Five Key Injuries of the Wrist and Hand
October 6, 2013
Reprints
Related Articles
-
Walking at Work: A Helping Hand for a Healthier Heart
-
Examining the Effects of Cannabis on the Heart
-
Lifestyle Interventions and HbA1c in Prediabetic Patients
-
Rapid Reversal of Anticoagulation Reduces Mortality from Intracerebral Hemorrhage
-
Outcomes Are Better for Acute Stroke Patients Who Arrive Rapidly at Endovascular-Capable Centers
Five Key Injuries of the Wrist and Hand
This article is adapted from one that recently appeared in Pediatric Emergency Medicine Reports. I felt this might be of interest to a more general audience since it deals with some of the most common injuries seen in our departments, and those injuries may lead to litigation if not treated appropriately. The article describes important differences seen in children and adults, as they involve mechanism and the properties of growing bones. The bottom line for these injuries is: When in doubt, splint. The article also describes the latest approach to nail bed repair, which hopefully will decrease pain and improve healing in patients with subungual hematomas.
— Sandra M. Schneider, MD, Editor
Wrist and hand injuries are seen frequently in the emergency department (ED). Trauma to the wrist and hand (like most traumatic injuries) peaks during childhood, particularly in the teenage years, although there is a second peak in wrist fractures in the elderly. When considering all injuries to children, the distal upper extremity is by far the most often injured. A recent (2010), large, 10-year Swedish study1 found that among children aged 0 to 18 years, upper extremity fractures accounted for 68% of all fractures (n = 1500), with the remaining 32% being divided between lower extremity and axial fractures. Twenty-six percent of all fractures in this age group were of the distal radius, and hand/wrist fractures accounted for 17% overall.
Hand injuries peak in two age groups: toddlers and teenagers,2,3 a trend likely related to the increase in exploration and risk-taking in these two particular age groups, respectively. For example, toddlers use their hands to test hot water, reach for high branches, and put their fingers in the moving blades of fans. During adolescence, the hands serve both offensive (throwing, punching, tackling) and defensive (blocking, bracing, catching, falling) purposes.
The thumb is uniquely placed to oppose the other four digits with considerable strength and precision, and of the five key injuries, three of them fall directly along the thumb axis. Consider the difference between holding a pencil and holding a sledgehammer. The mechanics and concentrated innervation of the thumb make both of these actions possible. Thumb structure is truly amazing, allowing for a large range of motion, rivaled only by the human shoulder. As is true in the shoulder, the trade-off for this extraordinary mobility is a greater potential for injury and instability than the more fixed hinge joints, such as the knee.
The most frequent hand injuries lie on the margins of the hand.3 Overall, the three most commonly fractured bones of the hand are, in descending order, small finger metacarpal, small finger proximal phalanx, and thumb proximal phalanx. Scaphoid fractures, proximal thumb metacarpal fractures, and skier’s thumb injuries are less common, and occur mostly in the teenage and adult years. While injuries in this second group are statistically less common than other hand injuries, from a functional standpoint, these thumb axis injuries are perhaps the most important.
Definition of the Problem
These key hand and wrist injuries may go unrecognized in children and, as a result, may be improperly managed, causing greater pain and long-term limitation in function. On the other hand, early recognition of these five key injuries will minimize morbidity.
Epidemiology of Hand and Wrist Injuries
Age. In comparison to adults, children have a substantially greater incidence of all orthopedic injuries. Hand injuries alone account for approximately 2% of all pediatric ED visits each year. Multiple studies have reported that the incidence of hand and wrist fractures in the United States and Canada peaks at age 12 years, with more than 50% of all pediatric hand fractures occurring between ages 11 and 16 years. This spike is likely influenced by cultural factors, such as the popularity of more fracture-prone sports such as skateboarding, ice hockey, and aggressive/trick biking in this particular age group. A bimodal distribution of hand injuries in children has also been documented, with peaks in incidence around the 2-year-old age group and the 12- to 16-year-old age group.4 Both of these developmental stages are characterized by exploration and greater risk-taking, although the risks taken by teenagers tend to involve higher-energy mechanisms and, therefore, result in more fractures and more serious injuries. In the 0- to 4-year-old group, lacerations accounted for more than 50% of injuries, whereas in 12- to 16-year-olds, more than 50% of those who had radiographs had fractures.2
Time and Place. The most common time of hand and wrist injury is evening, with 57% of injuries occurring during this time period. By contrast, 39% occur during the daytime, and only 4% of injuries occur in the overnight (midnight to 8 a.m.) time period.2 In children in the developed world, this peak in hand and wrist fractures coincides with the hours immediately after school. Hand injuries occur most often during sports, with approximately 60% of all fractures in both males and females taking place on playing fields, courts, rinks, etc. Home is the next most common site, accounting for 25% of fractures, while school and road injuries are less common, together accounting for less than 15% of fractures.
