Pitfalls in Treating Hand Emergencies
February 1, 2020
Reprints
AUTHOR
Frank J. Edwards, MD, FACEP, Designated Institutional Official, Arnot Health Graduate Medical Education, Elmira, NY
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Assistant Professor of Emergency Medicine, Mt. Sinai, New York City
EXECUTIVE SUMMARY
• Hand injuries are common, and there are a number of pitfalls for emergency physicians and providers who treat them. When in doubt, consult a hand surgeon for advice, and provide follow-up for patients.
• A common injury is a "bite" to the metacarpals with tendon involvement. The injury is sustained when an individual punches another in the mouth, and the skin is lacerated by the teeth. Patients often are intoxicated or deny the mechanism of the injury.
• High-pressure spray devices for paint or grease, or even pressure washers, can penetrate the skin with little to no external injury. Pain nearly always is present. Many of these will require surgical treatment.
• A herpetic whitlow is an infection with the herpes virus. It can look like a paronychia on the finger. Be suspicious of this if there are vesicles present, particularly in healthcare workers, although the use of gloves has decreased this injury.
Traumatic and nontraumatic conditions involving the hand are among the more common clinical events seen in emergency departments (EDs) and urgent care centers. The hand’s anatomy is extremely complex, and there are several situations in which the proper diagnosis may be obscure, or when treatment interventions can go awry. Because of the hand’s crucial role in human function — from activities of daily living to communication and artistic expression — the stakes are very high. This article reviews the pitfalls that clinicians who encounter acute hand conditions must navigate successfully.
Introduction
About one to two of every 20 patients presenting to EDs will have complaints related to the hand, and approximately 6% of ED hand cases will have the potential for significant complications.1 About one in 10 hand injury patients will require hand surgery referral. Approximately 9% of worker’s compensation cases involve hand trauma.1 The functional outcome of traumatic or infectious conditions involving the hand depends on the nature of the condition, but the skill of the first physician or provider rendering care also plays a significant role in outcome. Providing ill-advised treatment or missing a potentially serious condition can lead to grave disability. Emergency clinicians need to be well-grounded in the initial evaluation and care of hand conditions and mindful of the pitfalls that can lead to serious downstream debility.
Review of Hand Anatomy 1,2
Nomenclature
Although the digits can be named numerically (1-5, with the thumb being 1), the most generally preferred nomenclature refers to the fingers by name: thumb, index, middle, ring, and little (or small or pinky) finger. The back of the hand (extensor surface) is referred to as the dorsal aspect. The flexor aspect is the volar or palmar aspect (this article primarily will use palmar). The sides of the hand are referred to as either radial or ulnar.
Vascular Supply
The blood supply to the hand is supplied through the radial and ulnar arteries, with the former distributed into the deep palmar arch, and the latter forming the superficial palmar arch. These arches supply blood to the fingers and thumb through branching arteries that travel along either side of the digit.
Nerve Supply
The radial nerve does not control any intrinsic hand muscles, but it has a large impact in hand movement by innervating the forearm muscles that control extension of the thumb, fingers, and wrist, along with supination of the hand. The radial nerve provides sensation to the dorsal-radial aspect of the hand.
The median nerve provides sensation to the thumb, index, middle, and the radial half of the ring finger on the palmar aspect. Motor-wise, it innervates the thenar muscles, thumb opposition muscles, and the two lumbricals radially. The recurrent motor branch of the median nerve innervates the thumb opponens, abductors, and flexors, and the thenar muscles in general — the “OAFT” muscles.
The ulnar nerve gives sensation to the little finger and the ulnar aspect of the volar half of the ring finger, and it provides motor function to the hypothenar muscles, along with the two ulnar lumbricals and all of the interossei.
Musculature
The thenar muscles consist of the abductor pollicis brevis, opponens pollicis, and flexor pollicis brevis, and they are innervated by the recurrent median nerve, as described earlier. However, the deep head of the flexor pollicis brevis is innervated by the ulnar nerve, and the adductor pollicis is activated by the ulnar nerve. The hypothenar muscles (abductor digiti minimi, flexor digiti minimi, and opponens digiti minimi) all are innervated by the ulnar nerve. There are three palmar interosseous muscles, innervated by the ulnar nerve, which adduct the index, ring, and little finger toward the middle finger. There are four dorsal interossei, also innervated by the ulnar nerve, which abduct the same digits away from the middle finger. The four lumbrical muscles (half innervated by the median nerve and half by the ulnar nerve) are unique in that they have no attachment to bone. Arising from the palmar portions of the flexor digitorum profundus (FDP) tendons, they attach near the lateral bands of the extensor mechanisms on the radial side of the fingers, flexing the metacarpophalangeal (MCP) joints and extending the interphalangeal (IP) joints of the index, middle, ring, and little fingers. They generally help coordinate flexion and extension of these digits.
Tendons
Running across the base of the dorsal aspect of the hand is a wide band of connective tissue known as the extensor retinaculum. Beneath this structure course nine extensor tendons, the middle four of which (extensors digitorum communis) provide extension to the index, middle, and ring fingers and are physically linked by juncturae in the distal dorsal hand. This means proximal lacerations to one or more of these tendons can be masked by the intact performance of another linked tendon. The extensor divides along the dorsum of the digit into a central mechanism that extends the proximal interphalangeal (PIP) joint and two lateral bands that extend the distal phalanx. The wrist is flexed by the flexor carpi radialis, flexor carpi ulnaris, and palmaris longus, and the thumb is flexed by the flexor pollicis longus. The index, middle, ring, and little fingers are flexed by two tendons each: the FDP and the flexor digitalis superficialis (FDS). The FDP courses deep to the FDS and flexes the distal phalanx, while the FDS flexes the fingers at the MCP and PIP joints.
Of note, flexor tendons are more at risk for the insidious spread of deep space infections because — unlike the extensor tendons — the flexors are encased in synovial sheaths.
Hand Examination1,2
General
The hand examination begins with a visual assessment for obvious mechanical damage to the integument (including lacerations, punctures, abrasions, and signs of thermal injury). Examine for changes in coloration suggesting ecchymosis, erythema, or the pallor of ischemia. Take note of any bony deformity indicating potential fractures or dislocations. Assess for soft tissue swelling. Next, palpate for specific areas of tenderness or crepitus, including over the collateral ligaments of affected digits, and always check the anatomical snuffbox for tenderness indicating a possible scaphoid fracture.
Range of Motion
After visual assessment, check the overall range of motion of the wrist and digits, paying special attention to possible rotational deformity of the fingers. In flexion, all fingers should point toward the scaphoid.
Vascular Assessment
Check the radial and ulnar artery pulses. The capillary refill should be less than three seconds. (The modified Allen’s test also may be done to assess the ability of the ulnar artery collaterals to supply blood to the hand if the radial artery becomes occluded. Have the patient make a fist for 30 seconds, then occlude the radial and ulnar arteries via firm pressure, and have the patient open the hand. The hand should appear blanched. Then release pressure over the ulnar artery. A normal test is when color returns to the hand within seven seconds).
