ECG Review: Fatigue in a Cancer Patient: Acute STEMI?
ECG Review: Fatigue in a Cancer Patient: Acute STEMI?
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
Figure — ECG from a 60-year-old man with lung cancer.
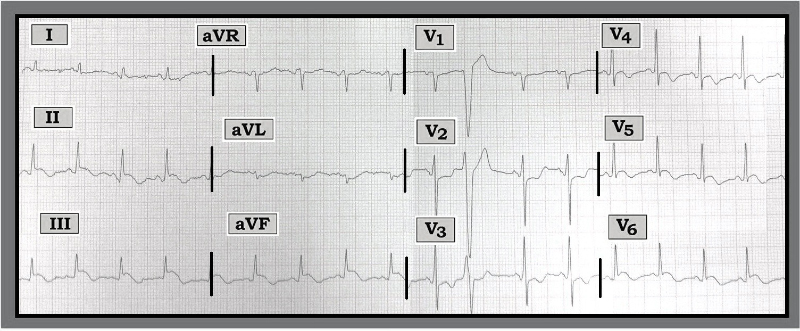
Scenario: The ECG shown above was obtained from a 60-year-old man undergoing chemotherapy and radiation therapy for lung cancer. He presented to the emergency department with weakness and palpitations, but no chest pain. Should the cath lab be activated for acute ST elevation myocardial infarction (STEMI)? Is anything else likely to be going on given this clinical history?
Interpretation: The rhythm in the figure is sinus tachycardia with one premature ventricular contraction. The PR and QRS intervals are normal; the QT is borderline prolonged. The axis is normal. There is no chamber enlargement. Regarding Q-R-S-T changes, there are no definite q waves and transition is normal (occurring between leads V2-to-V3). The most remarkable finding relates to ST-T wave changes.
There is coved ST elevation in inferior leads (II, III, aVF) and in lateral precordial (V4, V5, V6). In each of these leads, there appears to be T wave inversion following descent of the ST segment. In addition, there is scooped (reciprocal) ST depression in leads aVL and V2, V3.
The clear concern from the ECG above relates to the possibility of acute STEMI. As a result, emergent cardiac catheterization was performed. Surprisingly, the catheterization was unremarkable. There was absolutely no sign of acute coronary occlusion. Subsequent follow-up revealed a serum calcium level that was markedly elevated at 17 mg/dL.
There are several teaching points from this tracing. First, acute myocardial infarction is not the only cause of ST elevation. In addition to the more common other causes of ST elevation (early repolarization, acute pericarditis), ventricular aneurysm, cardiomyopathy, and hypercalcemia should be considered as potential “STEMI-mimics.” Second, comparison with prior tracings may be of invaluable assistance. Third, marked hypercalcemia (as was present in this case) may produce not only early ST segment peaking and coving, but also ST elevation. Fourth, even knowing that the serum calcium in this case was markedly elevated, the presence of seemingly reciprocal ST depression in leads aVL and V2 makes it impossible to rule out acute STEMI. Only by comparison with prior tracings did it become apparent that ST depression was longstanding and not acute.
The ECG shown above was obtained from a 60-year-old man undergoing chemotherapy and radiation therapy for lung cancer.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
