Evaluation and Management of Patients with Blast Injuries in the ED
Author: Charles Stewart, MD, FACEP, Emergency Physician, Colorado Springs, CO.
Peer Reviewers: J. Stephan Stapczynski, MD, Professor, Department of Emergency Medicine, University of Kentucky College of Medicine, Lexington; and Stephen A. Crabtree, DO, Assistant Professor, Center for Operational Medicine, Department of Emergency Medicine, Medical College of Georgia, Augusta.
Prior to 1995, United States civilian emergency physicians had little experience or interest in the effects of explosive devices. This abruptly changed with the destruction of the Alfred P. Murrah Federal building by a truck bomb in downtown Oklahoma City in 1995 that resulted in more than 750 casualties with 167 fatalities.1 This was followed by the explosion of a satchel bomb in Atlanta at the 1996 Olympics.2 Many smaller devices are found and/or exploded each year in the United States.3 Although we have passed the second anniversary of the World Trade Center attack on Sept. 11, 2001, multiple new threats of violence within the United States have been discovered. U.S. physicians have been forced to consider that they, too, may face the specter of explosions and blast injuries due to terrorism4 or accidents.
Recent terrorism incidents around the world have included an increasing use of suicidal/homicidal bombers who deliberately accompany the explosive device (often wearing it) to ensure that the maximum effect is derived from the explosive device. These bombers have walked or driven into buses, cafes, residential areas, guard-posts, and governmental buildings. The use of these devices in the United States has not yet occurred, but given the political climate, is very likely to occur. The emergency physician is likely to see the effects of these devices. Increasingly, information resources such as the Internet, terrorist training camps, and even library and television sources have made readily available the knowledge needed to construct these simple and very effective explosive devices.
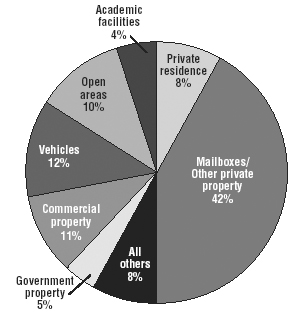
The threat of delivered explosives is not confined to mail rooms or government facilities nor do they require a proponent such as the "Unabomber."5 A substantial number of explosive devices have been placed in academic facilities and in public parks during events.6,7 (See Figure 1.) In addition, emergency physicians could encounter blast injury patients from industrial accidents or explosions at any time.
|
This article will review the current literature about blast injuries. Explosions have the potential to cause multi-system injuries involving multiple patients simultaneously. The potential mechanisms of injury, early signs of these injuries, and the natural course of the problems caused by explosive blasts will be discussed.
Investigation into blast injury is not a new area of study for those interested in combat medicine. Present knowledge of the effects of blast injury date back to the Balkan wars in 1914 when Franchino Rusca, a Swiss researcher, observed that three soldiers had been killed by an explosion without evidence of any external injuries.8 Using rabbits as an animal model, he demonstrated that the cause of death was pulmonary embolism. During World War I, blast injury was thought to be a nervous system disorder and labeled "shell-shock." (Psychological casualties were lumped together with those who had no visible injuries.)9 In World War II, a noteworthy number of casualties were found among civilians in both German and British cities after bombing raids. The term blast lung was coined for massive pulmonary hemorrhage from disruption of the alveolar architecture and formation of alveolar-venous fistulas resulting in air embolism.10 Following World War II, nuclear weapon blast injury was investigated intensively in the United States. Only since the onset of terrorist and suicide bombings in Ireland and the Near East have civilians been significantly concerned about the cause and treatment of blast injuries.9
Blast injury has an overall lethality of about 7.8% in open air.9 This jumps to nearly 49% when the blast occurs in confined spaces.11,12 About 70% of victims sustain minor soft-tissue injuries.7,12 Traumatic amputations occur in about 11% of victims. The 2001 World Trade Center explosion and subsequent building collapse was unusual, as most victims had either few injuries or died as the buildings crashed down on them.—The Editor
Mechanisms of Injury
Powerful explosions are the result of a change in chemical potential energy to kinetic injury in a very short period of time. As noted earlier, explosive agents cause both unique patterns of injury and very common injuries. Trauma caused by explosions traditionally has been divided into the injury caused by the direct effect of the blast wave (primary injuries); the effects caused by other objects that are accelerated by the explosive wave, (secondary injuries); the effects caused by movement of the victim (tertiary injuries); and miscellaneous effects caused by the explosion or explosives. (See Figure 2.)
|
The injury pattern following an explosion is partly random. This trauma results from a combination of the size of the explosive charge, the composition and nature of the explosive, the container, any shielding or protective barriers between the victim and the explosion, the surrounding environment, the method of delivery, and the distance between the explosion and the victim.
Nature of Explosives
A conventional explosion is the rapid chemical conversion of a solid or liquid into gas. Explosives are categorized as high-order explosives (HE) or low-order explosives (LE). HE and LE cause somewhat different injury patterns.
High-Order Explosives. High-order explosives are chemical materials that have an extremely high reaction rate. This reaction often is called a detonation. Examples of high-order explosives include nitroglycerin, dynamite, C-4, picric acid, Semtex, ammonium nitrate fuel oil mixture (ANFO), trinitrotoluene (TNT), and pentaeruthrotetranitrate (PETN).
When an HE detonates, it is converted almost instantaneously into a gas at very high pressure and temperature. For example, the major ingredient in Composition C-4 (Cyclotrimethylenetrinitramine or RDX [Royal Demolition eXplosive]) can generate an initial pressure of more than 4 million pounds per square inch (4x10E6 PSI).13 These high pressure gases rapidly expand from the original volume and generate a marked pressure wave—the blast wave that moves outward in all directions. The result is a sudden shattering blow to the immediate surroundings.
HEs further are categorized as primary and secondary high explosives. The primary HE is very sensitive, can be detonated very easily, and generally is used only in primary and electrical detonators. Secondary HEs are less sensitive, require a high energy shock wave to achieve detonation, and generally are safer to handle.