Nerve Assessment
Emergency clinicians should adopt a straightforward and well-practiced technique for rapidly assessing nerve function in the hand. (See Table 1.) Here is a common paradigm:
1. For the radial nerve, check motor function by having the patient extend the wrist against resistance. For sensation, check light touch or two-point discrimination over the dorsal base of the thumb, comparing it with the contralateral side, if needed.
2. For the median nerve motor function, have the patient touch the tip of the thumb against the tip of the index finger (the “OK” sign), which tests the anterior interosseous branch of the median nerve. Have the patient oppose the thumb tip against the little finger against resistance. Median nerve sensory function is checked at the tip of the index finger.
3. For the ulnar nerve motor function, have the patient pronate the hand and spread the fingers against resistance. Because the deep branch of the ulnar nerve also innervates the adductor pollicis, you can test that by looking for Froment’s sign. With the hand extended, have the patient grip a piece of paper between the thumb and the base of the index finger. In a normal exam, the thumb will remain extended at the IP joint. If the ulnar nerve is damaged, the median nerve will take over and cause the thumb IP joint to flex instead of adduct, which represents a positive Froment’s sign. Ulnar nerve sensation is tested at the tip of the little finger.
4. If a digital nerve injury is suspected, two-point discrimination on either side of the affected digit is a useful test. Normal discrimination is 5-6 mm at the distal digit.2 Assessment should be repeated several times to eliminate the probability of a patient randomly guessing the correct answer. Remember that trauma to a digital nerve carries with it a likelihood of concomitant digital artery injury.
Table 1. Nerve Examination of the Hand |
|||
|
Radial |
Median |
Ulnar |
|
|
Sensation |
Test sensation at the dorsal base of the thumb or the dorsal first web space |
Test sensation at the tip of the index finger |
Test sensation at the tip of the little finger |
|
Motor function |
Test patient’s ability to extend the wrist or to extend the thumb |
|
|
Tendon Evaluation
Tendons are tested by assessing movement against resistance, but caveats apply. Up to 90% of a tendon can be lacerated and yield movement that may appear normal and relatively painless without resistance applied against the movement. Pain with movement against resistance suggests tendon damage.2 If the laceration is on the hand’s dorsal surface and involves the extensor digitorum communis, extensor function may appear reasonably normal. Maintain a high index of suspicion for tendon injury when movement causes pain. Keep in mind that the position of the hand at the time of the laceration often differs from the position during examination; the injured portion of the tendon may have retracted beneath intact skin. When lacerations involve the palmar surface of the hand or fingers, care must be taken to assess the function of both the FDS and FDP. FDS function is assessed by the ability of the patient to flex at the MCP joint with the PIP and distal interphalangeal (DIP) in extension. FDP function is assessed by the patient’s ability to flex the DIP with the MCP and PIP joints immobilized by the examiner.
Other Examination Techniques
Digital blocks may assist tendon evaluation if pain limits the necessary steps. When exploring a wound to assess tendon damage in a digit, a Penrose drain held in place around the base of the digit by a hemostat for no more than 20 minutes (and with the drain extended no more than 150% of its resting length) can provide a bloodless field.2
Water Bath Ultrasound. Ultrason-ography can be extremely useful in assessing for tendon damage. The traditional method of using ultrasound gel can be painful because of the need to apply moderate pressure. However, the need for gel and pressure can be eliminated by using a water bath technique. Patients have reported minimal or no pain, with excellent technical results.3
Hand Infections
Deep Space Infections
Infections can develop and propagate subcutaneously within these spaces, forming localized abscesses that can be very destructive. All deep hand infections demand timely initiation of broad-spectrum intravenous (IV) antibiotics and urgent hand surgery consultation for operative exploration and drainage. These deep infections usually begin after penetrating trauma, but they can arise from contiguous spread.4 Cases have been reported of hand infections developing secondarily to septic wrist arthritis caused by Neisseria gonorrhoeae.5 Hematogenous seeding also may give rise to deep hand infections.1 Immunocompromised individuals are at greatest risk for deep hand infections. S. aureus, streptococci, and coliforms are the most common organisms.1 Suspect a deep space infection anytime there is dorsal hand swelling (with or without fluctuance), thenar and first web space swelling, loss of palmar concavity with swelling and tenderness, and other web space swelling and tenderness, especially in the presence of a puncture wound.4 Finger movement invariably will be painful.
Rapidly progressive symptoms with pain out of proportion to findings suggest the development of necrotizing fasciitis, a genuine medical emergency. Initial management is the same — IV broad-spectrum antibiotics and surgical intervention — but timeliness is of even greater urgency. Magnetic resonance imaging (MRI) can be extremely useful in delineating the nature and extent of the infection.6 The risk of necrotizing fasciitis is greater in immunocompromised patients, as well as in patients with diabetes mellitus, peripheral vascular disease, IV drug use, and chronic liver disease. The presence of crepitus, widespread tenderness, severe pain out of proportion to findings, fever, and signs of shock are red flags for necrotizing fasciitis.
Pitfall Alert. Early deep space hand infections, including necrotizing fasciitis, may be difficult to distinguish from cellulitis. Keep a low threshold for beginning parenteral antibiotics and consulting a hand surgeon when such conditions are suspected. (See Table 2.)
Table 2. Need for Referral to a Hand Surgeon |
|
|
Timeliness |
Condition |
|
Consultation needed emergently |
|
|
Appropriate for delayed follow-up |
|
Pyogenic Flexor Tenosynovitis
Most commonly associated with a penetrating injury, pyogenic flexor tenosynovitis (PFT) is suspected when Kanavel’s four cardinal signs are present: fusiform digital swelling; pain with passive finger extension; semi-flexed digital position; and tenderness to palpation along the flexor sheath, often extending into the palm itself.4 Staphylococcus aureus and Streptococcus species are the most common pathogens, and treatment is the same as for other deep space hand infections: parenteral antibiotics and surgical irrigation and debridement. Delayed treatment increases the potential for a poor functional outcome.7 The presence of abnormal laboratory values, including elevations in white blood cells, erythrocyte sedimentation rate, and C-reactive protein, are useful to confirm the diagnosis when clinical signs are suspicious but are not highly sensitive or specific. In general, laboratory markers have a poor negative predictive value.8
Pitfall Alert. In one study, even the presence of all four Kanavel signs was only 54% sensitive in predicting the presence of PFT.4 Given the poor outcomes associated with delayed treatment, keep a low threshold for obtaining hand surgery consultation when this condition is suspected.
