Leaving against medical advice: Should you take no for an answer?
By Catherine A. Marco, MD, FACEP, Associate Professor, Surgery, Medical College of Ohio; Attending Physician, St. Vincent Mercy Medical Center, Toledo; Arthur R. Derse, MD, JD, FACEP, Director of Medical and Legal Affairs and Associate Director, Center for the Study of Bioethics, Clinical Professor of Bioethics and Emergency Medicine, Medical College of Wisconsin, Milwaukee.
Editor’s note: Litigation involving patients leaving against medical advice is an interesting entity that our legal system has created. In a country that places such a high value on personal freedoms and individual choice, it would seem that if a patient makes a decision, he should be responsible. Unfortunately, that is not the case. Only after a patient has been informed of the risks, benefits, and alternatives can the providers be absolved of liability. Even then, crafty lawyers representing disgruntled family members, bring claims against the medical profession and hospitals. Proper documentation and recording conversations with family members and patients will reduce the potential risk. This month’s issue of ED Legal Letter will discuss the medicolegal risks to the physician, nurse, and hospitals associated with a patient leaving against medical advice (AMA) and provide strategies to prevent patients from leaving.
The Doctrine of Informed Consent
Since early in the last century, consent has been a legal requirement for medical treatment of a patient who has the capacity to make medical decisions.1 The doctrine of informed consent is a fundamental principle of the U.S. legal system, first established by case law in 1957.2 The term delineates both the necessity of voluntary choice by the patient for treatment, and the information that must be disclosed to the patient before the patient agrees to undergo the proposed treatment or procedure. Concomitantly, patients with decisional capacity also may refuse a proposed treatment or procedure. Informed consent and refusal of treatment are recognized as significant legal and ethical rights of patients.3 All adults with decisional capacity have the legal right to consent to medical care, or to refuse it.4 Although physicians possess the ability to make diagnoses and recommend treatment, it is presumed the patient is most capable of deciding whether the proposed interventions are compatible with his/her value system and goals.
Informed consent for procedures represents one of the most fundamental rights of patient autonomy in medical decision making.5-10 Many routine emergency department (ED) procedures, such as establishing intravenous lines and drawing blood, are performed with general consent to treatment, agreed to orally or in writing by all competent ED patients.
Other more invasive procedures absent an emergency should be performed following a discussion with the patient regarding the nature of the procedure, purpose, risks and benefits, and alternatives.11-13 However, compliance with informed consent discussions and documentation of informed consent varies widely.14
Three basic types of informed consent are recognized:
1. Express consent — the granting of authority to render treatment.
2. Implied consent — consent derived from the conduct of the person (e.g., a patient who holds his arm out for blood drawing implies his consent to the procedure, even though it has not been expressed verbally).
3. Consent implied in law (e.g., emergency treatment is indicated to save life or preserve health, for patients unable to give consent in life-threatening situations).
There are several notable exceptions to the duty to obtain informed consent. In emergent situations, when immediate treatment is indicated to prevent death or serious harm to the nondecisional patient, and no one is legally authorized to consent, interventions should not be delayed to obtain informed consent. Other exceptions to the duty to obtain informed consent include: patients who waive their right to consent, patients for whom the information would be so traumatic as to impair their ability to consent (the rarely used therapeutic privilege), and public health or legal requirements.
Numerous situations exist in which the best course of action is unclear. When uncertain, the best approach probably is to act in what is believed to be the patient’s best interest. The courts typically view favorably actions of a physician or nurse who acted reasonably, in accordance with the patient’s best interest and the standard of care.
State law varies somewhat concerning details of informed consent, particularly as applied in emergency situations. Knowledge of the law of the state in which the physician or nurse practices is paramount to the appropriate provision of medical care within the law.
Disclosure, Documentation in Consent Process
The duty to obtain informed consent falls upon the physician who will be performing the procedure.15,16 Similarly, the physician involved should assume responsibility for the discussion of the risks involved, if the patient refuses medical recommendations or plans to leave against medical advice.
How much information should be presented to patients regarding a proposed intervention? Certainly, sufficient information to weigh the risks and benefits should be presented. However, a plethora of information may be confusing or even intimidating to patients.
The reasonable person standard of disclosure suggests that sufficient information should be disclosed that would be material to a reasonable person to make a decision in that particular instance. Although most states favor the reasonable person disclosure, some states utilize the professional standard, which suggests that the physician should disclose what other physicians in the community would disclose in similar circumstances. The law requires disclosure of material risks, those that would be considered significant for decision making by a reasonable person. Remote risks, or commonly known risks, need not be disclosed in every case.
