2012 Salary Survey Results: Still standing: Infection prevention emerges — with a few battle scars — as recession fades
2012 Salary Survey Results
Still standing: Infection prevention emerges — with a few battle scars — as recession fades
More than two-thirds of IPs report a wage hike
Infection preventionists have generally weathered the Great Recession in good shape, though the field remains in flux as “old school” IPs leave and a new wave of IPs from more diverse backgrounds enter the field.
One very good sign is that 67% of IPs responding to the Hospital Infection Control & Prevention 2012 salary survey reported they received a raise in the last year. Breaking those numbers down, 51% reported an increase of 1% to 3%; while 11% were compensated an additional 4% to 6% and 4% received a hefty hike in the 7%-10% range. Still, 33% of IPs reported no increase in compensation.
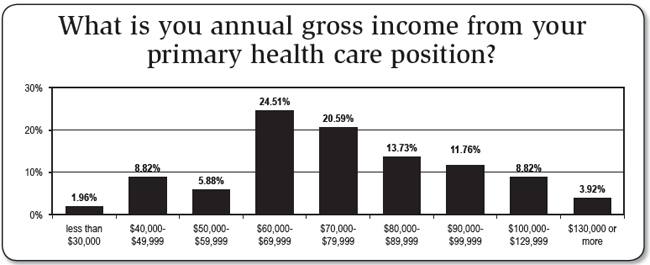
The HIC survey found that IPs were drawing a median salary in the $70,000 to $79,999 range, the same as reported in the 2011 report. In salary percentage breakdowns, 11% were making $49,999 or less; 6% were paid $50,000 to $59,999; and 25% had salaries in the $60,000 to $69,999 range. Another 21% were drawing wages in the $70,000 to $79,999 range. The median hospital size of respondents was 200 beds or less, with 37% reporting they worked in a hospital with less than 100 beds.
By comparison, the U.S. Bureau of Labor Statistics reports the median annual wage for a registered nurse was $65,950 in 2011.1 The best-paid 10% RNs made more than $96,630, while the bottom 10% earned less than $44,970. IPs traditionally have nursing backgrounds, but that is gradually changing as more job seekers with different areas of expertise enter the field.
“One of the most exciting things that has happened in the last decade is the entrance of the MPH — master’s in public health — into the profession,” says Patti Grant, RN, BSN, MS, CIC, the 2013 president of the Association for Professionals in Infection Control and Epidemiology (APIC). “And I don’t mean an RN or a med tech who decides to go back to school to get an MPH. I mean people who are getting an MPH and almost right out of school they jump from public health into infection prevention.”
A similar trend has been observed by Ruth Carrico, PhD, RN, CIC, an associate professor at the School of Public Health and Information Sciences at the University of Louisville, KY.
“I don’t really feel any longer that the nurse is the only one — or even necessarily the best person — to put in the role,” says Carrico, an IP for two decades before transitioning to academia. “I have had a lot of experience working with the MPH graduates. They lack the patient care experience, but they have other strengths — epidemiology and statistics, management, program evaluation and an understanding of the role the environment plays in disease and disease transmission.”
As people with non-nursing backgrounds enter the profession, one critical constant is the need for team-builders who can assess the needs of a given facility, she adds.
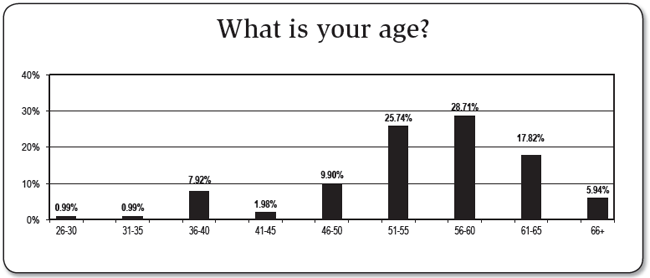
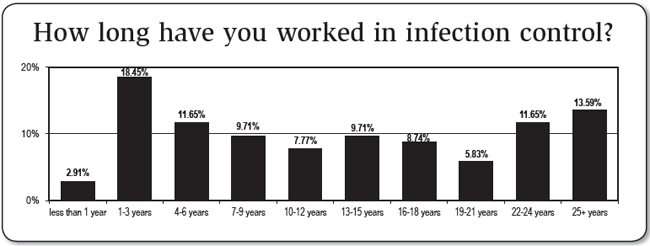
HIC survey respondents certainly had a wealth of experience, with 78% reported working in health care for at least 25 years. Many of these came to infection prevention as a second career, however, as 43% of respondents reported working in infection control less than a decade. Still, one-fourth of respondents had been in infection control at least 22 years. A similar demographic shift continues throughout many nursing-based professions, the graying of a well-seasoned work force. We asked Grant how APIC will put enough IPs in the field to ensure patient safety is not compromised in the coming years.
