Coding professionals don’t come a dime a dozen, so retention is key
Coding professionals don’t come a dime a dozen, so retention is key
In a coder’s market, incentives can help you get and keep good people
Jobs are in short supply in many industries throughout the country, but health care is looking for a few good workers — and not just nurses. Hospitals are finding it hard to locate and keep medical coders.
In fact, the national vacancy rate for billers and coders in 2001 was around 8.5%, according to the American Hospital Association. The Bureau of Labor Statistics projects that the number of medical records and health information management positions will grow by more than 36% by 2010.
Given the outlook for this job sector, recruiting and retaining quality coding professionals is essential. However, doing so in today’s tight labor market requires thoughtfulness, consistency, and investments of both time and money.
Step one is identifying suitable candidates. The process of taking a physician’s written notes regarding a patient’s diagnosis and treatment and converting that information into numeric code can be quite a challenge. "You have to have a good screening tool to identify the people who are appropriate for you to try to recruit into your organization," says Bill French, MBA, RHIA, CHQ, vice president of Madison, WI-based Metastar’s Hospital Payment Monitoring Program.
An applicant must be suited to a career that requires him/her to work quickly and accurately while relying on notes that may lack pertinent information. The absence of crucial information hinders the coder in his or her efforts to code properly, which reduces the coder’s productivity rate. Ascertaining that a coder has the ability to deal with problems in a positive way is important, French says.
Not surprisingly, a coder’s clinical background — or lack thereof — can be an issue during the recruitment process. "If you have clinical experience, it makes it easier to convert what you know medically to a code," says Steve Verno, CMBS, NREMT-P, CMMB, CMMC, compliance director for the Medical Association of Billers in Las Vegas.
Whether a coder’s prior experience comes from years of clinical training or years of coding, his or her resulting knowledge base is very attractive to health care employers. "The coder, typically, is in a health and information management department, which is typically not close to the source of patient care," says French. Having a good working knowledge of conditions and treatment modalities — whether the category is OB/GYN, emergency medicine, or radiography — can certainly help an employee code faster and more accurately.
Of course, there is always room for someone who has trained specifically as a coder. Darice Grzybowski, MA, RHIA, FAHIMA, encourages hospitals to "take an active role in recruiting students from local colleges and universities with HIM education programs." In addition, Grzybowski, who is National Industry Relations Manager for 3M Health Information Systems, recommends creating intern positions, so students will have some coding experience when they graduate.
Susan Cohen, RHIA, CCS, is responsible for both off-site and outsourced coding operations for Provider HealthNet Services (PHNS) in Allentown, PA. Among other services, PHNS provides coders, coding support, and auditing to hospitals. While Cohen says PHNS likes to recruit people from four-year programs, the firm also looks at nontraditional students if they have the right clinical background.
In particular, PHNS is always interested in people who have been nurses. Although she says PHNS "prefer[s] that employees go through a four-year program," hiring someone from a two-year coding program isn’t out of the question. "We would take someone with a two-year degree and mentor them" via testing, analysis/critique of the coder’s work, and continuing education, says Cohen. "Two-year programs give people a base — [they] learn the basics and the rules. A small community hospital would hire someone from a two-year program."
Grow your own
Two years ago, Baylor University Medical Center in Dallas faced a medical coder shortage: There were several vacancies and no people in the area to fill them. So the hospital created a six-month paid training program that has completely solved the shortage issue, says Dana Choate, RHIA, associate director for health information management at Baylor.
The program has seven spots each semester, she says. That number of spots was chosen because that was how many coder vacancies there were when the first class started. "We wanted to be out of hot water," she says. That was also the number that could be accommodated for the practical work experience part of the class, and it was the number for which Choate was able to justify the expense.
The first time the course was offered, there were 56 applicants. The second time, 83 people applied. By the third course, the hospital had 174 applications. With needs met for the time being, Baylor didn’t offer the course for two sessions. It is just getting ready to offer its fourth course.
"Initially, it was for people who worked in the hospital already and were looking for an opportunity to grow professionally but couldn’t afford to quit work and go to school." Aimed at clerical-level employees, the pay was higher than minimum wage, but about on a par with an entry-level administrative job, says Choate. The students also receive benefits.
Things have changed, however. Now, applications come in from across the country. "There are highly skilled individuals — nurses, nursing assistants, transcriptionists — who wanted to stay in health care but were looking for a different track," Choate says.
The course includes classroom work on medical terminology and ICD-9 and CPT codes, as well as classes in anatomy and pathophysiology. It also includes hands-on experience in a health information management department. "We think the work experience part of the class is critical to helping them understand what they will be doing in the real world," says Choate.