Informed consent is a process, primarily comprising the discussion between the physician and patient and the patient’s agreement to the proposed intervention. The piece of paper with signatures does not equal informed consent and cannot substitute for the discussion; however, it does provide evidence of the patient’s written indication that the informed consent process did take place. The consent form may be admitted as evidence in court of the patient’s understanding and agreement, but it also may be rebutted by other testimony that the informed consent process did not take place.
Informed Refusal
Equally important to the principle of patient autonomy is the competent patient’s right to refuse medical care. This right of refusal — even for life-sustaining medical treatment — has been recognized by state courts, based in the law of battery,17 and by the U.S. Supreme Court based in the liberty interest of the 14th Amendment of the Constitution.18 Refusal of care may occur at several levels, including general treatment, hospital admission, or specific tests or therapies. However, certain circumstances may override this right to refuse medical care, such as suicidal ideation, threats to other parties, and public health risks. Even though decisional patients have a right to refuse medical care, there is a corresponding responsibility on the part of the physician to inform the patient of the risks and consequences of refusal.19
As with informed consent, informed refusal is a process, not merely a signature on a form documenting that the patient is leaving AMA. The process should consist of determination of decisional capacity (e.g., Can the patient understand the consequences?), delivery of information, including risks of refusing treatment, and documentation of the process.
When a patient refuses indicated medical treatment, great care should be taken that the patient understands the consequences, and that if the patient should have a change of mind, the physician stands willing to treat the patient. A witness to the discussion can be helpful to later attest to the facts of the interaction.
Though every recommendation a patient chooses to refuse should be accompanied by an informed refusal discussion, an AMA form need not accompany every refusal. Reasonable patients may decline recommended medical care in many situations (e.g., the patient with a facial wound who refuses sutures). However, not every patient who can make medical decisions will choose what the reasonable patient would choose. In a case where the dangers to the patient’s health from refusal are great, and a reasonable patient would follow the course of action that the physician recommends (e.g., treatment and hospitalization for a probable myocardial infarction), but a particular patient who is decisional is not following the physician’s recommendation, an AMA form can act as an important document. It can represent the gravity of the refusal to the physician and the information that the patient understood before refusing treatment.
Assessing Decisional Capacity
In most clinical situations, emergency physicians (EPs) have little difficulty determining a patient’s implicit ability or competency to participate in the emergency medical decision-making process. In many cases, however, the precise determination of adequate capacity to make significant medical decisions can be very challenging. The assessment of medical decision-making capacity is an important and basic skill for EPs. Capacity is essential to the processes of informed consent and informed refusal of treatment.20-22
Definition of Decisional Capacity
Decisional capacity refers to a patient’s ability to make an authentic choice. Capacity reflects cognitive and affective functions, which are clinically manifest in intellect, memory, judgment, insight, language, attention, emotion, calculation, and expressive and receptive communication skills. Decisional capacity includes the following abilities:
1. Receive information
2. Process and understand information
3. Deliberate
4. Make and articulate a choice
Unlike the more static entity of legal competency, decisional capacity varies, as a function of host and environmental factors over time. Thus, capacity is a dynamic, task-specific, and changing talent; in practice, it may be assessed on a spectrum of capacity, pertaining to the particular health care decisions at hand. Impairment often is situational; the same patient may have the capacity to make one decision and not another, depending upon the gravity and consequences of the decision and the potential for harm. In emergency situations, physicians must promptly assess whether a patient is capable of making a decision.
Determination of Decisional Capacity
Although a thorough discussion of all medical decisions in the ED is impossible, patients participate more fully in the therapeutic ED encounter and in the decisions that affect their health when they possess adequate capacity to make medical decisions. In most clinical scenarios, capacity is easily and implicitly ascertained. In others, the EP may utilize a more standardized approach to capacity determination, particularly when the decisions involve potentially grave or serious consequences. A stepwise approach may be taken toward determination of decision-making capacity.23 Essential elements are summarized in Table 1.
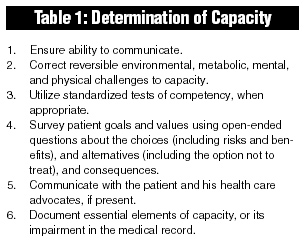
Standardized tests may be valuable in the determination of capacity.24-31 One example of a standardized test that is administered easily in emergency medicine is the Mini-Mental Status Examination (see Table 2).32
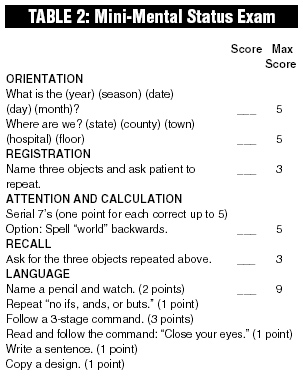
Another is the formulation by the President’s Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research (the Commission) and is one that is well recognized and useful.33
Elements of Capacity Determinations
Simply put, in assessing a patient’s ability to make a decision regarding health care, one must evaluate three elements of the capacity to make health care decisions: First, the patient must possess the ability to comprehend the information about the medical problem as well as to appreciate the effect of the disease and the consequences of various options for treatment, including forgoing treatment. Second, the patient must possess the ability to evaluate the options by comparing risks and benefits of each option, to deliberate in accordance with the patient’s own values, and to make choices that are not irrational. The patient also should be able to maintain a consistent choice over time. Third, the patient should be able to communicate his or her choice.
