Complications of Prosthetic Heart Valves in the Emergency Department
Complications of Prosthetic Heart Valves in the Emergency Department
Introduction
More than 100,000 prosthetic heart valves are implanted each year in North America, and another 300,000 are done annually worldwide.1 While these are life-saving procedures, they can also have catastrophic complications in the immediate post-operative period as well as in the following years.
Valve problems can be difficult to identify because the symptoms may be similar to those associated with common comorbidities such as cardiomyopathy, dysrhythmias, chronic obstructive pulmonary disease (COPD), and renal insufficiency. Severe valve complications are seen infrequently by most emergency physicians, so making the diagnosis can be very challenging.
Review of Prosthetic Valves
It is helpful to review the various types of valves and to understand the normal and abnormal clinical presentations of each kind of prosthesis. Broadly, implanted valves can be divided into mechanical or bioprosthetic. Mechanical valves are those that contain only nonbiologic materials, primarily pyrolytic carbon, fabric, and metal. Bioprosthetic valves contain some portion of biologic tissue combined with a fabric and metal support structure. They may be strutted or non-strutted. The struts point in the direction of blood flow and often are visible on chest radiographs. The choice of prosthesis is a complicated one based on many factors including pathology, patient lifestyle, age, gender, size, anatomy, surgeon preference, and risk of anticoagulation. It is important to remember that many patients who undergo valve replacement have had long-standing valvular disease. This process may compromise ventricular function, chamber dimensions, and pulmonary vascular resistance. Valve replacement may not prevent or fully reverse such damage.
The Starr-Edwards caged-ball valve, produced in 1960, was the first prosthetic valve and is a low-cost valve that continues to be used only in developing countries. Caged-ball valves create a wake of stagnant blood flow, which is thought to contribute to their higher risk of thromboembolism.2 Subsequently, single-leaflet, tilting disk, and bileaflet valves were developed. The St. Jude Medical valve, introduced in 1977, was the first bileaflet valve. This and other bileaflet valves are now the most commonly used mechanical valve replacements.3,4 (See Figure 1.)
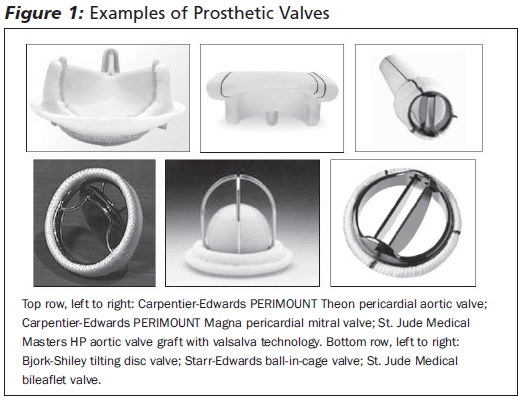 |
Mechanical valves are more durable and, consequently, are often favored in younger patients. Mechanical valves usually last 20-30 years.3,5-7 Mechanical valves, however, have a higher rate of thrombotic and thromboembolic complications compared to bioprosthetic valves, and require anticoagulation in most patients.3,8
Bioprosthetic valves are categorized by tissue origin. They are either of human origin, also called homografts, or of pig or bovine origin, also called heterografts. An explanted intact pig valve may be used with metal commissural support, or bovine pericardial tissue may be used to cover a metal support structure. Due to their lower thrombogenicity, bioprosthetic valves do not require anticoagulation; however, some clinicians may choose to maintain these patients on lifelong aspirin therapy.8 Patients with valvular pathology, especially of the mitral valve, are at a higher risk for atrial fibrillation and may be maintained on anticoagulation therapy for that reason alone, regardless of the type of prosthetic valve implanted. As bioprosthetic valves are becoming more durable, they are more frequently being utilized in younger patients.5,8-10
Composite valves, consisting of a mechanical valve built into a tissue graft, may be used to repair the aortic root and valve. These are not common, but may be placed in patients with Marfan's syndrome or others who develop an aneurysm or dissection of the ascending aorta.
Emergency physicians should realize that many patients have valve repair instead of valve replacement. Patients may not be aware of the difference, so a careful history and physical examination is essential. Valve repairs, almost always in the mitral or tricuspid position, are becoming more common because they are durable and the patient does not have to be anticoagulated after the first few months of valve healing. Often a ring or partial ring structure will be placed for repair support and may be visible on chest radiograph. In this procedure, the valve leaflets are the patient's native tissue. The distinction between valve repair and replacement is important because patients who have had valve repair are not subject to many of the complications discussed in this review.
When patients with prosthetic valves present to the emergency department, they are more likely to have their symptoms unrelated to the function of their valve. Factors that suggest the possibility that the patient's symptoms are related to valve dysfunction include surgery within the past four weeks; recent invasive procedure or infection; development of new, loud murmurs; muffling or absence of the normal click of a mechanical valve; rapid severe decompensation; cardiogenic shock; or severe acute congestive heart failure. Nonetheless, valvular dysfunction is an extremely challenging presentation that can confound the abilities of even the seasoned clinician.
Identification of Prosthetic Valves
Review of medical records is invaluable when evaluating a patient with a prosthetic valve. Check the patient's belongings for a wallet card. Most patients will be issued a card with the type of valve, specific model, serial number, surgeon, and institution where their surgery was performed. Many cards will also include a medical record number. Discharge summaries often describe the operation and post-operative course as well as a pre-discharge echocardiogram report.
Chest radiography can provide information about the location and type of prosthetic valve, as well as secondary signs of cardiac pathology such as enlarged heart size, pulmonary edema, and pleural effusion. Non-cardiac causes of similar symptoms such as pneumonia and pneumothorax also may be visualized.
