Pediatric Manifestations of Group A Streptococcal Disease
June 1, 2014
Reprints
Pediatric Manifestations of Group A Streptococcal Disease
Executive Summary
- Group A streptococcus (GAS) may cause disease both by direct infection, termed "suppurative disease," and also by the response of the body to an antecedent infection, termed "nonsuppurative disease." An invasive GAS infection is defined as one in which GAS can be isolated from a part of the body that is normally sterile, as would be the case in pneumonia but not in pharyngitis.
- A typical presentation of GAS pharyngitis begins with fever and sore throat. Other typical features include tonsillar exudates, tender and enlarged anterior cervical lymph nodes, and the notable absence of cough and coryza, which are hallmarks instead of viral pharyngitis.
- Most prevalent in 2- to 5-year-olds, impetigo begins as papules that progress to vesicles with erythematous bases.
- The clinical presentation of streptococcal infection in the nasopharynx of the young child is a subacute and protracted course, often ≥ 4 weeks long, consisting of intermittent symptoms of fever, coryza, cervical adenopathy, thin mucopurulent nasal discharge, gastrointestinal upset, and sometimes pharyngeal erythema.
- Young children and infants may become infected with GAS perianally, resulting in a painful, erythematous, and well-circumscribed dermatitis surrounding the child’s anus.
The gram-positive bacterium Streptococcus pyogenes (Group A streptococcus; GAS) is capable of causing a wide array of diseases in the pediatric population, many of which often prompt caretakers to seek emergency medical care for their children.1,2 GAS disease may be as minor as a routine sore throat or as life-threatening as necrotizing fasciitis, as obvious as a rash or as subtle as an aching joint. Illnesses caused by GAS have been with us since antiquity, and despite millennia of attention and treatments, the bacterium still possesses the ability to thrive in seemingly any body tissue and in any age group.3 GAS is almost certain to be a consistent presence in every emergency department, and its capacity to cause serious disease mandates a solid understanding of its diverse possible manifestations and their appropriate treatments.
— Ann M. Dietrich, MD, Editor
Introduction
GAS as an entity consists of a multitude of strains, and these are most often distinguished from one another by "emm typing," a process that separates strains based on the variability in the sequence of the gene coding for the GAS M protein virulence factor. Although more than 200 emm types are known, any one geographic area will typically circulate only a small subset of these. For instance, more than 95% of GAS disease in temperate, industrialized countries is caused by only 25 emm types of GAS, but this does not hold in other regions.4 While outbreaks of GAS may each be linked to specific emm types, this relationship is not consistent across time or geography, and invasive disease may be caused by many various emm types, unpredictably.5 GAS strain differentiation based on emm type is useful for clinical research and epidemiology, but it does not currently influence clinical practice. In a clinical setting, all strains of GAS may be treated the same way, but it is imperative not to confuse GAS with group B streptococci (Streptococcus agalactiae; GBS), Streptococcus pneumoniae, or other medically important species of streptococci.
GAS may cause disease both by direct infection, termed "suppurative disease," and also by the response of the body to an antecedent infection, termed "nonsuppurative disease."3 Streptococcal pharyngitis is the most common example of a suppurative GAS illness, and acute rheumatic fever is the most common example of nonsuppurative GAS disease. A further distinction is drawn among the suppurative diseases, between "invasive" and "noninvasive" infections. An invasive GAS infection is defined as one in which GAS can be isolated from a part of the body that is normally sterile, as would be the case in pneumonia but not in pharyngitis (See Figure 1).6
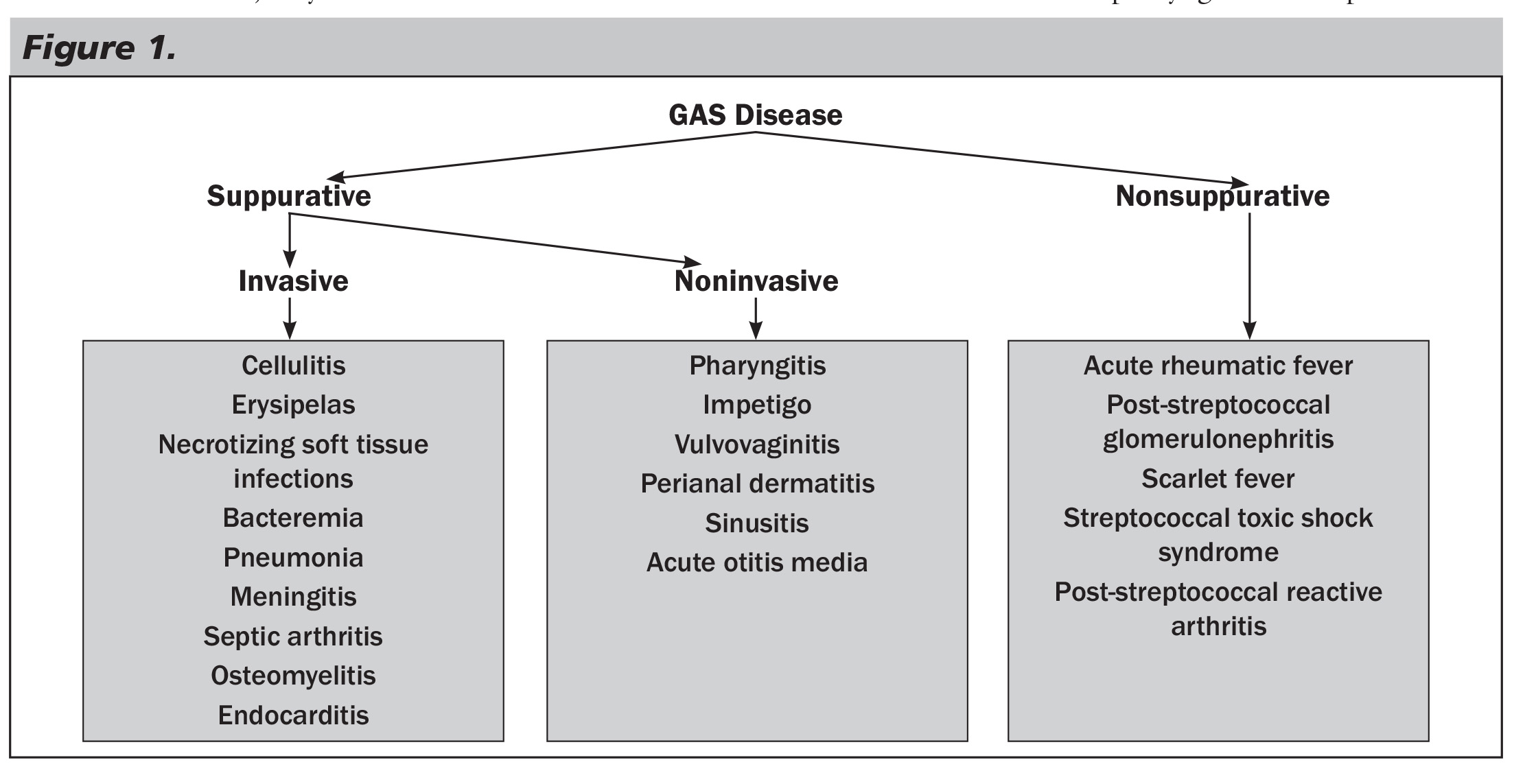
Suppurative GAS infections most often take the form of minor disease of the mucosa and skin, while invasive GAS can be life-threatening. The CDC estimates an incidence of more than 10 million cases of noninvasive GAS infection in the United States each year, primarily pharyngitis and impetigo, in contrast to approximately 10,000 annual cases of invasive GAS infection.7 Within the United States, nonsuppurative GAS disease is even more rare, with a total yearly incidence of a few thousand cases at most, though nonsuppurative disease is far more prevalent in the developing world, with acute rheumatic fever alone being two to five times more common in less-industrialized nations.8-10
