Evaluation and Treatment of Acute Arthritis
Evaluation and Treatment of Acute Arthritis
Authors:
P. Charles Inboriboon, MD, Senior Clinical Instructor, Department of Emergency Medicine, University of Rochester, NY.
Pim Jetanalin, MD, Bassett Healthcare, Department of Internal Medicine, Cooperstown, NY.
Peer Reviewer:
John H. Burton, MD, Vice Chair for Academic Affairs, Residency Program Director, Department of Emergency Medicine, Albany Medical Center, NY.
This article originally appeared in the January 4, 2010 issue of Emergency Medicine Reports.
Introduction
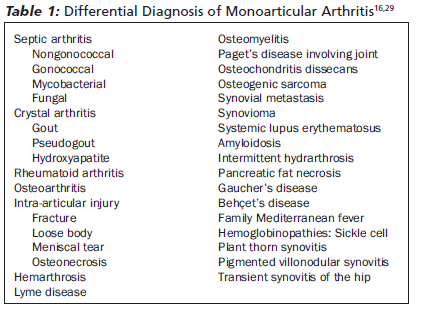
Patients with acute joint pain present a diagnostic dilemma for many emergency physicians. Classically the joints are hot, swollen, and tender, with reduced range of motion. The differential diagnosis for the painful joint is extensive. (See Table 1.) Distinguishing between the various causes can be difficult, especially since there may be more than one cause concomitantly.1 It is important to promptly diagnose and treat the various etiologies of joint pain, and paramount that septic arthritis be ruled out in all painful joints.
 |
Anatomy and Physiology of the Joint
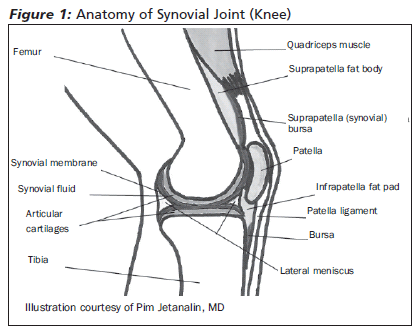
The parts of a synovial joint are illustrated in Figure 1. The synovium lies within the joint capsule, a connective tissue structure that surrounds the articular surfaces of two or more bones. It is responsible for the production of synovial fluid, which provides nutrition to the avascular articular cartilage and lubricates the cartilage surfaces. The synovium contains numerous immune-modulating cells involved in the recruitment of inflammatory cells that produce arthritis.2,3 Activation of these cells during inflammatory arthritis causes the synovium to outgrow its vasculature's ability to exchange nutrients and toxins. This leads to a hypoxic and acidotic joint environment and subsequent joint destruction.3
 |
The General Approach to the Hot Joint
The history should focus on the onset of symptoms, a comparison to previous joint pain, and concurrent symptoms such as rash or fever. A temporal history of disease progression is important, especially in the setting of polyarticular or migratory joint pain. Inquire into previous joint disease, rheumatic disorders, autoimmune disorders, diabetes, malignancies, history of intravenous drug use, and alcoholism. These factors are associated with various disease processes, including viral, reactive, rheumatoid, crystalloid, and septic arthritis. Ask about sexual exposure, travel, and exposure to tuberculosis and Lyme disease. Some medications can increase the likelihood of crystalloid, rheumatoid, and septic arthritis.
Physical Examination. The physical examination should focus on the affected joint, the general musculoskeletal exam, and a focused physical examination. Examine the affected joint and periarticular area for erythema, swelling, and tenderness to palpation. Compare findings to the contralateral joint. Arthritis typically presents with generalized findings. Focal findings may be indicative of periarticular pathology such as tendinitis or bursitis. Check the overlying skin for cellulitis, rashes, pustules, wounds, and other lesions suggesting infectious arthritis.
Diagnostic Adjuncts. Although diagnosing the specific cause(s) of acute joint pain is dependent on clinical suspicion, there are a number of diagnostic adjuncts. Remember that there may be more than one disease process affecting a joint, and that septic arthritis must be excluded in all cases of undifferentiated acute joint pain.
The most important tool used in acute arthritis is synovial fluid aspiration. Arthrocentesis is both diagnostic and therapeutic. Removal of joint fluid reduces pain by decreasing intra-articular pressure.4
Contraindications to arthrocentesis include superficial infection over the needle insertion site and coagulopathy. Prosthetic joints are a relative contraindication to arthrocentesis.
Arthrocentesis is performed blindly with the use of anatomic landmarks or with the use of ultrasound or fluoroscopy.5-10 During arthrocentesis, flow of synovial fluid may stop. Potential causes include temporary obstruction by synovial fronds, blockage by fibrin or other debris, loculated synovial fluid collections, or displacement of the needle outside the joint cavity. If flow becomes obstructed, a small amount of fluid can be injected back into the joint to clear any obstruction.4
Arthrocentesis is a generally safe procedure. The risk of infection from arthrocentesis is extremely low, at an incidence of 18 per 250,000 intra-articular steroid injections.11
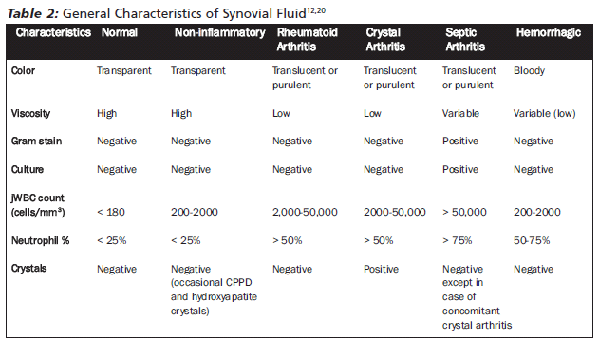
Synovial Fluid Analysis. Normal synovial fluid typically is colorless or pale yellow and clear. (See Table 2.) It is highly viscous and should be able to form a string stretching approximately 10 cm before surface tension is broken.12 In cases of inflammatory arthritis, viscosity can be markedly reduced. Cloudy fluid suggests the presence of inflammatory cells, fibrin, crystals, lipids, or amyloid. Bloody fluid is suggestive of trauma, tumors, or hematologic disorders.
