Hypertension Update
Hypertension Update
Author: Sula Mazimba, MD, Associate Clinical Professor of Medicine, Wright State Boonshoft School of Medicine, Dayton, OH.
Peer Reviewer: Norman Kaplan, MD, Professor of Internal Medicine, Department of Internal Medicine, University of Texas Southwestern Medical School, Dallas, TX.
Hypertension is one of the most common conditions that primary care physicians face on a daily basis in the office. Control of hypertension is one of the most important therapeutic actions that the physician can do to prevent the development of serious complications in his or her patients. Increasing scrutiny of the physician's success in this arena is being measured by third-party payers with the expectation of high performance. This issue reviews the recommendations of the Seventh Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. The topics covered include:
measurement-how pressure should be determined;
definition-what are the classifications;
white coat syndrome and ambulatory measurements-recognition;
risk assessment-how to determine the overall risk stratification;
laboratory evaluations-defining the tests that should accompany diagnosis;
causes-identifying the common and rare causes;
treatment-highlights the lifestyle modifications and pharmacotherapy options;
associated conditions-related conditions commonly associated with hypertension, such as diabetes and congestive heart failure.
-The Editor
Introduction
Hypertension is one of the leading primary risk factors for cardiovascular disease (CVD) and a leading cause of death in developed countries.1 Hypertension was estimated to contribute to about 50% of CVD worldwide as reported by the 2002 global burden of disease study.2 It is also one of the most important treatable risk factors contributing to cerebrovascular disease, the third leading cause of death, and a major cause of disability in U.S. adults.3 Approximately 65 million Americans during the time period 1999-2000 were reported by the National Health and Nutrition Examination Survey (NHANES) 1999-2000 data to have hypertension.4
Hypertension is defined as systolic blood pressure (SBP) of at least 140 mmHg and/or diastolic blood pressure (DBP) of at least 90 mmHg, or blood pressure (BP) that is controlled to guideline-recommended level using at least one antihypertensive medication. The prevalence of hypertension in the U.S. adult population has been increasing. The age-standardized prevalence rate for the U.S. adult population has increased from 28.8 % to 32.6% between the NHANES III (1988-1994) and the NHANES (1999-2004).5 The increase in the prevalence rate of hypertension can been attributed to several factors, including the rising percentage of Americans who are overweight or obese. An estimated 65% of the U.S. adult population had excess weight in 1999-2000, compared with 56% in 1994-1998.6 Aside from the impact of obesity on the prevalence rates of hypertension in the US, the growing elderly U.S. population has led to the increase in the prevalence of hypertension. BP generally increases with age to the point at which more than 50% of adults between the ages of 60 and 69 years had elevated BPs, while 75% of those aged 70 years and above had hypertension.7
The Framingham Heart Study reported that the lifetime risk of developing hypertension in nonhypertensive individuals who were between the ages of 55 and 65 who survived to the ages of 80 and 85 was about 90% in both men and women. The scope of the problem of hypertension also highlights some interesting challenges and gaps in healthcare delivery in the United States. According to the NHANES 1999-2000, of all the patients who had hypertension, 70% were aware of their diagnosis and 59% were on treatment. Only 34% of the individuals were adequately controlled on medications to the target goal of SBP less than 140 mmHg and DBP less than 90 mmHg.8 Uncontrolled hypertension leads to increased risk of ischemic heart disease (IHD) and stroke. In one meta-analysis study involving about one million patients, there was a linear increase in the risk of IHD and stroke as BP increased from values as low as 115 mmHg SBP and 75 mmHg DBP.9 The relative risk of dying from CVD is twice as high in individuals with SBP values between 130-139 and DBP 85-89 compared to individuals with normal blood pressures.10 These findings led to the recent reclassification of hypertension by the Seventh Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7).
