The WHI and Cognition
The WHI and Cognition
Abstracts & Commentary
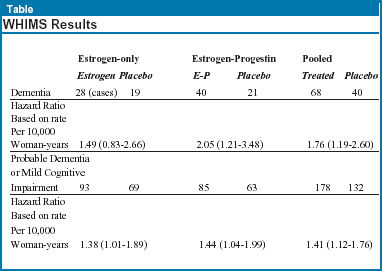
The women’s health initiative reported their results on cognition and dementia combining the canceled estrogen-only arm with the canceled estrogen-progestin arm of the randomized trial; the data are derived from an ancillary study of the trial entitled The Women’s Health Initiative Memory Study (WHIMS). It should be emphasized that the participants in WHIMS were 65-79 years old when they entered the study. In the estrogen-only arm of WHI, 2947 women, and in the estrogen-progestin arm, 4532 women were enrolled in WHIMS (see Table, below). The participants in both arms were pooled for analysis. Half the cases were classified as Alzheimer’s disease, the rest were mostly vascular dementia or mixed Alzheimer’s and vascular. In the estrogen-only arm, 1464 women in the treated group were available for analysis, 1483 in the placebo group; in the estrogen-progestin arm, there were 3693 women in the treated group and 3786 in the placebo group (Shumaker SA, et al. JAMA. 2004;291:2947-2958; Espeland MA, et al. JAMA. 2004;291:2959-2968).
Comment by Leon Speroff, MD
These results from the WHI do not differ substantially from the previous report a year ago when the WHI concluded that estrogen-progestin therapy increased the risk for probable dementia in women aged 65 years and older and did not prevent mild cognitive impairment.1,2 However, the only statistical significant finding in that report was increased dementia in elderly women (22 cases in the treated group and 10 cases in the placebo group) who were 75 and older and who had been exposed to a relatively short-term of estrogen-progestin therapy.
In the current report, the authors responsibly point out in their discussion that this study "may not represent primary prevention of Alzheimer’s disease."3 Will older women who have used hormone therapy for long durations early in their postmenopausal years be protected against dementia? The WHI recognized that this hypothesis could not be tested in this clinical trial because of the older age of the study participants. A prospective study of a homogeneous population in Utah (thus minimizing, if not eliminating, the healthy user bias) concluded that a reduction in the risk of Alzheimer’s required long-term treatment, initiated at least 10 years before symptoms of dementia appear.4 The favorable effects of hormone therapy on cognition and the risk of Alzheimer’s disease appear to be limited to women who initiate treatment close to their menopause.
Also worth noting in the current WHI report was an increase in dementia in the women with diabetes and hypertension in contrast to no increase in women without hypertension and without a history of diabetes. This emphasizes that the negative effects reported were concentrated in older women with pre-existing disease. Unfortunately, an analysis by age groups was not provided, probably because the small number of cases precluded subgroup analysis.
All cases of dementia diagnosed locally in 39 centers, and 50% of the cases of mild cognitive impairment were centrally adjudicated. Agreement in diagnoses was present in about 75% of the cases. Most disagreements resulted in a less serious classification, lowering the hazard ratio for dementia in the pooled participants to 1.54 (1.08-2.21).
In the WHIMS assessment of mental state, differences between treated and placebo groups emerged after 2 years of follow-up.5 The overall increased risk of impaired cognition in the estrogen-only arm was estimated to be 1.47 (1.04-2.07). The adverse effect was concentrated (if not limited) in the participants who had the lowest scores on the mental state test at baseline! Also of note, an as-treated analysis of adherent participants yielded smaller differences. This is a small effect, found in older women (the mean age in WHIMS was 71), exposed to what may be a dose of estrogen relatively high for this age group. Indeed, the WHI authors even state that this difference is "too small to have relevance in clinical practice."
Whether these effects are limited to women with pre-existing cerebrovascular disease is a question that hopefully will be answered when the WHI analyzes their data from magnetic resonance imaging. In addition, long-term follow-up of the youngest postmenopausal women in the overall WHI trial may eventually provide helpful information (but at least 10 or more years from now).
Keep in mind that the participants in the 2 arms of the overall trial were not identical.6 Specifically, the women in the estrogen-only arm had more already-diagnosed cardiovascular disease and greater previous use of hormone therapy, but at the same time, because of hysterectomies and oophorectomies, probably greater exposure to estrogen deficiency earlier in life. Therefore, the appropriateness of combining the 2 canceled arms of the trial (a maneuver designed to gain statistical power) can be questioned.
It is appropriate to conclude that hormone therapy equivalent to an estrogen dose of 0.625 mg conjugated estrogens does not improve cognitive function in older postmenopausal women. This dose of estrogen may adversely affect cognition in women with pre-existing cerebrovascular disease. One cannot disagree, therefore, with the conclusion that this dose of estrogen should not be initiated in women over age 65 in the expectation that deterioration in cognition will be prevented.
References
1. Shumaker SA, et al. JAMA. 2003;289:2651-2662.
2. Rapp SR, et al. JAMA. 2003;289:2663-2672.
3. Shumaker SA, et al. JAMA. 2004;291:2947-2958.
4. Zandi PP, et al. JAMA. 2002;288:2123-2129.
5. Espeland MA, et al. JAMA. 2004;291:2959-2968.
6. Stefanick ML, et al. Ann Epidemiol. 2003;13:S78-S86.
Leon Speroff, MD, Professor of Obstetrics and Gynecology, Oregon Health Sciences University, Portland, and Editor of OB/GYN Clinical Alert.
The womens health initiative reported their results on cognition and dementia combining the canceled estrogen-only arm with the canceled estrogen-progestin arm of the randomized trial; the data are derived from an ancillary study of the trial entitled The Womens Health Initiative Memory Study (WHIMS).Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
