The Role of the Social Work Case Manager Across the Continuum of Care
The continuum of care is defined as “an integrated system or package of healthcare support services that assures comprehensive, coordinated care for patients based on individualized service needs.” For patients with a disease, this covers all phases of illness, from diagnosis to the end of life.
Social workers play a vital role on the interdisciplinary care team across the continuum of care. Working in concert with RN case managers and other members of the healthcare team, they assist in guiding and tracking patients over time through physical health, mental health, and social services, spanning all levels of intensity. We will review the evolving role of social work professionals across the healthcare continuum, both within the acute care setting and beyond the walls of the hospital.
Case Management Across the Continuum
The continuum of care includes a wide range of services. Social workers are needed for high-risk patients at all points along that continuum. Examples of these services include:
- hospital;
- emergency care;
- urgent care;
- home health;
- skilled nursing facilities;
- hospice;
- adult day care;
- primary care;
- ambulatory care;
- sub-acute care;
- rehabilitative care;
- wellness centers.
The challenge for healthcare providers today is to understand the best methods of integrating these services. This is where case management comes in. Case management is the glue that holds the continuum of care together. Integrated care cannot happen without it. Case managers provide these important linkages across all healthcare settings and providers.
The Role of the Social Worker in Acute Care
The social worker role in acute care can vary depending on the type of model the hospital uses. The various combinations include:
- psychosocial support and interventions;
- discharge planning;
- psychosocial support, interventions, and discharge planning.
In some instances, a physician or RN case manager refer patients to social workers. In other examples, the social worker may self-refer. Patients also can request these services. In the integrated case management model, RN case managers assess patients to determine whether they meet high-risk criteria for referral. This is performed during the initial admission assessment.
As one reviews the data sets, note the social work referral triggers. These triggers must be individualized by each hospital implementing the tool. These triggers cover social workers who are performing some elements of discharge planning as well as psychosocial support and interventions. The case manager completes this assessment and refers to the social worker as needed. Additionally, the home care referral criteria are embedded in the assessment so referrals can be made to home care early in the stay.
The process of including these criteria in the admission assessment provides for an early and comprehensive referral based on predetermined criteria. This is critical in several ways:
- reduces the risk of overlooking high-risk patients;
- front-loads the referral process by making referrals early in the hospital stay;
- provides a structure for the RN and social work case manager to work together on high-risk patients;
- provides the social worker with information to help him or her determine if they will follow the case (they can refuse if no needs are identified);
- informs the social worker as to what psychosocial interventions might be needed during the hospital stay.
- provides information that might inform the discharge plan.
Acute Care Social Worker Case Loads
Social workers identify and carry psychosocially complex patients. Roughly 30% of all hospitalized patients will require the services of a social worker while in the hospital. Because only high-risk patients are followed, caseloads are consistent regardless of the patient’s clinical area.
Unit Type, Social Worker/Patient Ratio:
- Medical: 1:17;
- Neurology: 1:17;
- Surgical: 1:17;
- Intensive care: 1:17;
- Step-down (intermediate): 1:17;
- Pediatric: 1:17;
- Obstetrics/Gynecology: 1:17;
- Acute Rehabilitation: 1:17;
- Observation: 1:17.
The Social Worker in the Outpatient Setting
Community-based providers work with social work case managers to identify and treat patients with high-risk psychosocial needs that may affect their ability to manage their care in their home or other setting, including areas such as sub-acute. Patients who are struggling with managing their care are at greater risk for returns to the emergency department or admission to the hospital. While the clinical team manages the medical needs of the patient, the social work team manages those psychosocial triggers that, if not addressed, can cause negative outcomes for the patient. The identification of high-risk, high-cost, high-volume groups can provide a good starting point for identifying these patients.
Social workers, through high-risk screening, identify those patients at highest risk and intervene as needed. Examples of high-risk groups include:
- geriatric;
- chronically ill;
- underinsured;
- uninsured;
- behavioral health issues;
- substance abuse;
- homeless;
- catastrophic illnesses;
- frequent readmissions.
