Pediatric Spinal Trauma
Pediatric Spinal Trauma
Authors: Matthew DeLaney, MD, Assistant Professor, Department of Emergency Medicine, University of Alabama at Birmingham
Jason Booton, MD, Department of Emergency Medicine, University of Alabama at Birmingham
Peer Reviewer: Dennis A. Hernandez, MD, FAAP, FACEP, Medical Director, Pediatric Emergency Services, Florida Hospital, Core Faculty, Emergency Medicine Residency, Florida Hospital, Orlando
Spinal trauma is a rare yet important category of injury. Children account for 10% of spinal injuries, but account for 25% of the mortality. Pediatric patients who present with possible spinal injury pose several unique challenges to the emergency department provider. Unique anatomic and developmental features place pediatric patients at risk for spinal injuries that are not typically seen in the adult population. In addition, unlike adult patients, there is little consensus on the most appropriate workup for potentially injured patients. When evaluating pediatric patients, practitioners must balance the limited available clinical data with the risks and benefits of various imaging modalities. The authors review the spectrum of pediatric spinal injury.
— Ann M. Dietrich, MD, Editor
Epidemiology
Sixty to eighty percent of spinal injuries in children occur in the cervical region. The remaining 20-40% are split evenly between the thoracic and lumbar region. Boys are more likely than girls to experience spinal trauma. Despite developmental anatomy that places young patients at risk for spinal trauma, 76% of all spinal cord injuries occur in children older than the age of 8 years.1 Across all age groups, motor vehicle accidents are the most common mechanism of injury. Vitale et al found that of those injured in motor vehicle accidents, 67.7% were not wearing a seat belt.2 In addition to motor vehicle accidents, there is wide variability in the mechanisms of spinal injury in children. As children grow from infants, to toddlers, and finally to school age and adolescence, various mechanisms of injury become more prevalent.
Birth-associated trauma is a category of injury that is unique to infants. Rehan and Seshia estimated that spinal injury occurs in 1 in 29,000 live births.3 Aggressive delivery techniques and abnormal fetal presentation are thought to be responsible for the majority of injuries. Abrams found that 75% of newborn spinal injuries occurred in patients in the breech position.4
Toddlers retain the spinal instability and accompanying risk for high cervical injury. In addition to structural immaturity, young children who are learning to walk lack the dexterity, coordination, and fine-tuned protective reflexes that prevent falls and limit trauma later in life. As children start to walk, falls from ground level become a common mechanism of injury.
As children begin school and start participating in organized sports, athletics-related injuries are responsible for the largest number of spinal injuries. Among all sports, football causes the greatest number of injuries.5 The high number of football-related injuries is likely secondary to widespread participation in the sport rather than an indication of a disproportionate level of danger. Other less widely played sports such as gymnastics and diving account for a significant number of injuries.6 Caine et al found that the incidence of sports-related spinal injury increased with the age of the participants. As children grow, the strength, speed, and level of competition contributes to increased energy in collisions and an increased incidence of spinal cord injury.7 Teenagers are also at greatest risk for penetrating spinal injury, with gunshots being the most likely cause of penetrating trauma to the spine.
Cervical
Cervical fractures are the most common type of spinal injury, accounting for 56% of injuries. Dislocations and ligamentous combine to account for the remaining 44%. Older children show an increase in the incidence of bony injury, while younger children are more likely to experience dislocations or soft-tissue injury.8 Most cervical fractures occur in the region between the skull and C4. Due to their lack of anatomic maturity, children younger than 8 years are at increased risk for cervical spine trauma. The large majority of fatal spinal injuries occur in the cervical region. High cervical injuries, such as atlanto-occipital dislocation, occur almost twice as often in children when compared to adults. Fractures in the lower cervical spine show an increased association with maxillofacial trauma. After age 8 years, once the spine has matured, the incidence and injury patterns of trauma more closely approximate those of an adult.9
Pediatric patients are 2.5 times more likely to have an injury to the atlanto-occipital region. (See Figure 1.) Injury to this region occurs more frequently in younger children and accounts for 15% of fatal spinal injury.10 The stability at the interface between the skull and the spine is provided by a pair of alar ligaments that extend from the dens on C2 to the occipital condyles. Additional support is provided by the tectorial membrane, which is a continuation of the posterior longitudinal ligament that connects the dens to the skull in the region of the foramen magnum. These three ligaments provide the majority of the stabilization between the spine and the skull, as the atlas at C1 has no significant connection to the occiput. In children, the occipital condyles are relatively small, and when coupled with increased ligamentous laxity, there is a significant increase in the amount of motion that can occur, which leads to a higher incidence of disruptions at the interface of the skull and the spine.121
Figure 1. Atlanto-occipital, C1-C2 Injury
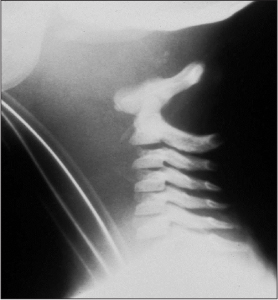
Thoracic
As with the cervical spine, thoracic and lumbar injuries occur most frequently as a result of motor vehicle accidents. In young children, isolated thoracic spine trauma can be seen in instances of child abuse. As children progress through school, sports-related trauma becomes a significant source of thoracic and lumbar injuries. Fractures in the thoracic region frequently involve multiple areas of bony injury and have a high rate of associated injuries. Forty percent of thoracic injuries have fractures at multiple spinal levels, and in one-third of the cases, the levels of injury are non-contiguous.12 Lumbar and thoracic injuries are commonly associated with injuries to the viscera and mesentery. Beaunoyer found that 37% of patients with thoracolumbar fractures after motor vehicle collisions required a laparotomy for non-orthopedic injuries.13
Sports-related injuries are responsible for a significant amount of pediatric spinal injury. At some point in their adolescent athletic careers, up to 30% of participants have acute low back pain, most commonly in the lumbar region.14 Sports such as diving, gymnastics, football, cheerleading, and wrestling that involve repetitive hyperextension, axial loading, twisting, and direct contact place the participant at higher risk of sustaining a lumbar injury. Football players have an increased rate of lumbar disc herniation, with even higher rates of injury in offensive and defensive linemen.15 Gymnasts are at increased risk of spondylolysis, spondylolisthesis, and lumbar disc degeneration. Sward et al found that up to 75% of competitive gymnasts had clinical evidence of disc degeneration. They found this rate to be significantly higher than the 31% rate of degeneration that they observed in a non-athletic patient population.16