GAS is primarily a pathogen of humans, and it is most commonly transmitted via direct contact or respiratory droplet. Though other animals may become infected or colonized with GAS, they do not substantively contribute to the human epidemiology of the bacterium. It is also important to note that GAS can exist with humans in an asymptomatic carrier state, and studies have measured a 10-20% rate of incidental pharyngeal colonization in school-aged children.11,12 Though GAS can at times be detected on inanimate environmental objects, it dessicates within hours and does not typically spread efficaciously via fomites. GAS can, however, infect via the ingestion of contaminated foods, and well-documented outbreaks have occurred by this mechanism.13
Suppurative Disease: Noninvasive Infections
Pharyngitis. Streptococcal pharyngitis ("strep throat") is the most well-known noninvasive infection caused by GAS. Pharyngitis is diagnosed in approximately 11-15 million patients per year in United States ambulatory and emergency settings, and of the pediatric presentations, 20-30% are caused by GAS, making it the most common bacterial etiology of pharyngitis.1,14 Despite this, it is important to note that most cases of pharyngitis are viral in origin. GAS pharyngitis is most prevalent in children 5-15 years of age, and it most frequently occurs in the winter to spring season.14 GAS pharyngitis is very rare in children younger than 3 years of age, and the disease need not be considered in this population, especially since children of such an age are at nearly no risk for the infamous sequelae of GAS infection.14-16
A typical presentation of GAS pharyngitis begins with fever and sore throat. Other typical features include tonsillar exudates, tender and enlarged anterior cervical lymph nodes, and the notable absence of cough and coryza, which instead are hallmarks of viral pharyngitis. GAS pharyngitis may also be accompanied by malaise, headache, and vomiting.2,17
Although clinical signs and symptoms describe many cases of GAS pharyngitis, they are not specific enough to establish the diagnosis in the absence of laboratory confirmation, and current guidelines advocate the use of bacteriologic testing before treatment in suspected cases of GAS pharyngitis.14,18,19 In pediatric patients presenting with signs and symptoms that are convincingly consistent with a viral etiology of pharyngitis, both testing and treatment for GAS should not be undertaken. If GAS pharyngitis is being considered, the patient first may be tested with a throat swab and rapid antigen detection test. Although the rapid antigen tests typically have only a 70-90% sensitivity, their fast turnaround times make them a useful first-line test. If this test is negative, a reflex bacterial culture should be performed. Treatment should not be undertaken until a positive test result is obtained.14
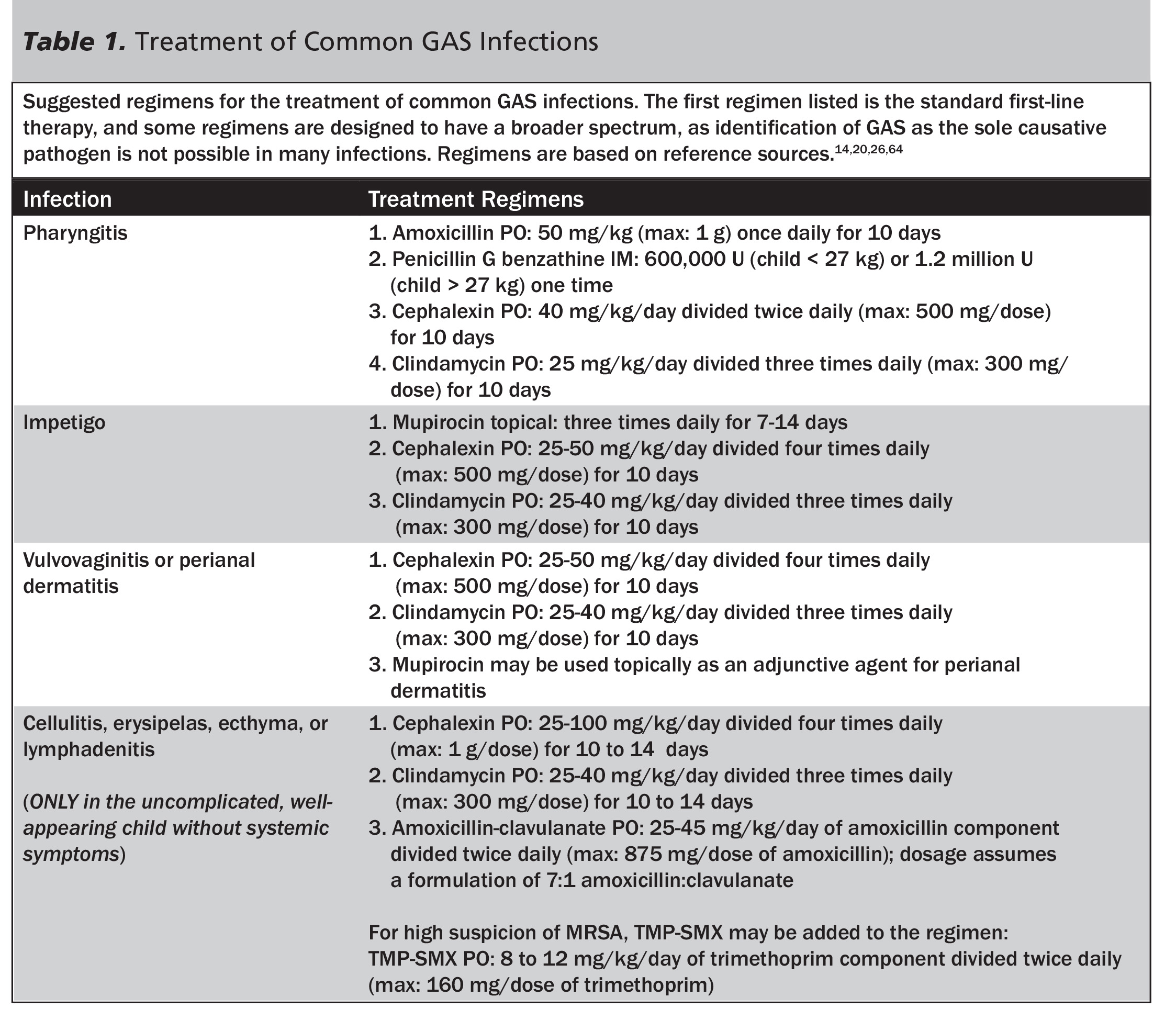
When GAS pharyngitis is confirmed, treatment with an appropriate antibiotic is indicated (see Table 1). Left to its own devices, GAS pharyngitis typically runs an uncomplicated and self-limited clinical course of only 5 days. However, the diagnosis and treatment of GAS pharyngitis is intended to accomplish three things: 1) prevention of post-infectious sequelae, such as acute rheumatic fever, 2) reduction of symptom length, and 3) reduction in GAS transmission. Penicillin, administered either intramuscularly or orally, is as effective now as historically, and there are no reports of penicillin-resistant GAS. Amoxicillin once daily also may be given, and this is a more palatable and common choice. For penicillin-allergic patients, a cephalosporin such as cephalexin may be used. In patients who cannot tolerate any beta-lactam antibiotic, either clindamycin or azithromycin may be used, though there are strains of GAS that are resistant to each of these antibiotics. A prudent treatment course is 10 days in length, and the data for short-course antibiotic treatment are not accepted by all authorities.20 If treatment adherence is suspected to be a problem, consideration of intramuscular penicillin is warranted, as a single injection will suffice. Children may return to school or daycare after 24 hours of antibiotic therapy, as there is insignificant disease transmission after this point.14,21-23 Children who are asymptomatic chronic pharyngeal carriers of GAS typically do not need treatment, provided they are otherwise well. Similarly, neither testing nor treatment is necessary for the asymptomatic contacts of children diagnosed with GAS pharyngitis.14,20
