Soft-Tissue Rheumatism: Diagnosis and Management
Soft-Tissue Rheumatism: Diagnosis and Management
Authors: Bradley Andersen, MD, Fellow, Rheumatology, Loma Linda University, Loma Linda, CA; and Keith Colburn, MD, Professor of Medicine, Chief of Rheumatology, Loma Linda University and Loma Linda VA Medical Center, Loma Linda, CA.
Peer Reviewer: John C. Jump, MD, Medical Director, Kettering Medical Center, Department of Physical Medicine and Rehabilitation, Electrodiagnostic Medicine, Kettering, OH.
Soft-tissue rheumatism often is a challenging disorder for the primary care physicians. The patient's symptoms often are vague, and the physical examination and laboratory testing often do not give comforting confirmatory findings. This issue reviews common conditions that afflict many of our patients and that, although often not serious, cause significant distress and morbidity. With the proper history and attention to presenting features, effective and professionally rewarding treatments are available.
The article is outlined principally by the typically affected body partshoulder to footand the PCP will find this organization helpful in the practical workup and treatment of these common conditions.
A non-medical family member from a distant state recently called me asking for my advice regarding his increasingly severe foot pain. He works while on his feet all day as a printer and described pain that was particularly bad in the morning when he first gets out of bed. My immediate impression was plantar fasciitiswhich he promptly wrote downand will take to his doctor for confirmation and treatment. I am waiting patiently to see if my telemedicine diagnosis was correct and if I will garner his unending praise due to my diagnostic acumen.
The Editor
Introduction
Soft-tissue rheumatism comprises a category of disorders that produce pain, swelling, or inflammation not caused by arthritis in the tissues and structures around a joint. The disorders include tendinitis, tenosynovitis, bursitis, capsulitis, enthesitis, myofascial pain syndrome, and fibromyalgia. Pain produced by these disorders is one of the most common and most misunderstood rheumatic complaints encountered by primary care practitioners. The history and, more importantly, the physical examination findings are central to diagnosing soft-tissue rheumatism syndromes because imaging and laboratory tests often are unhelpful.
While the etiologies of localized soft-tissue rheumatism syndromes are not entirely known, most syndromes are associated with repetitive low-grade trauma from mechanical overloading of muscles, tendons, ligaments, and fascia. Subsequent localized inflammation and degradation of the affected sites may be attributed to their poor vascular supply and the slow and often incomplete healing that accompanies decreased circulation. While these disorders can occur in the absence of systemic disease, they are associated with systemic diseases such as rheumatoid arthritis, ankylosing spondylitis, and diabetes mellitus, which produce a generalized vasculopathy. The pathophysiology of regional myofascial pain syndromes and fibromyalgia is unknown. These topics will be discussed in a future article.
Soft-tissue rheumatism syndromes may be either self-limiting or relieved by non-narcotic analgesics and nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs should be given in an analgesic dose range as the increased cardiovascular risk with anti-inflammatory dosage is not likely justified by the benefit. Intralesional corticosteroid injections are particularly effective in patients with localized disorders.
 |
 |
Disorders of the Shoulder
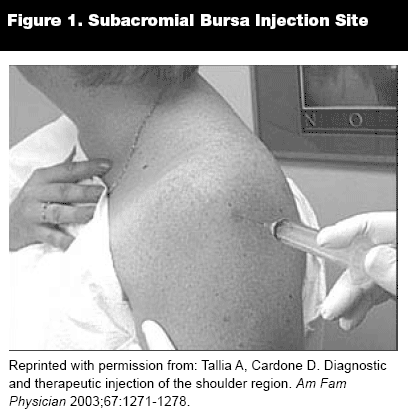
Supraspinatus Tendinitis (Subacromial Bursitis). One of the common causes of shoulder pain is supraspinatus tendinitis with or without co-existing subacromial bursitis. A bursa is a thin synovial membrane-lined sac located in areas of potential friction, i.e., tendon and bone juxtaposition. The subacromial bursa reduces friction between the tendon of the supraspinatus muscle inferiorly and the acromion superiorly. In persons younger than 30 years old, rotator cuff tendinitis often results from an athletic injury in which the arm is in an overhead position. In most individuals aged 25-50 years, there often is an antecedent history of repetitive movements above the head producing repeated episodes of mechanical impingement. In people older than 50 years, chronic supraspinatus tendinitis often is associated with rotator cuff tears.
Patients with supraspinatus tendinitis often complain of anterolateral shoulder pain. The pain often is worse at night when the patient attempts to lie on the affected side. The pain is aggravated by abduction and internal rotation of the shoulder. Patients may have trouble washing their hair or reaching up behind their back while dressing. The patient often notes a catching of the shoulder during use. The painful arch is usually between 60 degrees and 120 degrees of abduction when the greater tuberosity passes under the acromion and the coracoacromial ligament. The patient may have painful passive range of motion and limited active range of motion, especially with abduction. The range of motion often is greater with the shoulder externally rotated (thumb up) than with the shoulder internally rotated (thumb down).
Management for supraspinatus tendinitis includes short periods of rest, physical therapy, and NSAIDs. When these conservative treatments fail, injection of a mixture of corticosteroid and lidocaine into the subacromial bursa may be helpful. This should be combined with 4-7 days of pendulum exercises and avoidance of abduction prior to a program of shoulder strengthening exercises.