Each of these elements can be delineated further. First, the patient must possess a set of values and goals, including a framework for comparing options and the ability to make reasonably consistent choices. Second, the patient must have the ability to communicate and to understand information, including the ability to give and receive information; the possession of linguistic and conceptual skills needed for at least a basic understanding of the relevant information; and sufficient life experience to appreciate the meaning of potential alternatives. Third, the patient must have the ability to reason and to deliberate about one’s choices, including the ability to compare the impact on alternative outcomes on personal goals and life plans, some ability to employ probabilistic reasoning about uncertain outcomes, and the ability to give appropriate weight in a present decision to various future outcomes.34
That analysis may at first look to be a daunting standard by which to be measured even for those who have full decision-making capacity. However, the Commission recommended that the measurement of decisional capacity not be absolute, but rather measured by a sliding scale. "Generally, determination of the capacity to decide on a course of treatment must relate to the individual abilities of the patient, the requirements of the task at hand, and the consequences likely to flow from the decision. Thus, when the consequences for well-being are substantial, there is a greater need to be certain of that the patient possesses the necessary level of capacity."35 When a decision to forego treatment could result in death, the need to be certain that the patient has decision-making capacity is greatest.
A lack of decision-making capacity may be caused by any break in the chain of decision making: the ability to understand, to reason and evaluate, and to communicate a decision. Obviously, patients in a coma, infants, and the profoundly mentally disabled lack decision-making capacity for all medical decisions. Some other patients, such as those at the end of life with metabolic abnormalities, disorientation, or early dementia, though impaired to a certain extent, may yet retain some degree of decision-making capacity.
Thus, decision-making capacity has two seemingly contrary characteristics. Decision-making capacity has characteristics of a continuum36 (i.e., a sliding scale that relates to the complexity, importance, and consequences of the decision in relation to the patient’s abilities). The more grave the decision, the higher the standard. Yet, in the final analysis, at a given point in time, for a given patient, with a specific health care decision to make, it is all or none: A patient either has the capacity to make a specific health care decision or does not.
Pitfalls in the Determination of Capacity37
Clinicians may fall prey to many misconceptions in the determination of capacity. Following are some aspects to consider.
1. Capacity isn’t an all-or-nothing phenomenon. Capacity is a dynamic, task-specific, and changing phenomenon; in practice it may be assessed on a spectrum of capacity, pertaining to the particular health care decisions at hand. Often, impairment is situational; the same patient may be competent for one decision and not for another, depending upon the gravity and consequences of the decision and the potential for harm. In emergency situations, physicians must assess promptly whether a patient is capable of making the particular decision at hand.
2. Legal competence is not the same as medical decision-making capacity. Though competence and incompetence are commonly used terms, they have specific meanings as legal terms. Technically, a patient remains legally competent until a court says otherwise. A court of law may determine a patient to be incompetent and appoint a guardian to make important decisions for the patient, including those concerning health care. However, many patients who have not been declared incompetent by a court nonetheless have problems with their ability to make health care decisions. Clinicians often are faced with patients who never have been declared incompetent by a court, and either have questionable decision-making capacity or, as in the case of the comatose patient, have no decision-making capacity at all.
3. Capacity is not consistent over time. Numerous threats and barriers to capacity exist, many of which are reversible, or may change over time.38 Although an in-depth review of causes of altered mental status is beyond the scope of this issue, some examples of challenging clinical settings may include minors;39,40 elderly patients; patients with dementia;41,42 intoxicated patients; psychiatric patients; patients of other cultures or languages; patients with physical communication impairments, severe pain, or organic disease states;43,44 research subjects; and numerous other clinical settings. Even in such circumstances, where some impairment of capacity may be suspected, a sliding-scale approach should be used, remembering that most barriers are relative, rather than absolute. EPs must be aware of potential barriers to capacity, but must make an individual assessment of capacity relevant to the specific clinical setting and decision at hand.45-47 Even individuals who have some impairment of capacity may demonstrate adequate understanding of the decision at hand, and its ramifications, to make an appropriate informed choice. Every effort should be made to correct reversible etiologies of diminished capacity.
