A Literature-Based Approach to the Identification and Management of Pediatric Foreign Bodies
Authors: Lance Brown, MD, MPH, FACEP, Fellow, Pediatric Emergency Medicine, Department of Emergency Medicine, Loma Linda University Medical Center, CA; and Bernard Dannenberg, MD, FAAP, FACEP, Fellowship Director, Pediatric Emergency Medicine; Assistant Professor of Emergency Medicine, Department of Emergency Medicine, Loma Linda University Medical Center, CA.
Peer Reviewer: Steven M. Winograd, MD, FACEP, Attending Physician, Department of Emergency Medicine, Jeannette District Memorial Hospital, Jeannette, PA; Attending Physician, St. Clair Memorial Hospital, University of Pittsburgh Medical Center.
Successfully managing a child with a foreign body can be a tremendously rewarding experience for an emergency physician. Retrieving the offending object in a calm and efficient manner can make the emergency physician a hero in the eyes of many families. Alternatively, emerging from a bloody area without the object can have the opposite effect. Equally frustrating is the experience of confidently telling a family that there is no foreign body only to find out later there was one that resulted in complications.
All emergency physicians who see children in their practices will come across foreign bodies on occasion. Children seem to have boundless imagination when it comes to where they will position a foreign body and what they will use. Older siblings also may provide support and encouragement to the younger child. The traditional approach to these patients characteristically has been based on anecdotal tales, fits of creativity, and common sense. This article reviews the available literature in an attempt to build an evidence-based approach to the identification and management of foreign bodies in the nose, ear, gastrointestinal tract, airways, genitourinary tract, and the rectum.— The Editor
Nasal Foreign Bodies: Identification
Nasal foreign bodies predominantly are seen in preschool-aged children. In one study of 60 children with nasal foreign bodies, the age range was from 16 months to 9 years, with an average age of 3 years.1 A series involving 78 children with nasal foreign bodies, reported an age range from 1 to 6 years of age with an average age of 2 and a half years.2 In this study, 70% of the children were between 2 and 4 years of age. The list of objects removed from noses in children is lengthy. The most commonly reported objects include beads, plastic toy parts, wads of paper, food (including corn kernels, beans, and seeds), and small rocks.1,2 Girls have been reported to be somewhat more likely to put objects up their noses; this is thought to be due to the disproportionate number of hair beads that girls put up their noses.2
The most frequent presenting symptoms described in the literature include pain or discomfort in 23-55% of patients1,2 and odor and nasal discharge in 14-36% of patients.1,2 Bleeding is uncommon and characteristically is seen when objects are sharp or pointed.2 Although the presenting complaint is typically straightforward (namely "something up the nose"), special attention should be made to what could be called "occult" nasal foreign bodies. On occasion, a child will present with unilateral foul nasal discharge without a history of nasal foreign body. The frequency with which nasal foreign bodies present with unilateral foul nasal discharge or bad breath is common enough, and other causes are rare enough to suggest that any young child with unilateral nasal discharge should be suspected of having a nasal foreign body until shown otherwise.3 In one study, this "occult" presentation was seen 7% of the time.1
Nasal Foreign Bodies: Management
Most papers describing techniques for removing nasal foreign bodies are small case reports extolling the virtues of the author’s favorite technique4-9 or otolaryngology reviews based on literature that is decades old.10 One author of a letter to the editor went so far as to call himself a "purveyor of and cheerleader for" a particular technique.5 In these circumstances, an unbiased view would seem unlikely. In addition, given the vast array of objects with different friability, consistency, sharpness, shape, and absorbency, it would seem prudent for emergency physicians to have familiarity with multiple techniques to best meet the individual needs of the patient based on the type of object encountered.
Emergency physicians reasonably can expect to remove the vast majority of nasal foreign bodies without consultation with a subspecialist. In the two largest studies available, success rates for emergency physicians ranged from 92% to 98%.1,2 Emergency physicians should be prepared to employ more than one technique in any patient, as one could reasonably expect to use multiple attempts about 25% of the time and multiple techniques 15% of the time.1 The various techniques described in the literature are outlined below.
Forceps and Hooks. A commonly used technique is simply to grab the object with forceps and pull it out.1,2 The use of straight, mosquito, and alligator forceps is described in the literature.2 This technique is best applied to objects that are anterior and easily grasped. Objects that are large, posterior, smooth, or round are the worst candidates for this technique. Objects that fall apart easily, such as wads of paper and soft foods, also are not optimally removed by this technique.1 Similarly, a hooked probed could be used. In this technique, the probe is passed over the object and turned so that the object is hooked posteriorly and pulled out. Objects that are too large to allow the hook to pass, those that fall apart when contacted, or those posteriorly placed should not be removed using this technique.
The instruments used for these techniques are made of hard metal, and mucosal damage and bleeding may occur. This usually is mild and relieved with a brief period of direct pressure after the object is removed. A more serious potential complication is pushing the object posteriorly. Pushing the object posteriorly makes the object more difficult to remove on subsequent attempts and may lead to aspiration of the foreign body. There were no reports of aspiration following attempted nasal foreign body removal in the literature.
Positive Pressure. This technique involves generating air pressure behind the object to expel it anteriorly. Two techniques are described: the "kiss"5,6,11,12 and "ambu-bag insufflation techniques."4,8,12 The process is quite straightforward in concept and implementation. In both techniques, the contralateral (i.e., uninvolved) nostril is occluded by lateral pressure with the examiner’s finger. A forceful puff of air is then given in the patient’s mouth. In the kiss technique, the parent blows into the patient’s mouth. In ambu-bag insufflation, a small mask is used over just the mouth, a seal is formed, and a forceful puff of air is applied through the patient’s mouth. This technique is particularly good for large, posterior objects like beads, rocks, and beans, which may occlude the entire nasal passage .1 The kiss technique involves total parental involvement and can be rewarding to the parent. The ambu-bag technique can be expensive, and sometimes it is difficult to get a good seal around the mouth. There is a theoretical risk of barotrauma to the tympanic membranes or lungs, but this complication has not been reported in the literature.