“I really believe APIC’s educational and training programs are second to none,” Grant says. “No matter what discipline people come to us from, they are going to get excellent training.”
Defining the IP role
Currently, the public perception — and even to some extent the health care perception — of infection prevention remains somewhat undefined, which may nevertheless be an improvement over prior years when few patients even knew hospital infection control programs existed.
“From my perspective, one of the challenges is we still don’t really know what the role is,” Carrico says. “If you look at a nurse, a physician, a respiratory therapist — you know what those roles mean. Infection prevention still has a very nebulous quality to it. We haven’t really done a good job in quantifying the value of an experienced IP. We need to make sure that our organizations understand the value that we bring.”
To address this situation and do some forward-thinking on a changing profession, APIC published a competency model last year that put patient safety as the primary goal and identified four critical areas of expertise: leadership and program management; performance improvement and implementation science; infection prevention and control; and technical expertise.2
APIC views the model as part of the association’s long-standing efforts to define and advance the profession. “The competency model really is a very well-researched road map to ensure that as IPs enter the profession they know how to progress and become the best that they can be in the patient safety effort,” Grant says.
If there is a current gap in the identified core competencies, it is probably the “leadership” component, Carrico adds.
“We are learning more and more about the actual skill sets, the level of knowledge that is required for the job,” she says. “We are at the point now of trying to take this and not only lead implementation of this information, but really lead a change within the health care system.”
The content areas correspond to the core competencies as defined by the Certification Board of Infection Control and Epidemiology (CBIC). “Board certification in infection prevention [CIC] is critical to professional development,” the APIC paper notes. “It represents the bridge between the novice and the proficient professional.”
In the HIC survey, 45% of respondents cited CIC as the certification that best described their position. Moreover, the value of having a certified IP continues to be documented in the literature. In a recent study, IPs with certification in infection control were twice as likely to identify good infection control practices as their colleagues without certification.3
“Certification is based upon the job analysis that is performed every several years,” Carrico says. “So the development of that certification — which is our way of demonstrating competence — is linked to what we say our job tasks are. As those change, the certification process itself ultimately changes. As our role in infection prevention continues to evolve, so will the certification process. We continuously have to look at the profession, at what is required and what is necessary. “
References
- U.S. News and World Report. Best Healthcare Jobs: Registered Nurse. http://money.usnews.com/careers/best-jobs/registered-nurse
- Murphy DM, Hanchett M, Farber MR, et al. Competency in infection prevention: A conceptual approach to guide current and future practice. Am J Infect Control 2012;40: 296-303.
- Saint S, Greene TM, Olmsted RN, et al, Perceived strength of evidence supporting best practices to prevent health care-associated infection: results from a national survey of infection prevention personnel. Am J Infect Control 2013;(41);100-106.
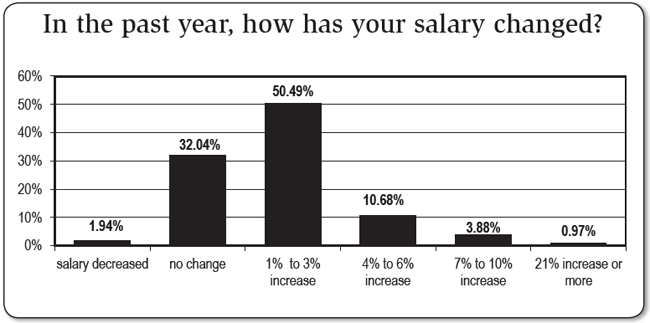

Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