The blast wave refers to an intense rise in pressure—often called over pressure—that is created by the detonation of a high explosive.9 (See Table 1.)
|
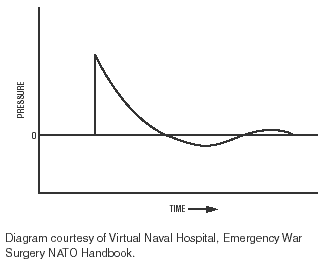
A typical pressure wave from a high explosive explosion in air is shown in the diagram in Figure 3.
|
The pressure rises almost instantaneously in the ambient environment and then decays exponentially. The peak pressure and the duration of the initial positive phase of the blast wave depend on the size of the explosion and the distance from the center of the detonation. In air, the peak pressure is proportional to the cube root of the weight of explosives and inverse of the cube of the distance from the detonation. It also depends on the type of explosives used. The extent of damage due to the pressure wave is dependent on:
- the peak of the initial positive pressure wave (an overpressure of 60-80 PSI is considered potentially lethal);
- the duration of the overpressure;
- the medium in which it explodes;
- the distance from the incident blast wave; and
- focusing due to a confined area or walls.
This blast wave has three components:
- a single spike of increased pressure;
- an exponential decay with time; and
- a much longer duration negative pressure wave with pressure below initial ambient pressure.
This increase in pressure can be so abrupt that it can shatter materials—also known as a shock wave. This effect is termed brisance and varies from one HE to another. Because the explosive gases continue to expand outward, the pressure wave rapidly deteriorates into an acoustic wave. Until the wave deteriorates enough to completely engulf the body simultaneously, tissue damage will depend on both the magnitude of the pressure spike and the duration of the force (represented by the area under the curve).
A blast wave that would cause only modest injury in the open can be lethal if the victim is in a confined area or near a reflecting surface such as a solid wall or a building.9 If the pressure wave is near a solid barrier, the pressure exerted at the reflecting surface may be many times that of the incident blast wave.
For a single, sharp rising blast wave, the damage to human structures is a function of the peak pressure and the duration of the initial positive phase.
The rapid production of immense amounts of gas creates a block flow of the surrounding medium away from the explosion. Blast wind refers to this rapid bulk movement of air and other gases from the explosion site. It occurs with both LEs and HEs.
Low-Order Explosives. LEs are designed to burn and subsequently release energy relatively slowly. These explosives often are called propellants because the most common use is to propel a projectile through a barrel. The principal military uses for LEs are as propellants and in fuses. Typical improvised LEs include pipe bombs, gunpowder, black powder, and petroleum-based bombs such as Molotov cocktails or gasoline tankers. Since LEs do not form shock waves, they do not have the quality of brisance.
The process of rapid, progressive burning of a low-order explosive is called deflagration. This burning takes place so slowly that when the LE is set off in the open, the gases push aside the air with only a flame and no appreciable disturbance. If the LE is confined, the speed of the reaction markedly is increased, but does not approach that of a high-order explosion. The explosion has more of a pushing effect than a shattering effect (blast wind without a blast wave).
The explosion from low-order devices lacks the overpressure wave and, thus, injuries are due to ballistics (fragmentation), blast wind from the expansion of the gases, and thermal injuries from the heat of the explosion. Obviously, it is clinically impossible to tell whether fragment wounds have occurred because the fragment was propelled by an HE or an LE. Likewise, if the victim is flung by blast wind into a structure, it matters little to either the patient or the clinician that the explosion occurred from an HE or deflagration of an LE.
Source of Explosive
Explosive devices also may be characterized based on their source. The Bureau of Alcohol, Tobacco, and Firearms categorizes explosives as manufactured and improvised. A manufactured explosive implies a standard, mass-produced, and quality tested weapon. Improvised describes the use of alternative materials, weapons produced in small quantities, or a device that is used outside of its intended purpose. Improvised explosive devices may be professional in appearance and operation and may be quite lethal if designed by someone with training in explosives. (Note that by this definition, any experimental explosive device is an improvised device, since it is not set to standards, mass produced, and quality tested.) This rather unwieldy definition includes all experimental military devices produced by professional arms manufacturers.
Improvised explosive devices (and many military munitions) can be triggered in a variety of ways, including electronic transmitters and switches, tilt switches, thermal switches, and various types of motion detectors. Improvised weapons vary in the quality of the explosive used from use of commercial explosives, TNT, Semtex, C-4, ammonia-based fertilizer, and fuel oil (used widely as an industrial explosive), to a match-filled pipe bomb. High-quality improvised devices may resemble military weapons in effect. The variety of initiation methods, explosive filling, and fabrication techniques creates a threat that can be quite daunting to the professional explosive ordnance disposal crew. It also means that no matter how innocuous the appearance of an improvised device, the amateur should not touch the device.
Medium in Which the Explosion Occurs
Another important concept that defines blast injury patterns is the medium in which the blast occurs. An underwater blast wave causes far more damage because water is incompressible.9,14 A wave resulting from an underwater blast travels farther and moves faster than a wave from a similar explosion in the air. Blast injuries in water occur at greater distances and may be much more severe.
Another characteristic of blast waves is that they are indeed waves. The injury patterns they produce are related not only to the medium through which they travel, but also to the position of the victim’s body in relation to reflecting or deflecting objects that the wave strikes. For example, explosions near or within hard, solid surfaces become magnified 2-9 times as the shock wave is reflected.15 In fact, victims located between the blast and a building generally suffer 2-3 times the degree of injury that individuals in an open environment receive.12
Body armor provides a false sense of security during an explosive detonation. The body armor does protect the victim from shrapnel and, to a lesser extent, from objects picked up and flung by the blast wave, but it also provides a reflecting surface that can concentrate the power of the explosion as the blast wave reflects off the front and back of the armor. (Since the bulk of injuries from an explosive device are from secondary objects flung by the blast wave, the advantages of body armor outweigh the risk of enhancing the blast wave.) The medical provider should not assume that body armor will protect the victim from an explosion-related injury.16
Pathophysiology
Primary Blast Injury. Primary blast injuries are caused only by HEs and are due to the direct effects of the blast wave on the human body. (Since LEs do not form a supersonic blast wave, they cannot cause primary blast injury. This difference is the sole apparent clinical difference between wounds caused by an LE and those caused by an HE.)