Sacral fractures are a rare injury in both pediatric and adult trauma patients. In a retrospective analysis of more than 4000 pediatric trauma patients, Hart et al found that only 0.16% of patients had sacral fractures. Notably, all of the patients with sacral fractures were involved in high-velocity impact scenarios such as motor vehicle accidents or falls from a significant height.17 Fractures to the sacrum are often diagnosed based on physical exam findings and are thought to be frequently overlooked when patients have more severe trauma in other regions of the body. Dogan et al found no cases of neurologic deficit secondary to sacral fracture in their series on pediatric spinal trauma.18
Pathophysiology
Cervical. Children have multiple unique anatomical and biomechanical features that put them at risk for spinal cord injuries.19
A combination of increased head size and relative flexibility of the spinal column put children at risk for cervical spine injury. When compared to a mature adult, the pediatric cervical spine has a greater degree of flexibility and is able tolerate a significant amount of motion. The combination of underdeveloped paraspinal musculature and relative laxity of the ligaments and joint capsule allows for an increased amount of motion, which increases the likelihood of subluxation. In addition, the spine also has relatively horizontal facets, which limits articulation between vertebrae and allows for increased movement with flexion and extension. Prior to maturation, the upper cervical vertebrae show a slight physiologic wedging, which permits a greater degree of anterior movement and can contribute to cervical spine injury. The vertebrae themselves have multiple ossification centers that close throughout the first years of life. In young children, this delayed closure contributes to the overall increase in spinal laxity and hypermobility.20,21
In children, the size of their head often contributes to a greater portion of their overall weight than in adults. With increased head size overlying a relatively flexible cervical spine, pediatric patients are at risk for a “fulcrum” type effect. The cervical fulcrum of motion is located at C2/C3 until about 8 years of age, when growth and maturation shifts the fulcrum to C5/C6, where it remains throughout adulthood. In the age group younger than 8 years, caudal location of the fulcrum contributes to a significant number of high cervical and craniovertebral junction injuries. Children with conditions such as Marfan syndrome, achondroplasia, and Down syndrome have an increased amount of atlantoaxial instability and are thought to be at increased risk of cervical spine injury.22
Fractures in the area of C1 are rare, yet occur more than twice as often in children when compared to adults. Fractures to the ring of C1 are known as Jefferson fractures, and occur as a result of axial loading. Typically, these injuries occur secondary to diving-type accidents. Fractures to C2, odontoid fractures, are the most common location of cervical fracture in children. Hyperextension of the neck can result in bilateral pars interarticularis fractures, which are known as hangman’s fractures. This fracture pattern is seen most often in adolescents and adults, typically in the setting of contact sports or motor vehicle collisions. In a pediatric patient, this pattern of fracture should be concerning for possible non-accidental trauma.23
Traditionally, teachings held that children younger than 8 years had an increased occurrence of high cervical injury due to the location of their fulcrum, while children with mature spines were more likely to experience lower cervical spine injury, as seen in the adult population. Recent studies have drawn this generalization into question. Brown et al found that in sports-related trauma, in patients whose average age was 13.8 years, the large majority of trauma occurred in the C1-C4 region.24 Givens et al found that in a group of 20 children younger than 8 years of age with cervical spine trauma, 50% of the patients had an injury below the level of C4.25
SCIWORA. The pediatric spine has various features that give it a significant degree of flexibility. This laxity allows the pediatric spine to “bend before it breaks.” As a result, children are more at risk for soft-tissue injuries and can experience injuries to the spinal cord without any radiographic evidence. Spinal cord injury without radiographic abnormality, or SCIWORA, was first described by Pand and Wilberger in 1982. Initially the term was used to refer to patients who showed clinical signs of spinal cord injury without showing any bony abnormality on plain radiographs. SCIWORA was thought to occur due to the increased mobility of the pediatric spine. Cadaver studies have shown that the neonatal vertebral column can stretch 2 inches without disruption, while the spinal cord is only able to stretch 0.25 inches without showing signs of damage. Prior to spinal maturation around age 8, the pediatric spinal column is able to tolerate a significant amount of movement without incurring obvious signs of bony injury on radiographs. While the vertebral column has an increased range of motion, the spinal cord remains relatively immobile. The discrepancy in tolerable ranges of motion creates a situation in which spinal cord injury is possible without damaging the vertebral column.26
Younger children are at higher risk of SCIWORA due to the immaturity of their spinal column. As the spine matures, the risk of bony injury increases and the risk of SCIWORA decreases. The incidence of SCIWORA is difficult to verify, with estimates ranging from 5-67% of all cases of spinal trauma. In 2004, Pang found the mean incidence to be 34.8% in a review of studies that covered more than 40 years of literature.
The cervical spine has the highest incidence of SCIWORA, as this is typically the region of the spine with the largest range of motion. While most cases will occur in the cervical region, up to 15% of SCIWORA cases involve the thoracic spine. The upper thoracic spine is involved most often. This anatomic area is thought to be at higher risk of SCIWORA due to the presence of a watershed vascular supply zone and the distribution of nerve roots and dentate ligaments.27 Patients with thoracic SCIWORA typically have significant injuries to the thoracic, abdominal, or pelvic region, as it takes a significant amount of force to overcome the protective effect of the rib cage and cause injury to the thoracic spine. There are case reports of patients with lumbar and sacral SCIWORA-type injuries, but these are exceedingly rare.28
Two categories of SCIWORA-type injuries, delayed and recurrent, pose a particular diagnostic dilemma. In his initial study, Pang found that 52% of patients had a delay in symptom onset. The time of delay ranged from minutes up to four days. More than half of the patients in this study with a delayed onset of symptoms reported transient neurologic symptoms immediately following the initial injury.29 The etiology of the delay in symptom onset is somewhat unclear, with some authors hypothesizing that symptoms are a result of ongoing ischemia from an infarction in the spinal cord.30
Recurrent SCIWORA-type injuries comprise a second subset of patients.31 A recent study reported a 17% incidence of recurrent injuries; however, the incidence of these injuries seems to be declining as conservative spinal immobilization becomes more widespread.32,33 As the use of advanced neuroimaging such as MRI has become more widespread, the term SCIWORA has come under scrutiny. Previously, patients who displayed neurologic symptoms yet had unremarkable radiographs were diagnosed as having a SCIWORA-type injury. With the improved imaging capacity of MRI, spinal cord pathology is being visualized in patients who historically, with negative plain radiographs, would have been diagnosed with SCIWORA-type injury.
