Dramatically reduce your surgical infection rates
Set goals for 100% compliance
Would you like to be able to boast that your organization performed hundreds of surgeries without a single infection or reduced rates of surgical infections dramatically? By making specific process changes, these impressive results can be achieved.
At Gwinnett Hospital in Lawrenceville, GA, 478 hysterectomy procedures were performed without a single infection over an 11-month period, and 71 colon procedures were performed without a surgical infection in a seven-month period.
"The mission was to achieve, in 13 months, a breakthrough improvement in surgical infection prevention through system redesigns using proven evidence-based practices," says Gwen Hudson, RN, BSN, CNOR, surgical services project operations manager.
By analyzing surgical practices and making comparisons with national best practices, Baptist Medical Center in Jacksonville, FL, was able to dramatically reduce the infection rates of postoperative coronary artery bypass graft surgery (CABG) patients. As a result, the organization received the JCAHO’s Ernest A. Codman award, which recognizes the effective use of performance measurement in improving health care quality.
In addition to improving patient outcomes, dramatic reduction of surgical infections is something an organization can really brag about, says Wendy Solberg, CHE, Gwinnett’s director of quality resources, pointing to coverage of her organization’s successes in local and national newspapers.
"It felt so wonderful to be able to show these amazing outcomes to our community so that when people come to our hospital, they feel safe," she adds.
Here are specific changes that were made at the organizations:
• A multidisciplinary team was formed, and goals were identified.
At Gwinnett, the first step was forming a multidisciplinary team with pharmacy, preoperative holding, operating room, anesthesia, infection control, post-anesthesia care, and members of the medical staff.
The team’s first action was to develop an aim statement, as follows: "To improve the quality of care for patients undergoing surgery at Gwinnett Hospital System by decreasing the surgical site infection rate by 25%. Changes will be tested on colon and hysterectomy procedures with the goal of spreading improvements to all surgical procedures."
The following goals were set:
- 100% of eligible patients will receive appropriate prophylactic antibiotics within one hour of the surgical incision time.
- 100% of prophylactic antibiotics will be discontinued within 24 hours after surgery.
- Perioperative systems of care to be redesigned include elimination of preoperative shaving, intraoperative oxygen delivery at a higher concentration, and maintenance of perioperative normothermia.
At Baptist Medical Center, the chiefs of cardiovascular surgery and infectious disease met with an infection control nurse and cardiovascular case manager to review infection rates, and all agreed that cardiovascular surgery infection rates should be evaluated for improvements.
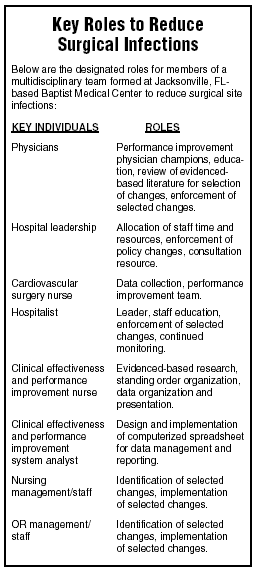
"We found opportunities that might improve outcomes of our patients and avoiding undesirable consequences like infection," says Missi Halvorsen, RN, BSN, senior consultant for JCAHO/regulatory accreditation. (See chart listing roles for the organization’s multidisciplinary team, below.)
The group found that cardiovascular surgery infection rates were above the Centers for Disease Control and Prevention’s (CDC) National Noso-comial Infections Surveillance System benchmark. Additionally, chest-cavity infection was identified as a problem, and preoperative antibiotic-to-incision time was greater than CDC recommendations. Three goals were identified: To decrease postoperative CABG surgical wound infection rates, decrease timing of prophylactic administration of antibiotics, and have zero cases of mediastinitis.
• System process changes were implemented.
At Baptist, the following baseline data were collected to identify areas of potential impact on infection rate: CABG postoperative wound infections, cases of mediastinitis, and observation of infection control aspects of care, including analysis of clinical practice in skin preparation, wound care, and antibiotic timing.
The clinical staff then identified and implemented five changes: Clipping rather than shaving hair for operative site preparation, infusion of insulin for 72 hours postoperatively to maintain blood sugars between 126-175 mg/dL, standardizing postoperative surgical wound care, reinforcing use of antibiotics to nares, and reducing antibiotic infusion-to-incision time to between 30 minutes to 60 minutes.