The overall incidence of primary blast injury is about 20%. This can be divided into about 1% for open-air explosions and 30-40% for closed-space explosions. (The victims of primary blast injury almost always have other types of injury, such as penetrating wounds from flying debris or blunt trauma from impact on immovable objects).17
The extent of damage from the explosion depends upon:
- the peak of the initial positive wave (this is directly related to the magnitude of the explosion);
- the duration of the overpressure;
- the medium in which it explodes;
- the distance from the incident blast wave; and
- the nature and number of reflections in confined areas and with reflecting walls.
Three Possible Mechanisms of Injury of Primary Blast Injury. The first mechanism of injury usually described as the etiology of primary blast injury is the implosion of gas-filled spaces as the high pressure blast wave compresses them.18,19 This theory states that the organs that are most vulnerable to blast injury are those containing air because the air readily is compressed. Hollow organs are compressed and disrupted by the rapid external pressure increase. The resulting force causes shearing of vascular beds, ear damage, pulmonary contusions, pneumothorax, and gastrointestinal (GI) hemorrhage. In some cases, the force of a pressure wave can be significant enough that it forces air into a blood vessel, creating air emboli. There isn’t enough time during the passage of the overpressure phase of the blast wave for gas to transfer from the lungs to the outside world through the trachea.20
The second possible major mechanism of primary blast injury often is termed spalling. This is thought to occur when a blast wave moves from a dense medium such as water to a less dense medium such as air. This often is compared to the effect of striking the outside of a rusty bucket with a hammer and watching the flakes of rust fly off the inside of the bucket. In human tissues, the transfer of reflected blast injury through the dense substrates such as muscle and liver into the less dense material of the GI tract and lungs may cause spalling. Spalling also is believed to occur when the blast wave transits from the rib cage into the lung.
The third possible mechanism of primary blast injury is the inertial effect related to the differences in tissue density and speed of the blast wave through the tissues of different densities. This may be the most important effect of the blast injury and currently is thought to be the major cause of primary blast injuries. The differences in speed of movement result in shearing and tearing forces expressed as a stress wave propagated into the underlying tissues.21,22 The resulting forces exceed the tensile strength of the material and cause shearing of vascular beds, pulmonary contusions, and GI hemorrhages.23
The true mechanism of primary blast injury likely is some combination of these theoretical mechanisms. Of these, the shearing and tearing forces appear to fit best. Primary blast injury is common in the ear, the respiratory tract, and the GI tract.
Ear Damage. Of the three organ systems, the ear is the most easily damaged, but it also is the easiest to protect. The structures of the ear are designed to collect and magnify sounds, so that the tympanic membrane moves with the sounds. Unfortunately, the ear’s structures also collect and magnify pressure waves. At a pressure of about 35 kilopascals (5 PSI), the human eardrum may rupture. With an overpressure of 100 kPa (14 PSI) almost all eardrums rupture. The eardrum most frequently ruptures into the inferior pars tensa. At lesser pressures, the overpressure may cause hemorrhage into the drum without a rupture. With extremely high pressures, the drum may be destroyed and the ossicles dislocated or fractured.
Rupture of the eardrum will cause pain, hearing loss, and may cause tinnitus. Eardrum perforations, hearing loss, and dizziness may interfere with daily activities and may affect the individual’s quality of life.24
Physical examination may reveal blood in the external canal. Examination of the tympanic membrane with an otoscope may show evidence of the perforation.
It often is held as gospel that rupture of the tympanic membrane is a marker for serious gastrointestinal or pulmonary injury. If the patient has ear protection, this may not be the case. Likewise, if the patient is in the water with his head out of the water, the tympanic membranes may not be exposed to an underwater blast wave. Isolated eardrum rupture does not appear to be a good marker of either concealed pulmonary blast injury or poor prognosis.25
Auditory barotrauma is quite common in blast injuries. In the Oklahoma City bombing, the incidence of auditory injury was 35%.1,13 This does not count those patients with partial, temporary hearing loss or those who complained of tinnitus for an extended period of time.24
Pulmonary Damage. The lungs have been considered to be the non-auditory organs most at risk for suffering primary blast injury. Blast lung is a direct consequence of the supersonic pressure wave generated by an HE.26 (See Figure 4.) It is the most common fatal injury caused by the primary blast injury among the initial survivors of the explosion. These lung injuries may not be apparent externally or immediately, but may lead to death if not diagnosed and treated promptly. An overpressure of about 40 PSI causes lung injuries.
|
Damage to the lungs can include pulmonary contusions with or without a laceration, and/or pulmonary barotrauma such as pneumothorax, pulmonary interstitial emphysema, pneumomediastinum, or subcutaneous emphysema.
It is best to assume that if a patient is wheezing after a blast injury, that the wheezing is due to a pulmonary contusion. Other causes of wheezing may be pulmonary edema from myocardial contusion or infarction, or exacerbation of underlying disorders such as asthma or chronic obstructive pulmonary disease (COPD).
The most common lung injury associated with a blast wave is a pulmonary contusion. This may take the form of micro-hemorrhages with perivascular/peribronchial disruption. It appears to be more common on the side closest to the explosion, but this may be influenced by the geometry of the surrounding area and reflected energy.27-29 The alveolar wall may be torn, causing a blood-filled emphysematous change to the lung. Pulmonary contusions may develop with or without a pulmonary laceration.
Pulmonary contusions impair gas exchange at the alveolar level. The changes seen on microscopic examination closely resemble the pulmonary contusions seen in non-penetrating blunt chest trauma.
Parallel thoracic ecchymoses, once thought to be along the ribs, may be seen with larger blast loads.20,28 These ecchymoses parallel the intercostal spaces. Rib fractures may occur due to blast injury, but are much more likely to be due to secondary or tertiary blast injury mechanisms, at least in survivors.29,30
The patient may have minimal or no symptoms initially. The patient also may complain of chest pain or respiratory distress. Signs of blast lung usually are present at the time of the initial evaluation, but have been reported as late as 48 hours after the explosion occurs.
The overpressure may cause pulmonary barotrauma, including pneumothorax or pneumomediastinum. The patient may develop pulmonary interstitial emphysema, subcutaneous emphysema, and systemic air embolism with larger blast loads.20,22,23 Significant bronchopleural fistulae may lead to air embolism. Air emboli may present in a variety of ways, including shock, myocardial infarction, spinal infarction, or cerebrovascular accident.