Impetigo (pyoderma). Impetigo, also known as pyoderma, is a superficial skin infection that is typically caused by either GAS or Staphylococcus aureus. Most prevalent in 2- to 5-year-olds, impetigo begins as papules that progress to vesicles with erythematous bases. These lesions are frequently observed on the face (periorally and nasally) and extremities, and they soon unroof to leave erosions that crust over with a classic "golden" or "honey-crusted" appearance. Impetigo may also present with bullae, in which case it is unlikely to be caused by GAS but rather by S. aureus. Impetigo is unlikely to present with fever or other systemic illness.2,24
Differential diagnosis for impetigo includes atopic or contact dermatitis, scabies, herpes, and Stevens-Johnson syndrome. Additionally, if an impetiginous lesion extends through the dermis, it may be reclassified as "ecthyma" and it may be accompanied by fever or other signs of more serious illness.
While the strains of GAS that cause impetigo frequently differ from those that cause pharyngitis and invasive disease, they are all sensitive to penicillin.25 However, given the significant proportion of impetigo cases caused by S. aureus, it is also mandatory to cover this organism. When the impetiginous lesion is confined to a small area and there are no signs of systemic illness, impetigo may be treated with topical agents. Mupirocin may be used topically, 2-3 times per day for 1-2 weeks. If the impetigo is more extensive or is unresponsive to topical treatment, therapy with oral antibiotics should be undertaken. Acceptable antibiotic regimens include 10 days of amoxicillin-clavulanate, cephalexin, or clindamycin.26 If community-acquired Methicillin-resistant S. aureus (MRSA) is common in the patient’s region, extra consideration should be given to the use of clindamycin or to the combination use of cephalexin with trimethoprim-sulfamethoxazole (see Table 1).
GAS in the Young Child. Of special note, while GAS is unlikely to cause typical pharyngitis in children younger than 3 years old, it may still infect their upper respiratory tract, causing an illness notably dissimilar to GAS pharyngitis. The clinical presentation of streptococcal infection in the nasopharynx of the young child is a subacute and protracted course, often ≥ 4 weeks long, consisting of intermittent symptoms of fever, coryza, cervical adenopathy, thin mucopurulent nasal discharge, gastrointestinal upset, and sometimes pharyngeal erythema.27
While this form of nasopharyngeal streptococcal infection has been well-described and studied since the 1940s, it now commands little attention, primarily because the life-threatening sequelae of GAS disease are rare in children younger than 3 years old.16 However, identification and treatment of GAS nasopharyngeal disease in young children may hasten symptom resolution and prevent transmission to other family members. Diagnosis may be established by either pharyngeal or nasal swab, though the latter may be more sensitive in young children.15 Treatment is identical to that for GAS pharyngitis.
Vulvovaginitis and Perianal Infection. Though seldom appreciated, GAS may be a cause of vulvovaginitis, particularly in a pediatric population.2,27 GAS is not a typical colonizer of vaginal mucosa, and its identification and eradication have been shown to produce symptom resolution. In one recent study, 21% of prepubertal girls with vulvovaginitis were found to have GAS infection.28,29 It is often postulated via correlative data that autoinnoculation from pharyngeal infection or colonization may precipitate GAS vulvovaginitis.
In a similar vein, young children and infants may become infected with GAS perianally, resulting in a painful, erythematous, and well-circumscribed dermatitis surrounding the child’s anus. Perianal GAS should be considered in the differential diagnosis of diaper rash with perianal involvement. The discomfort of this infection may secondarily cause constipation in the child.2
Testing of both vulvovaginitis and perianal infection may be performed via swab of the affected area and either rapid antigen testing or bacterial culture. If GAS is identified, then a treatment regimen similar to that for GAS pharyngitis may be followed for either of these infections. If no causative organism is identified, antibiotic coverage should be broadened to include S. aureus and particularly MRSA, as these bacteria may also cause vulvovaginitis and perianal infections (see Table 1).
