Acute Abdominal Pain in Special Populations, Part I: Pediatric Patients
Part I: Pediatric Patients
Authors: Larissa I. Velez, MD, Assistant Professor, Assistant Director of Emergency Medicine Residency Program, University of Texas Southwestern Medical Center, Dallas; Fernando L. Benitez, MD, Assistant Professor, Emergency Medicine, University of Texas Southwestern Medical Center, Dallas; and Salvador E. Villanueva, MD, Assistant Professor, Emergency Medicine, University of Puerto Rico.
Peer Reviewers: J. Stephan Stapczynski, MD, Chair, Emergency Medicine Department, Maricopa Medical Center, Phoenix, AZ; and O. John Ma, MD, Professor and Vice Chair of Emergency Medicine, Truman Medical Center, University of Missouri—Kansas City School of Medicine.
Acute abdominal pain, defined in this article as any non-traumatic cause of abdominal pain of less than one week duration, can be one of the most challenging complaints in the emergency department (ED).1 It is estimated that 5-10% of ED visits are due to abdominal pain.2,3 The final etiologic diagnoses range from a simple problem to a complicated, life-threatening disease. Even with our current diagnostic abilities, up to 40% of the patients are discharged from the EDs with a diagnosis of "undifferentiated abdominal pain."4
When evaluating a patient with acute abdominal pain, obtain a pertinent history (duration, character, severity, and radiation of the pain, associated symptoms) and perform a thorough, yet focused, physical examination. Keep in mind the common diagnoses for each patient population and patterns of pain that are typical for some diagnoses. Finally, judiciously use laboratory and radiologic studies to exclude or confirm the presence of life-threatening conditions.
While the diagnosis of abdominal pain of uncertain etiology is an acceptable discharge diagnosis, care must be taken to ensure adequate follow up of these patients. Appropriate discharge instructions always must be provided, and follow up should be arranged.3 All of these precautions will ensure that the patient understands and is satisfied with ED care.
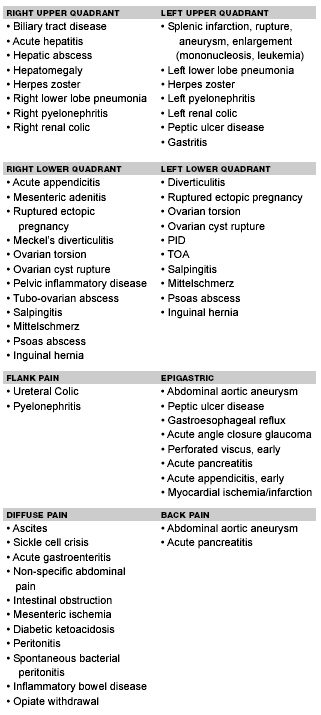
A comprehensive review of abdominal pain is beyond the scope of this discussion. Table 1 lists some of the most common causes of acute abdominal pain. This article instead will focus on specific populations presenting with abdominal pain to the ED and their specific or unique diagnoses. The pediatric, elderly, pregnant, and immunocompromised patients are special populations that pose a particular challenge to clinicians. These high-risk groups often present atypically, and serious conditions can be missed or misdiagnosed. Finally, this article will discuss unusual diagnoses that often present with abdominal pain as one of the main symptoms.
Part I of this article will discuss pediatric patients, and part II will cover elderly, pregnant and immunocompromised patients.—The Editor
Table 1.
Common Causes of Acute Abdominal Pain
Special Populations
This article will discuss abdominal pain in four special populations: pediatric patients, the elderly, the pregnant, and the immunocompromised. Each of these segments of the population has unique problems and very often has atypical and/or delayed presentations. Knowing the particularities helps focus the diagnostic workup and helps establish an accurate diagnosis. This segment will focus on pediatric patients.