 |
Obtain a Gram stain and cultures of the synovial fluid if septic arthritis is suspected. If there is sufficient fluid, obtain a cell count. An elevated polymorphonuclear leukocyte (PMN) count suggests an inflammatory and/or infectious process. Examine the synovial fluid for crystals. Monosodium urate crystals (MSU) are strongly birefringent and are easily identified under a polarized microscope.
Re-evaluation in Undiagnosed Cases. If there is low suspicion for septic arthritis and the initial evaluation is not diagnostic, arrange for follow up in 2-5 days for re-evaluation as an outpatient. At that time, serum testing, radiographs, and synovial fluid analysis should be repeated and other imaging modalities considered.13
Case 1. A 76-year-old male with diabetes and rheumatoid arthritis presents with a 2-day history of increasing right knee pain, especially with weight bearing. He denies trauma.
On physical examination, he is afebrile. There is a healing non-infected abrasion over the anterior tibial surface. The right knee joint is warm, diffusely tender, and slightly swollen with an appreciable effusion. The complete blood cell count (CBC) is normal, the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) levels are slightly elevated. The right knee X-ray shows chronic arthritic changes. Arthrocentesis yields 10 cc of cloudy fluid. The synovial white blood cell count is 76,000 with 90% polymorphonuclear cells. The Gram stain is negative, and the cultures are pending.
Septic Arthritis
Epidemiology. In the general population, the annual incidence of septic arthritis ranges from 2-5 per 100,000 persons.14,15 The rate is 10-30 times higher in patients with rheumatoid arthritis or prosthetic joints.12,14 It is estimated that 8-27% of patients who present to the emergency department with acute arthritis eventually will be diagnosed with septic arthritis.16 Even with timely diagnosis, hospitalization, and antibiotic therapy, the mortality rate is estimated at 7-25%.5,12,16-18 The mortality rate can approach 50% in patients with Staphylococcus aureus-associated septic arthritis.5 One-third to one-half of survivors suffer permanent loss of joint function.5,11
Pathophysiology. Bacteria invade the synovial space via hematogenous spread or direct invasion. Bacterial invasion of synovial space leads to joint destruction through pathogen-mediated inflammation, host response-mediated inflammation, and tissue ischemia. Bacterial enzymes and toxins directly damage cartilage. Host-mediated cytokines activate proteolytic enzymes that autodigest cartilage and bone. Vascular congestion and local inflammation contribute to development of a purulent effusion. This growing effusion eventually leads to elevated joint pressure that tamponades synovial blood flow and causes cartilage anoxia.19 Septic arthritis can lead to joint destruction in as few as 10 days and can progress to systemic sepsis.20
Gram-positive organisms are the most common pathogens in non-gonococcal septic arthritis (70-80% of cases). Staphylococcus is the most common organism, followed by streptococcus.11,16-18,21,22 Most infections occur from disruptions to skin or mucosal barriers.19 Community-acquired methicillin resistant Staphylococcus aureus (CaMRSA) associated septic arthritis is increasing in incidence and, in some regions, is the predominant organism.22,23 Patients with prosthetic hardware are also at risk for coagulase negative staphylococci infection.
Gram-negative infection accounts for 15-20% of non-gonococcal septic arthritis cases, most often H. influenza, E. coli, and P. aeruginosa.11,21 Gram-negative bacteria usually originate from the gastrointestinal or genitourinary system.19 It more commonly affects elderly and immunocompromised patients.22
Anaerobes, fungi, tuberculosis, and brucellosis are rare causes of septic arthritis. They are more common in immunocompromised patients or in specific at-risk populations.20,24 Anaerobic bacteria joint infections generally occur in the setting of penetrating trauma.22,25 Brucellosis-associated septic arthritis is rare and typically occurs in patients with a history of occupational exposure.20,24
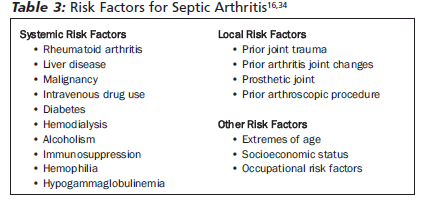
Factors that impair normal joint function put specific joints at increased risk for septic arthritis. (See Table 3.) These factors include prior joint trauma, the presence of arthritic changes, and the presence of joint prosthesis.19 It is estimated that 46% of bacterial arthritis cases occur in joints with pre-existing joint damage.20 Systemic disorders that increase the risk for septic arthritis include diabetes, pre-existing rheumatoid arthritis, liver disease, chronic kidney disease, malignancy, intravenous drug use, hemodialysis, alcoholism, organ transplant, hemophilia, hypogammaglobulinemia, and acquired immune deficiency syndrome (AIDS).19,21,26 Extremes of age (newborns and those older than 80 years), diabetes, and HIV infection increase the risk of infection19 and also increase the risk of death from septic arthritis.17
 |
Clinical Presentation. The septic joint typically is acutely hot, painful, and swollen, with reduced range of motion. Patients typically present early, but a later presentation may be seen with prosthesis infection or low-virulence organisms like tuberculosis.18,25 It is monoarticular in 80-90% of cases.19-21,24,25 The most commonly affected joints are the knee (50%), hip, and shoulder.6,11,19,20,22 In pediatric patients, the hip is the most common site.27 Septic arthritis in fibrocartilaginous joints of the skeleton such as sternoclavicular, sacroiliac, and intervertebral disk spaces is strongly associated with intravenous drug abusers.28
The absence of fever does not rule out septic arthritis.16,19 The presence of fever, rigors, and diaphoresis is neither specific nor sensitive.6,11,16,18-20,22,26 In children, septic arthritis usually is accompanied by fever, malaise, poor appetite, irritability, and progressive reluctance to use the affected limb.28 Geriatric and immunocompromised patients are often afebrile.