Classification
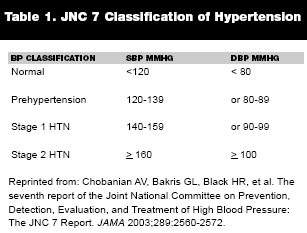
The JNC 7 has established a new type of classification for hypertension intended to capture individuals whose blood pressure may be regarded as "normal" but are at increased risk of overall mortality and disability from cardiovascular diseases. This is in keeping with longitudinal studies like the Framingham Heart Study, which showed that there is a double increase in mortality in individuals with SBP between 130-139 and DBP between 85-89.They added a new category called " prehypertension" with the intention of capturing this high-risk category of patients who otherwise would be dismissed as having "normal" BP levels. The prehypertension category identifies individuals in whom lifestyle modifications can be employed and the risk of progression of hypertension curtailed.8 There are three stages of hypertension in the classification adopted by the JNC 7. Normal blood pressure is classified as SBP below 120 and DBP less than 80. Prehypertension is SBP between 120-139 and DBP 80-89. Stage 1 hypertension is SBP between 140-159 and DBP 90-99. Stage 2 has been reclassified to include SBP equal or above 160 mmHg and DBP equal or above 100 mmHg.
Systolic and Diastolic Hypertension
It previously was thought that DBP was a more important risk factor for CVD than SBP.11 More recent studies are showing that SBP may be an even stronger predictor of CVD risk. DBP, however, is a more potent risk factor for CVD than SBP below the age of 50; thereafter, SBP assumes a greater risk than DBP.12
Isolated systolic hypertension is common in the elderly, partly because of the vascular rigidity and reduced compliance of the arterial vasculature that comes with the aging process.13 It has been shown that both SBP and DBP increase with age until about the fifth decade, when DBP begins to fall. The most plausible explanation for this decline in diastolic BP with age is the increased arterial stiffness, which causes a more rapid return of the reflected wave from the periphery so that it augments pressure during systole rather than during diastole, raising the systolic and lowering the diastolic pressure.14 The decrease in the DBP and increase in SBP with age means that pulse pressure (PP) rises with age. Thus, above the age of 60, PP and SBP becomes major predictors of cardiovascular risk.12 In the elderly, isolated SBP is very common. There is evidence to suggest that aggressive treatment of isolated SBP lowers total overall mortality, cardiovascular mortality, and heart failure.15,16 Thus attention must be paid to treating SBP to target goal in this age group.
 |
Measurement of Hypertension
The correct diagnosis and treatment of BP depends on obtaining accurate and valid BP measurements from a well functioning and adequately calibrated BP measuring device. The JNC 7 recommends that the patient be well rested, be seated for at least 5 minutes, and have legs resting on the floor and the arm supported at heart level. A mercury sphygmomanometer usually is preferred for accuracy; however, due to concerns with mercury spillages, an aneroid manometer is a good alternative if it is well calibrated. Electronic devices are being used more widely. At least two measurements should be taken two minutes apart for each visit, and the average value should be determined.17 The cuff must be the right size for the patient. The correct cuff should cover at least 80% of the arm. When using the manual method of measuring BP, the radial pulse must be palpated prior to applying the cuff pressure, and the pressure at which the pulse is obliterated when the cuff is inflated should be noted. This gives an estimation of the SBP. The cuff pressure at this point then is inflated 20-30 mmHg above the pressure point used to obliterate the radial pulse, before auscultation. When deflating the cuff, the rate of deflation should not exceed 2 mmHg per second. SBP is noted at the point of the appearance of the first Korotkoff sounds and DBP at the point of disappearance of the sounds.8 It is important to measure BP in both arms for individuals presenting for the first time for evaluation.
White Coat Hypertension and Masked Hypertension
In most individuals, BP measured in the office is higher than their readings at home or on a 24-hour ambulatory BP monitor. This phenomenon is termed the white coat effect. If the readings in the office are above 140/90, but are below 130/85 out of the office, isolated office hypertension or white coat hypertension is present. In some studies, data indicate that individuals with white coat hypertension have higher CVD risk than normotensive individuals, although their risk is lower than that of individuals with established hypertension.18 Conversely, there also are data showing that some individuals have normal BP readings in the office even though their home or ambulatory readings may be high. This is referred to as "masked hypertension." Masked hypertension is noted in as many as one-fifth of hypertensive patients.19 These individuals have a higher cardiovascular risk than individuals with white coat hypertension.20 They also may be predisposed more to target organ damage than normotensive individuals.21 Physicians should be alert to this condition, especially with hypertensive target organ damage that cannot be explained by the degree of office BP measurements.
