Time to put the gloves on: C. diff patient deaths hit a historic high
Time to put the gloves on: C. diff patient deaths hit a historic high
CDC stresses glove use, warning 'hand washing may not be sufficient.'
By Gary Evans, Executive Editor
Dramatic progress in reducing several major health care associated infections (HAIs) in recent years has been offset by the unrelenting rise of Clostridium difficile, the spore-forming pathogen that can cling steadfast to hands even after washing with soap and water.
 "These infections are linked to at least 14,000 American deaths every year," says Ileana Arias, PhD, principal deputy director at the CDC. "This is a high number, but the failure is more difficult to accept because these are treatable, often preventable deaths."
"These infections are linked to at least 14,000 American deaths every year," says Ileana Arias, PhD, principal deputy director at the CDC. "This is a high number, but the failure is more difficult to accept because these are treatable, often preventable deaths."
Indeed, there are some hopeful signs that hospital collaborative programs and antibiotic stewardship efforts may yet bring this nasty bug to bay. The CDC reported that C. diff infections (CDIs) declined 20% among 71 hospitals in three states participating in targeted prevention collaboratives.1,2
"How did they do that? Well, it involved engagement of the hospital leadership," says Cliff McDonald, MD, chief of the prevention and response branch in the CDC Division of Healthcare Quality Promotion. "It involved using these recommended practices, educating on them, and sharing [data and other information] with other hospitals in these collaboratives. And finally, they used the data for action. I think that there's a real reason for optimism here, especially as [CDI] data becomes more available — these rates all become more transparent and plain to people. I'm optimistic we're going to see this turn around."
 Though there is no national surveillance system for CDI, more states are enacting reporting requirements and a major initiative by the Centers for Medicare and Medicaid (CMS) will come on line in the next few years. Beginning in 2013, all hospitals participating in the CMS Inpatient Prospective Payment System Quality Reporting Program will be required to report facility-wide laboratory-identified (LabID)-CDI events using the CDC's National Healthcare Safety Network (NHSN) to qualify for their 2015 annual payment update. In addition, public reporting of hospital rates will begin in 2014 at the CMS Hospital Compare website.
Though there is no national surveillance system for CDI, more states are enacting reporting requirements and a major initiative by the Centers for Medicare and Medicaid (CMS) will come on line in the next few years. Beginning in 2013, all hospitals participating in the CMS Inpatient Prospective Payment System Quality Reporting Program will be required to report facility-wide laboratory-identified (LabID)-CDI events using the CDC's National Healthcare Safety Network (NHSN) to qualify for their 2015 annual payment update. In addition, public reporting of hospital rates will begin in 2014 at the CMS Hospital Compare website.
While these surveillance efforts will bring the epidemic into sharper focus, data and estimates cobbled together by the CDC from a number of sources are certainly clear enough to see that a formidable infection is attacking the health care system from stem to stern.
From 2000 to 2009, the number of hospitalized patients with any CDI discharge diagnoses more than doubled, from approximately 139,000 to 336,600, and the number with a primary CDI diagnosis more than tripled, from 33,000 to 111,000. CDI sequelae include diarrhea, colitis, toxic megacolon, sepsis, and death. The overall incidence, patient deaths, and excess health-care costs resulting from CDIs in hospitalized patients hit historic highs before plateauing, the CDC reported.
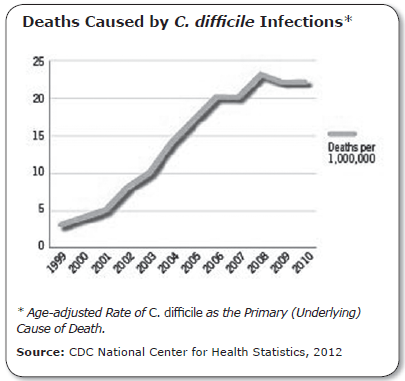
To cite a rather staggering statistic, CDI deaths increased 400% from 2000 to 2007. Almost half of CDI infections occur in people younger than 65, but 90% of deaths related to CDI occur in people 65 and older. Recent excess health-care costs of hospital-onset CDI are estimated to be $5,042–$7,179 per case. Overall, some $1 billion in medical costs are exacted annually by the CDI epidemic, which is being driven by the emergence of the highly virulent North American pulsed-field gel electrophoresis type 1 (NAP1) strain.
"Much of this increase has been related to an epidemic strain that first emerged in the year 2000, which causes more cases and a greater severity of disease," McDonald says.
NAP1, which debuted with a series of deadly hospital outbreaks, has been described as having everything but a sunny disposition: enhanced spore formation, a 20-fold increase in toxins, resistance to fluoroquinolones, lower infectious dose, and ability to survive indefinitely in the environment.