Patients who undergo valve repair instead of replacement often will have a radiopaque ring structure used for support. This is not a prosthetic valve and should not be confused with one if seen on a chest radiograph. (See Figure 2.)
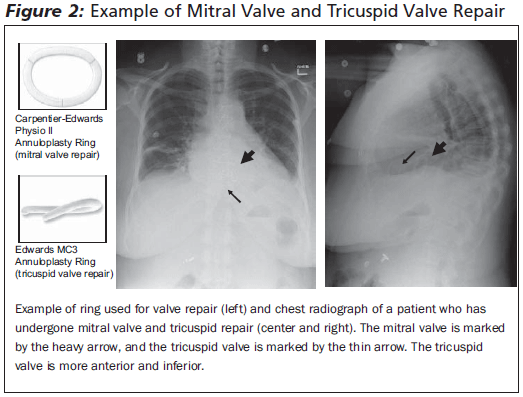 |
Prosthetic valves are more easily seen on radiographs in the lateral projection and may be easily missed on a limited AP radiograph. Tricuspid valves are directly over the spine in an AP projection, which often makes them difficult to visualize. The pulmonic valve is the most superior valve, lying just above the AV groove. The aortic and mitral valves are adjacent to one another in the center of the heart, with the mitral valve being more inferior and lateral. An AP view alone may be insufficient to distinguish between an aortic or mitral prosthetic valve. In a lateral chest radiograph, the aortic valve is more anterior and superior and oriented slightly more horizontally. In addition, the valve struts (if present) are oriented in the direction of blood flow. Struts of an aortic valve will be directed superiorly and toward the patient's right, whereas mitral valves will be oriented inferiorly and toward the patient's left. (See Figure 3.) In addition to location, the type of valve may be identified. The presence of a cage structure indicates a ball-in-cage type valve, but a base ring or struts may also be a clue. Carbon mechanical valves often are radiolucent and difficult to see on plain radiographs. Aortic homographs or bioprosthetic valves without struts may be completely radiolucent.7
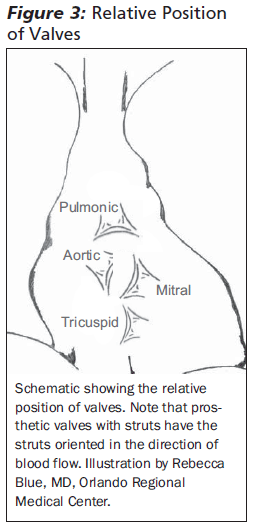 |
Physicians who are familiar with various prosthetic valves may be able to identify their location and, occasionally, the type of valve by auscultation. Extensive descriptions of the types of murmurs expected in normal valve function as well as various pathologic processes can be found in cardiology literature. Such murmur distinctions are beyond the scope of expertise of most emergency physicians. However, emergency physicians may utilize the sharp closing click of a mechanical valve to help identify the location of a prosthetic valve by remembering that prosthetic aortic valves should produce a closing click at the end of systole (S2), and mitral valves should produce a late diastolic click (closing as S1 begins). Tissue valve closing sounds mimic native valves.
Evaluation of the Patient
History. Patients with valve complications most commonly present to the emergency department with nonspecific complaints of chest pain, shortness of breath, palpitations, or increasing fatigue. Febrile patients should be questioned carefully about any recent invasive procedures, especially dental, within the past month.
Physical Examination. The patient should be closely examined for signs and symptoms of heart failure. This includes careful auscultation of the heart and lungs. When auscultating the heart of a patient with a mechanical prosthetic valve, physicians should listen for clicks. The absence of any click, or a click that sounds muffled, in a patient with a mechanical valve signals a major valve dysfunction, such as valve thrombosis or obstruction. A muffled click, however, is at times difficult to discern.
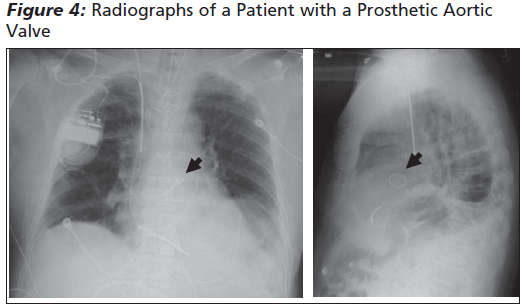 |
The presence of a new or changed murmur in a patient with any prosthetic valve also may signal dysfunction. However, most emergency physicians will not have knowledge of the baseline murmur of a particular valve type. Functioning prosthetic aortic valves may produce an early diastolic murmur, whereas functioning mitral valves may produce a late diastolic murmur. Simple general rules that may help identify pathologic murmurs are: a prosthetic mitral valve should not produce a holosystolic murmur; and a prosthetic aortic valve should not produce a sustained diastolic murmur. If either of these murmurs is heard, it should alert the emergency physician that valve dysfunction is likely.11
Ancillary Diagnostic Studies. Laboratory studies, chest radiography, electrocardiogram and an echocardiogram should be obtained. Laboratory studies include a complete blood count, electrolytes, creatinine, and coagulation profile. If the patient is febrile, blood cultures also should be obtained. Other studies that should be considered include cardiac biomarkers, brain natriuretic peptide, liver function tests, and, if hemolytic anemia is suspected, a peripheral blood smear. The electrocardiogram is not usually diagnostic for valve dysfunction.6,7 New conduction abnormalities including new bundle branch block and new heart block are possible and have been reported in association with the spread of valvular endocarditis and formation of a septal abscess.12
Radiography and Echocardiography. Chest radiography is useful, not only to identify the location and type of valve, but also to look for secondary signs of valve dysfunction. Severe structural failure in which the valve or a portion of it becomes dislodged is extremely rare.11 Chest radiography usually can identify such dislodged pieces, but abdominal and pelvic radiography also may be required. Additionally, the chest radiograph should be analyzed for cardiomegaly, vascular congestion, and pulmonary edema. Other causes for the patient's symptoms also should be considered, including pneumonia, pleural effusion, and pneumothorax.
