Hyponatremia
October 1, 2013
Reprints
Hyponatremia
Authors:
Matthew R. Ledoux, MD, Department of Pediatrics, The Brody School of Medicine at East Carolina University, Greenville, NC.
Ronald M. Perkin, MD, MA, FAAP, FCCM, Professor and Chairman, Department of Pediatrics, The Brody School of Medicine at East Carolina University, Medical Director, Children’s Hospital, University Health Systems of Eastern Carolina, Greenville, NC.
Peer Reviewer:
Jeffrey Linzer, MD, FAAP, FACEP, Assistant Professor of Pediatrics and Emergency Medicine, Emory University School of Medicine; Associate Medical Director for Compliance, Emergency Pediatric Group, Children’s Healthcare of Atlanta at Egleston and Hughes Spalding, Atlanta, GA.
Hyponatremia is a commonly encountered electrolyte abnormality in the acute care setting. Abnormalities may range from mild (serum sodium < 135 mEq/L) to severe (serum sodium < 120 mEq/L). Failure to identify and appropriately correct hyponatremia may result in significant morbidity, particularly neurologic sequelae, and mortality.
— Ann M. Dietrich, MD, Editor
Definition
Hyponatremia is reported as the most common electrolyte abnormality in hospitalized patients.1,2Commonly associated with morbidity, especially when the electrolyte disturbance progresses to severe hyponatremia, it may lead to additional complications and, at times, death. Defined as a total sodium serum concentration of less than 135 mEq/L, it is determined by the content of sodium and water in the body. Mild hyponatremia (serum sodium < 135 mEq/L) has been reported in 15-22% and moderate hyponatremia (serum sodium < 130 mEq/L) in 1-7% of hospitalized patients.2,3Severe hyponatremia is a serum sodium < 120 mEq/L and may be associated with significant morbidity and mortality. Early recognition of hyponatremia is critical to initiate timely therapy. In afebrile pediatric patients presenting with a first-time seizure, hyponatremia must be high on the differential diagnosis, as it is the most common cause of afebrile seizures in young children.4A diversity of symptoms may be associated with hyponatremia, and many of them are subtle. A high degree of suspicion is necessary to make a timely diagnosis. (See Table 1.)
| Table 1. Hyponatremia Signs and Symptoms7 |
|---|
|
There are many causes of hyponatremia. The classification of hyponatremia by the estimation of the overall clinical volume status makes a helpful way not only to determine the management of the patient, but also to classify the potential cause of the electrolyte abnormality.
Hyponatremia with Hyperosmolarity
There are two common causes of hyponatremia in the setting of hyperosmolarity due to hyperglycemia, with nonketogenic or diabetic ketoacidosis (DKA) being the ones more commonly encountered in the emergency department (ED). Hyperglycemia forces movement of water from the intracellular (ICF) compartment to the extracellular fluid compartment (ECF), resulting in a reported hyponatremia by measurement. Conversely, severe dehydration may occur in some patients in DKA, resulting in hypernatremia as free water is lost in the diuresis caused by glucosuria. The administration of exogenous agents, such as mannitol, can also result in hyperosmolar hypernatremia.
A quick way to estimate the effect of hyperglycemia on the sodium level is through calculations based on the patient’s current glucose level. A decrease of 1 mEq/L in the sodium concentration for each increase of 62 mg/dL of serum glucose up to 400 mg/dL is expected or based on 100 mg/dL increase in glucose, a resultant drop of 1.6 mEq/L.5The effect is more significant for a glucose > 400 mg/dL,6with a decrease of 4 mEq/L sodium for every 100 mg/dL.
Hypovolemic Hyponatremia
In hypovolemic hyponatremia, there is both a loss of sodium and a decrease in total body water. This is important, as it will influence the initial phases of correction and resuscitation.
Both extra-renal and renal losses of sodium and total body water are common causes of hypovolemic hyponatremia in children. The most common is extra-renal losses associated with acute gastroenteritis (vomiting and diarrhea). Gastroenteritis accounts for 160,000 hospitalizations in the United States per year, or 10% of hospital admissions in children younger than 5 years old.8Dehydration from gastroenteritis can cause isonatremic or hyponatremic dehydration, depending on the underlying cause of the gastroenteritis and the sodium content of the losses.
Renal causes of hyponatremia in the setting of hypovolemia include diuretic use, acute tubular necrosis, and renal tubular acidosis. Diuretics, most commonly thiazides, have been reported to cause hyponatremia in older patients and, in theory, could cause it in pediatric patients as well.9Hyponatremia occurs by increasing excretion of sodium and potassium and accentuating water loss.10Even though thiazide use is somewhat limited in pediatrics (e.g., certain congenital cardiac conditions), these patients are somewhat more vulnerable to electrolyte imbalance, so it is important for the clinician to consider evaluating the electrolytes of any child on a thiazide diuretic with any acute illness.
