Pediatric Thoracolumbar Spinal Injury: Frequently Hidden, but Not Harmless
Author: Jeffrey Proudfoot, DO, FACOEP, FACEP, Director of Pediatric Emergency Medicine, Maricopa Medical Center; Clinical Assistant Professor of Pediatrics, University of Arizona Health Sciences Center, Phoenix.
Peer Reviewer: George L. Foltin, MD, FAAP, FACEP, Associate Professor of Pediatrics, New York University School of Medicine, New York.
Although spinal injuries occur infrequently, a delay in the detection of thoracolumbar trauma may have devastating consequences for a child. The literature convincingly demonstrates that injuries to the thoracolumbar spine frequently go undetected and lead to substantial morbidity. It is critical that the emergency physican be familiar with injury patterns that may result in this type of injury. Early detection through a careful, thorough physical examination and the appropriate use of radiography significantly reduce a child’s risk for a poor outcome. The author presents an extensive review of the physiology, clinical detection, and management strategies for children with thoracolumbar injuries.— The Editor
Epidemiology
Pediatric spinal injuries are uncommon, constituting less than 2-4% of all childhood injuries; this accounts for the relative dearth of published research in this population.1,2 Thoracolumbar spinal injury (TLSI), accounts for up to 75% of all pediatric spine fractures.1-3 While the majority (80%) of thoracolumbar vertebral fractures do not have concomitant neurologic deficits, TLSI is a major source of functional disability in children who survive the initial injury.2-4 One-third to one-half of all patients with TLSI will experience a major complication in the course of their care.2
The major contributor to pediatric TLSI is high impact or rapid deceleration, blunt force injury from falls, or vehicular trauma. The automobile continues to be the principal, omnipresent environmental hazard causing lethal injury in children older than 1 year of age during the past decade. In 1999, 27,200 children younger than age 14 suffered injury in motor vehicle-related accidents, and children younger than 4 years accounted for one-third of all childhood motor vehicle deaths in 1998.5
Greater awareness of mechanism and injury patterns is a necessity, since thoracolumbar vertebral fracture without radiographic evidence of osseous disruption occurs more frequently in the immature pediatric spine. Estimates of spinal cord injury without radiographic abnormality (SCIWORA) in the thoracolumbar spine have ranged from 1-55% in a pediatric population with a mean age of 6 years.2,6-8 The average age of patients with osseous injury is 16 years. As many as 50% of children with TLSI commonly have concomitant traumatic injuries involving the head, abdomen, or chest, which serve as major distractors for both patients and emergency physicians. More than 15% of patients will have multiple levels of their spines involved.6 The incidence of TLSI with neurologic deficit also increases logarithmically with age.2,3 Diagnosis can be delayed as long as four days post-injury, and this results in poorer outcomes in children younger than 8 years of age.
Anatomic Differences
Intervertebral Discs. One of the major differences between the immature spine and an adult spine is the anatomic structure of the intervertebral discs of both the thoracic and lumbar spine. At birth, intervertebral discs make up roughly one-third of the spinal column height. Immature discs are composed of concentric lamellae layered to form a fibrous ring (annulus fibrosis), a central gelatinous nucleus pulposus, and two cartilaginous articular plates that do not extend to the margins of the disc. The nucleus pulposus of the developing spine is highly hydrophilic, making it an effective shock absorber. It occupies approximately 40% of the cross-sectional area of the disc. The cartilaginous end plates are in direct contact with the trabecula of the vertebral body, allowing for the transfer of nutrients and fluid to the intervetebral disc. The annulus fibrosis functions as a fibrous capsule to the intervertebral disc, combining minimal movement with strong intervertebral attachment. This allows axial loads to be transmitted and absorbed radially through the disc. The meshwork of vertebral trabecula is thin and supported circumferentially by a cylindrical wall of bone that is much thinner and weaker than the attached neural arch and appendages. Excessive loads on the spinal column preferentially cause fracture by herniation of the incompressible nucleus pulposus through the end plates, creating Schmorl’s nodes in the vertebral body. At age 7-8 years, the nucleus pulposus begins to be replaced with collagen fibers and diminishes in elasticity, causing load factors to be transmitted more directly to the periphery of the vertebral endplates. This process accelerates with age as discs lose their elasticity and height.
