2004 Salary Survey Results: Incentives are a growing trend in emergency department pay, link seen to pay for performance
2004 Salary Survey results
Incentives are a growing trend in emergency department pay, link seen to pay for performance
Physicians and nurse managers in emergency medicine stand a better change of boosting their income through incentive packages, as opposed to straight salary increases, according to industry observers. And if you did receive a significant salary boost in the past year, chances are you’re an ED nurse manager — not a physician manager.
"The biggest trend I’m seeing is incentive income," says Barbara Katz, who heads a Tampa, FL-based emergency medicine consulting firm specializing in ED physicians that bears her name.
In general, more administrative teams are giving incentives to nurse directors with bonus structures tied to performance targets, adds Diana S. Contino, RN, MBA, CEN, CCRN, a consultant with MedAmerica, an Oakland, CA-based medical practice support company for emergency services, and owner of Emergency Management Systems, a Laguna Niguel, CA-based consulting firm that specializes in staffing issues.
Where can such incentive structures be found? "It really depends on hospital leadership and if they subscribe to the pay-for-performance concept," Contino notes.
"Some facilities are increasing director incentives if they reach their goals and targets for such items as budget, staffing productivity, and supply expenses," she explains.
However, Katz adds, "You can have an incentive structure in any environment — even in academics." Structures for emergency physician managers vary widely, she says, but in general, they are based on finding ways to increase the income into the department.
Incentives and disincentives
Incentives for relative value units (RVUs), or the amount of billing, is the most common denominator for incentive programs, Katz points out, adding that hospitals are a bit behind groups when it comes to incentives for directors or managers.
"The big national groups can sometimes pay very high administrative stipends and create different kinds of incentives — not always based on clinical billing," she explains. "They could be based on an increased census over the past year, or quality assurance."
Many packages also involve disincentives, she notes. "If you have a doc seeing 4.5 patients per hour but not doing the documentation properly, that can impact the incentive."
At many large hospitals, says Katz, department directors may receive an administrative stipend on top of their clinical annual salary; in most of those cases, if there is an incentive program in place for physicians, they would not take part in that.
However, she adds, "This doesn’t rule out the possibility of a smaller hospital with lower volume, say 15,000-18,000, where the director is putting in as much clinical time as the rest of the staff; in which case, they would probably have the opportunity to take part in an incentive program."
Here is one model for an incentive package, offered by Katz: "Let’s say you’re in Tampa, and you’re earning $90 an hour," she poses.
"Incentives are based on a formula of 50% billing, 15% citizenship — monthly meetings, getting involved with committees — 15% could be based on documentation, how well and how quickly the charts are done. Then, the last 20% could be director’s discretion: Do you play well with others?’ Are there complaints from patients, family, nurses?" she asks.
The incentive bonus might then be set up so that each bonus point represents "X" dollars an hour — higher or lower, Katz explains.
For nurse managers, incentives and pay for performance structure vary from organization to organization, says Contino. Some are a straight percentage of the amount the department is under budget, she says.
"Others are structured as a total pool of money, say $10,000, and the director receives 20% for turnover rates at less than 5%, 20% for meeting budget, 20% for filling all positions, 20% for achieving departmental operational goals, and 20% for a successful accreditation survey," she notes.
"Others are just based upon meeting your budget targets, and the director receives the total pool of money set aside for bonuses."
Who received pay raises?
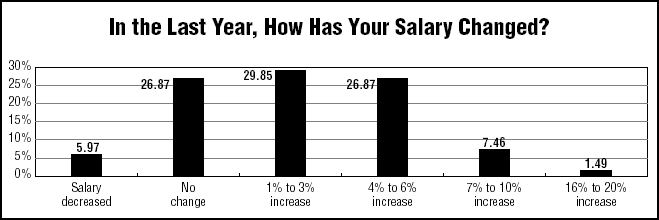
Most ED physician and nurse managers did receive an increase in the past year, although huge raises were rare. According to the ED Management 2004 Salary Survey, nearly two-thirds of the respondents (65.67%) received salary increases.
Of that total, 26.87% of the respondents had increases of between 4% and 6%, and 29.85% had increases of between 1% and 3%. Another 26.87% reported no change in their salary. (See chart, below.)
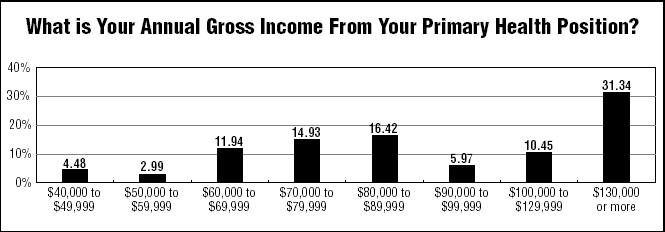
The survey was mailed in July to 1,108 subscribers. There were 67 responses, for a response rate of 6.5%.
Nearly one-third of respondents (31.43%) reported gross income of $130,000 or more. The second largest grouping was the $80,000-$89,999 range (16.42%), followed by $70,000-$79,999 (14.93%).
Still, for ED physician managers, "salaries are not going up," Katz asserts. The malpractice crisis has decimated the industry, she says.
"You wake up one morning, and your premium has increased 800% overnight; but that money is not going to come from the hospital." Increasingly, Katz adds, hospitals are starting to regard malpractice premiums as part of their total physician compensation — "and this includes department managers," she asserts.
