Emergency Ultrasound, Part III: Acute Trauma
Part III: Acute Trauma
Authors: Michael J. Lambert, MD, RDMS, Clinical Assistant Professor, Department of Emergency Medicine, University of Illinois College of Medicine, Fellowship Director, Emergency Ultrasound, Resurrection Medical Center, Chicago, IL; Joseph P. Wood, MD, JD, RDMS, Senior Associate Consultant, Mayo Clinic, Scottsdale, AZ.
Peer Reviewers: Anthony Macasaet, MD, FACEP, Assistant Professor and Vice Chair, The Chicago Medical School; Director, Emergency Medicine Ultrasound, Mt. Sinai Hospital, Chicago, IL; Kenneth H. Butler, DO, Associate Residency Director, University of Maryland Emergency Medicine Residency Program, University of Maryland School of Medicine, Baltimore.
No other imaging modality has the ability to diagnose certain critical traumatic conditions as quickly or as accurately as a bedside ultrasound examination. Trauma surgeons in Europe, Canada, and Japan have been utilizing diagnostic ultrasound as a routine part of their evaluation of the injured patient for more than 20 years.1,2 More recently, emergency physicians and trauma surgeons in the United States have adopted bedside ultrasound as an important adjunct to their clinical evaluation.3 Widespread adoption of bedside diagnostic ultrasound raises issues of training and credentialing, as well as the reliance that should be placed on bedside ultrasound exams and their ability to obviate the need for other diagnostic tests, such as diagnostic peritoneal lavage or computed tomography (CT) scanning.
The Focused Assessment with Sonography in Trauma (FAST) is a bedside ultrasound examination used primarily by emergency physicians and trauma surgeons to identify free intraperitoneal, intrathoracic, or pericardial fluid.4 This article will describe the sonographic acoustic windows and technique of the FAST examination. Understanding the sensitivity and specificity of this imaging modality for various conditions and age groups is necessary for the safe incorporation and integration of diagnostic ultrasound in a trauma evaluation algorithm.—The Editor
In general, emergency physicians and surgeons performing bedside ultrasound exams on trauma patients are looking for abnormal collections of fluid. Since fluid has an unmistakable appearance on ultrasound, it is not surprising the literature consistently has shown a high specificity when free fluid is identified.5,6 However, the failure to see free fluid on the ultrasound exam does not conclusively rule out an injury.7 While ultrasound has been shown to be highly sensitive in the detection of intrathoracic fluid, it will pick up free intraperitoneal fluid only about 80% of the time when fluid or other evidence of injuries is demonstrated by other means.8 Moreover, ultrasound should not be expected to identify retroperitoneal injuries or intestinal perforations with minimal associated bleeding.7
An important segment of the FAST exam is examining the heart for pericardial fluid. Long before emergency physicians and surgeons began performing FAST exams, ultrasound was considered the preferred gold standard imaging modality when hemopericardium was suspected. Emergency physicians and surgeons trained to perform FAST exams have demonstrated a sensitivity of 100% and specificity of 97% in looking for hemopericardium.9 The advantage of having this imaging modality readily available for use by the clinician evaluating the trauma patient is the shortened time to diagnosis and subsequent treatment. Plummer demonstrated a decreased time from presentation to treatment of hemopericardium from a baseline mean of 42.4 minutes to 15.5 minutes in patients presenting to an urban trauma center with penetrating thoracic injuries when emergency physicians and surgeons routinely performed a focused ultrasound exam of the heart.10 Moreover, properly trained physicians armed with ultrasound capability will examine more low-risk patients than their colleagues who do not possess this skill, since the cost and inconvenience of obtaining the study are reduced significantly by eliminating the need to call in a technician. Lowering the barrier to studying patients with thoracic trauma undoubtedly improves diagnostic accuracy, since the classic triad of distended neck veins, muffled heart tones, and hypotension is seen in only 40% of patients with hemopericardium.9
Physicians performing ultrasound examinations on children have long noticed the relative ease in visualizing the anatomy in the pediatric population. Children tend to have less fat, making it easier to clearly image intra-abdominal solid organs.11 Additionally, performing a bedside ultrasound exam rarely requires the sedation that may be needed, at times, to perform a CT scan. However, the literature has shown a lack of sensitivity for ultrasound in detecting intra-abdominal injuries in the pediatric population. While the specificity remains high if free fluid is identified on a FAST exam, the literature reports sensitivities as low as 30% in this population.12,14 Physicians utilizing bedside ultrasound in evaluating pediatric trauma must be cognizant of this lack of sensitivity in developing evaluation algorithms.