Septic Arthritis
Any joint in the hand, including the radiocarpal joints, is potentially susceptible to septic arthritis, which can be caused either by penetrating wounds or the contiguous spread of infection, for example a tenosynovitis or a felon.1 S. aureus and streptococci are the most common pathogens, although N. gonorrhoeae must be considered in sexually active patients. The joint will appear red and swollen, and any movement is painful. Definitive diagnosis is made with joint aspiration, where cell counts greater than 50,000 typically are seen. Hand surgery referral is necessary because open irrigation and drainage will be needed.4
Pitfall Alert. For this relatively uncommon condition, definitive diagnosis requires joint aspiration. Definitive treatment involves systemic antibiotics and irrigation of the joint, although close joint catheter irrigation also may be an option.1,4
Human Bites — Fight Bite
This injury occurs when a person’s fist makes violent contact with the teeth of another individual. The contact leads to a laceration over the dorsal aspect of one or more of the finger MCP joints where the extensor mechanism and the joint capsule are very close to the surface and prone to invasion and innoculation.4 Such a wound should be considered a fight bite until proven otherwise. Initially the injury may appear minimal and benign, but it must be taken seriously and treated with broad-spectrum antibiotics and urgent consultation for operative debridement and irrigation.
Pitfall Alert. Definitive treatment of these injuries often is delayed because many of these patients are intoxicated at the time of the injury or deny the real mechanism. Keep a high index of suspicion and a low threshold for beginning aggressive antibiotic treatment and urgent referral to a hand surgeon. In one series, 18% of patients for whom treatment was delayed by more than eight days required amputation.9
Animal Bites
As much as 80% of animal bites are from dogs, with cat bites making up most of the remainder. Most dog bites do not result in infections,10 but approximately 50% of cat bites become infected, and some require inpatient treatment.4,11 The bacteriology of infected dog and cat bites overlaps, with the predominant organisms in both being Pasteurella, Streptococcus, and Staphylococcus. Most will be polymicrobial, with mixed anaerobes and aerobes. Cats also are the primary zoologic reservoir of Bartonella henselae, the main organism deemed responsible for cat scratch disease.12
Pitfall Alert. Cat bites are more prone to infection because of the needle-like feline teeth that cause deep penetrating wounds, as opposed to the crushing and tearing-like action involved in canine bites. Clean and irrigate the wound as well as possible and provide prophylaxis with amoxicillin-clavulanate (IV, ampicillin-sulbactam), or if the patient is penicillin allergic, with doxycycline, sulfamethoxazole-trimethoprim, or a fluoroquinolone plus clindamycin.4 Cat-bite infections with Pasteurella are notoriously fast-moving, warranting close follow-up.
Paronychia
Paronychial infections occur most often secondary to trauma, possibly minor, to the tissue of a lateral nail fold. They are characterized by redness, swelling, and pain in this region. These cellulitis changes can progress to abscesses that sometimes extend beneath the nail itself and require partial debridement of the nail. The most common isolates are Staphylococcus and Streptococcus species. Early stages can be treated adequately with warm soaks and antibiotics. If fluctuance is present, a simple incision and drainage can be performed at the lateral nail fold. If there is pus subungually, the lateral one-fourth of the nail can be excised under digital block anesthesia after it is dissected away from the nail matrix.
Pitfall Alert. Chronic or recurrent paronychial infections may be caused by unusual organisms, including actinomycoses, atypical mycobacteria, and fungi, and they seldom respond to ED treatment.1,13 A known complication of paronychial infections is the development of distal phalanx osteomyelitis, of which osteolysis and soft tissue swelling are the most common radiographic findings.4 In addition, squamous cell carcinoma of the nail bed can present similar to a chronic paronychia.14 Chronic-appearing or recurrent paronychia should be referred for further evaluation.
Felon
Usually caused by S. aureus introduced by penetrating trauma, a felon is an abscess of the distal pulp, a space that is divided into multiple compartments by a series of vertical septa. A felon is an acute condition that tends to progress rapidly and usually is exquisitely painful and throbbing on presentation to the ED.1 Treatment requires an incision that adequately drains the septal spaces.
Pitfall Alert. An untreated felon can progress to septic arthritis, tenosynovitis, or osteomyelitis. Incision and drainage is performed with a longitudinal lateral incision that begins 5 mm distal to the DIP flexor crease on the ulnar aspect of the index, middle, or ring fingers, and the radial aspect of the thumb or little finger, and that passes through all the septa. Such an incision offers the least likelihood of complications involving scar formation on the “pincher” surfaces. The incision should be irrigated and packed for up to three days and should be accompanied empirically by an anti-methicillin-resistant S. aureus (MRSA) antibiotic.1,4
Herpetic Whitlow
A whitlow is the most common viral infection of the hand and can be caused by herpes simplex virus (HSVI or HSVII). Typical patients include adults with genital herpes, children with HSV gingivostomatitis,15 and health workers (especially those in the dental profession, although this is less common now in an era of increased awareness).1,15 The usual presentation involves an area of painful redness and vesicles on a distal digit. Occasionally, the presence of redness spreading proximally can confuse the picture with tenosynovitis.16
Pitfall Alert. A herpetic whitlow is a self-limited condition, usually resolving in three weeks or less, with the vesicles being contagious for the first two weeks. Antiviral treatment often is given, although no definitive data are available regarding efficacy. When considering if the patient’s painful, red fingertip condition may be a felon or a whitlow, the whitlow tends to be more indolent and less painful. Carefully search for vesicles. Incision and drainage is contraindicated in the case of a whitlow.4
Hand Trauma
High-Pressure Injection Injuries
High-pressure injection injuries are a genuine surgical emergency. Most of these injuries (more than 80%) happen at work, affecting manual laborers, painters, mechanics, farmers, water blasters, and others, most commonly when a hose ruptures or the individual inadvertently discharges a spray device transporting paint, paint thinner, diesel fuel, solvents, grease, or water under very high pressure.17 The injury most commonly occurs to the nondominant index finger. Although the patient usually is in severe pain, the injection site may appear minor initially.18 However, an intense inflammatory reaction develops, leading to extensive tissue destruction. One literature review found a 30% amputation rate after these injuries, with a lesser rate of amputation when wide surgical debridement occurred within six hours of the injury.18 Plain X-rays may be useful when a radiopaque substance like paint is involved. High-pressure water injection injuries generally do not have the same degree of inflammatory reaction, but cases of flexor tendon rupture have been reported.17
Pitfall Alert. High-pressure injection injuries may present initially with only a small puncture wound and minimal or no swelling of the affected digit,19 but rapid progression will occur, and surgical debridement is needed acutely.1,2,20-22 Start antibiotics, provide analgesia, and contact hand surgery emergently.
Crush Injuries
Although relatively uncommon, crush injuries of the hand are fraught with the likelihood of complications and poor long-term outcomes.23,24 These are related to the direct multi-structure trauma along with inflammatory damage accompanied by the potential development of compartment syndromes. The evaluation and management of patients presenting with a crushed or mangled hand involves analgesia, radiographs, tetanus prophylaxis, antibiotics, an assessment of function as good as the situation allows, along with urgent hand specialist involvement. A crush injury may present with intact skin and, in early stages, relatively moderate swelling. Be alert for the possibility of developing compartment syndrome. The hand has 10 individual muscular compartments, and compartment syndromes in the hand can begin insidiously and can be difficult to identify.
