Winter Sports Injuries
November 3, 2013
Reprints
Winter Sports Injuries
Whether we like it or not, winter is just around the corner. With it comes an entire set of emergency presentations. In addition to influenza, which we have covered several times in the past, cold exposure and icy roads and sidewalks bring an increased number of patients into our EDs, especially in the Northeast.
This paper reviews the most common injuries related to winter sports. Over the past decades, there has been an increase in the variety of winter sports, as well as increased participation by individuals at all levels of fitness. There have also been some improvements made that reduce injuries. For example, breakaway ski boots have reduced the number of tibia and ankle fractures. With some sports becoming more dangerous with jumps and aerial moves, helmets are beginning to be more common, but sadly not fast enough.
This review should help you get through this winter season and perhaps offer some advice for your patients, your family, and yourself.
— Sandra M. Schneider, MD, Editor
Executive Summary
- While downhill skiing and snowboarding look similar, the injuries associated with each are different. Ski injuries are most often of the knee or the ulnar collateral ligament. Snowboarding is associated with upper extremity injuries. Head injuries occur in both sports.
- Alcohol plays an important role in increasing the number of injuries seen in winter sports. It is most often seen in males involved in aggressive sports such as snowmobiling.
- Skier's thumb is an acute rupture of the ulnar collateral ligament. Patients present with pain at the insertion of the ligament, as well as pain upon pinching the thumb and index finger together. Many patients, but not all, will demonstrate lateral laxity when stressed. Patients should be splinted and receive orthopedic evaluation as an outpatient.
- Open fractures should receive prompt assessment and care. Where there is distal ischemia, reduction may be attempted prior to imaging. Otherwise, the wound should be covered, antibiotics started, and X-rays obtained. Patients should have an orthopedic evaluation in the ED.
Introduction
With the growing participation in winter sports, emergency physicians (EPs) can anticipate a rise in the number of patients seen who are injured while participating in these sports. In addition, older individuals are more likely to continue participation in the sports they love, often attempting the same level of performance that they had decades before. Knowledge of basic fundamentals of these sports, as well as their unique injury patterns, can help the EP anticipate injuries. This ultimately can lead to timely diagnosis and treatment and help avoid missing injuries that might otherwise be overlooked. As with any physician-patient encounter, opportunities may exist for intervention that may help prevent future injuries.
Northern climates have sports that are unique to their environment due to snowfall and ice formation. Some of these sports, such as ice hockey, began as games played on frozen lakes, but now are enjoyed year round and in indoor ice rinks in southern climates such as Florida, Texas, and Arizona. Even indoor skiing and tubing sites are being created and used year round. Thus, the geography of some winter sports is evolving. Given the different environments in which these sports are played, injury patterns are often unique to the specific sport. With the high number of winter sports participants and the ease at which travel around the world occurs, physicians anywhere should be aware of the inherent dangers and injury profiles of these sports.
Many winter sports involve competition at all levels, from the local pick-up hockey games to the Olympic Games. Some of these sports have been around for hundreds of years, such as sledding and skiing, whereas others are relatively new, such as snowboarding. All have seen a growth interest and, thus, development of newer and often safer equipment. It is important to note that some of these sports are still evolving; therefore, injury patterns referenced now are likely changing with time. Examples of this include the increased participation in acrobat skiing that involves aerial maneuvers, back-country snowboarding, and faster snowmobiles. This review is focused more on the recreational sporting activities of the public at large as opposed to the elite athlete, and is meant to be a general review. Many excellent reviews of the specific injuries exist that can be referenced for more detailed information.
Downhill Skiing
Downhill skiing is one of the most popular winter sports worldwide, with more than 200 million participants and growing.1,2 Snow skiing has been around for many years and has its roots back as far as about 5000 BC in Russia, where the oldest wooden skis were found, and Scandinavia in 2000 BC, where it was primarily a method of transportation.3,4 It is a sport that is challenging and physically demanding. Downhill skiing generally involves being transported to elevation on a chairlift, then descending down a slope that is either groomed or packed snow or natural powder. The skier wears rigid plastic boots that are attached to the skis by bindings that release when undesirable forces are placed on them, such as occurs when one loses control and crashes. Lightweight ski poles are often held in each hand to help with movement on flatter terrain and sometimes with turning. Helmets traditionally haven’t been worn, but their use is becoming more routine. Given the high speeds involved and skill needed, serious injuries occur at a surprisingly low rate. According to the National Ski Areas Association (NSAA) data, serious injuries occur one per one million skier/snowboarder visits. The 2011-2012 season saw 54 fatalities and 510 serious injuries in the United States. Injuries in general have dropped over the years to about two to three per 1000 skier-days.2 The reason is unclear, but it is generally thought that better equipment such as bindings may play a part. Injuries from skiing occur most commonly from ground level falls, but also commonly occur from collisions and falls from chair lifts.1,5
Knee sprains are the most common injury in skiers, making up nearly one-third of total injuries in adults.2,6,7 The medial collateral ligament (MCL) and anterior cruciate ligament (ACL) are involved in most cases. Traditionally, skiing was associated with a high incidence of mid-shaft tibia-fibula fractures, but this injury has declined in incidence significantly as ACL injuries have increased. It is generally believed that releasable bindings are the main reason for this trend. The rise in ACL injuries may also represent better recognition in light of MRI, arthroscopy, and the general availability of reparative techniques now widely used. Emergency evaluation of knee injuries should include a physical examination. As with all extremity injuries, evaluation of distal motor, sensory, and vascular function is important. Injury to the anterior cruciate ligament is assessed with a Lachman test or the pivot shift test. The Lachman test is done with the patient supine and knee bent. The examiner pulls on the upper calf and looks for excessive movement of the joint. At times, it is necessary to compare the two sides. The pivot shift test is done with the knee extended. The examiner twists the knee while pushing on the foot. There are good videos on YouTube for those unfamiliar with the exam. Both the Lachman and pivot shift test are positive when there is a complete tear of the ligament and, therefore, joint instability. In cases of acute injury, the test may be negative due to muscle spasm. As the test can be painful in an acute injury, aggressive technique is not indicated, as a patient with an ACL tear will be stable in a knee immobilizer.