Other renal causes of hyponatremia in pediatrics include renal tubular acidosis (RTA) and acute tubular necrosis (ATN). RTA in pediatrics presents as a hyperchloremic metabolic acidosis. There are three subtypes of RTA, with pathology occurring at different locations within the renal tubule. Specifically, RTA type 2, or proximal, can present with severe volume depletion and hyponatremia. ATN also can present with hyponatremia regardless of whether it has a pre-renal, intrinsic, or post-renal etiology. The hyponatremia in ATN usually occurs as a dilutional hyponatremia during the low urine output phase of ATN; however, at times it can be seen during the polyuria that often accompanies ATN if large amounts of sodium are also lost in the urine. Less common causes of hyponatremia and hypovolemia occur in pediatric patients who have severe burns or other causes of third spacing, including nephrotic syndrome, pancreatitis, ascites, peritonitis, and severe infections. The third spacing will stimulate the retention of free water secondary to the hypovolemia and, in turn, may present with hyponatremia.
In the hypovolemic patient, the primary concern with the physical exam is to determine if signs of poor perfusion and/or shock are present. If present, then resuscitation using isotonic fluid is indicated. It is recommended to use fluids such as 0.9% saline (normal saline).11In adults, multiple studies have looked at the benefit of other replacement fluids (colloids), and their use compared to crystalloids either shows no benefit or an increase in mortality and the increased need for renal replacement therapy.12-14Therefore, in children it is recommended to start with an initial bolus of 20 mL/kg of 0.9% saline over 5-10 minutes. Reevaluation of the patient’s perfusion and heart rate after the initial bolus will guide the need for additional fluid resuscitation. Multiple boluses of 20 mL/kg should be given until the patient is stabilized. Excessive fluid, when not needed for resuscitation, should be avoided, as it can not only cause hypervolemia but electrolyte abnormalities such as hyperchloremia, which has its own associated morbidity.15,16
Once the initial resuscitation is complete and labs have returned and show hyponatremia, focus on the correction and determination of the etiology of the hyponatremia becomes the next priority. When significant symptoms such as mental status changes, seizures, hypothermia, and/or coma are present, especially if the serum sodium is < 125 mEq/L, increasing the sodium to greater than 125 is a priority. The clinician should consider using 3% saline solution for this purpose. Normal saline has 154 mEq of sodium per liter, while 3% has 513 mEq of sodium per liter. The calculation for sodium replacement is as follows.
Equation #1:
Amount of sodium replacement (mEq) = 0.6 × (weight in kg) (125 serum sodium)
The sodium replacement can then be given using 3% saline.
Once the critical sodium and volume replacement has been accomplished in the hypovolemic patient, calculating the degree of dehydration should occur. The degree of dehydration may be estimated clinically on the patient presenting with hypovolemic hyponatremic dehydration. Volume deficits can be calculated using findings on the clinical exam (see Table 2), or by a calculation using a pre-illness weight, if available, and an illness weight.
Table 2. Clinical Observation in Dehydration17

Fluid Deficit (L) = pre-illness weight (kg) illness weight (kg)
% Dehydration = (pre-illness weight illness weight)/pre-illness weight × 100%
The patient’s clinical findings may be worse for hyponatremic dehydration than hypernatremic dehydration.
Following the initial volume resuscitation to correct tachycardia and poor perfusion, the patient’s maintenance fluid requirements should be carefully calculated based on water and sodium requirements. Careful monitoring should occur throughout the initial and ongoing resuscitation.
The next phase is slow correction of the fluid deficit and sodium depletion. The fluid deficit is calculated based on the degree of dehydration. It is often assumed the volume depletion was at least isotonic; therefore, the deficit must be added to the total sodium required to raise the serum sodium to normal (135 mEq/L) using equation #1. Both the rate and the sodium concentration should be taken into account once the correction phase begins.
The total volume replaced should be given using equation #2 over a minimum of 24-48 hours, or possibly even longer, depending on the length of time the patient took to become hyponatremic.
Equation #2:
Total volume replaced = maintenance needs + (deficit − resuscitation)
The most important management strategy of these patients is to follow electrolytes closely and assure that you are correcting it appropriately as an inpatient.
The replacement maintenance fluids should be carefully selected. While the issue is subject to debate, there is mounting evidence that isotonic fluids should not only be used for resuscitation but also in the replacement and maintenance portion of treatment.18For example, studies have shown that in children with gastroenteritis, the use of normal saline appears to be superior, not causing hyponatremia, decreasing the risk of dilutional hyponatremia, especially when the patient is mildly hyponatremic or isonatremic on presentation.19However, its use in patients who present with severe hyponatremia should be initiated with caution to assure a gradual sodium correction.