The most sensitive indicators of septic arthritis are joint pain (85%) and swelling (75%). These findings, though sensitive, are not specific; they are found in other inflammatory joint processes.16,18 Disproportionate pain, loss of function, erythema, or systemic symptoms should increase suspicion for septic arthritis in patients with arthritic disease.20
Diagnostic Tests. Normal ESR and CRP levels have a negative predictive value, but they do not rule out septic arthritis.1,5,7,20,29,30 ESR and CRP are useful for monitoring response to treatment in confirmed cases of septic arthritis.22 Blood cultures identify the offending organism in 50-70% of non-gonococcal septic arthritis cases.11
Plain radiographs provide no benefit in diagnosing septic arthritis but may be useful in looking for underlying joint damage or concurrent osteo-myelitis.11,22,31 Magnetic resonance imaging (MRI) and scintigraphy can distinguish septic arthritis from non-inflammatory arthritis, but do not differentiate between septic, rheumatoid, and crystalloid arthritis.16,22 Reserve scintigraphy for suspected cases of synovial fistulas and MRI for cases concerning for concomitant osteomyelitis.10,22
Arthrocentesis is necessary in all suspected cases of septic arthritis. Although needle aspiration through overlying cellulitis is a contraindication, some advocate going through infected skin when necessary.16 When arthrocentesis does not yield adequate fluid, a small amount of sterile saline can be used to irrigate the joint space in order to collect fluid for Gram stain and culture.12 Cloudy or purulent aspirate is suggestive of septic arthritis.4,21 It is also important to remember that the presence of crystals does not exclude the diagnosis of septic arthritis.1 Synovial protein, glucose, lactate, and serologic markers can increase suspicion for septic arthritis, but do not discriminate between other causes of inflammatory arthritis.22,25,32-34
An elevated joint white blood cell count (jWBC) and a predominance of polymorphonuclear cells are the most useful indicators of septic arthritis.15,32 A markedly elevated jWBC (> 50,000/mL) is highly suggestive of septic arthritis (88% specificity). However, a jWBC less than 50,000/mL does not rule out septic arthritis (sensitivity 61%). Treatment is indicated when there is high clinical suspicion for septic arthritis and an elevated jWBC (> 20,000/mL).13,35-37
Definitive diagnosis is confirmed by either Gram stain or culture. Unfortunately, Gram stain is positive in only half of all septic arthritis cases.6,25 Therefore, empiric antibiotics should be started in all suspected cases.20 Cultures will confirm the diagnosis. Polymerase chain reaction (PCR) testing is a potential new adjunct for diagnosing septic arthritis, and it may be useful when antibiotics are started before synovial fluid was obtained.38 It can identify borrelia, gonorrhea, and other species typically difficult to culture.25
Treatment. Patients with septic arthritis should be hospitalized and orthopedics consulted, especially in cases of suspected prosthesis infection.11,20 With early and aggressive treatment, 50% of patients with S. aureus-associated septic arthritis recover without residual joint damage.11 (Table 4 summarizes current antibiotic therapy.)11,22,24,25 Patients who are elderly, immunosuppressed, or intravenous drug abusers should be placed on broad-spectrum antibiotics to cover both gram-positive and gram-negative organisms.11,21,22 Young, healthy, sexually active patients with low suspicion for non-gonococcal arthritis should be treated for gonorrhea (see next section).