Thoracic Pathophysiology. The thoracolumbar junction is the most common site of injury. The thoracic spine is stiff and fairly immobile due in part to its kyphotic orientation and the support provided by ribs and intracostal musculature. The lumbar spine is lordotic and offers a much greater range of mobility. The interface between the relatively stiff thoracic spine and the flexible lumbar spine makes the thoracolumbar junction a high-risk area for injury.34
Lumbosacral Pathophysiology. While compression fractures account for the majority of fractures to the thoracic and lumbar spine, mechanisms of injury can have a significant effect on the fracture pattern.35 Axial loading typically results in a burst pattern, while hyperflexion destabilizes the posterior column and can result in a compression pattern of fracture. Flexion-distraction or “seat belt” injuries were originally described by Chance in 1948 and involve a compression fracture of the anterior column with a disruption of the posterior column.35 These injuries are usually secondary to hyperflexion, often due to being restrained by a seat belt. These injuries typically occur at the thoracolumbar junction and have associated visceral injury in up to 50% of the cases.36
Spondylolysis and spondylolisthesis are common causes of pediatric lumbar pain. The term spondylolysis can be used broadly to describe degenerative changes that occur in the vertebrae or can specifically refer to fractures or osteophytic changes that involve the pars interarticularis, which is the part of the vertebra between the superior and inferior facets. Spondylolysis can be caused by a congenital defect, may occur as a result of a specific traumatic event, or can occur as a result of repetitive stress and motion over time. Up to 5% of the general population is thought to have some degree of spondylolysis, and the incidence tends to increase with patient age. Significantly higher rates are found in athletes such as divers and gymnasts who perform repeated hyperextension of the lumbar spine.37 Although spondylolysis can occur throughout the length of the spine, the lumbar and sacral spine are most commonly affected in pediatric patients. The most common area of involvement is the L5/S1 interface.38
Spondylolisthesis refers to the anterior or posterior displacement of one vertebra on another. This slippage can be caused by a single event or, more commonly, can occur as a result of a defect in the pars interarticularis. Spondylolysis is a specific risk factor for developing spondylolisthesis, and it is estimated that 30% of patients with spondylolysis will develop some component of spondylolithesis. As with spondylolysis, athletes are thought to have an increased rate of spondylolisthesis. Athletes who have repetitive hyperextension are more likely to develop spondylolytic changes, which then increase the likelihood of developing vertebral displacement or spondylolisthesis. Mayer et al found that up to 15% of high school athletes had significant vertebral displacement seen on screening lumbar radiographs.39
Sacral fractures are typically a result of high-velocity injuries. The sacrum articulates with the bony pelvis. This anatomic association protects the sacrum from significant damage during lower-impact injuries. In order for the sacrum to be injured, the body must be placed under a significant amount of stress and strain. When enough force is applied to cause an injury to the sacrum, there is a significant rate of injury to the adjacent body structures, as the force needed to injure the sacrum is likely to injure the pelvis as well. While sacral fractures are rare, it is estimated that up to 50% of patients with a sacral fracture will have a concomitant pelvic fracture.40
Differential Diagnosis
Providers should keep a broad differential diagnosis in pediatric patients with suspected spinal trauma. Often these patients will have a significant mechanism of injury and have a high rate of injury to other parts of the body. Providers in the emergency department should perform a complete physical exam on any patient with suspected spinal trauma to ensure that there are no other associated injuries.
Diagnosis
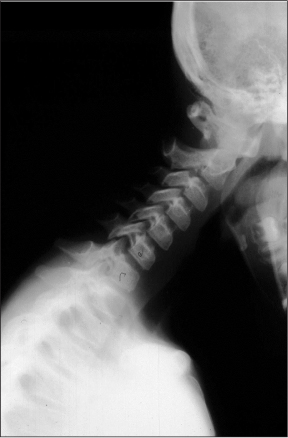
Plain Films. Plain radiographs are the most appropriate initial screening test for patients suspected of having spinal trauma. For pediatric patients, the lateral cervical spine radiograph has the highest sensitivity for detecting cervical spine injury when compared to other views using plain radiographs. (See Figure 2.)
Figure 2. Cervical Spine Fracture on Lateral Cervical Spine Radiograph
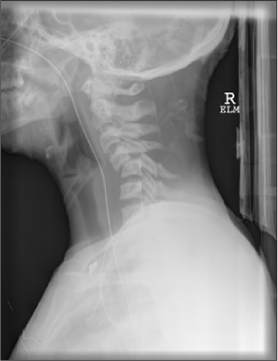
Silva et al examined the role that various plain radiographs play in the workup of suspected cervical spine injury. When compared to a gold standard of a CT scan, the lateral radiograph had the highest sensitivity. Adding additional views such as the open-mouth odontoid view did not improve the sensitivity and caused a decrease in specificity.41 (See Figure 3.) Additional studies have found that lateral and AP radiographs were able to identify 87% of cervical spine injuries in patients younger than 9 years old. Adding other views did not improve the diagnostic accuracy.