The diagnosis of an MCL tear will have tenderness over the insertion of the ligament. Testing involves applying vagus and varus stress to the knee. Patients should receive X-rays to rule out a fracture, and a knee immobilizer along with orthopedic follow up. Many ACL injuries will ultimately require operative repair.8 Some MCL tears can be managed conservatively.
Approximately one-third of downhill skiing injuries involve the upper extremity, mainly the shoulder and ulnar collateral ligament in the thumb (commonly referred to as gamekeeper’s or skier’s thumb).2 A wide range of shoulder injuries occur, as listed in Table 1. Evaluation of shoulder injuries initially should involve a careful physical exam assessing for any neuro-vascular compromise, deformities, or any loss of range of motion (ROM). X-ray imaging is commonly needed and, aside from glenohumeral dislocations, most injuries can be treated with a sling, analgesics, passive ROM exercises, and close follow up. Patients must be educated as to the importance of keeping the shoulder mobile, even early in treatment, to avoid the devastating "frozen shoulder" or adhesive capsulitis that can evolve with immobilization.9 This is particularly true in older patients.
Table 1:Shoulder Injuries
| More Common | Less Common |
|
|
Sprain or strain of the ulnar collateral ligament (UCL) of the metacarpophalangeal joint of the thumb is the most common upper extremity injury, making up almost 10% of overall injuries.2 It is generally believed that this injury occurs in high frequency due to the use of ski poles. When a skier falls on an outstretched open hand with the pole in the palm, undue forces are placed on that joint. It is theorized that the straps that wrap around the wrist increase the likelihood of injury by not allowing the poles to fall away from the skier’s body during a crash. Therefore, current recommendations favor the use of ski poles without wrist straps. Patients present with pain at the site of insertion of the ulnar collateral ligament as well as pain with pinching the thumb and index finger. Some recommend X-rays prior to stressing the ligament, as it can potentially displace a nondisplaced fracture. Lateral laxity of greater than 35 degrees or more than 15 degrees when compared to the other side suggests a complete tear. However, lateral laxity is not always present shortly after an acute injury due to swelling and muscle contraction. Therefore, all patients with suspected skier’s thumb should have a splint applied and be referred to an orthopedist within one week.
Head injuries are commonly seen in the downhill ski population. They are the leading cause of death in ski accidents and the leading diagnosis requiring admission of child and adolescent skiers.1,5,10 Helmet usage is increasing and is done on a voluntary basis. Although controversy does exist, wearing a helmet has been shown to reduce the risk of head injuries.1 Head injuries occur primarily from falls on the slopes, but collisions with other skiers and snowboarders run a close second.1 Evaluation of the patient with a skiing-related head injury involves a careful neurologic assessment and appropriate spinal precautions. Although there are no specific guidelines for the care of skiers with a concussion, guidelines for other athletes should apply. These guidelines are reviewed later in this paper.
Spinal injuries occur much less often in skiers as opposed to snowboarders, but this gap may be closing due to the increase in skiers involved in aerial maneuvers such as jumps.2
Multisystem trauma is not often seen in downhill skiing, but when it dose occur, it should be managed in a standard fashion. There is growing concern that multisystem trauma may become more of a problem with the increasing popularity of back-country or out-of-bounds skiing and ski jumping.
Snowboarding
Snowboarding is one of the fastest growing winter sports and has only been mainstream for the past few decades. Modern snowboarding was developed in the 1960s and, thus, was a fairly recent addition to the Olympic Games in 1998.11 The number of U.S. snowboarders was estimated to increase from 4.3 million in 2000 to nearly 6.1 million in 2010, with the largest cohort ages 12-24.12,13 The number of recorded U.S. fatalities in the 2009-2010 season was 13 (12 male/1 female).12,13 Most snowboarding is done at standard ski resorts, with the majority of ski resorts allowing both traditional skiing and snowboarding. There are some ski resorts that do not allow snowboarding.