Vertebral Bodies. Twelve thoracic and five lumbar vertebral bodies are the fundamental structural elements that serve to protect the spinal cord in the thoracolumbar region. Each vertebra consists of an anterior body connected to a posterior neural arch with paired inferior, superior, and transverse vertebral processes. Growth is constant at all vertebral levels until age 2, when the lumbar vertebrae begin increasing in both lateral and anterior-posterior diameters more than the thoracic elements, in response to the greater axial load-bearing that accompanies increasing upright physical activity. The anterior and posterior longitudinal ligaments, along with the ligament flavum and interspinous and supraspinous ligaments, serve to maintain functional integrity of the vertebral column and allow limited movement of vertebrae relative to one another without destabilization. Initially, the infant spine forms a simple, continuous, convex curvature, but as it matures, it evolves to a lordotic curvature in the cervical region, and later in the lumbar region. This is coincident with the development of improving muscular strength and tone of the cervical and lumbar paraspinous muscles. The thoracolumbar musculoskeletal system assumes the architecture of a tripod, with the vertebral column anteriorly being stabilized at each level by posterior-lateral tensioned erector spinae musculature on either side. This functional architecture allows limited segmental mobility of individual vertebra, while providing significant vertical stability against outside injury forces. Immature vertebrae initially are wedge-shaped, with a notching of the anterior vertebral body representative of fetal notochord remnants. The vertebral end plates float over the superior aspect of each vertebral body, and remain separated by a zone of endochondral ossification that persists until puberty and final epiphyseal closure. This endochondral zone represents the weakest structural element of the vertebral-ligamentous complex and, therefore, is the most frequent site of injury in the growing child. These injuries can be very subtle, with the diagnosis often missed until later in life when abnormalities of bony growth become evident.8,9 Often, it is then too late to take corrective action, and the child is left with permanent structural or functional impairment. This occurs frequently in child athletes who push the limits of performance at the risk of injury.
Biomechanical Properties
Thoracic Spine. In contrast to the highly mobile and poorly supported cervical spine, the superior 9-10 thoracic vertebrae are well protected by a combination of anatomic factors. Articulations between the vertebral transverse processes and the ribs form a flexible cage that limits rotation at any isolated vertebral process, yet allows progressive rotation of the entire thoracic spine at approximately 8° per vertebrae above T8, decreasing to 2° below T10. This is consistent with the gradual transition of the articulating facets in the thoracic vertebrae from high thoracic coronal orientation to the sagittal alignment present in the lumbar spine. The enclosed thoracic contents also serve as a cushion from direct anterior trauma and protect the thoracic vertebral bodies. Flexion and extension is restricted similarly by the thoracic contents, the posterior ligamentous tension of the supraspinous and interspinous ligaments, and the inherent anterior convexity of the assembled thoracic vertebrae derived from wedge-shaped vertebral bodies. The transition of the thoracolumbar junction at T11-12 and L1 allows maximum flexion and extension at this level, as T11 and T12 function more like the lumbar vertebrae. They have less protection and stability, are more susceptible to injury forces, and also absorb the cumulative sum of rotational or axial loads placed on the upper half of the torso. The majority of TLSI occurs at this level in the form of burst or compression fractures with displacement of bone into the spinal canal. Neurologic injury levels in the developing thoracolumbar spine mimic adult levels after 1 year of age and usually are incomplete.2,10 The thoracic vertebral canal represents the narrowest diameter of the entire thoracolumbar spine and is the least forgiving to encroachment from bony or soft-tissue fragments before neural elements become affected.
Lumbar Spine. The lumbar vertebrae are aligned in a lordotic (posterior convex) curvature, with the center of gravity posterior to the vertebral processes. This alignment confers transfer of up to one-third of the weight-bearing support to the posterior elements of the lumbar vertebrae at adulthood. Fractures to the lumbar vertebrae characteristically involve L1 to L3, with disruption of the posterior elements with longitudinal separation (distraction) and high potential instability.3,11,12 The normal rotational axis in the anterior-posterior plane for flexion and extension passes through the center of the nucleus pulposus. With blunt force trauma to the abdomen, abdominal contents often are compressed against the anterior aspect of the vertebral body, and a forward shift occurs in the axis of rotation to a location just anterior to the abdominal wall.13 This shifted rotational axis magnifies the distractive forces on the posterior elements of the intervertebral ligaments, with the potential for resulting rupture and vertebral instability.1,11,12,14
Determination of Stability
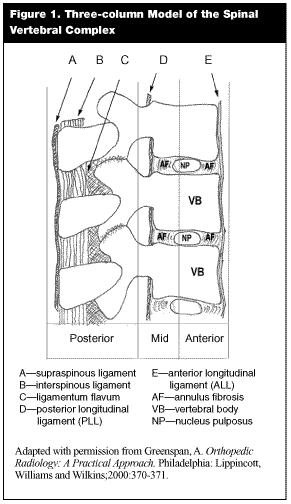
The three-column model of TLSI was proposed by Denis in 1983 to predict the biomechanical stability of the vertebral-ligamentous complex in response to fracture or injury and the subsequent need for treatment with active immobilization or fixation.15 (See Figure 1.) This was derived from morphologic characteristics of each fracture and then refined to reflect computed tomography (CT) scan findings consistent with each fracture type. The three column model modified an earlier model defining disruption of the posterior ligamentous complex as the required determinant of biomechanical instability. Instability with the three column concept recognizes that at least two of the three columns must be disrupted to create an unstable fracture. Stability has been quantified by degree of severity.6,16,17
This predictive model has been used in conjunction with injury forces and mechanisms of injury producing fracture to classify all vertebral fractures into four major categories. (See Table 1.) These categories further can be subdivided to prognosticate outcomes based on selection of the fracture type and extent of treatment. This classification involves the same standard variables that are applied to appendicular skeletal fractures: 1) presumptive mechanism of injury; 2) fracture pattern and location; and 3) degree of comminution and displacement.2,19,20

Fracture Types
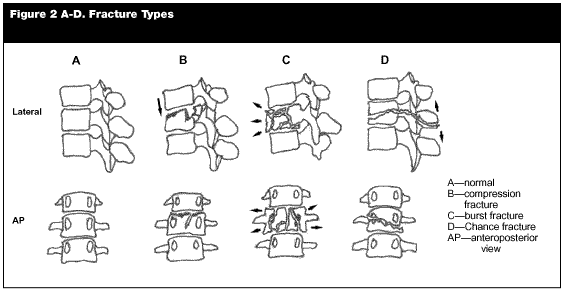
Compression Fractures. Vertebral compression fractures constitute up to 75% of all thoracolumbar fractures and are defined as disruption of the anterior spinal column with an intact middle/posterior column.13 Figure 2A shows a normal anterior spinal column. The usual mechanism of injury is an axial loading or hyperflexion that distributes the compressive force over the anterior surface of vertebral endplates. (See Figure 2B.) Thoracic vertebrae respond with forced anterior flexion because of their normal anatomical kyphosis. With sufficient force, endplate failure occurs, with subsequent collapse of the thin cortical bone of the anterior cylindrical vertebral wall, creating a simple wedge fracture. Lateral compression fractures occur with similar forces applied laterally. Neurological injury is rare.11,20-22 Concomitant increases in the tension of the posterior ligamentous complex initially resists increased flexion. Continued application of increasing force can overcome this resistance, resulting in disruption of the posterior ligamentous complex and creation of an unstable compression fracture.
