ECG Review: WCT in a Renal Patient
ECG Review
WCT in a Renal Patient
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
This article originally appeared in the May 15, 2013, issue of Internal Medicine Alert. It was edited by Stephen Brunton, MD, and peer reviewed by Gerald Roberts, MD. Dr. Brunton is Adjunct Clinical Professor, University of North Carolina, Chapel Hill, and Dr. Roberts is Senior Attending Physician, Long Island Jewish Medical Center, NS/LIJ Health Care System, New Hyde Park, NY. Dr. Brunton serves on the advisory board for Abbott, Amarin, Boehringer Ingelheim, Duchesnay, Janssen, Lilly, Novo Nordisk, Sunovion, and Teva; he serves on the speakers bureau of Boehringer Ingelheim, Janssen, Lilly, Novo Nordisk, and Teva. Dr. Roberts reports no financial relationship to this field of study.
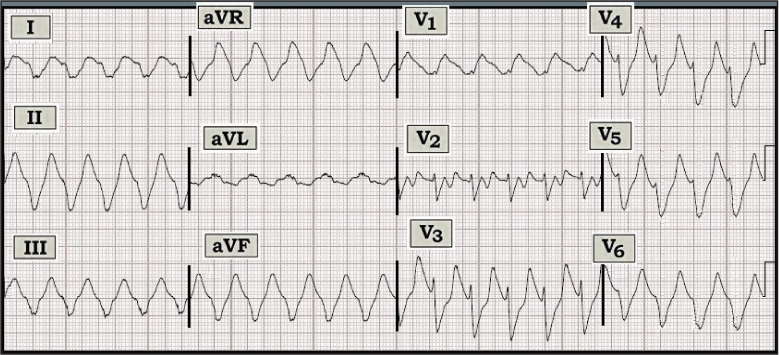
Figure — 12-lead ECG from a young adult with renal disease and diabetes.
Scenario: The ECG shown above was obtained from an acutely ill but alert and hemodynamically stable patient. How certain are you that the rhythm is ventricular tachycardia (VT)? Might there be another explanation if the patient in question was a young adult with renal disease and diabetes?
Interpretation: The rhythm in the figure is a regular wide complex tachycardia (WCT) at a rate of about 135/minute. No P waves are seen. One should clearly assume VT until proven otherwise.
VT is by far the most common cause of a regular WCT when normal sinus P waves are not seen. This is especially true when the patient is an older adult and has underlying heart disease. In addition to statistical likelihood, there are a number of morphologic features on this tracing that would seem to overwhelmingly favor the diagnosis of VT: 1) the QRS complex is markedly widened and amorphous (it does not resemble any pattern of bundle branch block); 2) the axis during the tachycardia shows extreme deviation (totally negative complexes in leads I and aVF that define an indeterminate axis); 3) the QRS complex in lead V6 is entirely negative; and 4) the QRS in lead aVR is entirely positive.
The above said, clinical circumstances in this case differ from the usual setting for VT. This is the key to recognizing the correct diagnosis. This young adult with renal disease presented to the hospital in diabetic ketoacidosis. Serum potassium at the time this tracing was done was 9.8 mEq/L. Thus, the reason for QRS widening is marked hyperkalemia! This case underscores the importance of clinical context in ECG interpretation. Rather than antiarrhythmic medication or emergency cardioversion, this patient was treated with intravenous calcium gluconate, glucose plus insulin, and emergency dialysis. ECG abnormalities promptly resolved.
The ECG shown above was obtained from an acutely ill but alert and hemodynamically stable patient. How certain are you that the rhythm is ventricular tachycardia (VT)? Might there be another explanation if the patient in question was a young adult with renal disease and diabetes?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