Pediatric Patients
It is estimated that 10% of children in the ED have an abdominal complaint.5 Still, missed diagnoses remain frequent in emergency medicine. Causes for these missed diagnoses include the child’s inability to provide a good history, including the characterization of the pain. Pain localization also is poor in children.6,7 The clinical signs of an abdominal emergency in pediatric patients include vomiting, abdominal pain, and fever.6 Children may present with systemic and non-specific symptoms such as lethargy, poor feeding, weight loss, irritability, or malaise.5 Signs and symptoms also are age-dependent, with the younger patients having the more atypical presentations.
The diagnostic etiologies are divided broadly by age (neonate, infant/toddler, and older children). Besides age, an attempt should be made to determine if the abdominal complaint is an acute or chronic problem, as chronic problems rarely are life-threatening.
When evaluating a pediatric patient, perform a systematic physical examination and leave the abdomen for last. This will help with the initial apprehension the patient has and also will allow for a more thorough examination before eliciting pain and possibly losing the patient’s cooperation. When examining the abdomen, start with the least tender areas first and finish with the most tender area. Try to engage the child in distracting conversation while performing the examination and move slowly and non-threateningly.
Necrotizing Enterocolitis (NEC). NEC is the most common gastrointestinal (GI) emergency in the neonatal period.8 It is an acute fulminant disease associated with focal and/or diffuse ulceration and necrosis of the distal small intestine and the colon.9 Prematurity is the most important risk factor. NEC is a disease of neonates, having its usual onset in fewer than five days of life; however, it can present up to four weeks after birth.
Patients present with diffuse abdominal pain, abdominal distention, lethargy, vomiting, and GI bleeding. Peritonitis with acidosis, sepsis, and shock can occur rapidly.9
Plain abdominal films initially can show an asymmetric pattern of bowel gas with varying degrees of dilatation.10 Later, the plain films will demonstrate pneumatosis intestinalis (air in bowel wall) in 70-80% of cases.9 This is a specific finding in NEC.7 Air also can be seen in the stomach wall (pneumatosis gastralis) and in the portal system.
The management includes aggressive supportive management, fluid resuscitation, gastric decompression, and emergent surgical consultation. Extensive resection of non-viable bowel may be necessary, resulting in short bowel syndrome in survivors. Antibiotics (ticarcillin [Ticar] and gentamicin [Garamycin], or a third-generation cephalosporin) are used for ill-appearing infants.
A pitfall with this condition is failure to consider NEC as a diagnosis outside the neonatal intensive care unit.
Volvulus. In embryonic development, the gut rotates around the superior mesenteric artery and then becomes attached to the retroperitoneum at several points (i.e., duodenum and cecum). If malrotation occurs, the duodenum and cecum remain in close proximity, and the structures can rotate around their vascular supply, resulting in what is called volvulus. Malrotation of the gut thus can predispose patients to volvulus.7 Volvulus will develop in about 75% of the patients with malrotation. Typically, about 90% of the cases occur in the first year of life, with the majority of cases presenting in the first month of life. The volvulus can be partial or incomplete, thus giving intermittent symptoms. A complete volvulus can result in bowel necrosis after 1-2 hours. The patients present with bilious vomiting and abdominal distention. They will be acutely ill-appearing and can present in shock. Plain films may suggest diagnosis, showing air-fluid levels and a "double bubble" sign and absence of bowel gas distal to the volvulus. The upper gastrointestinal series (UGIS) is considered the most useful study. It will show the typical corkscrew appearance.5
Management includes fluid resuscitation, stomach decompression with a nasogastric tube, and emergent surgical consultation. Antibiotics (ampicillin [Omnipen, Polycillin, Principen], gentamicin, and clindamycin [Cleocin] or metronidazole [Flagyl, Trikacide, Florazole-ER) are used for ill-appearing infants.
Physicians should remember that volvulus is associated with malrotation.