Euvolemic Hyponatremia
In the setting of hyponatremia with normal intravascular volume status, euvolemia, the most common cause is syndrome of inappropriate antidiuretic hormone (SIADH). A number of other uncommon causes also occasionally can be seen, such as water intoxication, desmopressin use for nocturnal enuresis, treatment of diabetes insipidus or hemophilia, as well as glucocorticoid deficiency and hypothyroid disease.
SIADH
SIADH was originally described in adults diagnosed with bronchogenic carcinoma in 1957.20It has since been described not only in adults but in children with varying diagnoses and after many different procedures, drugs, and injuries.
SIADH often can be a difficult diagnosis to make. However, it is imperative that it is made because the management of the hyponatremia from SIADH is different from the management of other causes of hyponatremia. Helpful criteria in making the diagnosis include: decreased urine output (< 1 mL/kg/hour); serum osmolality < 279 mOsm/L; urine osmolality > 250 mOsm/L; and hyponatremia (Na < 130 mEq/L), with normal volume status and the absence of renal and adrenal disease.21
SIADH is seen in the setting of euvolemia and is the inappropriate response hormonally in that state. Antidiuretic hormone (ADH, arginine vasopressin) is normally produced in response to low-volume states to increase free water retention, resulting in concentration of the urine. If this occurs abnormally in a euvolemic state, the resulting increase in total body water and near normal total body sodium will present as hyponatremia, essentially a dilution of the serum sodium concentration. The urine sodium prior to therapy is most commonly greater than 20 mEq/L. The effect of the inappropriately secreted ADH is the inability to dilute urine. In addition to this, a natural natriuresis also occurs in an effort to excrete free water. This is reportedly counteracted in some part by the effects of renin, aldosterone, and atrial natriuretic peptide.22
SIADH can be seen for many reasons. Most often it is seen and explained secondary to a central nervous system (CNS) injury or pathology, such as meningitis, encephalitis, stroke, or intracranial hemorrhage, but it is also seen secondary to surgery on the brain and spinal cord. (See Table 3.) One study found that 33% of children undergoing spinal fusion, regardless of the reason for the surgery, developed SIADH.23
| Table 3. Conditions Associated with SIADH |
|---|
* See Table 4 |
Recognizing that pathology and/or manipulation of the CNS has a high potential of causing SIADH facilitates a clinician’s early recognition and appropriate fluid and electrolyte management. In addition to the CNS etiologies, other pathology has also been associated with hyponatremia, most likely from a secondary SIADH. Pulmonary infections and pathology, including tumors, have also been linked to SIADH and hyponatremia. One study showed that approximately 45% of all patients with community-acquired pneumonia also had hyponatremia at the time of diagnosis, with most hyponatremia being mild (serum sodium 130-135 mEq/liter), and only a handful with more severe hyponatremia (less than 130 mEq/liter).24It is important to consider hyponatremia in any ill child, especially with pulmonary or CNS disease.
In addition, many drugs have been known to cause hyponatremia. Many of these drugs can cause hyponatremia because they affect the balance of ADH, often inducing release of ADH or mimicking it.
In addition to diuretics that can cause abnormalities in water and sodium homeostasis, other drugs such as antidepressants, antipsychotics, anti-seizure medications, and cancer treatment medications can also create an imbalance of water in the body thought to be caused by abnormal production of ADH.25(See Table 4.)
| Table 4. Drugs Known to Cause Hyponatremia |
|---|
Diuretics
|
Antidepressants
|
Antipsychotics
|
|
Antiepileptic
|
Chemotherapy
|
Analgesics
|
Anti-arrhythmic
|
While many of these drugs are not commonly used in pediatrics, they should be considered in a patient presenting with hyponatremia of unknown cause. Desmopressin, a synthetic anti-diuretic hormone (DDAVP®or Stimate26The clinician should be attuned to this as a cause of hyponatremia. While children using this medication are often told not to drink fluids one hour prior to administration and eight hours thereafter, a mobile young child may not be able to resist the desire to drink and, thus, may develop moderate to severe hyponatremia.
Hormone Causes. Primary adrenal insufficiency, both inherited and acquired, as well as hypopituitarism, can also present with hyponatremia. These disorders of the hypothalamic-pituitary-adrenal axis cause disruption of the water-sodium balance of the body.27The abnormal balance is due to the inappropriate secretion of ADH, which can be explained partially by the deficiency of cortisol, thus causing a low blood pressure and cardiac output. It also has been postulated that renal sensitivity to ADH may also occur, as well as renal hemodynamics with decreased distal fluid delivery to the nephron.28In Addison’s disease (primary adrenal insufficiency), hyponatremia is often found in addition to other electrolyte abnormalities such as hyperkalemia. The deficiency of aldosterone seen in Addison’s contributes to hyponatremia due to salt wasting and an imbalance of water due to the resultant hypovolemia.