Snowboarding is performed by descending down an incline on a board with both feet secured to the board by bindings. Since both feet are secured to the same object, the movement patterns differ and, thus, the injury patterns seen are different. Another major difference from skiing is that the bindings on the snowboards are mostly non-releasable, as opposed to skis, which are meant to release if enough torque is placed on them.
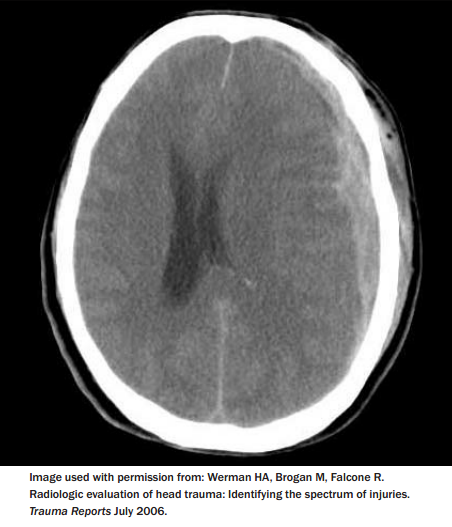
In contrast with alpine skiing, snowboarding is associated with more upper extremity injuries (most commonly wrist injuries), shoulder injuries, ankle injuries, spinal injuries, and head injuries.14-18 (See Table 1.) Head injuries make up nearly one-quarter of snowboarding injuries and are more likely to be seen in male participants. Head injuries account for nearly one-half of the snowboarding injury transfers to trauma centers.1,3 Most of these head injuries occur from loss of the board edge and falling on mild to moderate slopes.1 Snowboarders are more likely to suffer from intracranial hemorrhage requiring craniotomy than skiers, and more frequently require longer rehabilitation and ongoing care. Interestingly, snowboarders are more likely to sustain a subdural hematoma as compared to skiers, who are more likely to have a skull fracture.1 (See Figure for a CT image of subdural hematoma.) Fortunately, most head injuries seen are mild, and the most common diagnosis is concussion. Table 2 shows the incidence of injury to various regions of the brain.19 A growing use of helmets has been associated with a decrease in the number of head injuries and may change some of these patterns of injury.20,21
Table 2: Head Injury Patterns
|
Figure: CT of Subdural Hematoma
A variety of upper extremity injuries/shoulder injuries occur with snowboarding as with skiing.22 (See Table 1.) Injury patterns have changed slightly over time, with an increase in clavicle fractures seen, along with a decrease in medial collateral ligament (MCL) and ankle injuries in snowboarders.15 The major mechanism of injury in snowboarding is falling forward, with torsion of the body coming in second.16 This explains why the upper extremity sustains most of the trauma. There are data to suggest that wrist protectors may aid in the prevention of wrist injuries, especially in beginners who are much more prone to wrist injury.14
Wrist injuries should be assessed by determining neurovascular status and using X-ray imaging when indicated. The most common fracture is the distal radius (Colles’ fracture), which in many cases requires closed reduction to properly align. If displaced, reduction can be performed with or without conscious sedation and/or the use of a hematoma block. Several excellent reviews exist regarding safe and effective sedation in the emergency department.23-25 A splint is then applied and orthopedic referral suggested.
Clavicle fractures, for the most part, are non-operative and are usually managed in a sling. Clavicular straps that once were popular are not commonly used, as they may impinge on nerves and are unnecessary for alignment. Clavicle fractures have a fairly high incidence of malunion, especially the distal third of the clavicle, but function is usually preserved and surgery is usually unnecessary.26 The physical exam should focus on ruling out a brachial plexus injury from bone fragments, performing a vascular assessment of the upper extremity, and assuring adequate lung sounds bilaterally. The most vital aspect of management of clavicle fractures is to educate the patient that mobility of the shoulder is vital and must be maintained. This is usually done in the acute phase by having patients perform pendulum exercises. A resulting frozen shoulder from adhesive capsulitis is a devastating outcome for those patients who keep the shoulder immobile for too long.
Snowboarding lends itself to the more frequent use of terrain parks, which are separate areas of alpine ski resorts that have above the ground metal rails, jumps, and half pipes. Snowboarding in these areas often involves aerial maneuvers, which are associated with an increased risk of head, spine, and abdominal injury and tend to be more serious injuries.18,27 As a result of this greater frequency of abdominal injuries, splenic injuries are seen more often in snowboarders, with a male preponderance.28 Thus, the clinician should inquire as to whether the injury occurred in a terrain park or involved any aerial maneuvers. If so, a level of suspicion should focus the clinical evaluation on occult intra-abdominal injury, such as splenic laceration and spinal injury. Given the high incidence of head injuries and the possible concurrent alcohol use, a low threshold for imaging should exist, along with appropriate spinal precautions. Intra-abdominal injuries are best excluded by contrast-enhanced computerized tomography (CT) of the abdomen and pelvis; however, a quick ultrasound of the abdomen (FAST) can help determine the presence or absence of free fluid in the abdomen.