Blast lung is characterized clinically by the triad of apnea, bradycardia, and hypotension. The clinician should suspect blast lung in any victim who presents with dyspnea, cough, hemoptysis, or chest pain following blast exposure.
A simple frontal chest x-ray is diagnostic for most cases of pulmonary barotrauma from blast. Blast lung produces a characteristic butterfly pattern on chest x-ray. The pulmonary injuries found may range from scattered isolated petechiae to confluent pulmonary hemorrhages. The radiographic evidence of pulmonary injury usually begins within hours of the explosion and begins to resolve within one week.31
Gastrointestinal Damage. GI injuries may not be apparent externally. They have a great potential to cause death and may be much more difficult to protect against.
GI injuries once were thought to occur with the same frequency as lung injury. A recent large Israeli case series found that abdominal injuries were seen only with massive trauma.32 In this series, all patients were injured from open air explosions. The patient may have a greater risk for GI injury when exposed to an underwater explosion.33
The GI injury of primary blast injury is inconsistent in presentation. It may consist of hemorrhage beneath the visceral peritoneum or may extend into the mesentery, colon, and cecum.27,28 Contused bowel may necrose and perforate several days after the initial trauma. The perforated bowel may be apparent immediately, or may perforate only after a delay of up to 48 hours.34,35
Pneumoperitoneum is a relatively rare complication of GI barotrauma.36 This complication has a wide differential diagnosis ranging from perforated viscus to simple dissection of air through the retroperitoneum.
The colon is the most common site of both hemorrhage and perforation.33 This is thought to be because the colon has the most bowel gas accumulation in the GI tract.
Solid organ laceration and testicular rupture also are seen due to primary blast injury, but are less frequent and often are associated with large blast loads.37 The most common solid organ lesions reported were subcapsular hematomas in the liver, spleen, and kidneys.31 Mesenteric, scrotal, and retroperitoneal hemorrhages have been reported.28
These lesions can lead to the clinical signs of absent bowel sounds, bright red blood per rectum, guarding, and rebound tenderness. The clinical symptoms can include abdominal pain, nausea, vomiting, diarrhea, and tenesmus. Blast injury to the GI tract should be suspected in anyone exposed to an explosion who has abdominal pain, nausea, vomiting, hematemesis, rectal pain, testicular pain, unexplained hypovolemia, or any finding compatible with an acute abdomen.
The clinician should be aware that the abundant high-velocity fragments associated with recent suicide bombs also may cause intra-abdominal injuries. These injuries certainly can include penetrating bowel injuries.38 Initial symptoms of penetration are the same as outlined above.
Brain Injury. Primary blast injury can cause concussion or traumatic brain injury, although this finding is difficult to differentiate from the concussion due to impact with another object. The clinician should be quick to consider computed tomography (CT) or magnetic resonance imaging (MRI) in these patients.
Cardiac Injury. Myocardial contusion may occur with arrhythmia or hypotension.39
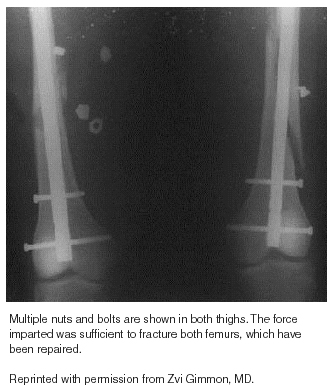
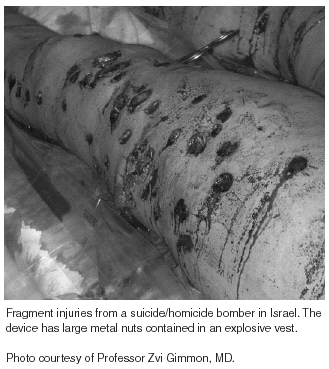
Secondary Blast Injury. Secondary blast injury is caused by the bomb fragments and other debris that are propelled by the intense energy release of the explosion. (These fragments often erroneously are referred to as "shrapnel." Shrapnel is the name for an artillery round containing multiple round lead balls that was designed during World War I by then-Lt. Shrapnel. This round essentially functions as a very large shotgun with several hundred half-inch lead balls.) (See Figures 5-7.) Conventional military explosives may create multiple fragments with initial velocities of up to 2500 m/second (8202 feet/second).40 (In contrast, the very fast moving M-16 round has a muzzle velocity of 2800 feet [853 meters] per second.)41
|
|
|
These flying projectiles can produce both penetrating and blunt trauma, depending on the size of the projectile and the speed at which it travels. With these speeds, the victim does not have to be in close proximity to the explosion. Individuals far from the scene of an explosion can be struck and injured by this debris. After the 1998 terrorist bombing of the U.S. Embassy in Nairobi, flying glass wounded victims up to 2 kilometers away.39 (The reason for the "stand-off distances" noted in the accompanying tables is to decrease to acceptable limits the number of injuries that occur from flying debris when the bomb explodes.) The farther away a person is from the explosion, the less serious the injury.
Terrorist devices often have additional objects such as nails, nuts, and bolts added to the explosive mixture to increase the effects of secondary blast injury. These fragments are of high mass and kinetic energy, and the damage that they inflict at close range is considerable. Military devices such as shells and grenades may be designed to increase the number of fragments (shrapnel) flung by the explosion.
Secondary blast injuries are much more common than primary blast injuries. Indeed, secondary blast injury is the most common cause of death in blast victims. The penetrating injuries occur most often in the exposed areas such as the head, neck, and extremities.
Glass causes many of the secondary blast injuries (up to 50% of all blast injuries). Victims who are peppered with glass often are difficult to distinguish from victims who are peppered with glass and have penetrating injuries.42
Secondary blast injuries may not be obvious initially. A seemingly small abrasion or wound may mask the entrance wound for a substantial fragment.
