About Face: A Review of Facial Paralysis for Emergency Clinicians
November 15, 2020
Reprints
AUTHOR
Frank J. Edwards, MD, FACEP, Designated Institutional Official, Research Director, Arnot Ogden Medical Center GME, Elmira, NY
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Clinical Assistant Professor of Emergency Medicine, Mt. Sinai Medical School and Bon Secours Hospital, NY
EXECUTIVE SUMMARY
- Although the most common cause of facial nerve weakness is Bell’s palsy, pursue a careful history along with a detailed otolaryngologic and neurologic exam to avoid missing other causes.
- The facial nerve is primarily a motor nerve; associated sensory and parasympathetic components of this nerve may produce symptoms when this nerve is diseased.
- The long course of the facial nerve and its many branches may produce symptoms and physical findings in addition to facial weakness.
- An important distinction when evaluating acute unilateral facial weakness is whether the weakness is confined to the lower face vs. weakness involving both the upper and lower face.
- The inability to fully close the eyelid may lead to corneal dryness; initiate artificial tear ointment and nocturnal patching to prevent permanent damage.
- Send serologic testing and initiate empiric antibiotic therapy for Lyme disease when facial nerve palsy presents from an endemic area.
Emergency medicine clinicians routinely encounter patients with facial paralysis and need a straightforward way to filter through the wide range of differential diagnoses. Although the majority of these patients can be diagnosed and appropriately treated based on the results of the history and exam, clinicians must be confident they can identify those individuals with more serious and potentially life-threatening conditions presenting with facial palsy and understand the next steps in evaluation.
This article reviews the fundamentals of facial paralysis, including its epidemiology, anatomy, and differential diagnosis. The article’s primary goal is to provide clinicians with a practical, straightforward approach to reaching the correct diagnosis and avoiding pitfalls along the way. The article also gives a state-of-the-science review of treatment modalities, with special attention to the treatment of Lyme disease — an increasingly major concern in endemic areas for patients who present with facial paralysis.
The Epidemiology of Facial Paralysis
The annual incidence of facial paralysis of various causes is estimated to be in the range of 20 to 30 cases per 100,000 population (0.02% to 0.03%).1,2 The majority of cases are attributed to Bell’s palsy (53.7% to 75%),2,3 which will be discussed in detail later. Bell’s palsy is presumably of viral origin, more common in older individuals, and, as noted later, is considered a diagnosis of exclusion. The following etiologies are seen in the majority of cases not diagnosed as Bell’s palsy, although the reported rates vary: herpes zoster (Ramsay Hunt syndrome), Lyme disease, otitis media, cerebrovascular accident (CVA), malignant otitis externa, mastoiditis, post-surgical and post-traumatic causes, human immunodeficiency virus (HIV) infection, sarcoidosis, Guillain-Barré syndrome, tumors, Sjögren’s syndrome, eclampsia, amyloidosis, and many others. (See Table 1.) There are rarely reported cases of central nerve (CN) VII paralysis following certain influenza vaccines.3,4 The rate of facial palsy caused by bacterial otitis media was considerably greater in pre-antibiotic times,5 estimated to be at least 10 times higher than the current rate of approximately 0.2%.4
Table 1. Causes of Facial Paralysis |
|
Anatomy and Function of the Facial Nerve
Although it is primarily a motor nerve, the facial nerve has sensory and parasympathetic components as well. It arises from the pons and has a highly complex pathway, coursing between the origins of the abducens nerve (CN V) and the vestibulocochlear nerve (CN VIII). Then it travels through the 3-cm-long Fallopian canal in the temporal bone, having a segment in the internal auditory canal where it shares space with CN VIII, gives rise to the geniculate ganglion, and runs in close proximity to the middle ear chamber. The complex course of the facial nerve through the temporal bone is the longest bony passage of any nerve in the body. This prolonged placement within a solid structure makes it particularly vulnerable to the effects of inflammation and edema.5
During its transit through the temporal bone, CN VII sends branches to the stapedius and the chorda tympani.
After exiting the bony cranium at the stylomastoid foramen, it courses through the parotid glad and divides into upper and lower divisions that further branch into five main divisions, fanning out to innervate the scalp musculature, the muscles of facial expression, the platysma, the stylohyoid and buccinator muscles, and the posterior belly of the digastric. Non-motor facial nerve components are responsible for the sense of taste in the anterior two-thirds of the tongue, along with sensation in parts of the soft palate, pharynx, and external auditory meatus. CN VII also is involved in the secretory functions of the sublingual, submandibular, and other glands.4
Differential Diagnosis
Bell’s Palsy
Bell’s palsy is named after Sir Charles Bell (1774-1842), an Edinburgh and London surgeon, anatomist, and artist who administered to wounded soldiers at the Battle of Waterloo. Also known as idiopathic facial paralysis, Bell’s palsy is the most common mono-neuropathy and the most common cause of facial paralysis (53.7% to 75%).2-4,6 The incidence rises with age and is higher in patients with diabetes and during pregnancy.7 It is usually reported as having no gender predominance, although in one series of patients at a tertiary facial nerve center, researchers observed a higher percentage of females with the condition. 4,8,9
Motor control of the facial muscles arises from the cortex and arrives at the muscles through the facial nerve and its branches. However, innervation of the upper facial muscles involves both cerebral hemispheres, whereas control of the lower face involves only the contralateral hemisphere. Therefore, a central lesion such as a stroke or a tumor affecting one hemisphere still will allow motor control of the upper face.
Bell’s palsy involves a pathologic process that affects the lower motor (peripheral) neuron of CN VII, thus blocking all motor input from either hemisphere and causing paralysis of both the upper and lower face. This is a crucial diagnostic feature. Facial paralysis of a central nature spares the forehead musculature. Bell’s palsy does not. It leads to forehead weakness and difficulty closing the eye fully, although the extent to which this occurs can be subtle in early or mild cases.