There is a growing interest and participation in snowboarding and skiing in the back country. Paralleling this trend is a rise in the number of deaths from snow avalanche.3 Death from avalanche usually results from asphyxiation, and the snowboard may predispose participants to a higher risk of death when avalanche occurs, since the bindings don’t release. This makes it harder for the victim to dig out when buried and for others to extract the snowboarder from under the snow. This form of boarding exposes people to more risk of environmental hazards, such as hypothermia, frostbite, avalanche, and falling into crevasses. Standard mountaineering skills are warranted. Back-country skiing should be reserved for those with intermediate to expert snowboarding skills, mountaineering experience, those using appropriate equipment, and those who are physically fit. It should not be done alone. Otherwise, they place themselves in a higher-risk situation.
Cross-country Skiing
Cross-country skiing (also referred to as ski touring) is a type of Nordic skiing in which the skier uses slender skis and poles to move across snow-covered terrain that is fairly flat. As a form of Nordic skiing, only the toe of the boot, and not the heel, is fixed to the ski. Other forms of Nordic skiing include ski jumping, telemark skiing, and biathlon. Cross-country skiing is most popular in Scandinavia and Canada, with some participation in the United States and Europe.
Injury data are scarce pertaining to cross-country skiing since it often takes place in non-designated areas and is not as regionalized like downhill skiing, where clinics and local hospitals will concentrate the injuries for data collection. This form of skiing at the recreational level and competitive level is considered an endurance sport and, thus, is fraught with mostly overuse injuries (75%) vs. acute trauma (25%).29 Of the traumatic injuries seen, most occur on downhill terrain and involve the lower extremity.30 There are a variety of injuries seen, but good data don’t exist as to the specific incidence of each. (See Table 3.) The most common overuse injuries occur in the shoulder and upper torso.31 The most common traumatic injuries are MCL and ulnar collateral ligament (UCL) thumb sprains.32 The latter are usually the result of a fall while the skier is holding ski poles.
Table 3: Cross-country Skiing Injuries
| Overuse | Trauma |
|
*most common upper extremity injury |
There are two major techniques to cross-country skiing: classic and skating. The classic technique involves more of a shuffling or gliding forward on one ski, while the skating technique involves more of a lateral push off similar to skating. There has been no significant difference in injury pattern found between the two techniques.33 Prevention strategies should focus on strength training and conditioning, proper technique, and letting go of the poles when falling. Use of poles without wrist straps is recommended, as it is for downhill skiing to prevent UCL injuries.
Ice Skating
There is a paucity of literature regarding injuries during ice skating. Ice skating is enjoyed as a recreational activity as well as a competitive venue. In most settings, skaters do not wear protective equipment.34 As one would guess, collisions with the ice are a major source of injury. This is in contrast to ice hockey, in which players are heavily padded and, thus, don’t sustain many injuries due to impact with the ice surface. Injuries occur more often in beginning skaters,35 with fractures and lacerations of the hand quite common.36 Falls on the outstretched hand or onto the elbow are common, with the associated fractures to the wrist and elbows. Skate blades are particularly sharp, especially for more serious skaters, and can cause significant lacerations. In one case seen by the editor, the blade penetrated the anus, leading to an extensive rectal laceration. As with many other sports, alcohol tends to increase the risk of injury.37
Another common injury is a fracture of the coccyx. The diagnosis is generally made clinically, as imaging is difficult and high radiation levels are needed. Finding a fracture does little to alter the treatment or prognosis. Open fractures are rare but should be ruled out with an appropriate rectal examination. Most pharmacies carry donut pillows, which are designed to keep weight off the coccyx. Analgesics and time are needed. Some patients will find stool softeners to be beneficial.
Figure skaters who train regularly are more skilled and, thus, prone to overuse injuries vs. traumatic injuries.38,39 Stress fractures are not uncommon injuries in figure skaters.38
Ice Hockey
Ice hockey is a team sport in which skaters use sticks to move a hard rubber puck around the ice surface while attempting to put it in the opponent’s net. It is a fast-paced sport that is played around the world, but is most popular in Canada, the United States, and Europe. The International Ice Hockey Federation has 52 full members (countries in which field teams in international competition). It is the official winter sport of Canada and dates back to the first official recorded game in Montreal in 1875.40 Originally played on frozen ponds, lakes, and rivers, it has evolved into a worldwide sport for which many countries field Olympic teams. Like other winter sports, involvement in ice hockey grew over the past decade, with more than 500,000 players registered in the United States and more than 600,000 registered in Canada for 2012-2013. These statistics don’t take into account kids who play on ponds, lakes, and parks and doesn’t include the thousands of adults who play in various leagues throughout the United States and Canada.