Injection Technique. Patient and doctor safety and patient comfort are important when performing injections. A stabilizing point of contact should be maintained while performing injections (not shown in figures). One way of accomplishing this is for a right-handed doctor to hold the syringe firmly in the left hand with the palm up, with the syringe gripped between the middle finger and the thumb, and the index finger placed on the skin about an inch from the injection site. The physician then uses the right hand to guide the needle and inject the medication in the desired location. (A left-handed physician should hold the syringe in the right hand and use the left hand to guide the needle and inject the medication.) This avoids stabbing the patient or oneself with the needle because of the stability of the position of the index finger firmly placed on the patient. A 22- to 27-gauge needle (smaller is better from the patient's perspective) approximately 1.5 inches in length can be used to access the subacromial bursa. With the patient sitting with the hands placed in the lap, the needle is inserted approximately 1 cm inferior to the midpoint of the lateral edge of the acromion. The needle is inserted medially and slightly anterior in a horizontal plane. Inject 1-3 mL of anesthesia (bupivacaine or lidocaine) and 1 mL (40 mg) of steroid preparation. Do not inject if high resistance is encountered.
Rotator Cuff Tear. Rotator cuff tears are found in 20% of people 60-69 years of age and 51% of people older than 80 years. Rotator cuff tears may be extremely painful or barely felt. They may be acute particularly after falling on an outstretched arm or chronic due to chronic impingement and inflammation or repetitive use of the shoulder, such as from pitching baseball, swimming, or playing tennis. Tears may be partial or complete. The physical examination findings of a partial supraspinatus tear often are indistinguishable to examination findings of supraspinatus tendinitis. Patients with partial rotator cuff tears often have weakness of abduction and external rotation in addition to the examination findings of supraspinatus tendinitis mentioned above. Further evidence supporting the diagnosis of a partial-thickness tear is the patient's failure to respond to pharmacologic therapy. Patients with full-thickness tears are unable to initiate shoulder abduction from 0 to 20 degrees. The diagnosis of a rotator cuff tear can be verified with ultrasound, magnetic resonance imaging (MRI) scan, or a shoulder arthrogram. Suspected partial-thickness tears are best verified with an ultrasound. Incomplete tears often are treated by conservative means. Complete tears often require surgical repair, but they often are problematic in older individuals.
Adhesive Capsulitis. Adhesive capsulitis is an idiopathic, painful restriction of all active and passive movements of the glenohumeral joint. Adhesive capsulitis is more common in women than men and usually occurs during or after the fifth decade of life. Diabetes mellitus and thyroid disease (hyper- and hypothyroid) commonly are associated with adhesive capsulitis. Shoulder immobilization due to shoulder trauma or rotator cuff disease may contribute to the development of adhesive capsulitis. Adhesive capsulitis is a self-limiting condition with symptoms lasting between 12 and 42 months. The three phases of adhesive capsulitis are a painful inflammatory phase (2-9 months), an adhesive phase in which pain eases but the shoulder remains frozen (4-12 months), and a recovery phase in which the patient slowly regains shoulder mobility. Patients should be assured that the condition usually resolves spontaneously. Early initiation of physical therapy and possible corticosteroid injection may maintain range of motion and limit pain in the inflammatory phase. Gradual mobilization dictated by the patient's pain tolerance should be encouraged. Manipulation under anesthesia is effective in increasing shoulder mobility for those unable to endure the pain and disability of a frozen shoulder.
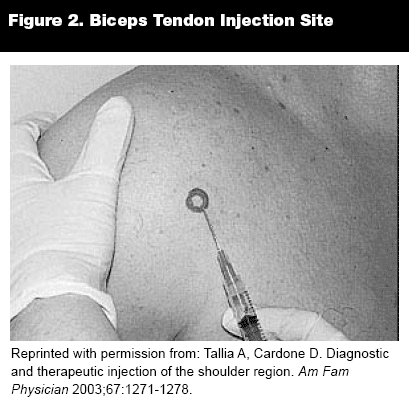
Bicipital Tendinitis. Bicipital tendinitis presents as localized pain and tenderness elicited by palpation over the anterior aspect of the shoulder in the area of the bicipital groove. The pain is aggravated by overhead activities, shoulder extension, and resisted supination or flexion of the forearm. The inflammation of the long head of the biceps tendon and its sheath often is due to impingement beneath the coracoacromial arch. Bicipital tendinitis commonly occurs with rotator cuff impingement syndrome or rotator cuff tear. Conservative treatment includes rest, icing, therapeutic ultrasound, NSAIDs, and corticosteroid injections. Surgical transfer of the tendon may be necessary when these measures fail.