Nasal Wash. A technique recently described in the literature involves nasal irrigation.7 In this technique, a bulb syringe with 7 cc of sterile saline is inserted into the nostril opposite from the one containing the foreign body (i.e., the contralateral side). The bulb then is forcefully squeezed and the expectation is for the foreign body to be expelled anteriorly. A single article describes three cases in which this technique was used successfully.7 Critiques of this technique express concern regarding the risk of aspiration and choking.13
Balloon Catheter. This technique involves the use of a catheter such as a small Foley catheter or a Fogarty biliary balloon catheter.1,14,15 In this technique, a catheter that is 8 French in size or smaller (5 or 6 French has been recommended if available in the emergency department1 [ED]) is lubricated and passed beyond the object with the balloon deflated. The balloon then is partially inflated, and the catheter is withdrawn. The object should be swept anteriorly and out of the nose with the catheter as it is withdrawn. The balloon catheter technique particularly is good for solid, round objects that are not easily grasped with forceps and do not completely occlude the nasal passage.14 Epistaxis as a complication from this technique has been described in one case in the literature, and this patient’s bleeding stopped after a few minutes of direct pressure.1
Adhesives. A single case report in the literature reviewed the use of an adhesive to remove a nasal foreign body.9 The authors describe using cyanoacrylate glue to coat the cut surface of a hollow plastic swab stick. The glued end of the stick was then pressed against the object for 60 seconds. The bead was removed without difficulty. Gluing the object, the swab stick, or both to the nasal mucosa would seem to be an obvious, if not yet reported, potential complication of this procedure.
Suction Catheter. The literature contains a few cases of nasal foreign body removal by suction catheter.1,2,16 The most detailed description involves using a Schunkt-neck suction catheter that has a plastic umbrella at the tip.1 In this technique, the suction end of the catheter is placed against the object, and the suction is then turned on to between 100 mmHg and 140 mmHg. The object is removed as the catheter is withdrawn with suction applied. There is a risk of pushing the object posteriorly with this technique.
Ear Foreign Bodies: Identification
Foreign bodies of the ear canal usually are seen in an older group of patients than foreign bodies of the nose. In a study that included patients up to 17 years of age, 134 ear foreign bodies presented to a pediatric ED. Thirty-seven percent were in children ages 2-4 years; 36% were in patients ages 5-8 years of age; and 27% were in patients ages 9-16 years.2 In another series at a specialized otolaryngology referral hospital, children with ear foreign bodies ranged from 10 months to 17 years of age, and 74% of these patients were younger than 8 years of age.17 In one interesting study involving children and adults who were predominantly indigent or incarcerated, the mean age was 23.5 years, with 57% of the patients older than 12 years of age.18 The most commonly reported ear foreign bodies included cockroaches (16% of cases), wads of paper (15%), plastic toy parts (7%), earring fasteners (7%), hair beads (6%), and fruit seeds (4%).2 One notable foreign body that has been described in the literature in fewer than a dozen cases is the disc battery. These are small, flat batteries that power watches and other small electronic devices. They easily fit into most children’s ear canals. These batteries can cause extensive tissue damage if left undiagnosed or untreated.19-25
Ear foreign bodies can have quite a varied presentation. The most common is a simple statement by the patient or family that something is in the ear canal. Pain may occur in as many as 90% of cases.2 Decreased hearing might be expected in fewer than one-third of cases.2 Bleeding is an uncommon complaint unless the object is sharp or pointed, or the parent has attempted to remove the object.2 Cockroaches squirming around in the ear canal can be a particularly disturbing experience for patients and prompt immediate presentation for removal.2,18 Occasionally, a patient may present with persistent cough or hiccups as the only manifestation of their ear canal foreign body.17,26,27 Foreign bodies also may present as cases of seemingly straightforward otitis externa. This scenario particularly may be destructive if the object is a disc battery and there is a delay in the identification of the foreign body or its removal is delayed.19 Fortunately, disc batteries are metallic, and if a computerized tomographic (CT) scan is performed to rule out mastoiditis, the radiopaque foreign body should be identified readily in the external auditory canal.19
Ear Foreign Bodies: Management
There is very little literature describing the management of foreign bodies in the ear canal. The larger studies are from otolaryngologists who see a selected referral base of patients.17,18,28,29 Included in these reports are failed first attempts by other practitioners, including emergency physicians. These studies seem to emphasize the complications of procedures performed by emergency physicians and operative techniques, general anesthesia, and the use of an operating microscope.17,18,28,29 Other papers are simple case reports of the successful removal of foreign bodies 9,30-32 or case series that emphasize a single technique.33 Only one article mentions the use of procedural sedation (ketamine) in the outpatient setting.28 In contrast, Baker reported in 1987 on 134 ear foreign bodies seen in a pediatric ED or walk-in clinic that initially were managed by pediatric emergency physicians or physician’s assistants. Baker found that 80% of the ear foreign bodies were removed by these emergency practitioners without otolaryngology consultation.2 Parental attempts at removing the objects at home significantly increased complications and the need for referral.2 Given that emergency physicians should expect to manage most ear foreign bodies without consultation, emergency physicians should be familiar with a wide variety of alternative techniques for removal.
Forceps and Hooks. A simple concept is to grab the object and pull it out. A variety of forceps have been used for this purpose and include straight, mosquito, and alligator forceps.2 This technique is particularly successful with smaller objects in the lateral third of the ear canal.17 In one study, this technique was successful more than half of the time.2 Similarly, small hooked probes or ear curettes have been described as useful. The hooked instrument is passed beyond the object (deeper in the canal) and then turned so that the object is hooked from behind and withdrawn with the instrument. This technique fails when the object obstructs too much of the canal for the hooked probe to pass beyond the object. Both hooks and forceps usually are made of metal, and the medial (bony) canal easily can be lacerated, resulting in pain and bleeding. Similarly, the middle ear structures can be damaged if either the object is pushed further into the canal or the instrument is positioned too deeply in the ear canal.