Bell’s palsy is unilateral more than 99% of the time.7 In general, bilateral facial palsy is very uncommon and has a wide range of causes, including sarcoidosis.10 When bilateral facial palsy is present, it is associated with other cranial nerve involvement in approximately half of the cases.8 In general, patients with bilateral facial paralysis should be admitted to the hospital for further workup.11 Other infectious causes of bilateral facial nerve palsy include Borrelia burgdorferi, Epstein-Barr virus, Haemophilus influenzae, and tuberculosis.12 Be aware, though, that the process that generates Bell’s palsy occasionally will cause dysfunction of other cranial nerves, which may complicate the clinical picture.13 Cold exposure and preeclampsia also have been implicated as risk factors in the generation of Bell’s palsy.6
Patients with Bell’s palsy often note a viral prodrome. The onset of weakness itself tends to be rapid, usually peaking within three days, although it can progress for a week.4 Patients often report paresthesias on the affected side, along with ear discomfort, hyper-acute hearing, and changes in taste. As mentioned, a frequent sign and symptom is the inability to fully close or rapidly blink the affected eye. This leads to corneal drying and is addressed by the clinician early on with artificial tear ointment and nocturnal patching to forestall significant corneal damage.1,4 The majority of patients with Bell’s palsy will have complete or near complete recovery of function, usually within the range of three weeks. However, approximately 15% will have greater or lesser degrees of permanent paralysis.1
For clinicians, Bell’s palsy is a diagnosis of exclusion. Bell’s palsy is considered idiopathic in origin, although research involving polymerase chain reaction assays of endoneurial fluid, muscle, and saliva has implicated herpes simplex type 1 (HSV I).6,7,14,15 Other postulated etiologies include ischemia, structural issues, inflammation, and cold stimulation.6
Treatment of Bell’s Palsy
Steroids. There is ample evidence that steroids are beneficial in shortening the recovery time in Bell’s palsy and significantly decreasing the number of individuals who have incomplete return to normal facial strength.3,16-18 Unless there are significant contraindications, all patients diagnosed with Bell’s palsy should receive steroids. A common steroid regimen for adults is prednisone 50 mg to 60 mg per day for 10 days, with tapering optional.4 The course of steroids appears to have benefit even if given as much as a week after the onset of symptoms. A recommended regimen for children is 1 mg/kg/day methylprednisolone for 10 days, followed by tapering.19 However, patients should be alerted that even with steroid treatment, as much as 30% may not achieve a complete return to baseline facial strength.17
Antiviral Agents. Because HSV appears to be a factor in some percentage of Bell’s palsy patients, antiviral agents have long been used. But, unlike the fairly strong body of research evidence for the efficacy of steroids in improving outcome, the data are weaker and more conflicting regarding antiviral agents, especially when they are used alone without a course of steroids.20 Nonetheless, there is reasonable evidence to warrant recommending the routine use of antivirals for Bell’s palsy — in combination with steroids — for Bell’s palsy when the facial weakness is moderate to severe.1,3,4,13,16,17
A common regimen uses the following agents, both of which are better absorbed than acyclovir and have more convenient dosing schedules: valacyclovir 1,000 mg three times per day (TID)for seven days, or famciclovir 250 mg TID for seven days.4 Although antivirals in combination with steroids have minimal side effects and often are used in all cases, be aware that some texts do not recommend the addition of antivirals to the steroid course in cases of mild Bell’s palsy.4 Exercise routine caution when prescribing steroids to patients with diabetes, hypertension, peptic ulcer disease, or osteoporosis. (See Table 2.)
Table 2. Treatment Regimens for Facial Paralysis |
|
|
Condition |
Treatment |
|
Bell’s palsy (idiopathic facial paralysis) |
|
|
Ramsay Hunt syndrome (herpes zoster oticus) |
|
|
Facial paralysis with concern for possible Lyme disease |
|
|
TID = three times per day; BID = twice per day |
|
Although seldom practical for the emergency clinician, subspecialists use tools such as the six-point House-Brackmann scale to grade and track the degree of CN VII nerve paralysis.21 For emergency department (ED) purposes, Bell’s palsy can be considered severe when there is obvious facial deformity at rest and the patient cannot close the affected eye. Additionally, extremely severe or complete facial paralysis in Bell’s palsy warrants timely consultation with a surgical subspecialist; temporal bone decompression of the facial nerve occasionally is considered.