Injection Technique. When performing an injection for biceps tendinitis, care should be taken not to inject the tendon itself as this may result in rupture. With the patient sitting with the hands placed in the lap, palpate the long head of the biceps marking the point of maximum tenderness. Use a 22- to 27-gauge, 1.5-inch needle. Insert the needle directly adjacent to the tendon and inject a fraction of the anesthesia (2-3 mL of bupivacaine or lidocaine) and steroid 1 mL (40 mg). Redirect the needle superiorly and inferiorly along the tendon, injecting further fractions. Injection should be free flowing with little resistance.
 |
 |
Disorders of the Elbow
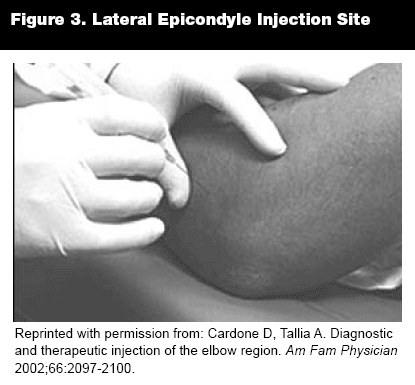
Lateral Epicondylitis (Tennis Elbow). Lateral epicondylitis is the most commonly diagnosed elbow disorder. It presents as a history of work- or activity-related pain around the lateral epicondyle. Lateral epicondylitis affects men and women equally and more commonly after age 40. It is caused by minute tears in the proximal insertion of the extensor muscles of the forearm due to repetitive wrist supination or dorsiflexion (required for a power grip). On physical examination, there is tenderness to palpation 1-2 cm distal to the lateral epicondyle, and lateral elbow pain is produced by supination or wrist dorsiflexion against resistance. Treatment includes watchful waiting with activity modification, both oral and topical NSAIDs, bracing (tennis elbow brace), ultrasonography, iontophoresis, and corticosteroid injections.
Injection Technique. With the elbow flexed and pronated, identify the area of maximal tenderness just proximal to the radial head. Insert a 25-gauge, 1- to 1.5-inch needle perpendicular to the skin down to the level of the bone and then pull back several millimeters. Slowly and evenly inject 1-3 mL of anesthesia (bupivacaine or lidocaine) and 0.5 mL (20 mg) of steroid preparation. Alternatively, one can inject from a point 2-3 cm distal to the lateral epicondyle parallel to the extensor tendons but not into the tendon itself.
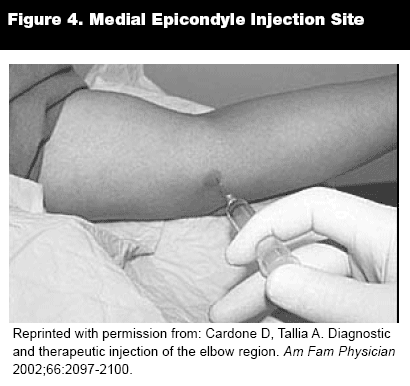
Medial Epicondylitis (Golfer's Elbow). Medial epicondylitis is much less common than lateral epicondylitis. It manifests as medial elbow and proximal forearm pain that occurs with high-speed wrist flexion and forearm pronation. It results from repetitive microscopic tears of the common flexor tendon at the medial epicondyle of the humerus. Patients experience tenderness over the medial epicondyle, and the pain is reproduced with wrist flexion or pronation against resistance. Treatment is similar to that for lateral epicondylitis.
Injection Technique. Corticosteroid injections should remain on the anterior portion of the medial epicondyle as the ulnar nerve runs in the groove posterior to the medial epicondyle. With the elbow flexed and supinated, mark the area of most tenderness just distal to the medial epicondyle. Insert a 25- or 27- gauge, 1- to 1.5-inch needle down to the level of the bone and then pull back several millimeters. Inject 1-3 mL of anesthesia (bupivacaine or lidocaine) and 0.5 mL (20 mg) of steroid preparation. Alternatively, one can inject from 2-3 cm distal to the medial epicondyle parallel to the flexor tendons.
Olecranon Bursitis. Olecranon bursitis is most frequently caused by repetitive mild trauma to the olecranon process. Other etiologies include inflammatory conditions such as gout, pseudogout, rheumatoid arthritis, and infection. In most cases, olecranon bursitis presents with swelling, warmth, and mild pain over the olecranon process. The range of motion of the elbow usually is normal. Septic bursitis causes pain, erythema, and limitations in motion. A bursa that is not painful or erythematous often is treated with aspiration with or without corticosteroid injection. The recurrence rate following aspiration is high, particularly without concurrent remediation of any underlying etiologies. Fluid gram stain and crystal analysis help to differentiate infection from gout or pseudogout. An infected bursa requires either daily aspiration or surgical debridement along with antibiotic treatment.
Injection Technique. With the patient lying supine and the elbow maximally flexed as much as the patient can tolerate without causing discomfort, insert the needle distally into the base of the bursa. A 22- to 27-gauge needle can be used for a non-inflammatory process. If an inflammatory process such as gout is suspected, an 18- or 20-gauge needle frequently is required to aspirate fluid from the bursa. The skin and injection tract should be anesthetized (bupivacaine or lidocaine) when using larger-gauge needles. When the needle is in the correct location, fluid is aspirated easily. For noninfectious process, 0.5-1 ml (20-40 mg) of steroid can be injected.
 |
 |
 |
 |
Disorders of the Hand and Wrist
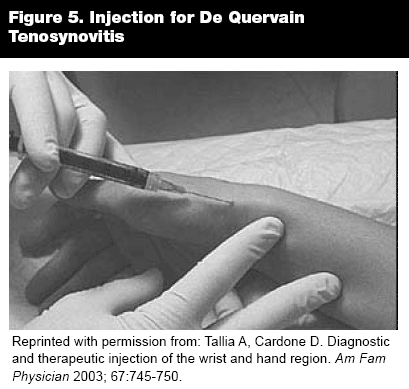
De Quervain Tenosynovitis. De Quervain tenosynovitis is characterized by pain at the radial wrist and the base of the thumb during pinch grip, grasping, and lifting. Repetitive thumb use causes inflammation, thickening, and stenosis of the tendon sheath of the abductor pollicis longus and extensor pollicis brevis tendons. De Quervain tenosynovitis also may occur in association with rheumatoid arthritis, psoriatic arthritis, and pregnancy. The affected tendon usually is tender and often swollen 1-2 cm proximal to the radial styloid. The pain is worsened when patients position their thumbs inside a closed fist and while ulnar deviating the wrist (Finklestein test). Conservative approaches such as ice, thumb spica splinting, and NSAIDs may be considered. A local steroid injection may be the most effective treatment for De Quervain tenosynovitis.