Hyponatremia can also be seen in primary hypothyroid disease.29It has been shown in a retrospective review that there is a direct relationship between TSH and serum sodium levels. One study found that for every 10 mU/L increase in TSH, there was a decrease in serum sodium by 0.14 mEq/L.30The relationship between hypothyroidism and hyponatremia seems to be due, in part, to reduced cardiac output and renal perfusion. This, in turn, causes an inappropriate secretion of ADH in an otherwise euvolemic patient. The result is that the kidneys retain free water and consequently dilute the sodium serum concentration.
What is clear is that abnormalities and pathology anywhere along the hypothalamic-pituitary axis, as well as primary endocrine abnormalities, can adversely affect water and sodium balance and result in hyponatremia. Thus, in any patient presenting with hyponatremia, a primary endocrine cause should be considered. Endocrine causes of hyponatremia require hormone replacement to facilitate correction of the hyponatremia.
Water Intoxication
Water intoxication can occur either intentionally or accidentally and can cause hyponatremia. In most cases, it causes euvolemic hyponatremia if urine output is maintained; however, if for any reason urine output does not match the volume of water ingested, it will cause hypervolemia.
A common misconception is that drowning can lead to severe water intoxication and result in severe electrolyte abnormalities. However, it is not common to have such abnormalities following a drowning event. Swimming in fresh water does have some risk of developing hyponatremia, not only by accidental ingestion of large amounts of free water, which would be the most common cause for children, but also in athletes swimming in events including triathlons. The hyponatremia in triathletes is thought to be primarily due to abnormal regulation of ADH, as well as free water ingestion for hydration, but can occur partially as accidental ingestion. One case report found that a child suffered severe hyponatremia and developed seizures following ingestion of water during swimming lessons.31
Another cause of hyponatremia occurs among endurance athletes. With the increasing popularity of long-distance exercise, including half marathons, marathons, and triathlons, the incidence of participants developing hyponatremia seems to be on the increase. There appear to be some risk factors associated with the development of hyponatremia among these athletes. (See Table 5.) Work done in the 1980s in New Zealand and South Africa found that consumption of large quantities of water was the primary risk factor.32,33
| Table 5. Risk Factors for the Development of Exercise-induced Hyponatremia34 |
|---|
|
One study of Boston Marathon participants found that 13 % of the 488 participants sampled had hyponatremia (defined as < 135 mmol/L) and 0.6% had severe hyponatremia (< 120 mmol/L).35Athletes other than runners, such as triathletes and endurance swimmers, also appear to be affected. One study out of Zurich found that six of the 36 participants in an ultra-endurance swim developed hyponatremia following the 26 km swim.36Females were more likely to develop hyponatremia, which was found in 36% of females participating.36In addition, multiple reports have shown severe consequences associated with the hyponatremia can develop, including seizures requiring intubation, pulmonary edema, and cerebral edema leading to death.37-39It is believed this is not only caused by the ingestion of free water but also the dysregulation of ADH in the setting of salt loss from excessive sweating and ingestion of hypotonic fluids during exercise.
Water intoxication can also occur during the treatment of medical problems, including constipation and impaction.40Multiple case reports have shown that "tap-water" enemas can cause hyponatremia from free-water absorption across the colonic mucosa.41This has also been seen in adults with various irrigation solutions utilized during endoscopic surgery.
Child abuse should also be considered as a potential etiology for hyponatremia. This should be considered in any case in which the history doesn’t exactly make sense or in a child who was previously healthy and in whom other red flags or signs of abuse are present. In 2003, Arieff et al documented three cases of children who subsequently died after they were forced to ingest large quantities of water as acts of child abuse.42
A more common cause of hyponatremia in infants is improperly mixed formula. This may be accidental or intentional without harmful intent by the caregiver trying to extend the amount of formula available. A clinician should consider asking the parents how they make the formula. If the parents are using powdered formula, the clinician should confirm that they are using one scoop to two ounces of water, which is universal for all commercially based over-the-counter formulas providing 20 calories per ounce.
Psychogenic polydipsia, although not common in pediatrics, also should be considered. This is commonly seen in psychiatric patients and patients taking medications that accentuate the thirst response or sense of a dry mouth, commonly seen among many antipsychotics. This was described by Hariprasad et al in 1980 in a series of 20 psychotic patients with serum sodium levels being measured as low as 98-124 mEq/L.43Given the low morbidity and mortality of these patients, and the fact that most had few if any symptoms, the hyponatremia most likely occurred over time, demonstrating the chronicity of the hyponatremia and the ability for the brain to adapt. However, deaths, as well as seizures and coma, have been reported from hyponatremia related to these medications.44
Drug abuse also may precipitate or be associated with hyponatremia. One case report demonstrated that on two occasions the same patient presented with acute kidney injury from recurrent bath salt ingestion.45In another study, Van Dijken et al demonstrated a high incidence of hyponatremia among female participants using ecstasy. The study evaluated 63 subjects confirmed to be using the drug by urine toxicology screen and 44 controls not using it. The study found 14% of ecstasy users had hyponatremia, with 26% of female users affected.46It is possible that not only the effects of the drug but also the polydipsia associated with ecstasy use may contribute to electrolyte abnormalities, especially hyponatremia.
