Critical Path Network: Use algorithm to treat abdominal pain
Critical Path Network
Use algorithm to treat abdominal pain
When a 52-year-old woman came to the emergency department (ED) at University of California at Irvine (UCI) Medical Center in Orange with severe abdominal pain, nausea, and a low-grade fever, staff were able to use a new abdominal pain pathway to streamline her care.
"The ED and waiting area were completely full, but her labs were returned before she ever reached the treatment area for further care," reports Darlene Bradley, RN, MSN, MAOM, CCRN, CEN, director of emergency/trauma services.
Based on those results, the woman was quickly diagnosed with pyelonephritis. "She received her fluids, pain control, and antibiotics, and was discharged from the ED soon after," Bradley says.
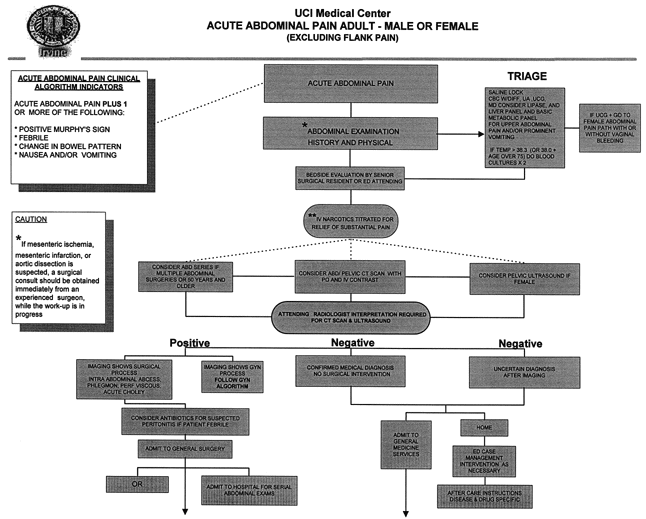
If the patient had remained in the waiting room, she would have experienced progressive illness and pain, Bradley says. "The pathway allowed her to receive treatment much earlier than she would have otherwise." (See algorithm for Acute Abdominal Pain Adult — Male or Female, below.)
Here are some of the benefits of using the abdominal pain algorithm:
1. Care is more consistent.
Nurses are given a quarterly report on the use of the algorithm, including cost per discharge, resource utilization, and clinical indicators, says Tania Bridgeman, PhD, RN, the hospital’s product line development manager. These data are used as a quality improvement tool for nursing, notes Bradley.
"The nurses enjoy hearing how many patients were identified in the abdominal pain program, how many had the pathway utilized, and what the outcomes of the usage were," she says.

Ensuring consistent care
The process ensures that care is consistent, says Bridgeman. "We look for patterns or trends in practice we need to address. If none are detected, we know that an established standard of care is being followed," she says.
Quarterly reports determine the level of compliance, says Bradley. "The reports also maintain the high level of interest necessary for new methods of managing health care delivery," she adds.
2. There is a collaborative approach between nursing and medicine.
Since the program was jointly developed, nurses and physicians have a mutual interest in the outcomes and the success of the program, says Bradley.
The pathway is a good learning tool, she notes. "Physicians and nurses develop an understanding of how to make a differential diagnosis, as well as the various indications for treatment," Bradley says.
The algorithm was developed using best-practice standards and evidence-based practice, particularly with prescribing practices, says Bradley.
"Physicians and nurses use the pathway to learn the value of order sets and the appropriate antibiotic orders and dosages for infectious diseases," she explains.
3. Length of stay is reduced.
With the pathway, patients receive treatment and evaluation procedures beginning at triage, says Bridgeman.
"If the patient cannot be moved immediately to the treatment area, at least the labs are already being processed so the physician can make a determination as to what’s going on with the patient," she explains.
Bridgeman adds that this process has cut the patient’s total length of stay from an average of 4.1 hours to 3.46 hours, a 16% decrease.
Because there is an associated physician order set, nurses can initiate the triage labs and tests as soon as the patient is admitted, Bridgeman points out. "They can remind physicians to utilize the order set."
The algorithm is enlarged and posted on the wall of the ED, she adds.
4. Costs are lower.
Bradley reports an average cost reduction of $100 per patient, an 11% average decrease in cost per case. The pathway ensures that antibiotics selected are low cost and that the labs and X-rays ordered are essential for the diagnosis of the patient, she explains.
"Without such a detailed pathway, providers often may order more labs or X-rays than is needed to make the diagnosis," she adds.
5. Return visits are reduced.
Bradley notes that the pathway includes a listing of antibiotics for primary pathogens: gram negatives, E. coli, Klebsiella, and anaerobes.
"Each drug has the associated costs per day, along with the preferred choices and alerts to renal problems and nosocomial infections," she says.
The goal is to prescribe the antibiotic that most likely would affect the infectious organism, she adds.
"Patients often return to the ED because their complaints or symptoms have not resolved. In some cases, this may be attributed to the ineffectiveness of the prescribed antibiotic," she says. "With the pathway, return visits are less likely to occur."
6. Patients express more satisfaction with their ED visit.
Earlier interventions are more satisfying to patients, says Bradley.
"The patient receives immediate education about the process and what will happen in their course of stay," she explains.
In the ED’s customer satisfaction survey, patients often express a positive opinion about the process, according to Bradley.
"Patients comment about the rapid intervention they received, such as the labs being done much earlier in the process than would have been expected," she says.
[For more information about the abdominal pain algorithm, contact:
Darlene Bradley, RN, MSN, MAOM, CCRN, CEN, Emergency/Trauma Services, UCI Medical Center, 101 The City Drive, Route 128, Orange, CA 92868-3298. Telephone: (714) 456-5248. Fax: (714) 456-5390. E-mail: [email protected].
Tania Bridgeman, PhD, RN, UCI Medical Center, Product Line Development, 200 S. Manchester, Suite 835, Route 163, Orange, CA 92868-3298. Telephone: (714) 456-3697. Fax: (714) 456-8968. E-mail: [email protected].]
Share your hospital’s pathway successes
Hospital Case Management welcomes guest columns about clinical path development and use.
Articles should include any results (length of stay, cost, or process improvements) that use of your pathway has helped achieve and should be from 800 to 1,200 words long.
Send your article submissions to:
Russ Underwood, Managing Editor, Hospital Case Management, P.O. Box 740056, Atlanta, GA 30374. Telephone: (404) 262-5460. Fax: (404) 262-5447.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
