2001 Salary Survey Results: Nursing shortage may work in your favor for salary boost
2001 Salary Survey Results
Nursing shortage may work in your favor for salary boost
In tight times, EHPs still need to prove their worth
Employee health professionals (EHPs) may be benefiting from efforts to retain experienced nurses, as they reported somewhat higher salary increases this year in the exclusive 2001 Hospital Employee Health survey. But continuing financial concerns at hospitals make it imperative for EHPs to demonstrate the value of their work in reduced injury rates, medical claims, absenteeism, and enhanced working conditions, employee health experts say.
"If you want to hold your own, you’ve got to communicate the value of what you bring to the organization," says Charlene M. Gliniecki, RN, MS, COHN-S, a former employee health manager who is now vice president of human resources at El Camino Hospital in Mountainview, CA. "Even though it’s obvious to us what we do and why we do it, people in the executive level don’t always see how all the pieces fit together unless we tell them."
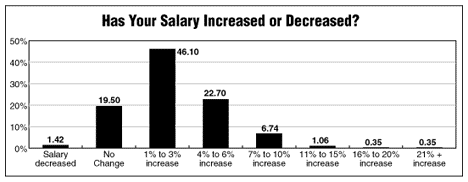
This year, 23% of EHPs responding to the survey said they received a 4% to 6% salary increase and 7% earned 7% to 10% more, while a total of only 24% reported raises in those higher levels last year. Still, most of those EHPs received modest raises in 2001; about half (46%) received a 1% to 3% raise. Almost 20% said they received no salary increase. However, some of them may receive an annual bonus or profit sharing.
 |
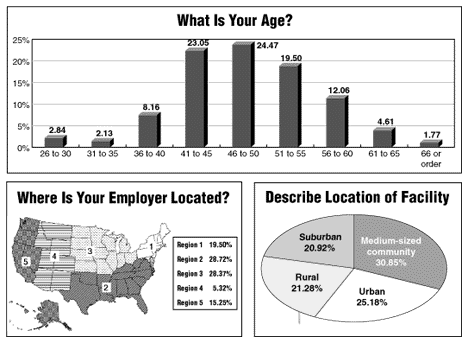
Salaries were highest in the Northeast and West Coast, reflecting the higher cost of living there. There were no substantial differences between for-profit and not-for-profit hospitals. Salary adjustments are becoming more commonplace as some hospitals seek to remain competitive with other facilities in their region.
For example, Sewickley (PA) Valley Hospital conducted an overall salary and wage evaluation. "There were people who got substantial raises," says MaryAnn Gruden, MSN, CRNP, NP-C, COHN-S/CM, employee health nurse practitioner. She also is executive president of the Association of Occupational Health Professionals in Healthcare (AOHP), based in Reston, VA. "We want to retain and recruit employees and we want to be competitive in the marketplace," she says. "Those salaries will be reviewed annually and adjustments will be made accordingly."
EH staffing still a problem
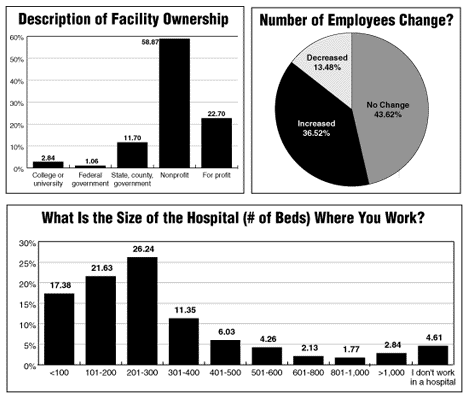
Unfortunately, most EHPs did not get something else they need in their work: increased staff. Almost half (44%) of the survey participants reported no change in staffing, while 13.5% saw a reduction. About a third (36.5%) said they added employees in their department in the past year.
"Most of the people I talk to are still struggling a lot with their staffing," says Gruden, noting that an AOHP survey showed concerns about inadequate staffing. "I’d be interested in learning more about that group that got the increases and what they did. Would they share their secrets with the rest of us?"