Figure 3. Normal Open Mouth View
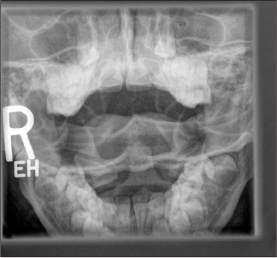
Other views such as the odontoid view can be difficult to obtain in young children, and are not typically needed when evaluating a pediatric patient.42 Oblique views, which can increase the sensitivity of plain films in the detection of cervical spine injury in adult patients, have not been shown to have the same benefit in pediatric patients.43 Children who present with possible cervical spine injury should have an anteroposterior and a lateral radiograph performed as part of their initial evaluation in the emergency department. (See Figure 4.)
Figure 4. Normal AP Spine Film
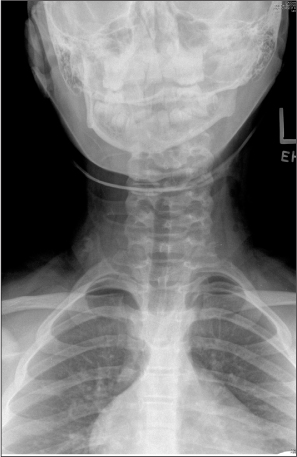
When evaluating pediatric cervical spine radiographs, providers should be aware of pseudo-subluxation of the cervical spine. Pseudo-subluxation occurs when there is anterior displacement of the vertebrae. This radiographic finding can be a result of cervical spine injury, but more commonly is a normal variant. Cattell et al found 3 mm of anterior displacement at C2/3 in 40% of patients, and 14% of patients had displacement at C3/4. While this anterior displacement can be a normal variant, any child with a history of trauma, pain in the cervical region, and an abnormal-appearing radiograph should be treated as if he or she has a legitimate cervical spine injury until proven otherwise.44
In addition to pseudo-subluxation, there are several other normal radiographic variants that can be seen in children. Findings such as a lack of cervical lordosis, anterior vertebral wedging, or a widened atlantoaxial distance are often pathologic in adult patients, but can be seen sometimes in pediatric patients.45 While these normal anatomic variants may mimic underlying disease, patients who have a concerning exam in the area of these findings should be treated as if they have a significant cervical spine injury until further studies can be obtained.
Historically, flexion-extension radiographs have been used to evaluate patients who were thought to have a potential ligamentous injury. (See Figure 5.) Typically, these patients would have neurologic deficits without an obvious fracture on traditional radiographs. Flexion-extension films can be difficult to obtain, with up to 50% of adults being unable to undergo adequate imaging. Often the exam is limited due to patient pain and muscle spasm.46 When compared to CT scans, flexion-extension films offer little diagnostic yield. Dwek et al found that in patients who had a normal anteroposterior and lateral radiograph, the flexion-extension radiographs did not offer any increase in diagnostic yield.47 Patients with suspected ligamentous injury and negative plain films should undergo MRI or CT scan rather than having flexion-extension radiographs performed.
Figure 5. Flexion/extension Film That Shows C6/C7 Ligamentous Injury
Pediatric patients with suspected thoracic and lumbar injury can be evaluated using anteroposterior and lateral radiographs. Typically, a significant, high-energy mechanism is required to cause injury to the thoracic and lumbar region. Patients who are at risk for spinal injury to this area have an increased rate of systemic injury and likely need further evaluation with CT scan or MRI. For patients with a significant mechanism of injury, CT scans of the thorax and abdomen can be used to obtain reformatted images of the spine, rather than obtaining separate spinal images.48
Sacral fractures in children may not be appreciated on the standard radiographs that are ordered as part of the patient’s workup. Hart et al17 found that only 30% of patients with spinal injury had specific imaging of the sacrum performed. In adult patients, typical views such as the anteroposterior pelvis or Judet views can be suboptimal in terms of identifying sacral fractures. It is thought that pediatric patients who have these studies performed may have a similar rate of missed fracture. Lateral or 30-degree cephalad sacral views provide a more adequate view of the sacrum in a patient with suspected injury. Given the high incidence of pelvic fractures in the setting of sacral fractures, and the high forces necessary to generate these types of injuries, patients with a high pre-test probability of sacral or pelvic injury should undergo a pelvic CT scan.49
CT
CT scan is more accurate at identifying spinal injury when compared to plain radiographs. Despite its superior diagnostic characteristics, performing a CT scan on a pediatric patient involves exposure to a considerable amount of radiation and is not a benign endeavor. The biggest risk from CT scans is the associated exposure to ionizing radiation. There is thought to be a linear association between exposure to radiation and the development of thyroid cancer later in life. The highest levels of association have been found in children younger than the age of 15 years. While the exact rate of malignancy is somewhat difficult to pinpoint, all efforts should be made to limit the amount of radiation used during the evaluation of pediatric trauma patients.50
While CT scan is superior to plain radiographs in identifying bony injury, it should not be used routinely to clear the entire cervical spine. Guidelines from the American Association of Neurological Surgeons state that “CT of the cervical spine should be used judiciously to define bony anatomy at specific levels but is not recommended as a means to clear the entire cervical spine in children.”51
While bony injury can typically be detected on plain radiographs, there is a high rate of missed cervical spine fractures during the initial assessment of pediatric trauma patients. Avellino et al reported a misdiagnosis rate of 19% by emergency providers during the initial evaluation of patients with suspected cervical spine injury. Fourteen percent of the patients were diagnosed as having fractures that were later found to be normal anatomic variations. Five percent of the patients had true missed fractures that were not appreciated during the initial assessment. Plain radiographs can be difficult to interpret in the pediatric patient, and there is a significant rate of missed cervical spine fractures during the initial evaluation. Providers should consider CT scan with reformatted views if there is continued clinical concern for spinal injury after the initial assessment.52 (See Figures 6, 7, and 8.)