Diagnostic ultrasound particularly can be helpful in the evaluation of the pregnant trauma patient.13 While it lacks the sensitivity of CT scanning, the lack of ionizing radiation may seem like an attractive trade-off to both the clinician and patient. Additionally, the ultrasound exam readily may demonstrate the presence of fetal cardiac activity or movement.15 However, bedside ultrasonography by emergency physicians and surgeons should not be used to evaluate the placenta or to rule out uterine rupture.
Finally, emergency physicians and surgeons initiating the use of FAST exams in their trauma algorithm should be aware of the learning curve before dispositioning patients based on their ultrasound examinations and interpretations. The novice sonologist undoubtedly will not match the sensitivities and specificities quoted in this article.1 The wise clinician will take a formal course, including hands-on training, and then perform a significant number of "learning" studies, comparing their findings to a gold standard imaging procedure.16 Only after the clinician’s ultrasound exams have a high concordance with the concurrent gold standard exam should the bedside exam be utilized in clinical decision-making. In our experience of training residents and attending emergency physicians and surgeons, the learning curve is highly variable.
Trauma Ultrasound Imaging Technique
The FAST exam is a rapid ultrasound examination utilizing four sonographic windows in an effort to identify the presence or absence of free fluid in three anatomical areas (pericardium, pleural, and peritoneum) of the body. The purpose of this sonographic examination in the acutely traumatized patient is to rapidly identify a patient’s most life-threatening injuries.20 There are several advantages to utilizing ultrasound compared to other traditional imaging modalities in the initial evaluation of the trauma patient. The examination can be performed very rapidly; it can be accomplished at the patient’s bedside; it is safe in pregnant patients; serial examinations can be entertained to detect ongoing bleeding; and the true costs are relatively inexpensive.21 Ultrasound, however, never will completely replace the need for other imaging studies in selected trauma patients. It has a limited role in evaluating specific solid organ injuries, diaphragmatic tears, or retroperitoneal injuries. Although we firmly believe that all acutely injured trauma patients with injuries sustained to the thoraco-abdominal region have indications for a FAST scan, the specific clinical indications for a FAST scan in the trauma patient are outlined in Table 1.

Transducers
There is no single best transducer for imaging the trauma patient. The majority of sonologists evaluating trauma patients are using a microconvex transducer. In the trauma setting, a single microconvex probe is fast, easy, and inexpensive. The main advantage of the microconvex is that the footprint of the transducer can fit very easily between the ribs when evaluating the upper quadrants and the heart. An alternative approach is a larger convex probe to evaluate the upper quadrants and the suprapubic window, and a phased array transducer or microconvex to interrogate the heart. Although the larger convex probe will have superior image resolution in the abdominal component of the FAST examination, the large size of its footprint limits its use in evaluating the heart.
Sonographic Windows
The FAST exam makes use of four sonographic windows (see Table 2) in which the sonologist rapidly can evaluate the acutely injured trauma patient. We recommend that every sonologist adhere to a methodical, systematic approach when performing this or any other ultrasound examination.

By repeatedly performing the examination in the same sequence, and obtaining all the necessary information for each window, one can significantly reduce operator error. This section will review the four windows of the FAST exam, including an optional cardiac window: the parasternal long axis. Each of the four FAST sonographic windows described in detail below will review the following:
• Transducer Positioning. The location on the surface of the patient’s body where the ultrasound probe typically is positioned to obtain a window to the organs of interest is described. Most trauma patients arrive via emergency medical services (EMS) on a gurney in a supine position. Often, cervical spine precautions are taken, and the patient arrives with a cervical collar and backboard. In an ideal scanning situation, a sonologist likely would reposition the patient to obtain the best possible window. This frequently is not possible in the acutely injured trauma patient. Therefore, the FAST windows summarized below will be described and illustrated assuming a supine position.