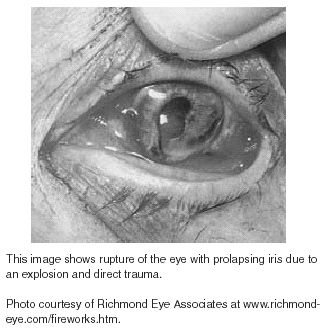
Up to 10% of blast survivors have significant eye injuries.43 (See Figure 8.) These injuries may be perforations from high-velocity projectiles. Glass is notorious for causing these ocular injuries. Window fragments often don’t kill, but they can cause blindness and ruptured globes. At the speed that explosively propelled fragments of glass travel, there is no time for the blink reflex to operate. These injuries may occur with minimal initial discomfort and may present days after the event. Symptoms include eye pain and irritation, foreign body sensation, alterations of vision, periorbital swelling, or periocular contusions. Signs can include loss of vision, decreased visual acuity, globe perforation or rupture, lid lacerations, and subconjunctival hemorrhage around the point of entry.
|
Tertiary Blast Injuries. Tertiary blast injuries are caused when the victim’s body is propelled into another object by the blast winds.20,44 Tertiary effects result from the bulk flow of gas away from the explosion. Blast winds can generate a body acceleration of more than 15 gs. They most often occur when the victim is quite close to the explosion.
This displacement of the victim can take place relatively far from the point of detonation if the victim is positioned in the path gases must take to vent from a structure, such as a doorway, window, or hatch. Likewise, if the patient is in an alley, magnification of the blast wind may occur due to the configuration of the buildings.
The deceleration caused by impact into a rigid structure causes the majority of injuries. A person who is flung into a fortified immovable object with a velocity greater than 26 feet/second (7.92 meters/second) has a mortality rate of about 50%.45 The most common injuries are fractures and closed head injuries. Isolated body parts may be broken, dislocated, or even amputated. Injuries from this mechanism also depend on what the victim hits in the environment and can range from simple contusions to impalement. Victims may tumble along the ground, sustaining abrasions, contusions, and "road rash."
Miscellaneous Blast Effects (Quaternary Blast Injuries). This category of injury includes burns from fire or radiation, crush injury associated with structural collapse, poisoning from carbon monoxide or other toxic products of the explosion, and inhalation of dust or chemicals from the explosion.
The unprotected human body can survive a blast with a peak overpressure of 30 PSI (206 kPa), but buildings and other structures collapse with the stress of only a few pounds per square inch. This means that people may survive the effects of the blast only to be injured by collapsing buildings.
The blast may be a vector for chemical and biological warfare agents. The effects of these agents on the body may well overshadow any part of the explosive energy.
Patients who have been exposed to a blast in an enclosed area should have carboxyhemoglobin levels obtained. Inhalation of irritant gases or dusts also may trigger wheezing in these patients.
Immediate Death. Fatal injuries may occur due to blast effects involving the head, chest, and abdomen and often are seen in victims who are close to the detonation.46 Indeed, in some of these victims close to the site of the blast, parts of the victim (or perpetrator) may become missiles that kill or wound other victims.47 Immediate death may occur from massive pulmonary bleeding with rapid suffocation despite good care. The patient may develop a massive air embolism or may sustain a significant brain injury. The patient may suffer a traumatic amputation and exsanguinate before help arrives. Finally, the patient may have a crush injury or impalement injury that causes rapid death before extrication can occur.
The field physician or paramedic should consider a patient dead in the field when:
- there is an amputated body part without signs of life;
- there are no effective respirations;
- there is no palpable pulse; and
- there are dilated pupils.
Persons with immediate, severe respiratory insufficiency that is caused by a blast effect have far less chance of survival.
Cardiopulmonary resuscitation (CPR) at the scene never is indicated. There will be too many injured, not enough medical providers, and no significant chance of successful resuscitation in this blunt trauma patient.
Evaluation and Management
Expect that the most severely injured patients will arrive after the less injured. The less injured often skip EMS and proceed directly to the closest hospitals. For a rough prediction of the number of "first wave" of casualties, double the first hour’s casualty count. Remember that a secondary device may be employed that can cause substantial additional casualties, which may include EMS, fire, police, and media.
Most of the injuries seen after a conventional explosive detonates are blunt, penetrating, and thermal trauma that is well known to prehospital providers, emergency physicians, and trauma surgeons.48 Much of this trauma includes soft-tissue, orthopedic, or head injuries.11,49,50 The approach to the casualty with blast-related injury, therefore, is the same as for any other trauma victim.
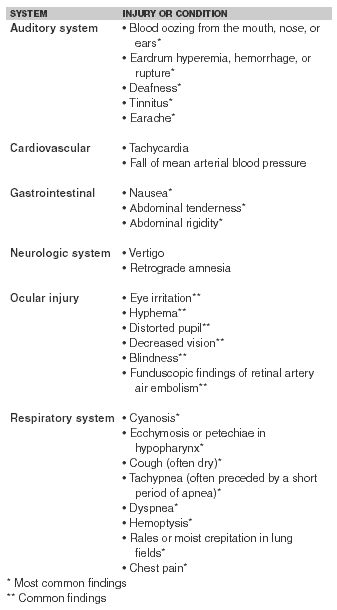
The first and most important step of management is assessment of life support needs and ensuring that the patient has an adequate airway, appropriate ventilation, and adequate circulation. A thorough physical examination then should be performed. The clinician should look for sentinel signs of potentially significant blast exposure. (See Tables 2 and 3.) Unfortunately, when the health care provider is faced with dramatic injuries such as amputations, fragment injuries, and multiple critically ill patients, it is altogether too easy to miss the subtle signs of blast injury. If the clinician does not consider the possibility of primary blast injury, the patient’s care may be complicated further.
|
|
For each patient, attempt to determine the distance from the explosion and whether the victim was in the open air or in an enclosure. If the patient was wearing body armor, this should be noted in the record. Body armor increases the chance and severity of primary blast injury, but provides significant protection against fragment injuries.
Distance obviously decreases the risk of primary blast injury (at least in the open). (See Table 4.) If the patient was in water, this should be noted, and the suspicion for intra-abdominal blast injury heightened.
Laboratory and Radiographic Studies
There are few screening studies that are of any benefit in the casualty with primary blast injury. A chest x-ray, however, should be obtained in all patients who have been near a significant explosion. The clinician should look for evidence of pulmonary contusion (as noted earlier) and barotrauma. A chest x-ray also may show free air under the diaphragm, signifying hollow viscus rupture in the abdomen.