The initial treatment of patients with facial paralysis must include protection for the eye that has difficulty closing completely. Corneal drying is common and can lead to great discomfort and serious corneal erosions. Always recommend the use of artificial tear ointment and nocturnal patching.1,4,13
Lyme Disease
The spirochete Borrelia burgdorferi causes Lyme disease, which is the most frequently reported vectorborne illness in the United States. Disseminated Lyme disease has many extracutaneous manifestations, including CN VII palsy, which often may occur without the presence of a typical Lyme erythema migrans rash and minus the recalled history of a proximate tick bite.22 Interestingly, Lyme disease is the most common infectious cause of bilateral facial paralysis.10
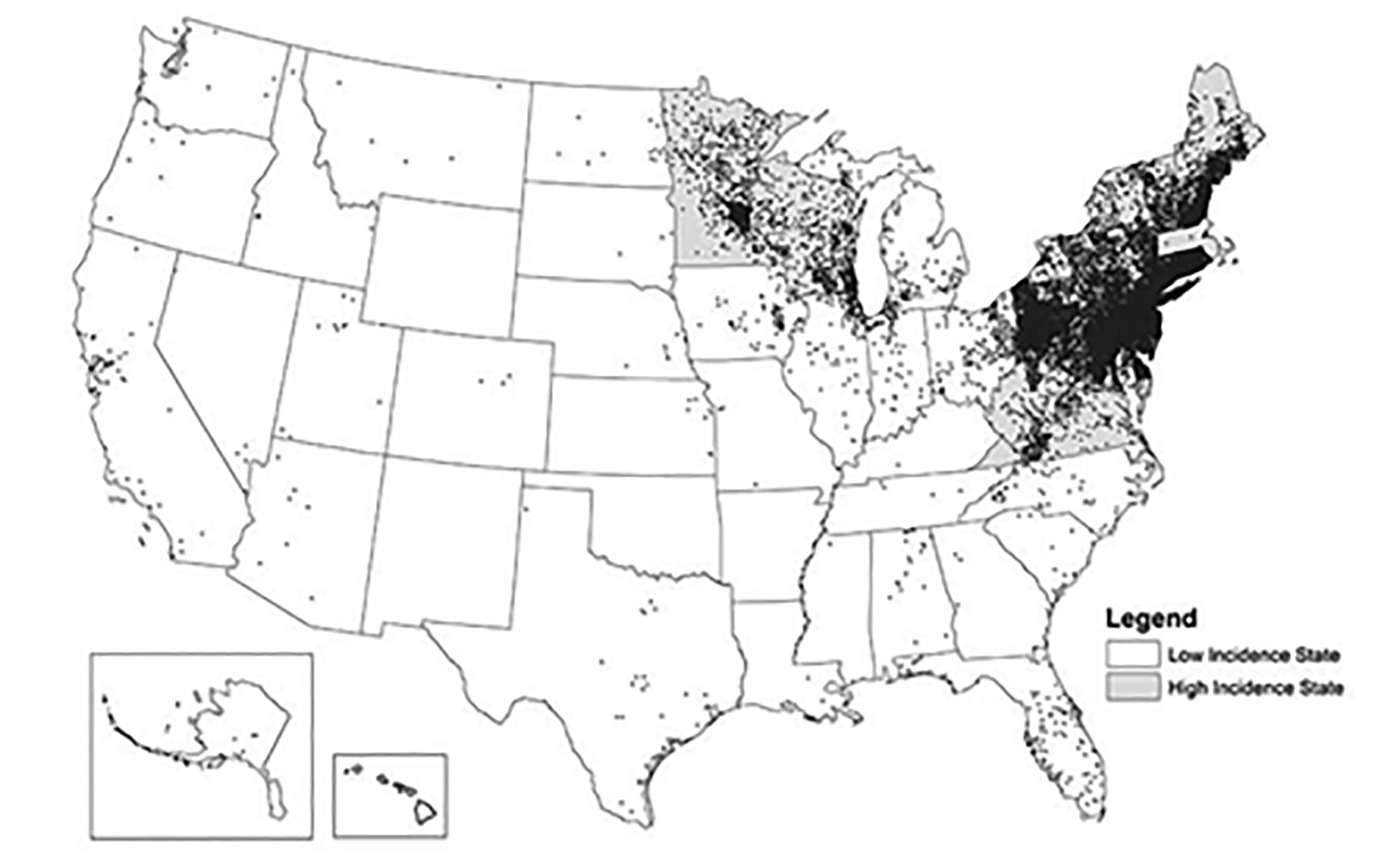
Lyme-related facial paralysis coming from early disseminated Lyme disease can be clinically impossible to distinguish from idiopathic Bell’s palsy in the ED prior to the results of serologic testing. In a study of facial paralysis in children in an endemic region, up to 34% of cases were linked to Lyme disease, especially if the facial palsy was accompanied by fever and headache.23 Another study on Long Island suggested that 25% of cases of “Bell’s palsy” in this highly endemic region are Lyme related.24 Clearly, in some areas of the country, empiric antibiotic treatment accompanied by testing for B. burgdorferi should be initiated in the ED for patients at risk for tick exposure because of geographic location and time of year.1,4,13 (See Figure 1.)
Figure 1. Reported Cases of Lyme Disease — United States, 2018 |
 |
|
1 dot placed randomly within county of residence for each confirmed case Each dot represents one case of Lyme disease and is placed randomly in the patient’s county of residence. The presence of a dot in a state does not necessarily mean that Lyme disease was acquired in that state. People travel between states, and the place of residence is sometimes different from the place where the patient became infected. Many high incidence states have modified surveillance practices. Contact your state health department for more information. |
|
Source: Centers for Disease Control and Prevention, National Center for Emerging and Zoonotic Infectious Diseases, Division of Vector-Borne Diseases |
The agent of choice for Lyme disease is doxycycline, adult dosage 100 mg twice per day (BID) for 14 days. If the patient cannot tolerate doxycycline, use amoxicillin 500 mg BID for 14 days. Despite the traditional caution regarding exposing children to doxycycline, its excellent efficacy against B. burgdorferi and its good central nervous system penetration warrants consideration for use in children older than 8 years of age at a dosage of 4 mg/kg (max 100 mg) BID for 14 days.13 Alternatively, the dosage of amoxicillin for children is 50 mg/kg (max 500 mg) TID for 14 days. (See Table 2.)
