ECG REVIEW
Does the AV Block Get Worse?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
This article originally appeared in the December 15, 2013, issue of Internal Medicine Alert. It was edited by Stephen Brunton, MD, and peer reviewed by Gerald Roberts, MD. Dr. Brunton is Adjunct Clinical Professor, University of North Carolina, Chapel Hill, and Dr. Roberts is Senior Attending Physician, Long Island Jewish Medical Center, NS/LIJ Health Care System, New Hyde Park, NY. Dr. Brunton serves on the advisory board for Abbott, Amarin, Boehringer Ingelheim, Duchesnay, Janssen, Lilly, Novo Nordisk, Sunovion, and Teva; he serves on the speakers bureau of Boehringer Ingelheim, Janssen, Lilly, Novo Nordisk, and Teva. Dr. Roberts reports no financial relationship to this field of study.
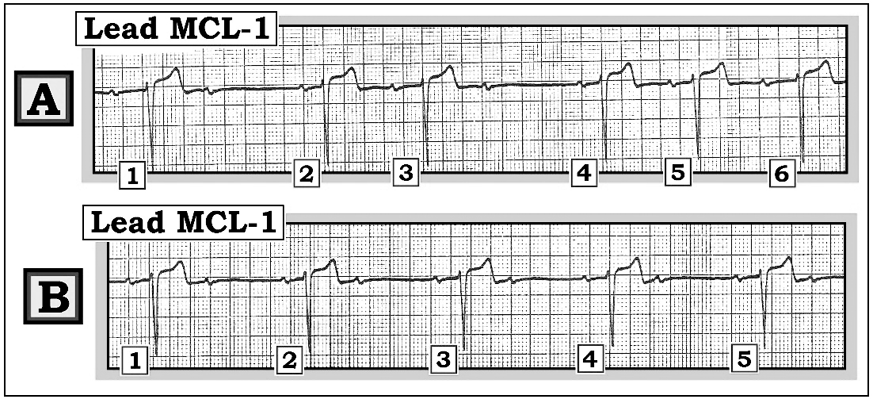
Figure — Sequential tracings from a patient with syncope.
Scenario: Imagine the ECG tracings shown above were sequentially obtained from a patient with syncope. What kind of atrioventricular (AV) block is present in each tracing? Does the degree of AV block worsen from tracing A to tracing B?
Interpretation: Beginning with tracing A, there is group beating. The QRS complex is narrow. Underlying sinus arrhythmia is present. The PR interval progressively increases within each group until a beat is dropped. This is second-degree AV block, Mobitz Type I (AV Wenckebach).
In tracing B obtained a little while later on this same patient, the overall ventricular rate has slowed. The QRS complex is again narrow. Now, only one out of every two P waves is conducted to the ventricles. Every other P wave does conduct — as evidenced by the constant (albeit slightly prolonged) PR interval preceding each QRS complex. This is second-degree AV block with 2:1 AV conduction.
Although at first glance one might think that the degree of AV block in tracing B has become "worse," this is not the case. Note that the underlying atrial rate is faster in tracing B than it was in tracing A. Thus, only one out of every two P waves is able to penetrate the AV node when the atrial rate is 80-85/minute — whereas a greater percentage of P waves penetrate in Tracing A when the atrial rate is slower (in the 60-70/minute range).
Distinction between Mobitz I vs Mobitz II second-degree AV block is not possible from inspection of tracing B alone. Because there is never conduction of two consecutive P waves in a row, we simply cannot tell if the PR interval would prolong if given a chance to do so. This distinction is important because Mobitz II usually requires treatment with pacing, whereas Mobitz I does not. That said, it is probable that tracings A and B both represent Mobitz I because: 1) Mobitz I AV block is far more common than Mobitz II; 2) the QRS complex is narrow (whereas Mobitz II usually manifests QRS widening; 3) the PR interval for beats that conduct in Tracing B appears to be long (more common with Mobitz I); and 4) it is rare for a patient to switch back-and-forth between Mobitz I and Mobitz II conduction defects, and we know that Tracing A clearly manifests Mobitz I AV block.