Those who make it to the course have to promise to work in the Baylor system for two years after graduation. The first graduates have now been at Baylor for more than two years and seem content to stay there, says Choate. "We even did some employee satisfaction testing with the students and asked if they would still be working here if they hadn’t had to sign the two-year agreement. The answer was an overwhelming yes."
Once the students complete the course, they are eligible to work toward an entry-level coding credential from the American Health Information Management Association (AHIMA) in Chicago, says Jessica Rudd, RHIA, coding instructor for the course. After coders have two or three years of experience, they can sit for a certified coding specialist exam.
The cost of the program wasn’t insubstantial, says Choate: some $300,000 for books, computers, salaries, and the cost of educational consultants to design the course.
Was it worth it? From an accounts receivable perspective, the ability to fill vacancies has allowed the hospital to drop some $2 million from outstanding A/R. In addition, there hasn’t been a real need to go looking outside the hospital for coders — something that would make many hospitals green with envy. "It was a risk," Choate says. "But it was definitely worth it."
Keep what you’ve got
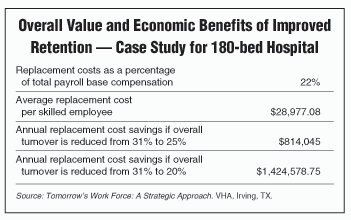
Turnover is costly, so why not keep the employees you have? (See chart depicting the cost of employee turnover at one hospital, below.) In order to keep good coders, employers must first understand why coders leave.
Coding can be very stressful, says Verno of the Medical Association of Billers. "Burnout is a problem. A lot of them have a tendency to burn out in a few years because [coding] is a monotonous task, and it’s difficult to read the charts sometimes," he says.
Additionally, money matters. According to AHIMA’s on-line membership profile information (data compiled beginning in 2001, representing more than 17,000 people), 42.5% of respondents make between $30,000 and $39,999 per year. Another 17.5% earned from $40,000 to $49,999, while 29.2% earned $20,000 to $29,999. Those who ranked in the $30,000 to $39,999 range were almost equally divided in their work settings among long-term care, physician offices, integrated delivery systems, and acute care hospitals.
"In the past, coders have not been highly paid, but coder salaries are becoming more competitive," says Grzybowski. "The minute you increase salaries, you’ll probably see improved retention."
But money alone won’t guarantee retention. "To keep coders, you’ve got to have a good environment," says Verno. "You’ve got to put them in a quiet room, keep them away from phones and interruptions so they can meet their quota," he says. "If you pay them a decent salary and give them a decent working environment, they’ll stay."
French suggests taking it one step further. "You have to provide some communication system for the coder — some intermediary to ask a question in such a way to get an answer from a physician. Not all coders are capable of or desirous of doing that," he says. Establishing a liaison between physicians and coders is like building a bridge between the clinical and health information management sides of the river. "It all boils down to a communication challenge," says French.
Grzybowski doesn’t stop there. To keep good coders, "offer flexible working hours," she says. "Many coders are parents, and many are single parents. Some flexibility in work schedules can create employee loyalty and improve retention and recruitment," she says. "Also, consider offering both part-time and full-time positions."
Telecommuting can be a viable option for coders as well. "There are all kinds of reasons to have at-home coding, but you have to extend the support system to that person working at home," French cautions.
"In some HIM organizations, especially those with electronic records, there may be an opportunity to establish a remote coding program and offer coders the alternative of coding from home," Grzybowski agrees.
The role of incentive
Cohen says part of her firm’s success is due to providing coders with various career options. "We don’t limit what coders can do: They may code, they may audit, they may take further training," she explains. "We have a nice ladder where somebody can move to a higher level based upon their performance." This tiered promotion apparatus gives employees a concrete way to build their careers.
PHNS invests in continual training programs to help employees ascend this internal career ladder. "We have an in-house training program," says Cohen. "It’s great for people to be mentored and receive training from highly seasoned coders."
Continuing education is an area that, while necessary, often gets cut when budgets are tight. "Many hospitals have been forced to cut back on travel budgets for coders to attend industry seminars, but there are less expensive alternatives for coder education," says Grzybowski. She mentions on-line courses, audio seminars, videos, and books as good sources of education. "Providing ongoing training is an important benefit that will help you retain and recruit coders," she says.
In addition to continual training opportunities, Cohen says hospitals should consider offering "a system of recognition for performance."
Grzybowski agrees. "As long as you balance coder productivity incentive programs with a continued emphasis on coding quality, there’s nothing wrong with having these programs in place," she says. "Give [coders] an incentive for high achievement as long as that achievement isn’t measured in increasing case mix,’ which can be interpreted as fraudulent upcoding," she warns.
Jobs are in short supply in many industries throughout the country, but health care is looking for a few good workers and not just nurses. Hospitals are finding it hard to locate and keep medical coders.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