Gender. The male-to-female ratio of hand and wrist injuries increases with age, ranging from a low of 2.7:1 among young children (younger than 8 years old) to a high of 5.5:1 among teenagers and adults. This increased proportion of fractures in male adolescents is thought to be due, in part, to more aggressive and high-risk behaviors. The gender gap in the incidence of fractures is closing, however, as during the past two decades the number of adolescent females participating in organized sports has increased.5 An epidemiologic study in an urban center2 found a significantly lower discrepancy (ratio 1.4:1) between male and female patients in terms of hand and finger injuries, but this study included contusions, lacerations, and other diagnoses in addition to fractures.
Etiology and Pathophysiology
In general, the mechanisms of injury to the hand and wrist include crush, axial loading, transverse force, traction, shear, or a combination of forces. Younger children have a particular tendency toward crush injuries, especially hands being caught in car and home doors. Athletes tend to sustain axial loading injuries related to falls.6 Transverse forces may be created by objects directly striking the hand, such as hockey or lacrosse sticks, balls, and bats. The hand is more adapted to withstand strong palmar forces rather than dorsal forces. Because of this design, a transverse force is more likely to result in fracture when the force is to the dorsum of the hand rather than to the palm. Traction and shear occur when fingers are caught in a jersey, crevasse, or rope. The mechanisms, diagnostic tests, and treatment guidelines for each particular injury will be discussed in the section that follows.
Key Injury #1: Scaphoid Fractures
Scaphoid fractures are by far the most frequent bony injuries of the wrist in both pediatric and adult patients.7 In pediatric patients, however, scaphoid injuries account for a smaller percentage of the total number of fractures, approximately 0.4% of all pediatric fractures.8 Scaphoid fractures in the first decade of life are unusual, particularly in patients younger than 7 years of age. The peak incidence is in adolescence, around 15 years of age.9 Dislocations and dissociations of the wrist are also very rare in children.
The usual mechanism of scaphoid injury is a fall onto a dorsiflexed or extended hand. (See Figure 1.) During the fall, the force of the body’s weight is transmitted from the ground to the metacarpals and carpals, then to the radius, the humerus, through the shoulder, and to the axial skeleton. The injuries that result from falls are distributed along this axis, and if sufficient force is present, the weakest portion of this axis will fracture or buckle. In the pediatric skeleton, the growth plates are the softest portion of bone and, thus, are predisposed to injury. Overall, distal radius physeal injuries are much more common than carpal injuries. If the hand is in extension during a fall impact, radial-side injuries are most common. Another mechanism of note is direct lateral impact of the wrist, which may cause distal pole scaphoid fractures.
Figure 1. Scaphoid Fracture Mechanism
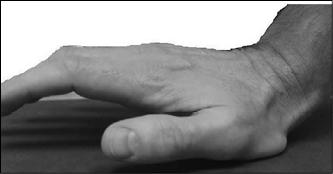
The scaphoid is unique among carpals in that it bridges the two rows of bones, extending from the epiphysis of the radius proximally to the trapezoid and trapezium distally, and lying radial to the lunate (proximal row) and capitate (distal row). With this unique position within the wrist, forces acting on the scaphoid are multiple, including axial load, traction, lateral force, and AP force. While the forces causing scaphoid fractures are similar for adults and children, anatomic developmental differences result in distinct fracture locations within the bone. The relatively decreased number of scaphoid fractures in pediatric wrists is largely due to late ossification. Ossification of a child’s scaphoid begins around age 5-7 years in the most distal portion and spreads proximately until completion of ossification around age 13-15 years.8 In adults, the majority (70%) of scaphoid fractures involve the waist, while only 15% of pediatric scaphoid fractures are located at the scaphoid waist. Pediatric scaphoid fractures typically occur in the distal half (59-87% in multiple studies),10-12 usually at the tubercle (52%) and the distal third (33%).
After bone maturation at 13-15 years, the scaphoid fracture pattern progressively approximates the adult, with more waist fractures. (See Figure 2.) The most critical fractures involve the proximal third, the region at risk due to retrograde perfusion of the scaphoid from distal to proximal. Like scaphoid fractures overall, these higher-risk proximal third fractures occur less frequently in pediatric patients, and are particularly rare in children younger than 7 years old. Nonunions are extremely uncommon if early and proper immobilization is used. There are reports of pediatric scaphoid malunions that have resulted from a missed or delayed diagnosis. Malunions result in significant morbidity and it is therefore imperative that the emergency physician is keen to recognize scaphoid fractures, orders images appropriately, and maintains suspicion for radiologically occult fractures.