• Sonographic Landmarks. In each FAST window that is obtained, the sonographic information for the anatomical area of interest should be identified and documented in each image.
• Schematic Diagrams. To identify anatomical landmarks and pathological conditions within each FAST window, line art drawings are provided that correspond to the images obtained from each of these four windows.
• Interpretation of Pathological Findings. Each of the FAST windows includes post processing text annotation and symbols to illustrate abnormal findings.
• Common Pitfalls. Each of the FAST windows described addresses specific pitfalls common to the novice sonologist interrogating the trauma patient. Knowledge of these particular pitfalls points out the importance of sonographic landmarks and defining organ boundaries.
Fast Window No. 1: Subxiphoid (Subcostal) View of the Heart
In the subxiphoid view, the transducer is placed in the epigastric region of the patient’s body. The probe is positioned under the xiphoid process of the sternum and directed toward the left shoulder. The sonographic landmarks of the subxyphoid window are the liver, the heart and its four chambers, and the surrounding pericardium.
Pathological Findings. Hemopericardium. Sonographically, blood within the pericardial space will appear anechoic between the hyperechoic pericardium and the epicardium of the heart. (See Figure 1.)
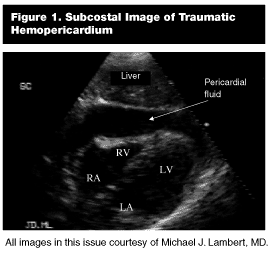
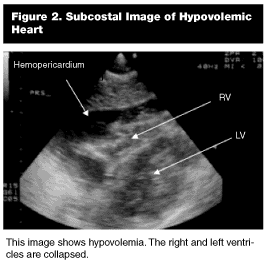
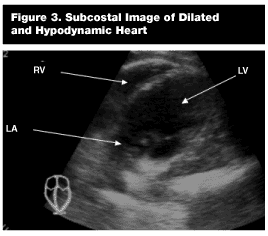
Gross Wall Motion Abnormality. The overall contractility of the heart vs a normal subject. Although still images will not illustrate the gross wall motion abnormality, the overall chamber sizes are compared with normal-sized chambers. A hyperdynamic and contracted heart often will parallel hypovolemia. (See Figure 2.) A hypodynamic and dilated heart (see Figure 3) may reveal a cardiac precursor to the traumatic event. This finding drastically may change management (fluid volume) of the traumatic hypotensive patient.
Pitfalls. Transducer Surface Position. The novice sonologist commonly will direct the probe perpendicular to the surface (aiming at the patient’s mid-back) rather than toward the patient’s left shoulder. To visualize the heart from the subxyphoid position, the probe will assume a nearly horizontal plane. By positioning the transducer cord within the palm of one’s hand, it is easier to get to a horizontal position. If the common grasp of the probe positions the cord between the extensor surface of thumb and index finger, the heel of one’s hand may interfere with placing the probe in a horizontal plane.
Heart Borders. Another common pitfall is having the depth or range of the ultrasound system set too shallow. This leaves only a portion of the heart visualized. As with any ultrasound application, the organ of interest needs to have its borders defined. It is better to have the default setting of the depth or range set too far (with the organ of interest visualized in near field) than too shallow (with the organ of interest cut off in far field).
Fast Window No. 1 (Optional): Parasternal View of the Heart
In the optional parasternal view, the transducer is placed in the 4th or 5th intercostal space just left of the sternum. The probe is positioned perpendicular to the chest with the indicator directed toward the right shoulder. The sonographic landmarks of the parasternal window are the right and left ventricles of the heart, the left atrium, the aortic outflow tract, and the surrounding pericardium.