Irrigation. Irrigation is the second most commonly used technique for ear foreign body removal.2 Irrigation involves instilling warm water or saline into the ear canal under some pressure via a syringe. A 14- or 16-gauge angiocath may be attached to the end of the syringe to better direct the flow.17 One study reported an impressive 88% success rate for an electric irrigation syringe designed and marketed specifically for ear foreign bodies. Generalization of these results is questionable as the clinicians used the syringe in only about half of the potential cases.33 Irrigation is appropriate only if there is a reasonable expectation that the tympanic membrane is intact. Although there are no formal published data on this, it would seem reasonable to expect an intact tympanic membrane if either the tympanic membrane can be seen and is intact or the object visually is noted to be in the lateral part of the ear canal (not too deep), the object is not suspected of being sharp, there is no bleeding or dried blood present, and there have been no parental attempts at removal. Irrigation generally is not recommended for objects that might absorb water and swell within the ear canal, such as vegetable pieces, beans, and other soft food.17 Irrigation is strictly contraindicated if there is suspected tympanic membrane perforation or if the object is suspected of being a disc battery (irrigation promotes destructive alkaline fluid leakage). Although patients complain that the procedure is loud, irrigation has the advantage of generally causing no injury if unsuccessful and usually can be performed in young children, as some movement during the procedure generally causes no harm.
Adhesive. The use of cyanoacrylate to remove foreign bodies in the ear canal has been described in a very small number of cases. One case in the literature describes a teenager with a bead in the ear canal.9 The authors describe using cyanoacrylate glue to coat the cut surface of a hollow plastic swab stick. The glued end of the stick was then pressed against the object for 60 seconds. The object was removed without difficulty. Gluing the object, the swab stick, or both to the ear canal would seem to be a potential complication of this procedure. This procedure requires a certain degree of patient cooperation and has been discussed as being inappropriate for younger children.30
Chemicals to Dissolve the Foreign Body. Plastic foam (i.e., Styrofoam) is a particularly challenging foreign body. Plastic foam "peanuts" used in shipping can be compressed by attempts at removal and make a firm, compact plug that completely occludes the ear canal. Similarly, the material can be friable and break off in pieces with attempted removal. Two case reports in the literature report the successful removal of plastic foam from the ear canals of school-aged children using a small amount of ethyl chloride in one case and 0.1 mL of pure acetone (obtained from the hospital lab) in the other.31,32 In both cases, the plastic foam apparently dissolved upon contact with the liquid but had not dissolved with contact with water during prior attempts at irrigation. The residue from the plastic foam was then irrigated out after inspection of the tympanic membrane. Neither patient had any complications during the procedure or at follow up; there were no complaints of burning or pain on instillation of the chemicals. The ototoxic effects of these chemicals are unknown. In cases of tympanic membrane perforation, this technique would not be advisable because the effects of the chemicals on the middle ear structures are unknown.
Bugs in the Ear. Cockroaches are relatively common ear foreign bodies.2,17,18 The generally accepted approach is to kill the insect with mineral oil, microscope immersion oil, or lidocaine18 and then remove the insect with either forceps or irrigation.17,18 The choice of fluid to instill to kill the insect is debated. Lidocaine is readily available in the ED, effective in most cases, and well tolerated by most patients. Interestingly, in three cases in the literature, lidocaine irrigation made the cockroaches crawl rapidly out of the ear canal on their own.18 Care must be taken to avoid instilling these solutions into the canal if the tympanic membrane is perforated, as lidocaine in the middle ear has been described as a cause of vertigo.34 Every effort should be made to assure that all of the bug parts are removed. Cockroaches in particular tend to pull apart easily, and any of the barbed legs left as a retained foreign body will be expected to induce delayed inflammation.17
Suction. Suction may be an effective technique for removing some foreign bodies. The small Frazier suction catheters may work, but also may push the object further into the ear canal.17 One author recommends using the Schuknecht foreign body suction catheter for round, smooth foreign bodies.17 This catheter may not be available in some hospitals.
General Comments About Nose and Ear Foreign Bodies
Nose and ear foreign bodies are relatively common in the ED. The emergency physician should expect removal of most objects without consultation2 and, therefore, should have familiarity with and gain experience in multiple techniques. Interestingly, there is very little information regarding the use of procedural sedation (e.g., ketamine) for the removal of pediatric nose and ear foreign bodies.28 The use of procedural sedation is becoming common in most EDs, and emergency physicians should be familiar with multiple pharmacological strategies (in addition to physical restraint, which still has a primary role in many quick procedures) for sedating young children for procedures such as foreign body removal.35 If the emergency physician is unsuccessful in removing a foreign body, many of these objects can be left in place for an office referral the next morning if the family is deemed reliable. One notable exception is the disc battery, which can cause extensive damage. Disc batteries should be removed promptly, and urgent consultation is appropriate if needed. Once a foreign body has been identified, it has been recommended that both ears and both nasal passages be examined for other foreign bodies.17
Gastrointestinal (Swallowed) Foreign Bodies: Identification and Management
In addition to foreign bodies in the nose and ears, children also may swallow nonfood material. Often, this injestion (e.g., eating some sand or dirt on the playground) causes no harm and does not prompt a physician visit. Rarely, the results can be deadly.36-38 The number of actual foreign body ingestions is unknown. One source of data is from the poison control centers. In 2000, there were 77,763 foreign body ingestions in children younger than 6 years reported to regional poison control centers in the United States.39 The initial clinical presentation of foreign body ingestion can range from asymptomatic to severe distress.40 (See Figure 1.) The literature in this area can be divided into a few areas of study: descriptive studies of fairly large numbers of ingestion cases,36-38,40,41 studies primarily or exclusively about coin ingestions,42-53 and studies about disc batteries.54-58
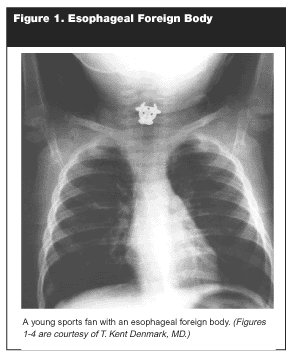 |
Large Case Series. There are many case reports in the literature on isolated cases.59-61 For example, a 9-year-old boy ingested pheasant that had been shot with a shotgun. A few days later he was diagnosed with appendicitis. The lumen of the appendix was found to be obstructed with bird shot.59 Although there is some degree of amazement over cases like this, they are not particularly instructive in understanding and developing an approach to the diagnosis and management of gastrointestinal foreign bodies. More instructive are large series used to formulate medical decision making regarding gastrointestinal foreign bodies.
