Collaborative effort in Washington state slashes non-essential use of the ED by Medicaid patients, delivering millions in projected savings
Collaborative effort in Washington state slashes non-essential use of the ED by Medicaid patients, delivering millions in projected savings
Emergency providers say the approach can work in other states, too, but a collaborative framework is key.
An unprecedented, state-wide effort aimed at curbing non-essential use of the ED by Medicaid recipients appears to be making an impact in Washington state. Preliminary results, including data from the first six months of the initiative, suggest the “ER is for Emergencies Program” is saving the state more than 10% in Medicaid fee-for-service emergency costs, and that accumulated savings could reach $31 million in the program’s first year, slightly exceeding initial goals. These findings are included in Emergency Department Utilization: Assumed Savings from Best Practices Implementation, a report to the Washington state legislature by the Washington State Health Care Authority (WSHCA), one of the groups that spearheaded the approach, along with the Washington Chapter of the American College of Emergency Physicians (WA-ACEP), the Washington State Hospital Association (WSHA), and the Washington State Medical Association (WSMA).
Other findings in the report include a 23% reduction in ED visits among Medicaid recipients with five or more visits, a 250% increase in the number of providers who have registered in the state’s Prescription Monitoring Program, a database designed to facilitate the identification of patients with narcotic-seeking behavior. In addition, the number of shared care plans, intended to improve care coordination for patients, has doubled, and the number of hospitals exchanging ED information electronically has grown from 17 to 85. (The full report from WSHCA can be accessed at www.hca.wa.gov/leg_reports.html.)
There is no question that this is an auspicious beginning for the program — particularly considering the contentious back and forth that prompted its creation in the first place. The state legislature had first threatened to limit Medicaid payments to EDs for visits or conditions deemed not medically necessary or appropriate for the emergency setting. The legislators backed down when the state’s emergency physicians came up with the outlines of what became the “ER is for Emergencies Program.”
Now that the approach is getting positive results, ED leaders and politicians in other states are eyeing the approach to see if a similar effort might work elsewhere. Indeed, in a news release coinciding with WSHCA’s report on the program, Andrew Sama, MD, FACEP, the president of ACEP, called the effort a “model for the nation,” and he noted the approach proves that medical providers can work together to improve patient care and save money.
Consider IT-driven communication tools
The “ER is for Emergencies Program” consists of seven best practices that were developed by WA-ACEP, in collaboration with the other partnering groups. The seven best practices include:
- Adoption of an emergency department information exchange (EDIE) so that EDs can quickly share information about patient visits to other hospitals;
- Education for patients about appropriate use of the ED;
- A process for disseminating lists of frequent users so that they can be identified by the EDIE;
- A process to equip frequent users with care plans and assist them in getting in to see their PCPs within 72 to 96 hours of their ED visit;
- Adoption of strict guidelines for the prescribing of narcotics;
- Provider enrollment in a state Prescription Monitoring Program (PMP), so that providers can see in an online database what prescriptions have been previously filled by patients; and
- Regular review of feedback reports on ED utilization so that hospitals can take corrective action, where needed.
While there were certainly technical challenges on a global level across the state to get the EDIE up and running, implementation of the best practices at the hospital level was not too overwhelming, explains Nathan Schlicher, MD, the associate medical director at St. Joseph Medical Center in Tacoma, WA, and a newly appointed state senator who is now on sabbatical from the ED so that he can attend the state’s legislative session. “Getting the feedback reports is something that takes some getting used to, but I think they are useful,” he says. “But [the seven best practices] were mostly things that physicians had wanted to see for a long time to make their jobs better, so getting people on board was not that difficult.”
Julianna Yu, MD, FACEP, the section head for emergency medicine at Virginia Mason Medical Center (VMMC) in Seattle, WA, says physicians there were also mostly supportive of the seven best practices, although there were some initial concerns that implementation of the stricter guidelines for narcotic prescribing would increase the number of patient complaints. However, she explains that ample use of educational signage and patient handouts that explain the narcotic prescribing policy, as well as why it is important, have gone a long way toward easing these concerns. (See patient handout, Fig. 1, below.)