Herpes Zoster
Facial palsy caused by a reactivation of herpes zoster virus (HZV) in the geniculate ganglion of CN VII is known as Ramsay Hunt syndrome or herpes zoster oticus. Although Ramsay Hunt syndrome may closely resemble Bell’s palsy in the initial stage, there are several distinguishing clinical features. Primary among them is that the onset of Ramsay Hunt typically is followed within a few days by a vesicular eruption that may appear variably on the pinna, the external auditory canal, the oral cavity, the face, the neck, or even the tympanic membrane itself.4 Additionally, zoster facial paralysis usually is accompanied by considerably more pain in and around the ear than Bell’s palsy.4,25
The pain — often preceding the rash — is characteristically out of proportion to clinical findings. Because of the intimate proximity of the CN VIII (vestibulocochlear nerve) to the CN VII (facial nerve) as the two run through the temporal bone, vertigo and sensorineural hearing loss also may be associated with the Ramsay Hunt picture, and the hearing reduction may be long-lasting.4,25
Before the eruption of vesicles, it may be difficult to differentiate acute zoster oticus from idiopathic facial paralysis (Bell’s palsy). Because there is less chance of full recovery with zoster facial paralysis, antiviral agents in combination with steroids are recommended.25,26 The evidence for the efficacy of antiviral agents in treating zoster is stronger than for steroids, but both have been shown to hasten healing and reduce acute pain. However, neither appears to reduce the chance of postherpetic neuralgia.
There are caveats, though. To avoid compromising the immune system, steroids should never be given as a single agent without antivirals in treating zoster. Furthermore, steroids should be used with caution or avoided in patients with diabetes, hypertension, peptic ulcer disease, or osteoporosis. Patients who are already immunocompromised or who have severe neurologic symptoms should be considered for admission and treatment with intravenous acyclovir.
Because HZV is less sensitive than HSV to antivirals, it is even more important to use those that are better absorbed than acyclovir. Standard antiviral regimens for zoster are: valacyclovir 1,000 mg TID for seven days; or famciclovir 250 mg TID for seven days.4,25 A common steroid regimen for adults is prednisone 50 mg to 60 mg per day for 10 days, with optional tapering. (See Table 2.)
Although not necessarily a concern in the initial ED evaluation of a patient with facial paralysis, emergency clinicians should be aware that a small percentage of patients with zoster-related facial paralysis will not display vesicles — a condition known as zoster sine herpete.27
Otitis Media/Mastoiditis
Prior to the advent and widespread use of modern antibiotics, otitis media and mastoiditis were much more common causes of acute facial paralysis.5,28 Whereas the annual incidence was once in the range of 0.5%, it is now reported to be as low as 0.005%.12 But it still must remain in the differential, as a recent case series demonstrated among children.29
Adults with acute suppurative otitis media appear to have a higher risk of developing facial nerve palsy than children.12 The mechanism involves a spread of inflammation and possible erosion into the Fallopian canal of the temporal bone through which the facial nerve tunnels.28 Myringotomy and intravenous antibiotics are recommended to adequately treat this aggressive infection of the Fallopian canal. Adequate treatment has been reported to result in a high rate of return of facial nerve function.30 Its presence necessitates timely otolaryngology consultation. The most common organisms recovered from patients with infectious complications of otitis media are Streptococcus pneumonia and Staphylococcus species.28
Mastoiditis is an exceedingly uncommon modern cause of facial nerve paralysis, but it remains in the differential. Treatment would involve aggressive antibiotic therapy and likely surgical debridement, although, interestingly, mastoiditis with facial nerve palsy can be mimicked by granulomatous, autoimmune, and neoplastic conditions, but usually with a more indolent time course.31
Cerebrovascular Accidents
The first priority when caring for patients with facial paralysis is making certain the deficit does not arise from a central process. Usually, this is straightforward and can be accomplished through the history and examination without the need for imaging.1
To review, the forehead musculature receives innervation from corticobulbar fibers arising from both cortices. The muscles of the lower face are controlled by fibers from the contralateral cortex only.32 Therefore, a middle cerebral artery stroke may result in lower facial weakness while upper facial strength is preserved. Patients suffering facial paralysis from a central cause will be able to wrinkle their forehead and close their eyes normally. When the facial nerve itself is affected, as in Bell’s palsy, there will be weakness of both the upper and lower face.
There is an important exception to this rule. Certain very rare posterior strokes, either embolic or hemorrhagic, that affect areas of the pons near the origin of the facial nerve can present with lower motor neuron upper and lower facial weakness resembling Bell’s palsy.33-35 Clinical descriptions of most such cases indicate that patients had additional neurologic findings, including ataxia, dysarthria, occulovestibular dysfunction, and horizontal gaze deficits. The latter is not surprising given the proximity of the facial nerve nucleus to that of the abducens (CN VI) nucleus in the dorsal pons.35 Because of the rare possibility of a pontine stroke mimicking Bell’s palsy, clinicians should make a full neurologic exam with special attention to extraocular movements, a standard feature in the evaluation of patients with facial palsy. Magnetic resonance imaging (MRI) is indicated whenever a stroke is suspected in such cases.
Malignant Otitis Externa
High on the list of external auditory canal conditions that can lead to facial paralysis is malignant otitis externa (MOE), a serious infection caused by Pseudomonas aeruginosa 98% of the time and seen most often (86% to 90% of cases) in elderly diabetic patients. It carries high rates of morbidity and mortality.
Hallmark symptoms include severe pain, purulent auditory canal discharge, and hearing loss. It generally will not present a diagnostic dilemma to emergency clinicians.36,37 Treatment involves prolonged systemic antipseudomonal antibiotics, topical antibiotics/corticosteroid preparations in the auditory canal, and surgical debridement to remove granulation tissue or purulent exudate. Clinical suspicion of MOE should lead to imaging with contrast-enhanced computed tomography (CT) or MRI.