In fact, sometimes low staffing may go hand-in-hand with salary increases, notes Gliniecki. "This is a common practice when [companies] look at improving the productivity of the work force," she says. "You look at doing the work with less people, but you make a commitment to pay [those] people more."
 |
New regulations can raise the profile of employee health. In the first-ever sentinel event alert on worker safety, the Joint Commission on Accreditation of Healthcare Organizations in Oakbrook Terrace, IL, announced it would assess organizational compliance with needlestick prevention. (See "Joint Commission targets needle safety in surveys," in this issue.) Employee health is part of a broader team that works on needlesticks and other safety issues. EHPs will still need to demonstrate their value to that team, says Gliniecki. One way for EHPs to improve their visibility is by quantifying the value of their activities to administration, she says.
In a weak economy, EHPs have to make sure they remain key players in the hospital, explains Deborah V. DiBenedetto, MBA, RN, COHN-S/ CM, ABDA, a Yonkers, NY-based occupational health consultant and president of American Asso-ciation of Occupational Health Nurses (AAOHN) in Atlanta. "We’ve got to be aggressive and asser-tive and take command. That’s what we have to do in the marketplace today."
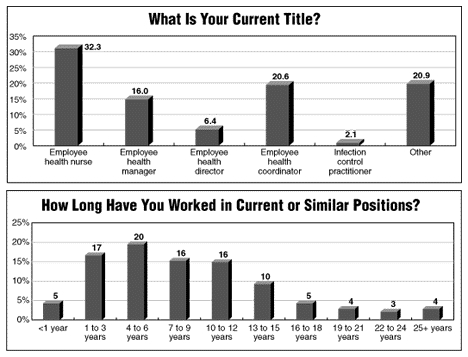
Most EHPs are seasoned professionals. In the HEH survey, 52% of respondents said they have worked in health care for 25 or more years. More than half have worked in their current position for 10 or more years.
 |
A major draw for those in employee health is flexibility. Two-thirds (68%) said flexible work schedules are extremely or very important to them. Just 13% said that benefit is not provided. Hospitals also are supporting nurses who want to further their education. Some 92% of respondents said they could receive tuition reimbursement. About 59% said that benefit is extremely or very important. At the same time, the growing cost of certain benefits may erode whatever gains EHPs make in salary. In the survey, 62% of EHPs said their contribution to the cost of medical benefits rose in the past 12 months.
For those who have been in their positions for 10 or more years and have developed a strong expertise in employee health, possibilities for career growth may not be readily apparent. Taking on additional duties, such as coordinating the hospital’s overall safety program or compliance with the Americans with Disabilities Act, may be a path for greater compensation, Gliniecki says.
Certification continues to be an important professional accomplishment, stresses Gruden. "I think certification is extremely important as a way to build your credibility in the organization and to stay current in all the issues that are impacting in employee health," she says.
Yet in the HEH survey, just 13.5% of EHPs reported having attained their COHN-S. Another 9% were certified in infection control. Even some business-oriented education can be helpful, DiBenedetto notes. Professional organizations such as the AAOHN provide workshops on demonstrating the value of employee health activities. Some EHPs are adding revenue to the hospital by providing their services to outside customers, she explains.
EHPs contribute to the hospital’s bottom line just by keeping staff healthy or getting them back to work. For example, a return-to-work program that matches employees to appropriate assignments may save money by reducing lost workdays, she says. EHPs also may be able to show how accident reviews or hazard evaluations led to a reduction in injuries.
If they need benchmarking data, EHPs can use information from the National Surveillance System for Healthcare Workers (NaSH) of the Centers for Disease Control and Prevention, the EPINet system run by the International Health Care Worker Safety Center at the University of Virginia in Charlottesville (www.med.virginia.edu/medcntr/centers/epinet/), or the Bureau of Labor Statistics (www.osha.gov/oshstats/work.html).
"Make sure people know what we do," Gliniecki advises. "Make sure to communicate the results. Make sure we can show how our contribution is tied into the main strategic plan or the objectives of the organization. It is absolutely essential that we run our departments almost like a business. We realize that we are accountable for the results and we are here to provide support to the organization, to solve problems for the organization."
 |
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