Suppurative Sequelae. The suppurative sequelae of GAS infection may arise via direct bacterial extension or by hematogenous spread, with the structures of the head and neck particularly sensitive to the immediate extension of an otherwise-uncomplicated GAS pharyngitis. Acute otitis media and sinusitis are frequently cited as the most common infectious sequelae of GAS pharyngitis, and both maintain their typical clinical manifestations (e.g., ear pain in the former and coryza and postnasal drip in the latter). Diagnosis, if it occurs at all, may be made by a clinical history of contemporaneous pharyngitis and a positive throat swab.30 Treatment is the same as for GAS pharyngitis, though a prolonged course of antibiosis may be required for bacterial sinusitis.
Less common suppurative complications of GAS pharyngitis include peritonsillar cellulitis or abscess and other deep-space neck infections, such as retropharyngeal abscess.31,32 Treatment for these includes prompt antibiosis, advanced imaging of ill-appearing patients (e.g., CT of the neck soft tissue), and drainage of any purulent spaces. Initial antibiotic choice should include coverage of anaerobes and MRSA. GAS pharyngitis may also extend to cause mastoiditis or bacterial cervical lymphadenitis, and treatment for these conditions should include antibiotic coverage for GAS. It is advisable to remember that GAS pharyngitis might extend to any contiguous space, and there are reports of conditions such as mediastinitis, orbital cellulitis, and brain abscess that originated as GAS pharyngitis.33 Indeed, GAS pharyngitis or any other noninvasive GAS infection has the capacity to evolve into myriad forms of invasive GAS disease.
Suppurative Disease: Invasive Infections
Characteristics and Epidemiology. An "invasive" GAS infection is a suppurative GAS infection in which GAS can be isolated from a part of the body that is normally sterile.6 Sites such as the pharynx, sinuses, and epidermis always harbor bacteria, and are therefore sites of superficial GAS infection; in contrast, the lungs, bloodstream, bones, and most other organs are typically sterile, and GAS infections of these tissues are, by definition, invasive (see Figure 1). The annual incidence of pediatric invasive GAS in an industrialized nation has been measured to be 1.9 cases per 100,000 children, accounting for 1.06-2.5 of each 1000 pediatric admissions, and having an overall case fatality rate of 2-4%.34,35 The incidence of invasive GAS among infants is notably higher at 5.3 cases per 100,000 children < 1 year of age.36 Invasive GAS is primarily a community-acquired disease, and more than 80% of children found to have invasive GAS were previously healthy. Importantly, however, the presence of an underlying condition has been linked to an increased risk of death in cases of invasive GAS.35,37 It cannot be overstated that invasive GAS is far less common than superficial GAS, but the gravity and uniqueness of these infections merits attention.7
Prior to the antibiotic era, GAS was a major pathogen of neonatal sepsis. However, the role of GAS in neonatal sepsis has declined, and recent reviews of the literature have found few cases of invasive neonatal GAS disease. Still, given the mortality of the condition, care providers should continue to respect the possibility that neonates of any age may suffer from GAS infection, whether obtained by vertical transmission or by postpartum contact with infected family members.38,39
Historically, the most common sites of invasive GAS infection in the non-neonatal pediatric population have been the skin and its associated soft tissues, with 50-70% of all invasive GAS in children occurring in these organs (e.g., cellulitis, erysipelas, necrotizing fasciitis, peritonsillar abscess, etc.). However, it is notable that a large number of these cases were associated with a primary infection of Varicella zoster (chickenpox), and such cases have become much less frequent since widespread vaccine use, circa 2000. In one study in the United States, the fraction of Varicella-associated pediatric invasive GAS dropped from 27% to 2% after vaccine implementation.34 Given a case rate of 5.2 per 100,000 of invasive GAS in chickenpox, a separate study estimated that at least 10% of all pediatric invasive GAS could be prevented by universal vaccination of 1-year-olds.35 After skin infections, bacteremia without localization accounts for 9-16% of pediatric invasive GAS, making it the second-most-common type of invasive GAS. The remaining balance of invasive GAS disease is composed of GAS pneumonia (more common after influenza infection), arthritis, meningitis, endocarditis, peritonitis, osteomyelitis, and other rare infections.34,40,41
Of all invasive GAS infections, perhaps none is as feared as necrotizing fasciitis, a member of the broader category of necrotizing soft tissue infections. The presence of GAS defines Type II (monomicrobial) necrotizing fasciitis, a rapidly progressive infection of deep tissues, including the muscle fascia and subcutaneous fat, which often leads to the loss of limb or life. Additionally, GAS may also be present in Type I (polymicrobial) necrotizing fasciitis. Mortality among pediatric necrotizing fasciitis patients can be estimated to be 10-20%, with survivors in some studies facing median hospital stays of several weeks and a complication rate of 85%.35,42,43 While immunosuppression and skin trauma can predispose a child to necrotizing fasciitis, it can also develop in an apparently spontaneous way. Because necrotizing fasciitis is initially a process of the deep tissue, its surface manifestations may be subtle and falsely reassuring. The skin of an affected area may be warm, swollen, and erythematous with indistinct margins, and a hallmark finding on exam is pain that is out of proportion to other exam findings. Advanced necrotizing fasciitis may display other classic features, such as bullae or crepitus, but it is preferable to identify the disease prior to the appearance of these. When there is suspicion of necrotizing fasciitis, surgical consultation should be obtained, with surgical exploration being the definitive diagnostic modality for this disease. Laboratory and radiographic studies have insufficient sensitivity to exclude the diagnosis of necrotizing fasciitis, though some studies suggest that CT holds promise in this regard.44,45
Treatment. Pediatric patients with suspected invasive GAS should be admitted to the hospital, and their care will likely require the input of multiple specialists. In specific cases, such as a well-appearing child with lymphadenitis, outpatient management may be considered (see Table 1). However, for most children with suspected invasive GAS, inpatient care will be necessary. Surgical consultation and source control will often be required, as is the case for septic arthritis, necrotizing fasciitis, and retropharyngeal abscess, among other conditions. Another primary consideration is the stability of the patient: children with septic physiology with or without compromise in end-organ function require intensive care and standard supportive measures, such as aggressive fluid resuscitation.