Pseudohyponatremia
Pseudohyponatremia is the falsely low measurement of sodium concentration. It occurs when the extracellular fluid (ECF) water content, which is normally 93%, is decreased. This decrease occurs when the other 7% of the ECF compartment is increased. Usually the other 7% is made up of proteins and lipids. In the setting of hyperlipidemia or an increase in the ECF concentration of proteins, as in multiple myeloma, the concentration of sodium will be reported low by some clinical laboratory devices.47An important clue will be the osmolality is normal. It is important for clinicians to be aware of the techniques and methods used by their laboratory services to calculate and report electrolytes to avoid a delay in the diagnosis of pseudohyponatremia. Case reports have shown how this phenomenon can be misleading and result in a delay in proper treatment and, in rare cases, death.48
Iatrogenic Hyponatremia
Iatrogenic causes of hyponatremia are important for discussion. Easly and Tillman just recently summarized literature published since 2006. (See Table 6.)
Table 6. Summary of the Literature49
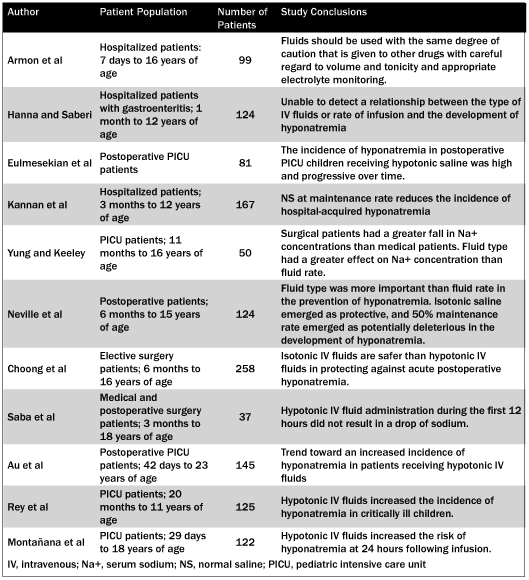
Recently, published articles have demonstrated that the infusion of hypotonic fluid as maintenance intravenous therapy has the risk of causing hyponatremia. Some would argue against its use altogether as a maintenance therapy. For instance, Neville et al and Moritz et al both argue that the fluid of choice is isotonic saline and should be used routinely in gastroenteritis.18,19
There are strong evidence and case reports that support that the use of hypotonic fluids, as bolus therapy presents a severe risk of morbidity and mortality and its use should be discouraged.61Jackson and Bolte propose that hypotonic fluids as stock solutions in pre-hospital (first responders) settings and the ED should be removed to eliminate the possibility of their being used, eliminating them as being a cause of morbidity or mortality.62
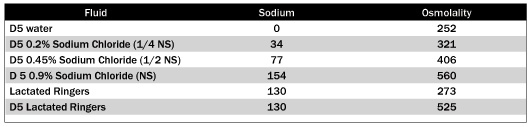
It is clear from the studies that isotonic fluid should be the only choice for fluid resuscitation and bolus therapy. In addition, the use of hypotonic fluid for children should not be chosen without a great amount of thought as to the underlying disease process and the child’s sodium and free-water needs. This is supported by Moritz et al, who have published a great deal on this topic and recommend against the routine use of hypotonic fluids except when clinically indicated.63-65They also remind us of the warnings released by the Institute for Safe Medications Practices (ISMP), a nonprofit organization that is devoted to medication error prevention, in regard to hospital-acquired hyponatremia.66What is clear is that the patient’s free-water and sodium needs and losses, as well as serum electrolytes, should be taken into account when selecting a maintenance fluid therapy. Table 7 lists common IV fluids used for maintenance therapy in children and their sodium composition and osmolality. In addition, ongoing monitoring of the serum sodium levels should be performed as frequently as clinically indicated to ensure the patient is not developing worsening hyponatremia or too rapid correction of the hyponatremia.
Table 7. Sodium Composition of Common Parenteral Fluids
Hypervolemic Hyponatremia
Hyponatremia in the setting of fluid overload is usually seen in the setting of liver disease or heart failure. The hypervolemia in heart failure occurs because of the overall decrease in blood pressure secondary to decreased cardiac function and the subsequent activation of baroreceptors. This results in the secretion of ADH, which stimulates the retention of fluid within the renal tubules. The resulting free-water retention without an overall increase in total body sodium will cause the hyponatremia seen in heart failure.
Likewise, in liver disease, the overall vasodilation from the liver failure will cause a decrease in cardiac output and free-water retention. This is also accentuated by the common finding of hypoalbuminemia that will perpetuate fluid retention due to third spacing and lowered cardiac output, causing a hypervolemia and hyponatremia.