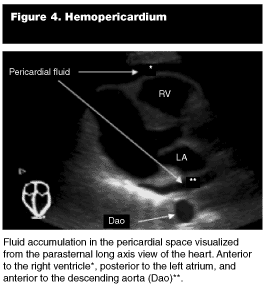
Pathological Findings. Hemopericardium. Sonographically, blood within the pericardial space will appear anechoic between the hyperechoic pericardium and the epicardium of the heart. This typically is best visualized inferior to the left ventricle. (See Figure 4.)
Pitfalls. Transducer Surface Position. The parasternal view can be difficult to obtain in a supine patient. Closely spaced ribs and lung interposed between the transducer and the heart challenge the sonologist. If the clinical situation permits, elevating the head of the bed and rolling the patient on his left side can aid in obtaining a better window. A phased array transducer (small footprint, electronically fired and steered), if available, can make tight spaces much easier to maneuver.
Image Interpretation. Occasionally, a large pleural effusion can mimic a pericardial effusion from a parasternal long axis approach. The key landmark is the descending aorta. (See Figure 4.) Fluid anterior to the descending aorta is in the pericardial space. Fluid posterior to the descending aorta is in the pleural space. As with any abnormality found on ultrasound, documentation in another plane strengthens the diagnosis.
Fast Window No. 2: Right Upper Quadrant (Morison’s Pouch)
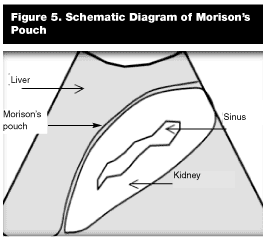
In the right upper quadrant view, the transducer is placed more or less between the 11th and 12th ribs in the mid-axillary line with the indicator of the probe directed toward the right axilla, slicing the body into a coronal plane. Depending upon the patient’s anatomy or body habitus, the probe might be positioned slightly more cephalad, caudal, anterior, or posterior to obtain the best window of Morison’s pouch. The sonographic landmarks of the right upper quadrant window are the liver, kidney, and diaphragm. (See the comparison view of schematic diagram, Figure 5.)
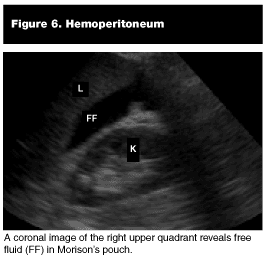
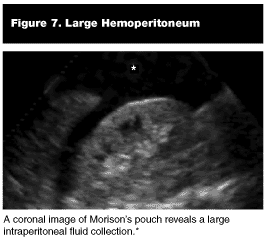
Pathological Findings. Hemoperitoneum. Blood within the abdominal cavity is sonographically apparent as an anechoic (jet black) region between the liver and right kidney. (See Figures 6 and 7.)
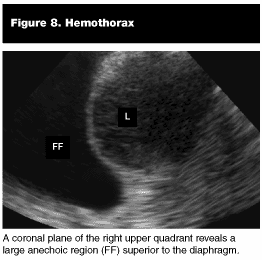
Hemothorax. Blood within the chest cavity is sonographically apparent as an anechoic (jet black) region superior to the diaphragm. (See Figure 8.)
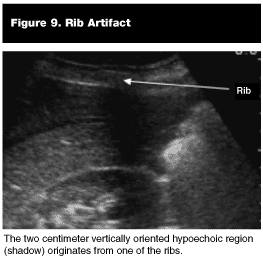
Pitfalls. Transducer Surface Position. Although a coronal plane is described above for the right upper quadrant view, ribs (see Figure 9) and gas commonly frustrate the novice sonologist. By rotating the probe so it lies parallel to the ribs within the intercostal space, nuisance shadow artifacts from the ribs can be excluded. Also, by utilizing the liver as an acoustic window, we can minimize the amount of attenuation (progressive weakening) the sound beam encounters in its round trip from the probe.
Fast Window No. 3: Left Upper Quadrant (Splenorenal View)
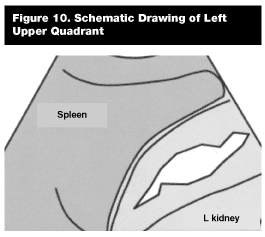
In the left upper quadrant view, the transducer is placed between the 10th and 11th ribs in the posterior-axillary line with the indicator of the probe directed toward the left axilla, slicing the body into a coronal plane. The sonographic landmarks of the left upper quadrant window are the spleen, kidney, and diaphragm. (See the comparison view of schematic diagram, Figure 10.)