In addition to resuscitative interventions, treatment with antibiotics is of paramount importance. As is the case with all GAS, the strains of GAS responsible for invasive GAS are universally susceptible to beta-lactam antibiotics, such as penicillin. However, it is not often possible to quickly confirm GAS as the causative agent in a sick child, so initial antibiotic therapy should be broad, including coverage for MRSA, gram negatives, and anaerobic bacteria. Therapy may later be narrowed when cultures prove GAS, so long as the patient is improving. All antibiotics should be delivered intravenously, as the gastrointestinal tract provides slower drug uptake, and the gut may be compromised in a seriously ill child. Expert bodies advise that treatment courses of 2 or more weeks may be necessary for many invasive GAS infections.20
Apart from the intravenous use of penicillin, overwhelming infections with GAS have shown a better response to antibiotic therapies, which include protein synthesis inhibition such as that provided by the macrolide antibiotic clindamycin. In both an animal model and a restrospective review of human children with invasive GAS, significantly better outcomes were obtained with clindamycin than with penicillin alone.46,47 This observation has multiple proposed explanations, including macrolide inhibition of GAS toxin protein production and a possible lack of bacterial penicillin binding proteins when GAS infections are overwhelming and have reached the stationary phase of bacterial growth. In any case, the empiric data are compelling, and serious invasive GAS infections should receive dual intravenous antibiotic therapy with penicillin G (200,000-400,000 units/kg per day, divided every 4-6 hours, maximum daily dose of 24 million units) and clindamycin (25-40 mg/kg per day, divided every 6-8 hours, maximum daily dose of 2.7 g). Clindamycin should not be used in isolation, due to occasional GAS resistance to this drug.14
Nonsuppurative Disease: Toxin-mediated Disease
Scarlet Fever. Scarlet fever is a GAS disease defined by the presence of a suppurative GAS infection in combination with a toxin-mediated, pathognomonic exanthem. Importantly, all of the dramatic cutaneous findings of scarlet fever are caused not by local infection but by circulating bacterial toxins: one or more of certain streptococcal toxins, termed streptococcal pyrogenic exotoxin A, B, and C, must be present for scarlet fever to occur, and only a subset of GAS strains produce these toxins.48
In its typical presentation, the rash of scarlet fever begins 1-2 days after the onset of GAS pharyngitis, although it may rarely follow cutaneous or other GAS infections.20 The rash generally starts on the head and neck, expanding centrifugally through the torso and then extremities to produce a confluent, blanching erythematous exanthem, which classically contains innumerable tiny papules that impart a rough, sandpaper-like texture. Pruritis is not universal. Circumoral pallor may be present, and an affected child’s tongue may develop a thick white coat, which is later sloughed to reveal a uniformly bright-red color, in a transition from "white" to "red" strawberry tongue. In flexural and load-bearing parts of the body, the rash may contain linear petechiae, termed "Pastia lines." Approximately 5 days after rash onset, affected skin will begin to desquamate, proceeding over a period which may be as long as several weeks.17 The treatment and potential sequelae of scarlet fever are in every way the same as those of GAS pharyngitis.20
Though the rash of scarlet fever is not harmful, the disease itself has long been a feared clinical entity, and this is almost certainly due to its epidemiologic characteristics in the 1800s. Before this time, scarlet fever was well-described but not particularly virulent. For unclear reasons, in the early 1800s pandemic scarlet fever began to occur regularly. The disease in this era was both more prevalent and more deadly, with case-fatality rates of 15-30% from associated sepsis, and by mid-century it had become the most common infectious killer of children. Then, even before the advent of antibiotics, it suddenly stopped: by the end of the century, mortality for scarlet fever in both Europe and the United States dropped below 1%. The incidence of the disease decreased as well, though not always in lockstep with its virulence, and data from the mid-twentieth century United States show a mortality rate of 0.1 per 100,000 people.49,50 Scarlet fever remains similarly benign and non-prevalent today, though occasional outbreaks do still occur.13,51
Toxic Shock Syndrome. Some GAS infections may become complicated by shock and end-organ dysfunction in a disease termed Streptococcal toxic shock syndrome (STSS), an entity whose effects are mediated by bacterial toxins. STSS should not be confused with Staphylococcal toxic shock syndrome, though the two syndromes have much in common.52 By definition, STSS in children is diagnosed when an invasive GAS infection is attended by hypotension (systolic blood pressure lower than the fifth percentile for age) and two or more of the following criteria: renal impairment (creatinine two times or more the upper limit of normal for age), coagulopathy (platelet count ≤ 100,000/µL or disseminated intravascular coagulation), hepatic involvement (ALT, AST, or total bilirubin levels two times or more the upper limit of normal for age), acute respiratory distress syndrome, a generalized erythematous macular rash that may desquamate, and soft tissue necrosis.6,52 It is estimated that STSS complicates 4-7% of pediatric invasive GAS, and it brings with it a case fatality rate of 4-27%, with most reports favoring the latter end of this range.35,52-54 Adults with STSS do less well, with the mortality rate for STSS in the general population being 36%.36
GAS is capable of producing a variety of toxins that lead to STSS, and chief among these are the toxins that act as superantigens. A superantigen is a toxin that causes the indiscriminate and widespread activation of the host immune system by binding directly to both the T-cell receptor on T cells and the MHC class II molecule on antigen presenting cells. This mechanism bypasses the normal, careful process of antigen display and recognition, leading to the non-specific activation of immune cells and a massive release of inflammatory cytokines (TNFa, interferon-γ, IL-1, etc). The resulting unregulated activation of the immune system is thought to underlie the shock and organ dysfunction that defines STSS.5,52 Streptococcal toxins capable of acting as superantigens include at least the pyrogenic exotoxins A, B, C, F, G, H, J, and the mitogenic exotoxins Z and Z-2.17,52
The management of pediatric STSS is in many ways similar to that of invasive GAS in general, and the initial antibiotic regimen should cover GAS, with both a beta-lactam agent and clindamycin, and also gram-negative bacteria and MRSA.20 Resuscitation efforts for STSS will often need to be more aggressive; however; in one large case series, coma and respiratory failure were each observed in more than two-thirds of patients, and more than half of all fatalities occurred in the first 24 hours of hospital admission.54 Because the pathogenesis of STSS is thought to hinge on humoral exotoxins, intravenous immunoglobulin (IVIG) may be an effective treatment, and in vitro data show that IVIG reduces T-cell activation and cytokine production in the presence of toxin. Although the low incidence of STSS has precluded definitive trials, several human studies have also shown a survival benefit of IVIG. Only one study directly examined the effect of IVIG in pediatric STSS, and though it found no benefit, it was restrospective in design and suffered from selection bias. Expert sources currently recommend the use of IVIG or at least recommend that it may be considered, and a commonly suggested regimen is a single dose of 1-2 g/kg.5,20,52,53
Nonsuppurative Disease: Immune-mediated Disease
Acute Rheumatic Fever. Acute rheumatic fever (ARF) is an autoimmune inflammatory sequela of GAS pharyngitis with characteristic clinical manifestations in the brain, joints, skin, and heart. Most common in patients who are 5-15 years old, ARF has had a sharply decreased presence in industrialized nations since the 1950s, and the World Health Organization estimates its current incidence at 0.5 cases per 100,000 school-age children.9 This decline is not believed to be explicable entirely by antibiotics and is thought instead to be a combination phenomenon, related also to public health conditions and a change in the prevalence of specific "rheumatogenic" GAS strains.17 Notably, the incidence of ARF in developing countries remains high, with local incidences varying from 20-200 cases per 100,000 school-age children.8,9,55 The sequelae of ARF include chronic rheumatic heart disease (estimated to occur in 60% of ARF cases), heart failure, stroke, and infective endocarditis. Accounting for these morbid conditions, ARF has been estimated to underlie at least 400,000 deaths worldwide annually.8
The potential manifestations of ARF are numerous and varied, and the disease is therefore diagnosed by the Jones criteria, a set of five major and four minor criteria, of which two major or one major and two minor criteria must be present to establish the diagnosis (see Table 2).56 The Jones criteria also mandate evidence of an antecedent GAS infection, which typically would have occurred 2-6 weeks prior to ARF onset, though it may have gone unnoticed. Evidence of antecedent GAS infection includes: positive throat culture, rapid antigen test, or streptococcal antibody test, with the latter investigation most likely to provide an accurate result so many weeks after active infection.