Ambulatory Measurements
In some cases, it may be important to measure a patient's BP levels during his or her normal daily routine. This is done with an ambulatory blood pressure monitoring device (ABPM). Ambulatory BP values are usually lower than office BP measurements. Hypertension is diagnosed when the average BP readings are greater than 135/85 mmHg when awake and more than 120/75 mmHg during sleep.8
 |
 |
Individuals whose 24-hour ambulatory readings exceeded 135/85 mmHg have a two-fold greater risk of cardiovascular events than those with BP values lower than 135/85 mmHg.22 Indications for ABPM are listed in Table 3.
Patient Evaluation
The objectives of hypertensive patient evaluation are three-fold:
Assess the patient's lifestyle risk factors, cardiovascular risk factors, and co-morbid conditions that may help guide treatment plan;
Identify secondary causes of hypertension; and
Assess the level of target organ involvement.
Risk Assessment
Risk assessment involves taking a detailed history and physical examination. A detailed medical history should focus on obtaining information about the presence of pre-existing medical conditions such as diabetes, dyslipidemias, cardiovascular accidents, peripheral vascular disease, and renal disease. A careful review of medications is important, and the physician should inquire about the use of oral contraceptive pills (OCP), steroids, as well as over-the-counter medications such as nasal drops and non-steroidal anti-inflammatory drugs (NSAIDs).
The physician must ask about the use of street drugs such as cocaine and amphetamines, which can cause difficult-to-control BP.
Lifestyle habits such as the use of tobacco or alcohol, level of physical activity, dietary salt use, and sleep patterns (including snoring) must be identified.
 |
The physical examination should identify possible identifiable causes of HTN (see Table 4) while at the same time attempting to elicit end organ involvement. Attention should be paid to calculating the body mass index (BMI), and waist circumference should be measured.
 |
The physical examination should include evaluation of the thyroid, lungs, heart, abdominal masses (polycystic kidneys), presence or absence of edema in the lower extremities, as well as listening for abdominal (evidence of renal or general atherosclerosis) and carotid bruits. End organs damage should be assessed carefully. These target organs include: eyes (fundoscopy), kidneys (urinalysis look for proteinuria, red blood cell casts), central nervous system (neurological deficits), aorta (assess for pulsatile abdominal masses), and heart (left ventricular enlargement, heart failure).
See figure 1 (PDF).
Heart rate must be measured for at least 30 seconds or a full minute in the presence of an arrhythmia. Heart rate has been shown to provide prognostic information. Patients with a higher resting heart rate may be at risk for cardiovascular disease.23 Patients with reduced heart variability also have been shown to have higher a CV mortality rate.24
Laboratory Evaluation
The recommended laboratory tests include 12 lead ECG, urinalysis, and a basic chemistry panel looking at serum potassium, glucose, calcium, and creatinine. It must be noted that serum creatinine may not be very sensitive in estimating renal function; however, it can be used in the Cockroft-Gault formula to estimate creatinine clearance. A fasting lipoprotein profile that includes HDL and LDL cholesterol and triglycerides must be measured. Other optional tests that can be done in selected patients include a dip stick urinalysis that measures microalbuminuria. High sensitivity C-reactive protein and homocysteine levels may be considered in some patients with CVD without the traditional risk factors.
Screening for identifiable causes of hypertension is indicated only in situations where there is a strong indication to suspect secondary causes of hypertension or in cases in which BP has been difficult to control. Otherwise, testing for secondary causes of hypertension is not recommended routinely.
Identifiable Causes of Hypertension
This accounts for about 10% of all causes of hypertension. Extensive screening is not recommended unless there is suspicion from the laboratory tests or clinical presentation. Some of the factors that should prompt a physician to look for these secondary causes include:
Onset of hypertension before the age of 30 or after the age of 55.
Uncontrolled hypertension or hypertension that was previously controlled and suddenly becomes resistant to medications.
Worsening of renal function with initiation of angiotensin converting enzymes inhibitor (ACEI) or angiotensin receptor blocker (ARB) medications. In this situation, suspect the presence of bilateral renal artery stenosis. A renal ultrasound with Doppler flow should be ordered.
In hypertension with unprovoked hypokalemia, suspect mineralcorticoid excess and measure 24-hour urinary aldosterone level or plasma aldosterone and renin activity ratio.