4. Blood alcohol level does not predict competence. A blood alcohol level test has limited utility in the determination of capacity.48 Although the blood alcohol level may be useful as a baseline comparison in some circumstances, the clinical effects of alcohol are so variable as to make the absolute level relatively unreliable in predicting mental status or capacity.
Some patients whose blood alcohol level is zero may be impaired in decision-making capacity due to other intoxicants or disorders. Other patients whose blood alcohol level would not allow them to legally operate a motor vehicle still may be able to agree or refuse to accept medical treatment or to express important personal values about that treatment.
5. Capacity does not only need to be assessed when patients refuse recommended treatment. Although the importance of capacity seems heightened when a patient refuses recommended therapy, in reality, it is equally important to ensure capacity when patients accept or reject any therapy recommended to them.
In all medical encounters, health care providers are making some judgment of this capacity. For those encounters where capacity is at issue, a formal judgment should be made. Physicians caring for ED patients should consider the patient’s decision-making capacity before presenting the patient with significant health care decisions.
6. Psychiatric disorders do not preclude having decisional capacity. Although the existence of a psychiatric disorder may be important information to the physician who is assessing capacity, a psychiatric diagnosis per se does not rule out adequate decisional capacity. Many psychiatric patients are managed adequately with appropriate therapy and may participate actively in health care decisions. A patient who is depressed and actively suicidal lacks the ability to make medical decisions, while a schizophrenic patient who is compliant with a medication regimen may be able to make important medical decisions. In many states, patients who are not an immediate danger to themselves or others may have the right to refuse psychotropic medications unless ordered by a court.
7. Mental health professionals are not the only qualified personnel to determine capacity. Although psychiatrists and psychologists are trained specifically to assess mental status and capacity, any EP should regularly determine capacity in his/her patients, and in any case, the EP may be ultimately responsible for making judgments about the decision-making capacity of ED patients.
8. Minors are not able to provide consent or refuse. By legal definition, minors (younger than 18 years in most states) are not competent to make major health care decisions. Many states give adolescent minors limited autonomy; they specifically may be allowed to obtain contraception or treatment for venereal disease or substance abuse without parental permission. In many states, minors who are married or living independently and supporting themselves are considered to be emancipated minors and competent to make their own health care decisions. Moreover, developing case law on the mature minor now recognizes that as the adolescent’s age increases toward maturity, he or she should have a progressively greater part in the decision-making process for important medical decisions. Thus, a 17-year-old facing acute leukemia might have a great part in the decision-making process about whether and how to treat the disease.
9. Avoid an overly paternalistic approach to decision making. Simply disagreeing with the physician’s recommended course of action does not render a patient incompetent. Too often, physicians are guilty of becoming defensive or condescending when a patient who possesses adequate capacity disagrees with the recommended treatment. Statements such as, "You have to be admitted!" or "You could DIE if you leave!" are not amenable to a positive interaction and are unlikely to successfully change the patient’s opinion. As stated above, reasonable patients can make choices against the advice of the physician. The physician should make an effort to understand the patient’s reasons for the choice rather than assuming all choices made contrary to advice show a de facto incapacity.
When Decisional Capacity is Impaired
When an EP has established that impairment of decision-making capacity exists, and that the emergency exception to informed consent does not apply, the next step is to identify a surrogate decision maker. In some cases, a patient may have executed a legal document that identifies a surrogate and outlines specific instructions. That document could be in the form of a health care power of attorney or other advance directive. Where the patient has identified a surrogate, disclosure and consent should involve that individual. In the absence of such identification, consent usually is sought from close family members. Not all states give close family members the authority to make health care decisions for an incapacitated patient. However, even if family members do not have legal authority to make decisions, physicians often turn to them for input, because eventually, and in most cases, a family member would be appointed legal guardian for the patient. However, some states have codified the next-of-kin hierarchy of health care decision makers for incapacitated patients. To the extent that the care needed is more urgent, the physician’s responsibility to seek out, inform, and obtain consent from a surrogate may be lessened.
It is important to recognize, however, that the emergency exception to informed consent will not override a formerly decisional patient’s previously expressed wishes regarding care. A physician who knows, for example, that a patient would refuse treatment cannot wait until an emergency exists and then proceed without consent. Nonetheless, honoring patient-centered values suggests that once the course that optimizes patient safety and interests is identified, it should be initiated, despite possible objections from either the decision-impaired patient or others. However, when clinicians must act for the benefit of the patient over the nondecisional patient’s objections, they should strive to share decision-making power by involving the patients and their representatives as much as possible. When a surrogate makes decisions for an incapacitated patient, the basis for decision should be one of the following:
1. Substituted Judgment. This is the guideline the surrogate uses if the patient has expressed a preference before becoming incompetent, or if the surrogate knows the patient’s preferences well enough to determine what the patient would choose if he or she still were decisional.