Figure 2. Radiograph of Scaphoid Fracture
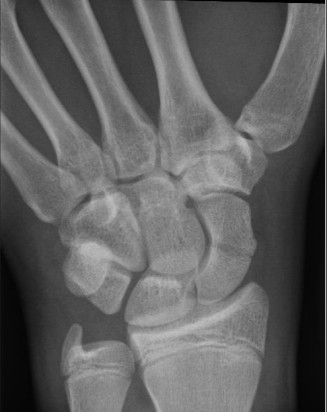
A careful physical exam is important with wrist injuries and should be used in conjunction with the appropriate radiographic studies to maximize the diagnostic ability of the provider. In particular, physical exam components that can alert the clinician to subtle injuries of the scaphoid are as follows:
• Tenderness of scaphoid tubercle: Have the patient extend the wrist, and press on tuberosity at proximal wrist crease (dorsal and radial aspect of wrist). Any tenderness when compared to the contralateral side represents a positive test (87% sensitivity, 57% specificity).13
• Snuff box tenderness: Have the patient actively abduct and extend the thumb (may also ulnar deviate) and press between the extensor pollicis longus and extensor pollicis brevis tendons. Pressure in the snuff box should be placed with the examiner’s fingertip to assess for tenderness. Comparison to the opposing hand may increase the accuracy of this test (90% sensitivity, 40% specificity, less in younger children).13
• Active ulnar deviation: Have the patient move the hand laterally while keeping the wrist flat. Pain with movement signifies a positive test (52% positive predictive value, 100% negative predictive value).13
• Axial loading of thumb: The examiner should grasp the thumb distally and place pressure on the thumb along its axis toward the wrist. Any pain reaction is a positive test. As with snuff box tenderness, observation of the patient’s reaction is generally more useful than questioning alone, which will result in a large number of false positives.13
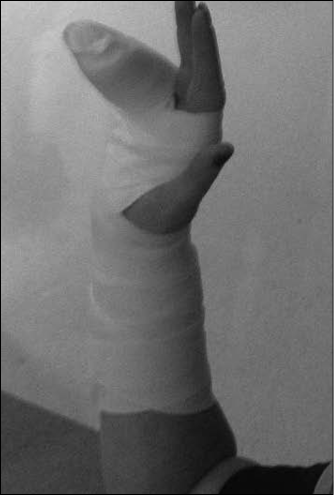
If one or more of the above four tests are positive, radiographs should be obtained with navicular views and the wrist should be treated empirically for a scaphoid fracture. Many authors advocate the use of a long-arm thumb spica cast for immobilization of scaphoid fractures to prevent pronation and supination of the hand. A cast or splint used for a scaphoid fracture must hold the hand radially deviated, or at least in a neutral position. A short-arm thumb spica splint may be used for suspected scaphoid fractures. (See Figure 3.) Any ulnar deviation will cause separation of fracture fragments as strain is placed across the scaphoid, and prevent proper healing.
Figure 3. Thumb Spica Splint
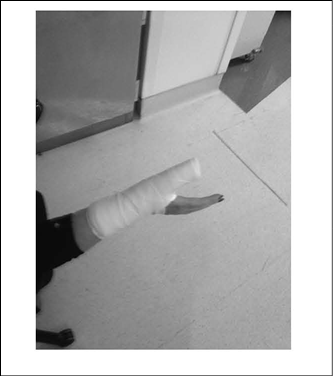
The use of specific radiographic views can aid in the diagnosis of occult scaphoid fractures. The use of ulnar deviation alone and/or the use of a "scaphoid" or "navicular" view (ulnar deviation with 20-40 degree cranial angulation of the X-ray beam) will maximize fracture diagnosis. Additionally, it is important to obtain, at minimum, three views of the wrist, including scaphoid, semipronated, and AP radiographs.14
While scaphoid fractures may occur in isolation, the great forces necessary to fracture the scaphoid often result in a second or third fracture, as occurs 5-12% of the time.15 The most frequent concurrent injuries are distal radius fractures. When the possibility of scaphoid fracture exists, a four-tiered system of treatment has been recommended by Buttaravoli:13
- Negative physical exam, negative radiograph, low suspicion mechanism: No splinting is required, follow up as needed if pain is not improved in 5 days.
- One or more physical exam tests are positive, negative radiograph: Immobilize in a short-arm thumb spica splint and recommend follow up with an orthopedic or hand specialist in 5-7 days, and/or obtain repeat X-rays in 14 days. Alternatively, more sensitive imaging such as CT or MRI may be warranted in the acute setting.
- A positive fracture on the radiographs with no displacement (defined as less than 1 mm separation and no cortex step off): Immobilize in a long-arm thumb spica splint and recommend follow up with an orthopedic or hand specialist in 5-7 days.
- A positive fracture on the radiographs with displacement greater than 1 mm, angulation, comminution, any proximal pole fracture, or instability: Emergent orthopedic/hand consultation and long-arm thumb spica.
Key Injury #2: Thumb Metacarpal Fractures (Including Bennett and Rolando Fractures)
The thumb metacarpal is uniquely designed and positioned to allow for both power grip and the finer movements of the so-called pincer grasp. The ability to perform both of these functions smoothly is contingent upon smooth articulation between the thumb metacarpal and trapezium. Disruption in this important surface of the carpal metacarpal (CMC) joint often results in severe limitation of pincer grasp and power grip, which, in turn, greatly impairs the whole hand function. Two important fractures in the thumb metacarpal include the Bennett and Rolando fractures.