Other disease processes that also may produce hypervolemia, such as nephrotic syndrome or hypoalbuminemia, may present with hyponatremia if the kidneys are not able to retain enough sodium to prevent hyponatremia.
Prevention of Neurologic Complications During Treatment
In patients with hyponatremia, the primary clinical concern is determining the rapidity with which the hyponatremia has developed: Is it acute or chronic? In the acute development of hyponatremia, the concern is that if the fall in serum osmolality (sodium is the largest contributor) occurs quickly, the shift of water into the brain can be dramatic and cerebral edema can occur, causing permanent neurological impairment.
The brain has a unique mechanism to protect itself from the fall in sodium and osmolality that may occur over time. This mechanism, however, can cause another complication if the hyponatremia is corrected too quickly. This protection occurs by the brain excreting electrolytes out of the intracellular space, thus normalizing the fluid balance within the brain. However, this mechanism can also be the cause of osmotic demyelination syndrome, previously known as central pontine myelinolysis.67This syndrome occurs if the hyponatremia has been present for more than 48 hours and the serum sodium correction occurs too quickly. Neurologic findings include paresthesia, confusion, coma, seizures, or the inability to move or speak, also known as "locked in."67However, case reports show that this tends to occur when serum sodium is < 120 mEq/L.
Most causes of hyponatremia, excluding acute water intoxication, occur over a period of time and, thus, during initial diagnosis should be corrected cautiously. Often, treating the underlying cause or removing the stimulus for the hyponatremia (for example, discontinuing thiazide diuretics) can help return the sodium to normal without much difficulty.
During the correction phase, sodium should be monitored closely, possibly as often as every two hours, to ensure that correction occurs at a rate of 10-12 mEq/L/24-hour period. This recommendation comes from the evidence that osmotic demyelination is often seen at correction rates > 20 mEq/L over 24 hours. Additional contributing risk factors include initial serum sodium concentration and the length of time the hyponatremia has been present. Most cases occurred in the setting of severe hyponatremia < 105 mEq/L and almost all < 120 mEq/L.
Conclusion
Hyponatremia is a common electrolyte abnormality. The initial workup should be a detailed history to attempt to clarify the etiology. Rapid correction should only occur when the sodium is < 120 mEq/L and if seizures or other neurologic symptoms are present, and should be corrected only to 125, after which point a slow and deliberate correction should take place. Evaluating the volume status of the patient and classifying into hypovolemic, euvolemic, or hypervolemic will better delineate the etiology and the management strategies. Slow correction is imperative to ensure neurologic complications do not occur. Health care personnel should also consider the routine use of isotonic fluids for both bolus and maintenance therapy to avoid the risk of iatrogenic hyponatremia.
References
- Adrogue HJ, Madias NE. Hyponatremia. N Engl J Med 2000;342(21):1581-1589.
- Ellison DH, Berl T. Clinical practice. The syndrome of inappropriate antidiuresis. N Engl J Med 2007;356(20):2064-2072.
- Upadhyay A, Jaber B, Madias N. Incidence and prevalence of hyponatremia. Am J Med 2006;119(Suppl 1):S30-S35.
- Corneli HM, Gormley CJ, Baker RC. Hyponatremia and seizures presenting in the first two years of life. Pediatr Emerg Care 1985;1(4):190-193.
- Oh G, Anderson S, Tancredi D, et al. Hyponatremia in pediatric diabetic ketoacidosis: Reevaluating the correction factor for hyperglycemia. Arch Pediatr Adolesc Med 2009;163(8):771-772.
- Hillier TA, Abbott RD, Barrett EJ. Hyponatremia: Evaluating the correction factor for hyperglycemia. Am J Med 1999;106(4):399-403.
- Farrell C, Del Rio M. Hyponatremia. Pediatr Rev 2007;28(11):426-428.
- Chang HG, Glass RI, Smith PF, et al. Disease burden and risk factors for hospitalizations associated with rotavirus infection among children in New York State, 1989 through 2000. Pediatr Infect Dis J 2003;22(9):808-814.
- Sonnenlick M, Friedlander Y, Rosin A. Diuretic induced severe hyponatremia. review and analysis of 129 reported patients. Chest 1993;103:601.
- Cesar K, Magaldi A. Thiazide induces water absorption in the inner medullary collecting duct of normal and Brattleboro rats. Am J Physiol 1999;277:F756.
- Kleinman M,. Chameides L, Schexnayder SM, et al. Part 14: Pediatric advanced life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010;122:S876-S908.
- Perner A, Haase N, Guttormsen AB, et al. Hydroxyethyl starch 130/0.42 versus ringer’s acetate in severe sepsis. N Engl J Med 2012;367(2):124-134.
