Pneumococcal Pneumonia — Bring Back the Microbiology Laboratory!
Pneumococcal Pneumonia—Bring Back the Microbiology Laboratory!
Abstract & Commentary
Synopsis: When it is possible to obtain an adequate sputum specimen in a timely fashion, the sensitivities of Gram stain and culture in the diagnosis of pneumococcal pneumonia in bacteremic patients are high.
Source: Musher DM, et al. Diagnostic Value of Microscopic Examination of Gram-Stained Sputum and Sputum Cultures in Patients with Bacteremic Pneumococcal Pneumonia. Clin Infect Dis. 2004;39:165-169.
Musher and colleagues in Houston examined the usefulness of examination of Gram-stained sputum specimens and of sputum culture for the diagnosis of pneumococcal pneumonia. They included all 105 patients with bacteremic pneumococcal pneumonia seen over 6 years at their VA hospital, and examined the results of the first sputum specimen submitted to the laboratory. A sputum specimen was adequate if there were at least 10 WBC for each epithelial cell. A positive sputum Gram stain (predominant Gram-positive cocci in pairs and chains) was detected in 33 (31%), and a positive culture in 46 (44%) of the patients. However, no sputum was submitted from 31 patients, and in 16, the sample was judged inadequate. When these cases are excluded from analysis, the sensitivity of the Gram stain was 57%, and that of culture was 79% (see Table 1, below).

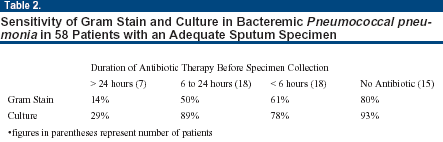
Antibiotic therapy prior to specimen collection significantly decreased the sensitivities of both Gram stain and culture (see Table 2, below). The sensitivities of Gram stain and culture, when sputum was obtained prior to antibiotic administration, were 80% and 93%, respectively. There was a marked decrease in sensitivities when specimens were obtained 24 hours or more after the initiation of antibiotic therapy.
Comment by Stan Derensinski, MD, FACP
A number of studies, many published in pulmonology journals, have reported that sputum Gram stain and culture are ineffective in the diagnosis of pneumococcal pneumonia. This has led to recommendations by organizations such as the American Thoracic Society, that attempts at microbiologic diagnosis not be performed in patients with community acquired pneumonia. As, however, pointed out by Musher et al, the studies upon which those recommendations were based, commonly included in their denominator patients, from whom no adequate sputum specimen was obtained. The current study demonstrates that sputum examination and culture are effective in the diagnosis of pneumococcal pneumonia and, if the specimen is obtained within a reasonable time after the initiation of antibiotic therapy, quite sensitive.
Since this study only examined patients with bacteremic pneumococcal pneumonia, it provides no information regarding the specificity of the Gram stain, nor does it examine its accuracy in the diagnosis of bacterial pneumonia of other etiology. Musher et al cite publications that suggest that Gram stain is even more effective in these diagnoses.
The current IDSA guidelines for treatment of community-acquired pneumonia call for the administration of a first dose of antibiotic within 4 hours of registration, a tactic associated with improved outcomes in hospitalized patients. Thus, the need to obtain an adequate sputum sample must not delay the initiation of empiric therapy beyond that time point. If an adequate specimen cannot be obtained before the first dose of antibiotic is given, Musher et al suggest that "microscopic evaluation of a Gram-stained sputum sample is likely to be useful within the first 6 to 12 hours of therapy, and a culture may provide useful data using a sputum sample obtained up to 24 hours after antimicrobial therapy has been begun." Although not discussed in this article, the urinary antigen test for Streptococcus pneumoniae may also be diagnostically useful.
Stan Deresinski, MD, FACP Clinical Professor of Medicine, Stanford; Associate Chief of Infectious Diseases, Santa Clara Valley Medical Center, is Editor for Infectious Disease Alert.
Musher and colleagues in Houston examined the usefulness of examination of Gram-stained sputum specimens and of sputum culture for the diagnosis of pneumococcal pneumonia. They included all 105 patients with bacteremic pneumococcal pneumonia seen over 6 years at their VA hospital, and examined the results of the first sputum specimen submitted to the laboratory.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