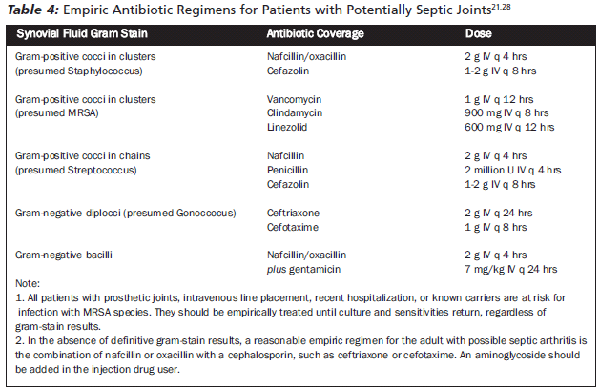 |
There are no data on the optimal duration of antibiotic treatment. IV antibiotics are continued for up to two weeks or until clinical improvement, followed by appropriate oral antibiotics for an additional 2-6 weeks.20,22 Clinical improvement and inflammatory markers such as ESR and CRP are useful in guiding duration of antibiotic therapy.22
Drainage of the infected joint is recommended to decrease joint damage caused by pathogens, host inflammation, and elevated intra-articular pressure. Drainage can be performed through serial needle aspirations or surgery.24,25 There is no demonstrated superiority of one treatment over the other;22 however, arthroscopic or open joint drainage is indicated when serial aspirations do not yield satisfactory results and in cases of complicated fluid collections or osteomyelitis.20 In addition to antibiotic therapy and joint drainage, treat underlying comorbidities and discontinue immunosuppressants.11,20
Gonococcal Arthritis
Gonococcal arthritis is the most common cause of non-traumatic monoarthritis in young sexually active persons.27 It is estimated that 3% of patients with untreated gonorrhea infections develop gonococcal arthritis.11 Infected women tend to have a more asymptomatic gonococcal infections than males and are therefore more likely to present with untreated infections.19 There is a 3:1 female to male predominance.7,19
Gonococcal arthritis presents as a migratory polyarthralgia that affects the knees, ankles, and wrists.25 It is often associated with fever, tender tenosynovitis, painless vesicles, pustules, macules, and/or papules on the extremities.11,19,32 However, 30-40% of the time it presents solely as a monoarticular arthritis.19
The diagnosis of gonococcal arthritis rests largely on clinical suspicion. Consider obtaining oropharyngeal, genital, and anorectal cultures in addition to blood cultures based on the clinical history and exam. Up to 80% of suspected cases of gonococcal septic arthritis will be identified by peripheral culture.21 PCR also may aid in confirming the diagnosis of gonococcal arthritis. With early and aggressive treatment, 95% of patients with gonococcal arthritis recover without any residual joint damage.11
Case 1 Revisit. The patient's history, elevated jWBC, ESR, CRP, and WBC suggest septic arthritis. The patient is started on IV antibiotics and admitted to orthopedics.
Case 2. A 56-year-old male with a history of gout and chronic kidney disease presents with left elbow pain that has worsened over the last 24 hours. He reports the pain is typical of his previous gout attacks. He denies fever, chills, or rigors.
On physical examination, he appears well and is afebrile. The left elbow reveals a gouty tophus. The joint is slightly red, tender, warm to touch, and has a palpable effusion. Pain is elicited with both passive and active movement.
The patient receives analgesia. The CBC is normal; ESR and CRP are slightly elevated. X-rays of the left elbow show no fracture but reveal joint destruction consistent with chronic gouty arthritis. Arthrocentesis yields synovial fluid that appears thick and white, with a jWBC of 36,000, 70% polymorphonuclear cells. The Gram stain is negative, and the cultures are sent. Polarized microscopy shows needle-shaped crystals and strongly negative birefrigence.
Gout
Epidemiology. Gout is an inflammatory arthritis caused by deposition of sodium urate crystals in joints. It afflicts more than 2.1 million Americans.39 The prevalence is greater in men than women, affecting 0.7-1.4% of men and 0.5-0.6% of women. Its prevalence is greatest over age 65, with 4.4-5.2% of men and 1.8-2.0% of women affected.11 The overwhelming majority of women (90%) are post-menopausal at the time of their first gout attack.40
Pathophysiology. An elevated uric acid level is a prerequisite to developing gout.41 High levels of uric acid form uric acid salts that are deposited in the joint synovium.11 The crystals activate inflammatory mediators that stimulate the migration of neutrophils into the synovial spaces and the release of proteolytic enzymes that damage the joint.11 Gout crystal-protein complexes, known as tophi, deposit outside the synovium in tendons, cartilage, ligaments, bones, and bursae. They commonly deposit in the ears, nose, feet, fingers, knees, and around or in the olecranon and prepatellar bursae.
A gout flare can last from several hours to weeks. A typical flare is self-limited to 2-3 weeks.11,42 Untreated, most patients will have improvement in joint pain by day 5, and improvement of swelling by day 7. If left untreated, most patients will develop recurrent acute arthritis that eventually will lead to chronic arthritis. Without the use of urate-lowering agents, 20-40% of patients will develop chronic tophaceous gouty arthritis.11
Risk factors for gout include high alcohol intake, hyperlipidemia, obesity, renal disease, lymphoproliferative, and myeloproliferative disorders, and family history of gout.11,43 Various medications have been implicated in the development of gout, including diuretics, low-dose aspirin, cyclosporins, ethambutol, pyrazinamide, nicotinic acid, intravenous heparin, tacrolimus, and other cytotoxic drugs.11,43,44 Diuretics are associated with 75% of cases in the elderly. This proportion approaches 95-100% in geriatric women. There also is increasing evidence of an association between gout and coronary artery disease, especially in women.24,43
Clinical Presentation. Gout presents as an acute onset of pain with inflammation, including erythema, redness, and joint warmth. An attack often follows the intake of purine-rich foods, minor trauma, alcohol intake, surgery, or infection.43 A single joint is involved in about 85-90% of first attacks44; more than half of first attacks occur in the first metatarsophalangeal joint.11,42,43 Other commonly affected joints include the wrist, elbows, knees, and ankles. The patient may have systemic symptoms including fever, chills, and fatigue. Gout in elderly patients may be more indolent or chronic and more commonly polyarticular.11
In select cases, the clinical diagnosis of acute primary gout arthritis can be made without synovial fluid analysis. The criteria developed by the American College of Rheumatology are outlined in Table 5. If the patient does not meet these criteria, consider an alternative diagnosis such as infection.