Ice hockey is primarily played in indoor ice arenas where the field of ice is surrounded by boards. However, the boards also provide another obstacle with which players can collide and become injured. Injuries from ice hockey are the result of trauma (80%) and overuse (20%).41 Injuries can occur in a number of different ways. Most commonly, injuries occur during body checking, in which a defensive player attempts to gain possession of the puck by a body-to-body collision intended to separate the puck carrier from the puck.42 These collisions create injury more commonly in open ice than when a player is checked into the boards.43 Defensive players have been shown to have a slightly higher rate of injury.44 After body checking, injuries occur commonly from contact with the sticks or pucks. Common injuries to the upper extremity include scaphoid fractures, UCL injury, and acromioclavicular joint sprains and dislocations.41 In contrast, soft-tissue injuries predominate in the lower extremity, such as thigh contusions, adductor hip strains, and MCL injuries.41
Controversy exists as to the optimal age to begin body checking in ice hockey. In the United States, body checking used to begin around age 11-12 (peewee level), compared to Quebec where body checking begins at age 13-14 (bantam level). Recently, body checking in the younger players was found to be associated with a three-fold increase in game-related injuries.45 This has prompted USA hockey to change the age of body checking to the bantam level (ages 13-14). This move seems intuitive to many, but proponents of early body checking argue that if physical contact is allowed from the beginning, kids will learn to skate with more awareness and will better protect themselves. Injuries due to physical contact occur at a much greater frequency the first year or two after the introduction of body checking, but these spikes in injury incidence then decline after players get used to this style of hockey.46
Concussions are some of the more common injuries in ice hockey and, therefore, assessment and management as well as return to play are vital skills. Signs and symptoms of concussion are listed in Table 4 and typically are most severe during the first 24-48 hours, and then slowly abate over the following days to weeks.47 Players diagnosed with a concussion should be removed from play (including non-contact practice) until a full evaluation is performed. Depending on the severity of symptoms, a player may require brain imaging if there is a loss of consciousness, abnormal neurologic exam, or other concerns for intracranial hemorrhage. In most cases, imaging is not necessary. Rest with as little stimulation as possible is optimal. Some athletes with ongoing symptoms should be referred for neuropsychological testing (NP), which is often more sensitive for detecting brain dysfunction from concussion than the physician’s clinical exam. Most players, however, can be managed without NP testing.48
Table 4: Concussion Signs and Symptoms
| Signs Observed by Medical Staff | Symptoms Reported by Athlete |
|
|
The CDC has published information for general use by clinicians, which includes a pocket card. Recognition of concussion is often easier than making return-to-play decisions. It is not uncommon for hockey players who have sustained a concussion to present to the emergency department for evaluation and foremost on their mind is "When can I play again?" Return-to-play decisions should be made by a physician who has been trained in the evaluation and management of concussions.48 Generally, return to play is a graduated stepwise process in which first the activity level is increased to see if any recurrence of symptoms occurs. If so, the patient goes back to the beginning and must undergo another period of rest.48
Dental injuries are common, particularly in athletes who do not wear mouth guards. While well-fitting mouth guards can be custom fitted by a dentist, there is no evidence that these prevent injury better than less expensive store-bought devices. Helmets with face shields also prevent dental and facial injuries, once far more common in the sport.
Injury patterns at the youth level differ from those at the high school, college, and adult elite levels. At an elite level, most injuries occur during competition as opposed to practice.44 Youth hockey players are much more likely to experience concussion or various soft-tissue contusions, as opposed to older athletes who are more likely to have sprains or ligamentous injury.45 In addition, the preseason practice injury rate was found to be greater than twice that of regular season practices.43 Most of these injuries include various contusions, strains, and sprains from body-to-body contact, with the most common serious injury being medial collateral ligament (MCL) tear.44
Snowmobiling
Snowmobiling is a popular sport that involves operating a motorized sled on snow and ice surfaces. It is enjoyed by more than two million people in North America and accounts for approximately 14,000 injuries and 200 deaths annually.49 Snowmobiling often involves high speeds, sometimes in excess of 100 mph, on natural terrain; thus, multisystem trauma and head injuries are a leading cause of morbidity and mortality.50 Head injuries are the leading cause of death in snowmobiling accidents in both adults and pediatric populations.50-52 Snowmobiling injuries are, for the most part, due to human error, and male gender and alcohol consumption have been found to be the biggest risk factors.51,53 Interestingly, only 15% of snowmobile accidents occur on groomed, designated trails where roughly 80% of riding occurs.1 That is to say that most injuries occur while riding on ungroomed trails and on roadways. Several risk factors have been identified, with the most common being poor lighting conditions, which explains why riding groomed trails is associated with safer snowmobile operation.50 Other risk factors include alcohol consumption and excessive speed.50 Snowmobiling is enjoyed by a wide age range, including older children. In children, the most common injury is to the head, followed by the extremities, with head injury being the most common cause of death.54 Despite this, helmet laws are often non-existent or do not pertain to private property in many states.55 Perhaps the most alarming statistic is the finding that only 35% of riders who were fatally injured were wearing a helmet.56
Given the likelihood of high-speed injuries with snowmobiling, emergency physicians should become very familiar with ATLS and the management of the multisystem trauma patient. Many snowmobile accidents involve multisystem trauma and concurrent alcohol intoxication. This requires a high index of suspicion for occult injuries.
