New tools to anticipate disasters, epidemics, flu outbreaks
April 1, 2014
Reprints
Related Articles
-
Walking at Work: A Helping Hand for a Healthier Heart
-
Examining the Effects of Cannabis on the Heart
-
Lifestyle Interventions and HbA1c in Prediabetic Patients
-
Rapid Reversal of Anticoagulation Reduces Mortality from Intracerebral Hemorrhage
-
Outcomes Are Better for Acute Stroke Patients Who Arrive Rapidly at Endovascular-Capable Centers
New tools to anticipate disasters, epidemics, flu outbreaks
Hospital and ED leaders understand that regular practice drills and pre-planning are critical to facilitating an effective response when disasters or serious infectious disease outbreaks occur. And now they have three new tools at their disposal to help them better forecast what resources and staffing would be needed to deal with several different disaster scenarios, given their own unique regional and facility characteristics.
Executive Summary
Researchers at the Johns Hopkins National Center for the Study of Preparedness and Catastrophic Event Response (PACER) in Baltimore, MD, have unveiled three new web-based tools that hospitals, EDs, and public health authorities can use to help them prepare for surges related to disasters, epidemics, and seasonal flu outbreaks.
- The prediction models, including EMCAPS 2.0, Surge, and FluCast, are designed to give health care administrators a better idea of anticipated patient volumes as well as the number and types of injuries that are likely to result from specific disaster scenarios.
- The web-based tools are being made available free of charge. Users just need to register and establish an account on the PACER website.
- Further refinements to all three tools are planned as user feedback is collected and results are assessed.
Figure 1: PACER Website
The tools were developed by researchers at the Johns Hopkins National Center for the Study of Preparedness and Catastrophic Event Response (PACER) in Baltimore, MD, and they are being made available for free through a PACER applications suite website. (See Figure 1) Interested users just need to register and establish an account to access the applications.
The new tools, which were unveiled in February at the U.S. Department of Homeland Security’s University Centers of Excellence Innovation Showcase in Washington, DC, include:
• EMCAPS 2.0: An update to the Electronic Mass Casualty Assessment and Planning Scenarios program;
• Surge: An application designed to help individual hospitals or units within hospitals determine surge capacity and the potential impact of various surge response strategies;
• FluCast: A program that can help EDs predict how many flu patients they are likely to see in a given week based on their own hospital’s historical data, as well as information collected by Google Flu Trends, a web-based tool that gauges regional influenza activity by monitoring Internet-based searches for flu information.
Access EMCAPS via the web
Whereas the first version of EMCAPS was a downloadable file, EMCAPS 2.0 is now part of PACER’s web-based suite of applications, so it can be accessed from anywhere a user has access to the web, explains Lauren Sauer, MS, PACER’s program manager. "It is immediately more robust. We have added a lot of evidence behind the scenarios," she explains. "We have also added three or four new [disaster] scenarios, so we now have 11 disaster scenarios that have been identified as risk areas by [the U.S. Department of] Homeland Security."
Figure 2: EMCAPS

For instance, users of the EMCAPS 2.0 tool can now model disasters related to several different types of explosions, food contamination, toxic gas, the nerve agent sarin, anthrax, pneumonic plague, pandemic influenza, and mustard gas. (See Figure 2 on p. 41.) The new EMCAPS tool was developed by a team led by Jim Scheulen, PA, MBA, a PACER researcher and executive director of the Johns Hopkins Office of Critical Event Preparedness and Response.
Sauer notes that the user interface for EMCAPS 2.0 has been significantly improved, making the tool more user-friendly and visually oriented. "We have visuals on the EMCAPS home screen of each event," she explains. "The inputs are easier to enter and the outputs are a lot more graphical, nicer looking, and cleaner. They have more information associated with each scenario."
Further, all the assumptions and other information required to run a particular scenario are now readily available to the user, so there is no need for the kind of digging that users used to have go through to model a disaster using the first version of the tool, notes Sauer.
For example, for one of the explosion scenarios, users would see all the different types of injuries anticipated and the different health care and first-responder decision-making information associated with those injuries in a table up front, observes Sauer. "On top of that would be a black diagram showing the radius of impact of the blast and a representative image that reflects what the casualties and injuries associated with the blast would look like."
Also, EMCAPS 2.0 has been updated with the latest census data so planners can run simulations based on fairly accurate population densities for their regions or cities. "It is a dynamic and easy-to-use tool that makes it especially beneficial for planning, training, and education," adds Sauer.
Further, Sauer stresses there will be additional refinements. "We are constantly updating the literature and the evidence behind the scenarios, so that is always our next step," she says. "Additionally, we would like to see an iPhone or iPad application in the future, and we have had discussions about making a downloadable file of the new version of EMCAPS. And on top of that, we are talking about linking EMCAPS with Surge to create a really robust picture of a disaster for a health care setting."
Use Surge to determine/add capacity
The Surge application was developed by Gabor Kelen, MD, FACEP, FAAEM, FRCP(C), the founding director of PACER and professor and chair of the Department of Emergency Medicine at Johns Hopkins University. He describes the tool as being complementary to EMCAPS 2.0.
"The EMCAPS tool helps predict the kind of surge you might expect in a given catastrophic event or disaster, and it can be tailored to your local area," he explains. "The Surge tool gives a region, hospital unit, or even an individual ward the ability to determine what your capacity actually is to absorb victims, and then you get to play with various maneuvers in order to create incremental capacity."