Figure 6. CT of Cervical Spine Fracture
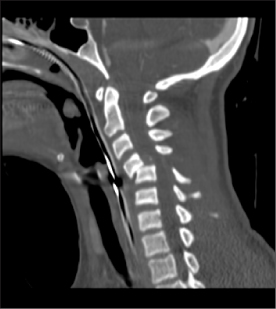
Figure 7. CT of Cervical Spine Fracture
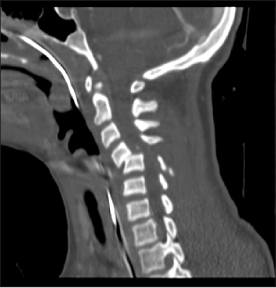
Figure 8. CT of Cervical Spine Fracture
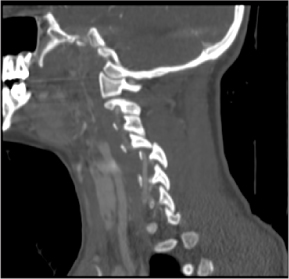
CT scans may be useful in evaluating pediatric patients who are thought to have a high risk of cervical spine injury. There are limited data to suggest that CT scan may be helpful in identifying bony injury in obtunded pediatric patients. In a review of the literature on pediatric cervical spine injury, Slack et al suggest that CT scan should be considered in obtunded pediatric trauma patients when an exam is limited or unobtainable.53 Keenan et al found that in children who presented with head injury, performing a CT scan during the initial evaluation actually reduced the number of repeat radiographs that were needed to evaluate the cervical spine during the course of the patient’s hospitalization. While CT scans may reduce the subsequent exposure to radiation, the provider must weigh this benefit with the significant exposure to radiation when a CT scan is used over plain radiographs during the initial assessment.54
In addition to the risk from exposure to radiation, CT scan has some technical limitations that make it less useful in the workup of a certain subset of pediatric trauma patients. In children younger than the age of 5 years, ligamentous injury is much more common than bony injury. Although CT scan outperforms plain radiography in its ability to detect bony injury, it is much less sensitive in terms of detecting ligamentous injury. In these patients with possible ligamentous injury, CT scans will often add little information that cannot be obtained from the plain radiographs. In a retrospective review of more than 600 cases, Hernandez et al looked at the role of CT when compared to plain radiographs in the workup of pediatric trauma patients with suspected cervical spine injury. While only 2.7% of patients had a cervical spine injury, all of these patients had abnormal diagnostic findings on their plain radiographs. There were no cases in which the CT scan showed any new significant findings. Given this very low yield, the authors concluded that there was little to no role for CT scan in patients younger than the age of 5 years.55 Given the insensitivity of CT scan in detecting ligamentous injury, the adequacy of plain radiographs, and the exposure to ionizing radiation, various authors have suggested that CT plays a very limited role in the workup of pediatric patients with suspected cervical spine injury.56
MRI
Magnetic resonance imaging, or MRI, is better than CT scan at identifying ligamentous or soft-tissue injury to the cervical spine. Given the somewhat limited availability of MRI in most emergency departments, it is not commonly used as the first imaging modality during the initial assessment of a pediatric trauma patient. In young patients who are non-verbal or in older patients who are obtunded, MRI has been shown to be useful in evaluating the cervical spine.
Flynn et al looked at the role that MRI plays in the evaluation of children with suspected spinal cord injury. MRIs were obtained if the patient was obtunded or non-verbal, had equivocal plain films, had neurologic symptoms without abnormality on plain radiograph, or if the patient had continued pain on clinical testing after three days of immobilization. In the group of children who underwent MRI, 66% had the initial diagnosis confirmed, and 34% received a new diagnosis based on the MRI results.57 For the majority of pediatric trauma patients, MRI is not necessary, as plain radiographs and the physical exam can be used to identify or exclude the large majority of cases; however, it may be a helpful study in patients in whom the exam is limited or the workup remains somewhat equivocal.
For pediatric trauma patients, the history and physical exam should be the primary factors that determine which imaging studies, if any, need to be obtained. Plain radiographs are typically the most appropriate screening study for spinal injury. With a low clinical suspicion of injury and negative radiographs, patients likely do not need further imaging. CT scan has a limited role in the evaluation of the cervical spine, but can be useful in evaluating thoracic and lumbar trauma, in which there is an increased risk of coexisting trauma. When the physical exam is limited by clinical condition, or if the initial workup is inconclusive or the patient has an abnormal neurologic exam, MRI can provide added clinical information.23
Emergency Department Management
Typically patients arrive in the emergency department with spinal immobilization in place that was started by the pre-hospital providers. Despite the widespread prevalence of spinal immobilization protocols, the science behind these practices is somewhat limited. In 2009, a Cochrane Collaboration systematic review looked at the role of spinal immobilization and found no connection between immobilization and mortality, neurologic injury, or spinal stability. Despite the lack of evidence for its use, it is standard practice to immobilize patients with suspected spinal injury.58 Placing patients in spinal immobilization is not always a benign intervention. Patients who have their spines immobilized have an increase in pain and have been noted to have a diminished forced vital capacity.59 The goal of spinal immobilization is to keep the patient in a neutral position. In a child, maintaining a neutral position can be difficult given the size of the child’s head relative to the rest of the body. Curran et al examined various immobilization techniques used in pediatric patients with suspected spinal trauma. Up to 20% of pediatric patients placed on a spinal backboard were noted to have greater than 10 degrees of cervical flexion.60 Some authors have suggested that elevating the patient’s thorax can lessen the amount of cervical flexion. This approach can be problematic in a trauma patient who may have both cervical and thoracic injury, as manipulating the thoracic region could worsen an underlying injury.61 Given the limited evidence for spinal immobilization and the reported risk involved, patients should be evaluated promptly and immobilization should be removed as soon as is clinically possible.
Clearing the cervical spine in a pediatric trauma patient can be difficult. Given the lack of validated clinical decision rules, and the wide variety of imaging modalities, there is significant variation in the approach taken to evaluate these patients. While no low-risk clinical criteria have been prospectively validated in pediatric patients, if a patient is verbal, has a normal exam, and lacks any obvious high-risk features, it is reasonable to remove the cervical collar without further testing. In patients with pain on exam or higher suspicion of injury, plain radiographs should be the initial imaging study. CT scan can be used to clarify any areas on plain film that are concerning for bony injury. MRI is the study of choice in patients who are obtunded, have abnormal neurologic findings, or in any patient with suspected ligamentous injury. Patients with significant spinal injury will require inpatient management. Patients with a benign exam can be safely discharged from the emergency department.