Hypertrophic Pyloric Stenosis (HPS). This is the most common cause of infantile GI obstruction. It occurs in about 1 of every 250 live births and is most common in first-born males between 4-8 weeks of age.7,11 The infants have progressive gastric outlet obstruction from the hypertrophied pyloric muscle. Patients present with non-bilious projectile vomiting and failure to thrive. Despite this, they exhibit hunger and a vigorous sucking reflex. As the vomiting progresses, the patients develop dehydration and a hypochloremic, hypokalemic metabolic alkalosis. In some cases, an "olive," representing the hypertrophied pylorus, can be palpated in the right upper abdomen or epigastrium.5 The olive is considered a pathognomonic finding in HPS.7 Peristaltic waves also can be seen in HPS, often preceding the vomiting episodes.
Currently, the diagnosis often is made early by ultrasound (US) before classic physical examination findings or laboratory findings become evident. US has a diagnostic accuracy of about 95%. A pyloric muscle width of 2.5-3 mm is considered normal.12 The sonographic criteria for HPS are a pyloric muscle thickness greater than 3 mm (the most widely used criterion), a pyloric channel length greater than 17 mm, and a pyloric muscle length greater than 19 mm.13 A barium (upper GI series) study will show the characteristic string sign.12
The management of HPS is aimed at correcting the dehydration, hypokalemia, and acid-base problems, and surgical consultation for pyloromyotomy.
The early diagnosis of HPS can be best confirmed with US showing a pyloric muscle thickness of greater than 3 mm.
Intussusception. Intussusception occurs when a segment of bowel invaginates into another segment, causing obstruction. Subsequent bowel edema leads to ischemia. It is the most common cause of intestinal obstruction in those younger than 2 years.5 The age range of presentation for intussusception is 6-18 months. The condition is more common in males and in the warmer months.14 Most often, intussusception presumably is due to inflamed Peyer’s patches, but in 2-8% a recognizable lead point can be identified, such as a Meckel’s diverticulum, duplication cyst, intestinal polyps, or lymphoma.6 Adenovirus and rotavirus can be preceding illnesses.5 In fact, the rotavirus vaccine was withdrawn from the market because of its association with intussusception.
Most commonly, the intussusception is ileocolic; however, ileoileal or other forms are possible. Patients present with episodic crying, irritability, and pulling of the legs up to the abdomen. Patients may appear well between episodes; however, some patients present only with lethargy and prostration.5 The classic presentation (i.e., abdominal pain, vomiting, and bloody stools) is seen in only 10-33% of cases.5,6 Currant jelly stools are a late finding and represent bowel ischemia. The classic physical examination finding is called Dance’s sign: a sausage-like mass in the right upper quadrant and an empty space in the right lower quadrant representing the displaced cecum.
Plain films are unreliable and are sometimes normal. A soft-tissue mass in the right upper quadrant and an abrupt cut-off of colonic air are suggestive of intussusception. Dilated loops of small bowel with air-fluid levels proximal to the obstruction may be present. US is very accurate and reliable, having a 98-100% sensitivity, 90-100% specificity, and 100% negative predictive value for diagnosing intussusception.15-17 The US will visualize a target or donut sign in transverse section and sandwich or pseudokidney sign in longitudinal section. The US also can confirm the completeness of the reduction. The US may be helpful in screening for patients who will require a barium enema, but most pediatric centers proceed straight to the barium enema if intussusception is suspected, because it can be both diagnostic and therapeutic in reducing the intussusception.
Non-operative reduction is best. Most cases of intussusception can be reduced using an enema of barium, air, or saline.14 The barium enema still is the gold standard, and can be both diagnostic and therapeutic in 45-85% of cases. Surgical reduction must be performed if reduction fails or if there is perforation or peritonitis.14
Treatment strategies include volume resuscitation, emergent surgical consultation, and gastric decompression. Antibiotics should be used for ill-appearing patients. Ampicillin, gentamicin, and clindamycin or metronidazole are the usual choices. Most centers will admit all patients after a successful reduction and observe those for re-intussusception.
