ECG Review: A Funny Feeling in My Chest
ECG Review
A Funny Feeling in My Chest
By Ken Grauer, MD, Professor, Department of Community Health and Family Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
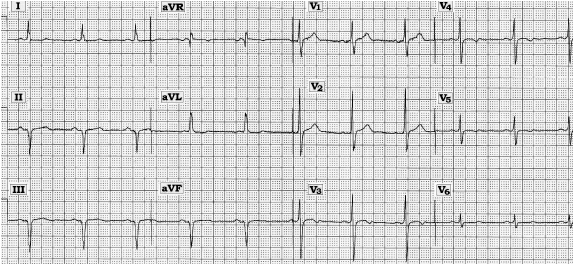
Scenario: The ECG shown above was obtained from a 42-year-old man who presented with the complaint of "a funny feeling in my chest." A prior ECG had been done a few years earlier for a similar concern, and was interpreted as showing "possible old inferior infarction vs left anterior hemiblock." How do you interpret his current tracing? Does it explain his symptoms? Does it correlate with the interpretation of his previous ECG?
Interpretation
The rhythm is sinus at 65 beats/minute. The temptation is there to interpret the rest of this ECG as showing normal intervals, left axis deviation with inferior QS complexes consistent with prior inferior infarction vs left anterior hemiblock. Alas, this is not what is occurring.
The first clue to something amiss lies in lead V1, which manifests an R > S wave. This is distinctly unusual, since the S wave is almost always predominant in right-sided lead V1. Diagnostic entities to consider as the cause of a tall R > S wave in lead V1 include right ventricular hypertrophy, right bundle branch block when the QRS complex is wide, posterior infarction, cardiomyopathy, normal variant, and accessory pathway conduction as occurs with Wolff-Parkinson-White (WPW) syndrome.
Close inspection of the PR segment and the initial (ascending) portion of the QRS complex in each of the precordial leads reveals ever-so-slight (but real) slurring, consistent with the delta wave of WPW. This delta wave is best seen in the above tracing in leads V4,V5. The QRS complex is not always widened with WPW. This is because: 1) the accessory pathway (AP) may hook into the regular conduction system close to the Bundle of His, resulting in a much shorter path of conduction through unspecialized myocardial tissue; and/or 2) there may be simultaneous conduction down the normal and accessory pathway, with net effect cancelling some of the QRS widening.
We suspect the prior ECG on this patient was misinterpreted. WPW is notorious for producing "pseudo-infarct" patterns (as seen in the inferior leads here). Similarly, no clinical significance can be derived in the setting of AP conduction from the ST-T wave abnormalities seen in the anterior precordial leads. Whether the "funny feeling" in this patient's chest is the result of WPW-associated arrhythmias is a question requiring clinical correlation.
The ECG shown above was obtained from a 42-year-old man who presented with the complaint of "a funny feeling in my chest."Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