Cholesteatomas
Cholesteatomas arise from the abnormal proliferation of squamous epithelial cells, primarily in the middle ear, but they can extend into the external auditory canal. Chronic and indolent in nature, this uncommon entity can erode and destroy surrounding tissue, including the auditory ossicles and mastoid air cells. When a cholesteatoma impinges on the Fallopian canal of the temporal bone, it will damage CN VII and cause facial paralysis.37 Cholesteatoma is caused most commonly by repeated middle ear infections, although some may be caused by congenital dermoid cysts.21
Typical presenting symptoms include ear canal discharge and hearing loss. The tympanic membrane usually appears grossly abnormal. MRI or contrast-enhanced CTs are warranted when there is any clinical suspicion of this condition. Treatment is surgical, usually a mastoidectomy to remove the disease from the bone and tympanoplasty to repair the eardrum.
Tumors of the External Auditory Canal
Neoplasms, such as Ewing sarcoma, squamous cell carcinoma, and osteosarcoma, can disrupt the temporal bone and lead to rare instances of facial paralysis. There also are case reports of benign middle ear osteomas causing facial paralysis.38 Any suspicion of these entities based on a chronic or indolent time course and clinical findings should lead to imaging with MRI or contrast-enhanced CT.37
Trauma
Unilateral lower motor neuron facial paralysis can arise from injuries to that portion of the temporal bone through which CV VII traverses — most commonly a basilar skull fracture. Estimates are that 7% to 10% of temporal bone fractures cause injuries to the facial nerve.39 The onset of neuropathy may be delayed by several days or more as edema and inflammation develop.40 Other signs of basilar skull fracture, such as hemotympanum, post-auricular or periorbital ecchymosis, and cerebrospinal fluid rhinorrhea, may be present.
Basilar skull fractures causing immediate facial nerve injury are candidates for surgery. Such a finding warrants emergency consult with a surgical subspecialist. The denser the paralysis, the lower the chances are for full functional recovery.41 Facial nerve paralysis also has been reported rarely after barotrauma and lightning injuries.39
Other Tumors
The following is a list, certainly not exhaustive, of neoplasms that have been associated with facial paralysis that were not already mentioned in the earlier section on external auditory canal pathology: parotid gland tumors; leukemia (possibly bilateral facial paralysis); temporal bone histiocytosis; hemangiomas; rhabdomyosarcoma; facial nerve neuromas; and schwannomas.42-44 For the emergency medicine clinician, the time course is the key to suspecting a neoplastic cause for a patient’s facial paralysis. Typically, the course of onset is gradual and occurs over more than several weeks.42 Concern for the presence of a neoplastic entity obviously warrants MRI or high-resolution CT scanning.
Post-Surgical
For the sake of completeness, we will briefly mention that facial paralysis may occur with any surgical procedure that takes place in close proximity to the facial nerve, especially procedures involving the parotid gland, middle ear, mastoids, and uncommonly after the removal of vestibular schwannomas.42,45 Because these injuries generally become apparent during the immediate post-operative period, such conditions will not present a diagnostic puzzle to the emergency clinician. The operating surgeon should be involved in the case as quickly as possible.
Despite the routine use of electromyographic monitoring during parotid surgery to identify the course of the facial nerve, parotid surgery still has been reported to cause temporary facial paralysis in 40% of cases and permanent injury in approximately 5% of parotid procedures.46
Emergency Department Approach to Facial Paralysis
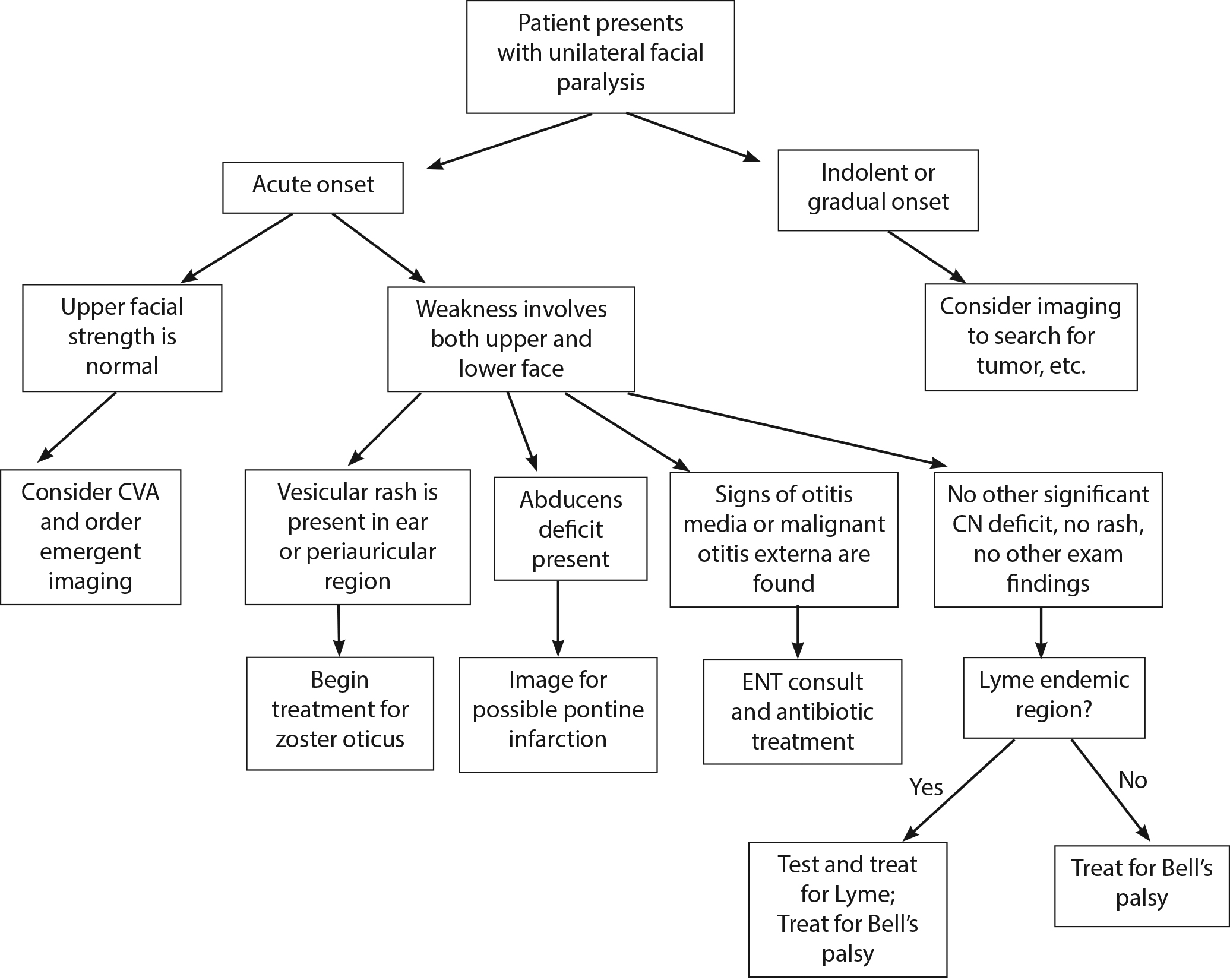
Although the list of entities that can cause facial paralysis is dauntingly long, the ED approach is straightforward. (See Figure 2.) Two causes of unilateral facial weakness are far and away the most common: Bell’s palsy and strokes.3
Figure 2. Emergency Department Evaluation for Facial Paralysis |
 |
|
CVA = cerebrovascular accident; CN = central nerve; ENT = ear, nose, and throat/otolaryngologist |
The ED approach begins by sorting the acute-onset palsy into those caused by peripheral (lower motor neuron) facial nerve dysfunction vs. those precipitated by a central lesion. As already discussed, a stroke spares the forehead. Have the patient smile, lift their eyebrows, and close their eyes. If the entire forehead wrinkles symmetrically, the brows raise equally, and the patient can shut both eyes completely, we are dealing with a stroke. If the time course of onset is indolent and in the range of weeks, the problem could be a possible central neoplasm. Such patients, of course, require emergent imaging.1