A CT of the head, chest, or abdomen should be obtained if the history or physical examination suggests pathology in these areas. If the patient is unconscious, these CT studies are not optional.
The only laboratory study that is useful is serial hemoglobin determinations. These appear to be useful in casualties who have severe bleeding. The data may be used as a guide for blood transfusion requirements. Victims of major trauma should have baseline blood counts, hematocrit, hemoglobin, and crossmatching for potential transfusion. (See Figure 9 for an algorithm on assessment of patients with blast injury.)
Treatment
Auditory. There is no specific treatment for blast-related ear injuries. The physician should caution the victim to avoid any further auditory injury. The patient should be transferred to a quiet environment, if possible. The patient’s ears should be evaluated within 24 hours.
Debris gently should be removed from the external canal. The canal may be irrigated with an antiseptic solution if necessary. Neither antibiotics nor ear drops are recommended, particularly if the patient has a ruptured tympanic membrane. Tympanoplasty is reserved only for failures of conservative therapy.
Pulmonary. Blast lung is treated by correcting the effects of barotrauma if any is found. Gas exchange is supported. The provider should be aware that positive pressure ventilation may exacerbate pneumothorax and cause air embolism in the presence of bronchopleural fistula. The patient’s body should be positioned to ensure that the effects of air embolism are minimized.
In victims with mild respiratory distress, supplemental oxygen by nasal cannula is appropriate. Those patients with significant respiratory distress or hemoptysis should have an endotracheal tube placed. This is not without hazard, however.
Positive pressure ventilation markedly increases the possibility of both air embolism and pulmonary barotrauma. The provider should take the least invasive measure that still provides appropriate airway support in these patients.51 Avoid peak end-expiratory pressure (PEEP) and high ventilation pressures.
In one study using thoracic CT scans of patients with pulmonary contusion (not blast injury), patients with less than 18% contusion did not require intubation or ventilation.52 Patients with more than 28% contusion always required ventilation.
Because the combination of positive pressure ventilation and blast lung injury poses such a high risk for tension pneumothorax, some authors suggest bilateral prophylactic chest tubes after intubation. If the patient needs air evacuation, this becomes more desirable. If a patient with a blast lung injury abruptly decompensates, the clinician should presume that the patient has a tension pneumothorax and treat accordingly.
If the patient survives the blast lung and other trauma, there is a good chance that he will regain lung function within a year.53
Hypotension. Hypotension in blast injury victims can be due to several mechanisms:
- blood loss due to wounds (otherwise not related to the cardiovascular system);
- blood loss due to gastrointestinal hemorrhage;
- blood loss due to intra-abdominal solid organ rupture;
- hypotension from compression of vessels and heart by pneumothorax;
- hypotension due to the cardiovascular effects of an air embolism; and
- hypotension due to vagal reflexes.
The patient’s fluid volume should be supported without excessive fluid replacement. Often, blood products or colloid solutions should be used rather than crystalloid. Too much fluid replacement of course can cause increased respiratory distress as either congestive heart failure or acute respiratory distress syndrome.
Gastrointestinal. Blast injury of the GI tract can be managed in much the same way as blunt trauma of the abdomen. If the patient has an obvious penetrating wound of the abdomen, then urgent surgical management is indicated. If the patient is unconscious but hemodynamically stable or is conscious with abdominal complaints and is hemodynamically unstable, then fluid resuscitation should be undertaken. If the patient’s blood pressure stabilizes and remains stable, then a CT scan of the abdomen is appropriate. If the blood pressure does not improve, then urgent surgical management is indicated.
If the patient is conscious with abdominal findings and is hemodynamically stable, then an abdominal CT scan should be obtained. If the patient is stable, then an abdominal CT scan with oral and intravenous contrast is a reasonable screening procedure.
While abdominal CT scan is appropriately specific, it may not be sufficiently sensitive to identify hollow viscus injury.31 If patients who have been scanned continue to have signs of abdominal pathology, then a diagnostic peritoneal lavage is appropriate. If the effluent contains significant red blood cells, bacteria, bile, or fecal matter, then urgent laparotomy is indicated. CT must precede peritoneal lavage or false positive air and fluid will be introduced.
In the context of a mass casualty incident, there should be a low threshold for laparotomy when a hollow viscus injury is suspected. Close observation may not be available because of the number of casualties. Clinical signs and symptoms of early bowel injury, particularly in children, may be so subtle as to be easily missed in the patient with multiple injuries.54
Wound Management. For lacerations and fragment wounds, avoid primary closure and consider the use of delayed primary closure in these wounds. There is about an 80% rate of infection when fragment wounds are sutured. All debris that is flung by the explosion is not radiopaque, and the wise provider carefully should explore injuries and consider CT, ultrasound, or MRI of wounds to evaluate for radiolucent foreign bodies. Update the tetanus status as appropriate.
Air Embolism. Air embolism should be treated as soon as the diagnosis is considered. The first step should be to place the patient on high flow oxygen. Next, the patient should be positioned properly. The usual recommended positioning is the left lateral decubitus position with the head down. If only one lung is injured, the injured lung should be placed in the dependent position (which may override the left side down position described above.) By placing the injured lung down, the alveolar oxygen pressure is lower with a subsequent decreased risk of air entering the lungs. It should be noted that a recent review article about gas embolism opined that a flat position would be more appropriate.55 The review article also discusses use of increased fluids, heparin, and corticosteroids as treatments for gas embolism. This review article does not cite any work about blast injury in its bibliography and does not mention blast lung injury as an etiology of gas embolism. The author feels that there isn’t enough evidence specific to blast lung as an etiology of gas embolism to make a more specific recommendation.
The definitive treatment for air embolism is hyperbaric oxygenation, which often is not available in a timely fashion. Hyperbaric oxygenation will reduce the bubble size (by Boyle’s gas law), increase tissue oxygenation, and increase the solubility of the gas. The United States Navy protocols for gas embolism and decompression sickness would be an appropriate reference.
Disposition
The disposition of these patients depends on the injury sustained by each victim. Those who were close to the center of the explosion should be considered for observation for at least 24 hours.