For high-speed crashes or those involving intoxicated patients, a CT scan of the chest, abdomen, and pelvis may be indicated, even if the physical exam is equivocal or if the patient is altered. For isolated fractures not involving high-speed crashes, CT is not necessary. Displaced and open fractures require urgent attention with an initial assessment of neurovascular status. If intact, then reduction can usually wait for X-ray imaging. However, where there is vascular insufficiency distal to the injury, reduction can be attempted prior to X-rays, especially if imaging will be delayed. Open fractures should have minimal exposure. They should be quickly irrigated if obvious contamination is evident and covered with a sterile dressing. Intravenous antibiotics are indicated prophylactically. Open fractures are graded as shown in Table 5, which has implications for treatment.
Table 5: Grading of Open Fractures
| Grade | Characteristics |
|
I |
Small, < 1 cm, clean wound |
|
II |
Larger, > 1 cm, clean wound without extensive soft-tissue damage |
|
III |
Extensive tissue laceration, damage, or loss, or segmental fracture; fractures that have been open for > 8 hours |
Clearly the above information suggests that preventative strategies can target high-risk behaviors such as drinking alcohol and operating a snowmobile in unfamiliar territory after dark. Also, programs aimed at improving helmet compliance may yield better injury statistics.
Sledding
Winter snow sledding is a sport that is enjoyed in northern climates by people of all ages, but most commonly children and adolescents. Sledding is most commonly defined as travelling downhill on snow with some sort of sled, which can range from the elaborate flexible flyer to an improvised sled such as a cafeteria tray. The activity is performed in a seated or lying position, either head first or feet first. Sledding is done in both the recreational and competitive venue (bobsledding, luge, skeleton). The activity is enjoyed in rough natural environments as well as structured park environments designed specifically for this activity.
The injury patterns can vary slightly depending on the environment in which the activity is done. In more rural, natural environments, collisions are more likely to occur with structures such as trees and rocks and are less likely with other sledders. In contrast, public sledding parks often have higher volumes of sledders, and collisions with other sleds and with pedestrians are more likely.
Sleds come in a variety of different forms and vary in complexity from simple sheets of plastic to higher-tech sleds made of wood and metal with maneuvering capability. Sleds can be single-person vehicles such as saucers or multi-person toboggans.
One review found that there were an estimated 57,000 ED visits in the United States during the 2001-2002 winter for sledding-related injuries.57 Sledding speeds, even in recreational areas, can be significant. In one study in Rochester, NY, the average maximum speed attained during a run was 19 mph, with the highest recorded as 25 mph. Plastic tube devices were the fastest. In this study, no individual was observed wearing a helmet.58 Although sledding is enjoyed by multiple age ranges, most injuries occur in the 5- to 14-year-old age range, and are the result of falls or collisions.57 The body part injured has also varied depending on the age, with children younger than age 9 most likely to experience head and neck injuries. Older children (7-18 years) were more likely to sustain an extremity injury.59 Sledding accidents that lead to injury are most commonly from a collision with a stationary object.59
Opportunities exist for injury prevention, given that more than 50% of injuries were of the head and neck region, but less than 5% of sledders wore helmets.59 Injury prevention can also be focused on sled construction and the development of safe obstruction-free sledding hills.
Special Considerations in the Older Adult
The aging Baby Boomer generation is participating in athletic activities in large numbers. Despite increased fitness of this group, age-related effects need to be addressed. Older adults are more susceptible to hypothermia and dehydration. They are less likely to drink when dehydrated, as their thirst response may be blunted or they may be taking diuretics. Even with exercise and calcium/vitamin D replacement, bones weaken with age, making fractures more common.
Physicians can intervene by helping advise patients as to proper attire for winter sports. Layering of clothing is vital, with the base layers not made of cotton but instead with synthetic fibers that wick moisture away from the body. The next layer should be an insulating layer that helps maintain core temperature. The current trend is to wear a separate outer shell made of a breathable, water- and wind-resistant material such as Gore-Tex. This way, if temperatures rise, then the insulating layer can be removed, leaving just the base layer and outer shell. Also, hydration during outdoor winter sports can be easily maintained using various products such as camelbacks, small lightweight backpacks that are hydration compatible, or waist-mounted water bottles.