Remember that intussusception is the most common cause of intestinal obstruction in those younger than 2 years. Suspect intussusception instead of colic if the child is older than 4 months and presents with episodic abdominal pain.
Hernias. Inguinal hernias occur in about 10-20 per 1000 live births.5 Prematurity and low birth weight increase the risk.7 Most hernias are unilateral and are more common on the right side. The male to female ratio is 4:1, but females incarcerate more often.5 Incarceration is the primary complication of inguinal hernias, and it occurs more commonly in children than in adults. This explains the fact that inguinal hernias are the most common indication for surgery in those younger than 2 years.
Patients with incarceration present with abdominal or inguinal pain, an inguinal or scrotal mass, nausea, vomiting, and occasionally low grade fever.
Attempt reduction if the child appears well. This is accomplished by using analgesia, sedation, and placing the patient in a Trendelenburg position.7 Slow gentle pressure should be applied to the hernia. If the hernia is reduced easily, outpatient surgical referral must be arranged. However, do not reduce if the patient is ill or toxic-appearing. In these cases where incarceration or strangulation is suspected, give fluid resuscitation, antibiotics, and immediately consult the surgeon.
Physicians should not attempt manual reduction in those cases where a strangulated hernia is suspected.
Appendicitis. Acute appendicitis is the most common non-traumatic surgical emergency in children, having an estimated incidence of 4 out of every 1000 children.7 Its occurrence is rare in those younger than 3 years, but it still can occur.5,6 The peak ages for acute appendicitis are between ages 6 and 14 years. A good rule is that there are more atypical presentations in younger patients.
Abdominal pain, especially in the right lower quadrant, fever, vomiting, and anorexia are good indicators of appendicitis in children. Patients can have diarrhea due to sigmoid colon irritation. If the appendix is retrocecal, they may have only flank pain and dysuria.5 Probably due to the atypical presentations, appendicitis is still a commonly missed diagnosis for this age group.
Another complication of atypical presentations is the high rate of perforation seen in children. One author reports that 79% of the perforations occur in those younger than 3 years.18 Pediatric patients also progress to gangrene and perforation faster.5,19 After perforation, younger patients also do not wall off the perforation as well.7 This leads to diffuse peritonitis and sepsis.
The complete blood count (CBC) and urinalysis (U/A) rarely help in making the diagnosis. Leukocytosis is common, but not specific, for appendicitis. Pyuria without bacteriuria often is seen as a result of an inflamed appendix in close proximity to the ureters.7
Imaging is most useful in those with an uncertain clinical diagnosis. A fecalith can be seen in 10% of the cases, but the plain films often are normal or non-specific. US is an excellent imaging test in children. Benefits of US in pediatric patients include non-invasiveness, avoidance of procedural sedation, and availability.7 However, US may be technically difficult in obese patients and may require calling in a technician from home at night. Furthermore, the US is both operator- and interpreter-dependent. Criteria used for diagnosing appendicitis with US include a non-compressible appendix greater than 6 mm in diameter.7 The US also can visualize an appendicolith, peri-appendiceal fluid collections, and abscesses.20 The US has sensitivity and specificity in the range of 90-95% for the diagnosis of acute appendicitis.
Computerized tomography (CT) scan is at least as useful in children as in adults. An appendiceal CT scan has a sensitivity and specificity in the range of 95-100%.21,22 The CT scan is best at looking for complications of appendicitis and for ruling out other commonly mistaken diagnoses, such as mesenteric adenitis and inflammatory bowel disease.6 The CT scan is the imaging modality of choice for diagnosing acute appendicitis in many institutions. Use of intravenous (IV), oral, or rectal contrast is institution-specific.7
The management involves keeping the patient on an empty stomach and obtaining a surgical consultation. Antibiotics should be used if there are signs of perforation or abscess formation.