One interesting paper from the late 1960s looked at 1250 cases of sub-diaphragmatic foreign bodies (objects that had traversed the esophagus) in children.41 This series encompassed cases from 1949-1965 and included foreign bodies such as bib fastenings and safety pins. Of these 1250 foreign bodies, 1234 (98.7%) passed spontaneously with only two of these children described as having a "slight admixture of blood to the bowel movements."
A more contemporary study from Hong Kong reported on 1265 cases of foreign body ingestions including those noted to be in the esophagus.38 The age range of these patients was from 7 months to 16 years with a mean age of 5.2 years. Of those, 552 cases of proven foreign bodies (verified either radiographically or endoscopically), 271 (49%) were coins, 155 (29%) were fish bones, 78 (13%) were metallic objects (including seven batteries, 41 sharp objects like needles and screws, and 30 blunt objects such as keys and metal caps), 16 (3%) were other bones (chicken, pork, and duck), 10 (1.6%) were rubber or plastic, and 22 other objects including glass marbles, shrimp and crab shells, and a seed. In this study, there was a single death due to systemic sepsis in an 8-year-old developmentally delayed child who presented five days after a piece of chicken bone became lodged in the esophagus, which lead to an empyema and a fistula between the esophagus and left mainstem bronchus. In addition, there were three serious complications that included another developmentally delayed child who swallowed a toothpick that subsequently perforated her terminal ileum, a child who developed a neck abscess from a fish bone ingestion, and a 2-year-old with a previous ileostomy in whom a coin became impacted 5 cm proximal to the ileostomy. Therefore, this series reported a total of four serious complications (0.7% of 552), and three of these were in developmentally delayed school-aged children, and one was a child with an abnormal gastrointestinal tract.
The authors reported on those objects that spontaneously passed. Of coins, 10% of those identified at the level of the upper esophagus passed on their own, as did 15% of coins at the mid-esophagus, 36% of coins in the distal esophagus, and 82% of coins in the stomach. One hundred percent of coins in the intestines passed without incident (except in the case of the child with the ileostomy). Of 41 children who had radiographically proven sharp object ingestion (i.e., pins, needles, and screws), 10 underwent endoscopic removal from the esophagus or stomach, and 31 (76%) were discovered at the level of the stomach or bowel and passed without incident. All seven of the disc batteries passed without incident. Bones, when visualized, were discovered in the tonsils and larynx 95% of the time. One patient developed a retropharyngeal abscess that was drained; otherwise, the bones were removed without incident.
A second smaller series of 663 cases from South Africa found similar results.40 In this study, three patients required emergency airway management. Fewer than half of the children with dysphagia or vomiting and a history of foreign body ingestion had identifiable foreign bodies in the oropharynx or upper esophagus. Interestingly, about a quarter of the children with foreign bodies in the upper esophagus were asymptomatic. All 223 foreign bodies discovered below the esophagus passed without incident, including 11 alkaline disc batteries.
These large studies are instructive and offer the opportunity to make some general comments about ingested foreign bodies. Foreign bodies in the stomach or intestines should be expected to pass spontaneously about 99% of the time (even if the object is sharp) if the child has normal anatomy. Complications primarily arise from esophageal foreign bodies, and a substantial percentage of these foreign bodies do pass on their own. The higher the object is in the esophagus, the less likely it is to pass spontaneously. Children with a history of foreign body ingestion and apparent symptoms may have no identifiable foreign body. Similarly, children with esophageal foreign bodies that necessitate removal may be asymptomatic. Finally, the ED physician should be wary of developmentally delayed children who may present in an atypical fashion and have more complications.
Coins. The identification and management of ingested coins provokes controversy among specialties, sparking a debate on the primary care approach vs. an ED approach.42,62
The ED approach has been developed from several studies involving ED patients.43,44,46,48,63 Given that nearly all coins pass through the gastrointestinal tract once they successfully traverse the esophagus, the majority of the literature focuses on esophageal coins. In one retrospective chart review of 73 children with esophageal coins identified in the ED, all of the 58 children with proximal or middle esophageal coins underwent removal procedures. Of the 15 children with distal esophageal coins, nine had their coins pass spontaneously into the stomach.43 Five of these 73 children were asymptomatic at presentation. Prolonged retention of the foreign body appeared to lead to minor esophageal ulceration, erosion, or local swelling in the seven children who underwent endoscopy more than 64 hours after the ingestion.43 These authors recommended that all children who have swallowed coins have radiographs taken, even if they are asymptomatic, to facilitate early identification of esophageal coins and avert potential complications.
In another study, 30 cases of children who had esophageal coins identified on x-rays were studied prospectively.46 Nine of the 30 patients were asymptomatic. In yet another study of 25 patients with esophageal coins, 11 were asymptomatic at the time of presentation.63 In both of these papers, the authors recommended that all children suspected of swallowing a coin undergo radiography to facilitate the early identification of esophageal coins, which may be present in asymptomatic patients.
The spontaneous passage of esophageal coins in children also has been studied. In a retrospective study of 116 esophageal coins, 22% of proximal, 33% of middle, and 37% of distal esophageal coins passed spontaneously within 24 hours.44 In other words, the majority of esophageal coins identified in an ED do not pass spontaneously.
From these studies, it was recommended that all children who are suspected of swallowing a coin undergo radiography; those with identified esophageal coins should undergo a procedure to remove the coin or assist the coin forward into the stomach. Observation for 12-24 hours also has been suggested for distal esophageal coins, as more than one-third of them may pass on their own.44
This recommendation was not well received by primary care physicians, who had been following these cases at home without x-rays or interventions.62 Studies of primary care physician practices and surveys of families at home revealed that perhaps as many as 85% of coin ingestions are managed by families without ever involving the poison control center or a physician.45 It was recognized that those patients presenting to an ED are a selected group (either self-selected or physician selected in transfer) and would be expected to have greater severity of symptoms and a higher frequency of complications.42
Because subdiaphragmatic coins almost always pass without incident, one technique that has been studied to localize metallic foreign bodies is the use of handheld metal detectors.53,64,65 If the coin can be localized in the abdomen, expectant observation would be all that is required. These handheld metal detectors have a reported sensitivity of 96-100% in the hands of emergency physicians. The readily available x-ray suite, ease of getting an x-ray (even in an uncooperative child), and the additional information obtained (i.e., presence of more than one foreign body, presence of long, sharp objects initially thought to be coins, more exact location, the absence of any metallic foreign body, etc.) from an x-ray may explain why handheld metal detectors aren’t more widely applied in the ED.