The intervertebral disc plays a crucial role in the genesis of compression fractures. Immature intervertebral discs contain a hydrophilic nucleus pulposus that is fluid, and therefore incompressible, but serves to redistribute vertical compressive forces equally in a radial-horizontal fashion to the annulus, which has the elasticity to distort, recover, and transmit loads onto adjacent vertebrae. Forces that exceed the ability of discs to compensate can cause rupture of the nucleus pulposus through the endplate and into the central spongiosa of the vertebral body. Extension of these fractures to the periphery is rare and consistent with the low incidence of vertebral body fracture in young children. As collagen replaces the fluid of the nucleus late in the first decade, elasticity declines and the pulposus and annulus function as a unitary solid. Vertical force vectors no longer are dissipated, but act directly on the periphery of the more ossified vertebral body, resulting in the classic compression or burst fracture. Compression fractures are the most common type of vertebral fracture.
Burst Fracture. Thoracic burst fractures are a result of compressive axial loading, with or without flexion, exceeding simple vertebral body compression. This fracture results in fragmentation, with centrifugal displacement of the bone. (See Figure 2C.) The extent of displacement is directly proportional to the magnitude of injury force. Burst fractures, by definition, involve both anterior and middle column failure but may be considered stable if the posterior column remains intact. The superior vertebral end plate is most commonly involved, usually at the thoracolumbar junction.23 Posterior column involvement is possible with severe compressive forces. The fragments of disc and vertebral bone are displaced centrifugally, with the potential to breech the posterior longitudinal ligament (PLL) and compress the neural elements of the spinal canal.10,12,24,25
An unstable burst fracture is one in which the posterior column is disrupted as a result of the distraction forces that accompanies forced flexion. Neurological deficits have been reported to be variable and poorly correlated with the extent of spinal canal compromise.12
Flexion-Distraction Fractures. The classic flexion-distraction fracture (FDF) of thoracolumbar vertebrae was described radiographically by Chance in 1948, and since has been referred to as the Chance fracture.4,22,25,26 This fracture pattern is horizontal splitting of the vertebrae through the body, pedicles, and neural arch. (See Figure 2D.) The posterior ligamentous complex is completely distracted in tension, while the anterior column is involved in proportion to the magnitude of the injuring forces. The anterior longitudinal ligament (ALL) usually remains intact but can be stripped from the anterior surface of the vertebral body or disrupted if kinetic energy is sufficient. The mechanism of injury consists of high energy rotational flexion forces applied to an axis anterior to the vertebral body. The original description by Chance was of a pure osseous lesion, but since has been applied to similar injury involving combined osteoligamentous or pure soft-tissue (ligamentous or disc) injury. Since the description by Chance, FDF commonly have been reported in association with improper lap belt restraint of children involved in motor vehicle accidents. Consequently, Chance fractures now are referred to as the lap belt or seat belt fracture injury unique to young children.27-31 Stability is dependent on the degree of involvement of the anterior spinal column. Disruption of the ALL makes this injury highly unstable in flexion. Without involvement of the ALL, neurological involvement is surprisingly rare, reported in fewer than 10% of patients.26 Associated intra-abdominal organ injury is common, since abdominal contents are compressed between the restraining seat belt and the anterior vertebral body.32-37
FDF in which the axis of rotation remains posterior to the ALL (the normal anatomic situation) results in compressive failure of the anterior column and distraction failure of both middle and posterior columns. Complete disruption of the posterior longitudinal ligament (PLL) and facet joint capsules make subluxation possible.
Translational Fractures. This category encompasses a combination of mechanisms causing spinal fractures that result in failure of all three spinal columns; more specifically, shear injuries, flexion-rotation, and fracture dislocation. Translational injuries disrupt the alignment of the spinal canal and thereby displace the neural elements in the transverse plane. This group, therefore, exhibits the highest incidence of associated neurologic deficits.