Physicians should remember to appreciate the fast rate of perforation and higher likelihood of peritonitis in this population.
Physicians should take care not to exclude appendicitis because of pyuria, which can be due to an inflamed appendix in close proximity to the ureter.
Mesenteric Adenitis. Mesenteric adenitis is a common diagnosis in pediatric patients with acute abdominal pain. It is easily confused with appendicitis. US has become a good diagnostic modality that is helpful in distinguishing between these two diagnoses. The US criteria for mesenteric adenitis include nodes greater than 10 mm in longitudinal diameter and increased in number.6 The CT scan also is helpful in excluding acute appendicitis as the cause of the right lower quadrant pain.21 The management is conservative, as it is a self-limited illness.
Physicians should remember to consider mesenteric adenitis in the differential diagnosis of pediatric patients with unclear right lower quadrant pain.
Acute Gastroenteritis (AGE). AGE can cause significant, diffuse abdominal pain in children. Usually, the diagnosis can be established by the presence of fever, vomiting, diarrhea, and mild intermittent crampy abdominal pain. However, AGE always should be considered a diagnosis of exclusion. Plain radiographs can show multiple distended loops and air-fluid levels. The US may show free fluid between loops, but radiology mainly is used to exclude other diagnoses.6
The treatment of AGE is supportive, with adequate fluid replacement and correction of electrolyte disturbances. Physicians should remember to regard AGE as a diagnosis of exclusion.
Hemolytic-Uremic Syndrome (HUS). HUS is one of the most common causes of acute renal failure in children.23 The condition is rare in those older than 5 years of age. The most common cause of HUS is the verotoxin (also known as shiga-like toxin) produced by E. coli 0157:H7. The renal vascular endothelium is damaged, resulting in hemolysis and decreased renal function.
The patients present with abdominal pain, diarrhea, and, occasionally, fever. The stools can be bloody. The condition progresses to hemolytic anemia, renal insufficiency, and thrombocytopenia. Up to 40% of the patients develop seizures, and some develop encephalopathy.
The CBC will demonstrate anemia and thrombocytopenia. Hemolysis also can be demonstrated by an increased indirect bilirubinemia, elevated lactate dehydrogenase (LDH), and hemoglobinuria. Azotemia and hyperkalemia can be seen with renal failure.
The management mainly is supportive, and may include hemodialysis. Plasmapheresis is used in some cases, especially if there is neurologic involvement. Renal transplantation may be required for those who develop permanent renal failure.
The cause for HUS is verotoxin, or shiga-like toxin, produced by E. coli 0157:H7.
Henoch-Schonlein Purpura (HSP). This is a systemic vasculitis associated with abdominal pain, joint pain, occasional renal involvement, and a purpuric rash. It is most common between the ages of 4 and 11 years. The diagnosis usually is clinical, made by the presence of a palpable purpuric rash in the buttocks and lower extremities, abdominal pain with nausea, vomiting and diarrhea, microscopic hematuria, and arthralgias. Many patients will have occult heme-positive stools. The abdominal pain typically is diffuse, intermittent, and colicky in nature, caused by edema and vasculitis of the intestines.
Intussusception occurs in HSP and should be sought in patients with severe abdominal pain, distention, or bilious vomiting.
Most patients can be managed as outpatients once life-threatening conditions have been excluded. Steroids are advocated by some for the more severe cases.
Remember that HSP presents with palpable purpura, abdominal pain, joint pain, and renal involvement. There is an association with intussusception.
Hirschsprung’s Disease (Congenital Aganglionic Megacolon). This is caused by a congenital absence of ganglion cells beginning at the internal anal sphincter and extending proximally to involve a variable length of intestine. The areas affected cannot relax, causing a functional colonic obstruction. Stool accumulates proximally, resulting in massive colonic dilatation.