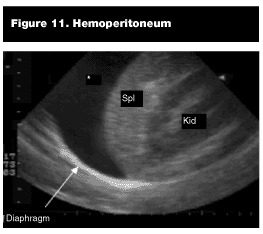
Pathological Findings. Hemoperitoneum. Blood within the abdominal cavity is sonographically apparent as an anechoic (jet black) region adjacent to the spleen either subdiaphragmatic or within the splenorenal recess. (See Figure 11). Occasionally, it can be isolated just inferior to the kidney in the paracolic gutter.
Hemothorax. Blood within the chest cavity is sonographically apparent as an anechoic (jet black) region superior to the diaphragm.
Pitfalls. Transducer Surface Position. In general, the inexperienced sonographer typically positions the probe at a level similar to that with which he had success in the right upper quadrant (11th intercostal space in mid-axillary line). Unfortunately, this frequently leads to poor image acquisition due to the location of the splenic flexor of the transverse colon and the stomach. When examining the left upper quadrant, the probe typically needs to be positioned more cephalad and posterior than the right upper quadrant window.
Fast Window No. 4: Pelvic (Suprapubic View)
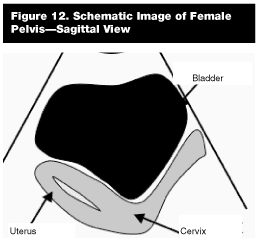
In the suprapubic view, the transducer is placed just superior to the pubic bone and tilted slightly caudal to visualize the true pelvis. The pelvis commonly is interrogated in both a longitudinal and transverse plane. Our initial choice is to start with a longitudinal approach and then move to a transverse plane. In the longitudinal view, the indicator of the probe directed toward the patient’s navel, slicing the body in a midline sagittal plane. To better understand the anatomy of the captured still image, imagine a frozen section of the patient’s body sliced in half from the nose through the perineum, and the right side of the body removed. If the remaining left side was visualized through a triangular frame over the pelvis, the left side of the screen would be toward the patient’s head and the right side toward her feet. The sonographic landmarks for the longitudinal suprapubic window of the pelvis are the bladder, uterus (or prostate), and rectum. (See comparison view of longitudinal suprapubic schematic diagram, Figure 12.)
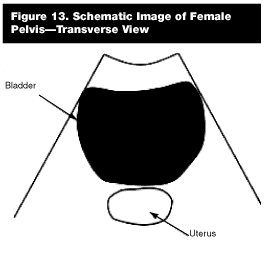
In the transverse view of the pelvis, the indicator is directed toward the patient’s right iliac crest, slicing the body into an axial plane. When viewing the image on the monitor, the left side of the screen represents the patient’s right side of the body, and the right side of the screen represents the patient’s left side (similar to CAT scans). The sonographic landmarks of the pelvis through a transverse window are the bladder and uterus or prostate. (See the comparison view of schematic diagram, Figure 13.)
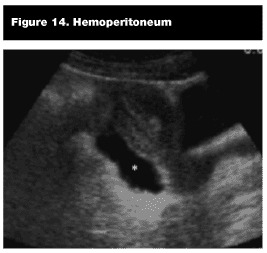
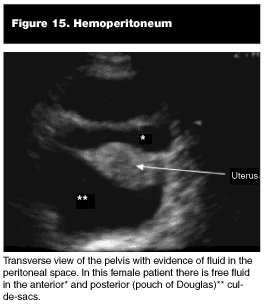
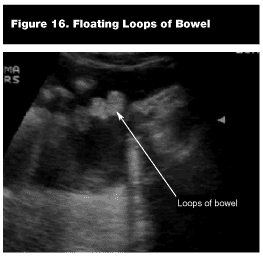
Pathological Findings. Hemoperitoneum. Blood within the pelvic cavity is sonographically apparent as anechoic (black) region between the rectum and uterus or prostate. (See Figure 14.) In the female patient, fluid also can be visualized between the uterus and bladder (anterior cul-de-sac). (See Figure 15.) Bowel commonly is found floating in fluid superior and posterior to the bladder. (See Figure 16.)