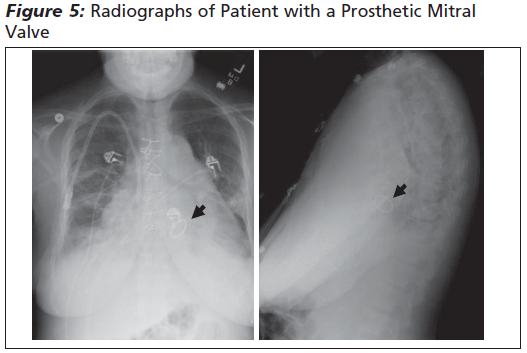 |
Echocardiography is the key ancillary test to evaluate prosthetic valve function. Echocardiography can detect pericardial effusion with tamponade, valve dysfunction, ventricular dysfunction, intracardiac vegetations or thrombus, and aortic pathology. Echocardiography also can determine the position and type of valve prosthesis in most cases. In patients with a high clinical index of suspicion for endocarditis, aortic dissection, or more subtle valvular pathology, transesophageal echocardiogram (TEE) is indicated due to its higher resolution. The rapid performance of a TEE, however, is difficult in most institutions, if it is available at all.
Emergent Treatment
The emergent treatment of patients with prosthetic heart valves should be directed toward stabilizing the patient and identifying the cause of the acute decline. Antibiotics should be administered as quickly as possible following collection of blood cultures from febrile patients13-16 with the consideration of endocarditis.
Patients with evidence of acute thromboembolic events need assessment of their coagulation status. Patients with acute cerebral vascular accidents should be treated as other stroke patients, but careful attention should be paid to ensure that thrombotic and hemorrhagic strokes are correctly identified and that embolic strokes have not undergone hemorrhagic transformation. While it may be necessary to stop or hold anticoagulation for a patient with a mechanical valve who has an intracranial hemorrhage, that decision should be made carefully and with the understanding that such patients are at high risk for thromboembolic events.
Those with acute congestive heart failure should be provided supplemental oxygen, nitrates, morphine, diuretics, and respiratory support as needed. Acute mitral or aortic regurgitation likely will require surgical intervention, but afterload reduction with nitroprusside or nicardipine infusion may help stabilize the patient. Beta blockade also may be a reasonable choice if the patient is known to have good left ventricular function and is tachycardic. Patients with acute deterioration due to severe aortic stenosis may require small amounts of fluid resuscitation and inotropic therapy. It is important to remember that fluid balance is delicate in these patients. Patients with critical aortic stenosis can progress to total cardiovascular collapse if given nitroglycerin or any other agent that reduces preload or coronary artery perfusion by lowering systemic blood pressure.
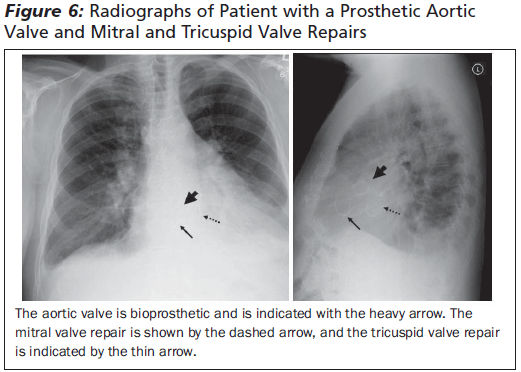 |
If chest radiography and clinical evaluation of the patient suggests acute structural failure of a prosthetic valve, patients should be managed as those with severe, acute regurgitation. Finally, if acute valve thrombosis is suspected, thrombolytics may be considered in consultation with cardiothoracic surgery.17-24 The use of thrombolytics for prosthetic valve thrombosis remains controversial, and many surgeons prefer to take the patient emergently for valve replacement, especially since patients who develop a thrombus are at higher risk for recurrence. Therefore, definitive treatment will most commonly be valve replacement with a less thrombogenic valve. Unless the patient will be undergoing urgent operative treatment, anticoagulation in the emergency department is reasonable. Unfractionated heparin has the advantage of being reversible, but many institutions utilize low-molecular-weight heparins as well. Warfarin will not reach therapeutic levels for several days and, consequently, is not useful in the emergency setting.13
Severe Complications of Prosthetic Valves
Early Complications. Early complications are those occurring within four weeks of valve replacement. The most dangerous situation in the early post-operative period is cardiac tamponade. Patients may have bleeding or inflammation leading to a pericardial effusion. If the effusion develops over several days or weeks, the patient may also have hepatic congestion leading to improper metabolism of warfarin and subsequent warfarin toxicity. Obviously, this situation is an immediate, life-threatening emergency. The best solution is to have a cardiothoracic surgeon take the patient emergently to the operating room. In those uncommon instances when the patient is in extremis, intervention in the emergency department may be indicated. While emergency physicians are most commonly trained to perform needle pericardiocentesis, patients with recent valve replacement are likely to have blood and clots in the pericardial space that are too large to aspirate with a needle.
If needle pericardiocentesis is unable to remove enough blood to temporarily stabilize a patient in profound shock, the following aggressive approach may be lifesaving while awaiting the arrival of the cardiothoracic surgeon or if one is not available. Open the lower two centimeters of the midline incision by cutting the fascial sutures. Then, gently insert a gloved finger through the thin layers of fascia and into the pericardium, taking care to stay on the diaphragm along the back of the sternum. At this point, it should be possible to remove enough fluid to relieve the tamponade. If not, it may also be necessary to gently sweep a finger around the heart in the pericardial space to release loculations of fluid that may be preventing the heart from filling. A Yankauer suction tip may also be placed into the space after a plane is developed. The patient will likely need simultaneous vasopressor support with catecholamines, aggressive volume resuscitation, correction of acid-base derangements, and airway management. The wound should be packed with povidone-iodine soaked gauze and an occlusive dressing before the patient is transferred or taken to the operating room for definitive management.