The management of esophageal coins has been studied. In a well designed, prospective, double-blind, placebo-controlled trial, glucagon was found to be ineffective.49 Unless future pharmacologic therapy for esophageal dilation/relaxation is developed, mechanical means of either removing or pushing the coin into the stomach are the available treatments. The current techniques include bougienage, endoscopy, and use of a Foley catheter to remove the object.51,52,66 Although there is a single study of 31 children who underwent esophageal bougienage performed by emergency physicians,50 this typically is referred to an institutionally specific consultant (e.g., pediatric gastrointestinal specialist, otolaryngologist, pediatric surgeon, or interventional radiologist). The use of a Foley catheter balloon under fluoroscopic control also has been studied.67 The authors reviewed their seven-year experience with 276 esophageal foreign bodies. The authors selected smooth radiopague esophageal foreign bodies for the study. One hundred seventy-three children underwent attempted balloon extraction, and 146 were accomplished successfully. Fifteen remained lodged in the esophagus and were removed by endoscopy, and 12 passed into the stomach and were managed conservatively. The only complication was epistaxis in a single patient. The authors recommend the balloon extraction technique as a safe and effective alternative to endoscopy for the removal of selected esophageal foreign bodies. A literature-based cost analysis for removal techniques for esophageal coin removal comparing endoscopic removal, Foley catheter removal, and bougienage removal was conducted.68 The removal of esophageal coins by Foley catheter ($660) or bougienage ($614) was significantly less expensive than the use of endoscopy ($2701).
Disc Batteries. There are two case reports of battery ingestions in the literature that are quite concerning. Both children had relatively large, flat, disc-type batteries lodged in the esophagus. They were symptomatic for several days prior to seeking medical attention. One child died from exanguination after an esophageal-aortic fistula developed, and the other died from massive hematemesis from a tracheo-esophageal fistula.69,70 From these early catastrophic cases, an interest in battery ingestions led to a small body of literature on the topic.
Of this literature, Litovitz and Schmitz reported on the largest numbers of cases. In three separate articles covering cases from 1978 to 1990 and published between 1983 and 1992, a total of 2552 cases of battery ingestions were reported in the literature.54,57,69 More than 80% of the patients were asymptomatic. There were only two deaths, and these were the same two cases that are mentioned above and were previously reported in the literature.69,70 Only 22 of 2383 (0.9%) of the ingestions involved batteries lodged in the esophagus. In seven of these cases, the battery spontaneously passed into the stomach. Esophageal erosions were noted on one patient who underwent endoscopy just four hours after ingestion. All of the 48 patients with subdiaphragmatic batteries and complications were symptomatic, including bloody or melanotic stools, vomiting, and/or abdominal pain. One 2-and-a-half-year-old had a disc battery lodged in a Meckel’s diverticulum, which led to bowel perforation. Gastrointestinal bleeding was more common when the battery split open in the gastrointestinal tract.
Recommendations for the management of disc battery ingestions mirror those for coin ingestions. All children in the ED suspected of ingesting batteries should undergo x-ray. If the disc battery is seen in the esophagus, arrange emergent removal by the appropriate local endoscopist. Asymptomatic children with subdiaphragmatic intact batteries should be observed at home, as they would be expected to pass the battery without difficulty. Symptomatic children with subdiaphragmatic batteries should have an appropriate surgical consultation to discuss surgical removal of the battery, especially if the battery has split open or is not progressing along the gastrointestinal tract on sequential x-rays. Bowel perforation and other clear indications for laparotomy require surgery as they would in other circumstances.
Aspirated Foreign Bodies: Identification
The identification of a patient with an aspirated foreign body can be quite subtle. Foreign body aspiration is a relatively uncommon event and large, pediatric tertiary-care referral centers can expect to see between three and 29 cases per year.72-77 There are several articles in the literature that retrospectively describe years (if not decades) of experience with aspirated foreign bodies by various institutions.72-77 (See Table 1.)
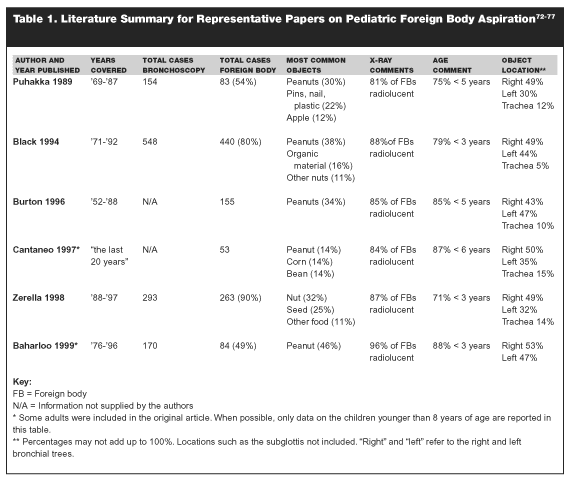 |
Signs and symptoms associated with aspirated foreign bodies include choking (reportedly seen 22-86% of the time), coughing (22-77%), dyspnea or breathlessness (4-49%), fever (12-37%), and wheezing (22-40%).72,74-77 Stridor was reported in 1% of patients in one study72 and 61% of patients in another study.72 Hemoptysis uncommonly was seen (1-11%).74,75 Patients were asymptomatic 1-6% of the time.72-75 These signs and symptoms are insensitive and not specific. One study reported on the symptomatology of patients with a negative bronchoscopy for foreign body.76 Eighteen percent had a choking episode, 64% were wheezing on examination, 29% had severe coughing, and 29% had acute dyspnea.
From these studies, several generalizations can be made. (See Table 1.) As with other foreign bodies, young children are at the greatest risk. Most aspirated foreign bodies are radiolucent (i.e., don’t show up on x-rays). Peanuts consistently are shown to be the most common objects aspirated. It is only slightly more common for foreign bodies to end up in the right bronchial tree compared to the left. (See Figures 2A and 2B.)