Injection Technique. Mark the most sensitive portion of the tendon. Insert a 25- or 27-gauge, 1-inch needle at a 30- to 40-degree angle into the radial aspect of the anatomic snuffbox parallel to the course of the tendons. Inject 1-2 mL of anesthesia (bupivacaine or lidocaine) and 0.5 mL (20 mg) of steroid preparation. Take care not to inject the tendon itself, which is indicated by high resistance.
Ganglia. Ganglia are unilocular or multilocular cysts found near or attached to tendon sheaths and joint capsules. They occur in adults ages 20-50 years old with higher prevalence in females (3:1 female-to-male ratio). Containing a thick jelly-like fluid, ganglion cysts usually develop spontaneously, possibly due to cumulative trauma. Dorsal wrist ganglions (60-70%) generally stem from the scapholunate joint. Palmar wrist ganglions (20-25%) typically arise from the radiocarpal joint. A small percentage of ganglia are bound to the flexor tendon sheath. Most ganglia are relatively painless and resolve spontaneously. If pressure from a ganglion causes pain or numbness due to peripheral nerve impingement, aspiration with or without injection of a corticosteroid can be effective.
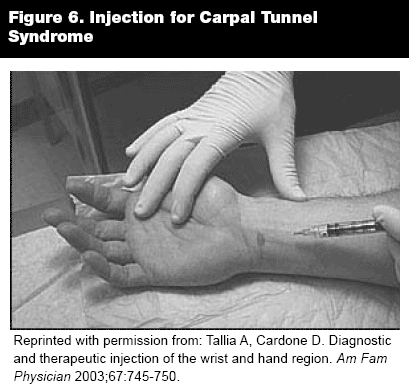
Carpal Tunnel Syndrome. Carpal tunnel syndrome, caused by compression of the median nerve by surrounding structures within the carpal tunnel, most frequently is a result of nonspecific common flexor tenosynovitis possibly due to overuse injury. Other contributing factors in carpal tunnel syndrome include inflammatory conditions (rheumatoid arthritis, psoriatic arthritis, and systemic lupus erythematosus), metabolic disorders (diabetes mellitus, obesity, and hypothyroidism), infections, and pregnancy. The symptoms of burning pain and numbness of the palmar thumb and the index and middle fingers usually are worse at night. The pain may radiate to the forearm, elbow, and shoulder. If the compression is severe, thenar muscle atrophy and loss of grip strength may develop. A sensation of tingling in the distribution of the nerve produced by tapping over the carpal tunnel (Tinel sign) or causing a 90-degree wrist flexion for one minute (Phalen wrist flexion sign) are indicative of carpal tunnel syndrome. For patients unable to flex the wrist due to arthritis, compression of the median nerve for longer than 30 seconds produces the same effect. Electrodiagnostic studies may help in confirming the diagnosis, but results are operator dependent.
Initial treatment should include avoidance of repetitive wrist motions and splinting the wrist in a neutral position. Wrist splinting tends to be more effective if used within three months of the onset of symptoms. Splinting throughout the day provides greater improvement of symptoms, but compliance is improved when splinting is only at night. Other conservative treatments include NSAIDs and corticosteroid injection. In many patients, surgery is eventually required to release the median nerve.
Injection Technique. A 25- to 27-gauge needle approximately 1 inch in length can be used to inject the carpal tunnel. The needle should be inserted at a 30- to 45-degree angle just proximal to the wrist crease and ulnar to the palmaris longus tendon. The needle should be advanced toward the web space between the long and ring finger to a depth of approximately 2 cm. If the needle meets obstruction or if the patient experiences paresthesias, the needle should be withdrawn and redirected to avoid injecting the body of the tendon or the ulnar nerve. Slowly inject 0.5 cc bupivacaine or lidocaine and 0.5 mL (20 mg) of steroid preparation.
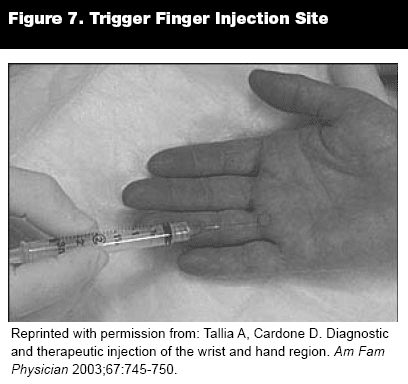
Stenosing Digital Tenosynovitis (Trigger Finger). Trigger finger occurs when a tendon cannot glide within its sheath because of a nodular thickening or stenosis at the first annular (A-1) pulley of the digit. This most commonly is due to repetitive strain injury with gripping activities. Secondary causes include inflammatory arthritis, diabetes mellitus, hypothyroidism, and infections. Patients complain that their fingers catch or lock in a flexed position when a portion of tendon becomes unable to move distal to the pulley. Many times the finger must be extended manually. Conservative therapy includes NSAIDs, restriction of gripping activities, and splinting. Kneading massage along the tendon sometimes may reduce the degree of nodularity. Corticosteroid injections into the tendon sheath are effective. Surgical release of the A-1 pulley rarely is needed.