Rapid eye blinking is a good method for exposing the inability to close the eye fully.4
Related to this is “Bell’s phenomenon,” which refers to a normal response of the globes to rotate upward and laterally when the eyes close (the palpebral oculogyric reflex). This may be observed when a patient with facial nerve paralysis attempts but fails to close the affected eye.47
As already mentioned, one type of cerebrovascular accident breaks the “strokes-spare-the-forehead” rule. Lower pontine infarctions can affect the infra-nuclear facial nerve and present a picture of dense unilateral upper and lower facial paralysis mimicking Bell’s palsy.33,34 Because the abducens nucleus lies in proximity to the emerging facial nerve, however, this syndrome is likely to be accompanied by difficulty abducting the ipsilateral eye.48 Therefore, along with assessing facial nerve function, always test extraocular movements in patients with facial palsy.
Give special focus during history taking to these issues: the time course of onset, the presence or absence of a prodrome, the presence of tingling and/or pain or changes in taste, tick bites within the previous month, and whether there has been any recent head trauma or any surgical procedures involving the parotid gland or temporal bone structures, such as the middle ear.
Bell’s palsy has an acute onset that generally peaks within three days and is not infrequently associated with a prodrome, facial tingling, hyperacusis, and aching around the ear. Zoster oticus (Ramsay Hunt syndrome) causes pain that tends to be out of proportion to findings, and severe zoster oticus cases often are accompanied by hearing disturbance and vestibular vertigo. Severe headache or mental status changes in the context of facial paralysis should raise suspicion for meningitis or subarachnoid hemorrhage. The general historical milieu also includes whether the patient currently lives in or has recently traveled through a high prevalence region for Lyme disease.1,4
Keeping in mind that the most important entities to rule out are strokes and ear infections,1 physical exam features that need to be checked in all patients with facial palsy include:
- a neurologic exam beginning with cranial nerves;
- a careful check of the external auditory canal for inflammation, lesions, or masses;
- an assessment of the tympanic membrane for signs of otitis media;
- a search of the skin of the auricle, periauricular region, and face for vesicular lesions; and
- palpation of the mastoid region for tenderness suggesting infection. A bedside test of hearing also may be useful.
Laboratory and Radiologic Evaluation
Patients with classic Bell’s palsy signs and symptoms can be diagnosed clinically and do not otherwise require laboratory testing or imaging.1,3,4,13,16 An exception to this precept exists in Lyme disease endemic regions. Patients who present as Bell’s palsy and are geographically at risk for Lyme disease should be serologically tested for antibodies to B. burgdorferi, starting with an enzyme-linked immunoassay (ELISA) test and followed up with the more sensitive and specific Western blot immunoassay if initial results are positive or indeterminate, with antibiotic treatment begun empirically, as discussed earlier.22
Suspicion for stroke mandates the routine imaging with CT scanning and/or MRI. An MRI should be obtained if there is suspicion for a pontine stroke. If there is concern for temporal bone pathology or a parotid lesion, the recommended study is either a gadolinium-enhanced MRI or a fine-cut, non-contrast CT scan of the concerning region.16 If an autoimmune condition is under consideration, recommended laboratory tests include a complete blood count, C-reactive protein, erythrocyte sedimentation rate, antinuclear antibodies, rheumatoid factor, antiphospholipid antibody, antineutrophil cytoplasmic antibody, and angiotensin converting enzyme.16
Summary
Facial paralysis can be caused by upper motor neuron (central) or lower motor neuron (peripheral) pathology. The clinical distinction usually is straightforward: With rare exception, central causes (such as strokes or tumors) spare the forehead. The exception to this rule involves certain pontine strokes. These entities are very uncommon and usually appear to have additional neurologic signs, such as abducens palsy, dysarthria, ataxia, and occulovestibular dysfunction.35 Always perform a general neurologic exam and check extraocular movements carefully in individuals with facial palsy. Concern for the presence of an acute CVA mandates immediate imaging with CT and consideration for MRI.