Flexion-Rotation Fractures. In contrast to FDF that involve the primary injury acting in the sagittal plane, the addition of rotatory forces places stress on the facet capsules. Failure of the posterior ligamaments along with facet capsules allows the vertebral body and disc to dislocate obliquely, disrupting all three spinal columns. During dislocation, the superior articulating facet of the vertebrae inferior to the level of injury is fractured on one side and the contralateral facet capsule fails in distraction. This appearance on plain radiography is pathognomonic for rotatory failure. Fractures of the transverse process and rib commonly are seen associated with flexion-rotation fractures.
Shear Fractures. Translational fractures are secondary to horizontal shearing forces created by direct localized injury vectors that pass through the spine at different vertebral levels. Usually, the spine is forced into extension with subsequent disruption of the ALL, and the disc annulus is ruptured or torn as affected vertebrae translate anterior or posterior relative to the remainder of the vertebral column. If the superior vertebrae shears anteriorly (more common), its posterior elements (neural arch and spinous process) often fracture and remain behind as the spinal cord and nerves are compressed by traction from the anterior displacement of the vertebral body across the static superior end plate of the inferior vertebral body. This results from superior articulating facets of the inferior vertebrae blocking anterior movement of the inferior facets of the superior vertebrae. If the superior vertebrae shears in a posterior direction, it simply ruptures facet capsular attachments and transects the PLL while compressing neural elements between its posterior moving vertebral body and the fixed posterior elements of the inferior vertebrae. Vertebrae and posterior arches usually remain intact in the latter circumstance. Paraplegia, dural tears, and gross instability frequent are results of shear fractures.
Hyperextension Fracture. Extension fractures are caused by forces opposite of those that cause hyperflexion fractures; i.e., rapid posterior movement of the head, neck, and upper body, usually as a result of a sudden, blunt force from the posterior direction. Compression occurs to the posterior column while tension distracts the ALL and the anterior aspect of the annulus fibrosus. Given enough force, the ALL can be avulsed off the anterior vertebral surface with or without bony fragments, causing anterior and middle column failure. Fracture of the pars interarticularis or lamina also have been described.11,16 Hyperextension fracture sometimes is called the "lumberjack fracture," as the mechanism was described in lumberjacks struck from behind by falling timber.11
Clinical Presentation and Evaluation
TLSI can be very difficult to detect and diagnose. TLSI requires injury from high energy, blunt force trauma, most commonly from motor vehicle-related (occupant or pedestrian) accidents, falls, crush or sports injuries, and non-accidental trauma. While the mechanism of injury may be obvious from history, competing priorities of the ABCs and primary and secondary survey of trauma care take precedence over neurologic or orthopedic examination. Rapid detection and treatment of intra-abdominal or intrathoracic trauma are priorities to diagnose life-threatening bleeding or compromise of vital organ function, since patients rarely present with isolated TLSI from major trauma.
Children or infants with concomitant or distracting non-life-threatening injuries that are obvious on physical examination can serve to lower a physician’s index of suspicion of TLSI. A complete general physical examination is difficult in a frightened or agitated child who is restrained in a collar on a backboard. The neurologic examination, which could detect deficits and reveal possible TLSI, requires cooperation and a minimum level of speech development to communicate the subtleties of anesthesia, paraesthesia, etc, and rarely is optimal in traumatized children. Once initial radiographic studies have been completed, a thorough inspection and palpatory examination of the entire spine is mandatory. Heavy dependency on injury patterns, awareness of age-injury associations, knowledge of injury mechanisms, serial exams, and an overall high index of suspicion is the favored approach.38
Injury Age Groups
Infants. The 0-2 year age group has proportionally larger heads and weak neck musculature, which contribute to a high center of gravity and head-first orientation of the body during ejection or unrestrained movement. Smaller torsos mean equivalent injury forces are inflicted over more anatomic areas, raising the potential for multiple injuries. Head injury from contact with fixed objects, usually a dashboard or windshield, commonly is associated with spinal injuries in this age group. An added concern for emergency physicians is a smaller percentage of TLSI caused by non-accidental trauma (NAT).5,39 Incidence of TLSI secondary to NAT has been estimated from 0-3% of all spinal injuries by several investigators.1 Variations in reporting, delayed diagnosis of injuries, lack of autopsy findings, unrecognized trauma and SCIWORA make accurate incidence difficult. Most patients in this age group will not have clinical findings on presentation.1,40,41
One retrospective series of more than 1100 pediatric TLSI trauma patients reported 11% of emergency department (ED) patients with a delayed diagnosis of injury (DDI), some as long as two weeks post-injury.10 Two patients in the same series with injuries (non-TLSI) from NAT were missed on first presentation. Some investigators propose that DDI is unavoidable in multiple trauma, but the issue is of high importance for emergency physicians, who may discharge pediatric patients back to the same social situations only to have them return later moribund or terminal. Estimates are high that many children with fatal cases of NAT have been seen at least once previously by a physician. Delayed presentation also contributes to a paucity of findings. In another series of 156 patients, more than 54% had TLSI but only 7% had neurologic findings; two patients had SCIWORA.3 Thirty-five percent of the spinal fractures had minimal or no pain on presentation to the ED.3 The mechanism of injury for TLSI in NAT is unclear but is thought to be secondary to hyperflexion or hyperextension, possibly associated with shaking or direct blunt-force blows.1
In spite of the above risks, anatomic advantages like high elasticity of the intervertebral discs, relatively strong ligamentous attachments, and rapid healing impart some protection against TLSI. Injury forces usually are absorbed over multiple segments, and failure of the annulus fibrosus in response to trauma has not been reported in immature spines.2,41 Physeal disruption is the rule in fractures, but when combined with usually spontaneous re-approximation there can be stabilization of what would be an unstable injury in older age patients. Growth can remain unaffected and deformities may correct over time, depending on location and degree of disruption.