Injection Technique. With the hand supinated and fingers extended, palpate for an area of swelling at the proximal palmar crease of the finger. After marking the area, introduce a 25- to 27-gauge, 5/8- to 1-inch needle at a 30- to 40-degree angle, directing the needle either proximally or distally toward the area of swelling. Inject 0.25 mL of methylprednisolone (80 mg/mL). Do not inject if high resistance is encountered.
Dupuytren Contracture. Dupuytren disease is a fibroproliferative thickening and shortening of the fibrous aponeurotic sheets that lie superficial to the flexor tendons and small muscles of the hand. It presents as a palmar nodule that, in time, develops into a cord. This cord gradually contracts, leading to contracture of the fingers. The fingers most commonly affected are the ring and little fingers, followed by the long and index fingers. The disease is more common in men older than 40 years of Celtic or Scandinavian origins. There is an association with diabetes, smoking, alcohol intake, manual labor, and possibly anticonvulsant medications. Radiation therapy and corticosteroid injections may provide some relief in early stages of disease. Referral to a hand surgeon is necessary when the metacarpophalangeal joint is contracted 30 degrees or when the proximal interphalangeal joint is contracted.
Disorders of the Hip
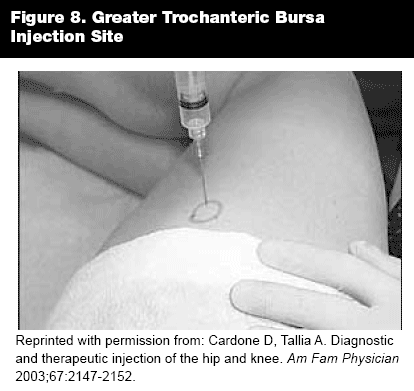
Trochanteric Bursitis. Trochanteric bursitis presents as acute or chronic pain over the greater trochanter and the lateral thigh and often is confused with hip joint pain, which usually is felt in the groin and high buttock. Trochanteric bursitis is caused by either overuse or strenuous activity. Pain often prevents patients from lying on the affected hip. The greater trochanter is tender to palpation, and the pain may be increased with abduction of the hip against resistance. Contributing factors include leg-length discrepancy, scoliosis, obesity, and osteoarthritis of the lumbar spine or hip. Treatment includes rest, physical therapy, exercises stretching the iliotibial band, NSAIDs, and corticosteroid injection.
Injection Technique. With the patient in a lateral recumbent position with the affected hip up, mark the area of greatest tenderness over the greater trochanter. Use a 1.5- to 3-inch, 22- or 25-gauge needle. Insert the needle perpendicular to the skin until the trochanter is reached and then withdraw the needle slightly. Inject a portion of the anesthesia (3-5 mL of bupivacaine or lidocaine) and corticosteroid 1 mL (40 mg). Redirect the needle superior, inferior, anterior, and posterior in the area of a quarter injecting further fractions of the medication.
Iliopectineal (Iliopsoas) Bursitis. When inflamed, the iliopectineal bursa located anterior to the hip joint causes groin and anterior thigh pain and sometimes groin swelling just lateral to the femoral pulse. The bursa becomes more tense and painful with passive hip hyperextension and sometimes flexion of the hip against resistance. To relieve the pain, patients may position the affected hip in 20-30 degrees of flexion. Injection of corticosteroid into the bursa is effective but should be performed by a specialist such as a rheumatologist, a pain specialist, or an orthopedic surgeon.
Ischial (Ischialgluteal) Bursitis. Ischial bursitis, or weaver's bottom, is caused by trauma or prolonged sitting on hard surfaces especially in thin individuals. Patients present with pain and sometimes swelling over the ischial tuberosity radiating down the posterior thigh. Palpation should be done with the hip flexed as this moves the gluteus maximus off the tuberosity. Treatment includes soft-seated cushions, avoidance of extended sitting, NSAIDs, and corticosteroid injections.
Piriformis Syndrome. Piriformis syndrome develops when the sciatic nerve is either compressed or irritated by the piriformis muscle. The chief symptom is buttock pain, sometimes with radiation down the posterior thigh and lower leg. It is most frequently associated with blunt, local trauma. Patients may walk with the hip externally rotated. This reduces the stretch on the piriformis and relieves pain. The pain often can be aggravated by passive flexion, adduction, and internal rotation (FAIR test) of the hip joint. Patients often experience tenderness with palpation of the sciatic notch or while sitting with a wallet in the rear pocket. Treatment of piriformis syndrome consists of stretching exercises, ice and heat, ultrasound, and, in more refractory cases, image-guided corticosteroid injections.