Because of nerve damage, the patient may not display the classic early sign of paresthesia.2,25 Worsening pain is the most consistent finding, along with tense edema. A patient with an escalating requirement for analgesia should raise concern for compartment syndrome. Measuring individual hand compartment pressures is difficult, even for hand specialists, and the diagnosis generally is made clinically.2 Fasciotomy is required urgently.
Pitfall Alert. Worsening pain is the best early indicator of hand compartment syndromes. Emergent hand surgery referral for fasciotomy may spare the patient severe complications, including amputation.
Tendon Injuries
Tendon injuries can be open (lacerations) or closed (ruptures or avulsions). (See Table 3.)
Table 3. Common Tendon Injuries of the Hand |
|||
|
Mallet Finger “Baseball Finger” |
Boutonnière Deformity “Buttonhole Deformity” |
Jersey Finger “Football Finger” |
|
|
Mechanism |
Sudden forced flexion of the DIP joint |
Sudden forced flexion of the PIP joint |
Sudden forced extension of a flexed DIP joint |
|
Injured Tendon |
Rupture of the extensor tendon at or near its insertion on the dorsal base of the distal phalanx, with or without an avulsion fracture |
Rupture of the central slip of the extensor mechanism at or near its insertion on the dorsal base of the middle phalanx |
Rupture of the flexor tendon at or near its insertion on the palmar (volar) base of the distal phalanx |
|
Exam Findings |
|
|
|
|
Treatment |
|
|
|
|
DIP = distal interphalangeal; PIP = proximal interphalangeal |
|||
Lacerations
By virtue of their more superficial location, extensor tendons are involved in lacerations more commonly than flexor tendons. Although some emergency clinicians have expertise in the repair of extensor tendon lacerations, the trend is toward referral of extensor tendon lacerations for delayed operative repair by a hand surgeon.2 An extensor tendon laceration of less than 25% can be treated without tendon repair. The repair of flexor tendon lacerations is inherently more complex and should not be attempted in the ED. The function of both FDP and FDS must be tested and documented, as described earlier. It is possible to have a laceration involving up to 90% of the tendon with the preservation of function, although pain and often some degree of weakness will be present. Water bath ultrasound is a useful technique to assess tendon integrity.3 If a tendon laceration that will need referral to a hand specialist for delayed repair is found or suspected, thoroughly irrigate the wound and loosely close the skin. Administer antibiotics and update tetanus status as needed.
Tendon Ruptures (or Avulsions)
The three major types of closed tendon injuries are mallet finger, boutonnière deformity, and jersey finger.
The very common mallet finger injury (also called baseball finger) is a rupture of the extensor tendon at its insertion on the dorsal base of the distal phalanx, where it sometimes avulses a tiny fragment of the bone. The injury is caused by the sudden jamming of an extended finger that hyperflexes the DIP joint. The patient will have point tenderness over the dorsal base of the distal phalanx, and pain and difficulty extending the DIP joint against resistance, although pain often makes this aspect of the exam difficult to interpret. The treatment of mallet finger injuries without bony avulsion involves splinting the DIP in a mild degree of continuous hyperextension for up to two to three months.26 Mallet finger injuries that involve an avulsion should be splinted and referred to a hand surgeon. If the tendon does not heal properly, the patient is left with a permanent inability to extend the DIP.
The boutonnière deformity also is an extensor tendon injury. In this case, the PIP is suddenly flexed, which causes a rupture of the central slip of the extensor mechanism that inserts at the base of the dorsal middle phalanx just distal to the PIP.1 This allows the PIP joint to flex and pop up between the lateral bands of the extensor mechanism like a button going into a button hole (boutonnière), resulting in the PIP being held in flexion while the lateral bands exert traction distally and extend the DIP joint. The full-blown deformity may evolve over time, and initially the main clinical sign may be painful and/or futile attempts to extend the PIP, accompanied by point tenderness over the proximal base of the dorsal middle phalanx just past the PIP joint where the central slip ruptured. If the condition is suspected, apply a splint that provides for slight PIP extension and slight DIP flexion and refer the patient to hand surgery.2
Jersey finger (or football finger) is a flexor tendon injury, specifically a rupture of the FDP at or near its insertion on the palmar base of the distal phalanx. The classic mechanism is that of a sudden forced extension of a flexed DIP, as when a player is grabbing tightly onto the jersey of another player when that player breaks free, causing the finger to straighten.1 On examination, the patient will have pain and the inability to flex the DIP, which can be seen easily when the patient tries to make a fist. There will be tenderness over the region of the dorsal base of the distal phalanx. The ring finger is involved most commonly, and ultrasound may assist in localizing the tendon rupture.26 Ultimate treatment of a jersey finger is operative repair. Splint the finger in a neutral or flexed position and refer to hand surgery.
Pitfall Alert. Any pain with motion or difficulty with function during resistance testing of the extensor or flexor tendons should be taken as potential evidence of at least a partial tendon laceration or rupture, which would warrant splinting and a specialist referral.
Lacerations
Deeper Injuries
Hand laceration repair is complicated dramatically by the multiplicity of structures deep to the skin that can be damaged. Furthermore, the identification of nerve or tendon injuries secondary to hand lacerations by clinical exam alone can be difficult. One study compared the success rate of emergency clinicians to that of hand surgeons in identifying these injuries in patients who subsequently underwent surgical exploration and repair. Emergency physicians and hand surgeons both correctly identified only 68.2% of flexor tendon injuries. However, the ED providers diagnosed fewer extensor tendon injuries than the hand surgeons did (ED providers 65.6% vs. hand surgeons 75%), with similar results for nerve injuries (ED providers 54.5% vs. hand surgeons 78.8%).27 The take-home point is that even hand surgeons missed a substantial number of tendon and nerve injuries caused by lacerations.
For lacerations over or near the thenar eminence, emergency clinicians should be especially concerned about the recurrent motor branch of the median nerve. It arises at the proximal base of the thenar eminence and runs across the eminence toward the first MCP joint, innervating the thenar muscles of opposition. An unrecognized injury to this nerve will result in thenar wasting and an inability to oppose the thumb — a functional deficit that explains the nerve’s nickname: “the million-dollar nerve.”
Prophylactic Antibiotics. There are no studies that show a benefit to routine antibiotic prophylaxis for hand lacerations.28 Clinicians must make a decision based upon mechanism, depth, and degree of contamination.
Pitfall Alert. Deep lacerations to the thenar region necessitate careful testing of thumb opposition and specialist referral if there is any suspicion of injury to the recurrent motor branch of the median nerve.