2. Best Interest. This is the standard the surrogate must use when he or she has no clear evidence of what the patient might choose. It is what is best for this particular patient in these particular circumstances. The best interest test does not always mandate treatment. For instance, a patient’s legal guardian might refuse life-sustaining treatment based upon the patient’s best interest in the light of the diagnosis, prognosis, and medical goals of treatment.
Patients Who Leave AMA
Studies have identified varying incidences of patients leaving against medical advice. Inpatient studies have shown that 1-7% of patients leave against medical advice.49,50 Psychiatric inpatient units may experience AMA rates of 5-35%. ED studies have demonstrated rates of 0.1-3.5%.50,51 Pre-hospital refusal rates often are higher and may represent 5-30% of EMS calls.52-55
Numerous studies have identified factors associated with patients who leave against medical advice, including male gender, young age, history of alcohol abuse, history of drug abuse, history of psychiatric diagnosis, lack of medical insurance, non-Caucasian ethnicity, previous history of leaving AMA, and comorbidities.56-66
Several studies have demonstrated higher death rates, higher rates of future admission, and higher resource utilization among patients who leave against medical advice.67-74
A recent study of out-of-hospital refusal of care demonstrated that of 5.1% of patients who refused transport, 3% of those patients required a subsequent EMS dispatch within one week, 20% had a subsequent ED visit, 2% were hospitalized, and a measurable, but small, mortality rate of 0.0001%, primarily among the pediatric and geriatric populations.75
Among elderly patients who refuse initial EMS transport, the majority (70%) seek follow-up care, and a significant percentage (32%) required hospital admission at follow-up. Interestingly, many (49%) elderly patients who refused transport indicated that they would have complied with transport had a physician suggested it.76
Among minors whose parents refuse EMS transport, the majority (84%) complied with follow-up, but only 11% required hospital admission, due to respiratory or cardiac complaints.77
Results of several studies showed that the reasons for leaving AMA include family pressures or responsibilities, financial concerns, drug/alcohol dependence, feelings of panic, anger, personality disorders, wish for treatment elsewhere, phobic feelings, fear of pain, and fear of serious diagnosis.78-81
EMTALA Issues
The Emergency Medical Treatment and Labor Act (EMTALA) and its subsequent regulations require certain expectations when patients refuse medical screening, treatment, stabilization, or transfer.82 The burden of proof is on the institution to demonstrate that the patient voluntarily refused evaluation or treatment. Patients also may voluntarily refuse evaluation and treatment even after initially consenting. Voluntary withdrawal of the patient’s request for evaluation and treatment is recognized as a valid reason to discontinue further evaluation or treatment.
Institutions should attempt to avoid long waiting times that may lead patients to leave prior to evaluation (leaving without being seen [LWBS]). Hospitals should attempt to determine and document why patients leave prior to evaluation, and ensure that they are aware that the hospital is willing to provide a medical screening examination.83
Hospitals should have policies to document findings and practices for LWBS patients. For example, the staff may call the patient, check the waiting area three times, and document the patient’s absence. That action may be followed by physician review, and if appropriate, attempts to contact the patient to advise a return for evaluation. Those actions should be documented in the medical record.
In addition to concerns about the patient’s well-being, hospitals also should be concerned about medicolegal ramifications, including possible EMTALA violations and leaving AMA before a medical screening exam, or before treatment or stabilization. Patients should be informed of their rights to a medical screening examination, appropriate determination of capacity should be performed, risks and benefits should be explained to the patient, written refusal should be obtained if possible, and documented by the physician and a witness if the patient is unwilling to sign a refusal. Alternative sources of medical care should be identified and offered to the patient, as well as an expression of the willingness to provide the patient medical care should the patient return.
Other Issues in the Process of Consent
Some patients may refuse a medical intervention because of religious reasons. The example of adult Jehovah’s Witness patients who refuse blood transfusions is commonly known.84 Such patients, if deemed to have appropriate decisional capacity, can refuse treatment, even if it results in an adverse outcome, including death. However, parents do not have the legal authority to impose their own religious beliefs on their children to the detriment of their physical health. If parents do not consent to necessary emergency life-saving interventions for their children, it is appropriate to treat the child over the parents’ objections, at the same time seeking a court order for legal authorization.
Depending upon state law, some patients may be held for mandatory medical treatment, despite their refusal. Examples may include treatment for tuberculosis or other infectious diseases.