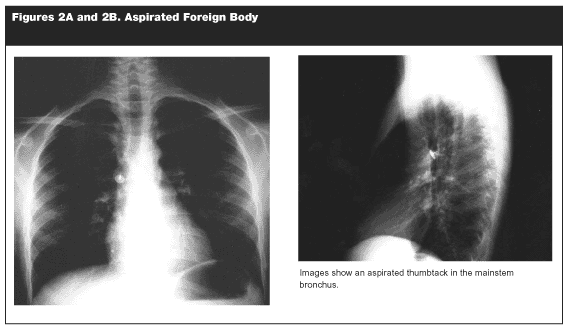 |
The use of inspiratory/expiratory x-rays and lateral decubitus films for the identification of aspirated foreign bodies, although traditionally and historically used to identify aspirated foreign bodies, has little literature support. The most common x-ray findings reported are hyperinflation/airtrapping (that would be expected to be made more prominent by inspiratory/expiratory or decubitus films), atelectasis, and pneumonia.73-77 Some work has been done using magnetic resonance imaging (MRI) to identify peanuts in the airways, but this has not been widely studied or accepted, perhaps due to sedation concerns for this relatively lengthy procedure.78
Aspirated Foreign Bodies: Management
In cases of suspected aspirated foreign bodies, the diagnostic and therapeutic technique of choice is bronchoscopy. This typically is performed by a pediatric surgeon, pediatric otolaryngologist, or pediatric pulmonologist. Unsuccessful bronchoscopy typically indicates the need for thoracotomy to remove the object and prevent long-term complications including foreign body migration into vital structures, hemorrhage, and persistent or recurrent pneumonia.
Rarely, a child will have partial airway obstruction that will progress to complete airway obstruction either en route to or in the ED. All emergency physicians should have training in age-specific foreign body expulsion (as usually taught in a basic life support course) and in the use of Magill forceps and alternative airway maneuvers (such as needle jet ventilation) for these rare events.79 Partial airway obstruction or persistent severe coughing should not be treated with chest percussion or external blows to remove the foreign body (i.e., back blows or abdominal thrusts) as the foreign body may move more proximal in the airway. This may result in complete airway obstruction and death.
Genitourinary Foreign Bodies
Recent literature on pediatric vaginal foreign bodies is almost nonexistent. One review article from the mid-1980s reviewed literature going back as far as 1939.80 Several general comments can be made based on this decades-old literature. Persistent vaginal discharge or bleeding in a prepubertal girl should prompt an evaluation for vaginal foreign body (usually in the operating room under general anesthesia using vaginoscopy). Although a variety of objects have been described (including coins, safety pins, hair pins, fruit pits, small toys, and pen tops) wads of toilet paper probably are the most common. (See Figure 3.)
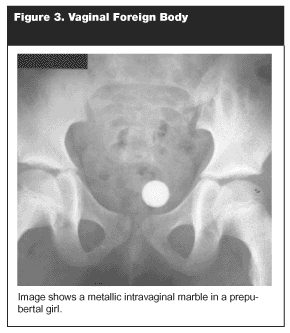 |
One more recent article reported on 12 girls ages 10 years and younger who presented to a clinic with vaginal complaints and ultimately were determined to have vaginal foreign bodies.79 This facility had a protocol whereby all of these girls were seen by a child protection team. Two of the girls had concurrent sexually transmitted diseases, and eight met diagnostic criteria for confirmed sexual abuse. If these findings are generalizable, sexual abuse should be considered in cases of vaginal foreign bodies.
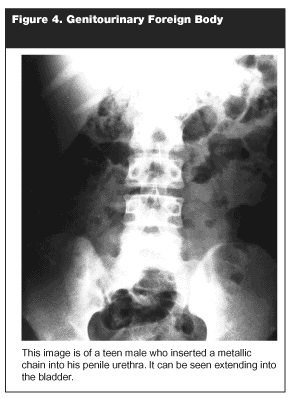
No literature on male genitourinary foreign bodies was found. A single case at our own institution of a teen male who put a chain into his urethra and required a laparotomy for removal is presented (See Figure 4.).
 |
Rectal Foreign Bodies
The literature identifies two pediatric groups at risk for rectal foreign bodies. Young children may be at risk for broken or retained glass rectal thermometers, and older teenagers may be at risk during sexual exploration.
Although used less frequently now, 20 years ago a report of 16 young children with broken or retained glass rectal thermometers identified during a 10-year time period was published.82 None of these children had congenital anomalies. Eleven infants passed the broken thermometer pieces spontaneously. The others had the thermometer removed manually, and all did well on follow up.
Older teens, just like adults, participate in sexual exploration and behavior. A long list of objects has been described as identified retained rectal foreign bodies in the literature.83,84 Common objects include dildos, vibrators, fruits, vegetables, and bottles or jars.83,84 In the mid-1980s a review of the world’s literature on rectal foreign bodies showed only two cases in children younger than 10 years.84 Three percent of 182 cases were deemed to be from assault, and fewer than 1% were from smuggling. The possibility of drug smuggling or body packing in addition to sexual assault would be expected in a small minority of cases. Removal of these rectal objects under procedural sedation in the ED has been described.85 Physicians unfamiliar with this procedure should defer to their surgical consultant for removal.
Conclusions
Emergency physicians should expect to see foreign bodies in their clinical practice. Knowledge and experience with a variety of techniques for the removal of nose and ear foreign bodies (including the use of procedural sedation when needed) should be a part of all emergency physicians’ practices. Familiarity with the identification and management of ingested and aspirated foreign bodies can minimize the risk of potentially serious but uncommon complications. Familiarity with the issues regarding genitourinary and rectal foreign bodies keeps these uncommon problems in mind to avoid missing these diagnoses.
References
1. Kadish HA, Corneli HM. Removal of nasal foreign bodies in the pediatric population. Am J Emerg Med 1997;15:54-56.
2. Baker MD. Foreign bodies of the ears and nose in childhood. Pediatr Emerg Care 1987;3:67-70.
3. Waters TA, Peacock WF. Nasal emergencies and sinusitis. In: Tintinalli JE, et al, eds. Emergency Medicine—A Comprehensive Study Guide. 5th ed. New York: McGraw Hill; 2000:1532-1539.