- Myburgh JA, Finfer S, Bellomo R, et al. Hydroxyethyl starch or saline for fluid resuscitation in intensive care. N Engl J Med 2012;367(20):1901-1911.
- McIntyre LA, Fergusson DA, Cook DJ, et al. Fluid resuscitation with 5% albumin versus normal saline in early septic shock: A pilot randomized, controlled trial. J Crit Care 2012;27(3):317.e1,317.e6.
- Boniatti MM, Cardoso PR, Castilho RK, et al. Is hyperchloremia associated with mortality in critically ill patients? A prospective cohort study. J Crit Care 2011;26:175-179.
- Tani M, Morimatsu H, Takatsu F, et al. The incidence and prognostic value of hypochloremia in critically ill patients. Scientific World Journal 2012;2012:474185.
- Robertson J, Shilkofski N, editors. The Harriet Lane Handbook, 17th ed. 2005: Elsevier Mosby.
- Moritz ML, Ayus JC. Improving intravenous fluid therapy in children with gastroenteritis. Pediatr Nephrol 2010;25(8):1383-1384.
- Neville KA, Verge CF, Rosenberg AR, et al. Isotonic is better than hypotonic saline for intravenous rehydration of children with gastroenteritis: A prospective randomized study. Arch Dis Child 2006;91(3):226-232.
- Schwartz W, Bennett W, Curelop S, Et a. A syndrome of renal sodium loss and hyponatremia probably resulting from inappropriate secretion of antidiuretic hormone. Am J Med 1957;23:529-542.
- Lieh-Lai MW, Stanitski DF, Sarnaik AP, et al. Syndrome of inappropriate antidiuretic hormone secretion in children following spinal fusion. Crit Care Med 1999;27(3):622-627.
- Robertson GL. Antidiuretic hormone. normal and disordered function. Endocrinol Metab Clin North Am 2001;30(3):671,94, vii.
- Lieh-Lai MW, Stanitski DF, Sarnaik AP, et al. Syndrome of inappropriate antidiuretic hormone secretion in children following spinal fusion. Crit Care Med 1999;27(3):622-627.
- Don M, Valerio G, Korppi M, et al. Hyponatremia in pediatric community-acquired pneumonia. Pediatr Nephrol 2008;23(12):2247-2253.
- Liamis G, Milionis H, Elisaf M. A review of drug-induced hyponatremia. Am J Kidney Dis 2008; 52(1):144-153.
- Taketomo C, Hodding J, Kraus D. Pediatric Dosage Handbook. In: 18th ed. Lexi Comp; 2012:404.
- Oelkers W. Hyponatremia and inappropriate secretion of vasopressin (antidiuretic hormone) in patients with hypopituitarism. N Engl J Med 1989;321(8):492-496.
- Liamis G, Milionis HJ, Elisaf M. Endocrine disorders: Causes of hyponatremia not to neglect. Ann Med 2011;43(3):179-187.
- Shakir MK, Krook LS, Schraml FV, et al. Symptomatic hyponatremia in association with a low-iodine diet and levothyroxine withdrawal prior to I131 in patients with metastatic thyroid carcinoma. Thyroid 2008;18(7):787-792.
- Warner MH, Holding S, Kilpatrick ES. The effect of newly diagnosed hypothyroidism on serum sodium concentrations: A retrospective study. Clin Endocrinol 2006;64:598-599.
- Bennett HJ, Wagner T, Fields A. Acute hyponatremia and seizures in an infant after a swimming lesson. Pediatrics 1983;72(1):125-127.
- Noakes T, Goodwin N, Rayner B, et al. Water intoxication: A possible complication during endurance exercise. Med Sci Sports Exerc 1985;17(3):370-375.
- Frizzell RT, Lang GH, Lowance DC, et al. Hyponatremia and ultramarathon running. JAMA 1986;255:772-774.
- Rosner MH, Kirven J. Exercise-associated hyponatremia. Clin J Am Soc Nephrol 2007;2:151-161.
- Almond CS, Shin AY, Fortescue EB, et al. Hyponatremia among runners in the boston marathon. N Engl J Med 2005;352(15):1550-1556.
- Wagner S, Knechtle B, Knechtle P, et al. Higher prevalence of exercise-associated hyponatremia in female than in male open-water ultra-endurance swimmers: The marathon-swim’ in lake zurich. Eur J Appl Physiol 2012;112(3):1095-1106.
- Ayus JC, Varon J, Arieff AI. Hyponatremia, cerebral edema, and non-cardiogenic pulmonary edema in marathon runners. Ann Intern Med 2000;132:711-714.
- Smith S. Marathon runner’s death linked to excessive fluid intake. The New York Times August 13, 2002.
- Nearman S. Local woman dies two days after race. Washington Times October 30, 2002.
- Blanc P, Carbajal R, Paupe A, et al. Water intoxication following preparation for barium enema. Arch Pediatr 1995;2(9):871-873.