Various authors have proposed a similar approach to clearing the cervical spine in the emergency department. The biggest point of debate typically involves the definition of high-risk criteria. The goal of identifying these high-risk elements of the exam or history is to establish a pre-test probability of spinal injury. While multiple studies have attempted to identify these features, there is still not a standard set of criteria that has been widely validated, as there is with adult patients and the NEXUS and Canadian Cervical Spine Rule decision rules. With ongoing debate about the features that help determine the pre-test probability of spinal injury, it is difficult to establish a widely accepted algorithm for the clinical clearance of the pediatric cervical spine. As a result, there is moderate variation in the approach taken to the pediatric trauma patient between various institutions.62
Clinical Decision Rules
Several clinical decision rules exist in an effort to use clinical criteria to identify patients with a cervical spine injury. Decision tools such as the NEXUS and Canadian Cervical Spine Rule were not designed specifically to evaluate the pediatric trauma patient. While some authors have attempted to validate these criteria in pediatric patients, there are significant limitations to using this approach to exclude a cervical spine injury. In addition, several authors have attempted to derive independent criteria that can exclude pediatric cervical spine injury. To date, there is not a clinical decision rule that has adequate performance to identify or exclude a pediatric spinal injury.
The NEXUS criteria was derived from a large prospective study. The criteria consist of five clinical features. The high-risk clinical features were identified as altered mental status, intoxication, focal neurologic deficit, cervical spine tenderness, and distracting injury. If a trauma patient had none of these high-risk features, the criteria were found to be approximately 99% sensitive for excluding cervical spine injury.63
Viccellio et al applied these NEXUS criteria to pediatric trauma patients. In looking at 3065 pediatric patients younger than the age of 18 years, 2160 were between 8 and 17 years of age. Out of the thousands of patients enrolled, there were only 30 cases of cervical spine injury. Among the injured patients, only four of the 30 were younger than 9 years old, and there were no injured patients younger than the age of 2 years. The authors of this study reported a 100% sensitivity (95% confidence interval: 87.8%-100%) in identifying cervical spine injury when applying NEXUS criteria to pediatric patients. There were several notable limitations to this study. First, the rate of cervical spine injury across all pediatric age groups was very low. Notably, there were no patients with injury younger than the age of 2 years. In addition, cervical spine tenderness was the most common characteristic identified in patients with cervical spine injury. In young, pre-verbal children, it can be very difficult to accurately identify spinal tenderness to palpation. While NEXUS criteria may be used reliably in older pediatric trauma patients, there are significant limitations to using them to evaluate younger children who present with possible cervical spine injury.64
Given the difficulty that young children have in identifying spinal tenderness, several authors have examined modified protocols based on the original NEXUS criteria. Anderson et al examined 575 pediatric trauma patients between the ages of 0 and 3 years of age who were admitted to the hospital. In addition to applying the NEXUS criteria, all of these patients underwent plain cervical spine radiography. By combining the radiographs with the high-risk features from the initial NEXUS study, cervical spine injury could be excluded in approximately 80% of the admitted patients without further testing.65
The Canadian Cervical Spine Rule involves a set of criteria that attempts to identify patients who are at low risk of having clinically important cervical spine injury. In adult patients, this rule has been reported to have a superior sensitivity and specificity when compared to the NEXUS criteria.66 As with the NEXUS criteria, various authors have attempted to evaluate pediatric trauma patients using the CCR criteria. Ehrlich et al found that the Canadian Cervical Spine Rule had a sensitivity of 86% and a specificity of 94% when applied to trauma patients younger than 10 years of age. This study was limited both by its retrospective design and the limited prevalence of pediatric cervical spine injury. Given the limited performance of the Canadian Cervical Spine Rule when applied to pediatric patients, this criterion should not be used to risk-stratify pediatric trauma patients.67
There are no well-validated clinical prediction rules that can be used to identify cervical spine injury in pediatric patients. Various authors have proposed various decision instruments to evaluate pediatric patients; however, most of these studies are either retrospective or have very small numbers of enrolled patients. Lee et al identified 10 high-risk criteria. In a study of 56 patients, there were no cases of missed cervical spine injury if none of the criteria were met.68
Pieretti-Vanmarcke et al used four criteria in a retrospective analysis of trauma patients between the ages of 0 and 3 years of age. High-risk criteria consisted of an overall Glasgow coma score of less than 14, a GCS eye opening score of 1, being involved in a motor vehicle collision, and age greater than 2 years. While the retrospective design of this study is a significant limitation, the criteria had a negative predictive value of 99.9%.69
Leonard et al proposed eight risk factors for cervical spine injury. High-risk features were identified as altered mental status, intoxication, focal neurologic deficit, complaint of neck pain, substantial torso injury, high-risk motor vehicle accident or diving, predisposing condition, and torticollis. Patients who had none of these criteria were thought to have a low risk of cervical spine injury, with a sensitivity of 98% for the detection of significant cervical spine injury.70 Some of these studies show promise in identifying pediatric patients who are at risk for significant cervical spine injury. To date, none of these criteria have been prospectively validated, and providers should not rely heavily on these studies when evaluating pediatric patients. In addition to the methodological limitations, some of these criteria are so broad that they offer little diagnostic advantage over clinical gestalt. For example, Leonard et al label “complaint of neck pain” as a high-risk feature. While this chief complaint logically increases the pre-test probability of cervical spine trauma, most providers would not pursue a workup for spinal trauma in a patient who has no complaint of neck pain.
Summary
Pediatric spinal trauma presents a unique challenge to emergency practitioners. While not the most common type of injury seen in the emergency department, spinal trauma has a significant rate of morbidity, mortality, and associated injury. Rather than relying on a specific set of guidelines, providers must consider the mechanism of injury and physical exam in each patient, while weighing the risks and benefits of various testing modalities.
References
1. Mahan ST. Multiple level injuries in pediatric spinal trauma. J Trauma 2009;67:537-542.
2. Vitale MG, Goss JM, Matsumoto H, et al. J Pediatr Orthop 2007;26(6):745-749.
3. Rehan VK, Seshia MM. Spinal cord birth injury — diagnostic difficulties. Arch Dis Child 1993;69:92–94.
4. Abrams IF, Bresnan MJ, Zuckerman JE. Cervical cord injuries secondary to hypertension of the head in breech presentation. Obstet Gynecol 1973;41:369-378.