The majority of patients seen in EDs and urgent care centers with unilateral facial paralysis will receive a diagnosis of Bell’s palsy (idiopathic facial paralysis), the cause of which in many cases is likely HSV, but this has not been definitely proven. Nonetheless, a diagnosis of Bell’s palsy can be made safely on clinical grounds alone, and the patient can be treated with steroids and antivirals (famciclovir or valacyclovir). Corneal drying is a common complication and needs aggressive preventive treatment with artificial tear ointment and patching. The majority of patients will recover full facial function.
All Bell’s palsy patients diagnosed in Lyme disease endemic areas during tick season are assumed to be infected with B. burgdorferi until proven otherwise. Begin two-step testing and start the patient empirically on a course of doxycycline (or amoxicillin). Ramsay Hunt syndrome or zoster oticus is shingles of the facial nerve and may present similarly to Bell’s palsy, although the pain tends to be more severe and there often are concomitant symptoms involving vestibulocochlear nerve dysfunction, including vertigo. Check all facial paralysis patients carefully for the presence of a vesicular rash in or around the ear. Ramsay Hunt patients should always be treated with antivirals (famciclovir or valacyclovir).
Severe otitis media, mastoiditis, and malignant otitis externa (seen primarily in elderly patients with diabetes) are less common causes of facial paralysis. However, they carry a high risk of morbidity and must be ruled out through examination. If these causes are identified, they require aggressive treatment.
Patients with facial paralysis after head trauma or maxillofacial surgery require emergent imaging and consultation. Patients with a gradual onset of facial paralysis extending over several weeks or more must be evaluated with imaging for entities such as cholesteatoma and various tumors involving the temporal bone or the central nervous system.
In conclusion, it is instructive to look at a 2013 study published in the Annals of Emergency Medicine.48 The investigators who undertook this important work examined the records of more than 40,000 patients discharged from the ED with a diagnosis of Bell’s palsy. The results showed a very low incidence (0.8%) of misdiagnosis detected within 90 days of the initial visit.48 The great majority (85.4%) of missed conditions involved cerebrovascular accidents, zoster oticus, Guillain-Barré syndrome, and otitis media. Diabetes and increasing age were risk factors positively associated with making an incorrect diagnosis of Bell’s palsy.
REFERENCES
- Gupta N, Andrus P. Acute peripheral neurologic disorders. In: Tintinalli JE, et al, eds. Emergency Medicine: A Comprehensive Study Guide [electronic version]. 9th ed. McGraw Hill; 2020.
- Atolini N, Jorge JJ, de Faria Gignon V, et al. Facial nerve palsy: Incidence of different etiologies in a tertiary ambulatory setting. Intl Arch Otorhinolaryngol 2009;13:167-171.
- Gliden DH. Clinical practice. Bell’s palsy. N Engl J Med 2004;351:1323-1331.
- Stettler BA. Brain and cranial nerve disorders. In: Walls RM, Hockberger RS, Gausche-Hill M, et al, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice [electronic version]. 9th ed. Elsevier; 2018; chapter 95.
- Cawthorne T, Haynes DR. Facial palsy. BMJ 1956;Nov 24:1197-1200.
- Zhang W, Xu L, Luo T, et al. The etiology of Bell’s palsy: A review. J Neurol 2019;267:1896-1905.
- Ahmed A. When is facial paralysis Bell palsy? Current diagnosis and treatment Cleve Clin J Med 2005;72:398-405.
- Jung J, Park DC, Jung SY, et al. Bilateral facial palsy. Acta Otolaryngol 2019;139:934-938.
- Hohman MH, Hadlock TA. Etiology, diagnosis, and management of facial palsy: 2000 patients at a facial nerve center. Laryngoscope 2014;124:E283-E293.
- Jain V, Deshmukh A, Gollump S. Bilateral facial paralysis: Case presentation and discussion of differential diagnosis. J Gen Intern Med 2006;21:C7-C10.
- Pothiawala S, Lateef F. Bilateral facial nerve palsy: A diagnostic dilemma. Case Rep Emerg Med 2012;2012:458371.
- Ellefsen B, Bonding P. Facial palsy in acute otitis media. Clin Otolaryngol Allied Sci 1996;21:393-395.
- Garro A, Nigrovic LE. Managing peripheral facial palsy. Ann Emerg Med 2018;71:618-624.
- Murakami S, Mizobuchi M, Nakashiro Y, et al. Bell palsy and herpes simplex virus: Identification of viral DNA in endoneurial fluid and muscle. Ann Intern Med 1996;124:27-30.
- Furuta Y, Fukada S, Chida E, et al. Reactivation of herpes simplex virus type 1 in patients with Bell’s palsy. J Med Virol 1998;54:162-166.
- Jowett N. A general approach to facial palsy. Otolaryngol Clin North Am 2018;51:1019-1031.
- Gronseth GS, Paduga R, American Academy of Neurology. Evidence-based guideline update: Steroids and antivirals for Bell palsy – Report of the Guideline Development Subcommittee of the American Academy of Neurology. Neurology 2012;79:2209-2213.
- Madhok VB, Gagyor I, Daly F, et al. Corticosteroids for Bell’s palsy (idiopathic facial paralysis). Cochrane Database Syst Rev 2016;7:CD001942.