Concomitant reversal of any anticoagulation is indicated, but should not delay the transfer of the patient to the operating room, since a pericardial window can be placed with very little blood loss. While it is reasonable to provide these patients with immediately available fresh frozen plasma, platelets, and packed red blood cells, the physician should not administer vitamin K. It has no immediate effect and will make it difficult or impossible to maintain appropriate anticoagulation in the post-operative period.
Another early complication of prosthetic valve placement is new or recurrent atrial fibrillation. Careful attention to anticoagulation and rate control is required, since many patients who undergo valve replacement have limited cardiac reserves.
Another complication of prosthetic valves that may cause fever in the early post-operative period is postpericardiotomy syndrome, a condition similar to Dressler's syndrome. The condition is related to the activation and release of cytokines that produces a generalized inflammatory state. It may cause low-grade fever, night sweats, or difficulties with thermoregulation (patients rapidly get hot, then cold), flu-like symptoms, and fluid retention. Patients are prone to atrial arrhythmias and have elevated markers of inflammation such as C-reactive protein and erythrocyte sedimentation rate. Because patients with this condition retain fluid and have chest radiograph appearances similar to congestive heart failure, they often are misdiagnosed as such. Patients with this syndrome should be treated with diuretics, nonsteroidal anti-inflammatory drugs (NSAIDs) if they are not on warfarin, and reassurance that they will improve. Patients should be monitored for atrial arrhythmias. While the syndrome can have a relapsing course, it usually spontaneously resolves with a favorable prognosis.25 In severe cases or in patients who are unable to take NSAIDs, a short course of tapering steroids may be beneficial.
A common complaint of patients presenting to the emergency department after cardiac surgery is chest pain. While evaluation for myocardial infarction is appropriate in those with accompanying coronary artery disease, one should remember that cardiac biomarkers may remain elevated for several days after major cardiac surgery. The most common cause of chest pain is noncompliance with the analgesic prescribed.
Late Complications. While patients are at highest risk for problems during the first month following surgery, complications may develop at any time. The most common late problems are related to anticoagulation. Patients will either have a spontaneous or traumatic hemorrhage, or they are not sufficiently anticoagulated and have a thromboembolic event. While thrombus on the valve is of concern and potentially deadly, a thromboembolic event at a distant location such as the brain, kidneys, or lower extremities may be the first sign of an intracardiac thrombus.
Other complications of patients with prosthetic valves include late-onset atrial fibrillation and endocardial infection. Patients with prosthetic valves, especially those in the mitral position, are at higher risk for atrial fibrillation for the rest of their lives. Even patients with a bioprosthetic valve may require anticoagulation if they develop atrial fibrillation. While the highest risk for infectious endocarditis is in the early post-operative period, there is a continual long term risk that the valve will be hematogenously seeded.
Infectious Endocarditis
One of the deadliest complications of prosthetic valves is infectious endocarditis. In addition to the presence of a foreign body, patients with prosthetic valves have frequent hematogenous exposures through multiple arterial or venous puncture sites. Multiple blood cultures should be considered during febrile illnesses prior to the administration of antibiotics (ideally, the first and last samples should be drawn from different sites at least one hour apart).26-28
Endocarditis in patients with prosthetic valves accounts for 15% of all endocarditis cases and can be divided into early and late endocarditis.13 Early prosthetic valve endocarditis occurs within six months of implantation and is most commonly caused by Staphylococcus epidermidis, gram-negative bacteria, or fungi. Late prosthetic valve endocarditis is any infection occurring six months or more after implantation. The bacteria involved are the same as those seen in native valve endocarditis, including Staphylococcus aureus, Streptococcus viridans, Enterococcus, Streptococcus bovis, Haemophilus parainfluenza, Haemophilus aphrophilus, Actinobacillus actinomycetemcomitans, Cardibacterium hominis, Eikenella corrodens, and Kingella kingae (HACEK organisms).28 Even with aggressive therapy, the mortality rate of infectious endocarditis may be as high as 80% for early endocarditis and as high as 50% for late endocarditis.29
Patients with endocarditis most commonly present with fever and malaise. They also may have complaints of dyspnea, chest pain, neurologic symptoms or other signs of systemic emboli. Because patients with prosthetic valves and endocarditis are at risk for mycotic cerebral aneurysms, brain imaging is recommended. Laboratory abnormalities in patients with endocarditis, such as an elevated white blood cell count, C-reactive protein, or erythrocyte sedimentation rate, are nonspecific and common to other infectious processes. These patients often have microscopic hematuria from emboli to the kidneys and may be mildly anemic.
The diagnosis of prosthetic valve endocarditis may be difficult. Two positive blood cultures from different sites are definitive, but endocarditis may exist with negative blood cultures. The presence of vegetations on the valve(s) also confirms the diagnosis, but visualization of them may require TEE. It is rare to visualize vegetations on the disks of prosthetic valves, but paravalvular abscesses may be identified as echo-dense or echo-lucent areas adjacent to the valve sewing ring.