Migratory polyarthritis and carditis are the two most common features of ARF and are also two of the major Jones criteria. The migratory arthritis of ARF typically affects one of the large joints for a few days to a week and then "migrates" on, from joint to joint. Long-lasting articular damage is rare. In contrast to this, the carditis of ARF is considerably more dangerous. It may affect all tissues of the heart, and its endocardial involvement often leads to mitral and/or aortic valvulitis with regurgitation. This acute insult often then progresses to chronic rheumatic heart disease, which is typified variously by regurgitation and/or stenosis of the damaged valves, frequently in a permanent way. This cardiac damage is the primary source of the high morbidity and mortality that is attributable to ARF.
The major Jones criteria are completed by chorea, erythema marginatum, and subcutaneous nodules. The chorea of ARF (Sydenham chorea, St. Vitus dance) typically occurs months after GAS infection, rather than weeks, and is characterized by purposeless involuntary movements, incoordination, emotional lability, and other CNS effects. It follows a self-limited course of several months to a full resolution, but it may recur sporadically throughout a patient’s life. Erythema marginatum is the classical rash of ARF, though it occurs in only 2% of cases. It is composed of transient lesions of the trunk and sometimes extremities that are macular, erythematous, and non-pruritic. The lesions, which may be annular to somewhat serpiginous, typically have a crisp outer border, for which they are named. This rash is self-limited and non-injurious. The final major Jones criterion is fulfilled by the presence of subcutaneous nodules, which are firm, nonpainful nodules that typically occur over the bony prominences of extensor surfaces in no more than 1% of ARF patients. They, too, are self-limited and non-injurious. The minor Jones criteria consist of arthralgias, fever, prolonged PR interval on ECG, and elevations in acute-phase reactants, such as CRP or ESR.17,56
It is essential to note that ARF may be nearly completely prevented by the adequate treatment of GAS pharyngitis. Data from studies of epidemic ARF within the 1940s-1950s U.S. military suggest strongly that standard treatment of GAS pharyngitis is adequate to prevent the development of ARF in almost all cases, even when treatment is started up to 9 days after symptom onset.57 Despite this, prevention will never be complete, as some GAS infections go unnoticed or untreated. Given the current low incidence of ARF in industrialized countries, some modern commentators now recommend against the treatment of GAS pharyngitis with antibiotics, arguing that the harmful side effects of antibiotics outweigh their benefits.58 While this line of reasoning may have merit, it is not supported by any of the major authorities, all of which still advocate the full-treatment approach without qualification.14,20
The complete treatment of ARF has several important facets. Importantly, all new diagnoses of ARF must first be treated with a full course of an antibiotic that is appropriate for the treatment of GAS pharyngitis. This should be done even if no clinical or historical evidence of GAS pharyngitis can be found.20 Second, aspirin (50-70 mg/kg/day for 2-4 weeks then tapered for 4-6 weeks) should be used to combat the inflammation of ARF and to reduce its symptoms. Third, all children diagnosed with ARF should undergo a period of antimicrobial prophylaxis to prevent recurrent attacks. Prophylaxis in children should continue for 5 years or until the child is 21 years old, whichever is longer. This period may need to be extended if rheumatic heart disease is present. Appropriate prophylactic regimens include 1.2 million units of intramuscular penicillin G every 4 weeks or 250 mg of oral penicillin V twice daily. Macrolides or sulfadiazine may be used for prophylaxis in patients with penicillin allergies. Rheumatic heart disease, if present, may necessitate the involvement of a cardiologist for management of heart failure.17,20
Post-streptococcal Glomerulonephritis. Acute post-streptococcal glomerulonephritis (PSGN) is an immune-mediated sequela of GAS infection that is defined by acute renal injury, sometimes to the point of complete renal failure. While PSGN may affect people of any age group, it is most prevalent among school-age children, and in many areas it is the most common cause of pediatric nephritis. Population studies estimate the incidence of PSGN to be 0.3 cases per 100,000 person-years in more developed countries and a strikingly higher 24.3 cases per 100,000 person-years in less developed countries, a disparity that is reminiscent of the demographics of other GAS sequelae.10,16,17
Though the exact pathogenesis of PSGN is still under investigation, it is widely believed that specific streptococcal antigens deposit into the glomerulus and cause an in situ immune reaction that leads to parenchymal damage and dysfunction. Importantly, PSGN may follow GAS infections of either the respiratory tract or the skin, as opposed to ARF, which only develops after respiratory tract infections. The latent period between GAS infection and PSGN onset is typically 10-21 days, and in contrast to ARF, even adequate treatment of a GAS infection will not necessarily prevent PSGN. The clinical manifestations of PSGN are quite variable and range from microscopic hematuria alone to edema, hypertension, oliguria, elevated creatinine, and gross hematuria.10,59
The treatment of PSGN is primarily supportive in nature, with severe cases requiring dialysis. Additionally, all diagnoses of PSGN should receive a full course of an antibiotic that is appropriate for the treatment of GAS pharyngitis. As with ARF, this should be done even in the absence of any clinical or historical evidence of GAS infection. While ARF is quite likely to recur in an individual, PSGN is fortunately very unlikely to affect the same individual more than once, and antimicrobial prophylaxis is therefore unnecessary. Most children affected by PSGN will make a spontaneous full recovery, though a small percentage may continue to have mild renal dysfunction.10,17