Suspect pheochromocytoma when hypertension is labile and is associated with paroxysmal headaches, palpitations, or profound sweating. Evaluate by measuring 24-hour urinary metanephrines or normetanephrines.
Patients with recurrent flash pulmonary edema, sometimes found with renovascular hypertension.
Cushing syndrome must be suspected if the patient has the characteristic features such as truncal obesity, purple abdominal striae, and buffalo hump against the background of glucose intolerance. Measure a 24-hour urinary cortisol or dexamethasone suppression test to assess for this disorder.
Hypertension in the setting of hypercalcemia should lead to investigation for hyperparathyroidism, and serum intact parathyroid hormone (PTH) level should be ordered.
Hyperthyroidism as a cause of hypertension should be suspected if patients show signs of thyrotoxicosis such as sweating, palpitations, heat intolerance, and weight loss. Measure thyroid stimulating hormone (TSH), free T3, and T4 if indicated.
It is important to consider obstructive sleep apnea in patients who are obese with resistant hypertension. A detailed history regarding habits such snoring, daytime somnolence, and irregular breathing patterns including episodes of apnea should be sought from the partner. A sleep study for confirmation is indicated.
In patients with decreased pulses in the lower extremities or delayed femoral pulses when compared to the radial pulse, one should consider a possibility of coarctation of the aorta. Evaluate with CT angiography of the aorta.
Treatment
Multiple studies have documented that treatment of hypertension reduces overall mortality rate and CVD complications.25,26 Nonetheless, the majority of Americans with hypertension are untreated or undertreated.
The goal of treatment is to reduce the SBP to less than 140 mmHg and DBP to less than 90 mmHg. Target goals are lower for specific patient groups, such as those with co-morbid diabetes or renal disease. In these patients, the target goal of SBP reduction is less than 130 mmHg and DBP to less than 80 mmHg.26-28 Beside the ultimate goal of reducing the absolute levels of systolic and diastolic pressures, it is also important for physicians to help their patients reduce their overall CVD risk profile. There is a tendency for clustering of other risk factors in patients with hypertension. The INTERHEART study conducted in 52 countries showed that 9 out of 10 cases of acute myocardial infarctions could be attributed to various combinations of the 9 modifiable risk factors.27
Lifestyle Modifications
Lifestyle modification should be recommended for all hypertensive patients as an integral part of treatment.28 Some of the lifestyle changes that should be promoted include physical activity, smoking cessation, weight reduction, and dietary modifications including a reduction in salt intake. It was shown in one study that weight loss can reduce the incidence of hypertension by as much as 77%, while a low-salt diet reduced the incidence of hypertension by 35%.29 Adoption of a diet that is rich in vegetables, fruits, and nuts and low in saturated fats has been shown to reduce BP and augment the effects of anti-hypertensive medications. In the Dietary Approaches to Stop Hypertension (DASH) diet, a diet rich in fruits, vegetables, and low-fat dairy products but low in saturated and trans fats has been shown to lower incidence of hypertension. The effect of the DASH diet in lowering BP was comparable to that seen with a single antihypertensive drug.30 Patients must be encouraged to quit smoking and, if they use alcohol, to drink moderately, which is defined as no more than two drinks per day for men and no more than one drink per day for women.
Pharmacotherapy
There are five main classes of drugs that often are used in treating hypertension: calcium channel blockers (CCB), beta blockers (BB), angiotensin converting enzyme inhibitors (ACEI), aldosterone receptor blockers (ARB), and thiazide diuretics. Other classes include alpha-1 receptor blockers such as doxazosin; aldosterone antagonists such as spiranolactone; direct vasodilators such as hydralazine; central alpha-2 agonists and other centrally acting medications such as clonidine and methyldopa. In addition, the direct renin inhibitor aliskiren is available.