If prosthetic valve endocarditis is suspected, broad-spectrum antibiotics should be started as quickly as possible after cultures are obtained. A cardiothoracic surgeon should be consulted as soon as possible. Prompt surgical therapy is recommended because delay is associated with further tissue destruction, systemic embolic events, and hemodynamic decompensation.13
Antimicrobial Therapy for Endocarditis
The presence of a prosthetic valve creates areas of stagnant blood flow that may lead to thrombus and/or vegetation formation. These structures sequester bacteria from the bloodstream, so long durations of antibiotic therapy are necessary. Parenteral therapy is preferred because sustained, high, predictable bloodstream levels of antibiotics are required. Because of the duration of therapy, levels of vancomycin and aminoglycosides should be monitored.14
Staphylococcus aureus is now the most common organism causing endocarditis, but empiric therapy in the emergency department if the diagnosis is suspected and therapy initiated should be broad spectrum, including coverage for gram-positive bacteria and gram-negative bacteria. Commonly, a beta-lactam or vancomycin is used in combination with an aminoglycoside. Theoretically, cell wall active agents such as beta-lactams and vancomycin provide increased entry of aminoglycosides into bacterial cells, thereby increasing their efficacy.14,15 For suspected prosthetic valve endocarditis, an example antibiotic regimen would be vancomycin, loading dose 15 mg/kg followed by 500 mg every six hours, plus gentamicin 1-3 mg/kg loading dose followed by 1 mg/kg every 8 hours. Alternatively ceftriaxone 1-2 g every 12 hours could be used instead of vancomycin.27,28,30 Expert consultation regarding antibiotic selection should be sought.
Thromboembolic Complications
Neurologic events in patients with prosthetic valves should be considered to be valve-related until proven otherwise. Thromboembolic events are estimated to occur at a rate of 0.6% to 2.3% per patient year.5,13 The rate of events for patients with mechanical valves on anticoagulation therapy is similar to that of patients with bioprosthetic valves. The rate of thromboembolic events varies as well with other risk factors such as atrial fibrillation or left ventricular dysfunction. Systemic emboli may arise from either obstructing or nonobstructing thrombosis, but patients with nonobstructing thrombus more commonly present with systemic symptoms. In addition, most patients with a thromboembolic event are found to be inadequately anticoagulated.
Treatment of ischemic strokes should begin with determination of the adequacy of anticoagulation. If it is suboptimal, therapy should be reinstituted or adjusted to maintain therapeutic effect. If anticoagulation has been adequate, aspirin should be started as well as raising the target INR. Given the need to maintain anticoagulation, it is important to monitor patients carefully for hemorrhagic transformation of an ischemic stroke. In cases of thromboembolic stroke, thrombus may not be visualized on the valve because of the limitations of echocardiography, small size of the thrombus, or the fact that the thrombus is no longer there.31,32 The intestines, kidneys, and other solid organs are other possible sites of thromboembolism.
Valve Obstruction
Prosthetic valves may become obstructed due to thrombosis, pannus formation, or a combination of both. Valve thrombosis may be obstructive or non-obstructive. Thrombosis may occur slowly as a chronic progressive worsening of function or may occur more acutely. Inadequate anticoagulation is almost always associated with left-sided heart valve thrombosis.3,6,7
Patients with obstructive valve thrombosis typically present with acute pulmonary edema, dyspnea, cardiogenic shock, or systemic thromboembolism. New murmurs or muffled heart sounds may be heard. A patient with a mechanical prosthetic valve and severe acute congestive heart failure who does not have a distinct click on physical examination should prompt the consideration of valvular obstruction. While prosthetic valve thrombosis can be identified with transthoracic echocardiography and fluoroscopy about 85% of the time, TEE remains the most sensitive test32 and is essential for valves in the mitral position, yet may be difficult to obtain in urgent and emergent fashion.
Treatment of valve thrombosis is controversial. Some surgeons recommend thrombolytics as first-line agents.17,20-22 Success rates range from 71-88%, with rates of significant bleeding or embolism 15-25%. Mortality rates from thrombolytic therapy are estimated to be 3-12%, but that remains lower than the 12-46% mortality rate for valve thrombosis surgery. Proponents of early surgical intervention argue that the 25% chance of a cerebral vascular accident, many of which are large, hemiplegic strokes, is much too high of a risk to warrant the use of thrombolytics in patients with left-sided valve thrombosis. They also argue that patients who develop thrombus on a prosthetic valve once are at a higher risk for recurrence and opt to debride the thrombosed valve or replace it with a less thrombogenic one.18,23,24 The benefit-to-risk ratio, however, may be more in favor of thrombolytic therapy for patients with right-sided valve thrombosis as compared to left-sided valve thrombosis, since embolization to the lungs is less likely to have devastating long-term consequences than embolization to the brain.
Valve obstruction due to tissue overgrowth (pannus formation) with or without thrombus at the annulus is another cause of stenosis or regurgitation. The pannus may block the normal opening and closing of the valve.
Prosthetic valve stenosis from pannus formation or thrombus presents with signs and symptoms similar to native valve stenosis. Prominent symptoms may include dyspnea and angina. Patients with prosthetic mitral valve stenosis may present with acute pulmonary edema or, if the condition develops chronically, hemoptysis and pulmonary hypertension. Electrocardiography may show evidence of left atrial enlargement or atrial fibrillation.
Patients with prosthetic aortic valve stenosis may have exertional syncope. New or worsening murmurs, reports of syncope or near syncope, and worsening dyspnea should raise suspicion for this type of valvular stenosis. The diagnosis can be confirmed with echocardiography examining the extent of disk motion. Patients with acute severe aortic stenosis may require gentle fluid resuscitation and inotropic therapy. It is important to remember that these patients should not be overloaded with fluid and that preload reduction with agents such as nitroglycerin may lead to cardiovascular collapse.