In addition, it is important to consider the category of “rising risk” patients. These are patients who may fall into low- or moderate-risk categories but are at risk for poor outcomes without case management intervention. The intervention needed may be less than other patients, but will be important in maintaining these patients in the community.
Each provider setting must choose the criteria most relevant to them and their patient population. Note that some criteria are high-risk, some are financial, and some are social. Each criterion may bring issues that cannot be managed well by patients and/or their support systems. Below is a high-risk screen that provides the social worker with a tool that helps identify the specific areas that may require social work intervention or support.
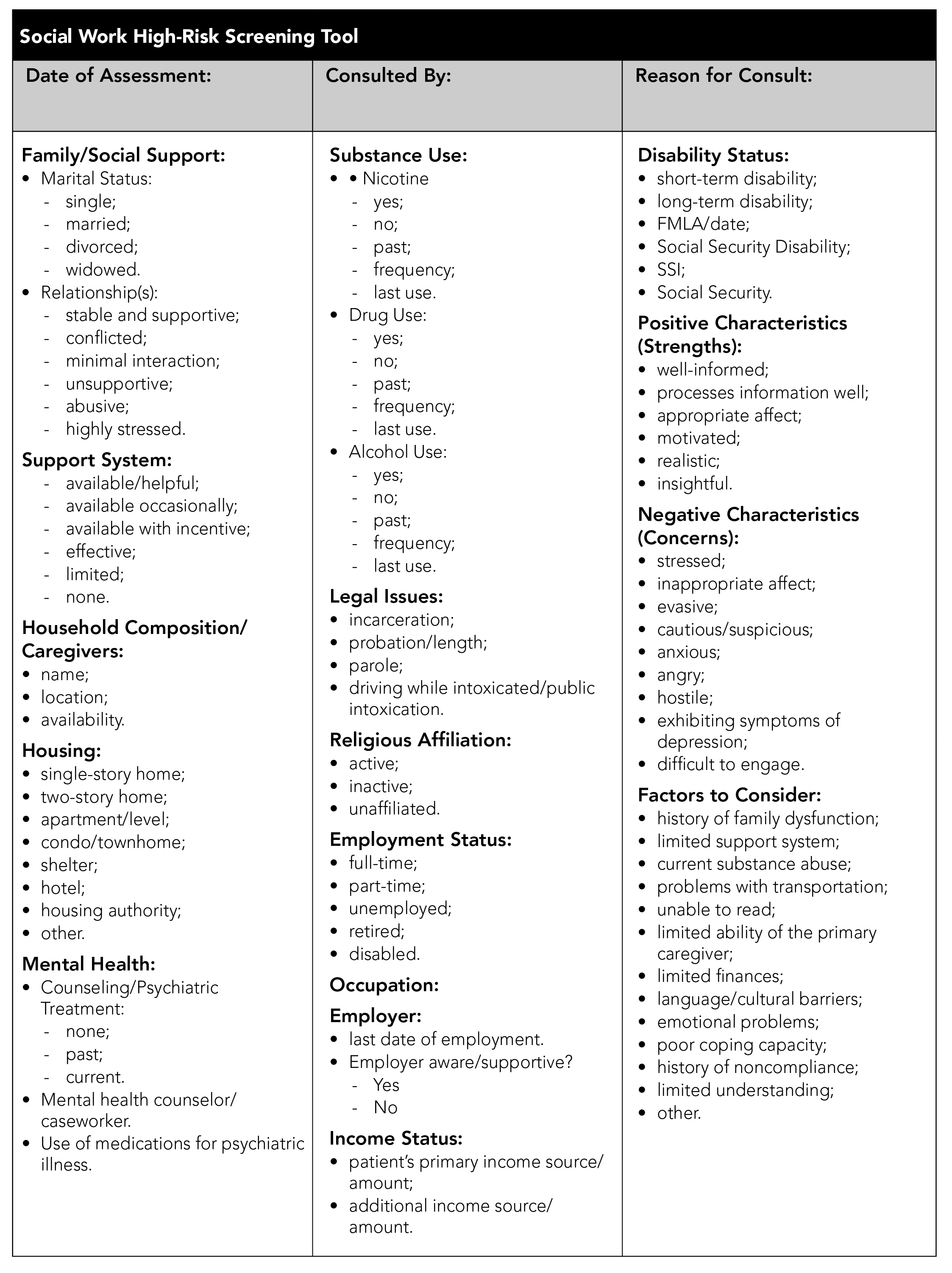
Social workers function as the primary case manager for patients with psychosocial or financial issues. They also might provide support to patients with clinical issues. In the second case, the social worker collaborates with the RN case manager. Some patients only might require some brief counseling. As in the acute care setting, the social worker may carry some patients for a short period. Others may require long-term support.