- Chertow GM, Brady HR. Hyponatraemia from tap-water enema. Lancet 1994;344(8924):748.
- Arieff A, Kronlund B. Fatal child abuse by forced water intoxication. Pediatrics 1999;103(6):1292-1295.
- Hariprasad MK, Eisinger RP, Nadler IM, et al. Hyponatremia in psychogenic polydipsia. Arch Intern Med 1980;140(12):1639-1642.
- Hayashi T, Ishida Y, Miyashita T, et al. Fatal water intoxication in a schizophrenic patient — an autopsy case. J Clin Forensic Med 2005;12(3):157-159.
- Adebamiro A, Perazella MA. Recurrent acute kidney injury following bath salts intoxication. Am J Kidney Dis 2012;59(2):273-275.
- van Dijken GD, Blom RE, Hene RJ, Boer WH. High incidence of mild hyponatraemia in females using ecstasy at a rave party. Nephrol Dial Transplant 2013;28:2277-2283.
- Weisberg LS. Pseudohyponatremia: A reappraisal. Am J Med 1989;86(3):315-318.
- Frier BM, Steer CR, Baird JD, et al. Misleading plasma electrolytes in diabetic children with severe hyperlipidaemia. Arch Dis Child 1980;55(10):771-775.
- Easley D, Tillman E. Hospital-acquired hyponatremia in pediatric patients: A review of the literature. J Pediatr Pharmacol Ther 2013;18(2):105-111.
- Armon K, Riordan A, Playfor S. Hyponatremia and hypokalemia during intravenous fluid administration. Arch Dis Child 2008;93(4):285-287.
- Hanna M, Saberi M. Incidence of hyponatremia in children with gastroenteritis treated with hypotonic intravenous fluids. Pediatr Nephrol 2010;25(8):1471-1475.
- Eulemesekian P, Perez A, Minces P, Bohn A. Hospital acquired hyponatremia in post-operative patients: Prospective observational study. Pediatr Crit Care Med 2010;11(4):479-483.
- Kannan L, Lodha R, Vivekanandhan S, et al. Intravenous fluid regimen and hyponatremia among children: A randomized controlled trial. Pediatr Nephol 2010;25:2303-2309.
- Yung M, Keeley S. Randomized controlled trial of intravenous maintenance fluids. J Paediatr Child Health 2009;45(1-2):9-14.
- Neville K, Sandeman D, Rubinstein A, et al. Prevention of hyponatremia during maintenance intravenous fluid administration: A prospective randomized study of fluid type versus fluid rate. J Pediatr 2010;156(2):313-319.
- Choong K, Arora S, Cheng J, et al. Hypotonic versus isotonic maintenance fluids after surgery for children: A randomized controlled trial. Pediatrics 2011;125(5):857-866.
- Saba T, Fairbairn J, Houghton F. A randomized controlled trial of isotonic versus hypotonic maintenance intravenous fluids in hospitalized children. BMC Pediatr 2011;23(11):82-91.
- Au A, Ray P, McByrde K. Incidence of postoperative hyponatremia and complications in critically ill children treated with hyponatremic and normotonic solutions. J Pediatr 2008;152(1):33-38.
- Rey C, Los-Arcos M, Hernandez A. Hypotonic versus isotonic fluid as maintenance fluids in critically ill children: A multicenter prospective randomized study. Acta Paediatr 2011;100(8):1138-1143.
- Montañana P, Alapont VM, Ocon A. The use of isotonic fluid as maintenance therapy prevents iatrogenic hyponatremia in pediatrics: A randomized, controlled open study. Pediatr Crit Care Med 2008;9(6):589-597.
- Koczmara C, Wade A, Skippen P, et al. Hospital acquired acute hyponatremia and report of pediatric deaths. Dynamics 2010;21(1):21-26.
- Jackson J, Bolte RG. Risks of intravenous administration of hypotonic fluids for pediatric patients in ED and prehospital settings: Let’s remove the handle from the pump. Am J Emerg Med 2000;18(3):269-270.
- Moritz ML, Ayus JC. Prevention of hospital-acquired hyponatremia: Do we have the answers? Pediatrics 2011;128(5):980-983.
- Moritz ML, Ayus JC. Prevention of hospital-acquired hyponatremia: A case for using isotonic saline. Pediatrics 2003;111(2):227-230.
- Moritz ML, Ayus JC. Intravenous fluid management for the acutely ill child. Curr Opin Pediatr 2011;23(2):186-193.
- ISMP warns that IV solutions administered post-op can cause low sodium levels and death in healthy children. Institute for Safe Medication Practices. August 14, 2009.
- Sterns RH, Riggs JE, Schochet SS, Jr. Osmotic demyelination syndrome following correction of hyponatremia. N Engl J Med 1986;314(24):1535-1542.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