5. Cantu RC, Li YM, Abdulhamid M, et al. Return to play after cervical spine injury in sports. Curr Sports Med Rep 2013;12(1):14-17.
6. Mahan ST, Mooney DP, Karlin LI, et al. Multiple level injuries in pediatric spinal trauma. J Trauma 2009;67 (3):537-542.
7. Caine D, Caine C, Maffulli N. Incidence and distribution of pediatric sport-related injuries. Clin J Sport Med 2006;16(6):500-513.
8. Kokoska ER, Keller MS, Rallo MC, et al. Characteristics of pediatric cervical spine injuries. J Pediatr Surg 2001;36:100-105.
9. Cirak B, Ziegfeld S, Knight VM, et al. Spinal injuries in children. J Pediatr Surg 2004;39(4):607-612.
10. Hamilton MG, Myles ST. Pediatric spinal injury: Review of 61 deaths. J Neurosurg 1992;77(5):705-708.
11. Bonadio WA. Cervical spine trauma in children: Part I. General concepts, normal anatomy, radiographic evaluation. Am J Emerg Med 1993;11(2):158-165.
12. Slotkin JR, Lu Y, Wood KB. Thoracolumbar spinal trauma in children. Neurosurg Clin N Am 2007;18(4): 621-630.
13. Beaunoyer M, Lallier S, Blanchard H. Abdominal injuries associated with thoracolumbar fractures after motor vehicle collision. J Pediatr Surg 2001;36: 760-762.
14. Dreisinger TE, Nelso B. Management of back pain in athletes. Sports Med 1996;21(4):313-320.
15. Hsu WK. Performance-based outcomes following lumbar discectomy in professional athletes in the National Football League. Spine 2010;35(12):1247-1251.
16. Swärd L, Hellström M, Jacobsson B, et al. Disc degeneration and associated abnormalities of the spine in elite gymnasts. A magnetic resonance imaging study. Spine 1991;16(4):437-443.
17. Hart DJ, Wang MY, Griffith P, et al. Pediatric sacral fractures. Spine 2004;29(6):667-670.
18. Dogan, S, Safavi-Abbasi S, Theodore N, et al. Thoracolumbar and sacral spinal injuries in children and adolescents: A review of 89 cases. J Neurosurg (6 Suppl Pediatrics) 2007;106:426-433.
19. Cirak B, Ziegfeld S, Knight VM, et al. J Pediatr Surg 2004;39(4):607-612.
20. Roche C, Carty H. Spinal trauma in children. Pediatr Radiol 2001;31:677–700.
21. Reilly C. Pediatric spine trauma. J Bone and Joint Surg 2007;89 Suppl 1:98-107.
22. Nitecki S, Moir CR. Predictive factors of the outcome of traumatic cervical spine fracture in children. J Pediatric Surg 1994;29:1409-1411.
23. Egloff AM, Kadom N, Vezina G, et al. Pediatric cervical spine trauma imaging: A practical approach. Pediatr Radiol 2009;39(5):447-456.
24. Brown RL, Brunn MA, Garcia VF. Cervical spine injuries in children: A review of 103 patients treated consecutively at a level 1 pediatric trauma center. J Pediatric Surg 2001;36:1107-1114.
25. Givens TG, Polley KA, Smith GF, et al. Pediatric cervical spine injury: A three year experience. J Trauma 1996;41(2):310-314.
26. Pang D, Wilberger JE. Spinal cord injury without radiographic abnormalities in children. J Neurosurg 1982;57(1): 114-129.
27. Pang D. Spinal cord injury without radiographic abnormality in children, 2 decades later. Neurosurgery. 2004;55(6): 1325-1342.
28. Trumble J, Myslinski J. Lower thoracic SCIWORA in a 3-year-old child: Case report. Pediatr Emerg Care 2000;16(2):91-93.
29. Ergun A, Oder W. Pediatric care report of spinal cord injury without radiographic abnormality (SCIWORA): Case report and literature review. Spinal Cord 2003;41(4):249-253.
30. Dickman CA, Zabramski JM, Rekate HL, et al. Spinal cord injuries in children without radiographic abnormalities. West J Med 1993;158(1):67-68.
31. Launay F, Leet AI, Sponseller PD. Pediatric spinal cord injury without radiographic abnormality: A meta-analysis. Clin Orthop Relat Res 2005;(433): 166-170.
32. Pang D. Spinal cord injury without radiographic abnormality in children, 2 decades later. Neurosurgery 2004;55(6):1325-1342.
33. Patel CK, Truumees, Roscjgrimd, JS, et al. Evaluation and Treatment of Thoracolumbar Junction Trauma. The University of Pennsylvania Orthopaedic Journal 2002;15:7-12.
34. Santiago R, Guenther E, Carroll K, et al. The clinical presentation of pediatric thoracolumbar fractures. J Trauma 2006;60:187-192.
35. Chance GQ. Note on a type of flexion fracture of the spine. Br J Radiol 1948;21(249):452.
36. Roche C, Carty H. Spinal trauma in children. Pediatr Radiol 2001;31 (10): 677-700.
37. Holliday RA. Inflammatory diseases of the temporal bone: Evaluation with CT and MR. Semin Ultrasound CT MR 1989;10(3):213-235.
38. Belfi LM, Ortiz AO, Katz DS. Computed tomography evaluation of spondylolysis and spondylolisthesis in asymptomatic patients. Spine 2006;31(24):E907-910.
39. Mayer F, Bonaventura K, Cassel M, et al. Medical results of preparticipation examination in adolescent athletes. Br J Sports Med 2012;46(7):524-530.
40. Schmidek HH, Smith DA, Kristiansen TK. Sacral fractures. Neurosurgery 1984;15(5):735-746.
41. Silva CT, Doria AS, Traubici J, et al. Do additional views improve the diagnostic performance of cervical spine radiography in pediatric trauma? AJR Am J Roentgenol 2010;194(2):500-508.
