Chronic Fatigue and Vasovagal Faints: Overlapping Syndromes?
Chronic Fatigue and Vasovagal Faints: Overlapping Syndromes?
Abstract & Commentary
Synopsis: CFS patients who have undiagnosed syncope should be investigated for vasovagal syncope, and the 2 disorders may share a common mechanism.
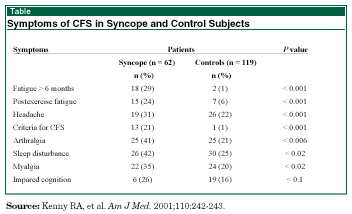
Source: Kenny RA, et al. Am J Med. 2001;110:242-243.
Chronic fatigue syndrome (cfs) is characterized by unexplained disabling fatigue. Lightheadedness or syncope reportedly occur in 40-90% of CFS patients, which suggests an overlap of these 2 syndromes.1
Kenny and colleagues determined the prevalence of CFS symptoms2 in consecutive patients with a primary diagnosis of vasovagal syncope confirmed by positive head-up tilt table testing. Patients with at least 2 syncopal episodes in the previous year without a cardiac cause for syncope and who did not have a diagnosis of CFS were studied. Study patients and age- and sex-matched controls completed a questionnaire for CFS symptoms.
Questionnaires completed by 62 syncope patients (63% women, mean age ± SD = 50 ± 21 years; range 16-83 years) were compared to questionnaires of 119 controls. The symptom criteria for CFS were fulfilled in 13 (21%) of patients but in only 1 control (see Table). Twelve of the 13 (92%) patients with CFS were women compared with 13 of the 49 (55%) patients without CFS.
 |
Kenny et al recommend that CFS patients who have undiagnosed syncope should be investigated for vasovagal syncope and suggest that the 2 disorders may share a common mechanism.
Comment by John J. Caronna, MD
Most people have fainted once or seen someone faint. The Framingham Study3 recorded information on fainting. In the entire 26 years of surveillance of more than 5000 subjects, at least 1 syncopal episode was reported by 3% of the men and 3.5% of the women. More than 75% of the subjects had only a single faint. Isolated syncope in the absence of overt neurological and cardiovascular disease was not associated with increased morbidity or mortality and was not a frequent indicator of undiagnosed cerebrovascular disease.
Recurrent vasovagal syncope, in contrast, is a clinical problem that often is unresponsive to treatment, but symptoms may be improved by the use of selective serotonin reuptake inhibitors (SSRIs).Therefore, recurrent fainting resembles CFS. Like CFS, recurrent syncope also can be a disabling disorder, and quality of life deteriorates as a function of the recurrence of episodes. Syncopal episodes not only can produce physical trauma but also can create serious psychological discomfort. Employment, education, and social interactions may be severely restricted. SSRIs can improve clinical outcome in patients with refractory syncope (ie, those who are unresponsive to beta-blocking, vagolytic, negative inotropic, and mineralocorticoid therapy). Perhaps this is because SSRIs cause postsynaptic serotonin receptors to down-regulate in the brainstem, thereby blunting the brain response to rapid shifts in cerebral serotonin levels.5
The causes of recurrent syncope are legion.6 Clinicians should add CFS to the list.
Dr. Caronna is Vice-Chairman, Department of Neurology, Cornell University Medical Center, Professor of Clinical Neurology, New York Presbyterian Hospital, New York, NY.
References
1. Bou-Holaigah I, et al. JAMA. 1995;274:961-967.
2. Fukuda K, et al. Ann Intern Med. 1994;121:953-959.
3. Savage DD, et al. Stroke. 1985;16:626-629.
4. DiGirolamo E, et al. J Am Coll Cardiol. 1999;33:
1227-1230.
5. Grubb BP, et al. J Am Coll Cardiol. 1994;24:490-494.
6. Ross TR. Syncope. In: Walton, ed. Major Problems in Neurology. London, England: WB Saunders; 1988.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