4. Cohen HA, Goldberg E, Horev Z. Removal of nasal foreign bodies in children [letter]. Clin Pediatr 1993;32:192.
5. Meadoff TM. Nasal foreign body removal [letter; comment]. Ann Emerg Med 1995;26:390.
6. Botma M, Bader R, Kubba H. A parent’s kiss’: Evaluating an unusual method for removing nasal foreign bodies in children. J Laryngol Otol 2000;114:598-600.
7. Lichenstein R, Giudice EL. Nasal wash technique for nasal foreign body removal. Pediatr Emerg Care 2000;16:59-60.
8. Finkelstein JA. Oral ambu-bag insufflation to remove unilateral nasal foreign bodies. Am J Emerg Med 1996;14:57-58.
9. Hanson RM, Stephens M. Cyanoacrylate-assisted foreign body removal from the ear and nose in children. J Paediatr Child Health 1994;30:77-78.
10. Kalan A, Tariq M. Foreign bodies in the nasal cavities: A comprehensive review of the aetiology, diagnostic pointers, and therapeutic measures. Postgrad Med J 2000;76:484-487.
11. Backlin SA. Positive-pressure technique for nasal foreign body removal in children. Ann Emerg Med 1995;25:554-555.
12. Manca D. Up your nose. Quick and somewhat dirty method of removing foreign bodies from children’s noses. Can Fam Physician 1997;43:223.
13. Handler SD. Nasal wash technique for nasal foreign body removal. Pediatr Emerg Care 2000;16:307.
14. Nandapalan V, McIlwain JC. Removal of nasal foreign bodies with a Fogarty biliary balloon catheter. J Laryngol Otol 1994;108:758-760.
15. Henry L, Chamberlain J. Removal of foreign bodies from esophagus and noses with the use of a Foley catheter. Surgery 1972;71:918-921.
16. D’Cruz O, Lakshman R. A solution for the foreign body in nose problem [letter]. Pediatrics 1988;81:174.
17. Ansley JF, Cunningham MJ. Treatment of aural foreign bodies in children. Pediatrics 1998;101:638-641.
18. Bressler K, Shelton C. Ear foreign-body removal: A review of 98 consecutive cases. Laryngoscope 1993;103:367-370.
19. Bhisitkul DM, Dunham M. An unsuspecting alkaline battery foreign body presenting as malignant otitis externa. Pediatr Emerg Care 1992;8:141-142.
20. Premachandra DJ, McRae D. Severe tissue destruction in the ear canal by alkaline button batteries. Postgrad Med J 1990;66:52-53.
21. McRae D, Premachandra DJ, Gatland DJ. Button batteries in the ear, nose and cervical esophagus: A destructive foreign body. J Otolaryngol 1989;18: 317-319.
22. Capo JM, Lucente FE. Alkaline battery foreign bodies in the ear and nose. Arch Otolaryngol Head Neck Surg 1986;112:562-563.
23. Kavanagh KT, Litovitz T. Miniature battery foreign bodies in auditory and nasal cavities. JAMA 1986;255:1470-1472.
24. Skinner DW, Chui P. The hazards of button-sized’ batteries as foreign bodies in the nose and ear. J Laryngol Otol 1986;100:1315-1318.
25. Rachlin LS. Assault with battery. N Engl J Med 1984;311:921-922.
26. Lossos I, Brever R. A rare case of hiccups. N Engl J Med 1988;318:711-712.
27. Wagner MS, Stapczynski JS. Persistent hiccups. Ann Emerg Med 1982;11: 24-26.
28. Mishra A, Shukla GK, Bhatia N. Aural foreign bodies. Indian J Pediatr 2000;67:267-269.
29. Balbani AP, Sanchez TG, Butugan O, et al. Ear and nose foreign body removal in children. Int J Pediatr Otorhinolaryngol 1998;46:37-42.
30. O’Donovan C. Crazy glue and foreign bodies [letter; comment]. Pediatrics 1999;103:857-858.
31. Brunskill AJ, Satterwaite K. Foreign bodies [letter]. Ann Emerg Med 1994;24:757.
32. White SJ, Brover S. The use of acetone to dissolve a Styrofoam impaction of the ear. Ann Emerg Med 1994;23:580-582.
33. Jones I, Moulton C. Use of an electric ear syringe in the emergency department. J Accid Emerg Med 1998;15:327-328.
34. Simmons FB, Glattke TJ, Downie DB. Lidocaine in the middle ear: A unique cause of vertigo. Arch Otolyngol 1973;98:42-43.
35. Krauss B. Management of acute pain and anxiety in children undergoing procedures in the emergency department. Pediatr Emerg Care 2001;17:115-122.
36. Loh KS, Tan LK, Smith JD, et al. Complications of foreign bodies in the esophagus. Otolaryngol Head Neck Surg 2000;123:613-616.
37. Byard RW. Mechanisms of unexpected death in infants and young children following foreign body ingestion. J Forensic Sci 1996;41:438-441.
38. Cheng W, Tam PK. Foreign-body ingestion in children: Experience with 1,265 cases. J Pediatr Surg 1999;34:1472-1476.
39. Litovitz TL, Klein-Schwartz W, White S, et al. 2000 Annual Report of the American Association of Poison Control Centers Toxic Exposure Surveillance System. Am J Emerg Med 2001;19:337-395.
40. Panieri E, Bass DH. The management of ingested foreign bodies in children a review of 663 cases. Eur J Emerg Med 1995;2:83-87.
41. Pellerin D, Fortier-Beaulieu M, Gueguen J. The fate of swallowed foreign bodies: Experience of 1250 instances of sub-diaphragmatic foreign bodies in children. Progr Pediatr Radiol 1969;2:286-302.
42. Paul RI, Christoffel KK, Binns HJ, et al. Foreign body ingestions in children: Risk of complication varies with site of initial health care contact. Pediatrics 1993;91:121-127.
43. Conners GP, Chamberlain JM, Ochsenschlager DW. Symptoms and spontaneous passage of esophageal coins. Arch Pediatr Adolesc Med 1995;149: 36-39.
44. Soprano JV, Fleisher GR, Mandl KD. The spontaneous passage of esophageal coins in children. Arch Pediatr Adolesc Med 1999;153:1073-1076.
45. Conners GP, Chamberlain JM, Weiner PR. Pediatric coin ingestion: A home-based survey. Am J Emerg Med 1995;13:638-640.