Bennett fractures are defined as fractures of the first metacarpal of the hand, with the fracture line extending from the base of the metacarpal (MC) to the CMC joint.16 (See Figure 4.) Bennett fractures are the most common thumb MC fractures. Involvement of the CMC makes this fracture unstable. The break occurs obliquely through the intra-articular surface of the base of the metacarpal. The most common mechanism of injury is axial loading of a flexed metacarpal. A Bennett fracture should be suspected clinically whenever there is a mechanism of punching a solid object or falling onto the thumb. Pain and focal tenderness at the base of the thumb are typical. A quick way to recognize a Bennett fracture radiologically is that a small fracture fragment stays with the carpals. When a Bennett fracture occurs, the proximal fragment is maintained in anatomic position due to strong attachment of the anterior oblique ligament to the tubercle of the trapezium. The distal fragment, however, which is attached to other tendons and ligaments of the hand, is pulled away from the joint by the forces exerted by adductor pollicis (which pulls the metacarpal head toward the palm) and the abductor pollicis longus (which subluxates the base in a dorsal, radial, and proximal direction).16
Figure 4. Bennett Fracture Radiograph
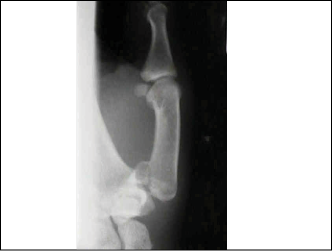
A Rolando fracture is defined as a comminuted fracture of the base of the thumb metacarpal. (See Figure 5.) The mechanism of a Rolando fracture is most often simultaneous hyperextension and hyperabduction. This fracture type is typically unstable and occurs less commonly than a Bennett fracture in the pediatric population. In contrast to a Bennett fracture, which has two fragments, a Rolando fracture has at least three fragments, often forming a "Y" visible in one plane. Treatment of the Rolando type fracture requires either closed reduction with percutaneous pinning or open reduction and internal fixation. The functional outcome despite optimal treatment is worse for Rolando fractures when compared to Bennett fractures. Listed below are physical exam signs that are associated with thumb metacarpal fractures. These signs may be seen with either Bennett or Rolando fractures:
- Point tenderness over the CMC joint;
- Ecchymosis of the thumb and thenar eminence;
- Weakness of pincer grasp: Have the patient grasp two sheets of paper, one in the left hand pincer, one in the right hand pincer, and pull them away. Inability of the patient to hold onto the paper indicates weakness.
- Lack of joint strength: Have the patient tear a sheet of paper.
Figure 5. Radiograph of Rolando Fracture
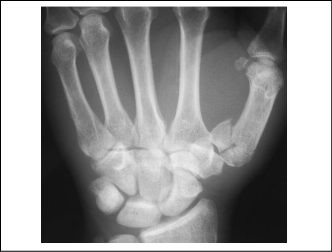
Treatment of thumb proximal metacarpal fractures depends primarily on the degree of displacement. Failure to recognize and properly repair this key injury is likely to result in malalignment of the fragments and poor healing.6 The fractures will likely require closed reduction and immobilization if displaced less than 1 mm, closed reduction with percutaneous pinning if displaced 1-3 mm, or open reduction and internal fixation if displaced more than 3 mm.
Key Injury #3: Skier’s Thumb
Skier’s thumb is an acute injury to the ulnar collateral ligament (UCL) caused by forced abduction and hyperextension of the thumb. It is a frequent injury in any sport that involves grasping a pole, such as skiing, hockey, lacrosse, or pole vaulting, or from a motor vehicle accident. The most common mechanism, however, is simply a fall onto the outstretched hand with an extended thumb. The injury can include either partial or total disruption of the UCL.17 A related condition called gamekeeper’s thumb is caused by repeated lesser tension forces on the UCL, such as those once exerted by Scottish hunters who would press the necks of small game animals against the ground using both thumbs in order to quickly break their necks. Below are physical exam tests for a skier’s thumb (UCL injury):
• Hold the thumb metacarpal stable, either in extension or at 30 degrees of flexion; stress the thumb in a radial direction. If there is more than 40 degrees of angulation or no clear endpoint, there is a complete tear of the UCL. If there is laxity of the joint as compared to the thumb MCP on the opposite hand, there is likely a partial tear (incomplete injury).
• Pincer grasp testing with a sheet of paper, as described previously, is also useful.
The Bennett fracture, Rolando fracture, and skier’s thumb all present with pincer grasp weakness. However, the injuries may be differentiated by the location of tenderness. Skier’s thumb (UCL tear) is characterized by point tenderness and instability at the thumb MCP joint, while a Bennett or Rolando fracture involves only the CMC joint. As with the evaluation of other thumb injuries, radiographs should be obtained of the patient suspected to have a skier’s thumb. It is important to remember that a skier’s thumb may or may not be visible on X-ray, and the most common radiographic finding is an avulsion fracture of the proximal thumb phalanx at the site of UCL attachment. (See Figure 6.) A Stener lesion is a particular type of UCL injury with palmar subluxation of the base of the proximal phalanx.17 A skier’s thumb should be repaired by an orthopedic and/or hand specialist within one week if the UCL tear is complete. Incomplete tears may need physical therapy and rehabilitation. In either case, ED treatment includes immobilization with a thumb spica splint or cast and subspecialty referral within 2-3 days.