Patients present with chronic constipation, obstipation, and failure to thrive.6 Hirschprung’s disease presents most often during infancy. Symptoms usually are present since birth, which helps differentiate this condition from functional constipation. Complications may arise, and patients may be ill appearing due to a toxic megacolon and enterocolitis.
Plain films can show air fluid levels, a dilated colon, and fecal impaction. The barium enema will show a narrow distal colon segment and proximal dilatation. This finding is highly suggestive of Hirschsprung’s disease, but the diagnosis must be confirmed by biopsy and rectal manometry.24
Management strategies include supportive management, colonic emptying with enemas or polyethylene glycol and aggressive evaluation and surgical consultation for complications. The definitive management is surgical resection of the aganglionic segment.
Remember to consider Hirschsprung’s disease in any case of constipation since birth.
Meckel’s Diverticulum. Meckel’s diverticulum is the most common congenital malformation of the small intestine. It follows the rule of twos:
- 2% of the population have them;
- there is a 2:1 male to female ratio;
- there are two types of tissue, gastric and pancreatic;
- they generally are located within two feet of the ileo-cecal junction;
- they are two inches long; and
- they become symptomatic in 2% of those who have it.5 Meckel’s diverticula can bleed or, less commonly, perforate.7
The classic presentation is in a pediatric patient younger than 5 years of age with massive painless rectal bleeding, with 50% of patients with the condition presenting by age 2. The bleeding is described as brick red. Many patients, however, complain of crampy abdominal pain. Rarely, inflammation and infection of the Meckel’s diverticulum (diverticulitis) can occur, mimicking appendicitis, and progressing to perforation and peritonitis.
The imaging modality of choice is a nuclear Technetium-pertechnetate scan, also called a Meckel’s scan.5,7 The CT scan is useful for identifying complications from a Meckel’s, such as intussusception and diverticulitis.25,26 Management includes fluid resuscitation, basic laboratories (i.e., CBC, platelets, prothrombin time [PT], partial thromboplastin time [PTT], international normalized ratio [INR]), blood product administration as needed, and evaluation for complications such as obstruction or perforation. Surgical consultation is indicated for resection of the Meckel’s diverticulum.
Other Conditions. Inflammatory bowel disease (IBD) often does not present until adolescence. Ulcerative colitis (UC) is a chronic mucosal inflammation of the colon. Patients present with bloody diarrhea, fecal urgency, crampy abdominal pain, tenesmus, fever, and a mucoid rectal discharge. Some have constipation. Peritonitis can be seen with toxic megacolon or fulminant colitis.27 Crohn’s disease is a transmural segmental inflammatory process of the GI tract. Since the whole width of the intestine is involved, fistula and abscess formation are common. Patients present with diarrhea, weight loss, and fever. Perforation can complicate Crohn’s disease. Patients with IBD often present to the ED with disease flares and complications from them. When IBD is suspected, consultation with a gastroenterologist is indicated. The consultation can occur as inpatient or outpatient, depending on the patient’s clinical condition.
Pancreatitis is uncommon in childhood. The most common causes for pediatric pancreatitis are trauma, infection, structural anomalies, systemic diseases, and drugs or toxins.28 The pediatric presentation of pancreatitis is similar to that of adults. The treatment is the same, with the exception that most children with pancreatitis will require admission.
Biliary tract disease also is uncommon in childhood and has dissimilar precipitating causes in younger children (hemolysis, sepsis, cystic fibrosis, Rocky Mountain Spotted Fever, and Kawasaki disease, among others).29,30 The clinical presentation of right upper quadrant pain is similar to that of adults, especially with older children and adolescents. Management is similar to that of adults and includes addressing the underlying problem.