Foreign Bodies
Missed foreign bodies can lead to significant complications29 and are a potential source of litigation in emergency medicine.30 It is good practice to evaluate all lacerations and penetrating wounds to the hands as if they might contain an occult foreign body, especially when the mechanism of injury (i.e., laceration due to shattered glass) increases the likelihood.1 Retained foreign bodies are most commonly of wood, glass, metal, or pieces of gravel. Plain X-rays are very good at detecting metal, gravel, and many types of glass and plastic, but they are poor at detecting wood, which is better (although not perfectly) visualized by ultrasound.31,32 Clinical signs of retained foreign bodies include unusual pain with palpation of puncture wounds, delayed infections, and persistent pain. Foreign bodies that can be visualized are generally appropriate to remove in the ED. However, cases of deep foreign bodies, especially involving a complex structure like the hand, are best referred to a specialist for further decision-making and removal if necessary.1
Pitfall Alert. Carefully assess all wounds for potential foreign bodies. If one cannot be visualized directly or by radiograph or ultrasound but suspicion remains high, further imaging, such as computed tomography (CT) or MRI, should be considered, along with referral to a hand surgeon.
Fractures
General
Approximately 90% of hand fractures can be managed nonoperatively with splinting. The challenge for emergency clinicians is to recognize when specialty referral is needed.33
Distal phalangeal fractures may involve the articular surface, the shaft, or the tuft, with the latter being the most common and often associated with nail bed injuries (see the discussion of nail bed injuries later). In general, distal phalanx fractures are treated with simple protective splinting. With open distal tuft fractures, there is no evidence that coverage with antibiotics is protective.2
Middle and proximal phalangeal fractures are less common. They usually are nondisplaced and stable, and if so, they can be treated with buddy taping. However, angulated and potentially unstable midshaft fractures, along with spiral fractures or intra-articular fractures, should be splinted and referred to hand surgery for possible internal fixation.2
Metacarpal fractures may be of the head, neck, shaft, or base. Nearly 90% of all metacarpal fractures are of the non-thumb metacarpals:34
1. All metacarpal head fractures require hand surgeon referral — emergently, if associated with a laceration suggesting a fight bite injury.
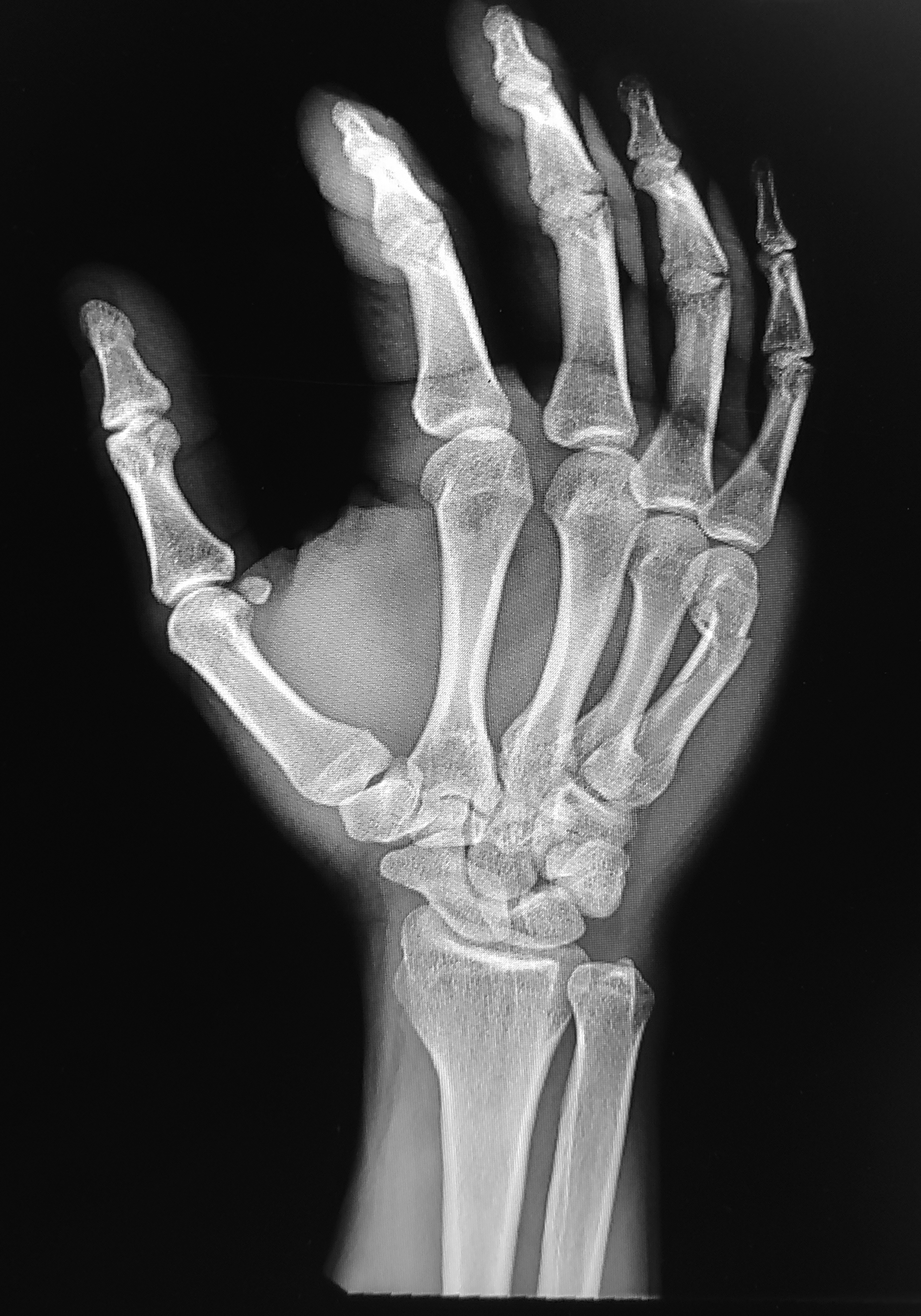
2. A fractured neck of the fifth metacarpal with palmar (volar) angulation is known as a boxer’s fracture and is the most common metacarpal fracture. (See Figure 1.) Some authors recommend anatomic reduction if the angulation exceeds 40 degrees, but a recent systematic review published in Orthopedics reported good functional results with soft splinting and buddy taping33 (little to ring finger) alone when angulation was less than 70 degrees.35 Patients should be checked in the ED for rotational deformity (as described in the examination section earlier), and if this is present or suspected, consult with hand surgery.
Figure 1. Boxer's Fracture |
 |
|
Image courtesy of Robert Wicelinski, DO |
3. Fourth metacarpal (ring finger) neck fractures can tolerate up to 30 degrees of angulation before reduction is needed.34
4. Second and third metacarpal neck fractures can tolerate 10 to 20 degrees of angulation.34
5. Metacarpal shaft fractures are more likely to develop rotational deformities than metacarpal neck fractures. These fractures can be splinted if there is no angulation or rotation. An acceptable degree of angulation for a fourth metacarpal shaft fracture is 20 degrees, and 30 degrees for a fifth metacarpal shaft fracture. If angulation exceeds this, internal fixation usually will be needed. No angulation is acceptable for second and third metacarpal shaft fractures.