Other Immune-mediated Disease. Several diseases exist as either minor or unproven sequelae of GAS infection. One notable member of this group is post-streptococcal reactive arthritis (PSRA), which is proposed to be an arthritic condition that develops after GAS infection in patients who do not otherwise fulfill the Jones criteria for ARF. In contrast to ARF, the arthritis of PSRA begins sooner after GAS infection, is non-migratory, and responds less well to aspirin and other NSAIDs. The course of PSRA is self-limited and does not permanently injure affected joints. The treatment of PSRA is debated, though nothing beyond a typical treatment course for GAS pharyngitis is routinely recommended. Occasional reports of PSRA describe carditis or other cardiac involvement, but this is rare. Extreme care should be taken to ensure that a case of PSRA is not simply a misdiagnosed case of ARF.17,60
Erythema nodosum (EN), a painful inflammation of subcutaneous fat, may also be a sequela of GAS infection. Though seldom discussed, preceding GAS infection may underlie nearly half of all EN cases, with the remainder caused by other systemic disease, including tuberculosis infection and Crohn’s disease. A typical presentation of EN will display tender, poorly demarcated nodules over extensor surfaces of the body, most commonly over the pretibial areas, which resolve spontaneously over several weeks without residual damage. Although confirmatory testing for recent GAS infection may help exclude more morbid possible causes of EN, this diagnostic step is not mandatory, nor is any treatment required. If treatment is desired for confirmed infection, an antibiotic course appropriate to GAS pharyngitis may be given, a short course of oral corticosteroids may be considered, and pain may be managed safely with NSAIDs.61
A final, highly controversial set of possible GAS sequelae are termed "pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections" (PANDAS). Proponents of PANDAS as an entity propose that GAS infections may both cause and exacerbate neuropsychiatric disorders, including tics and obsessive-compulsive disorder. In support of this possibility, they cite the well-established neuropsychiatric symptoms seen in the Sydenham chorea of ARF. To date, evidence of an association between GAS infections and neuropsychiatric disorders has been mixed, with most studies failing to show a clear link or causal relationship that is different than that commonly observed between many types of stressors and the worsening of a neuropsychiatric condition. Treatment of possible PANDAS cases should focus on the standard, unrelated therapies for GAS infections and neuropsychiatric disorders.62,63
References
- Choby BA. Diagnosis and treatment of streptococcal pharyngitis. Am Fam Physician 2009;79:383-390.
- Amieva-Wang NE, et al eds. A Practical Guide to Pediatric Emergency Medicine: Caring for Children in the Emergency Department. New York: Cambridge University Press; 2011.
- Stevens DL, Kaplan EL. Streptococcal Infections: Clinical Aspects, Microbiology, and Molecular Pathogenesis. New York: Oxford University Press; 2000.
- Steer AC, et al. Global emm type distribution of group A streptococci: systematic review and implications for vaccine development. Lancet Infect Dis 2009;9:611-616.
- Steer AC, et al. Invasive group A streptococcal disease. Drugs 2012;72:1213-1227.
- The Working Group on Severe Streptococcal Infections. Defining the group A streptococcal toxic shock syndrome: Rationale and consensus definition. JAMA 1993;269:390-391.
- Centers for Disease Control and Prevention. CDC: Group A Streptococcal (GAS) Disease. (2008). Available at: www.cdc.gov/ncidod/dbmd/diseaseinfo/Groupastreptococcal_t.htm. Accessed April 28, 2014.
- Carapetis JR, et al. The global burden of group A streptococcal diseases. Lancet Infect Dis 2005;5:685-694.
- World Health Organization. Immunization, Vaccines and Biologicals. Available at: www.who.int/vaccine_research/diseases/soa_bacterial/en/index3.html. Accessed April 29, 2014.
- Rodriguez-Iturbe B, Musser JM. The current state of poststreptococcal glomerulonephritis. J Am Soc Nephrol 2008;19:1855-1864.
- Martin JM, et al. Group A streptococci among school-aged children: Clinical characteristics and the carrier state. Pediatrics 2004;114:1212-1219.
- Shaikh N, et al. Prevalence of streptococcal pharyngitis and streptococcal carriage in children: A meta-analysis. Pediatrics 2010;126:e557-e564.
- Wong SS, Yuen K-Y. Streptococcus pyogenes and re-emergence of scarlet fever as a public health problem. Emerg Microbes Infect 2012;1:e2.
- Shulman ST, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis 2012;55:e86-e102.
- Woods WA, et al. Detection of group A streptococci in children under 3 years of age with pharyngitis. Pediatr Emerg Care 1999;15:338-340.
- Bingler MA, et al. Acute post-streptococcal glomerulonephritis in a 14-month-old boy: Why is this uncommon? Pediatr Nephrol Berl Ger 2007;22:448-450.
- Shulman ST, Tanz RR. Group A streptococcal pharyngitis and immune-mediated complications: From diagnosis to management. Expert Rev Anti Infect Ther 2010;8:137-150.
- Gereige R, Sautu B. Throat infections. Pediatr Rev 2011;32:459-469.
- McIsaac WJ, et al. Empirical validation of guidelines for the management of pharyngitis in children and adults. JAMA 2004;291:1587-1595.
- American Academy of Pediatrics Committee on Infectious Diseases. Pickering LK, ed. Red Book 2012 Report of the Committee on Infectious Diseases. 29th ed. 2012.
- Van Driel ML, et al. Different antibiotic treatments for group A streptococcal pharyngitis. Cochrane Database Syst Rev 2013;4:CD004406.
- Randolph MF, et al. Effect of antibiotic therapy on the clinical course of streptococcal pharyngitis. J Pediatr 1985;106:870-875.
- Casey JR, Pichichero ME. Metaanalysis of short course antibiotic treatment for group A streptococcal tonsillopharyngitis. Pediatr Infect Dis J 2005;24:909-917.
- Baddour LM. Impetigo. UpToDate Available at: www.uptodate.com/contents/impetigo. Accessed April 29, 2014.