Perhaps most importantly, head injuries can be more serious. A large number of older adults are anticoagulated, most often for atrial fibrillation. In addition, with age the brain shrinks, with increased tension to the bridging veins. Relatively minor injuries can cause bleeding in these patients. Because there is "extra space" between the brain and skull, symptoms may be less evident or may be delayed. Many providers have a lower threshold for ordering a CT scan in these patients compared to younger adults. Because there is a small risk of delayed bleeding in anticoagulated patients, some providers observe these patients for six hours, repeating the CT scan at that time. It has been shown that patients on clopidogrel have a higher incidence of intracranial hemorrhage after head injury when compared to those on warfarin.59 However, those on warfarin are more likely to have a delayed hemorrhage, albeit this is rare.60
Summary
With millions of people involved in winter sports, injuries presenting to emergency departments in northern climates have become a common occurrence. Certain injury patterns exist for each winter sport, which can be useful to the clinician when assessing an injured winter athlete. Musculoskeletal injuries predominate, with extremity injuries and head injuries the most common. Multisystem trauma does occur due to high speeds involved in some winter sports, such as extreme skiing, snowboarding, and snowmobiling. Thus, emergency physicians should have training and systems in place to stabilize and manage these patients. EPs should be familiar with Advanced Trauma Life Support (ATLS) principles in order to optimize outcomes. Opportunities exist for preventative public health measures and interventions by physicians that can reduce these injuries.
References
- Chaze B, McDonald P. Head injuries in winter sports: Downhill skiing, snowboarding, sledding, snowmobiling, ice skating, and ice hockey. Neurology Clinics 2008;26:325-332.
- Koehle M, Lloyd-Smith R, Taunton J. Alpine ski injuries and their prevention. Sports Med 2002;32(12);785-793.
- Van Tilburg C, Backcountry snowboarding: Medical and safety aspects. Wilderness and Environmental Medicine 1996;3:
225-231. - Wikipedia. "Ski." Last updated 10/13/2013. Accessed on 11/2/2013.
- Skokan EG, Junkins EP Jr, Kadish H. Serious winter sport injuries in children and adolescents requiring hospitalization. Am J Emerg Med 2003;21(2):95-99.
- Warme WJ, Feagin Jr JA, King P, et al. Ski injury statistics, 1982-1993, Jackson Hole Ski Resort. Am J Sports Med 1995;23(5):597-600.
- Deibert MC, Aronsson DD, Johnson RJ, et al. Skiing injuries in children, adolescents, and adults. J Bone Joint Surg Am 1998;80(1):25-32.
- Cross MJ. Anterior Cruciate Ligament Injuries: Treatment and rehabilitation. Internet Encyclopedia of Sports Medicine and Science. http://sportsci.org. 26 Feb 1998.
- Manske RC, Prohaska D. Diagnosis and management of adhesive capsulitis. Current Review of Musculoskeletal Medicine 2008;1(3-4):180-189.
- Hackam DJ, Kreller M, Pearl RH. Snow-related recreational injuries in children: Assessment of morbidity and management strategies. J Pediatric Surg 1999;34(1):65-68.
- Snowboarding. www.wikipedia.org. Accessed on 10/31/2013.
- Snowboarding statistics, verified 6/20/2012 from National Ski areas association, National Sporting Goods Association, National Ski & Snowboard retailers association. Accessed 10/31/2013.
- www.statisticbrain.com. Accessed 10/31/2013.
- Rønning R, Rønning I, Gerner T, et al, The efficacy of wrist protectors in preventing snowboarding injuries. Am J Sports Med 2001;29:581-585.
- Kim S, Endres NK, Johnson RJ, et al. Snowboarding injuries: Trends over time and comparisons with alpine skiing injuries. Am J Sports Med 2012;40:770-776.
- Biasca N, et al. An overview of snow-boarding injuries. Unfallchirurg 1995;98(1):33-39.
- Abu-Laban RB. Snowboarding injuries: An analysis and comparison with alpine skiing injuries. CMAJ 1991;145(9):
1097-1103. - Chow T. Spectrum of injuries from snowboarding. Journal of Trauma-Injury Infection & Critical Care 1996;41:
321-325. - Fukuda O, Takaba M, Saito M, et al. Head injuries in snowboarders compared with head injuries in skiers. A prospective analysis of 1076 patients from 1994 to 1999 in Niigata, Japan. Am J Sports Med 2001;29(4):437-440.
- Sulheim S, Holme I, Ekeland A, et al. Helmet use and risk of head injuries in alpine skiers and snowboarders. JAMA 2006;295(8):919-924.
- Hagel BE, Pless IB, Goulet C, et al. Effectiveness of helmets in skiers and snowboarders: Case control and case crossover study. BMJ 2005;330(7486):281-285.
- Kocher MS, et al. Shoulder injuries from alpine skiing and snowboarding. Aetiology, treatment, and prevention. Sports Medicine 1998;25(3):201-211.
- Mistry RB, Nahata MC. Ketamine for conscious sedation in pediatric emergency care. Pharmacotherapy 2005;25(8):
1104-1011. - Godambe SA, et al. Comparison of propofol/fentanyl versus ketamine/midazolam for brief orthopedic procedures. Pediatrics 2003;112:116-123.
- Innes G, et al. Procedural sedation and analgesia in the emergency department. Canadian consensus guidelines. J Emerg Med 1999;17:145-156.
- Clavical fractures. Wheeless’ textbook of orthopedics online. www.wheelessonline.com. Last updated January 15, 2013. Accessed 10/31/2013.
- Brooks MA, et al. Brief Report: Evaluation of skiing and snowboarding injuries sustained in terrain parks versus traditional slopes. Injury Prevention 2010;16:119-122.