Spinal Cord Injury without Radiographic Abnormality. TLSI SCIWORA has a reported incidence up to 50% in children, compared to fewer than 1% in adults. Since its description by Pang, it has been an anathema for emergency physicians.6,7,42,43 The mean age of occurrence of SCIWORA is 6 years, and it is associated with poorer neurologic recovery.8,44 Proposed mechanisms of SCIWORA include physeal separation, ligamentous disruption, and ligamentum flavum compression of the spinal cord secondary to infolding in hyperextension.40,44 Spinal cord infarction from compromise of collateral blood supply or disruption of the artery of Adamkiewicz supplying the spinal cord, hematoma formation from soft-tissue bleeding, and direct contusion of the thoracic spinal cord also contribute to nonosseous injury.2,6,41,44,45 Younger patients with SCIWORA have more neurotrauma and a poorer prognosis than the preadolescent group. Aggressive use of magnetic resonance imaging (MRI) is helpful in discriminating SCIWORA from simple soft-tissue injury.46,47
Preschool to Preadolescent. These children have matured from the top heavy infant somatotype to a lower center of gravity with stronger abdominal musculature. Lordosis of the cervical and lumbar vertebrae now replaces the kyphosis dominant alignment of the infant spine. The thoracolumbar junction is now becoming the point of greatest mobility in the thoracolumbar spine. Intervetebral discs begin to collagenize, allowing the transfer of more injury forces to the vertebral body, which has begun the process of ossifying the ring apophysis. The appendicular skeleton still is maturing, with open physes and incompletely developed iliac prominences. Improved motor control and increasing independence raises potential injury risks as this group becomes more active in sports and outdoor recreation. Bicycles, skateboards, scooters, rollerblades, all-terrain vehicles, trailbikes, and power watercraft are well accepted social enticements to these children. Increased visibility of the so-called extreme sports approach is encouragement to be daring; however, cognitve judgment and perception are not completely developed, making supervision important.48 Motor vehicle accidents remain the leading cause of injury and accidental death. In 1997, 77% of the 161 deaths secondary to riding in truck cargo areas were children or adolescents, yet many states have no statutes outlawing this practice.49
The lap belt or seat belt injury is common in this age group and well documented in the literature. 22,24,28,30,31,33,34,50 Children older than 4 years of age have outgrown child safety seats but do not have developed iliac crests to serve as anchor points for lap belts. In addition, the shoulder strap often crosses at neck level or too high to be used at all. The lap belt slides up over the abdomen during collision and creates the ideal environment for a hyperflexion injury (i.e., Chance fracture) with the rotational axis at the lap belt.25,27,28,30,33 Patients in this age group presenting to the ED with abdominal bruising or pain should raise clinical suspicion and precipitate a search for TLSI.24,27,28 Booster seat use can ensure proper restraint and eliminate this injury, but misuse is common.51 An estimated 85% of children who are placed in car seats and booster seats are improperly restrained.52-54
Adolescents (12 and Older). Organized, competitive athletics, risk-taking, and peer influence exemplify this group. As first-time operators of motor vehicles, the adolescent group has the single highest accident risk. Standard lap/shoulder belts are appropriate, and injury patterns are congruent with those of adults. SCIWORA rarely is seen. Typical osseous TLSI follows the standard mechanisms described previously. Injury prevention needs to be emphasized through proper use of safety equipment and procedures to limit serious injury.
Emergency Treatment
Emergency treament is instituted as with any other traumatic patient, with stabilization of the patient’s airway, breathing, and circulation (ABCs). A complete secondary survey examination of the neurologic system is essential to determine deficits and potential levels of injury. Positive findings require serial re-examination to document progression, accuracy, or improvement of injuries. Maintaining immobilization through use of a rigid spinal board is necessary to prevent any further iatrogenic injury. Typically, patients will be evaluated radiographically to assess the extent of any fracture and possible spinal cord involvement before any decision is made regarding neurosurgical intervention. There is some evidence that aggressive stabilization provides the optimum chance for positive outcomes. Specific surgical techniques and therapies exceed the scope of this article. High-dose steroid administration, albeit increasingly controversial, remains approved treatment when any neurologic defict is present secondary to TLSI. Once the ABCs have been addressed and stabilized, attention can be directed at delineating any areas of injury or deformity detected on secondary survey. Plain films typically are utilized to screen for obvious bony injury. Early use of MRI in pediatric patients with neurologic deficits can provide accurate assessment of bony and soft-tissue injury that may not be detectable by plain or CT radiography.