Ovarian torsion is more common on the right side and thus can be confused with acute appendicitis. Other ovarian pathology, such as follicular and luteal cysts and ovarian tumors, must be considered in the diagnosis of lower abdominal pain. The US is useful in distinguishing these conditions.7 Although uncommon, testicular torsion can present with abdominal pain. Testicular necrosis has been reported after 4-6 hours of ischemia, so rapid diagnosis and management is imperative. The US will confirm the diagnosis, but emergent urological consultation must be obtained first if the diagnosis is suspected by physical examination.7
In adolescence, gynecological and obstetrical problems must be added to the list of differential diagnoses. Pelvic inflammatory disease, tubo-ovarian abscesses, ectopic pregnancy, and problems such as Fitz-Hugh-Curtis syndrome need to be considered.
Hydrometrocolpos occurs due to an imperforate hymen or cervical or vaginal atresia. Once menarche starts, the menstrual products accumulate proximally. The patient typically complains of lower abdominal pain that may recur monthly, and a pelvic mass may be palpable, representing the blood-filled uterus. Urinary retention or constipation may be other presenting complaints. The condition generally is suspected when pubertal changes occur without menstrual bleeding. Imperforate hymen is diagnosed on physical examination when a bulging, intact membrane occludes the vaginal introitus. Hydrometrocolpos also can be diagnosed by US.6
Caustic ingestions also can present with epigastric or diffuse abdominal pain and can occur in the absence of a history of an ingestion. Children ingest caustic substances due to their exploratory nature. One important concept to remember is that oral burns are not predictive of more distal gastrointestinal burns. All patients with symptoms (i.e., vomiting, drooling, abdominal pain) after a caustic ingestion must undergo an endoscopic evaluation prior to discharge.
Pyelonephritis and renal colic may present with abdominal, not flank, pain in pediatric patients. Diagnostic procedures include plain films, US, or CT scan.6 The treatment is similar to that for adults, with hydration, analgesia, and antibiotics for those with an infection.
Non-abdominal Causes of Abdominal Pain. There are many causes of abdominal pain that are not due to an intra-abdominal pathology or are more systemic in nature. Although the causes are numerous, some of the most important to remember are: black widow spider bite, scorpion bite, lead poisoning, leukemia, sickle cell pain crisis, diabetic ketoacidosis,31 Streptococcal pharyngitis, lower lobe pneumonia, intestinal parasites, intestinal foreign bodies, cystic fibrosis, and familial Mediterranean fever.5,9,31
Acknowledgements: The authors would like to acknowledge the assistance of Collin Goto, MD, and Patricia Santiago-Muñoz, MD, in the preparation of this manuscript.
References
1. Clinical policy: Critical issues for the initial evaluation and management of patients presenting with a chief complaint of nontraumatic acute abdominal pain. Ann Emerg Med 2000;36:406-415.
2. Clinical policy for the initial approach to patients presenting with a chief complaint of nontraumatic acute abdominal pain. American College of Emergency Physicians. Ann Emerg Med 1994;23: 906-922.
3. Kamin RA, Norwicki TA, Courtney DS, et al. Pearls and pitfalls in the emergency department evaluation of abdominal pain. Emerg Med Clin North Am 2003;21:61-72, vi.
4. King, KE and Wightman JM. Abdominal pain. In Marx KA, et al, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. St. Louis: Mosby; 2002:185-194.
5. Pollack ES. Pediatric abdominal surgical emergencies. Pediatr Ann 1996;25:448-457.
6. Carty HM. Paediatric emergencies: Non-traumatic abdominal emergencies. Eur Radiol 2002;12:2835-2848.
7. McCollough M, Sharieff GQ. Abdominal surgical emergencies in infants and young children. Emerg Med Clin North Am 2003;21: 909-935.
8. Neu J, Weiss MD. Necrotizing enterocolitis: Pathophysiology and prevention. JPEN J Parenter Enteral Nutr 1999;23(5 Suppl):S13-7.
9. Roy CC, Morin CL, Weber AM. Gastrointestinal emergency problems in paediatric practice. Clin Gastroenterol 1981;10:225-254.