- Bessen DE, et al. Genetic correlates of throat and skin isolates of group A streptococci. J Infect Dis 1996;173:896-900.
- Stevens DL, et al. Practice guidelines for the diagnosis and management of skin and soft-tissue infections. Clin Infect Dis 2005;41:1373-1406.
- Powers GF, Boisvert PL. Age as a factor in streptococcosis. J Pediatr 1944;25:481-504.
- Hansen MT, et al. Streptococcus pyogenes pharyngeal colonization resulting in recurrent, prepubertal vulvovaginitis. J Pediatr Adolesc Gynecol 2007;20:315-317.
- Stricker T, et al. Vulvovaginitis in prepubertal girls. Arch Dis Child 2003;88:324-326.
- Pichichero ME. Complications of streptococcal tonsillopharyngitis. UpToDate Available at: www.uptodate.com/contents/complications-of-streptococcal-tonsillopharyngitis. Accessed April 30, 2014.
- Ehlers Klug T, et al. Fusobacterium necrophorum: Most prevalent pathogen in peritonsillar abscess in Denmark. Clin Infect Dis 2009;49:1467-1472.
- Khan ZZ. Group A Streptococcal Infections Medscape Available at http://emedicine.medscape.com/article/228936-overview. Accessed April 30, 2014.
- Costantinides F, et al. Rapidly progressing subperiosteal orbital abscess: An unexpected complication of a group-A streptococcal pharyngitis in a healthy young patient. Head Face Med 2012;8:28.
- Patel RA, et al. Reduction in pediatric hospitalizations for varicella-related invasive group a streptococcal infections in the varicella vaccine era. J Pediatr 2004;144:68-74.
- Laupland KB, et al. Invasive group A streptococcal disease in children and association with varicella-zoster virus infection. Pediatrics 2000;105:e60.
- O’Loughlin RE, et al. The epidemiology of invasive group A streptococcal infection and potential vaccine implications: United States, 2000-2004. Clin Infect Dis 2007;45:853-862.
- Megged O, et al. Group A streptococcus bacteraemia: Comparison of adults and children in a single medical centre. Clin Microbiol Infect 2006;12:156-162.
- Lardhi AA. Neonatal group A streptococcal meningitis: A case report and review of the literature. Cases J 2008;1:108.
- Miyairi I, et al. Neonatal invasive group A streptococcal disease: Case report and review of the literature. Pediatr Infect Dis J 2004;23:161-165.
- Bettinger JA, et al. Pandemic influenza in Canadian children: A summary of hospitalized pediatric cases. Vaccine 2010;28:3180-3184.
- Ampofo K, et al. Association of 2009 pandemic influenza A (H1N1) infection and increased hospitalization with parapneumonic empyema in children in Utah. J Oct 2010;29:905-909.
- Bingöl-Kologlu M, et al. Necrotizing fasciitis in children: Diagnostic and therapeutic aspects. J Pediatr Surg 2007;42:1892-1897.
- Fustes-Morales A, et al. Necrotizing fasciitis: Report of 39 pediatric cases. Arch Dermatol 2002;138:893-899.
- Wilson MP, Schneir AB. A case of necrotizing fasciitis with a LRINEC score of zero: Clinical suspicion should trump scoring systems. J Emerg Med 2013;44:928-931.
- Zacharias N, et al. Diagnosis of necrotizing soft tissue infections by computed tomography. Arch Surg 2010;145:452-455.
- Stevens DL, et al. The Eagle effect revisited: Efficacy of clindamycin, erythromycin, and penicillin in the treatment of streptococcal myositis. J Infect Dis 1988;158:23-28.
- Zimbelman J, et al. Improved outcome of clindamycin compared with beta-lactam antibiotic treatment for invasive Streptococcus pyogenes infection. Pediatr Infect Dis J 1999;18:1096-1100.
- Cunningham MW. Pathogenesis of group A streptococcal infections. Clin Microbiol Rev 2000;13:470-511.
- Katz AR, Morens DM. Severe streptococcal infections in historical perspective. Clin Infect Dis 1992;14:298-307.
- Krause RM. Evolving microbes and re-emerging streptococcal disease. Clin Lab Med 2002;22:835-848.
- Lamden KH. An outbreak of scarlet fever in a primary school. Arch Dis Child 2011;96:394-397.
- Chuang YY, et al. Toxic shock syndrome in children: Epidemiology, pathogenesis, and management. Paediatr Drugs 2005;7:11-25.
- Shah SS, et al. Intravenous immunoglobulin in children with streptococcal toxic shock syndrome. Clin Infect Dis 2009;49:1369-1376.
- Rodríguez-Nuñez A, et al. Clinical characteristics of children with group A streptococcal toxic shock syndrome admitted to pediatric intensive care units. Eur J Pediatr 2011;170:639-644.
- Tibazarwa KB, et al. Incidence of acute rheumatic fever in the world: A systematic review of population-based studies. Heart 2008;94:1534-1540.
- Guidelines for the diagnosis of rheumatic fever. Jones Criteria, 1992 update. Special Writing Group of the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease of the Council on Cardiovascular Disease in the Young of the American Heart Association. JAMA 1992;268:2069-2073.
- Wannamaker LW. et al. Prophylaxis of acute rheumatic fever by treatment of the preceding streptococcal infection with various amounts of depot penicillin. Am J Med 1951;10:673-695.
- Newman DH. Hippocrates’ Shadow: Secrets from the House of Medicine. New York: Scribner; 2008.
- Rodríguez-Iturbe B, Batsford S. Pathogenesis of poststreptococcal glomerulonephritis a century after Clemens von Pirquet. Kidney Int 2007;71:1094-1104.
- Mackie SL, Keat A. Poststreptococcal reactive arthritis: What is it and how do we know? Rheumatol Oxf 2004;43:949-954.
- Schwartz RA, Nervi SJ. Erythema nodosum: A sign of systemic disease. Am Fam Physician 2007;75:695-700.
- Kurlan R, et al. Streptococcal infection and exacerbations of childhood tics and obsessive-compulsive symptoms: A prospective blinded cohort study. Pediatrics 2008;121:1188-1197.
- Leckman JF, et al. Streptococcal upper respiratory tract infections and exacerbations of tic and obsessive-compulsive symptoms: A prospective longitudinal study. J Am Acad Child Adolesc Psychiatry 2011;50:108-118..
- Liu C, et al. Clinical practice guidelines by the Infectious Diseases Society of America for the treatment of methicillin-resistant Staphylococcus aureus infections in adults and children. Clin Infect Dis 2011;52:e18-55.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