Figure 6. Radiograph of Skier’s Thumb
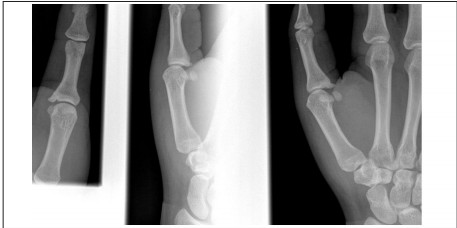
Key Injury #4: Phalanx Injury
Phalanx injuries are most commonly found distally, and in order of descending frequency are 5, 1, 4, 3, 2.5 Each digit has a different injury pattern, which is dependent upon location, mechanism of injury, and the amount of force applied. The thumb is unique in that it has only proximal and distal segments, with no middle phalanx. It also has the distinction of being the site of a pair of sesamoid bones, which are sometimes mistaken for fracture fragments. The thumb phalanx is very important functionally, since it helps provide the strength of grip and versatility of opposing each of the other four digits. The mechanisms of injury of thumb phalanges are similar to those of thumb metacarpals. Additionally, the thumb phalanges are susceptible to crush injuries, for example, in which the thumb encircles a baseball bat, hammer, or bicycle handlebar. A physical examination of the thumb phalanx should be performed carefully, assessing tenderness and changes in range of motion, and comparing it with the opposite thumb. The IP joint and MCP joint should be tested individually for movement and strength.
Index, long, ring, and small finger phalanx fractures can be divided into two groups based on location: proximal and middle phalanx injuries versus distal phalanx fractures. In the assessment of phalanx fractures, it is important to assess for rotation, which commonly occurs as the result of spiral or oblique fractures. Rotational deformities of the proximal and middle phalanges, when compared to the distal phalanges, are more likely to result in a greater degree of potential disability.18 As little as 10 degrees of rotational deformity of the middle or long finger may be disabling as a result of the alteration of fixed flexion planes.
A physical examination of each phalanx should be performed and compared with the other digits. The DIP and PIP joints should be tested individually for movement and strength. A comparison of nail positions with a closed hand is an invaluable tool for assessing rotation in phalanx fractures. Also, with complete flexion of the fingers, the planes of the middle and distal phalanges should come together at a point just proximal to and overlying the flexor tendons of the wrist. Additionally, performance of a complete motor exam with flexion of all joints may accentuate visibility of deformities and aid in diagnosis. In open fractures or lacerations, the closed fist position should be assessed during the examination, as this may reveal tendon injuries that are not visible with the hand in a position of extension. The proximal and middle phalanges, more so than their distal counterparts, tend to be unstable after reduction, especially with transverse fractures.18 Proximal phalanx fractures are often unstable due to the volar forces of interosseous muscles opposing the dorsal forces of the central slip. If a proximal or middle phalanx fracture is complete and unstable, it will often require open reduction with internal fixation (ORIF).
Tuft fractures are the most common distal phalanx injury. By definition, a tuft fracture is a comminuted fracture of the head and tuberosity of the distal phalanx, usually without any displacement or angulation. (See Figure 7.) Due to proximity of the fingernail dorsally, and septa volarly, these fractures are generally stable. They are commonly associated with lacerations, crush forces, and subungual hematomas. If a tuft fracture is open, thorough irrigation with debridement of devitalized tissue is necessary. The use of prophylactic antibiotics for open tuft fractures is still a subject of controversy.19 However, if any doubt exists about the severity of injury or infection risk, it is prudent to provide antibiotic prophylaxis.
Figure 7. Radiograph of Tuft Fracture
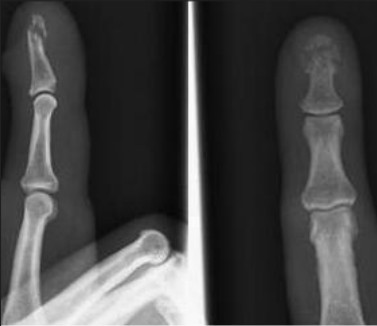
Subungual hematomas result from laceration of the nail bed, followed by blood accumulation under the nail. (See Figures 8 and 9.) The primary methods of managing acute nail bed lacerations have traditionally been trephination (making a hole for the blood to escape) or removal of the nail for suturing of the laceration. The decision to use trephination versus nail removal to repair the underlying laceration depends on the judgment of the treating physician; however, there are a few guidelines that may be of use. In the past, it was common practice to trephinate the nail if the hematoma covered 50% or less of the nail’s surface area, and to remove the nail and repair the nail bed if the hematoma covered greater than 50%.8 More recent studies comparing trephination to operative nail bed repair have shown no difference in outcome, even in hematomas that covered more than 50% of the nail.20 Additionally, a prospective study of trephination of large subungual hematomas demonstrated that trephination of simple hematomas was effective for pain relief without negative outcomes (i.e., infection, nail deformity) when the nail margin was intact. The majority of patients had normal nails at four months post-intervention.21 The authors conclude that the majority of subungual hematomas may be managed with trephination alone without nail removal.