- Babl FE, Mackay MT, Borland ML, et al. Bell’s Palsy in Children (BellPIC): Protocol for a multicentre, placebo-controlled randomized trial. BMC Pediatr 2017;17:53.
- Engström M, Berg T, Sternquist-Desatnik A, et al. Prednisolone and valaciclovir in Bell’s palsy: A randomized, double-blind, placebo-controlled, multicentre trial. Lancet Neurol 2008;7:993-1000.
- Choi JW, Park YH. Facial nerve paralysis in patients with chronic ear infections: Surgical outcomes and radiologic analysis. Clin Exp Otorhinolaryngol 2015;8:218-223.
- Shapiro ED. Clinical practice. Lyme disease. N Engl J Med 2014;370:1724-1731.
- Nigrovic LE, Thompson AD, Fine AM, Kimia A. Clinical predictors of Lyme disease among children with a peripheral facial palsy at an emergency department in a Lyme disease–endemic area. Pediatrics 2008;122:e1080-e1085.
- Halperin JJ, Golightly M. Lyme borreliosis in Bell’s palsy. Long Island Neuroborreliosis Collaborative Study Group. Neurology 1992;42:1268-1270.
- Cohen JI. Clinical practice. Herpes zoster. N Engl J Med 2013;369:255-263.
- de Ru JA, van Benthem PP. Combination therapy is preferable for patients with Ramsay Hunt syndrome. Otol Neurotol 2011;32:852.
- Furuta Y, Ohtani F, Kawabata H, et al. High prevalence of varicella-zoster virus reactivation in herpes simplex virus-seronegative patients with acute peripheral facial palsy. Clin Infect Dis 2000;30:529-533.
- Prasad S, Vishwas KV, Pedaprolu S, Kavyashree R. Facial nerve paralysis in acute suppurative otitis media – management. Indian J Otolaryngol Head Neck Surg 2017;69:58-61.
- Psillas G, Antoniades E, Ieridou F, Constantinidis J. Facial nerve palsy in children: A retrospective study of 124 cases. J Paediatr Child Health 2019;55:299-304.
- Popovtzer A, Raveh E, Bahar G, et al. Facial palsy associated with acute otitis media. Otolaryngol Head Neck Surg 2005;132:327-329.
- Maniu AA, Harabagiu O, Damian LO, et al. Mastoiditis and facial paralysis as initial manifestations of temporal bone systemic diseases – the significance of the histopathological examination. Rom J Morphol Embryol 2016;57:243-248.
- Blumenfeld H. Neuroanatomy Through Clinical Cases. 2nd ed. Sinauer Associates/Oxford University Press; 2010.
- Agarwal R, Manandhar L, Saluja P, Grandhi B. Pontine stroke presenting as isolated facial nerve palsy mimicking Bell’s palsy: A case report. J Med Case Rep 2011;5:287.
- Nguyen V, Reddy V, Varacallo M. Neuroanatomy, Cranial Nerve 6 (Abducens). In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan. https://www.ncbi.nlm.nih.gov/books/NBK430711/
- Min YG, Jung KH. Patterns of pontine strokes mimicking Bell’s palsy. BMC Neurol 2019;19:208.
- Tirelli G, Gatto A, Brancatelli S, Piccinato A. Malignant external otitis with facial nerve paralysis. Austin J Otolaryngol 2018;5:1097.
- Chatra PS. Lesions in the external auditory canal. Indian J Radiol Imaging 2001;21:274-278.
- Curtis K, Bance M, Carter M, Hong P. Middle ear osteoma causing progressive facial nerve weakness: A case report. J Med Case Rep 2014;8:310.
- Gordin E, Lee TS, Ducic Y, Arnaoutakis D. Facial nerve trauma: Evaluation and considerations in management. Craniomaxillofac Trauma Reconstr 2015;8:1-13.
- Leitch EF, Hanson JR. An unusual case of facial nerve palsy following soccer related minor head injury. Br J Sports Med 2006;40:e9.
- Adegbite AB, Khan MI, Tan L. Predicting recovery of facial nerve function following injury from a basilar skull fracture. J Neurosurg 1991;75:759-762.
- Ciorba A, Corazzi V, Conz V, et al. Facial nerve paralysis in children. World J Clin Cases 2015;3:973-979.
- Kirazli T, Öner K, Bilgen C, et al. Facial nerve neuroma: Clinical, diagnostic, and surgical features. Skull Base 2004;14:115-120.
- Sen S, Gupta A, Friedman P, Naina HV. Bilateral facial nerve palsy in acute B cell lymphoblastic leukemia: A case report and review of the literature. Indian J Hematol Blood Transfus 2016;32(Suppl 1):15-19.
- Rinaldi V, Casale M, Bressi F, et al. Facial nerve outcome after vestibular schwannoma surgery: Our experience. J Neurol Surg B Skull Base 2012;73:21-27.
- Hussain T, Nguyen LT, Whitney M, et al. Improved facial nerve identification during parotidectomy with fluorescently labeled peptide. Laryngoscope 2016;126:2711-2717.
- Jones DH. Bell’s phenomenon should not be regarded as pathognomonic sign. BMJ 2001;323:935.
- Tsukita K, Sakamaki-Tsukita H, Suenaga T. Combined abducens and peripheral facial nerve palsy. Intern Med 2018;57:3223-3224.
- Fahimi J, Navi BB, Kamel H. Potential misdiagnoses of Bell’s palsy in the emergency department. Ann Emerg Med 2013;63:428-434.
Emergency medicine clinicians routinely encounter patients with facial paralysis and need a straightforward way to filter through the wide range of differential diagnoses. This article reviews the fundamentals of facial paralysis, including its epidemiology, anatomy, and differential diagnosis.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