Structural Failure
Primary structural failure of modern prosthetic heart valves is extremely rare. Most structural failure is related to complications that occur at the interface of the valve and the native tissues.3,6,7 As in other complications, it may be an acute or slowly progressive disease process. Paravalvular regurgitation may be due to dehiscence, infection, or fibrosis and calcification of the native annulus, leading to inadequate contact between it and the sewing ring.33
Prosthetic valve regurgitation also presents similarly to native valve regurgitation. Regurgitation may be paravalvular or as a result of leaflet or disk deterioration. Bioprosthetic valves located near calcified nodules resulting from endocarditis are particularly vulnerable to regurgitation. Severity of chronic regurgitation may be quantified by echocardiography, and patients should be monitored at least annually for worsening.
Acute mitral valve regurgitation causes fulminant pulmonary edema and hemodynamic collapse. Chronic mitral valve regurgitation may produce fatigue and dyspnea on exertion, orthopnea, paroxysmal nocturnal dyspnea, and peripheral edema. Stabilization of the patient in the acute setting focuses on treatment of the pulmonary edema with nitrates, morphine, and diuretics. In a severely hypotensive patient, placement of an intra-aortic balloon pump may be considered in addition to catecholamime and ventilatory support.
Aortic valve regurgitation also may cause dyspnea, tachypnea, and chest pain. Acute aortic regurgitation is a surgical emergency. Afterload reducers such as nitroprusside may help stabilize the patient until surgical intervention and valve replacement are possible.27
Rare Complications
Patient–Prosthesis Mismatch. In spite of careful evaluation and planning by a cardiothoracic surgeon, rarely the functional area of a prosthetic valve may be too small for the cardiac demands of a particular patient. This phenomenon is termed patient-prosthesis mismatch. Severe aortic valve patient-prosthesis mismatch is associated with a mortality rate of up to 10 times higher than those with an adequate functional valve area.34-36 This difficulty can become apparent in the early and late post-operative period principally as heart failure.
Hemolytic Anemia. While the vast majority of patients with prosthetic valves will have some evidence of hemolysis, clinically significant anemia is rare without paraprosthetic regurgitation. Most patients may be treated simply with iron and folate supplementation, but severe, refractory anemia may require repeat valve surgery or surgical repair of a paravalvular leak.
Pseudoaneurysm. Left ventricular pseudoaneurysm is a rare complication of mitral valve replacement that occurs in up to 0.5% to 2.0% of cases.37 Unlike a true aneurysm, these pouches contain no myocardial cells. These pseudoaneurysms are typically associated with infection. Most frequently, the pseudoaneurysm will develop at the posterior annular suture line and can be diagnosed with echocardiogram. Left ventricular pseudoaneurysm requires surgical repair because it may rupture. Additionally, a pseudoaneurysm may form in the mitral aortic intervalvular fibrosa, creating a pouch between the posterior root of the aorta and the left ventricle.34
Chronic Management Issues
Recommendations for Anticoagulation in Patients with Valvular Replacement. The American College of Cardiology, American College of Chest Physicians, and American Heart Association have created guidelines for anticoagulation of patients with prosthetic valves.10 Patients with mechanical valves in the mitral position should be on warfarin with a goal INR of 2.5-3.5. Patients with mechanical valves in the aortic position should be anticoagulated to the same degree as those with mitral valves if the valve is a caged-ball or tilting disk valve. Bileaflet valves in the aortic position require warfarin, but with a lower goal INR of 2.0-3.0. Patients who fail anticoagulation or have other risk factors also may be maintained on daily aspirin. Aspirin therapy is recommended for all patients with mechanical valves by the American College of Cardiology and American Heart Association, but the possible risk of increased bleeding led the American College of Chest Physicians to recommend that the dual therapy be utilized only for patients with additional risk factors or those who fail warfarin therapy alone.10 (See Figure 7.)
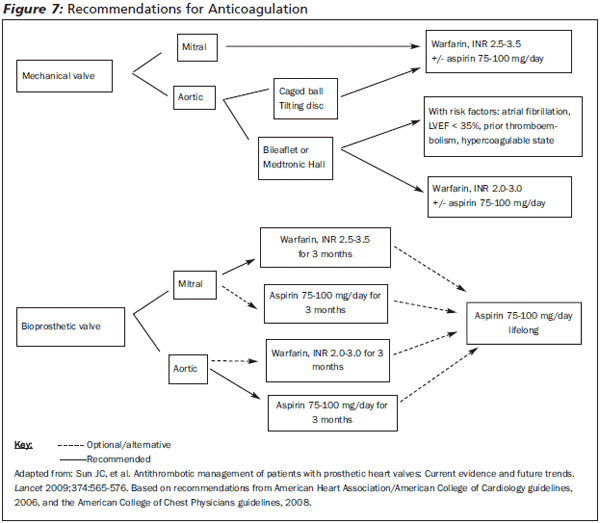 |
Patients with bioprosthetic valves in the aortic position are recommended to have aspirin daily for three months, and possibly be maintained on aspirin therapy for life. It is recommended that patients with bioprosthetic valves in the mitral position, and sometimes in the aortic position, should be anticoagulated with warfarin for three months with a goal INR of 2.5-3.5. These patients may or may not be maintained on lifelong aspirin therapy.10 In addition, many patients will have co-existing coronary artery disease or atrial fibrillation and will be maintained on clopidogrel or warfarin respectively, independent of their prosthetic valve.
Antibiotic Prophylaxis. In 2007, the American Heart Association and American College of Cardiology issued updated guidelines regarding the use of prophylactic antibiotics for invasive procedures in patients with prosthetic heart valves. These guidelines changed the previous recommendations for prophylactic antibiotics for all invasive dental, respiratory, abdominal, and genitourinary procedures. Their current recommendations are to provide prophylaxis for patients with prosthetic heart valves undergoing: high-risk procedures including dental procedures that involve perforation of the oral mucosa or manipulation of the gingival tissue or periapical region of teeth; and invasive procedures of the respiratory tract that involve biopsy or incision. These changes in the guidelines were prompted by a lack of evidence demonstrating the effectiveness of more liberal prophylaxis. In addition, there were concerns about adverse reactions related to antibiotic usage such as allergic reactions, development of antibiotic resistance, and severe side effects. It is noteworthy that these same guidelines also significantly reduce the number of cardiac conditions for which antibiotic prophylaxis is recommended.