Patients receiving community-based case management services are stratified into low-, moderate-, or high-risk groupings that further help identify the duration and level of support they may need.
While staffing varies and always should be individualized, there are some general parameters when staffing for a community-based setting. Many times, these caseloads are based on insurance coverage. Generally, Medicare patients present with clinical issues but also might experience financial or social issues. They represent the highest-risk group.
The second highest-risk group is the Medicaid patients who often present with social and behavioral health and/or chemical dependency issues. The lowest-risk groups are the commercially insured patients as they are employed and tend to be younger and more stable.
Social Workers’ Responsibilities
- Identify, screen, and assess in a timely manner those patients and families/significant others who require social work service consults.
- Integrate the social work plan into overall patient care through interdisciplinary collaboration.
- Provide professional social work services in the areas of comprehensive case management, discharge planning, continuing care services, advocacy, clinical social work services (including crisis intervention), and appropriate education to patients and families/significant others using appropriate modalities.
- Understand and use hospital and community-based resources and government funding. Refer patients, families/significant others, and hospital staff to appropriate services to ensure continuity and quality of care.
- Develop and use specialized knowledge of resources related to the needs of specific patient populations. Facilitate the business department’s efforts to obtain insurance coverage for hospital- and community-based services.
- Document patient care plans, staff interventions, and outcomes promptly and completely in the patient’s medical record. Complete statistical reports as required by the department and other programs.
- Identify service gaps and participate in other hospital and departmental programs to address and improve quality of care.
- Collaborate with case managers to identify, track, and resolve avoidable delay days and saved days throughout the hospital stay.
- Participate in and assume leadership of hospital and departmental committees.
- Collaborate with case managers to ensure complex patients receive appropriate and timely discharge planning.
Summary
Whether in the hospital or in the community, social workers are an integral part of the interdisciplinary care team. Optimizing the skill sets of each discipline is the best way to ensure patients receive the case management services they need and that the professional staff are working at the top of their license.
Social workers are educated in social, family, and stress management, among other skill sets. Below are examples of social work’s areas of expertise:
- biopsychosocial assessments and treatment planning;
- counseling regarding effect of illness and compliance with medical and transitional plans of care;
- crisis intervention regarding abuse and neglect, domestic violence, substance abuse, or trauma;
- identification of barriers to creating a safe and timely discharge plan.
By focusing on these important skill sets, social workers play a vital role in addressing the patient’s social or financial issues that may impede his or her achievement of positive clinical outcomes. Resources are limited in any practice setting, so identification and use of the educational preparation of social workers will result in better patient outcomes and improved job satisfaction for social workers across the continuum of care.
Social workers play a vital role on the interdisciplinary care team across the continuum of care. Working in concert with RN case managers and other members of the healthcare team, they assist in guiding and tracking patients over time through physical health, mental health, and social services, spanning all levels of intensity.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