Glove use is key
When you realize that NAP1 is only part of the problem, it's little wonder that C. diff continues to thrive in the absence of extremely intensive efforts and health care collaboratives. The problem has to be attacked on multiple fronts. For example, the very antibiotics that treat other infections may give rise to C. diff, which is practically impervious to the alcohol hand rubs ubiquitous in health care facilities. For this reason, many hospitals have moved back to soap and water for CDI patients, but even traditional hand washing may have little effect on the persistent spores.
The CDC is wary of undermining its critical hand hygiene recommendations, but emphasized glove use over any type of hand hygiene in this most recent report. "Wear gloves and gowns when treating patients with C. diff even during short visits. Hand sanitizer does not kill C. diff and hand washing may not be sufficient," the CDC noted.
This represents something of a shift from the CDC's previous endorsement of the 2008 compendium guidelines that state in an outbreak situation or in dealing with continuing CDI transmission, health care workers should "perform hand hygiene with soap and water preferentially, instead of alcohol hand hygiene products."3 However, a 2009 study led by internationally recognized CDI expert Dale Gerding, MD, found that soap and water doesn't effectively remove the spores.4 In that study, the only soap found effective against C. diff was an industrial soap used in manufacturing to remove substances like printer's ink. As a result, even facilities with high hand hygiene compliance risk ongoing cross transmission of C. diff via the hands of health care workers. "Glove use, with strict adherence to changing between patient contacts, is the best proven method for preventing hand contamination with C. diff from symptomatic patients," the CDC stated.
 The difference may be more of degree than kind, as CDI patients should be in contact precautions that call for the use of gloves when entering patient rooms and during patient care. A CDI prevention bundle used in one of the aforementioned collaboratives — 35 hospitals in New York City — called for use of contact precautions at the first suspicion of CDI, with hands washed with soap and water after removing gloves.
The difference may be more of degree than kind, as CDI patients should be in contact precautions that call for the use of gloves when entering patient rooms and during patient care. A CDI prevention bundle used in one of the aforementioned collaboratives — 35 hospitals in New York City — called for use of contact precautions at the first suspicion of CDI, with hands washed with soap and water after removing gloves.
Contact precautions would begin "at the time the test was ordered or when somebody develops diarrhea," says Brian Koll, MD, FACP, FIDSA, chairman of the NYC collaborative.
In that regard, the current situation with CDI testing is somewhat confusing. Nucleic acid amplification tests can be twice as sensitive as enzyme immunoassays (EIAs) and thus detect CDI more accurately when used in populations with an appropriate pretest probability (i.e., patients with more than three unformed stools in a 24-hour period without an identified cause), the CDC noted. However, in a case of seek and ye shall find, the increased sensitivity of the nucleic acid tests will likely yield higher hospital-onset CDI rates, the CDC warned. Currently, 35% of hospitals in the CDC's NHSN are using nucleic acid tests.
"The EIA tests are a lot cheaper and we know that, but when you start to put the whole ball of wax together t's not clear that EIAs are as cheap as it may look," McDonald says. "People are routinely ordering two or three of them in a row because they know they are not sensitive, and all that does is lead to more false positives. That is a waste of money because you have to isolate people who don't have CDI, and then you are still not catching all the people who do have CDI. It's kind of 'chasing the tail' a little."
Moving across the continuum
Similar to the situation with emerging gram negative rods, C. diff is moving across the health care continuum. Among CDIs identified in the CDC's Emerging Infections Program in 2010, 94% were associated with receiving health care. However, of those, 75% had onset among people not currently hospitalized, including recently discharged patients, outpatients, and nursing home residents.
"C. diff is not just a hospital problem," Arias says. "It's a patient safety concern in every type of medical patient care facility. Medical leadership, clinicians and cleaning staff can prevent these infections by following CDC recommendations and patients even can help catch C. diff early by telling doctors if they have diarrhea within several months of taking antibiotics." (See key tips for prevention, below.)
It takes a village: CDI prevention falls to all The Centers for Disease Control and Prevention recommends the following measures by various groups to prevent Clostridium difficile infections (CDI). Health Care Facility Administrators:
Clinicians:
States and Communities:
Patients:
|
Communication is critical for health care providers as well, given the historic problems with a variety of infections moving between facilities with little information exchanged on patient transfer. The CDC data show that 50% of CDI cases diagnosed in hospitals come in the front door with patients who are transferred or recently discharged from other facilities.
"This means that hospitals and likely other medical facilities as well are partly at the mercy of surrounding facilities, because patients so often transfer back and forth between facilities or are seen by so many providers," McDonald says. "An infection issue in one place can easily become a problem in another practice or facility too. This speaks to the need for strict adherence to infection prevention and control recommendations across all facility types, and the need for greater care coordination."
Indeed, the outsized role of health care is one of the important details in the CDC data, as only about 6% of CDIs are occuring beyond medical settings. Historically, there has been some question — including growing suspicion of retail meats in the food supply — regarding the general estimate that some 20% of CDIs were of unexplained origin.