Diagnostic Approach
Initial radiologic studies are usually plain radiography directed at areas of clinically evident trauma or areas of tenderness elicited on physical examination.
Full thoracic-lumbar anterior/posterior and lateral spine films are a minimum to detect bony disruption. Patients who are highly suspect for TLSI should be maintained in immobilization in the supine position on a rigid board until a cross-table lateral can confirm normal alignment and intevertebral spacing. A normal lateral by no means eliminates all possibility of injury but in the face of an otherwise normal physical examination can allow the patient to undergo remaining studies with cautious attention to limiting movement.
Oblique films add very little to the evaluation of traumatic injury and can require significant movement of the patient. CT or MRI should be employed if there is a high index of suspicion for injury or plain films are sub-optimal, as sometimes happens particularly with the higher thoracic vertebrae. Evidence suggests that the entire spinal column of a pediatric patient should be imaged if injury is present at any level.55 Initial use of CT evaluation should be avoided as abnormalities may be missed due to the axial orientation of vertebral fractures even with thin section imaging technique.56 Interpretation of plain thoracic and lumbar radiographs should be systematic and directed at alignment, standard curvatures and cartilaginous structures and spaces. (See Figure 3.)
Computed Tomography. CT has evolved significantly from its introduction to present day where high speed, sensitive scans of the vertebral column can be obtained with a minimum of effort and without movement of the patient.18 It is by far the preferred study of choice when searching for and evaluating occult vertebral fractures and the degree of encroachment on the neural elements of the vertebral foramen. Categorization based on CT findings also can allow some prediction regarding stability of the injured spine and need for immediate or delayed intervention. CT should be interpreted in concert with thoracolumbar spine radiographs because abnormalities may not be detected regardless of the size of imaging sections on CT.56
Magnetic Resonance Imaging. MRI is becoming more commonly utilized as trauma centers develop experience with imaging and detection of ligamentous and soft-tissue injuries. MRI is the imaging of choice for patients with SCIWORA. It has been shown to be extremely useful in assessing injuries to the bone, soft tissues, and spinal cord, and also for predicting spinal stability. In children, early use of MRI has been recommended. Limitations on its use in trauma persist.10,57 The prerequisite is a stable patient who can remain motionless for long periods of time, either voluntarily or while sedated. Patients requiring ventilator support or who have hardware in place are difficult to adapt to the MRI suite and take extensive preparation and planning, which are unlikely to be possible on an emergent basis.
Prevention
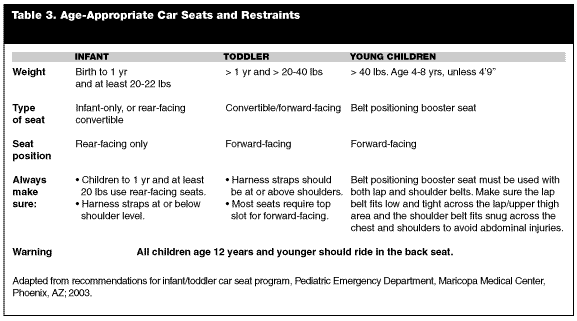
The majority of TLSI can be reduced by regular use of age-appropriate child car seats and restraints when children are passengers in motor vehicles. (See Table 3.) Estimates are that use of car seat and restraints reduce child fatalities by as much as 70% and injuries by as much as 50%.58 While all 50 states mandate use of seat belts or car seats for children, enforcement remains a low priority for most public safety agencies. Additionally, studies have indicated that as many as three-quarters of all car seats are improperly used or installed. Physicians themselves are poorly trained and informed on use of car seats.53 The American Academy of Pediatrics has published recommendations on car seat selection and use.59 Currently, rear-facing child restraint seats should be used in children who weigh up to 9 kg. Children may be switched to a forward-facing seat at age 1 year and when able to sit unsupported. Use of standard vehicle safety belts should be limited to those children older than age 2 who can be positioned with the lap belt snug across the thighs and with the shoulder belt across the chest. Use of lap-only belts puts children at higher risk for Chance-type TLSI. Children should not ride in the front passenger seat, particularly those equipped with passenger side passive air bags, as these have been associated with fatalities. As of November 2000, 98 children had been killed by passenger air bags. Nearly 20% of these deaths were infants in rear-facing car seats placed in front of a passenger airbag. Almost all children killed by passenger airbags were either unrestrained or improperly restrained at the time of the crash.59 Automakers have begun to address this by installing airbags that deploy at reduced energies. Simply seating children in rear seats confers limited protection even without restraint use.50 Travel in open cargo areas of trucks is to be condemned. Cargo area passengers are at 3-8 times greater risk of fatal injury.49
Summary
TLSI can be difficult to diagnose in the pediatric population. Injuries can be divided into well-defined categories and analysis of stability made based on the three-column model of spinal anatomy. A high index of suspicion and basic understanding of injury mechanisms, coupled with a thorough physical examination, can help identify clues to pediatric TLSI. Aggressive use of CT and MRI can identify subtle injuries as well as involvement of neural elements and provide prognostic information in children who have potential for neurologic recovery. Emergency physicians can avoid missing this rarely seen but important spinal injury.