46. Schunk JE, Corneli H, Bolte R. Pediatric coin ingestions: A prospective study of coin location and symptoms. AJDC 1989;143:546-548.
47. Caravati EM, Bennett DL, McElwee NE. Pediatric coin ingestion: A prospective study on the utility of routine roentgenograms. AJDC 1989;143:549-551.
48. Smith SA, Conners GP. Unexpected second foreign bodies in pediatric esophageal coin ingestions. Pediatr Emerg Care 1998;14:261-262.
49. Mehta D, Attia M, Quintana E, et al. Glucagon use for esophageal coin dislodgment in children: A prospective, double-blind, placebo controlled trial. Acad Emerg Med 2001;8:200-203.
50. Emslander HC, Bonadio W, Klatzo M. Efficacy of esophageal bougienage by emergency physicians in pediatric coin ingestions. Ann Emerg Med 1996;27: 726-729.
51. Conners GP. A literature-based comparison of three methods of pediatric esophageal coin removal. Pediatr Emerg Care 1997;13:154-157.
52. Calkins CM, Christians KK, Sell LL. Cost analysis in the management of esophageal coins: Endoscopy versus bougienage. J Pediatr Surg 1999;34: 412-414.
53. Bassett KE, Schunk JE, Logan L. Localizing ingested coins with a metal detector. Am J Emerg Med 1999;17:338-341.
54. Litovitz T, Schmitz BF. Ingestion of cylindrical and button batteries: An analysis of 2382 cases. Pediatrics 1992;89:747-757.
55. Ali LSM, Ramzi H. Button battery ingestion: Hazards of esophageal impaction. J Pediatr Surg 1999;34:1527-1531.
56. Votteler TP, Nash JC, Rutledge JC. The hazards of ingested alkaline disk batteries in children. JAMA 1983;249:2504-2506.
57. Litovitz TL. Button battery ingestions: A review of 56 cases. JAMA 1983;249; 2495-2500.
58. Kulig K, Rumack CM, Rumack BH, et al. Disk battery ingestion: Elevated urine mercury levels and enema removal of battery fragments. JAMA 1983; 249;2502-2504.
59. Larsen AR, Blanton RH. Appendicitis due to bird shot ingestion: A case study. Am Surg 2000;66:589-591.
60. Goh YH, Balakrishnan A. An unusual neck lump. J Pediatr Surg 2000;35: 1132-1133.
61. Stricker T, Kellenberger CJ, Neuhaus TJ, et al. Ingested pins causing perforation. Arch Dis Child 2001;84:165-166.
62. Joseph PR. Management of coin ingestion. AJDC 1990;144:449-450. [letter and reply].
63. Hodge D, Tecklenburg F, Fleisher G. Coin ingestion: Does every child need a radiograph. Ann Emerg Med 1985;14:443-446.
64. Seikel K, Primm PA, Elizondo BJ, et al. Handheld metal detector localization of ingested metallic foreign bodies: Accurate in any hands? Arch Pediatr Adolesc Med 1999;153;853-857.
65. Gooden EA, Forte V, Papsis B. Use of a commercially available metal detector for the localization of metallic foreign body ingestion in children. J Otolaryngol 2000;29:218-220.
66. Soprano JV, Mandl KD. Four strategies for the management of esophageal coins in children. Pediatrics 2000;105(1): e5.
67. Morrow SE, Bickler SW, Kennedy AP, et al. Balloon extraction of esophageal foreign bodies in children. J Pediatr Surg 1998 33(2):266-270.
68. Conners GP. A literature based comparison of three methods of pediatric esophageal coin removal. Pediatr Emerg Care 1997 13(2):154-157.
69. Shabino CL, Feinberg AN. Esophageal perforation secondary to alkaline battery ingestion. JACEP 1979;8:360-362.
70. Blatnik DS, Toohill RJ, Lehman RH. Fatal complications from alkaline battery foreign body in the esophagus. Ann Otol 1977;86:611-615.
71. Litovitz TL. Battery ingestions: Product accessibility and clinical course. Pediatrics 1985;75:469-476.
72. Puhakka H, Svedstrom E, Kero P, et al. Tracheobronchial foreign bodies. AJDC 1989;143:543-545.
73. Black RE, Johnson DG, Matlak, ME. Bronchoscopic removal of aspirated foreign bodies in children. J Pediatr Surg 1994;29:682-684.
74. Burton EM, Brick WG, Hall JD, et al. Tracheobronchial foreign body aspiration in children. South Med J 1996;89:195-197.
75. Cataneo AJM, Reibscheid SM, Ruiz RL, et al. Foreign body in the tracheobronchial tree. Clin Pediatr 1997;36:701-706.
76. Zarella JT, Dimler MD, McGill LC, et al. Foreign body aspiration in children: Value of radiography and complications of bronchoscopy. J Pediatr Surg 1998;33:1651-1654.
77. Baharloo F, Veyckemans F, Francis C, et al. Tracheobronchial foreign bodies: Presentation and management in children and adults. Chest 1999;115: 1357-1362.
78. Imaizumi H, Kaneko M, Nara S, et al. Definitive diagnosis and location of peanuts in the airways using magnetic resonance imaging techniques. Ann Emerg Med 1994;23:1379-1382.
79. Quinones FR, Saez MM, Serrano EMP, et al. Magill forceps: A vital forceps. Pediatr Emerg Care 1995;11:302-303.
80. Sanfilippo JS, Wakim NG. Bleeding and vulvovaginitis in the pediatric age group. Clin Obstet Gynecol 1987;30:653-661.
81. Herman-Giddens ME. Vaginal foreign bodies and child sexual abuse. Arch Pediatr Adolesc Med 1994;148:195-200.
82. Lau JTK, Ong GB. Broken and retained rectal thermometers in infants and young children. Aust Paediatr J 1981;17:93-94.
83. Yaman M, Deitel M, Burul CJ, et al. Foreign bodies in the rectum. Can J Surg 1993;36:173-177.
84. Busch DB, Starling JR. Rectal foreign bodies: Case reports and a comprehensive review of the world’s literature. Surgery 1986;100:512-519.
85. Wigle RL. Emergency department management of retained rectal foreign bodies. Am J Emerg Med 1988;6:385-389.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