There still are controversies regarding whether absolute BP reduction is the main benefit of all drugs or whether, indeed, there are clinically relevant class effects that may be important, independent of BP-lowering effect.31 More than 60% of hypertensive patients will need more than one agent to control their blood pressure.32 In patients with lower BP target goals, such as those with diabetes or kidney disease, three or more drugs may be needed. The JNC 7 recommends a thiazide diuretic as initial therapy. This recommendation comes, in part, from evidence provided by the finding of the Antihypertensive and Lipid Lowering treatment to prevent Heart Attack Trial (ALLHAT).33 This was a multicenter study with a population of more than 40,000 patients that was designed to compare three antihypertensive drugs: doxazosin, an alpha antagonist; lisinopril, an ACEI; and amlodipine, a CCB agonist with a thiazide diuretic (chlorithalidone) as initial therapy in individuals older than 55 years of age who had one additional CVD risk factor. Those receiving doxazosin had a higher incidence of heart failure, and that arm of the study was prematurely stopped.
The study showed that there was no difference in mortality and CHD among ACEI, CCB, and the thiazide diuretic. There was, in fact, a lower incidence of heart failure in those receiving the thiazide. In general, most patients tolerate thiazide diuretics well, although at higher doses the antihypertensive effect plateaus and side effects increase.34 Some of the adverse effects of thiazides are metabolic abnormalities such as hyperglycemia and erectile dysfunction.35 Although thiazide diuretics are inexpensive and well tolerated when compared to other classes of drugs, they remain underutilized.33 The JNC 7 recommends the addition of a second drug from another class if initial therapy does not adequately control the blood pressure to the recommended target levels. Multiple drug therapy in the control of hypertension has been shown to effectively lower BP, usually at relatively low doses of the individual drugs, thus resulting in fewer side effects.36 The use of fixed-dose combinations is not only cost effective but may increase compliance as well. Choice of the second class of medication depends, in part, on the coexisting medical conditions.
Diabetes and Hypertension
The coexistence of diabetes with hypertension increases the risk of developing renal disease and overall CVD mortality.37 The United Kingdom Prospective Diabetes Study (UKPDS) demonstrated that a reduction of SBP by 10 mmHg was associated with about a 15% reduction in diabetes mortality.38
The JNC 7 recommends that the treatment goal for hypertension in diabetic patients should be SBP less than 130 and DBP less than 80. In the HOPE trial of diabetic patients with high CVD risk, the addition of an ACEI reduced the risk of stroke by 33% and death by 25%.39 An ACEI can be used as initial therapy or second-line therapy in combination with a thiazide diuretic. For the prevention of microvascular complications in diabetic type 2 patients with kidney disease, use of either an ACEI or an ARB is recommended to prevent the progression of renal disease.40
Hypertension and Heart Failure
Heart failure (HF) leads to a reduction in cardiac output that leads to activation of the renin-angiotensin-aldosterone (RAA) and sympathetic nervous system. The activation of the RAAS attempts to compensate for the reduced cardiac output by vasoconstriction that leads to increased venous return and sodium retention, which leads to volume expansion. The overall long-term effects of an activated RAAS leads to cardiac remodeling, ventricular enlargement and fibrosis, and excess fluid retention, with the resultant effects of worsening HF and hypertension. Therefore, hypertensive patients with HF benefit from ACEIs, ARBs, and BBs, which help modulate the ill effects of these hormones.41 BBs temper the effects of an activated sympathetic system on the vasculature, and ACEIs and ARBs curb the effects of angiotensin II and aldosterone. HF patients also have been shown to benefit from thiazide diuretics.
By the same token, an aldosterone antagonist such as spironolactone is useful in patients with advanced HF.42 Aldosterone antagonists also are effective in the treatment of resistant hypertension.43
Hypertension and Cerebrovascular Disease
Hypertension is a major risk factor for stroke. It appears that thiazide diuretics, CCBs, and ARBs provide better stroke protection than BBs.44,45 A recent meta-analysis by Lindholm and colleagues showed that BBs are not as effective as other antihypertensive drugs in reducing the risk of stroke. They found that BBs had a 16% higher relative risk of stroke when compared to other agents.46 This may be explained by the fact that BBs lower the brachial pressures (peripheral) but do not lower central aortic pressures, which is a much stronger risk factor for stroke.47 It should be noted that the addition of a diuretic to an ACEI in the PROGRESS trial resulted in more than a 40% reduction in stroke recurrence.48
Hypertension and Kidney Disease
In patients with uncontrolled hypertension, the rate of renal function decline with age is much steeper than in those with normal pressures.49 Therefore, the target goal for SBP in patients with chronic kidney disease (CKD) is SBP less than 130 mmHg and diastolic less than 80 mmHg. ACEIs or ARBs slow the progression of renal decline in patients with diabetic nephropathy.50
Resistant Hypertension
Resistant hypertension is defined as failure to achieve the target goal of blood pressure in patients who are taking at least 3 drugs in adequate doses with a regimen that includes a diuretic and proper adoption of lifestyle modification. In these patients, it is important for the physician to ensure that the BP is measured correctly. If so, then consider evaluating for secondary causes of hypertension. It is important for the physician to inquire about over-the-counter medications, such as NSAIDs, that might increase blood pressure. Asking specifically about dietary and herbal supplements is important because some patients may not be willing to volunteer this information. Some herbal supplements, such as St John's wort, may increase blood pressure.