Figure 8. Subungual Hematoma
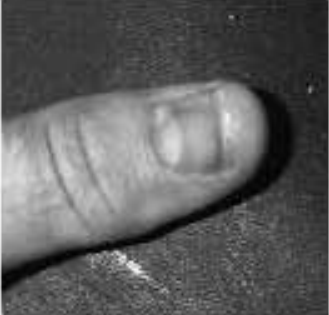
Figure 9. Radiograph of Subungual Hematoma
Trephination may be accomplished by using electrocautery, essentially creating a hole in the nail in communication with the hematoma. Additional effective methods include the use of a sterile 18-gauge needle spun gently to function as a drill bit. Regardless of the method utilized, the provider should be careful not to injure the nail bed. Further, holes created through trephination should be 2-4 mm in diameter to prevent clotting and obstruction of flow.8 The goal of treatment in all of these techniques is to decompress and protect the germinal matrix/nail fold complex, which will, in turn, re-create the nail. When the injury causes complete avulsion of the nail, the nail bed laceration should be repaired with 6-0 absorbable sutures and re-covered with either the avulsed nail (preferably), foil, or a non-adherent dressing inserted into the proximal fold. Damage to the matrix typically results in irregular regrowth of the nail, but this is almost uniformly transient.
Mallet finger, or dorsal avulsion fracture, occurs when an extended DIP is forced into flexion. A typical mechanism includes a direct blow to an extended fingertip, resulting in rapid flexion with resultant increased tension on the extensor mechanism, and a dorsal distal phalanx avulsion at the attachment of the extensor tendon attachment. Clinically, this presents with dorsal tenderness with the finger held in flexion with the inability to actively extend at the DIP joint.6 Upon radiographic evaluation, volar deviation and/or a small bone fragment attached to the extensor tendon may be visible. It is important to note that a mallet finger may represent ligamentous injury alone and does not require a fracture. Patients should be treated empirically in the setting of injury with associated inability to extend the finger at the DIP joint. Prognosis is better if there is a fracture with mallet finger. Mallet injuries are generally treated acutely with splinting in extension, but they often require operative intervention if the injury is complete, with deformity or inability to extend the DIP.
Simple transverse fractures of the distal phalanx are usually stable. Most simple transverse fractures require splinting only. However, if angulation is present, reduction and surgical intervention may be required. Surgical intervention may include the placement of alignment wires (K-wires) if closed reduction fails or greater than 30% of the articular surface of the bone is involved.6 Patients with simple transverse fractures should be splinted and should follow up with orthopedic surgery or a hand specialist. In general, fractures that are more complex should have more urgent follow-up.
Jersey finger occurs due to injury of the flexor digitorum profundus (FDP). Unlike mallet finger, which results in the inability to extend the DIP, the patient with jersey finger will be unable to actively flex the DIP. This injury most often involves the ring finger, and occurs from grabbing or getting fingers tangled in an athletic jersey.22 FDP rupture can be tested by holding the PIP stable and asking the patient to flex the finger or make a grasping motion. This injury may include a partial or complete injury to the FDP. Partial injuries are generally managed conservatively with splinting and therapy, while complete injuries require surgical intervention.17
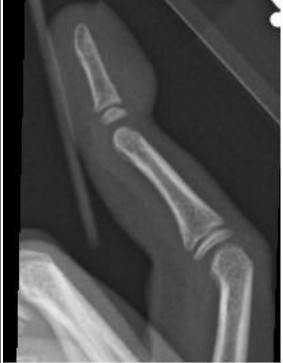
Finger dislocations are relatively common pediatric injuries. The most common type is dorsal dislocation at the proximal interphalangeal joint (PIP), with volar PIP dislocations being less common but equally important.23 (See Figure 10.) It is vital to distinguish between dorsal and volar PIP dislocations, since their treatments are different. The more prevalent dorsal dislocations occur with hyperextension and involve the middle phalanx moving dorsally in relation to the proximal phalanx.22 This motion causes a disruption in the volar plate (which stabilizes the joint from the palmar surface). Volar plate rupture may or may not involve an avulsion fracture, which would be seen best on lateral X-ray. Reduction of the dorsal dislocation includes the following: After the provision of analgesia via digital block, longitudinal traction is placed on the middle phalanx, followed by volar pressure on the middle phalanx and dorsal counter pressure on the proximal phalanx. After reduction, a finger splint should be placed. The finger should be splinted with the affected joint in a 30-degree flexed position. Splinting in the flexed position fosters improved healing of the volar plate.22 A volar dislocation, by contrast, involves injury to the central extensor slip. Pain on resisted extension is a cardinal sign of this injury.23 Since volar dislocations involve the disruption of dorsal structures, they should be splinted in full extension to bring the disrupted segments together. In some cases, a dislocation may reduce spontaneously, or the athlete may reduce it before arrival. If this occurs, the following physical signs will assist the ED physician in differentiating dorsal and volar dislocations. Dorsal dislocations typically present with focal volar tenderness, while volar dislocations will have dorsal tenderness.23 In either case, joint stability should be assessed, particularly in extension, and the patient should follow up with an orthopedic and/or hand specialist for further treatment.
