Is This Ventricular Tachycardia?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The ECG in the figure below was obtained from an elderly man with chest pain and shortness of breath. Is the rhythm ventricular tachycardia (VT)?
The ECG in the figure shows a regular wide complex tachycardia (WCT) rhythm at a rate of ~150 beats/minute. Sinus P waves are absent because there is no clearly upright P wave in lead II. The small upright deflection seen just before the QRS complex in lead V1 is too close to the QRS complex to be a P wave.
The differential diagnosis of a regular WCT rhythm without sinus P waves includes: VT, supraventricular tachycardia with either aberrant conduction or preexisting bundle branch block, or something else (e.g., a Wolff-Parkinson-White-related arrhythmia or a toxic effect, such as hyperkalemia).
Statistically, the overwhelming majority of WCT rhythms without sinus P waves will turn out to be VT. This is especially true in older individuals with underlying heart disease, in whom 90% or more of the regular WCT rhythms without sinus P waves are the result of VT.
Despite these statistics, I thought the rhythm in the figure was more likely to be supraventricular. QRS morphology is completely typical for right bundle branch block (RBBB) conduction. This is because there is a triphasic (rSR’) complex in lead V1, with the S wave descending below the baseline, and with a characteristic slender and taller terminal R’ complex. In addition, lateral leads I and V6 both manifest tall, slender R waves with terminal S waves. This specific pattern of QRS morphology for RBBB conduction in leads I, V1, and V6 is highly predictive of a supraventricular etiology.
There appears to be two to one atrial activity in several leads. This atrial activity is best seen in the form of two equally spaced, upright notches within each R-R interval in lead III; two rounded negative deflections within each R-R interval in leads II and aVF; and notching at the very end and very beginning of the QRS complex in lead V1.
Since the ventricular rate is ~150 beats/minute and there are two equally spaced atrial deflections, the QRS would be 150 × 2 = 300 beats/minute. The only rhythm that produces regular atrial activity at this fast of a rate is atrial flutter.
I thought the arrhythmia in the figure was most likely to be atrial flutter with two to one AV conduction. This patient was treated with beta-blockers, which resulted in successful conversion to sinus rhythm. The post-conversion tracing showed sinus P waves with an identical-looking QRS complex, which confirmed that the reason for QRS widening in the figure was preexisting RBBB.
For more information about and further discussion of this case, please click here.
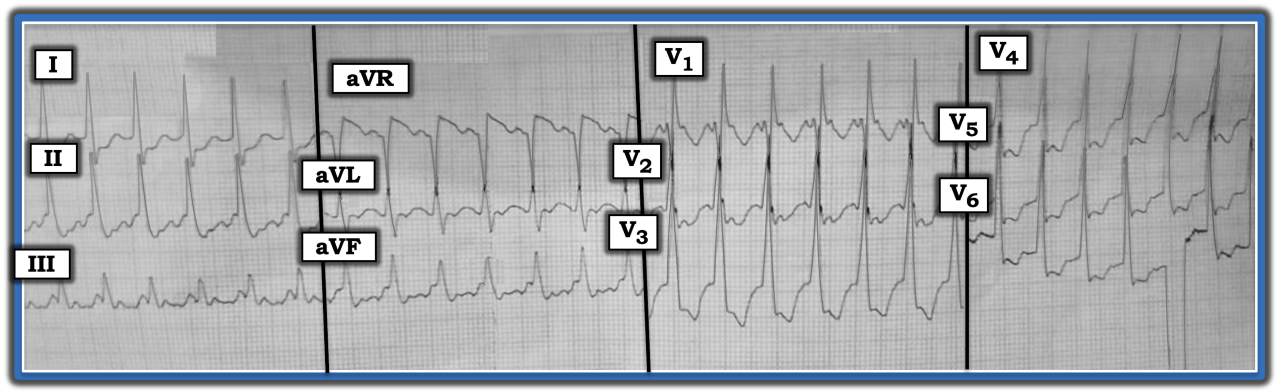
The ECG in the figure was obtained from an elderly man with chest pain and shortness of breath. Is the rhythm ventricular tachycardia?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