Pitfalls. Transducer Surface Position. The most common pitfall in the pelvic view is placing the transducer too superior to the pubic symphysis and not angling it inferiorly into the pelvis. If the bladder is full, it also will provide a better sonographic window into the pelvis.
Discussion
Utilization of bedside ultrasound by emergency physicians and trauma surgeons has the potential to improve patient outcomes at a lower cost. However, used inappropriately, it could paradoxically delay diagnosis if the unwary practitioner puts false reliance on a study that inherently lacks sensitivity or fails to show pathology because of the inexperience of the physician sonographer. Physicians utilizing bedside sonography must use it as one of several tools available in the evaluation of the trauma patient. Ultrasound examination of the heart and chest is highly sensitive in detecting pericardial fluid or hemothorax. Ultrasound examination of the abdomen is only about 80% sensitive in detecting free intraperitoneal fluid, and worthless in the search for intestinal perforations. However, sensitivities quoted in the literature are unlikely to be achieved by the novice sonographer. Consequently, the following approach is recommended for physicians wishing to add diagnostic ultrasound to their armamentarium:
1. Take a formal course designed for physicians initiating the use of bedside ultrasound in their emergency medicine practice. Such a course should cover basics of ultrasound, including some principles of physics and "knobology" (enough to assist in understanding the picture generated and how to improve it).
2. Perform bedside ultrasound on trauma patients as a part of the routine examination. However, during this "training phase," no disposition decisions should be based on the ultrasound exam. Rather, the novice sonographer should maintain a log in which he compares his findings on ultrasound with a concurrent gold standard study, such as CT scan or diagnostic laparotomy.
3. When the new sonographer has enough experience with the ultrasound machine such that she can perform a FAST exam in fewer than five minutes, and has a high concordance with concurrent studies, she is ready to incorporate this imaging modality into her trauma evaluation protocols.
The following protocols are recommended for the FAST examination:
1. All multi-trauma patients should receive a FAST examination as part of the initial assessment, if their vital signs permit. The FAST examination should not be performed on unstable patients with clinical indications requiring operative interventions.
2. Patients with positive findings on the FAST examination should have appropriate treatment or follow-up exams. For instance, a patient with penetrating trauma whose FAST examination shows a large pericardial fluid collection should be taken to the operating room for exploration and a pericardial window. Patients with blunt trauma and stable vital signs may undergo an abdominal CT after peritoneal fluid is demonstrated on the FAST examination. This will allow further delineation of the injury, which is helpful in determining the need for surgery.
3. Patients with stable vital signs and negative FAST studies should have further diagnostic studies based on other clinical criteria, such as mechanism of injury, past medical history, and findings on serial physical exams.
Finally, no discussion of ultrasound by a non-radiologist can ignore the politics of this situation. A jaded view would be that radiologists are the chief opposition to the use of ultrasound by emergency physicians and trauma surgeons because of the economic threat this paradigm shift poses. However, we are convinced the radiologists’ motive in voicing concerns is quality based. Emergency physicians and trauma surgeons who present a thoughtful plan for training and quality assurance are likely to find support from the administration, physician colleagues, and frequently the radiologist. The scope of the questions answered by the surgeon performing a FAST examination should be limited and dichotomous: "Is there pericardial fluid present? Is there free peritoneal fluid?" The savvy emergency physician or trauma surgeon will answer these questions only when the findings are clear. Patients whose exams are technically difficult or who have unclear findings will have their FAST examinations ignored with further testing performed in the radiology suite as clinically indicated. Taking this conservative approach will minimize any clinical errors while allowing many patients to benefit from the expedited care catalyzed by the performance of bedside ultrasound by the treating physician.
References
1. Gracias VH, Frankel HL, Gupta R, et al. Defining the learning curve for the Focused Abdominal Sonogram for Trauma (FAST) examination: Implications for credentialing. Am Surg 2001;67:364-368.