Unlike adults, who generally are deemed capable of making their own decisions, regardless of outcome, minors generally do not have this right. Under most circumstances, the right to consent or refuse care belongs to the parents of a minor. In some circumstances, the state does not allow parents to deny appropriate emergency medical care to children, under the doctrine of parens patriae, which refers to the state’s interest in the well-being of the child. According to this doctrine, physicians can and should treat emergency medical conditions of minors, even if the parents object.85,86 Some states have specific laws that address the procedural aspects of this practice. In general, a court order should be obtained, if it would not inappropriately delay treatment. However, if parents refuse treatment of a nonemergent condition, the parents’ wishes generally should be respected. In cases where the parents’ refusal constitutes child neglect, it should be reported to the appropriate authorities.
Emancipated minors may consent to or refuse their own medical care. The definition of emancipated minor varies by state, but typically includes minors who are or have been married, who are pregnant or are parents, or minors who live independently of their parents.
Mature minors are those who are intellectually and emotionally mature enough to comprehend the risks and benefits of the proposed treatment. In many states, mature minors are able to consent to or refuse their own medical care.
Reducing Legal Risk
Medicolegal concerns arise when treating patients who wish to leave against medical advice. It has been estimated that one in 300 AMA-discharged patients will file related lawsuits. However, a recent review of case law and the medical literature found few cases in which health care providers were sued (all unsuccessfully) for malpractice despite AMA discharge.87
Emergency physicians often wonder whether they should provide any care or treatment for patients who leave AMA, wondering if no treatment is better than an incomplete treatment. For example, if a patient with a diagnosed closed fracture that requires surgical reduction refuses treatment but asks for pain medication to take for the pain, a physician might think it better to refuse to apply a splint or provide pain medication, because the patient has refused medical advice. The concern is that it would appear to be giving substandard medical treatment rather than the standard of care. However, measures for patient comfort or health that the patient will accept should be provided with a statement to the patient that this treatment is not optimal treatment, but is only the treatment the patient will allow.
Provision of the best clinical care possible despite the patient’s refusal and making sure that appropriate documentation is made may provide the best medicolegal protection.88,89 (See Table 3.) Improved communication regarding waiting times, availability of expedited treatment for minor complaints, and telephone follow-up may improve patient compliance with medical evaluation and follow-up.90,91

Conclusion
Emergency physicians often encounter patients who refuse medical evaluation and treatment. When treating such patients, physicians should communicate calmly and in a nonconfrontational manner. Decisional capacity should be evaluated, and if appropriate, the physician should communicate with the patient regarding his concerns, and goals and values of therapy. If the patient possesses appropriate decisional capacity, understands the risks and benefits of the proposed intervention and refusal, and voluntarily chooses to refuse the intervention, the patient should be allowed to refuse medical care. The patient encounter and important aspects of the communication should be documented in the medical record. The best possible medical care under the circumstance should be provided in all cases.
Endnotes
1. Schloendorff v. Society of New York Hospital, 211 NY 125 (1914).
2. Salgo v. Leland Stanford Jr. Univ. Bd. of Trustees, 154 Cal. App. 2d 560, 578, 317 P.2d 170 (1957).
3. Meisel A, Kuczewski M. Legal and ethical myths about informed consent. Arch Intern Med 1996;156:2521-2526.
4. In re Farrell, 108 N.J. 335, 529 A.2d 404 (1987).
5. Prentice ED. Informed consent. The most important protector. Acad Emerg Med 1999;6:774-775.
6. Moskop JC. Informed consent in the emergency department. Emerg Med Clin N Am 1999;17:327-340.
7. Hansson MO. Balancing the quality of consent. J Med Ethics 1998;24:182-187.
8. Young Jr. WF. Informed consent. Ann Emerg Med 1997;30: 350-351.
9. Etchells E, Sharpe G, Walsh P, et al. Bioethics for clinicians: Consent. CMAJ 1996;155:177-180.
10. Faden RR, Beauchamp TL, King NMP. A History and Theory of Informed Consent. New York City: Oxford University Press; 1998, pp. 7-9.
11. Moskop, supra note 6, at 331-334.
12. Borak J, Veilleux S. Informed consent in emergency settings. Ann Emerg Med 1984;13:731-735.
13. Meisel, supra note 3.
14. Braddock CH, Edwards KA, Hasenberg NM et al. Informed decision making in outpatient practice: Time to get back to basics. JAMA 1999;282:2313-2320.
15. Davis v. Charles Gen. Hosp., 598 So.2d 1244 (1992).
16. Canterbury v. Spence, 464 F.2d 772 (D.C. Cir 1972).
17. Wons v. Public Health Trust of Dade County, 500 So.2d 679 (Fla.App. 3 Dist. 1987).
18. Cruzan v. Director of Missouri Department of Health, 497 U.S. 261, 110 S.Ct. 2841, 111 L.Ed.2d 224 (1990).
19. Truman v. Thomas, 27 Cal. 3d 285, 611 P.2d 902, 165 Cal.Rptr 308 (1980).
20. Meisel A, Roth L. What we do and do not know about informed consent. JAMA 1981;246:2473-2477.
21. Moskop, supra note 6.
22. Borak, supra note 12.
23. Drane J. Competency to give an informed consent: A model for making clinical assessments. JAMA 1984;252:925-927.
25. Tomoda A, Yasumiya R, Sumiyama T, et al. Validity and reliability of structured interview for competency incompetency assessment testing and ranking inventory. J Clin Psychol 1997;53:443-450.