 |
Pain occurs abruptly, reaching its maximum in one day. Pain that continues to worsen after one day should increase suspicion for another process such as septic arthritis. If there is pain out of proportion to typical flares or pain in a previously unaffected joint, consider septic arthritis.25
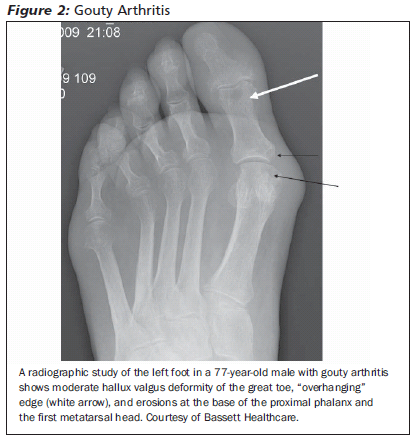
Diagnostic Testing. Radiographic findings suggestive of gout include asymmetric joint swelling and subcortical cysts without erosions. (See Figure 2.) Laboratory tests are not useful in diagnosing gout; in some cases, the uric acid level is normal. Definitive diagnosis of gout requires synovial fluid analysis,11,13 with monosodium urate monohydrate crystals in the synovial fluid and negative cultures.
 |
Treatment. Treatment focuses on treating acute pain and decreasing recurrent attacks.11 Early treatment is important to achieve rapid and complete relief of symptoms.44 NSAIDs are considered first-line treatment. They typically reduce major symptoms within 24 hours of initiation.40 More than 90% of patients with acute attacks achieve complete resolution of symptoms within 5-8 days of starting NSAIDs. The maximum dose commonly is started at the time of onset, continued for a full 24 hours, then tapered over the next 2-3 days.42 Potential side-effects of NSAIDs include peptic ulcer disease, gastritis, renal insufficiency, and fluid retention. When given to high-risk patients, short-term NSAID use is recommended.11 Gastrointestinal bleeding risk also can be reduced with co-administration of a proton-pump inhibitor.42 COX-2 inhibitors also have been effective in reducing the rate of GI bleeds, but the benefit must be weighed against the risk of cardiovascular events.32
Intra-articular steroid injection is an effective treatment for patients with one or two actively inflamed joints. Pain typically resolves 24-48 hours post-injection.42,45 It is recommended in patients with contraindications to NSAID use. The risk of systemic side effects is low, but ensure that the joint is not infected prior to injection.11 The dose for triamcinolone is 10 mg in knees and 8 mg in smaller joints.42
Systemic steroids are an alternative treatment and are recommended in those with contraindications to NSAIDs and in the elderly. Oral prednisolone, 35 mg daily for 5 days, is equivalent in effectiveness to naproxen.12 Alternatively, oral prednisone at 30-60 mg daily followed by a steady taper over 10-14 days is recommended. The taper should be extended to 3 weeks in patients with involvement of five or more joints.40,42 Use of a taper may reduce the chance of a rebound gout flare.42 Side effects of systemic steroid use include renal failure, fluid retention, ulcers, hypertension, and hyperglycemia. These are all rare and short-lived following the discontinuation of steroids.11
Synthetic adrenocorticotropin hormone (ACTH) can be used in the treatment of acute gout. ACTH stimulates cortisol and acts to inhibit inflammation.42 Its effectiveness is comparable to corticosteroid therapy.11,41 ACTH treatment can be given as a taper as follows: Day 1: 80 IU q 8 hrs, Day 2: 40 IU q 12 hrs, Day 3-14: 40 IU daily.42
Colchicine can be effective in up to 75% of young healthy patients who present shortly after onset of an acute gout flare.11 The exact mechanism of action is not clear, but it is believed that colchicine down-regulates cytokine function and suppresses crystal-protein complex induced inflammation.42 The recommended regimen for colchicine is 1 mg orally, followed by 0.5 mg every 2 hours until symptoms are relieved or toxicity develops.42 Relief typically occurs within 24 hours when given orally and within 8 hours when given IV.42 Even though intravenous colchicine is useful in rapidly aborting attacks, its use is not recommended. Extravasation of colchicine can cause tissue necrosis and thrombophlebitis. Colchicine has a narrow therapeutic window. Almost all users exhibit side effects, with the most common being nausea, vomiting, diarrhea, and/or abdominal pain.42,46 Colchicine is metabolized by the kidney and liver, so its use in patients with hepatic or renal insufficiency is problematic.11,42 It has been lethal at cumulative doses as low as 6-7 mg.42 Lethal side effects are more common when it is used intravenously or when it is administered to patients with renal or hepatic dysfunction. Side effects include alopecia, bone marrow suppression, neuromyopathy, renal failure, disseminated intravascular coagulation, seizures, arrhythmias, and hepatic necrosis.42,44 Given the high rate of experienced side effects compared to therapeutic benefit and its potential lethality, colchicine is recommended as second-line therapy when both NSAIDs and steroids are contraindicated.46
Local application of cold packs reduces pain and swelling.45 Instruct the patient to rest the afflicted joint for 1-2 days and arrange follow-up with the patient's treating physician.42
The presence of crystals does not rule out septic arthritis. Antibiotics can be started until culture results return.1 Failure to respond to therapy after 1 week should prompt re-evaluation of the diagnosis and management plan.13
Pseudogout
Epidemiology. Pseudogout is another crystalloid arthritis that presents as acute monoarticular or polyarticular arthritis. The term "pseudogout" refers to the acute, gout-like attacks that occur in some individuals.47 It is more common in females and typically occurs in the elderly.11 The average age at presentation is 65 years.11
Pathophysiology. Pseudogout results from the deposition of CPPD into articular cartilage. As in gout, these crystals lead to the influx of inflammatory proteins and cells that lead to inflammation. Unlike gout, CPPD crystals can invade joint space without any history of serum abnormality. The majority of cases are idiopathic, but 5% of cases are associated with hyperparathyroidism, hypothyroidism, hypomagnesemia, hypophosphatemia, or hemachromatosis.11
Clinical Presentation. Pseudogout typically involves large joints, with the knee being the most common, followed by the wrist and ankle. It rarely affects the first metatarsophalangeal joint.48 Similar to gout, acute pseudogout flares can be associated with fever and chills. Attacks can be precipitated by minor trauma or intercurrent conditions such as surgery, pregnancy, pneumonia, myocardial infarction, and cerebrovascular accidents.48
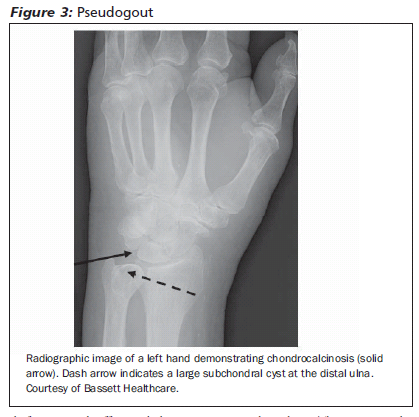
Diagnostic Tests. X-rays often show intra-articular calcifications called chondrocalcinosis, which appear as punctate or linear calcifications in fibrocartilage and hyaline cartilage.11 Radiographs may show calcification of the knee menisci, triangular ligament of the wrist, and in the cartilage.11 (See Figure 3.) Laboratory blood work generally is not useful.