There are data showing that the addition of an aldosterone antagonist such as spironolactone is helpful in controlling resistant hypertension.46
Hypertensive Emergencies
Hypertensive emergencies occur when BP elevation is associated with acute damage of end organs and, therefore, requires prompt reduction of blood pressure to limit organ damage. Some examples are hypertensive encephalopathy, hypertensive left ventricular failure, dissection of the aorta, pulmonary edema, and angina. Hypertensive urgencies, on the other hand, are situations in which BP is severely elevated but there is no evidence of progressive organ damage. Patients with hypertensive emergencies should be admitted to an intensive care unit, and the goal of BP treatment should be a gradual decrease. If the BP is brought down suddenly, it may precipitate organ ischemia due to reduced tissue perfusion. It is advisable, therefore, to lower BP by no more than 25% over an hour initially and then slowly over the next 24-48 hours.8 Medications used to treat hypertensive emergencies include vasodilators such as sodium nitroprusside, which acts immediately and is titrated as a drip. In the use of nitroprusside, care must be taken in patients with renal impairment because of the risk of thiocyanate poisoning. Monitoring of thiocyanate levels is indicated if the drug is given longer that 48 hours. Other vasodilators that can be used include nitroglycerin, especially in the setting of coronary heart disease or myocardial ischemia. The CCB nicardipine can be used in most hypertensive emergencies but is contraindicated in HF syndromes. Another class of medications used in hypertensive emergencies is adrenergic blockers, which include labetalol or esmolol.
Hypertensive emergencies have high mortality if not well treated, with 50% of individuals dying within 12 months.51 On the other hand, hypertensive urgencies can be treated with short-acting oral agents such as labetalol, and the patient can be discharged if the blood pressure comes down.
Summary
Hypertension remains a major public health problem not only in the United States, but globally as well. Primary care providers play a pivotal role in treating patients with hypertension. Unfortunately the vast majority of hypertensive patients are not even close to the recommended treatment goals. In the past, emphasis was placed on aggressively treating DBP while not paying much attention to SBP. SBP, however, is a greater risk for CVD than DBP, especially in the elderly population. Intensive treatment of hypertension is essential to reduce the burden of CVD morbidity and mortality.
To adequately control BP, most patients will require at least 2 medications. In addition, careful attention must be paid to special groups of patients such as diabetics and those with renal disease who require treatment to lower treatment goals. Efforts must be made to address the global risks of patients with hypertension, which tends to cluster with other medical conditions such as obstructive sleep apnea, metabolic syndrome, and diabetes.
References
1. MacMahon S, Alderman MH, Lindholm LH, et al. Blood-pressure-related disease is a global health priority. J Hypertension 2008;26:2071-2072.
2. World Health Organization. The World Health Report. Reducing risks, promoting healthy life. http://www.who.int/whr/en. 2002.
3. American Heart Association. Heart Disease and stroke statistics-2008 update. Dallas, Texas: America Heart Association; 2008.
4. Fields LE, Burt VL, Cutler JA, et al. The burden of adult hypertension in the United States 1999-2000: A rising tide. Hypertension 2004;44:398-404.
5. Cutler JA, Sorlie PD, Wolz M, et al. Trends in hypertension prevalence, awareness, treatment, and control rates in the United States: Adults between 1988-1994 and 1999-2004. Hypertension 2008;52: 818-852.