25. White BC. Competence to Consent. Washington, DC: Georgetown University Press; 1994, pp. 154-184.
26. Markson LJ, Kern DC, Annas GJ, et al. Physician assessment of patient competence. J Am Geriatr Soc 1994;42:1074-1080.
27. Appelbaum P, Mirkin S, Bateman A. Empirical assessment of competency to consent to psychiatric hospitalization. Am J Psychiatry 1981;138:1170-1176.
28. Bean G, Nishisato S, Rector NA, et al. The psychometric properties of the competency interview schedule. Can J Psychiatry 1994;39:368-376.
29. Kaufman DM, Zun L. A quantifiable, brief mental status examination for emergency patients. J Emerg Med 1995;13:449-456.
30. Grisso T, Appelbaum PS. Comparison of standards for assessing patients’ capacities to make treatment decisions. Am J Psychiatry 1995;152:1033-1037.
31. Grisso T, Appelbaum PS. Assessing Competence to Consent to Treatment: A Guide for Physicians and Other Health Professionals. New York City: Oxford University Press; 1998, pp. 17-30.
32. Folstein MF, Folstein SE, McHugh PR. "Mini-mental state": A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975;12:189-198.
33. President’s Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research. Making Health Care Decisions, Vol. 1. Washington, DC: U.S. Government Printing Office; 1992, pp. 55-68.
34. Id.
35. Id.
36. Freer J. Decision making in an incapacitated patient. J Clin Ethics 1993;4:55-58.
37. Ganzini L, Volicer L, Nelson W, Derse A. Pitfalls in Assessment of Decision-Making Capacity. Psychosomatics 2003; 44:237-243.
38. Dresser R, Whitehouse PJ. The incompetent patient on the slippery slope. Hastings Cent Rep 1994;24:6-12.
39. Tsai AK, Schafermeyer RW, Kalifon D et al. Evaluation and treatment of minors: Reference on consent. Ann Emerg Med 1993;22:1211-1217.
40. Jacobstein CR, Baren JM. Emergency department treatment of minors. Emerg Med Clin N Am 1999;17:341-352.
41. Fellows LK. Competency and consent in dementia. J Am Geriatr Soc 1998;46:922-926.
42. Rockwood K, Stadnyk J. The prevalence of dementia in the elderly: A review. Can J Psychiatry 1994;39:253-257.
43. Marson DC, Ingram KK, Cody HA, et al. Assessing the competency of patients with Alzheimer’s disease under different legal standards. Arch Neurol 1995;52:949-954.
44. Derogatis L, Morrow G, Fetting J, et al. The prevalence of psychiatric disorders among cancer patients. JAMA 1983;249:751-757.
45. Beachamp TL, Childress JF. Principles of Biomedical Ethics, 4th ed. New York City: Oxford University Press; 1994, pp. 138-141.
46. Derse AR, Rosen P, Friedman JB. Consent: Explicit and presumed. In: Iserson KV, Sanders AB, Mathieu D, PhD, eds. Ethics in Emergency Medicine, 2nd ed. Tucson, AZ: Galen Press Inc.; 1995, pp. 95-98.
47. Larkin GL, Marco CA, Abbott JT. Emergency determination of decision making capacity (DMC): Balancing autonomy and beneficence in the emergency department. Acad Emerg Med 2001;8:282-284.
48. Marco CA, Kelen GD. Acute Alcohol Intoxication. Emerg Med Clin North Am 1990;8:731-748.
49. Jones AA. Leaving a county hospital against medical advice. JAMA 1979;242:2758.
50. Duno R, Pousa E, Sans J, et al. Discharge against medical advice at a general hospital in Catalonia. Gen Hosp Psychiatry 2003;25:46-50.
51. Dubow D, Propp D, Narasimhan K. Emergency department discharges against medical advice. J Emerg Med 1992;10:513-516.
52. Lee TH, Short LW, Brand D, et al. Patients with acute chest pain who leave emergency departments against medical advice: Prevalence, clinical characteristics and natural history. J Gen Intern Med 1988;3:21-24.
53. Hipskind JE, Gren JM, Barr DJ. Patients who refuse transportation by ambulance: A case series. Prehospital Disaster Med 1997;12:278:283.
54. Stark G, Hedges JR, Neely K et al. Patients who initially refuse prehospital evaluation and/or therapy. Am J Emerg Med 1990;8:509-511.