Precautions
Ensure that physical activity of the victims is minimized after the blast explosion. Exertion after the blast explosion can increase the severity of primary blast injury. This was seen in World War II where some blast casualties appeared well, but died after vigorous exercise.56
The barotrauma that results from primary blast injury can be exacerbated by evacuation. Regardless of the altitude and distance of the flight, casualties with evidence of pneumothorax must have a chest tube placed. Evacuation aircraft should fly at the lowest possible altitude. Evacuation by long-distance, high-altitude flights should be avoided. Evacuation aircraft should be pressurized to at least 8000 feet (preferably 5000 feet).
If the victim has marginal oxygenation (PO2 < 60 mmHg), the clinician should recognize that oxygenation will worsen with ascent in an aircraft (with the increase in altitude and subsequent decreased barometric pressure).
Acute air embolism (AAE) may be the most common cause of rapid death in initial survivors of a blast. It often occurs when positive pressure ventilation is started.39,57,58
If the patient requires general anesthesia for any reason, a chest x-ray should be obtained, looking for evidence of barotrauma. It has been reported that blast victims have a higher morbidity rate when they receive general anesthesia during the first 24 hours after surgery. This may well be due to unrecognized primary blast injury and subsequent barotrauma from positive pressure ventilation during anesthesia.39 If barotrauma is noted and the patient requires general anesthesia, bilateral chest tubes are appropriate.58 If possible, local or spinal anesthesia may be better.
The evaluation of a patient with blast injuries depends on the nature of the explosion and fragments produced, the distance of the victim from the explosion, and the protection that the victim has from the blast wave and fragments. Most injuries result from fragments and debris hurled by the blast. When a victim is close and/or the explosion is large, the evaluation must include the possibility of blast-induced damage to air-filled or hollow structures. Explosive devices also may cause traumatic amputations from blast effects or from debris. If collapsed structures are involved, many injuries may be due to crushing from falling building debris and support structures. Management of most victims will follow usual trauma protocols for penetrating or crushing injuries. For victims close to the blast, the patient must be observed and evaluated for the possibility of primary blast injuries to air-filled structures.
References
1. Hogan DE, Waeckerle JF, Dire DJ, Lillibridge SR. Emergency department impact of the Oklahoma City terrorist bombing. Ann Emerg Med 1999;2:160-167.
2. CNN staff. Who planted the bomb? CNN web site www.cnn.com/US/9607/27/blast.investigation. Accessed 1/26/2004
3. Federal Bureau of Investigation Bomb Data Center. General Information Bulletin 96-1. 1996 Bombing Incidents. Washington, DC, US Department of Justice, 1996.
4. Eiseman B. Combat casualty management for tomorrow’s battlefield: Urban terrorism. J Trauma 2001;51:821-823.
5. Ottley T. Ted Kaczynski: The Unabomber. Court TV web site www.crimelibrary.com/terrorists_spies/terrorists/kaczynski/1.html. Accessed 1/26/2004.
6. Feliciano D, Anderson GV, Rozycki GS. Et al. Management of casualties from the bombing at the Centennial Olympics. Am J Surg 1998;176:538-543.
7. Peleg K, Aharonson-Daniel L, Michael M. Patterns of injury in hospitalized terrorist victims. Am J Emerg Med 2003;21:258-262.
8. Rusca F. Deutcsche Ztschr f. Chiurg 1915;132;315.
9. Elsayed NM. Toxicology of blast overpressure. Toxicology 1997;121:1-15.
10. Irwin R, Lerner MR, Ealer JF, et al. Cardiopulmonary physiology of primary blast injury. J Trauma 1997;43:650-655.
11. Mallonee S, Shariat S, Stennies G, et al. Physical injuries and fatalities resulting from the Oklahoma City bombing. JAMA 1996;276: 382-387.
12. Boffard KD, MacFarlane C. Urban bomb blast injuries: Patterns of injury and treatment. Surgery Annual 1993;25(pt 1)29-47.
13. Bailey A, Murray SG, The chemistry and physics of explosions in Explosives, Propellants, and Pyrotechnics. London UK, Brassey 1989; 1-19.
14. Landsberg PG. Underwater blast injuries. Trauma and Emergency Medicine 2000;17. Diving Medicine Online web site www.scuba-doc.com/uwblast.html. Accessed 1/26/2004.
15. Rice DC, Heck JJ. Terrorist Bombings: Ballistics, patterns of blast injury and tactical emergency care. The Tactical Edge Journal Summer 2000: 53-55.
16. Nerenberg J, Makris A, Klein H. The effectiveness of different personal protective ensembles in preventing injury to the thorax from blast-type anti-personnel mines. J Mine Action June 2000. http:/maic.jmu.edu/journal/4.2/Focus/Effectiveness/effect.htm. Accessed 1/26/2004.
17. Cernak I, Savic J, Ignajatovic D, et al. Blast injury from explosive munitions. J Trauma 1999;47:96-103.
18. Phillips YY, Richmond DR. Primary blast injury and basic research: A brief history. In: Bellamy RF, Zajtchuk R, eds. Conventional Warfare: Ballistic, Blast, and Burn Injuries. Washington DC, Office of the Surgeon General of the US Army, 1991;221-240.
19. Maynard RL, Coppel DL, Lowry KG. Blast injury of the lung. In: Cooper GJ, Dudley HAF, Gann DS, et al, eds. Scientific Foundations of Trauma. Oxford UK, Butterworth-Heinemann 1997: 214-224.
20. Stuhmiller JH, Phillips YY, Richmond DR. The physics and mechanisms of primary blast injury. In: Bellamy RF, Zajtchuk R, eds. Conventional Warfare: Ballistic, Blast, and Burn Injuries. Washington DC, Office of the Surgeon General of the US Army, 1991; 241-270.
21. Clemedson CJ, Jonsson A. Distribution of extra- and intrathoracic pressure variations in rabbits exposed to air shock waves. Acta Physiol Scand 1962;54:18-29.
22. Cooper GJ, Taylor DE. Biophysics of impact injury to the chest and abdomen. J Royal Army Med Corps 1989;135:58-67.
23. Cooper CJ, Townsend DJ, Cater SR et al. The role of stress waves in thoracic visceral injury from blast loading; Modification of stress transmission by foams and high-density materials. J Biomech 1991; 24:273-285.
24. Cohen JD, Ziv G, Bloom J. Blast injury of the ear in a confined space explosion: Auditory and vestibular evaluation. IMAJ 2002;4: 559-562.