Figure 10. Radiograph of Thumb Dislocation
In addition to the site-specific management strategies above, there are general principles for the management of phalanx fractures. Splinting generally represents adequate immobilization for phalanx fractures that do not involve greater than 30% of the physis and do not have persistent deformity after reduction. A variety of commercial finger splints can be used, with the most popular being constructed of formable aluminum and foam. (See Figure 11.) Tongue depressors and rolled gauze may also be used as an improvised splint and may be just as effective. It should be noted that thumb phalanx fractures and all proximal fractures require a splint that extends beyond the phalanx. This is important, as flexion/extension at the MCP joint will transfer deforming forces on the fracture fragments of the phalanx.18
Figure 11. Aluminum Foam Finger Splint

While phalanx shaft fractures are often managed conservatively with closed reduction and external immobilization, intra-articular fractures warrant mandatory orthopedic or hand specialist referral for operative intervention. Since complications of intra-articular fractures are common, the clinician must maintain a high degree of suspicion and ensure that adequate radiographic views are obtained to detect them. In the case of simple fractures reduced in the emergency department, re-imaging should generally be performed after reduction and immobilization to confirm the position of fracture fragments, and to ensure that angulation or displacement has not recurred during splinting.
Key Injury #5: Boxer’s Fracture
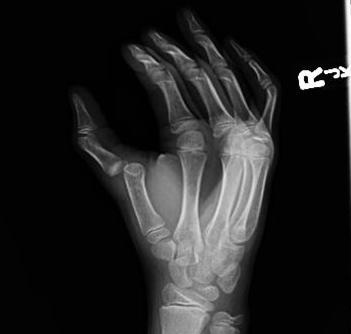
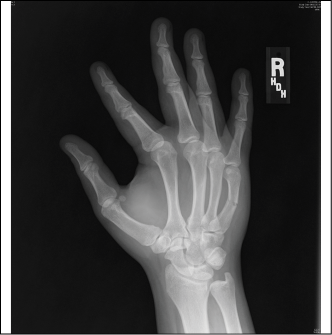
A boxer’s fracture is a metacarpal fracture that typically involves the 4th or 5th MC. (See Figure 12.) The mechanism of a boxer’s fracture is axial loading of the metacarpals as a result of punching a fixed object. Boxer’s fractures are uncommon in young children since they cannot generate the necessary fracturing force. Peak incidence is in males in their teens and 20s.5 Utilization of protective gloves in high-impact sports has decreased the incidence of this injury type. Patients with this injury type may present with diffuse dorsolateral hand pain and swelling, ecchymosis, and deformity.
Figure 12. Radiograph of Boxer’s Fracture
Closed fist injuries require a close assessment for rotational deformity or malalignment of the four middle and distal phalanges when the hand is held in flexion. A regular pattern of finger orientation and appearance of nail folds should be observed in comparison to the contralateral hand. Acceptable angulation for a metacarpal boxer’s fracture depends upon location. In contrast to the index and long finger metacarpals, in which very little (generally less than 10 degrees) of angulation is tolerated, 30 or 40 degrees of angulation of the ring and small finger metacarpals, respectively, may be acceptable.
In the assessment of a boxer’s fracture, it is important to evaluate for a fight bite, which is an injury that may or may not include a fracture resulting from a closed fist punching the opponent’s face and mouth.13 In general, any breach in the skin overlying the head of the metacarpals, in association with a punching injury, should be empirically treated as a fight bite and assumed to be contaminated by oral flora. If the injury is consistent with a fight bite, antibiotics should be given prophylactically, since these wounds are at a high risk of developing infections such as tenosynovitis or osteomyelitis. Recommended prophylaxis generally includes amoxicillin/clavulanic acid, as it provides broad coverage for flora from the human mouth (Eikenella, Streptococcus, and Staphylococcus species). Additionally, fight bites should be copiously irrigated and be allowed to heal via secondary intention without surgical closure. Patients with this injury type should be re-evaluated in 24-48 hours for infection. Any signs of infection at the follow-up visit or unplanned return to the ED following a closed fist injury should prompt strong consideration for IV antibiotics, hospital admission, and a hand or orthopedic consultation.
Overall Treatment of Hand and Wrist Injuries
Splinting of hand and wrist injuries is the standard of care for not only visible fractures but also suspected fractures and ligament and tendon injuries. Conversely, casting may be utilized in some ED settings; however, it is contraindicated in acute injuries with a significant risk of swelling.