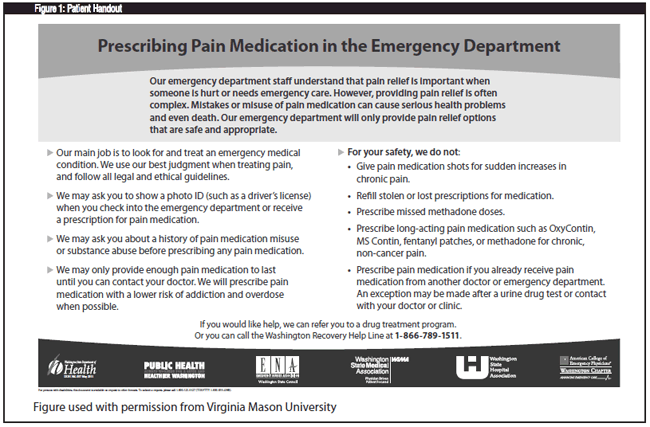
“One of the things we were able to demonstrate through the education of patients and providers was that there has been a marked increase in overdose deaths from prescription narcotics,” says Yu. “Having a lot of patient education visible in each of our treatment rooms, and having pamphlets and brochures to hand out to our patients at the time of the visit, have helped providers feel supported that they are really doing the right thing for our patients in the long run.”
In fact, the overall impact of the seven best practices in the ED at VMMC has been a gradual decrease in patient complaints over the past year, and an improvement in patient satisfaction, says Yu. “I think once things were really in place and our providers felt more comfortable with the day-to-day implementation of the seven best practices, they were able to see the benefits,” she adds.
In particular, Yu explains that the EDIE has been a valuable tool for conserving resources. “Since it is an information-sharing system between all of the Washington state EDs, it really helps EDs communicate with each other in a timely manner so that we can reduce over-testing and identify patients who are high-utilizers of emergency services,” she says. “For example, if we have a patient who has been at a nearby ED, perhaps that same day, and has had blood work and X-rays done, we are able to access that information right away when the patient arrives, so we can discuss any concerns with the patient up front and reduce over-testing.”
In addition, the state’s Prescription Monitoring Program has strengthened opioid guidelines that VMMC had put in place in 2011. “We had some time even before the seven best practices to really start focusing in on that aspect of emergency care, but once the state policy took effect in mid-2012, it helped to insure we are prescribing narcotics appropriately from the ED,” says Yu.
“We are able to pull up patient prescribing histories at the time of an ED visit.”
Watch for unintended consequences
From the start of the approach, emergency providers have been monitoring the program’s impact to make sure there are no unintended consequences from the effort, says Schlicher. “Right now, we haven’t seen that. People are still able to get care,” he says. “If anything, care is safer because patients who may have addiction issues or other reasons why they are shopping between hospitals are now receiving coordinated care, so they have stopped getting as many CT scans or other procedures than they were before we had any idea that they were shopping between institutions.”
In fact, making sure that there are no unintended consequences going forward is one of the reasons why Schlicher is now serving a stint in the state senate. “I want to be there as a physician and patient advocate to make those [potential consequences] clear ahead of time so that we don’t get into this kind of situation again,” he says.
Further, while the seven best practices have had a positive impact to date, Schlicher emphasizes that there is still ample room for further improvement to emergency care. In particular, he stresses that the state has done “a very poor job” with respect to mental health. “We have a long way to go. There are some laws we need to clean up, we need to work on increasing funding for mental health, and we really need to see how we can better utilize the resources we have,” he explains.
Yu agrees, noting that many patients with behavioral health needs have seen funding slashed for ongoing outpatient mental health care. “Many of these patients have a lot of social needs, so they are frequenting the ED, not necessarily for narcotics, but because they have struggles with coordinating their outpatient care, accessing follow-up appointments with their primary care providers, or getting regular refills for their chronic care medicines,” she explains.
Emergency departments across the state are also still seeing patients with unmet dental care needs, adds Yu. “Dental care is still a struggle for a lot of our patients,” she says. “So once we reduce their unnecessary use of the ED, we need to make sure that we have the appropriate outpatient resources available to these patients.”
While hefty challenges remain, Schlicher points out that there is now an infrastructure in place to assist stakeholders in working toward collaborative solutions. It is the kind of framework that he advises ED leaders and policy makers in other states to build. “I think it is really about building a coalition of the willing,” he says. “That is what we did. We got the hospitals and the medical associations together and we looked at this from the standpoint of: How can we improve our practice to deliver better patient care in a way that saves the state money? The elements that we came up with do all of those things.”
In the past, Schlicher notes that there were many instances in which health care organizations did not come to the table and propose a solution. “This time we did because we thought it was right and we wanted to try to rehabilitate a broken, strained relationship,” he says. “I think many ED providers struggle with that same challenge. I would just encourage them to look at the problem from a team work and collaborative basis rather than an adversarial one.”
Sources
- Nathan Schlicher, MD, Associate Medical Director, St. Joseph Medical Center, Tacoma, WA. E-mail: [email protected].
- Julianna Yu, MD, FACEP, Section Head, Emergency Medicine, Virginia Mason Medical Center, Seattle, WA. Phone: 206-583-6433.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