6. Metacarpal base fractures are less common and fraught with potential nerve damage and carpal-metacarpal dislocations and are at high risk for complications. Involve hand surgery early in the evaluation and management of these injuries.
7. Most fractures of the thumb metacarpal involve the base and may be intra-articular or extra-articular. Bennett’s fracture is an intra-articular fracture that involves subluxation at the carpometacarpal (CMC) joint. Rolando’s fracture involves comminution of the metacarpal base. ED treatment for either intra-articular or extra-articular thumb metacarpal fractures requires a thumb spica splint and specialty referral.2
Pitfall Alert. CMC joint dislocations may accompany metacarpal fractures and can be missed unless the clinician carefully assesses for their presence. No rotational deformity is acceptable for any type of metacarpal fracture.
Dislocations
Dislocations of the PIP are far more common than dislocations of the DIP or MCP joints. They usually arise from a sudden hyperextension force that causes dorsal angulation, disrupting the volar plate. Because the radial collateral ligament is weaker than the ulnar collateral, it often will be disrupted and lead to a dislocation with some degree of ulnar deviation.2 Reduction is accomplished by performing a digital block, then applying traction and slight hyperextension, followed by palm-ward (volarly directed) pressure against the base of the middle phalanx to bring it back into position. The inability to reduce a dislocation may indicate entrapment of an avulsion fragment or of the volar plate, and operative reduction may be needed. Always perform a post-reduction X-ray to check for alignment and fractures.
Dislocations associated with fractures have significant sequelae.36 After reduction, check for mobility and strength, and splint in about 30 degrees of flexion for several weeks. Palmar (volar) dislocations are much less common and may be associated with central slip ruptures. After reduction of a palmar-angulated dislocation, splint the PIP joint in slight hyperextension and arrange hand surgery follow-up.
Dislocations of the DIP are less common than PIP dislocations and usually are dorsally angulated. They are reduced in a similar fashion.
MCP joint dislocations are uncommon, usually are dorsally angulated, and involve rupture of the volar plate. Subluxation (with the articular surfaces still in contact) actually is more likely to occur than a frank dislocation. Reduction is accomplished by flexing the wrist and pressing over the dorsal proximal phalanx in a distal and palmar (volar) direction. Operative reduction may be needed.2
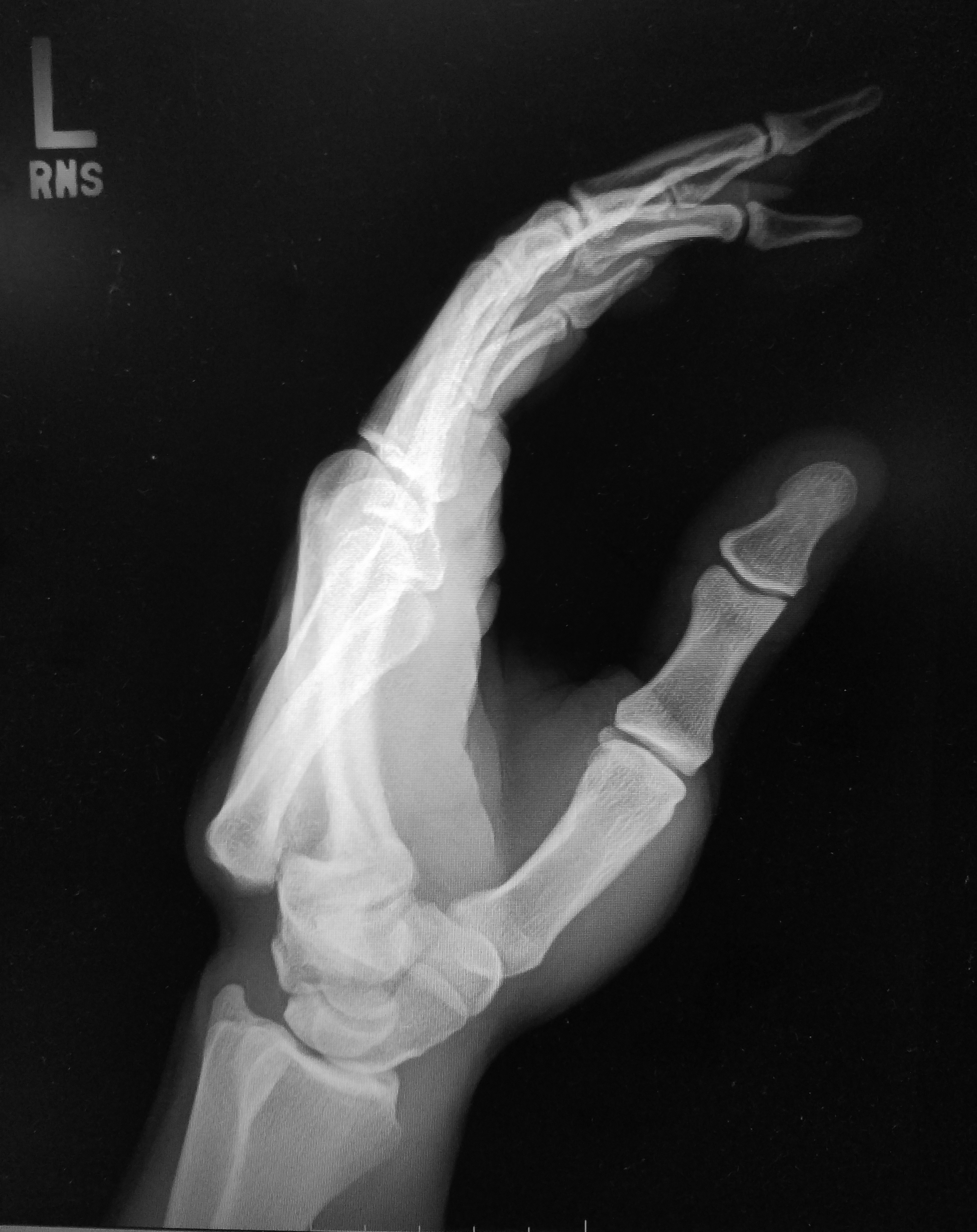
CMC joint dislocations are high-energy injuries and often are associated with fractures. (See Figure 2.) They will require orthopedic consultation.