 |
Arthrocentesis confirms the diagnosis of pseudogout. The typical jWBC level ranges from 10,000-20,000 cells/mm3.11 Any abnormally elevated level should increase suspicion for another processes, specifically septic arthritis. Crystal analysis demonstrates CPPD crystals, which are pleomorphic and weakly positive under microscopy light.
 |
Treatment. Treatment is similar to that for gout. Joint aspiration often relieves the pain. NSAIDs and steroids are the mainstays of pharmacologic treatment. Colchicine can be useful but is rarely necessary; its effectiveness is less predictable in pseudogout than in gout.47
Case 2 Revisited. Synovial fluid analysis shows no evidence of infection, and suspicion for septic arthritis is extremely low. The patient has contraindications to NSAID use given his underlying chronic kidney disease, so he is treated with 8 mg of intra-articular triamcinolone and discharged.
Case 3. A 52-year-old female with chronic knee, wrist, and hand stiffness and pain presents with increased left knee pain for the past 3 days. The pain and swelling have been gradual in onset. Her pain is worse in the morning and improves throughout the day. She previously tested positive for rheumatoid factor. She denies any fever or trauma.
On examination, the patient is afebrile and nontoxic. The left knee is warm and tender with a palpable effusion. The wrists exhibit mild swelling bilaterally, and the hands are swollen and red at metacarpophalangeal joints. The CBC is normal; ESR and CRP are slightly elevated. X-rays of the left knee reveal joint effusion, periarticular osteopenia, and erosions. An arthrocentesis reveals cloudy fluid with jWBC 5,000 cells/mm3. The Gram stain is negative, and the cultures are pending. There are no crystals on microscopy.
Rheumatoid Arthritis (RA)
Epidemiology. RA is the most common inflammatory arthritis,26 affecting approximately 1% of the general population.11,26 There is a four-fold increase in the incidence in those older than age 50, and it is 2-3 times more common in women.12 RA is associated with high levels of morbidity and shortened life span.26,49 Those afflicted are at greater risk for cardiovascular diseases, infection, cancer and lymphoproliferative malignancies, and renal disease.49 There has been a strong association between septic arthritis and RA. Septic arthritis can precede rheumatoid arthritis; however, it is unclear whether there is a causal relationship.26
Pathophysiology. RA is primarily an inflammation of the synovium. A proliferation of synovial cells leads to increased growth of the surrounding vasculature, causing increased tissue volume and edema. The inflammatory process produces cytokines and proteases that ultimately destroy the joint.
Clinical Presentation. RA is a systemic disease. Patients often present with fever, weight loss, or fatigue.50 They may have complaints of joint pain or swelling in multiple joints, which have been present for weeks or months. Swelling and pain are almost always symmetric. If they are not, consider alternative diagnoses such as gout or septic arthritis.11
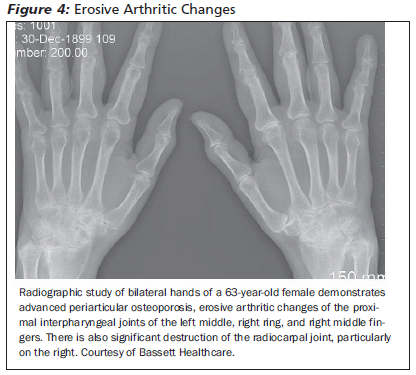
Diagnostic Tests. The diagnosis of RA is based on clinical findings, radiologic findings, and laboratory tests. Patients must meet four out of the six criteria outlined by the American College of Rheumatology in Table 6. Laboratory tests are not useful for diagnosing RA in the emergency department. Rheumatoid factor is not specific and may be positive in septic arthritis, lupus, Sjögren's syndrome, and even in normal patients.25,51 Radiographs typically show periarticular osteopenia in the hands or wrists. Over time, periarticular bony erosions and symmetrical joint space narrowing develop.50 Arthrocentesis is performed when patients present with pain out of proportion to their typical exacerbations.25 Synovial fluid aspirated from rheumatic joints typically is translucent and the jWBC is between 2,000 and 10,000 cells/mm3 with > 50% PMNs.20 The fluid should not contain crystals and bacteria.20
 |
Treatment. The goal of treating an RA flare is to reduce pain, prevent progression of disease, and maintain joint function. Non-selective NSAIDs and COX-2 inhibitors are useful for their anti-inflammatory and analgesic effects.52 The use of COX-2 inhibitors can reduce GI bleeding but must be balanced against the increasing risk of cardiovascular events.32
Joint aspiration is an effective way to immediately reduce pain and improve joint function. Intra-articular corticosteroid injection can improve symptoms within 24 hours and may provide benefit for more than 2 months.4 Cortisol should not be injected into any joint when there is a suspicion of septic arthritis. If adequate pain relief is accomplished, the patient can be discharged and referred to his or her rheumatologist. Chronic treatment with methotrexate, sulfasalazine, hydroxychloroquine, and/or anticytokine medications such as infliximab, etanercept, and anakira can be effective but require close evaluation.11
Case 3 Revisited. The patient has immediate improvement of pain after joint aspiration. The patient's pain is controlled with NSAIDs, and she is discharged to follow up with her rheumatologist.