"In the past, a lot of C. diff infections were considered to happen just generally in the community," says McDonald. "But this report shows that most of these so-called community infections actually occur in people with recent exposure to medical facilities. These infections are now a patient safety concern everywhere medical care is given. [Only] about 25% of C. diff infections first show symptoms among patients in hospitals, [but] hospitals still play a central role in prevention. This is because many of the most potent antibiotics are prescribed in hospitals today and many CDI infections first show symptoms soon after discharge from hospitals."
Fluoroquinolones have been associated with CDI onset, McDonald noted, as have clindamycin and cephalosporins.
A one-two punch
"C. diff infection most often requires a one–two punch of antibiotics plus medical care," he says. "Antibiotics destroy good bacteria that typically protect us from infection, leaving the door open for C. diff to take over. If a person swallows C. diff spores during this time of vulnerability, they can become infected. This usually happens in health care facilities, after a patient picks up C. diff spores from contaminated surfaces or if a health care provider directly spreads the spores to a patient and then the patient touches his or her face." (See CDC graphic of transmission scenario, below)
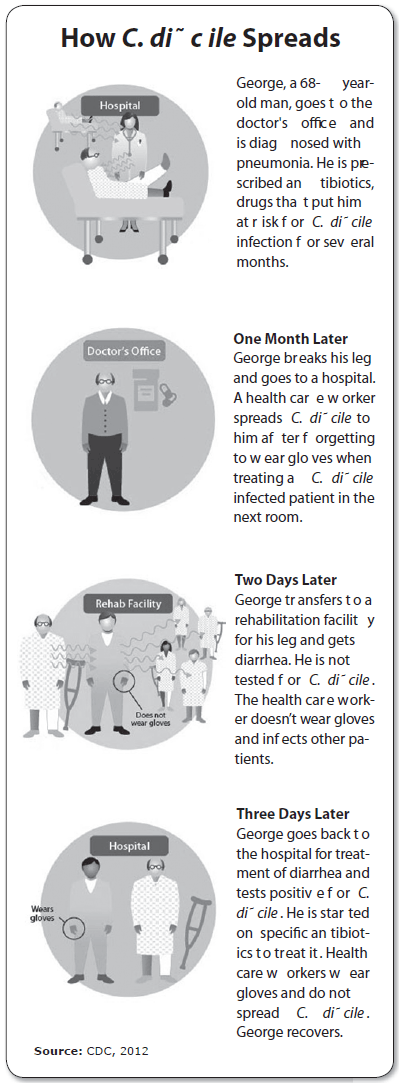
As infection preventionists are well aware, the patient environment is a critical issue, as infectious CDI spores can survive on surfaces and fomites for months. Because the spores resist killing by usual hospital disinfectants, an Environmental Protection Agency–registered disinfectant with a C. diff sporicidal label claim should be used to augment thorough physical cleaning, the CDC recommended.
While antibiotic stewardship programs are being widely discussed as the key intervention to meet the threat of CDI, such basic infection prevention efforts across the continuum are going to be just as important. In that regard, the aforementioned success of the collaboratives occurred largely in the absence of any antibiotic stewardship programs. Though the NYC collaborative is now moving on to an antibiotic stewardship component, the initial idea was to focus "on what we thought we could first control," Koll says.
Antibiotic stewardship has an important role in CDI prevention, but the reality in some cases is that drugs are needed to prevent another infection. "A person may have a life-threatening infection that requires an antibiotic that may also place them at risk for C. diff," McDonald says. "But it is important to avoid unnecessary antibiotic exposures — things like people going to their doctor with a viral illness and being prescribed an antibiotic."
Infections appear to manifest if people ingest C. diff spores within a few days of antibiotic exposure, which is distinctly different from the common misconception that people may already be colonized with the pathogen.
"What we are seeing with C. diff is that it is probably a new acquisition after the antibiotic exposure, rather than C. diff normally residing in the colon and then activating when an antibiotic is taken," he says.
References
- Centers for Disease Control and Prevention. Making Health Care Safer: Stopping Clostridium difficile infections. Vital Signs March 2012: http://1.usa.gov/GDlveX
- CDC. Vital Signs: Preventing Clostridium difficile Infections. MMWR 2012;61(09):157-162
- Society for Healthcare Epidemiology of America. Infectious Disease Society of America. Compendium of Strategies to Prevent Healthcare Associated Infections in Acute Care Hospitals. Infect Control Hosp Epidemiol; 2008;29:S81–S92.
- Edmonds S, Kasper D, Zepka C, et al. Clostridium difficile and hand hygiene: spore removal effectiveness of handwash products. Abstract 43. Society for Healthcare Epidemiology of America. San Diego; March 19 - 22, 2009.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