 |
 |
 |
 |
Disorders of the Knee
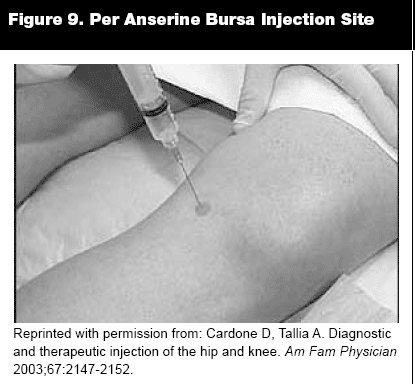
Anserine Bursitis. The pes anserine bursa lies beneath the conjoined tendons of the sartorius, gracilis, and semitendinosus muscles on the anteromedial portion of the proximal tibia. Along with knee flexion, these muscles protect the knee against rotary and valgus stress. Anserine bursitis usually results from anatomic strain on this conjoined tendon from osteoarthritis of the knee or strain from obesity. Patients with anserine bursitis complain of medial knee pain that often is worse when knees touch while lying on one's side or when getting up from a seated position. It predominantly affects middle-age to elderly women. On examination, patients have tenderness and sometimes slight swelling over the medial aspect of the knee an inch or two below the joint line. No knee joint effusion is present. Resisted knee flexion and valgus stress testing may aggravate the pain. Treatment consists of rest, physical therapy, NSAIDs, and corticosteroid injections.
Injection Technique. With the patient placed in the supine position, locate the point of maximal tenderness an inch or two below the medial joint line. A 1.5-inch, 22-gauge needle is inserted perpendicular to the tibia down to the bone and withdrawn slightly. Inject 1-3 mL of anesthesia (bupivacaine or lidocaine) and 1 mL (40 mg) of steroid preparation. Reposition the needle if high resistance is encountered.
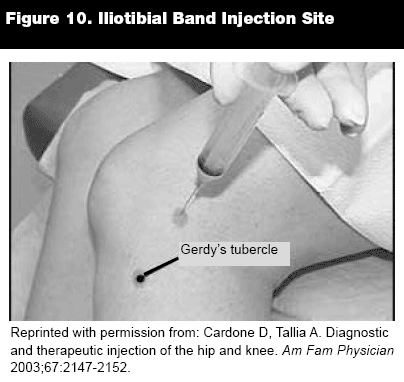
Iliotibial Band Syndrome. Iliotibial band syndrome is an overuse syndrome caused by excessive friction between the distal segment of the iliotibial band and the prominence of the lateral femoral condyle. Patients with iliotibial band syndrome describe diffuse pain over the lateral aspect of the knee joint after having completed activities with repetitive flexion and extension such as running or cycling. Physical examination reveals tenderness over the lateral tibial condyle of the femur or Gerdy's tubercle. The pain is worst when the patient is standing or the knee is in 30 degrees of flexion. Treatment consists of avoidance of repetitive flexion and extension, stretching of the iliotibial band and strengthening of the hip abductors, NSAIDs, and corticosteroid injections.
Injection Technique. With the patient placed in the supine position and the knee slightly flexed, locate the most tender site over the lateral tibial condyle. A 1.5-inch, 22- to 27-gauge needle is inserted perpendicular to the skin down to the bone and withdrawn slightly. Inject 1-3 mL of anesthesia (bupivacaine or lidocaine) and 1 mL (40 mg) of steroid preparation.
Popliteal Cysts (Baker Cysts). Almost all popliteal cysts develop from synovial herniation into the popliteal fossa due to increased synovial fluid in the knee joint. Conditions associated with popliteal cysts include osteoarthritis, rheumatoid arthritis, and injury of the meniscus, cruciate ligaments, or cartilage. Patients present with a minimally tender bulge in the popliteal space behind the knee. A ruptured cyst may dissect down the calf causing calf pain, swelling, and redness that mimic a deep venous thrombosis. Thrombosis may develop if the cyst compresses the popliteal vein. Definitive diagnosis of a popliteal cyst can be made with ultrasound. Conservative therapy includes correction of the intra-articular pathology, avoidance of traumatic activities to the knee, NSAIDs, and injection of corticosteroid. Surgical excision may be required in large symptomatic popliteal cysts.
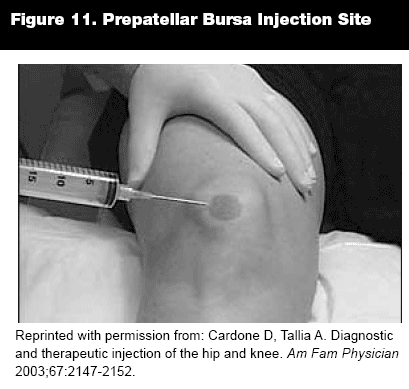
Prepatellar Bursitis (Housemaid Knee). Prepatellar bursitis presents as swelling and mild tenderness on the lower half of the anterior patella. The usual cause of prepatellar bursitis is repeated minor injuries from frequent kneeling. Less common causes include gout, pseudogout, and infection. Aspiration of the prepatellar bursa provides relief of discomfort and is important to rule out septic bursitis. Because the bursa does not communicate with the knee joint, septic bursitis can be treated with oral antibiotics for the organism cultured. For sterile bursitis, injection with corticosteroid is helpful. Individuals such as carpet layers or housemaids who chronically kneel should be advised to use knee pads.
