ECG Review: What Rhythm? What Artery?
ECG Review: What Rhythm? What Artery?
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
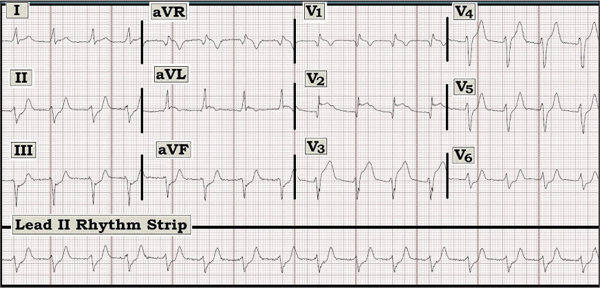
Figure — 12-lead ECG from a 55-year-old man with chest pressure.
Scenario: The 12-lead ECG and lead II rhythm strip shown above were obtained from a 55-year-old man with “chest pressure.” He is hemodynamically stable. What is the rhythm? Can you identify the “culprit” artery?
Interpretation: There are two key issues to address regarding this tracing. The first relates to determining the rhythm. Given that the patient is hemodynamically stable, there is at least a moment to contemplate what is seen. The QRS is slightly widened (to ~0.11 second). No P waves are seen. The rate is about 100/minute. Although the rhythm appears to be regular, careful measurement (with calipers) indicates that there is in fact slight variation in R-R intervals. This leaves us with the differential diagnosis of an almost regular wide rhythm at 100/minute in a hemodynamically stable patient with obvious ST-T wave abnormalities. The three entities to consider are: 1) a fascicular type of ventricular tachycardia; 2) accelerated AV nodal rhythm; or 3) atrial fibrillation. Because of the subtle irregularity in the rhythm and QRS morphology that “looks to be” supraventricular, we favor atrial fibrillation as the etiology of the rhythm. That said, we fully acknowledge that one cannot be certain of the rhythm from this single tracing. Moreover, this unfortunate patient has other more pressing concerns at the moment. Definitive rhythm diagnosis will almost certainly be revealed in this hemodynamically stable patient with ongoing monitoring over the next few minutes.
Of most concern about this tracing is the obvious extensive anteroseptal ST-elevation myocardial infarction. One should suspect a very proximal left anterior descending coronary artery occlusion because 1) there is marked ST elevation not only in leads V2 and V3, but also in leads V1, aVL, and aVR; 2) there are conduction abnormalities (right bundle branch block and left anterior hemiblock); 3) there is a non-sinus rhythm; and 4) Q waves are present in septal leads V1 and V2, with the Q in V1 in the presence of right bundle branch block strongly suggesting septal involvement. Acuity and extent of the infarct is further supported by marked reciprocal ST depression (in the inferior leads) and hyperacute T waves in multiple leads. This patient is at high risk of developing complete heart block and/or cardiogenic shock. Acute reperfusion is urgently needed.
For more information about coronary anatomy/infarct localization, please visit: https://www.kg-ekgpress.com/ecg_-_coronary_anatomy-mi_localization/.
The 12-lead ECG and lead II rhythm strip shown above were obtained from a 55-year-old man with chest pressure.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