References
1. Akbarnia BA. Disorders of the pediatric and adolescent spine: Pediatric spine fractures. Ortho Clin North Am 1999;30:521-535.
2. Ferguson RL. Thoracic and lumbar spinal trauma of the immature spine. In: Herkowitz H, Rothman R, Simeone F, et al, eds. Rothman-Simeone: The Spine. 4th ed. Philadelphia: WB Saunders; 1999.
3. Anderson JM, Schutt AH. Spinal injury in children: A review of 156 cases seen from 1950 through 1978. Mayo Clin Proc 1980;55: 499-504.
4. Chance GQ. Note on a type of flexion fracture of the spine. Br J Radiol 1948;21:452-453.
5. Swischuk LE. Spine and spinal cord trauma in battered child syndrome. Radiology 1969;92:733-738.
6. Yngve D, Harris W, Herndon W, et al. Spinal cord injury without osseous spine fracture. J Ped Orthop 1988;8:153-159.
7. Kewalramani LS, Kraus JF, Sterling HM. Acute spinal cord lesions in a pediatric population: Epidemiological and clinical features. Paraplegia 1980;18:206-219.
8. Hadley MN, Zabramski JM, Browner CM, et al. Pediatric spinal trauma: Review of 122 cases of spinal cord and vertebral column injuries. J Neurosurg 1988;68:18-24.
9. Kerttula LI, Serlo WS, Tervonen OA, et al. Post-traumatic findings of the spine after earlier vertebral fracture in young patients: Clinical and MRI study. Spine 2000;25:1104-1108.
10. Furnival RA, Woodward GA, Schunk JE. Delayed diagnosis of injury in pediatric trauma. Pediatrics 1996;98:56-61.
11. Garfin SR, Blair B, Eismont FJ, et al. Lumbar and sacral spine trauma. In: Skeletal Trauma: Fractures, Dislocations and Ligamentous Injuries, Vol 2. Philadelphia: WB Saunders;1998.
12. Garfin SR, Blair B, Eismont FJ, et al. Thoracic and upper lumbar spine injuries. In: Skeletal Trauma: Fractures, Dislocations and Ligamentous Injuries, Vol 2. Philadelphia: WB Saunders;1998.
13. Cohen MS, Blair B, Garfin SR. Thoracolumbar compression fractures. In: Levine AM, et al, eds. Spine Trauma Philadelphia: WB Saunders;1998.
14. Daffner R. The thoracic and lumbar spine. In: Rogers L, ed. Radiology of Skeletal Trauma. Philadelphia:Churchill Livingstone, HHS; 2002.
15. Denis F. Spinal instability as defined by the three-column spine concept in acute spinal trauma. Clin Ortho and Rel Res 1984;189:65-76.
16. Bucholz RW, Gill KG. Classification of injuries to the thoracolumbar spine. Ortho Clin NA 1986;17:67-73.
17. Garfin SR, Vaccaro AR. Orthopaedic knowledge. In: American Academy of Orthopedic Surgeons. Update: Spine. 1st ed. Rosemont, IL; AAOS: 1997.
18. McAfee PC, Yuan HA, Frederickson BE, et al. The value of computed tomography in thoracolumbar fractures. J Bone Joint Surg 1983; 65A:461-473.
19. Bohlman HH, Ducker TB, Levine AM, et al. Trauma. In: Herkowitz H, Rothman R, Simeone F, et al, eds. Rothman-Simeone: The Spine Vol. 2. 4th ed. Philadelphia:WB Saunders Co;1999.
20. Ogden JA. Injury to the thoracic spine. In: Skeletal Injury in the Child. 2nd ed. Philadelphia: WB Saunders Co; 1990:600-605.
21. Ogden JA. Injury to the Lumbar Spine. In: Skeletal Injury in the Child. 2nd ed. Philadelphia: WB Saunders Co; 1990:605-609.
22. Kandabarow A. Injuries of the thoracolumbar spine. Topics in Emergency Medicine 1997;19:65-80.
23. Ferguson RL. Spine trauma in adults. In: Herkowitz H, Rothman R, Simeone F, et al, eds. Rothman-Simeone: The Spine. Vol 2, 4th ed. Philadelphia: WB Saunders; 1999.
24. Velmahos GC, Tatevossian R, Demetriades D. The "seat belt" sign: A call for increased vigilance among physicians treating victims of motor vehicle accidents. Am Surgeon 1999;65:181-185.
25. Chance GQ. Note on a type of flexion fracture of the spine. Br J Radiol 1948;21:452.
26. Chapman JR, Anderson PA. Thoracolumbar spine fractures with neurologic deficit. Ortho Clin North Am 1994;25:595-612.
27. Rennie W, Mitchell N. Flexion distraction fractures of the thoracolumbar spine. J Bone and Joint Surg 1973;55A:386-390.
28. Johnson DL, Falci S. The diagnosis and dreatment of pediatric lumbar spine injuries caused by rear seat lap belts. Neurosurg 1990; 26:434-441.
29. Rogers LF. The roentgenographic appearance of transverse or Chance fractures of the spine: The seat belt fracture. Am J Roentgen 1971; 111:844-849.