Injection Technique. With the patient lying in the supine position, insert a 1- to 1.5-inch needle into the base of the inferior edge of the bursa. As in olecranon bursitis, use a 22- to 27-gauge needle for anesthesia in a non-inflammatory process and an 18- to 20-gauge needle to aspirate fluid in an inflammatory process. Anesthetize the skin and injection tract (bupivacaine or lidocaine) when using larger-gauge needles to aspirate fluid from the bursa. If injecting 1 mL (40 mg) of corticosteroid, use a hemostat to stabilize the needle while exchanging syringes.
 |
 |
Disorders of the Ankle and Foot
Achilles Tendinitis and Tendinosis. Achilles tendinitis, seen most often in athletes, typically presents with exercise-related burning posterior leg or heel pain. It also may occur with inflammatory conditions including spondyloarthropathies, rheumatoid arthritis, pseudogout, and repeated trauma from shoes rubbing over the base of the Achilles tendon. Tenderness, pain, and swelling occur approximately 2-3 cm proximal to the tendon insertion site. Pain is increased with dorsiflexion of the foot. Achilles tendinosis is a painless thickening and degeneration of the tendon commonly seen in middle-aged to elderly people as a result of recurrent micro-tears and vascular compromise. Conservative treatment for both conditions includes correct footwear, heel lifts, a splint with plantar flexion, careful stretching of the tendon, and weight loss.
Degeneration from chronic tendinitis or tendinosis, corticosteroid use, and fluoroquinolone-type antibiotics may predispose patients to Achilles tendon ruptures. It is not wise to inject corticosteroids around the Achilles tendon. Patients with Achilles tendon rupture report a feeling of being shot or kicked in the back of the leg. Failure of the normal foot plantar flexion when an examiner squeezes the calf (Thompson test) indicates an Achilles tendon rupture.
Retrocalcaneal Bursitis. Retrocalcaneal bursitis is an inflammation of the bursa situated between the calcaneus and the Achilles tendon insertion site. Middle-aged and elderly patients are most often affected. Patients complain of pain around the insertion of the Achilles tendon often made worse by wearing shoes. On examination, patients have a tender erythematous swelling "pump bump" at the insertion of the Achilles tendon. Treatment includes using a heel cup, wearing an open-back shoe, and stretching the tendon. Injection with corticosteroid is contraindicated as this may produce Achilles tendon rupture.
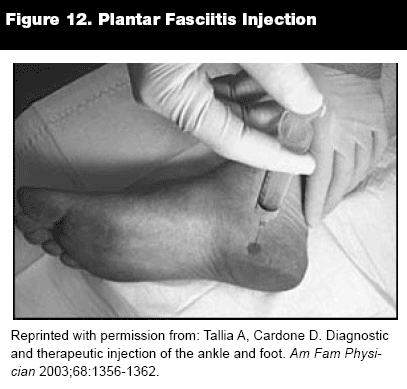
Plantar Fasciitis. Plantar fasciitis is degeneration of the dense tissue extending from the calcaneus to the metatarsal region due to repetitive use or excessive load on the fascia. Risk factors include obesity, employment involving prolonged standing, pes planus, and limited ankle mobility. Patients report burning or lancing plantar heel pain that is most prominent with the first few steps in the morning or after a period of sitting. The pain may be increased when walking barefoot or up stairs. The patient has tenderness in the region of the medial calcaneal tuberosity, and the pain increases with passive dorsiflexion of the foot. Treatment consists of shoe inserts, stretching exercises, night splints, and corticosteroid injections.
Injection Technique. With the patient lying in a supine position, locate the point of maximal tenderness distal to the calcaneus. Insert a 25-gauge, 1.5-inch needle perpendicular to the skin into the medial aspect of the heel as close as possible to the plantar surface of the calcaneus. Advance the needle 1/4 to 1/2 inch in depth. Do not inject into the heel fat pad as this may cause fat pad atrophy. Inject 1 mL of anesthesia (bupivacaine or lidocaine) and 1 mL (40 mg) of steroid preparation.
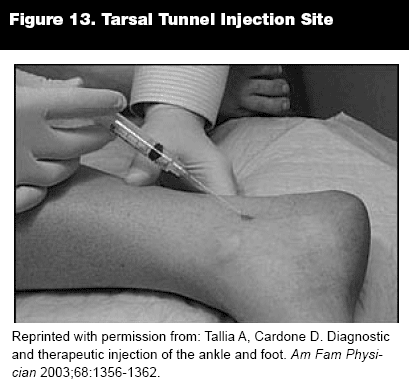
Tarsal Tunnel Syndrome. Tarsal tunnel syndrome is caused by compression of the posterior tibial nerve as it passes posterior and inferior to the medial malleolus. Patients present with burning pain and numbness felt from the medial malleolus radiating to the plantar heel and less often to the distal sole and toes. Percussion of the nerve may elicit a positive Tinel sign. Symptoms may be replicated with dorsiflexion and eversion of the foot. Treatment of this condition includes rest, changing shoes, strengthening exercises, NSAIDs, and corticosteroid injections. Surgery often is needed to decompress the nerve and provide relief.
Injection Technique. With the patient lying on the side with the affected foot down, mark the area just inferior and posterior to the medial malleolus. A 25- to 27-gauge, 1-inch needle is inserted at a 30-degree angle to the skin surface in a distal direction. Inject 0.5-1 mL of anesthesia and steroid 0.5 mL (20 mg). Take care not to inject the nerve that lies posterior to the posterior tibial tendon.