Summary
Acute joint pain has many causes. Septic arthritis should be considered in all patients with acute joint pain. Arthrocentesis should be performed whenever septic arthritis is a concern. Early diagnosis and management is important in all forms of acute arthritis to slow the progression of disease and preserve joint function.
References
1. Shah K, Spear J, Nathanson LA, et al. Does the presence of crystal arthritis rule out septic arthritis? J Emerg Med 2007;32: 23-26.
2. Goldring SR, Goldring MB. Biology of the normal joint. In: Firestein GS, et al. Kelley's Textbook of Rheumatology, 8th edition. Saunders; September 16, 2008: chapter 1.
3. West SG. Anatomy and physiology of the musculoskeletal system. In: West SG. Rheumatology Secrets, second edition. Hanley & Belfus, Inc., Philadelphia; 2002: chapter 3, 8-10.
4. Courtney P, Doherty M. Joint aspiration and injection and synovial fluid analysis. Best Practice & Research Clinical Rheumatology 2009;23:161-192.
5. Constantino TG, Roemer B, Leber EH. Septic arthritis and bursitis: Emergency ultrasound can facilitate diagnosis. J Emerg Med 2007;32:295-297.
6. Punzi L, Oliviero F. Arthrocentesis and synovial fluid analysis in clinical practice: Value of sonography in difficult cases. MRI and ultrasound in diagnosis and management. Ann NY Acad Sci 2009;1154: 152-158.
7. Tsung JW, Blalvas M. Emergency department diagnosis of pediatric hip effusion and guided arthrocentesis using point-of care altrasound. J Emerg Med 2008;35:393-399.
8. Shavit I, Eidelman M, Galbraith R. Sonography of the hip joint by the emergency ultrasound physician. Its role in the evaluation of children presenting with acute limp. Pediatr Emerg Care 2006;22: 570-573.
9. Wiler JL, Costantino TG, Filippone L, et al. Comparison of ultrasound-guided and landmark techniques for knee arthrocentesis. J Emerg Med 2008, Dec. 4 [Epub ahead of print].
10. Lin HM, Learch TJ, White EA, et al. Emergency joint aspiration: A guide for radiologists on call. Radiographics 2009;29:1140-1158.
11. Harrington L, Schneider JI. Atraumatic joint and limb pain in the elderly. Emerg Med Clin North Am 2006;24:389-412.
12. EL-Gabalawy HS. Synovial fluid analyses, synovial biopsy and synovial pathology. In: Firestein GS, et al. Kelley's Textbook of Rheumatology, 8th edition. Saunders; September 16, 2008: chapter 48.
13. Ma L, Cranney A, Holroyd-Leduc JM. Acute monarthritis: What is the cause of my patient's painful swollen joint? CMAJ 2009;180:59-65.
14. Favero M, Schiavon, F, Riato, L, et al. Rheumatoid arthritis is the major risk factor for septic arthritis in rheumatological settings. Autoimmunity Reviews 2008;8: 59-61.
15. Rios CL, Zehtabchi S. Septic arthritis in emergency department patients with joint pain. Searching for the optimal diagnostic tool. Ann Emerg Med 2008;52:567-569.
16. Margaretten ME, Kohlwes J, Moore D, et al. Does this adult patient have septic arthritis? JAMA 2007;297:1478-1488.
17. Li SF, Henderson J, Dickman E, et al. Laboratory in adults with monarticular arthritis: Can they rule out septic joint? Acad Emerg Med 2004;11:276-280.
18. Gupta MN, Sturrock RD, Field M. Prospective comparative study of patients with culture proven and high suspicion of adult onset septic arthritis. Ann Rheum Dis 2003;62:327-331.
19. Garcia De La Torre I, Nava-Zavala A, Gonococcal and nongonococcal arthritis. Rheum Dis Clin North Am 2009;35:63-73.
20. Kherani RB, Shojania K. Septic arthritis in patients with pre-existing inflammatory disease. CMAJ 2007;176:1606-1608.
21. George HO. Infectious Disorders, A. Septic arthritis. In: Klippel JH, et al. Primer on the Rheumatic Diseases, 13th edition, Springer; 2008:271-276.
22. Coakley G, Mathews C, Field M, et al. BSR & BHPR, BOA, RCGP and BSAC Guidelines for the Management of the hot swollen joint in adults. Rheumatology 2006:45:1039-1041.
