What Is the ‘Bix Rule?’
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The ECG in the figure below was obtained from a middle-aged man with a history of exertional chest pain and dyspnea. How would one interpret this tracing? Does the red arrow in lead II show a sinus P wave?
The red arrow in the figure was thought to be a sinus P wave. Instead, it probably is just one of two P waves that appear within each R-R interval. Normally, the PR interval shortens as the heart rate increases. As a result, it is unusual to see first-degree AV block with sinus tachycardia. Instead, recognition of atrial activity with a long PR interval in a patient with tachycardia (as is seen in the figure) should prompt consideration that a second P wave for each R-R interval may be “hiding” within each QRS complex. Awareness of this probability is known as the “Bix Rule.” This made me strongly suspect the rhythm in the figure was not sinus tachycardia with first-degree AV block, but rather atrial tachycardia with 2:1 block.
In support of my suspicion is the finding of subtle notching on the upstroke of the R wave in lead II, as well as an r’ deflection at the end of the QRS complex that I thought might represent a second P wave in leads III and aVF. Most of the time, distinction between sinus tachycardia and atrial tachycardia with 2:1 block can be determined by further monitoring. If the rhythm is sinus tachycardia, then the rate of the rhythm should slow as the patient’s clinical condition improves. It almost always will become clear within a short period there is only a single P wave for each QRS complex.
Elsewhere, although the QRS complex appears to be slightly widened (i.e., slightly more than half a large box in duration), it does not appear to be wide enough for complete left bundle branch block (LBBB), which requires QRS prolongation to at least 0.12 seconds. Instead, I suspected a combination of left ventricular hypertrophy (LVH) and incomplete LBBB, both of which may account for slight QRS widening.
Also, note there is marked increase in QRS amplitude, with significant “overlap” of R waves and/or S waves in most chest leads. As a result, despite up to 4 mm of ST depression in lead V4 (with significant ST depression also in lateral leads V5 and V6), this amount of ST depression probably is not disproportionate, considering the tremendous increase in QRS amplitude we see in most chest leads. As a result, I attributed the lateral lead ST depression to the combination of LVH and incomplete LBBB, not to ischemia.
I suspect the rhythm in the figure is atrial tachycardia with 2:1 block. In addition, there is marked LVH with LV “strain” and probable incomplete LBBB, but I thought it likely that there were no acute ST-T wave changes. Clinical correlation, further evaluation, and close follow-up will be needed to verify my impression.
For more information about and further discussion of this case, please click here.
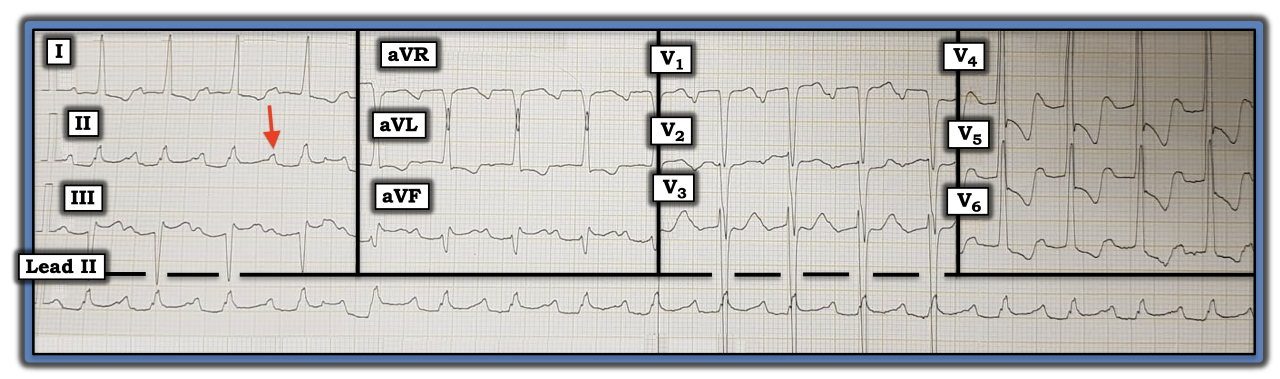
The ECG in the figure was obtained from a middle-aged man with a history of exertional chest pain and dyspnea. How would one interpret this tracing? Does the red arrow in lead II show a sinus P wave?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