The AHA/ ACC guidelines, however, remain controversial. The Australian guidelines for the prevention of endocarditis, the British Society of Antimicrobial Therapy, and the European Society for Cardiology all continue to recommend antibiotic prophylaxis for most or all invasive dental, gastrointestinal, respiratory, and genitourinary procedures that involve trauma to mucosal surfaces.15,38,39 The National Institute for Health and Clinical Excellence recommends prophylaxis for invasive genitourinary or gastrointestinal procedures at the site of known infection.40 Proponents of more liberal use of prophylactic antibiotics suggest that the lack of randomized controlled trials to support the practice does not necessarily invalidate the benefit of antibiotics, and they suggest that the risk of antibiotic usage was considered in prior risk-benefit analyses leading to previous guidelines. In addition, they believe that infectious endocarditis has such a high morbidity and mortality rate that even a small reduction in the likelihood of developing the disease warrants the utilization of antibiotics.
From the standpoint of an emergency physician, it is important to understand the controversy in order to educate patients, and to understand that patients with prosthetic valves are considered at high risk for the development of infectious endocarditis by all of the aforementioned expert panels. Therefore, all patients with prosthetic valves undergoing a procedure manipulating the gingival tissue (such as a mandibular nerve block or drainage of an oral abscess) in the emergency department should be provided antibiotic prophylaxis. In addition, the emergency department physician should consider prophylaxis in any patient with a prosthetic valve undergoing procedures violating the mucosal barrier in the respiratory, gastrointestinal, or genitourinary tracts (such as those undergoing endoscopy where biopsies will be taken) or trauma with significant skin contamination. Prophylaxis is not needed for endotracheal intubation, insertion of urinary catheters, vaginal delivery, endoscopy without biopsy, uterine dilation and curettage, or insertion/removal of an intrauterine device.
Typically, antibiotic prophylaxis for dental procedures consists of 2 g of amoxicillin given by mouth one hour prior to the procedure, or 600 mg clindamycin given orally or intravenously one hour prior to the procedure for patients who are penicillin-allergic. Patients who are unable to take oral medications may be administered 2 g of ampicillin intravenously, also administered one hour prior to the procedure.41
Summary
Prosthetic valves are becoming increasingly common as the population ages, surgical techniques improve, and implantable devices continue to be refined. These life-saving devices are associated with unique and sometimes catastrophic complications.
In addition to identifying and stabilizing patients with prosthetic valves who have acutely decompensated, emergency physicians can improve patient care and long-term prognosis by having a high level of suspicion for chronic valve dysfunction and ensuring that these patients are being followed closely by a primary physician. All patients with prosthetic valves should have coagulation studies when seen in the emergency department to minimize the complications of long-term anticoagulation and ensure adequacy of therapy. Patients should be educated about the need for evaluation if they develop fever. Patients with prosthetic valves should be provided antibiotics prior to invasive dental or respiratory tract procedures, including those performed in the emergency department. Finally, emergency physicians should be careful when prescribing medications for patients with mechanical heart valves because medication interactions are a common reason for inappropriate warfarin levels.
References
1. Rosamond W, Flegal K, Furie K, et al. Heart disease and stroke statistics2008 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 2008;117:e25-146.
2. Yoganathan AP, He Z, Jones SC. Fluid mechanics of heart valves. Annu Rev Biomed Eng 2004;6:331-362.
3. Butany J, Ahluwalia MS, Munroe C, et al. Mechanical heart valve prostheses: Identification and evaluation. Cardiovasc Pathol 2003;12:1-22.
4. Emery RW, Mettler E, Nicoloff DM. A new cardiac prosthesis: The St. Jude Medical cardiac valve: In vivo results. Circulation 1979;60(2 Pt 2):48-54.
5. Sun JC, Davidson MJ, Lamy A, et al. Antithrombotic management of patients with prosthetic heart valves: current evidence and future trends. Lancet 2009;374:565-576.
6. Khan SS, Gray RJ. Valvular emergencies. Cardiol Clin 1991;9:689-709.
7. Wellford AL, Wellford LA. Prosthetic heart valve. Emerg Med Clin North Am 1994;12:597-631.
8. Butchart EG. Antithrombotic management in patients with prosthetic valves: A comparison of American and European guidelines. Heart 2009;95:430-436.
9. Bonow RO, Carabello BA, Chatterjee K, et al. 2008 Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): Endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Circulation 2008;118:e523-661.
10. Bonow RO, Carabello BA, Kanu C, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (writing committee to revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): Developed in collaboration with the Society of Cardiovascular Anesthesiologists: endorsed by the Society for Cardiovascular Angiography and Interventions and the Society of Thoracic Surgeons. Circulation 2006;114:e84-231.
11. Chan L, Duncan T. Expeditious diagnosis of primary prosthetic valve failure. Am J Emerg Med 1999;17:179-181.
12. Daniell JE, Nelson BS, Ferry D. ED identification of cardiac septal abscess using conduction block on ECG. Am J Emerg Med 2000;18:730-734.
13. Vesey JM, Otto CM. Complications of prosthetic heart valves. Curr Cardiol Rep 2004;6:106-111.
14. McDonald JR. Acute infective endocarditis. Infect Dis Clin North Am 2009;23:643-664.
15. Elliott TS, Foweraker J, Gould FK, et al. Guidelines for the antibiotic treatment of endocarditis in adults: report of the Working Party of the British Society for Antimicrobial Chemotherapy. J Antimicrob Chemother 2004;54:971-981.