In hand and wrist injuries, splinting is most often accomplished with the hand in the "position of safety," with 15-30 degrees of wrist extension, 90 degrees of flexion at the MCP joints, and fingers in full extension.13 This position concomitantly provides stability while preserving function. Immobilization for each injury type is discussed in the preceding sections, and the most commonly used immobilization techniques for hand and wrist injuries are listed in Table 1.
| Table 1.Splint Types | ||
|---|---|---|
| Injury | Splint | Emergent Orthopedic Consult Needed? |
|
Scaphoid fracture |
Long-arm thumb spica (visible fracture) Short-arm thumb spica (suspected) |
Displaced scaphoid fracture Comminuted fracture |
|
Thumb MC and phalanx fracture |
Short-arm thumb spica |
Comminuted fracture Visible deformity Amputation |
|
Index MC |
Short-arm radial gutter splint (see Figure 14) |
Angulation > 10 degrees |
|
Long, ring, small finger MC |
Short-arm ulnar gutter splint (see Figure 13) |
Angulation of > 10, > 30, > 40 degrees, respectively |
|
Finger phalanx fracture |
Aluminum foam and/or buddy taping (see Figures 11 and 15) |
Finger cascade abnormal (rotational deformity) Visible deformity (reduction needed) Open (except tuft) Amputation |
Figure 13. Ulnar Gutter Splint
The time of immobilization varies with age and specific injury, with 4-8 weeks the most commonly recommended duration in young children, and 8-12 weeks in older patients. This determination will generally be made by the orthopedic or hand surgeon who can re-evaluate the patient in follow up and, therefore, better guide the duration of immobilization.
Figure 14. Radial Gutter Splint
Figure 15. Finger Buddy Taped

References
- Hedstrom EM, Svensson O, Bergstrom U, et al. Epidemiology of fractures in children and adolescents. Acta Orthop 2010 Feb 22 [Epub ahead of print].
- Fetter-Zareka A, Joseph MM. Hand and fingertip injuries in children. Pediatr Emerg Care 2002;18:341-345.
- Rajesh A, Basu AK, Vaidhyanath R, et al. Hand fractures: A study of their site and type in childhood. Clinical Radiology 2001;56:667-669.
- Vadivelu R, Dias JJ, Burke FD, et al. Hand injuries in children: A prospective study. J Pediatr Orthop 2006;26.
- Mahabir RC, Kazemi AR, Cannon WG, et al. Pediatric hand fractures: A review. Pediatr Emerg Care 2001;17:153-156.
- Peterson JJ, Bancroft LW. Injuries of the fingers and thumb in the athlete. Clin Sports Med 2006;25:527-542, vii-viii.
- Hart ES, Grottkau BE, Gleeson NB, et al. Broken bones: Common pediatric upper extremity fractures, part II. Orthopaedic Nursing 2006;25:311-323.
- Huckstadt T, Klitscher D, Weltzien A, et al. Pediatric fractures of the carpal scaphoid: A retrospective clinical and radiological study. J Pediatr Orthop 2007;27:447-450.
- Kozin SH, Waters PM. Chapter 8: Fractures and dislocations of the hand and carpus in children. In: Rockwood and Wilkins, Fractures in Children, 6th ed.
- Wulff RN, Schmidt, TL. Carpal fractures in children. J Pediatr Orthop 1998;18:462-465.
- Vahvanen V, Westerlund U. Fracture of the carpal scaphoid in children. Acta Orthop Scand 1980;51:909-913.
- Cristodoulou AG, Colton CL. Scaphoid fractures in children. J Pediatr Orthop 1986;6:37-39.
- Buttaravoli P. Chapter 130: Scaphoid fractures. In: Buttaravoli P. Minor Emergencies: Splinters to Fractures, 2nd ed.
- Steinburg D. Metacarpal fracture and dislocation. Emedicine.com. 2009.
- Boles C. Wrist, scaphoid fractures and complications. Emedicine.com. 2009.
- Rettig ME, Dassa GL, Raskin KB, et al. Wrist fractures in the athlete: Distal radius and carpal fractures. Clin Sports Med 1998;17:469-489.
- Leddy JP. Soft-tissue injuries of the hand in the athlete. AAOS Instructional Course Lectures, Volume 47.
- Alke J, Schraga E. Fracture, hand. Emedicine.com. 2009-2011.
- Altergott C, Garcia FJ, Nager AL. Pediatric fingertip injuries: Do prophylactic antibiotics alter infection rates? Pediatr Emerg Care 2008;24:148-152:
- Roser SE, Gellman H. Comparison of nail bed repair versus nail trephination for subungual hematomas in children. J Hand Surg [Am] 1999;24:1166-1170.
- Seaberg DC, Angelos WJ, Paris PM. Treatment of subungual hematomas with nail trephination: A prospective study. Am J Emerg Med 1991;9:209-210.
- Combs J. It’s not "just a finger." J Atheletic Training 2000;35:168-178.
- Cohen AR, Metzl JD. Sports-specific concerns in the young athlete: Basketball. Pediatr Emerg Care 2000;16:462-468.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