10. Buonomo C. The radiology of necrotizing enterocolitis. Radiol Clin North Am 1999;37:1187-1198, vii.
11. Rasmussen LA, Green, Hansen LP. The epidemiology of infantile hypertrophic pyloric stenosis in a Danish population, 1950-84. Int J Epidemiol 1989;18:413-417.
12. Kovalivker M, Erez I, Shneider N, et al. The value of ultrasound in the diagnosis of congenital hypertrophic pyloric stenosis. Clin Pediatr (Phila) 1993;32:281-283.
13. Teele RL, Smith EH. Ultrasound in the diagnosis of idiopathic hypertrophic pyloric stenosis. N Engl J Med 1977;296:1149-1150.
14. Roeyen G, Jansen M, Hubens G, et al. Intussusception in infants: An emergency in diagnosis and treatment. Eur J Emerg Med 1999; 6:73-76.
15. Daneman A, Alton DJ. Intussusception. Issues and controversies related to diagnosis and reduction. Radiol Clin North Am 1996;34: 743-756.
16. Stanley A, Logan H, Bate TW, et al. Ultrasound in the diagnosis and exclusion of intussusception. Ir Med J 1997;90:64-65.
17. Verschelden P, Filiatrault D, Garel L, et al. Intussusception in children: Reliability of US in diagnosis—a prospective study. Radiology 1992;184:741-744.
18. Daehlin L. Acute appendicitis during the first three years of life. Acta Chir Scand 1982;148:291-294.
19. Brender JD, Marcuse EK, Koepsell TD, et al. Childhood appendicitis: Factors associated with perforation. Pediatrics 1985;76:301-306.
20. Kao SC, Smith WL, Abu-Yousef MM, et al. Acute appendicitis in children: Sonographic findings. AJR Am J Roentgenol 1989;153: 375-379.
21. Rao PM, Rhea JT, Novelline RA, et al. The computed tomography appearance of recurrent and chronic appendicitis. Am J Emerg Med 1998;16:26-33.
22. Garcia Pena BM, Mandl KD, Kraus SJ, et al. Ultrasonography and limited computed tomography in the diagnosis and management of appendicitis in children. JAMA 1999;282:1041-1046.
23. Flynn JT. Causes, management approaches, and outcome of acute renal failure in children. Curr Opin Pediatr 1998;10:184-189.
24. Franken EA, Jr., Smith WL, Frey EE, et al. Intestinal motility disorders of infants and children: Classification, clinical manifestations and roentgenology. Crit Rev Diagn Imaging 1987;27:203-236.
25. Bennett GL, BA Birnbaum, Balthazar EJ. CT of Meckel’s diverticulitis in 11 patients. AJR Am J Roentgenol 2004;182:625-629.
26. Rossi P, Gourtsoyiannis N, Bezzi M, et al. Meckel’s diverticulum: Imaging diagnosis. AJR Am J Roentgenol 1996;166:567-573.
27. Roy MA. Inflammatory bowel disease. Surg Clin North Am 1997; 77:1419-1431.
28. Mader TJ, McHugh TP. Acute pancreatitis in children. Pediatr Emerg Care 1992;8:157-161.
29. Odom FC, Oliver BB, Kline M, et al. Gallbladder disease in patients 20 years of age and under. South Med J 1976;69:1299-1300.
30. Debray D, Pariente D, Gauthier F, et al. Cholelithiasis in infancy: A study of 40 cases. J Pediatr 1993;122:385-391.
31. Valerio D. Acute diabetic abdomen in childhood. Lancet 1976; 1(7950):66-68.
This article focuses on specific populations presenting with abdominal pain to the ED and their specific or unique diagnoses. The pediatric, elderly, pregnant, and immunocompromised patients are special populations that pose a particular challenge to clinicians. These high-risk groups often present atypically, and serious conditions can be missed or misdiagnosed. This article discusses unusual diagnoses that often present with abdominal pain as one of the main symptoms.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