16. Dajani AS, Taubert KA, Wilson W, et al. Prevention of bacterial endocarditis. Recommendations by the American Heart Association. JAMA 1997;277:1794-1801.
17. Aoyagi S, Fukunaga S, Suzuki S, et al. Obstruction of mechanical valve prostheses: Clinical diagnosis and surgical or nonsurgical treatment. Surg Today 1996;26:400-406.
18. Goldberg L, Mekel J. In response to Lengyel M, Vandor L. The role of thrombolysis in the management of left sided obstructive prosthetic valve thrombosisis there a case for it? J Heart Valve Dis 2001;10:638-649. J Heart Valve Dis 2002;11:452-3; author reply 453-454.
19. Gupta D, Kothari SS, Bahl VK, et al. Thrombolytic therapy for prosthetic valve thrombosis: Short- and long-term results. Am Heart J 2000;140:p. 906-916.
20. Lengyel M, Horstkotte D, Voller H, et al. Recommendations for the management of prosthetic valve thrombosis. J Heart Valve Dis 2005;14:567-575.
21. Lengyel M, Vandor L. The role of thrombolysis in the management of left-sided prosthetic valve thrombosis: A study of 85 cases diagnosed by transesophageal echocardiography. J Heart Valve Dis 2001;10:636-649.
22. Rinaldi CA, Heppell RM, Chambers JB. Treatment of left-sided prosthetic valve thrombosis: Thrombolysis or surgery? J Heart Valve Dis 2002;11:839-843.
23. Roudaut R, Lafitte S, Roudaut MF, et al. Fibrinolysis of mechanical prosthetic valve thrombosis: A single-center study of 127 cases. J Am Coll Cardiol 2003;41:653-658.
24. Roudaut R, Roques X, Lafitte S, et al. Surgery for prosthetic valve obstruction. A single center study of 136 patients. Eur J Cardiothorac Surg 2003;24:868-872.
25. Wessman DE, Stafford CM. The postcardiac injury syndrome: Case report and review of the literature. South Med J 2006;99:309-314.
26. Baddour LM, Wilson WR, Bayer AS, et al. Infective endocarditis: Diagnosis, antimicrobial therapy, and management of complications: a statement for healthcare professionals from the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease, Council on Cardiovascular Disease in the Young, and the Councils on Clinical Cardiology, Stroke, and Cardiovascular Surgery and Anesthesia, American Heart Association: endorsed by the Infectious Diseases Society of America. Circulation 2005;111:e394-434.
27. Dunmire SM. Infective Endocarditis and Valvular Heart Disease. In: Marx JA, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. Philadelphia: Mosby Elsevier; 2006:1300-1309.
28. Wilson W, Taubert KA, Gewitz M, et al. Prevention of infective endocarditis: Guidelines from the American Heart Association: A guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation 2007;116:1736-1754.
29. Wolff M, Witchitz S, Chastang C, et al. Prosthetic valve endocarditis in the ICU. Prognostic factors of overall survival in a series of 122 cases and consequences for treatment decision. Chest 1995;108: 688-694.
30. Wilson WR, Karchmer AW, Dajani AS, et al. Antibiotic treatment of adults with infective endocarditis due to streptococci, enterococci, staphylococci, and HACEK microorganisms. American Heart Association. JAMA 1995;274:1706-1713.
31. Koca V, Bozat T, Sarikamis C, et al. The use of transesophageal echocardiography guidance of thrombolytic therapy in prosthetic mitral valve thrombosis. J Heart Valve Dis 2000;9:374-378.
32. Montorsi P, De Bernardi F, Muratori M, et al. Role of cine-fluoroscopy, transthoracic, and transesophageal echocardiography in patients with suspected prosthetic heart valve thrombosis. Am J Cardiol 2000;85: 58-64.
33. Schoen FJ, Levy RJ. Bioprosthetic heart valve failure: Pathology and pathogenesis. Cardiol Clin 1984;2:717-739.
34. Afridi I, Apostolidou MA, Saad RM, et al. Pseudoaneurysms of the mitral-aortic intervalvular fibrosa: Dynamic characterization using transesophageal echocardiographic and Doppler techniques. J Am Coll Cardiol 1995;25:137-145.
35. Blais C, Dumesnil JG, Baillot R, et al. Impact of valve prosthesis-patient mismatch on short-term mortality after aortic valve replacement. Circulation 2003;108:983-988.
36. Rahimtoola SH. The problem of valve prosthesis-patient mismatch. Circulation 1978;58:20-24.
37. Otto C. Echocardiographic evaluation of prosthetic valve dysfunction. In: Textbook of Clinical Echocardiography. Philadelphia: WB Saunders; 2000.
38. Horstkotte D, Follath F, Gutschik E, et al. Guidelines on prevention, diagnosis and treatment of infective endocarditis executive summary; the task force on infective endocarditis of the European society of cardiology. Eur Heart J 2004;25:267-276.
39. Daly CG, Currie BJ, Jeyasingham MS, et al. A change of heart: The new infective endocarditis prophylaxis guidelines. Aust Dent J 2008;53:196-200; quiz 297.
40. Richey R, Wray D, Stokes T. Prophylaxis against infective endocarditis: Summary of NICE guidance. BMJ 2008;336:770-771.
41. Dajani AS, Taubert KA, Wilson W, et al. Prevention of bacterial endocarditis. Recommendations by the American Heart Association. Circulation 1997;96:358-366.
More than 100,000 prosthetic heart valves are implanted each year in North America, and another 300,000 are done annually worldwide.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