The resulting improvements in care led to a decrease in surgical wound infections and no cases of chest-cavity infections, Halvorsen states.
At Gwinnett, razors were replaced with clippers for preoperative hair removal, the concentration of oxygen delivery intraoperatively was increased, and appropriate prophylactic antibiotics were administered.
• Results were shared.
After the changes were implemented at Gwinnett, staff were informed whenever there was 100% compliance with any of the following: On-time administration of prophylactic antibiotics, appropriate selection of prophylactic antibiotics, patients with normal body temperature on arrival to post-anesthesia care unit, patients receiving > 80 fraction of inspired oxygen intraoperatively, patients with clippers utilized for preoperative hair removal, and antibiotics being discontinued within 24 hours after surgery.
"Positive results were shared at every opportunity," Hudson adds. "We posted results, education was reinforced, and enthusiasm for continuing improved patient care spread throughout the system."
• Initial goals were expanded to include additional populations.
Since the initial 13-month period, Gwinnett’s pilot population was expanded to include hip/ knee arthroplasty, vascular procedures, and ventral hernia repairs.
"It was our goal to spread to all surgical procedures within one year of the completion of this project, and we are well on our way to accomplishing this," Hudson says.
• The effectiveness of system changes are measured.
Ongoing monitoring is crucial, says Halvorsen. "Our project started in November of 2001 and is ongoing. We continue to collect the same data on each CABG patient to ensure we hold this gain," she says.
The key to ongoing success is a multidisciplinary team approach with strong physician leadership and involvement, Solberg notes.
"The team reviews the data and the practice patterns to improve our systems. These goals are also a component of our system quality goals that are tracked by our quality steering committee and our board’s quality and community health committee," she continues.
• Obstacles were identified and eliminated.
"The biggest surprises were the obstacles we encountered," Halvorsen says.
Problems in implementation of every system process change were addressed as they were identified, as follows:
1. Staff were resistant to clipping instead of shaving hair, so staff were re-educated and written orders for clipping were added to standing orders.
2. Baseline data revealed delays in preoperative antibiotic dosing when administered on the nursing unit. To reduce prophy- lactic antibiotic infusion to incision time to between 30 and 60 minutes, administration of antibiotic was moved from the patient’s room to the operating room and from nursing to anesthesiology.
3. To rectify problems with interdepartmental communication and data collection, meetings were held with all disciplines involved; letters were sent to OR, nursing, and anesthesiology departments; and standing orders were reworded.
4. For the goal of consistent administration of antibiotics to the nares, it was discovered that mupirocin was on national back order, and there was a problem getting agreement on acceptable substitutes. To resolve this, standing orders were reworded to specify acceptable substitutes.
5. Surgeons had different methodologies for postoperative wound care. To address this, there was standardization to one evidence-based practice, and this was added to the orders.
6. When changing from an insulin infusion for 72 hours postoperatively, as opposed to use of a sliding scale for treatment of elevated glucose levels, there was lack of staff familiarity with the new protocol. This led physicians to discontinue insulin drips prior to the 72-hour recommendation. "This was addressed with re-education of physicians and nurses about the new protocol," says Halvorsen.
[For more information about reducing surgical site infections, contact:
• Missi Halvorsen, RN, BSN, Senior Consultant, JCAHO/Regulatory Accreditation, Baptist Health, 1325 San Marco Blvd., #601, Jacksonville, FL 32207. Phone: (904) 202-4966. Fax: (904) 334-7628. E-mail: [email protected].
• Gwen Hudson, RN, BSN, Gwinnett Health System, 1000 Medical Center Blvd., Lawrenceville, GA 30045. Phone: (678) 442-4692. E-mail: [email protected].
• Wendy H. Solberg, CHE, Gwinnett Hospital System, 1000 Medical Center Blvd, Lawrenceville, GA 30045. Phone: (678) 442-3439. Fax: (770) 682-2247. E-mail: [email protected].]
Would you like to be able to boast that your organization performed hundreds of surgeries without a single infection or reduced rates of surgical infections dramatically? By making specific process changes, these impressive results can be achieved.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