25. Leibovici D, Gofrit ON, Shapira SC. Eardrum perforation in explosion survivors: Is it a marker of pulmonary blast injury? Ann Emerg Med 1999;34:168-172.
26. Yelverton JT. Blast biology. In: Cooper CJ, Dudley HAF, Gann DS, et al. eds. Scientific Foundations of Trauma. Oxford, UK Butterworth-Heinemann, 1997;189-199.
27. Mayorga MA. The pathology of primary blast overpressure injury. Toxicology 1997;121:17-28.
28. Sharpnack DD, Johnson AJ, Phillips YY. The pathology of primary blast injury. In: Bellamy RF, Zajtchuk R, eds. Conventional Warfare: Ballistic, Blast, and Burn Injuries. Washington, DC: Office of the Surgeon General of the United States Army; 1991:271-294.
29. Maynard RL, Coppel DL, Lowry KG. Blast injury of the lung. In: Cooper GJ, Dudley HAF, Gann DS, et al, eds. Scientific Foundations of Trauma. Oxford UK, Butterworth-Heinemann 1997: 214-224.
30. Pizov R, Oppenheim-Eden A, Matot I, et al. Blast lung injury from an explosion on a civilian bus. Chest 1999;115:165-172.
31. Argyros GJ. Management of primary blast injury. Toxicology 1997;121:105-115
32. Leibovici D, Gofrit ON, Stein M, et al. Blast injuries: Bus versus open-air bombings—a comparative studye of injuries in survivors of open-air versus confined space explosions. J Trauma 1996;41: 1030-1035.
33. Huller T. Bazini Y. Blast injury of the chest and abdomen. Arch Surg 1970;100:24.
34. Paran H, Neufeld D, Shwartz I, et al. Perforation of the terminal ileum induced by blast injury; delayed diagnosis or delayed perforation? J Trauma 1996;40:472-475.
35. Cripps NPJ, Cooper GJ. Risk of late perforation in intestinal contusions caused by explosive blast. Br J Surg 1997;84:1298-1303.
36. Oppenheim A, Pizov R, Pikarsky A, et al. Tension pneumoperitoneum after blast injury: Dramatic improvement in ventilatory and hemodynamic parameters after surgical decompression. J Trauma 1998;44:915-917.
37. Clemedson CJ, Pettersson H. Propagation of a high explosive air shock wave through different parts of an animal body. Am J Physiol 1956;84:119-126.
38. Almogy G, Makori A, Zamir O. Rectal penetrating injuries from blast trauma. IMAJ 2002;4:557-558.
39. Wightman JM, Gladish SL. Explosions and blast injuries. Ann Emerg Med 2001;37:664-678.
40. Warheads. Royal School of Artillery web site www.atra.mod.uk/atra/rsabst. Accessed 1/26/2004.
41. M16 history and weapon characteristics. GlobalSecurity.org web site www.globalsecurity.org/military/systems/ground/m16.htm. Accessed 1/21/04.
42. Wong TY Seet MB, Ang CL et al. Eye injuries in twentieth century warfare: A historical perspective. Survey Ophthalmol 1997;41: 433-459
43. Explosions and blast injuries: A primer for clinicians. Centers for Disease Control and Prevention web site www.cdc.gov/masstrauma/preparedness/primer.pdf. Accessed 1/21/04.
44. de Candole CA. Blast injury. Can Med Assoc J 1967;96:207-214.
45. Stapczynski JS. Blast injuries. Ann Emerg Med 1982;11:687-694.
46. Shuker S. Maxillofacial blast injuries. J Craniomaxillofac Surg 1995;23:91-98.
47. Braverman I, Wexler D, Oren M. A novel mode of infection with hepatitis B: Penetrating bone fragments due to the explosion of a suicide bomber. IMAJ 2002;4:528-529.
48. Weiner SL, Barrett J. Explosions and explosive device-related injuries. In: Trauma Management for Civilian and Military Physicians. Philadelphia; Saunders: 1986:13-26.
49. Hadden WA, Rutherford WH, Merrett JD. The injuries of terrorist bombing: A study of 1532 consecutive patients. British J Surg 1978;65:525-531.
50. Frykberg ER, Tepas JJ, Alexander RH. The 1983 Beirut Airport terrorist bombing: Injury patterns and implications for disaster management. Am Surg 1989;55:134-141.
51. Sorkine P, Szold O, Kluger Y, et al. Permissive hypercapnia ventilation in patients with severe pulmonary blast injury. J Trauma 1998; 45:35-38.
52. Wagner RB, Jamieson PM, Pulmonary contusion evaluation and classification by computed tomography. Surg Clin North Am 1989; 69:31-40.
53. Hirschberg B, Oppenheim-Eden A, Pizov R. Recovery from blast lung injury; One-year follow-up. Chest 1999;116:1683-1688.
54. Maxson RT. Management of pediatric trauma: Blast victims in a mass casualty incident. Clin Ped Emerg Med 2002;3:256-261.
55. Muth CM, Shank ES. Gas embolism. N Engl J Med 2000;342: 476-482.
56. Hutton JE Jr. Blast lung: History, concepts, and treatment. Current Concepts of Trauma Care 1986;9:8-14.
57. Ho AM-H, Ling E. Systemic air embolism after lung trauma. Anesthesiology 1999;90:564-575.
58. Phillips YY, Zajtchuk JT. The management of primary blast injury. In: Bellamy RF, Zajtchuk R, eds. Conventional Warfare: Ballistic, Blast, and Burn Injuries. Washington, DC: Office of the Surgeon General of the United States Army; 1991:295-335.
59. National Institute of Justice Final Report on Law Enforcement Robot Technology Assessment: Background April 2000. Accessed at www.nlectc.org/jpsg/robotassessment/background.html on 1/21/04.
60. Technical Support Working Group. Terrorist bomb threat stand-off card. www.tswg.gov/tswg/prods_pubs/newBTSCPress.htm. Accessed 1/28/2004.
This article will review the current literature about blast injuries. Explosions have the potential to cause multi-system injuries involving multiple patients simultaneously. The potential mechanisms of injury, early signs of these injuries, and the natural course of the problems caused by explosive blasts will be discussed.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.