42. Buhs C, Cullen M, Klein M, et al. The pediatric trauma C-spine: Is the ‘odontoid’ view necessary? J Pediatr Surg 2000;35(6):994-997.
43. Ralston ME, Ecklund K, Emans JB, et al. Role of oblique radiographs in blunt pediatric cervical spine injury. Pediatr Emerg Care 2003;19(2):68-72.
44. Cattell HS, Filtzer DL. Pseudo-subluxation and other normal variations in the cervical spine in children. A study of one hundred and sixty children. J Bone Joint Surg Am 1965;47(7):1295-1309.
45. Pizzutillo PD. Injury of the cervical spine in young children. Instr Course Lect 2006;55:633-639.
46. Como JJ, Diaz JJ, Dunham CM et-al. Practice management guidelines for identification of cervical spine injuries following trauma: Update from the eastern association for the surgery of trauma practice management guidelines committee. J Trauma 2009;67(3):651-659.
47. Dwek JR, Chung CB. Radiography of cervical spine injury in children: Are flexion-extension radiographs useful for acute trauma? AJR Am J Roentgenol 2000;174(6):1617-1619.
48. Slotkin JR, Lu Y, Wood KB. Thoracolumbar spinal trauma in children. Neurosurg Clin N Am 2007;18(4): 621-630.
49. Schmidek HH, Smith DA, Kristiansen TK. Sacral fractures. Neurosurgery 1984;15(5):735-746.
50. Ron E. Let’s not relive the past: A review of cancer risk after diagnostic or therapeutic irradiation. Pediatr Radiol 2002;32(10):739-744.
51. Management of pediatric cervical spine and spinal cord injuries. Neurosurgery 2002;50 (3 Suppl): S85-99.
52. Avellino AM, Mann FA, Grady MS, et al. The misdiagnosis of acute cervical spine injuries and fractures in infants and children: The 12-year experience of a level I pediatric and adult trauma center. Childs Nerv Syst 2005;21(2):122-127.
53. Slack SE, Clancy MJ. Clearing the cervical spine of paediatric trauma patients. Emerg Med J 2004;21(2):189-193.
54. Keenan HT, Hollingshead MC, Chung CJ, et al. Using CT of the cervical spine for early evaluation of pediatric patients with head trauma. AJR Am J Roentgenol 2001;177(6):1405-1409.
55. Hernandez JA, Chupik C, Swischuk LE. Cervical spine trauma in children under 5 years: Productivity of CT. Emerg Radiol 2004;10(4):176-178.
56. Basu S. Spinal injuries in children. Front Neurol 2012;3:96.
57. Flynn JM, Closkey RF, Mahboubi S, et al. Role of magnetic resonance imaging in the assessment of pediatric cervical spine injuries. J Pediatr Orthop 22(5): 573-577.
58. Jacobs LM, Schwartz R. Prospective analysis of acute cervical spine injury: A methodology to predict injury. Ann Emerg Med 1986;15(1):44-49.
59. Baker C, Kadish H, Schunk JE. Evaluation of pediatric cervical spine injuries. Am J Emerg Med 1999;17(3): 230-234.
60. Curran C, Dietrich AM, Bowman MJ, et al. Pediatric cervical-spine immobilization: Achieving neutral position? J Trauma 1995;39(4):729-732.
61. Herzenberg JE, Hensinger RN, Dedrick DK, et al. Emergency transport and positioning of young children who have an injury of the cervical spine. The standard backboard may be hazardous. J Bone Joint Surg Am 1989;71(1):15-22.
62. Chung S, Mikrogianakis A, Wales PW, et al. Trauma association of Canada Pediatric Subcommittee National Pediatric Cervical Spine Evaluation Pathway: Consensus guidelines. J Trauma 2011;70(4): 873-884.
63. Hoffman JR, Mower WR, Wolfson AB, et al. Validity of a set of clinical criteria to rule out injury to the cervical spine in patients with blunt trauma. National Emergency X-Radiography Utilization Study Group. N Engl J Med 2000;343(2):94-99.
64. Viccellio P, Simon H, Pressman BD, et al. A prospective multicenter study of cervical spine injury in children. Pediatrics 2001;108(2):E20.
65. Anderson RC, Kan P, Vanaman M, et al. Utility of a cervical spine clearance protocol after trauma in children between 0 and 3 years of age. J Neurosurg Pediatr 2010;5(3):292-296.
66. Stiell IG, Clement CM, Mcknight RD, et al. The Canadian C-spine rule versus the NEXUS low-risk criteria in patients with trauma. N Engl J Med 2003;349(26):2510-2518.
67. Ehrlich PF, Wee C, Drongowski R, et al. Canadian C-spine Rule and the National Emergency X-Radiography Utilization Low-Risk Criteria for C-spine radiography in young trauma patients. J Pediatr Surg 2009;44(5):987-991.
68. Lee SL, Sena M, Greenholz SK et-al. A multidisciplinary approach to the development of a cervical spine clearance protocol: Process, rationale, and initial results. J Pediatr Surg 2003;38(3):358-362.
69. Pieretti-vanmarcke R, Velmahos GC, Nance ML, et al. Clinical clearance of the cervical spine in blunt trauma patients younger than 3 years: A multi-center study of the american association for the surgery of trauma. J Trauma 2009;67(3):543-549.
70. Leonard JC, Kuppermann N, Olsen C, et al. Factors associated with cervical spine injury in children after blunt trauma. Ann Emerg Med 2011;58(2):145-155.
Spinal trauma is a rare yet important category of injury. Children account for 10% of spinal injuries, but account for 25% of the mortality. Pediatric patients who present with possible spinal injury pose several unique challenges to the emergency department provider. Unique anatomic and developmental features place pediatric patients at risk for spinal injuries that are not typically seen in the adult population. In addition, unlike adult patients, there is little consensus on the most appropriate workup for potentially injured patients. When evaluating pediatric patients, practitioners must balance the limited available clinical data with the risks and benefits of various imaging modalities. The authors review the spectrum of pediatric spinal injury.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
