ECG Review: The Coronaries Were Clean...
ECG Review: The Coronaries Were Clean...
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
This article originally appeared in the December 15, 2012, issue of Internal Medicine Alert. It was edited by Stephen Brunton, MD, and peer reviewed by Gerald Roberts, MD. Dr. Brunton is Adjunct Clinical Professor, University of North Carolina, Chapel Hill, and Dr. Roberts is Assistant Clinical Professor of Medicine, Albert Einstein College of Medicine, New York, NY. Dr. Brunton serves on the advisory board for Abbott, Boehringer Ingelheim, Janssen, Novo Nordisk, Sanofi, Sunovion, and Teva; he serves on the speakers bureau of Boehringer Ingelheim, Kowa, Novo Nordisk, and Teva. Dr. Roberts reports no financial relationship to this field of study.
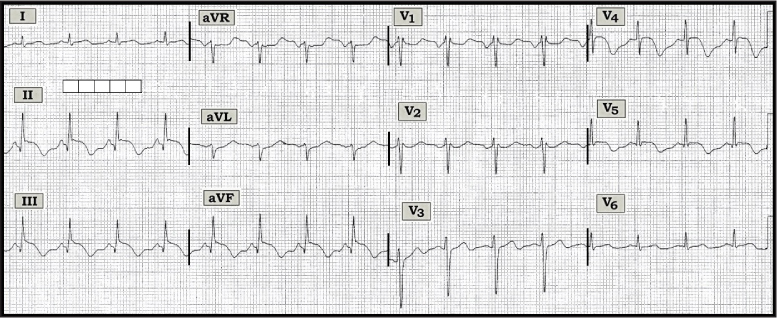
Figure — ECG obtained from a 74-year-old woman with renal colic but no chest pain.
Scenario: The ECG shown above was obtained from a 74-year-old woman who presented with abrupt onset of severe renal colic but no chest pain. Based on findings seen in her ECG, acute cardiac catheterization was performed. Her coronary arteries were normal on cath. Troponins were only minimally elevated. How would you interpret her ECG? How might you explain the finding of normal coronary arteries on cardiac catheterization?
Interpretation: The ECG shows sinus rhythm at a rate close to 100/minute. The PR and QRS intervals appear to be normal, but the QT is prolonged. The axis is normal (approximately +70 degrees). There is no chamber enlargement. An rSr’ complex is noted in lead V1.
Assessment of QRST changes is remarkable for the presence of inferior Q waves — normal transition (R wave becoming taller than the S wave between leads V3-to-V4) — and ST segment coving with marked elevation in the inferior leads. This is accompanied by deep T wave inversion. Similar abnormal ST segment coving and elevation (albeit not as marked) is also present in leads V4 and V5. Deep, symmetric T wave inversion that begins in lead V3 is seen in V4 and V5.
Despite the absence of chest pain, the impression from interpretation of this ECG was “probable acute ST-elevation myocardial infarction in need of immediate cardiac catheterization for possible reperfusion.” Surprisingly, cardiac catheterization revealed normal coronary arteries. Instead, the ventriculogram revealed apical ballooning with hypercontractility of the cardiac base characteristic of Takotsubo cardiomyopathy. The patient was treated supportively with recovery of left ventricular function over the next few weeks.
Takotsubo cardiomyopathy is an underappreciated cause of acute ECG abnormalities and new-onset heart failure. The entity was first described in Japan in 1990, with the name takotsubo being derived from a specially designed container used by Japanese fishermen to trap octopuses. The unusual round bottom and narrow neck design of takotsubo resembles the diagnostic picture on cardiac catheterization obtained as a result of ballooning of the cardiac apex with hypercontraction of the base. Other names attributed to this syndrome include stress cardiomyopathy and broken-heart syndrome, in reference to the common occurrence of severe physical or emotional stress prior to onset of the disorder. Awareness of this syndrome is important because the initial ECG may mimic a large apical infarction (with inferior and anterior ST segment elevation). Transient heart failure is common during the initial stages, but fortunately resolves within a few weeks in most cases.
For more information on this ECG Review and Takotsubo cardiomyopathy, please visit: https://www.kg-ekgpress.com/ecg_-_takotsubo/.
The ECG shown above was obtained from a 74-year-old woman who presented with abrupt onset of severe renal colic but no chest pain. Based on findings seen in her ECG, acute cardiac catheterization was performed. Her coronary arteries were normal on cath.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