- Geddes R, Irish K. Boarder belly: Splenic injuries resulting from ski and snowboarding accidents. Emergency Medicine Australia 2005;17:157-162.
- Renstrom P, Johnson RJ. Cross-country skiing injuries and biomechanics. Sports Medicine 1989;8(6):346-370.
- Boyle JJ, et al. Cross-country ski injuries: A prospective study. The Iowa Orthopedic Journal 1981;1:41-45.
- Orava S, et al. Overuse injuries in Cross-country skiing. British Journal of Sports Medicine 1985;19:158-160.
- Smith M, Matheson GO, Meeuwisse WH, Injuries in cross-country skiing: A critical appraisal of the literature. Sports Med 1996;21(3)239-250.
- Butcher JD, Brannen SJ. Comparison of Injuries in classic and skating Nordic ski techniques. Clinical Sports Medicine 1998;8(2):88-91.
- McGeehan J, Shields BJ, Smith GA. Children should wear helmets while ice-skating: A comparison of skating-related injuries. Pediatrics 2004;114(1);124-128.
- Williamson DM, Lowdon IMR. Ice-skating injuries. Injury 1986;17(3);
205-207. - Murphy NM, Riley P, Keys C, Ice-skating injuries to the hand. J Hand Surgery: British & European Volume 1990;15(3);349-351.
- Oakland CD. Ice skating injuries: Can they be reduced or prevented? Arch Emer Med 1990;7:95-99.
- Dubravcic-Simunjak S, Pecina M, Kuipers H, et al. The incidence of injuries in elite junior figure skaters. Am J Sports Med 2003;31(4);511-517.
- Bloch RM. Figure skating injuries. Phys Med Rehabil Clin N Am 1999;10(1):
177-188. - Wikipedia. "Ice_hockey." Accessed 10/25/2013.
- Daly P, Sim F, Simonet W. Ice hockey injuries. Sports Medicine 1990;10(2);
122-131. - Benson BW, Meeuwisse WH. Epidemiology of pediatric sports injuries: Team sports; ice hockey injuries. Basel, Karger 2005;49:86-119.
- Agel J, et al. Descriptive epidemiology of collegiate men’s ice hockey injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. Journal of Athletic Training 2007;42(2):241-248.
- Lorentzon R, et al. Incidence, nature, and causes of ice hockey injuries: A three-year prospective study of a Swedish elite ice hockey team. Am J Sports Med 1988;16:392-396.
- Emery CA, et al. Risk of injury associated with body checking among youth ice hockey players. JAMA 2010;303:
2265-2272. - Willer B, Kroetsch B, Darling S, et al. Injury rates in house league, select, and representative youth ice hockey. Medicine & Science in Sports & Exercise 2005;37(10):1658-1663
- McCrory P, Meeuwisse W, Echemendia R, et al. What is the lowest threshold to make a diagnosis of concussion? Br J Sports Med 2013;47:268-271.
- Harmon KG, Drezner JA, Gammons M, et al. American Medical Society for Sports Medicine position statement: Concussion in sport. Br J Sports Med 2013;47:15-26.
- Pierz JJ. Snowmobile injuries in North America. Clin Orthop Relat Res 2003;409:29-36.
- Stewart R, Black B. Snowmobile trauma: 10 years’ experience at Manitoba’s tertiary trauma centre. Canadian J Surgery 2004;47:90-94.
- Sy ML, Corden TE. The perils of snowmobiling. WMJ 2005;104(2):32-34.
- Rice MR, Avanos L, Kenney B. Snowmobile injuries and deaths in children: A review of national injury data and legislation. Pediatrics 2000;105(3 Pt 1):615-619.
- Beilman GJ, et al. Risk factors and patterns of injury in snowmobile crashes. Wilderness Environ Med 1999;10(4):
226-232. - Decou JM, et al. Snowmobile injuries and fatalities in children. J Pediatric Surg 2003;38(5):784-787.
- Manda R, et al. Snowmobile injuries and deaths in children: A review of the national injury data and state legislation. Pediatrics 2000;105:615-619.
- Landen MG, Middaugh J, Dannenberg AL. Injuries associated with snowmobiles, Alaska 1993-1994. Public health Rep 1999;114(1):48-52.
- Skarbek-Borowska S, Amanullah S, Mello M, et al. Emergency department visits for sledding injuries in children in the United States in 2001/2002. Acad Emerg Med 2006;13(2):181-185.
- Compelling LC, Garcia M, Rueckmann E, et al. Sledding: How fast do they go?
J Trauma 2009;66:S23-S26. - Ortega H, et al. Sledding-related injuries among children requiring emergency treatment. Pediatric Emergency Care 2005;21:839-843.
- Nishijima DK, Offerman SR, Ballard DW, et al. Immediate and delayed traumatic intracranial hemorrhage in patients with head trauma and preinjury warfarin or clopidogrel use. Ann Emerg Med 2012;59:460-468.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