2. McKinney, KL. Ultrasound of blunt abdominal trauma. Radiol Clin North Am 1999;37:879-893.
3. Plummer D. Diagnostic ultrasonography in the emergency department. Ann Emerg Med 1993;22:592-594.
4. Bennett MK, Jehle D. Ultrasonography in blunt abdominal trauma. Emerg Med Clin North Am 1997;15:763-787.
5. Ingeman JE, Plewa MC, Okasinski RE, et al. Emergency physician use of ultrasonography in blunt abdominal trauma. Acad Emerg Med 1996;3:931-937.
6. Branney SW, Wolfe RE, Moore EE, et al. Quantitative sensitivity of ultrasound in detecting free intraperitoneal fluid. J Trauma 1995; 39:325-330.
7. Chiu WC, Cushing BM, Rodriguez A, et al. Abdominal injuries without hemoperitoneum: A potential limitation of focused abdominal sonography for trauma. J Trauma 1997;42:617-623.
8. Rozycki GS, Oschner MG, Feliciano DV, et al. Early detection of hemoperitoneum by ultrasound examination of the upper right upper quadrant: A multicenter study. J Trauma 1998;45:878-883.
9. Rozycki GS, Feliciano DV, Schmidt JA, et al. The role of surgeon-performed ultrasound in patients with possible cardiac wounds. Ann Surg 1996;223:737-744.
10. Plummer D. The sensitivity, specificity, and accuracy of ED echocardiography. Acad Emerg Med (abstract) 1995;2:339.
11. Akgur FM, Aktug T, Kovanlikaya A. Initial evaluation of children sustaining blunt trauma: Ultrasonography vs. diagnostic peritoneal lavage. Eur J Pediatr Surg 1993;3:278.
12. Akgur FM, Tanyel FC, Akhan O, et al. The place of ultrasonographic examination in the initial evaluation of children sustaining blunt abdominal trauma. J Pediatr Surg 1993;28:78.
13. Boulanger BR, McLellan BA, Brenneman FD, et al. Emergent abdominal sonography as a screening test in a new diagnostic algorithm for blunt trauma. J Trauma 1996;40:867-874.
14. Luks FI, Lemire A, St-Vil D, et al. Blunt abdominal trauma in children: The practical value of ultrasonography. J Trauma 1993;34: 607-610.
15. Hilty W, Snoey ER. Trauma ultrasonography. In: Simon BC, Snoey ER, eds. Ultrasound in Emergency and Ambulatory Care. St. Louis: Mosby;1997:151-189.
16. Mateer J, Plummer D, Heller M, et al. Model curriculum for physician training in emergency ultrasonography. Ann Emerg Med 1994; 38:879.
17. Branney SW, Moore EE, Cantrill SV, et al. Ultrasound based key clinical pathway reduces the use of hospital resources for the evaluation of blunt abdominal trauma. J Trauma 1997;42:1086-1090.
18. Greenberg MD, Rosen CL. Evaluation of the patient with blunt chest trauma: An evidence based approach. Emerg Med Clin North Am 1999;17:41-62.
19. Rozycki GS, Oschner MG, Schmidt JA, et al. A prospective study of surgeon-performed ultrasound as the primary adjuvant modality for injured patient assessment. J Trauma 1995;39:492.
20. Hoffmann R, Nerlich M, Muggia-Sullam M, et al. Blunt abdominal trauma in cases of multiple trauma evaluated by ultrasonography: A prospective analysis of 291 patients. J Trauma 1992;32:452-458.
21. Healey MA, Simons RK, Winchell RJ, et al. A prospective evaluation of abdominal ultrasound in blunt trauma: Is it useful? J Trauma 1996;40;6:875-885.
The Focused Assessment with Sonography in Trauma (FAST) is a bedside ultrasound examination used primarily by emergency physicians and trauma surgeons to identify free intraperitoneal, intrathoracic, or pericardial fluid. This article describes the sonographic acoustic windows and technique of the FAST examination.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
