner violence use significantly more methamphetamine, cocaine, and alcohol than victims: A report by victims. Am J Emerg Med 2008;26:592-596.
- Witter RZ, Martyny JW, Mueller K, et al. Symptoms experienced by law enforcement personnel during methamphetamine lab investigations. J Occup Environ Hyg 2007;4:895-902.
- Centers for Disease Control and Prevention. Public health consequences among first responders to emergency events associated with illicit methamphetamine laboratories — selected states, 1996-1999. MMWR Morb Mortal Wkly Rep 2000;49:1021-1024.
- Gowing LR, Henry-Edwards SM, Irvine RJ, Ali RL. The health effects of ecstasy: A literature review. Drug Alcohol Rev 2002;21:53-63.
- Karch SB. Cathinone neurotoxicity (“The “3Ms”). Curr Neuropharmacol 2015;13:21-25.
- Graddy R, Buresh ME, Rastegar DA. New and emerging illicit psychoactive substances. Med Clin North Am 2018;102:697-714.
- Corazza O, Schifano F, Farre M, et al. Designer drugs on the internet: A phenomenon out-of-control? The emergence of hallucinogenic drug Bromo-Dragonfly. Curr Clin Pharmacol 2011;6:125-129.
- Dean BV, Stellpflug SJ, Burnett AM, Engebretsen KM. 2C or not 2C: Phenethylamine designer drug review. J Med Toxicol 2013;9:172-178.
- Carter N, Rutty GN, Milroy CM, Forrest AR. Deaths associated with MBDB misuse. Int J Legal Med 2000;113:168-170.
- Gee P, Schep LJ, Jensen BP, et al. Case series: Toxicity from 25B-NBOMe — a cluster of N-bomb cases. Clin Toxicol (Phila) 2016;54:141-146.
- Kyriakou C, Marinelli E, Frati P, et al. NBOMe: New potent hallucinogens — pharmacology, analytical methods, toxicities, fatalities: A review. Eur Rev Med Pharmacol Sci 2015;19:3270-3281.
The use and abuse of methamphetamine is a worsening global health problem that may be underestimated in light of the current opioid epidemic. Methamphetamines result in sympathetically mediated agitation and in psychiatric symptoms. Clinicians should be knowledgeable about the recognition and treatment of these disorders, as well as about the other complications, including arrhythmias, cerebrovascular accidents, seizures, dental issues, and systemic and local infections.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