Disparities seen in wages
There is a big disparity in physician manager salaries from state to state, but apparently no rhyme or reason, Katz says. "A physician in Maine will earn half what the same guy in the same ED in Texas is earning, and some of highest cost-of-living locations have the lowest salaries," she says.
The highest dollars are to be earned in Texas and Louisiana, Katz notes. In Odessa, TX, for example, an ED physician can earn three times as much as one on the Oregon coast — for example, $400,000 vs. $140,000.
Also near the top of the salary ladder are parts of the Midwest, northern Illinois, parts of Indiana, Minnesota, and Wisconsin, then small pockets in Kansas, she explains.
"Then, parts of the Southeast are scrambling to catch up, with South Carolina being one of the highest in the region," Katz continues "The Northeast is really working very hard to get their bucks up because they are one of the most expensive places to live, and they are climbing close to the Southeast."
And what about California, which is known for its high cost of living? "That depends," she explains. "It’s a huge HMO state, so it depends on the process for earning income, whether a group offers partnership potential, and so on." If you are a director of a group, as opposed to a hospital, you will make more money, Katz adds, noting that some small groups also rotate directorship.
Location sometimes can draw recruits to areas where compensation is lower, "but they still can’t underpay," she asserts.
Katz adds that she doesn’t see salaries for emergency physician managers improving anytime soon. "I do not see anything major in terms of increases in the next five to 10 years unless we are able to stabilize malpractice issues," she says.
Experience alone not enough
Experience alone may not be enough to earn the bigger bucks, note observers, and as the EDM Salary Survey shows, having years of experience does not necessarily set you apart from the competition.
Nearly 30% of the survey respondents have worked in the field for 10 or more years, and 13.43% have worked in the field for 16-18 years. Another 10.45% have been in the profession for seven to nine years. (See chart, below.)
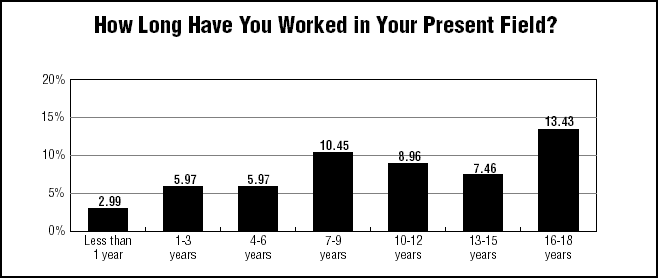
But industry organizations such as the Emergency Nurses Association (ENA) are seeking to help nurse directors complement their years of experience with management-specific skills, which in turn, they hope, will increase their value in the marketplace.
"Traditionally, nurse directors are promoted because they are wonderful clinicians," says Contino.
But nurses receive very little financial management education, says Contino, and she points specifically to revenue cycle management, data accuracy as it relates to front-end processes (registration), back-end processes (insurance verification and point of service collection), middle-clinical documentation, and chargemaster management and departmental budgeting.
"For those places that have management incentives and bonus plans, the more nurse directors know and can do, the higher the bonus structures are," she says.
Many of these topics are covered in a new a nurse manager training course, called "Key Concepts in Emergency Department Management," launched this year by ENA. "In 2004, the faculty taught over 350 emergency nurse directors, managers, and charge nurses," says Contino, who is part of that faculty.
Because the margins in health care have decreased, it is increasingly more important for nurse directors to be able to evaluate and change the fiscal management of their departments, Contino notes.
"Directors who are able to manage supplies and human resources, and assure their processes are positively impacting the revenue cycle, have a tendency to be promoted, to receive raises, and to achieve success in their organizations," she says.
More health care organizations are investing in nurse director education and training as well, Contino continues.
"The increased training is not only an investment in the individual, but also in the organization," she notes. "The more the nurse leaders know about finance and operations, the more they are able to meet and achieve financial and operational targets."
Changing management structure
Another trend Contino sees for nurse directors is a change in the management structure of the ED, especially EDs with more than 30,000 visits per year.
They are allowing the ED to have one nurse director and supporting assistant managers, clerical support, and dedicated charge nurses, she notes.
"The ED is the window of the hospital, and the staff admit and discharge exponentially more patients than the inpatient units," Contino says.
"EDs are also faced with challenges of high burnout among staff, recruiting challenges, and rapidly changing volumes that often require the leadership team to assist in the department."
On a positive notes, those departments, the EDM Salary Survey reports, steadily are increasing in staff size.
Of those who responded to the survey, 58.21% said the number of employees in their departments had increased, and another 28.36% said that number had not changed at all. Only 13.43% said the number of employees in their department had decreased. (See chart, below.)
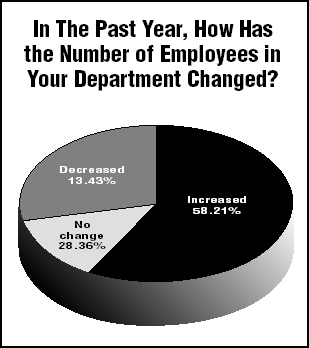
In light of this reality, Contino adds, "It is critical that this department receive adequate leadership support."
Not all EDs are seeing a shift in management structure, she says.
"On the flip side, small rural sites — or those faced with significant financial losses — will assign multiple department responsibility to one director," Contino notes. "Pay and responsibility are often dependent upon the fiscal success of the organizations."
Physicians and nurse managers in emergency medicine stand a better change of boosting their income through incentive packages, as opposed to straight salary increases, according to industry observers. And if you did receive a significant salary boost in the past year, chances are youre an ED nurse manager not a physician manager.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