Pitfall Alert. Always perform a post-reduction X-ray. Dislocations associated with fractures have significant sequelae.36
Figure 2. Carpometacarpal Dislocation |
 |
|
Image courtesy of Robert Wicelinski, DO |
Ligamentous Injuries
As mentioned earlier, dislocations of PIP, DIP, or MCP joints are associated commonly with partial or complete volar plate and collateral ligament ruptures. Always assess for joint motion and stability after performing a reduction. The most common ligamentous injury of the hand not involving a dislocation is a rupture of the ulnar collateral ligament of the thumb MCP joint. This injury is known commonly as gamekeeper’s thumb or skier’s thumb, and it is the result of hyper-abduction of the affected joint. It may be the result of chronic overuse or an acute injury, and it may be partial or complete. The injury is characterized by pain over the ulnar aspect of the MCP joint, accompanied by laxity of the joint when abducted. Acute ruptures may produce ecchymosis. Testing for laxity should be conducted with the thumb extended and with the joint flexed to 30 degrees. Compare laxity to the contralateral thumb. Treatment involves a thumb spica splint and referral for operative repair.37
Pitfall Alert. Acute complete thumb ulnar collateral ligament ruptures should be repaired within a week.2
Nail Bed Injuries
Subungual hematomas large enough to cause the patient significant discomfort should be drained by trephination.1 The most common trephination technique uses a microcautery unit. Although subungual hematomas arise from nail bed lacerations, most authorities now do not recommend the routine removal of intact nails to repair nail bed lacerations. This recommendation is based on studies that have demonstrated no significant difference in outcomes. However, if the nail is partially avulsed or disrupted, its remaining attachment to the nail bed should be carefully dissected away, and the nail bed laceration should be repaired meticulously with fine, dissolving sutures.38,39 The nail itself then can be cleaned, debrided, slipped back under the proximal nail fold, and sutured in place for one to two weeks to prevent synechia from forming under the nail fold that may create subsequent nail deformity.
Fifty percent of significant nail bed injuries are accompanied by distal phalangeal fractures.38 Technically open fractures, these injuries have not been shown to be associated with osteomyelitis, but the risk of tissue infection is considered enough to warrant antibiotic coverage and close follow-up.
Pitfall Alert. Significant subungual hematomas frequently lead to loss of the nail followed by regrowth. Patients should be alerted to this likelihood. If the nail is substantially disrupted, it should be removed, and the nail bed laceration should be repaired.
Amputations
Fingertip amputations are very common injuries. When the amputation involves only soft tissue at the tip and there is no bony involvement, healing by granulation and re-epithelialization yields good results. A general rule of “thumb” is that if less than 1 cm of tissue is lost, it will heal well by secondary intention. If a small portion of the distal phalanx is visible, it can be trimmed back with a bone rongeur. Apply a nonadherent dressing, give tetanus prophylaxis as needed, apply a protective splint, and consider antibiotic coverage. However, fingertip amputations that involve significant soft tissue or bone loss have the potential for adverse sequelae. They may need grafting and should be referred to a hand surgeon for management.1
Regarding traumatic amputations of major portions of the digits or of the hand itself, the criteria that hand surgeons use for decisions about reimplantation vary in different nations.40 In the United States, reimplantation generally is not performed for single finger amputations proximal to the FDS insertion; in circumstances involving crushing or avulsing injuries; or in which there has been an extended period of time since the injury.40 Isolated thumb amputations remain an indication for reimplantation with generally good results.41,42 Additionally, all amputations in children are considered potential cases for reimplantation.41 The hand surgeon should be contacted immediately because time is of the essence. Contraindications to reimplantation include self-inflicted amputations and multilevel amputations.
Pitfall Alert. Amputated parts can be rinsed gently with saline, wrapped in saline-soaked gauze, and placed in a plastic bag, which then can be placed in cool water. Avoid direct contact with ice.
Miscellaneous
Ring Removal
Regardless of whether the hand problem is infectious or traumatic, rings must be removed to prevent tissue ischemia in the event of worsening edema. Gold and silver rings can removed easily with a ring cutter, but some rings are made of hardened metal than can be problematic. Two well-described techniques that every emergency clinician should be aware of will allow the removal of most difficult-to-remove rings without the need to cut them off.
One method described by Kates43 in a population of older adults (whose rings had been in place without removal for decades) involves circumferentially wrapping an elastic blood-drawing tourniquet around the finger from the fingertip proximally, then holding the tourniquet in place for 10 minutes with a hemostat. Then the finger is lubricated, and the ring is removed with manual traction.
A second technique, described by Kingston et al,44 involves inserting two rubber bands on either side of the ring and applying a lubricating liquid to the finger. The operator then takes one rubber band in each hand and rotates (oscillates) the ring 180 degrees back and forth in one direction and then the other while exerting distal traction on the rubber bands. Titanium rings can be “cracked” using a channel lock. There are several videos of this technique on YouTube.
Bandaging
Be aware that two commonly used types of dressing materials for finger and hand injuries have been associated with necrosis and digital amputations.45-48 One is the tubular gauze material available from different manufacturers. There are two varieties of tubular dressing, one made of elasticized material, and one that is nonelastic. Both are designed to be pushed down over the affected digit, then twisted, with another layer applied as the material is drawn back toward the tip, and so forth, up and down, providing a dressing of multiple layers. However, sufficient constriction to cause vascular compromise can arise when too many layers of either are applied or when the twist at the base of the finger is overly aggressive. Problems can be avoided by never using more than two layers, by minimizing the twist at the base, and by giving the patient close follow-up instructions and a warning to return immediately if pain worsens. Be especially careful with children too young to accurately communicate the source of a discomfort.
The second type of dressing is a self-adhering elastic wrap (brand names Coban, CoFlex, and others) that is highly convenient for securing dressings to fingers and hands, but that has been associated with well-documented cases of digital necrosis leading to amputation, especially in children.47 One potential mechanism that allows these dressings to cause constriction and ischemia may be the accidental rolling of the dressing’s proximal edge. Proper dressing technique is to avoid applying the dressing material as the roll is being unrolled, which can allow too much elastic pressure to be exerted. Unroll the amount of dressing needed, cut it to length, and allow it to relax before the wrapping begins. Overlap the wrapping gently, minimizing pressure, and use the fewest layers possible. Avoid the possibility of a rolled up proximal edge occurring at the base of a finger by extending the dressing down onto the hand.
Pitfall Alert. Avoid causing digital necrosis disasters when using tubular gauze dressings or self-adhering elastic wraps through careful application and conscientious plans for follow-up and monitoring.
Summary
The hand is a very complex structure with a high potential for adverse outcomes. A careful history and physical examination along with consultation with a specialist and good follow-up are essential to a positive outcome.
REFERENCES
- Mailhot T, Lyn ET. Hand. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice [electronic version]. 8th ed. Philadelphia, PA: Elsevier; 2014: 534.
- Long B, Koyfman A. Injuries to the hand and digits. In: Tintinalli JE, MA OJ, Yealy DM, Meckler D, et al, eds. Tintinalli's Emergency Medicine: A Comprehensive Study Guide [electronic version]. 9th ed. New York: McGraw Hill; 2020; 1782.
- Blaivas M, Lyon M, Brannam L, et al. Water bath evaluation technique for emergency ultrasound of painful superficial structures. Am J Emerg Med 2004;22:589-593.
- Osterman M, Draeger R, Stern P. Acute hand infections. J Hand Surg Am 2014;39:1628-1635.
- Vidaurrazaga MM, Perlman DC. A case of purulent gonococcal arthritis. IDCases 2019;19:e00662.