23. Frazee BW, Fee C, Lambert L. How common is MRSA in adult septic arthritis? Ann Emerg Med 2009;54:695-700.
24. Mathews CJ, Coakley G. Septic arthritis: Current diagnostic and therapeutic algorithm. Curr Opin Rheumatol 2008;20: 457-462.
25. Mathews CJ, Kngsley G, Field M, et al. Management of septic arthritis: A systematic review. Ann Rheum Dis 2007;66; 440-445.
26. Edward CJ, Cooper C, Fisher D, et al. Importance of the disease process and disease modifying antirheumatic drug therapy in patients with rheumatoid arthritis. Arth Rheum 2007;57:1151-1157.
27. Visser S, Tupper J. Septic until proven otherwise: Approach to and treatment of the septic joint in adult patients. Can Family Physician 2009;55:374-375.
28. George HO, Siraj DS, Cook PP. Bacterial arthritis. In: Firestein GS et al. Kelley's Textbook of Rheumatology, 8th edition. Saunders; September 16, 2008: chapter 99.
29. Golbus J. Monoarticular arthritis. In Firestein GS, et al. Kelley's Textbook of Rheumatology, 8th edition, Saunders; September 16, 2008: chapter 36.
30. Boyd R, Martin B. Erythrocyte sedimentation rate and septic arthritis in children. Emerg Med J 2001;18:212-213.
31. Gilliland WR. Bacterial septic arthritis. In: West SG. Rheumatology Secrets, second edition, Hanley & Belfus, Inc., Philadelphia; 2002: 281-289.
32. Croom KF, Siddiqui MA. Etoricoxib: A review of its use in the symptomatic treatment of osteoarthritis, rheumatoid arthritis, ankylosing spondylitis and acute gouty arthritis. Drugs 2009;69:1513-1532.
33. Kopterides P. Synovial lactic acid and septic arthritis. JAMA 2007;298:40.
34. Margaretten ME, et al. In Reply: Synovial lactic acid and septic arthritis. JAMA 2007;298:40.
35. Garcia-De La Torre I. Advances in the management of septic arthritis. Infec Dis Clin North Am 2006;20:773-788.
36. McGillicuddy DC, Shah KH, Friedberg RP, et al. How sensitive is the synovial fluid white blood cell count in diagnosing septic arthritis? Am J Emerg Med 2007;25; 749-752.
37. Li SF, Cassidy C, Chang C, et al. Diagnostic utility of laboratory tests in septic arthritis. Emerg Med J 2007;24:75-77.
38. Gerlag DM, Tak PP. Synovial fluid analyses, synovial biopsy, and synovial pathology. In: Harris ED et al. Kelley's Textbook of Rheumatology, 7th edition, Saunders; 2005: chapter 46.
39. Monu JU, Pepe TL. Gout: A clinical and radiologic review. Radiol Clin North Am 2004;42:169-184.
40. Terkeltaub RA. Gout, C. Treatment. In: Klippel JH, et al. Primer on the Rheumatic Diseases, 13th edition, Springer; 2008: 258-262.
41. Terkeltaub RA. Clinical practice: Gout. N Eng J Med 2003;349:1647-1655.
42. Schlesinger N. Overview of the management of acute gout and the role of adrenocorticotropic hormone. Drug 2008;68: 407-415.
43. Choy, G. An update on the treatment options for gout and calcium pyrophosphate deposition. Expert Op Pharmacother 2005;6:2443-2453.
44. Wortmann RL. Gout and hyperuricemia. In: Firestein GS et al. Kelley's Textbook of Rheumatology, 8th edition, Saunders; September 16, 2008: chapter 87.
45. Bellamy N, Campbell J, Welch V, et al. Intraarticular corticosteroid for treatment of osteoarthritis of the knee. Cochrane Review 2009 Issue 3.
46. Schlesinger N, Schumacher R, Catton M, et al. Colchicine for acute gout. Cochrane Review 2006; Issue 4.
47. McCarthy G. Calcium pyrophosphate dihydrate, hydroxyapatite, and miscellaneous crystals. In: Klippel JH, et al. Primer on the Rheumatic Diseases, 13th edition, Springer; 2008: 263-270.
48. Terkeltaub R. Diseases associated with articular deposition of calcium pyrophosphate dihydrate and basic calcium phosphate crystals. In: Firestein GS et al. Kelley's Textbook of Rheumatology, 8th edition. Saunders; 2008: chapter 88.
49. Elliott JR, O'Dell J. Rheumatoid arthritis. In: West SG. Rheumatology Secrets, second edition. Philadelphia: Hanley & Belfus; 2002:117-127.
50. Tehlirian CV, Bathon JM. Rheumatoid arthritis. A. Clinical and laboratory manifestations. In: Klippel JH, et al. Primer on the Rheumatic Diseases, 13th edition. Springer; 2008:114-121.
51. Waldburger JM, Firestein GS. Rheumatoid arthritis. B. Epidemiology, pathology, and pathogenesis. In: Klippel JH, et al. Primer on the Rheumatic Diseases, 13th edition. Springer; 2008:122-132.
52. Oliver AM, ST Clair EW. Rheumatoid arthritis. C. Treatment and assessment. In: Klippel JH, et al. Primer on the Rheumatic Diseases, 13th edition. Springer; 2008:133-141.
Patients with acute joint pain present a diagnostic dilemma for many emergency physicians. Classically the joints are hot, swollen, and tender, with reduced range of motion. The differential diagnosis for the painful joint is extensive.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