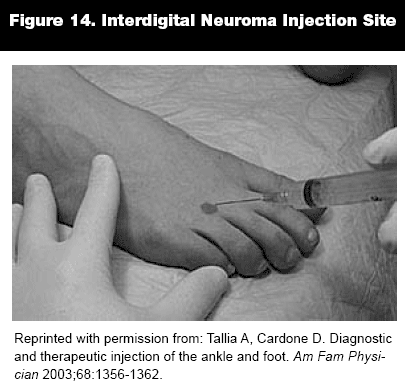
Morton Neuroma. Morton neuroma is an entrapment neuropathy of the interdigital nerve secondary to repetitive irritation of the nerve. This condition usually occurs in middle-aged women who wear high heels and tight-fitting shoes. The most common presenting complaint is a burning, aching pain with paresthesias located between the metatarsals and surrounding digits. The interdigital space of the third and fourth toes usually is affected. Firm squeezing of the metatarsal heads elicits pain in the affected interdigital space. Pain may be aggravated by passive and active toe dorsiflexion. Treatment consists of a metatarsal bar and shoes with a wide toe box, preferably without heels. A corticosteroid injection in the web space of the toe where the tenderness is palpated may be helpful.
Injection Technique. With patient lying in a supine position, the knee flexed, and the foot flat on the table, locate the area of tenderness in the dorsal interdigital space. A 25-gauge, 1-inch needle is inserted at a 45-degree angle to the skin surface, ½ to 1 inch between the metatarsal heads. Inject 0.5 cc of bupivacaine or lidocaine and 0.25 to 0.5 mL of steroid (10-20 mg).
Summary
Learning to manage soft-tissue rheumatic disorders can provide expedient and much-needed relief to patients who otherwise may suffer for prolonged periods waiting to see a specialist to perform procedures that a skilled primary care doctor can do. For difficult cases or cases that require skills not yet acquired, referral to a specialist is the best option.
References
1. Harris ED, et al. Kelley's Textbook of Rheumatology, 7th edition. Philadelphia: Elsevier Saunders; 2005:601-636.
2. Fam A, Lawry G, Kreder H. Musculoskeletal Examination and Joint Injection Techniques, Philadelphia: Mosby Saunders; 2006
3. Rakel R, et al. Conn's Current Therapy, Philadelphia: Elsevier Science; 2006:1203-1207.
4. Pile K, Kennedy L. Problem Solving in Rheumatology, Oxford: Atlas Medical Publishing; 2008: 11-37.
5. Cipriano J. Photographic Manual of Regional Orthopaedic and Neurological Tests, 4th edition. Philadelphia: Lippincott Williams & Wilkins; 2003:106-227, 326-421.
6. Reveille J. Soft-tissue rheumatism: Diagnosis and treatment. Am J Med 1997;102 (suppl 1A): 23S-29S.
7. Tallia A, Cardone D. Diagnostic and therapeutic injection of the shoulder region. Am Fam Physician 2003;67:1271-1278.
8. Cardone D, Tallia A. Diagnostic and therapeutic injection of the elbow region. Am Fam Physician 2002;66:2097-2100.
9. Slawson D. Best treatment for de Quervain's tenosynovitis uncertain. Am Fam Physician 2003;16:102-106.
10. Mazzone M, McCue T. Common conditions of the Achilles tendon. Am Fam Physician 2002;65:1805-1810.
11. Aldrige T. Diagnosing heel pain in adults. Am Fam Physician 2004;70:332-338.
12. Tallia A, Cardone D. Diagnostic and therapeutic injection of the ankle and foot. Am Fam Physician 2003;68:1356-1362.
13. Cardone D, Tallia A. Diagnostic and therapeutic injection of the hip and knee. Am Fam Physician 2003;67:2147-2152.
14. Tallia A, Cardone D. Diagnostic and therapeutic injection of the wrist and hand region. Am Fam Physician 2003;67:745-750.
15. Townley W, Baker R, Sheppard N, et al. Dupuytren's contracture unfolded. BMJ 2006;332:397-400.
16. Trojian T, Chu S. Dupuytren's disease: Diagnosis and treatment. Am Fam Physician 2007;76:86-89, 90.
17. Chumbley E, O'Connor G, Nirschl R. Evaluation of overuse elbow injuries. Am Fam Physician 2000;61:691-700.
18. Calmbach W, Hutchens M. Evaluation of patients presenting with knee pain: Part II. Differential fiagnosis. Am Fam Physician 2003;68:917-922.
19. Chakrabarty S, Zoorob M. Fibromyalgia. Am Fam Physician 2007;76:247-254.
20. Fritschy D, Fasel J, Imbert J, et al. The popliteal cyst. Knee Surg Sports Traumatol Arthrosc 2006;14:623-628.
21. Viera A. Management of carpal tunnel syndrome. Am Fam Physician 2003:68:265-272, 279-280.
22. Cole C, Seto C, Gazewood J. Plantar fasciitis: Evidence-based review of diagnosis and therapy. Am Fam Physician 2005;72:2237-2242, 2247-2248.
23. Johnson G, Cadwallader K, Scheffel S, et al. Treatment of lateral epicondylitis. Am Fam Physician 2007;76:843-848, 849-850; 853.
Soft-tissue rheumatism often is a challenging disorder for the primary care physicians. The patient's symptoms often are vague, and the physical examination and laboratory testing often do not give comforting confirmatory findings. This issue reviews common conditions that afflict many of our patients and that, although often not serious, cause significant distress and morbidity. With the proper history and attention to presenting features, effective and professionally rewarding treatments are available.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