- Patel DB, Emmanuel NB, Stevanovic MV, et al. Hand infections: Anatomy, types and spread of infection, imaging findings, and treatment options. Radiographics 2014;34:1968-1986.
- Dailiana ZH, Rigopoulos N, Varitimidis S, et al. Purulent flexor tenosynovitis: Factors influencing the functional outcome. J Hand Surg Eur Vol 2008;33:280-285.
- Bishop GB, Born T, Kakar S, et al. The diagnostic accuracy of inflammatory blood markers for purulent flexor tenosynovitis. J Hand Surg Am 2013;38:2201-2211.
- Shoji K, Cavanaugh Z, Rodner C. Acute fight bite. J Hand Surg Am 2013;18:1612-1614.
- Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft-tissue infections. Clin Infect Dis 2005;41:1373-1406.
- Aghababian RV, Conte JE Jr. Mammalian bite wounds. Ann Emerg Med 1980;9:79-83.
- Abrahamian FM, Goldstein EJ. Microbiology of animal bite wound infections. Clin Microbiol Rev 2011;24:231-246.
- Al-Qattan MM, Helmi AA. Chronic hand infections. J Hand Surg Am 2014;39:1636-1645.
- Li PF, Zhu N, Lu H. Squamous cell carcinoma of the nail bed: A case report. World J Clin Cases 2019;7:3590-3594.
- Hoff NP, Gerber PA. Herpetic whitlow. CMAJ 2012;184:E924.
- Brkljac M, Bitar S, Naqui Z. A case report of herpetic whitlow with positive Kanavel’s cardinal signs: A diagnostic and treatment difficulty. Case Rep Orthop 2014;2014:906487.
- Costas-Chavarri A, Turker T, Kutz JE. Flexor tendon lacerations due to high-pressure water injection injury: A case report. Hand 2012;7:121-123.
- Hogan CJ, Ruland RT. High-pressure injection injuries to the upper extremity: A review of the literature. J Orthop Trauma 2006;20;503-511.
- Wilson T, Hack JB. Case report: High-pressure injection hand injury. Emergency Medicine 2015;47:261-263.
- Verhoeven N, Hierner R. High-pressure injection injury of the hand: An often underestimated trauma: Case report with study of the literature. Strategies Trauma Limb Reconstr 2008;3:27-33.
- Rosenwasser MP, Wei DH. High-pressure injection injuries to the hand. J Am Acad Orthop Surg 2014;22:38-45.
- Yazar M, Gul Z, Gunenc AC, et al. High pressure paint gun injury of the index finger: A case report. Plast Aesthet Res 2015;2:350-352.
- Lee JS, Kim YH. Factors associated with limited hand motion after hand trauma. Medicine 2019;98:e14183.
- Graham TJ. The exploded hand syndrome: Logical evaluation and comprehensive treatment of the severely crushed hand. J Hand Surg Am 2006;31:1012-1023.
- Goodman AD, Got CJ, Weiss AC. Crush injuries of the hand. J Hand Surg Am 2017;42:456-563.
- Bachoura A, Ferikes A, Lubahn JD. A review of mallet finger and jersey finger injuries in the athlete. Curr Rev Musculoskelet Med 2017;10:1-9.
- Nassab R, Kok K, Constantinides J, Rajaratnam V. The diagnostic accuracy of clinical examination in hand lacerations. Int J Surg 2007;5:105-108.
- Zehtabchi S. Evidence-based emergency medicine/critically appraised topic. The role of antibiotic prophylaxis for prevention of infection in patients with simple hand lacerations. Ann Emerg Med 2007;49:682-689.
- Salati SA, Rather A. Missed foreign bodies in the hand: An experience from a center in Kashmir. Libyan J Med 2010 Apr 12;5. doi:10.3402/ljm.v5i0.5083.
- Moore GP, Pfaff JA. Malpractice cases in wound care and a legal concept: Special defense. West J Emerge Med 2008;9:238-239.
- Graham DD Jr. Ultrasound in the emergency department: Detection of wooden foreign bodies in the soft tissues. J Emerg Med 2002;22:75-79.
- Manthey DE, Storrow AB, Milbourn JM, Wagner BJ. Ultrasound versus radiography in the detection of soft-tissue foreign bodies. Ann Emerg Med 1996;28:7-9.
- Richards T, Clement R, Russell I, Newington Dl. Acute hand injury splinting — the good, the bad and the ugly. Ann R Coll Surg Engl 2018;100:92-96.
- Kollitz KM, Hammert WC, Vedder NB, Huang JI. Metacarpal fractures: Treatment and complications. Hand 2014;9:16-23.
- Dunn JC, Kusnezov N, Orr JD, et al. The boxer’s fracture: Splint immobilization is not necessary. Orthopedics 2016;39:188-192.
- Calfee RP, Sommerkamp TG. Fracture-dislocation about the finger joints. J Hand Surg Am 2009;34:1140-1147.
- Beutel BG, Melamed E, Rettig ME. The Stener lesion and complete ulnar collateral ligament injuries of the thumb: A review. Bull Hosp Jt Dis 2019;77:11-20.
- Bharathi RR, Bajantri B. Nail bed injuries and deformities of nail. Indian J Plast Surg 2011;44:197-202.
- George A, Alexander R, Manju C. Management of nail bed injuries associated with fingertip injuries. Indian J Orthop 2017;51:709-713.
- Shauver MJ, Nishizuka T, Hirata H, Chung KC. Traumatic finger amputation treatment preference among hand surgeons in the United States and Japan. Plast Reconstr Surg 2016;137:1193-1202.
- Kaplan FT, Raskin KB. Indications and surgical techniques for digit replantation. Bull Hosp Jt Dis 2001-2002;60:179-188.
- Agarwal JP, Trovato MJ, Agarwal S, et al. Selected outcomes of thumb replantation after isolated thumb amputation injury. J Hand Surg Am 2010;35:1485-1490.
- Kates SL. A novel method of ring removal from the aging finger. Geriatr Orthop Surg Rehabil 2010;1:78-79.
- Kingston D, Bopf D, Dhanjee U, McLean A. Evaluation of a two rubber band technique for finger ring removal. Ann R Coll Surg Engl 2016;98:300-302.
- Neal JM. Iatrogenic digital ischemia. Ann Emerg Med 1986;15:382-383.
- Norris RL, Gilbert GH. Digital necrosis necessitating amputation after tube gauze dressing application in the ED. Am J Emerg Med 2006;24:618-621.
- Makarewich CA, Lang P, Hutchinson DT. Digital ischemia after applicaition of self-adherent elastic wrap dressing: A case series. Pediatrics 2018;141. doi: 10.1542/peds.2016-3067.
- Bjorklund KA, Rice DM, Amalfi AN. Pediatric digital necrosis secondary to dressing application: A case series. Hand 2018;13:NP14-NP16.
Traumatic and nontraumatic conditions involving the hand are among the more common clinical events seen in emergency departments. This article reviews the pitfalls that clinicians who encounter acute hand conditions must navigate successfully.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