6. Hedley AA, Ogden CL, Johnson CL, et al .Prevalence of overweight and obesity among US children and adolescents and adults, 1999-2002. JAMA 2004;291:2847-2850.
7. Burt VL, Whelton P, Roccella EJ, et al. Prevalence of hypertension in the US adult population. Results from the Third National Health and Nutrition Examination Survey, 1998-1991. Hypertension 1995;25:305-313.
8. Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The JNC 7 Report. JAMA 2003;289:2560-2572.
9. Lewington S, Clarke R, Qizilbash N, et al. Age-specific relevance of usual blood pressure to vascular mortality: A meta-analysis of individual data for one million adults in 61 prospective studies. Prospective Studies Collaboration. Lancet 2002;360:1903-1913.
10. Vasan RS, Larson MG, Leip EP, et al. Impact of high-normal blood pressure on the risk of cardiovascular disease. N Engl J Med 2001;345:1291-1297.
11. Pachon V. A new approach to sphygmomanometry. Presse Med 1913;12:229-331.
12. Franklin SS, Larson MG, Khan SA, et al. Does the relation of blood pressure to coronary heart disease risk change with aging? The Framingham Heart Study. Circulation 2001;103:1245-1249.
13. Franklin SS, Gustin W IV, Wong ND, et al. Hemodynamic patterns of age-related changes in blood pressure. Circulation 1997;96:308-315.
14. Safar ME. Pulse pressure in essential hypertension: Clinical and therapeutical implications. J Hypertens 1989;7:769-776.
15. Kostis JB, Davis BR, Cutler J, et al. Prevention of heart failure by antihypertensive drug treatment in older persons with isolated systolic hypertension. SHEP Cooperative Research Group. JAMA 1997;278:212-216.
16. SHEP Cooperative Research Group. Prevention of stroke by antihypertensive drug treatment in older persons with isolated systolic hypertension. Final results of the Systolic Hypertension in the Elderly Program (SHEP). JAMA 1991;265:3255-3264.
17. Perloff D, Grim C, Flack J, et al. Human blood pressure determination by sphygmomanometry. Circulation 1993;88:2460-2470.
18. Verdecchia P, Reboldi GP, Angeli F, et al. Short and long term incidence of stroke in white coat hypertension. Hypertension 2005;45:203-208.
19. Wing LM, Brown MA, Beilin LJ, et al. "Reverse white-coat hypertension" in older hypertensive. J Hypertens 2002;20:639-644.
20. Mancia G. Reversed white-coat hypertension: Definition, mechanisms and prognostic implications. J Hypertens 2002;20:579-581.
21. Liu JE, Roman MJ, Pini R, et al. Cardiac and arterial target organ damage in adults with elevated ambulatory and normal office blood pressure. Ann Intern Med 1999;131:564-572.
22. Verdecchia P. Prognostic value of ambulatory blood pressure: Current evidence and clinical implications. Hypertension 2000;35:844-851.
23. Gillman MW, Kannel WB, Belanger A, et al. Influence of heart rate on mortality among persons with hypertension: The Framingham Study. Am Heart J 1993;125:1148-1154.
24. Tsuji H, Venditti FJ Jr, Manders ES, et al. Reduced heart rate variability and mortality risk in an elderly cohort. The Framingham Heart Study. Circulation 1994;90:878-883.
25. Hansson L, Zanchetti A, Carruthers SG, et al. Effects of intensive blood-pressure lowering and low-dose aspirin in patients with hypertension: Principal results of the Hypertension Optimal Treatment (HOT) randomized trial. HOT Study Group. Lancet 1998;351:1755-1762.
26. American Diabetes Association. Treatment of hypertension in adults with diabetes. Diabetes Care 2003;26:S80-S82.
27. Yusuf S, Hawken S, Ounpuu S, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): Case-control study. Lancet 2004;364:937-952.
28. Whelton PK, He J, Appel LJ, et al. Primary prevention of hypertension: Clinical and public health advisory from The National High Blood Pressure Education Program. JAMA 2002;288:1882-1888.
29. He J, Whelton PK, Appel LJ, et al. Long-term effects of weight loss and dietary sodium reduction on incidence of hypertension. Hypertension 2000;35:544-549.
30. Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med 2001;344:3-10.
31. Kaplan NM, Opie LH. Controversies in hypertension. Lancet 2006;367:168-176.
32. Cushman WC, Ford CE, Cutler JA, et al. Success and predictors of blood pressure control in diverse North American settings: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). J Clin Hypertens (Greenwich) 2002;4:393-404.
33. Psaty BM, Manolio TA, Smith NL, et al. Time trends in high blood pressure control and the use of antihypertensive medications in older adults: The Cardiovascular Health Study. Arch Intern Med 2002; 162:2325-2332.
34. Black HR. The evolution of low-dose diuretic therapy: The lessons from clinical trials. Am J Med 1996;101:47S-52S.
35. Grimm RH Jr, Grandits GA, Prineas RJ, et al. Long-term effects on sexual function of five antihypertensive drugs and nutritional hygienic treatment in hypertensive men and women. Treatment of Mild Hypertension Study (TOMHS). Hypertension 1997;29:8-14.
36. Law MR, Wald NJ, Morris JK, et al. Value of low dose combination treatment with blood pressure lowering drugs: Analysis of 354 randomized trials. BMJ 2003; 326: 1427-1434.
37. [No authors listed.] Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. UK Prospective Diabetes Study Group. BMJ 1998;317:703-713.
38. Adler AI, Stratton IM, Neil HA, et al. Association of systolic blood pressure with macrovascular and microvascular complications of type 2 diabetes (UKPDS 36): Prospective observational study. BMJ 2000;321:412-419.
39. Heart Outcomes Prevention Evaluation Study Investigators. Effects of ramipril on cardiovascular and microvascular outcomes in people with diabetes mellitus: Results of the HOPE study and MICRO-HOPE sub study. Lancet 2000;355:253-259.
40. Remuzzi G, Schieppati A, Ruggenenti P. Clinical practice: Nephropathy in patients with type 2 diabetes. N Engl J Med 2002;346:1145-1151.
41. The European Trial on Reduction of Cardiac Events with Perindopril in Stable Coronary Artery Disease investigators. Efficacy of perindopril in reduction of cardiovascular events among patients with stable coronary artery disease: Randomized, double-blind, placebo-controlled, multicentre trial (the EUROPA Study). Lancet 2003;362:782-788.
42. Pitt B, Zannad F, Remme WJ, et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J Med 1999;341:709-717.
43. Canzanello VJ, Jensen PL, Schwartz GL. Are aneroid sphygmomanometers accurate in hospital and clinic settings? Arch Intern Med 2001;161:729-731.
44. Messerli FH, Grossman E, Lever AF. Do thiazide diuretics confer specific protection against strokes? Arch Intern Med 2003;163:2557-2560.
45. The ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs. diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA 2002;288:2981-2997.
46. Lindholm L H, Carlberg B, Samuelsson O, et al. Should beta blockers remain first choice in the treatment of primary hypertension? A meta-analysis. Lancet 2005;366:1545-1553.
47. Williams B, Lacy PS, Thom SM, et al. Diff erential impact of blood pressure-lowering drugs on central aortic pressure and clinical outcomes: Principal results of the Conduit Artery Function Evaluation (CAFE) study. Circulation 2006;113: 1213-1225.
48. PROGRESS Collaborative Group. Randomized trial of a perindopril-based blood-pressure-lowering regimen among 6,105 individuals with previous stroke or transient ischemic attack. Lancet 2001;358:1033-1041.
49. Bakris GL, Williams M, Dworkin L, et al. Preserving renal function in adults with hypertension and diabetes: A consensus approach. National Kidney Foundation Hypertension and Diabetes Executive Committees Working Group. Am J Kidney Dis 2000;36:646-661.
50. Maki DD, Ma JZ, Louis TA, et al. Long-term effects of antihypertensive agents on proteinuria and renal function. Arch Intern Med 1995;155:1073-1080.
51. Keith NH, Wagnere HP, Barker MW. Some different types of essential hypertension: Their course and prognosis. Am J Med Sc 1939;197;332-343.
Hypertension is one of the most common conditions that primary care physicians face on a daily basis in the office. Control of hypertension is one of the most important therapeutic actions that the physician can do to prevent the development of serious complications in his or her patients.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