Surge can be scaled to distinguish between an intensive care unit and a general floor or some other space. "You can do bed planning at a regional level, at multiple hospitals, an entire system, or you can look at just burn units in metropolitan New York," says Kelen.
Further, whereas EMCAPS may be more of a planning tool, Surge can be used for planning as well as in the heat of the moment to quickly determine capacity. For instance, in the case of a mass emergency, EMS systems typically call around to see how many patients a hospital can accept. "With Surge, you would know [the answer] in a matter of minutes, if not seconds, because you would have your basic data pre-loaded," says Kelen. In addition, hospitals would be able to report how quickly they could create more capacity by using the Surge tool to assess the impact of different space-creating maneuvers, he says.
"We know [Surge] works pretty well in terms of the mechanics of it. We tested it in old-fashioned algorithmic ways to see that it actually does what it is supposed to do, and we used data from our five hospitals to get a sense," says Kelen. "We used national data as well. We used data from real live disasters and we modeled out and simulated in other programs the reality of freeing up beds."
Also embedded in the tool are algorithms comprised of surge-related research data pertaining to how quickly beds can be freed up and what the contributions are of various techniques for adding bed capacity. "For all of these kinds of products, they are only as good as the fixed assumptions that are put in, so we have made [those] fairly robust," observes Kelen.
While Surge is embedded with some fixed assumptions, it also enables users to adjust these inputs so that they are more closely in line with specific, local circumstances. "We allow you to open up the hood and tinker with the data," says Kelen. "You get to do quite a few inputs even in the off-the-shelf product."
For example, users can input such data as average length-of-stay (LOS) for patients, how many transfers come in, and the typical distribution of admissions from ED transfers. "You get to put in those kinds of [data points], as opposed to us determining them, although there is also an off-the-shelf version of assumptions," explains Kelen. "However, it doesn’t take a lot of sophistication to open up the hood and play with [the data]."
As with the two other applications that PACER has unveiled, further refinements are planned for Surge, so that the tool can more comprehensively consider needed staffing as well as resources when making determinations about capacity. "We have done a considerable amount of work looking at a number of these different disaster scenarios and determining what supplies are required over a period of time to take care of any given patient who is burned or has anthrax poisoning or who is perhaps a victim of a mass casualty bombing," says Kelen. "We can put those kinds of variables into the model, and the same thing can be done with nurse and physician staffing."
With this added data, hospital or ED administrators could determine whether they could meet their standards of care if they opened up beds or whether they would have to relax their standard of care, and by how much, notes Kelen. "There are a lot more variables to put in. The algorithms become much more complicated this way but you can always go back to the plain vanilla version, which is kind of what we have now, as sophisticated as the tool already is," he says.
Stay ahead of flu outbreaks
Every year, EDs across the country struggle with how to stay one step ahead of patient surges from influenza. FluCast is designed to help them do just that by essentially estimating the number of flu patients a specific hospital is likely to see in a given week based on the facility’s own historical data and information from Google Flu Trends, an Internet-based tool that monitors search traffic related to influenza.
FluCast was developed by a team led by Richard Rothman, MD, PhD, a professor and vice chair for research in the Department of Emergency Medicine at Johns Hopkins, and Andrea Dugas, MD, an assistant professor in the Department of Emergency Medicine. For the past two years, they have been testing and fine-turning the prediction model underlying the application, but now they are ready for EDs to put it to use across the country.
"Our hospital epidemiology and infection control office has begun running some forecasts. We’re looking forward to seeing how [the tool] performs," explains Rothman. "We don’t yet know how many EDs will take this up, but we will work with various national emergency medicine organizations to disseminate the tool and should be able to see if and how others, both locally and nationally, may benefit from using it in the future."
Figure 3: Flu Statistics from FluCast
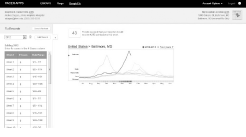
FluCast is very easy to use, adds Rothman. "It basically just requires having your weekly flu census," he says. "The first time log-on may require 20 to 30 minutes, with weekly updates taking just a minute or two to be able to see your local prediction." (See Figure 3)
Rothman acknowledges that developers don’t yet have a systematic way to measure the impact of the tool, but they are planning to work with various agencies to devise a method for assessing impact in the future. He also anticipates a process that will include continual improvements. "We will use the web tool to monitor how often it is used and then solicit feedback from selected users," he says. "Comparing predicted versus observed trends will allow us to refine the model as needed."
Editor’s note: Hospitals and ED administrators can access the new tools via the PACER website at www.pacerapps.org.
Sources:
- Gabor Kelen, MD, FACEP, FAAEM, FRCP(C), Founding Director, Johns Hopkins National Center for the Study of Preparedness and Catastrophic Event Response (PACER), and Professor and Chair, Department of Emergency Medicine, Johns Hopkins University, Baltimore, MD.
E-mail: [email protected]. - Lauren Sauer, MS, Program Manager, Johns Hopkins National Center for the Study of Preparedness and Catastrophic Event response (PACER), Baltimore, MD. E-mail: [email protected].
- Richard Rothman, MD, PhD, Professor and Vice Chair for Research, Department of Emergency Medicine, Johns Hopkins University, Baltimore, MD. E-mail: rrothma1
@jhmi.edu.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