30. Voss L, Cole PA, D’Amato C. Pediatric Chance fractures from lapbelts: Unique case report of three in one accident. J Ortho Trauma 1996;10:421-428.
31. Gertzbein SD, Court-Brown CM. Flexion-distraction injuries of the lumbar spine: Mechanisms of injury and classification. Clin Ortho and Related Res 1998;227:52-60.
32. Letts M , Davidson D, Fleuriau-ChateauP, et al. Seat belt fracture with late development of an enterocolic fistual in a child. Spine 1999; 24:1151-1155.
33. Agran PF, Dunkle DE, Winn DG. Injuries to a sample of seatbelted children evaluated and treated in a hospital emergency room. J Trauma 1987;27:58-64.
34. Smith WS, Kaufer M. Patterns and mechanisms of lumbar injuries associated with lap seatbelts. J Bone Joint Surg 1969;51A:239-254.
35. DeCou JM, Abrams RS, Gauderer MWL. Seat-belt transection of the pararenal vena cava in a 5-year-old child: Survival with caval ligation. J Ped Surg 1999;34:1074-1076.
36. Beaunoyer M, St-Vil D, Lallier M, et al. Abdominal injuries associated with thoraco-lumbar fractures after motor vehicle collision. J Ped Surg 2001;36:760-762.
37. Letts M, Davidson D, Fleurian-Chateau P, et al. Seat belt fracture with late development of an enterocolic fistula in a child. Spine 1999; 24:1151-1155.
38. Jordan B. Lap belt complex. Recognition and assessment of seat belt injuries in pediatric trauma patients. J Emerg Med Serv 2001;26: 36-43.
39. Gabos PG, Tuten HR, Leet A. Fracture-dislocation of the lumbar spine in an abused child. Pediatrics 1998;101:473-477.
40. Trumble J, Myslinski J. Lower thoracic SCIWORA in a 3-year-old child: Case report. Ped Emerg Care 2000;16:91-93.
41. Aufdermaur M. Spinal injuries in juveniles: Necropsy findings in twelve cases. J Bone Joint Surg 1974; 56:513-519.
42. Pang D, Wilberger JE. Spinal cord injury without radiographic abnormalities in children. J Neurosurg 1982;57:114-129.
43. Pang D, Wilberger JE. Spinal cord injury without radiographic abnormalities in children-the SCIWORA syndrome. J Trauma 1989;29: 654-664.
44. Yazici M, Alanay A, Aksoy MC, et al. Traumatic L1-L2 Dislocation without fracture in a 6-year-old girl: Incomplete neurologic deficit and total recovery. Spine 1999; 24:1483-1486.
45. Green NE, Swiontkowski MF. Thoracolumbar spine fractures. In: Skeletal Trauma in Children Vol 3. Philadelphia: WB Saunders; 1998.
46. Tehranzadeh J, Andrews C, Wong E. Lumbar spine imaging: Normal variants, imaging pitfalls, and artifacts. Radiologic Clin North Am 2000;38:1-34.
47. Sledge JB, Allred D, Hyman J. Use of magnetic resonance imaging in evaluating injuries to the pediatric thoracolumbar spine. J Ped Ortho 2001;21:288-293.
48. Sneed RC, Stover SL, Fine PR. Spinal cord injury associated with all-terrain vehicle accidents. Pediatrics 1986;77: 271-274.
49. Bull MJ, Agran P, Laraque D, et al. Children in pickup trucks. Pediatrics 2000;106:875-879.
50. Wittenberg E, Goldie SJ, Graham JD. Predictors of hazardous child seating behavior in fatal motor vehicle crashes:1990-1998. Pediatrics 2001;208:438-442.
51. Winston FK. The danger of premature graduation to seat belts for young children. Pediatrics 2000;105:1179-1183.
52. McKay MP, Curtis LA. Child safety: Do doctors know enough? Am J Emerg Med 2002;20:32-34.
53. Bull MJ, Agran P, Garcia V, et al. Selecting and using the most appropriate car safety seats for growing children: Guidelines for counseling parents. Pediatrics 2002;103:550-553.
54. Berns SD, Vaca F. NHTSA Notes Commentary: We need to give children a boost before we buckle them. Ann Emerg Med 2001;37: 407-410.
55. Vacccaro AR, An HS, Lin S, et al. Noncontiguous injuries of the spine. J Spinal Disord 1992; 5:320-329.
56. Glass RBJ, Sivit CJ, Sturm PF, et al. Lumbar spine injury in a pediatric population: Difficulties with computed tomographic diagnosis. J Trauma 1994;37:815-819.
57. Kulkarni MV, McArdle CB, Kopanicky D, et al.Acute spinal cord injury MR Imaging at 1.5 T. Neuroradiology 1987;164:837-843.
58. McKay MP, Curtis LA. Child safety seats: Do doctors know enough? Am J Emerg Med 2002;20:32-34.
59. Injury facts from safe kids org. www.safekids.org/tier3_cd.cfm?content_item_id=1133&folder_id=540. (Accessed 5/13/2003.)
Although spinal injuries occur infrequently, a delay in the detection of thoracolumbar trauma may have devastating consequences for a child. It is critical that the emergency physican be familiar with injury patterns that may result in this type of injury.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.