55. Moss ST, Chan TC, Buchanan J, et al. Outcome study of prehospital patients signed out against medical advice by field paramedics. Ann Emerg Med 1998;31:347-350.
56. Duno, supra note 50.
57. Jones, supra note 49.
58. Corley MC, Lunk K. Men patients who leave a general hospital against medical advice: Mortality rate within six months. J Stud Alcohol 1981;42:1058-1061.
59. Saitz R, Ghali WA, Moskowitz MA. Characteristics of patients with pneumonia who are discharged from hospitals against medical advice. Am J Med 1999;107:507-509.
60. Aliyu ZY. Discharge against medical advice: Sociodemographic, clinical and financial perspectives. Int J Clin Pract 2002;56:325-327.
61. Krakowski AJ. Patients who sign against medical advice. Psych J Univ Ottawa 1985;10:254-259.
62. Link K, Brody CE, Chan J. Leaving a medical service against advice. Va Med 1983;110:100-102.
63. Pages KP, Russo JE, Wingerson DK, et al. Predictors and outcome of discharge against medical advice from the psychiatric units of a general hospital. Psychiatr Serv 1998;49:1187-1192.
64. Anis AH, Sun H, Guh DP, et al. Leaving hospital against medical advice among HIV-positive patients. CMAJ 2002;167:633-637.
65. Jeremiah J, O’Sullivan P, Stein MD. Who leaves against medical advice? J Gen Intern Med 1995;10:403-405.
66. Bradbury RC, Golee JH, Steen PM. Comparing uninsured and privately insured hospital patients: Admission severity, health outcomes and resource use. Health Serv Manage Res 2001;14:203-210.
67. Hwang SW, Li J, Gupta R, et al. What happens to patients who leave hospital against medical advice? CMAJ 2003;168:417-420.
68. Corley, supra note 58.
69. Pages , supra note 63, at 1187-1192.
70. Weingart SN, David RB, Phillips RS. Patients discharged against medical advice from a general medicine service. J Gen Intern Med 1998;13:5685-5671.
71. Moss, supra note 55, at 247-250.
72. Sainsbury SJ. Emergency patients who leave without being seen: Are urgently ill or injured patients leaving without being seen? Mil Med 1990;155:460-464.
73. Hwang, supra note 67.
74. Anis, supra note 64.
75. Knight S, Olson LM, Cook LJ et al. Against all advice: An analysis of out-of-hospital refusals of care. Ann Emerg Med 2003;42:689-696.
76. Vilke GM, Sardar W, Fisher R, et al. Follow-up of elderly patients who refuse transport after accessing 9-1-1. Prehosp Emerg Care 2002;6:391-395.
77. Seltzer AG, Vilke GM, Chan TC, et al. Outcome study of minors after parental refusal of paramedic transport. Prehosp Emerg Care 2001;5:278-283.
78. Krakowski AJ. Patients who sign against medical advice. Psych J Univ Ottawa 1985;10:254-259.
79. Dubow, supra note 51.
80. Selbst SM. Leaving against medical advice. Ped Emerg Care 1986;2:266-268.
81. Vilke, supra note 76.
82. EMTALA 1986, Emergency Medical Treatment and Labor Act. 42 U.S.C. §1395dd(e)(2). (1986), Interim Final Rule with Comment Period, 50 Fed. Reg. 32086 (1994).
83. 64 Fed Reg 36070, 61353, 61359 (1999).
84. Wons, supra note 17.
85. George GE. Law and Emergency Care. St. Louis: CV Mosby; 1980, pp. 48-50.
86. Bergen CC. Legal aspects of emergency department pediatrics. In: Fleisher G, Ludwig S, eds: Textbook of Pediatric Emergency Medicine. Baltimore: Williams & Wilkins; 1983, pp. 1201-1209.
87. Devitt PJ, Devitt AC, Dewan M. An examination of whether discharging patients against medical advice protects physicians from malpractice charges. Psychiatr Serv 2000;51:899-902.
88. Id.
89. Devitt PJ, Devitt AC, Dewan M. Does identifying a discharge as "against medical advice" confer legal protection? J Fam Pract 2000;49:224-227.
90. Arendt KW, Sadosty AT, Weaver AL et al. The left-without-being-seen patients: What would keep them from leaving? Ann Emerg Med 2003;42:317-323.
91. Strinko JM, Howard CA, Schaeffer SL. Reducing risk with telephone follow-up of patients who leave against medical advice or fail to complete an ED visit. J Emerg Nurs 2000;26:223-232.
This months issue of ED Legal Letter will discuss the medicolegal risks to the physician, nurse, and hospitals associated with a patient leaving against medical advice and provide strategies to prevent patients from leaving.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
